Posterior Cervical Foraminotomy: An Intraoperative Masterclass

Key Takeaway
Join us in the OR for a comprehensive masterclass on Posterior Cervical Foraminotomy. This guide covers everything from detailed surgical anatomy and meticulous preoperative planning to the precise, step-by-step intraoperative technique. We'll explore crucial patient positioning, instrument use, and critical pearls to navigate potential pitfalls, ensuring optimal decompression for cervical radiculopathy. Master this essential procedure for superior patient outcomes.
Introduction and Epidemiology
Cervical radiculopathy is a clinical diagnosis defined by the presence of motor or sensory changes or complaints in a specific dermatomal distribution. It represents a significant source of morbidity in the adult population, characterized by neurologic dysfunction resulting from the mechanical compression and subsequent inflammation of the exiting cervical nerve roots. The annual incidence of cervical radiculopathy is estimated to be approximately 83 per 100,000 individuals, with a peak incidence occurring in the fifth and sixth decades of life.

The natural history of cervical radiculopathy demonstrates that while many patients experience spontaneous resolution of acute symptoms, a substantial cohort develops chronic morbidity. Epidemiological data suggest that about half of the adult population will experience neck and radicular symptoms at some point during their lifetime. In patients managed strictly nonoperatively, up to 66% will exhibit persistent symptoms at long term follow up. Furthermore, up to 23% of patients with persistent neck or radicular pain will be unable to return to their original occupation, highlighting the profound socioeconomic impact of this pathology.
Posterior cervical foraminotomy is a classic, motion preserving surgical technique designed to achieve direct neural decompression. By specifically targeting the dorsal compressive elements namely the superior articular facet of the caudal segment and the ligamentum flavum surgeons can relieve pressure on the nerve root without the need for arthrodesis. This approach remains a highly effective intervention for unilateral radiculopathy, particularly in the setting of foraminal stenosis or lateral soft disc herniations.

Surgical Anatomy and Biomechanics
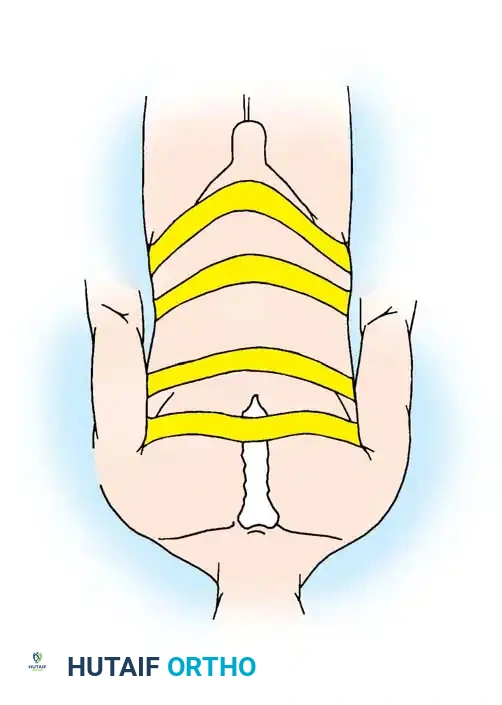
A rigorous understanding of posterior cervical osteology and neural anatomy is paramount for the safe execution of a posterior cervical foraminotomy. Cervical radiculopathy is largely due to mechanical compression of the exiting cervical nerve roots within the intervertebral foramen.

Boundaries of the Intervertebral Foramen
The cervical intervertebral foramen is a dynamic osteoligamentous canal bounded by several critical structures. Ventrally, the foramen is bordered by the intervertebral disc and the uncovertebral joint (joint of Luschka). Cranially and caudally, the borders are defined by the respective pedicles of the adjacent vertebrae. Dorsally, the foramen is bordered by the facet joint (zygapophyseal joint), specifically the superior articular facet of the caudal segment and the inferior articular facet of the cranial segment. For example, at the C5-C6 foramen, the dorsal boundary is predominantly formed by the superior articular facet of C6.

In the subaxial cervical spine, the normal foramen averages 9 to 12 mm in height and 4 to 6 mm in width. In a healthy, young individual, the exiting cervical nerve root occupies approximately one third of the available cross sectional area within the foramen. The nerve root is accompanied by radicular arteries, venous plexuses, and a dural sleeve.
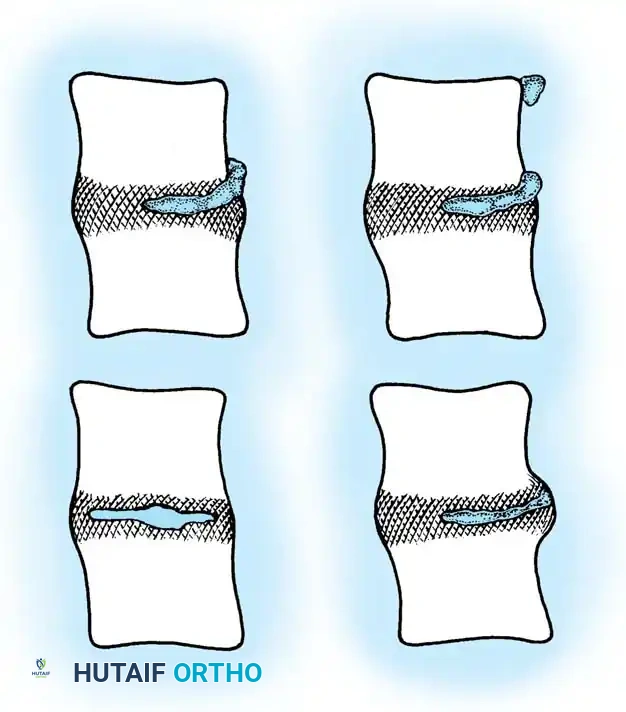
Pathogenesis of Foraminal Stenosis
With increasing age, a cascade of degenerative changes alters the biomechanics and dimensions of the foramen. Any process that causes impingement of the exiting cervical nerve roots can lead to cervical radiculopathy. Potential etiologies include cervical spondylosis leading to foraminal stenosis due to uncinate hypertrophy ventrally or facet hypertrophy dorsally. Disc herniation, segmental instability, and anterolisthesis or retrolisthesis further compromise foraminal volume. As osteophyte formation progresses, the proportion of the foramen occupied by the nerve root increases drastically, leading to mechanical tethering, localized ischemia, and the clinical manifestation of radiculopathy.

Biomechanical Considerations of Facet Resection
The facet joints in the subaxial cervical spine are oriented at approximately 45 degrees to the axial plane and are critical for load sharing and rotational stability. During a posterior foraminotomy, bone is resected from the medial aspect of the facet joint. Biomechanical studies dictate that resection of up to 50% of the medial facet joint does not significantly alter the segmental stability or load bearing capacity of the cervical spine. Resection exceeding 50% risks iatrogenic instability, increased capsular strain, and subsequent subluxation or kyphotic deformity.


Indications and Contraindications
The decision to proceed with a posterior cervical foraminotomy relies on a precise correlation between clinical presentation and advanced imaging. When a patient presents with radiculopathy, a complete history and physical examination is of paramount importance.
Questions must address the duration of symptoms, location and nature of the pain, distribution of altered sensation and numbness, presence of motor weakness, and any associated manifestations. Because radiculopathy can be associated with central canal stenosis, the presence or absence of myelopathic signs balance difficulties, loss of bowel or bladder control, signs of dysdiadochokinesia, Hoffman sign, or hyperreflexia must be elucidated.
Differential Diagnosis
The differential diagnosis for upper extremity radicular pain is broad. Surgeons must distinguish cervical radiculopathy from cervical myelopathy or myeloradiculopathy. Peripheral entrapment syndromes such as pronator syndrome, carpal tunnel syndrome, and cubital tunnel syndrome must be ruled out, occasionally necessitating electromyography and nerve conduction studies. Other differentials include brachial neuritis (Parsonage Turner syndrome), rotator cuff pathology, and superior sulcus tumors (Pancoast tumors).

Selection Criteria for Posterior Foraminotomy
Ideal candidates for posterior cervical foraminotomy possess unilateral radiculopathy driven by posterolateral soft disc herniations or foraminal stenosis secondary to facet hypertrophy. It is particularly advantageous for pathology at the C7-T1 level, where an anterior approach is often obstructed by the sternum and clavicle.
Contraindications include the presence of cervical kyphosis, as posterior element resection can exacerbate deformity. Significant axial neck pain, central canal stenosis, ventral midline disc herniations, and gross segmental instability are also primary contraindications for this motion preserving technique.

| Clinical Scenario | Operative Indication Status | Rationale and Considerations |
|---|---|---|
| Unilateral foraminal soft disc herniation | Primary Indication | Excellent access to lateral recess and foramen; avoids anterior fusion. |
| Foraminal stenosis from facet hypertrophy | Primary Indication | Direct dorsal decompression of the superior articular facet. |
| Cervical Myelopathy | Absolute Contraindication | Posterior foraminotomy does not address central canal stenosis. |
| Cervical Kyphosis | Absolute Contraindication | Posterior resection exacerbates kyphotic deformity and instability. |
| Broad based ventral central disc herniation | Relative Contraindication | Inability to safely retract the cervical spinal cord to retrieve ventral pathology. |
| Multilevel bilateral radiculopathy | Relative Contraindication | Extensive bilateral facet resections increase risk of iatrogenic instability. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is essential to mitigate intraoperative complications and ensure adequate neural decompression.
Imaging Modalities
Plain radiographs of the cervical spine, including anteroposterior, lateral, odontoid, oblique, and lateral flexion and extension views, are utilized initially to evaluate for the presence of cervical pathology, overall sagittal alignment, and dynamic instability. Oblique views are particularly useful for visualizing the osseous boundaries of the intervertebral foramina.
If symptoms have been present for at least 6 weeks and are refractory to conservative management, additional imaging is indicated. Cervical spine magnetic resonance imaging is the gold standard for evaluating soft tissue structures, disc herniations, and neural element compression. If magnetic resonance imaging is contraindicated due to implanted devices, a cervical computed tomography myelogram is highly beneficial. Furthermore, a high resolution computed tomography scan with coronal and sagittal reconstructions is invaluable for operative planning, specifically to assess the degree of facet hypertrophy, osteophyte morphology, and the course of the vertebral artery.

Patient Positioning
The procedure is performed under general endotracheal anesthesia. Neuromonitoring, including somatosensory evoked potentials and motor evoked potentials, is recommended. The patient is positioned prone on a Jackson table or standard operating table with chest rolls.
Cranial stabilization is typically achieved using Mayfield tongs or a Gardner Wells horseshoe headrest. The neck is maintained in a neutral position or slight flexion to open the posterior interlaminar spaces and foramina. Excessive flexion must be avoided to prevent spinal cord tethering or hypoperfusion.

The shoulders are often taped caudally to facilitate intraoperative fluoroscopic visualization of the lower cervical spine. The bed is placed in a reverse Trendelenburg position (approximately 15 to 20 degrees) to decrease venous pressure in the epidural plexus, thereby minimizing intraoperative bleeding.

Detailed Surgical Approach and Technique
The posterior cervical foraminotomy relies on meticulous microsurgical technique to safely expose and decompress the nerve root while preserving the biomechanical integrity of the functional spinal unit.
Incision and Muscular Dissection
Following standard sterile prep and drape, a precise midline longitudinal incision is made centered over the targeted pathology, confirmed via lateral fluoroscopy. The incision is carried down through the subcutaneous tissue to the nuchal ligament.
A subperiosteal dissection of the paraspinal musculature is performed unilaterally on the symptomatic side. The dissection is carried laterally along the spinous process, lamina, and out to the lateral margin of the facet mass. It is critical to strictly preserve the facet joint capsules of the adjacent, non operative levels to prevent adjacent segment instability. Self retaining retractors, such as a McCulloch or a tubular retractor system for minimally invasive approaches, are deployed to maintain exposure.

Identification of Topographical Landmarks
The primary landmark for the foraminotomy is the "V point." This is the junction where the inferior margin of the cranial lamina meets the superior margin of the caudal lamina, transitioning into the medial aspect of the facet joint. The descending inferior articular process of the cranial vertebra overlaps the ascending superior articular process of the caudal vertebra like shingles on a roof.

Osseous Resection and Facet Decompression
Using a high speed drill with a 3 mm cutting burr or a diamond burr, the surgeon begins thinning the lateral aspect of the cranial lamina and the medial aspect of the facet joint. The goal is to perform a "keyhole" foraminotomy (the Scoville technique).
The drilling targets the medial third to medial half of the facet joint. The superior articular facet of the caudal segment is the primary dorsal compressive structure. By resecting the medial aspect of this superior articular facet, the surgeon directly unroofs the dorsal aspect of the intervertebral foramen. Continuous irrigation is utilized to prevent thermal injury to the underlying neural elements.

Ligamentum Flavum Resection and Neural Exposure
Once the bone is thinned to a translucent cortical shell, a micro curette is used to fracture the remaining bone away from the underlying ligamentum flavum. The ligamentum flavum is then carefully resected using 1 mm and 2 mm Kerrison rongeurs.
Removal of the ligamentum flavum exposes the lateral edge of the dura and the proximal portion of the exiting nerve root. The nerve root is enveloped in a venous plexus, which can bleed briskly. Bipolar electrocautery (set at a low wattage) and hemostatic agents such as Gelfoam soaked in thrombin or flowable hemostatic matrices are utilized to achieve hemostasis.

Decompression and Disc Fragment Retrieval
The nerve root is traced laterally along its course through the foramen. A micro nerve hook is passed gently along the dorsal and ventral aspects of the root to confirm patency and ensure no residual osteophytic compression remains from the superior articular facet.
If a soft disc herniation is the primary pathology, the nerve root is gently retracted cranially using a specialized root retractor. The ventral epidural space is explored. An annulotomy is performed if the fragment is not already extruded, and micro pituitary rongeurs are used to retrieve the offending disc material.

Closure
Following copious irrigation and confirmation of absolute hemostasis, the retractors are removed. The fascial layer is closed tightly using interrupted, heavy absorbable sutures to prevent muscular herniation and dead space formation. A subfascial drain may be placed at the surgeon's discretion, particularly if epidural venous bleeding was significant. The subcutaneous tissue and skin are closed in standard layered fashion.
Complications and Management
While posterior cervical foraminotomy is generally safe and effective, surgeons must be prepared to manage several specific intraoperative and postoperative complications.

Iatrogenic instability is a primary concern if excessive bone is resected. Resection of greater than 50% of the facet joint significantly alters the kinematics of the cervical spine, potentially leading to delayed kyphosis or subluxation. If excessive resection occurs intraoperatively, the surgeon must be prepared to convert the procedure to a posterior cervical instrumented fusion.
Neurologic injury, including damage to the exiting nerve root or the spinal cord, is a catastrophic complication. Excessive retraction of the nerve root to access a ventral disc herniation can result in transient or permanent motor deficits. C5 nerve root palsy is a known phenomenon following cervical decompression, often presenting as deltoid and biceps weakness in the immediate postoperative period.
Incidental durotomies can occur during the resection of the ligamentum flavum or manipulation of the nerve root sleeve. Due to the confined space, primary suture repair of a lateral root sleeve tear is exceptionally difficult.
| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Inadequate Neural Decompression | 2% - 5% | Ensure complete resection of the medial superior articular facet. Confirm patency with a nerve hook laterally to the pedicle border. |
| Iatrogenic Instability | < 2% | Limit facet resection to < 50%. Preserve adjacent level capsules. Salvage: Posterior instrumented fusion. |
| Incidental Durotomy | 1% - 4% | Meticulous use of Kerrison rongeurs. Salvage: Fibrin glue, muscle patch, dural sealant matrix, postoperative flat bedrest. |
| Epidural Hematoma | < 1% | Meticulous hemostasis of the epidural venous plexus. Use of subfascial drains. Salvage: Emergent surgical evacuation if neurologic deficit arises. |
| Wrong Level Surgery | < 1% | Mandatory intraoperative fluoroscopic localization prior to incision and after exposure. |
| C5 Nerve Root Palsy | 3% - 7% | Avoid excessive root retraction. Maintain mean arterial pressure intraoperatively. Management is largely supportive and expectant. |
Post Operative Rehabilitation Protocols
Postoperative management following a posterior cervical foraminotomy is focused on early mobilization and restoration of cervical kinematics, as the procedure does not require the biological healing of an arthrodesis.
Patients are typically observed in the post anesthesia care unit for neurologic monitoring and can often be discharged on the same day or following an overnight observation. A soft cervical collar may be provided for one to two weeks strictly for comfort and soft tissue support, though it is not biomechanically required.

During the first two weeks, patients are instructed to perform gentle, pain free isometric neck exercises and avoid heavy lifting (greater than 10 pounds) or extreme ranges of motion. Wound care involves keeping the incision clean and dry until suture removal at approximately 14 days.
Formal physical therapy is initiated at two to four weeks postoperatively, focusing on progressive range of motion, cervical core strengthening, and scapular stabilization. Return to physically demanding occupations or contact sports is generally permitted at 6 to 12 weeks, contingent upon the complete resolution of radicular symptoms, restoration of full motor strength, and a painless range of motion.
Summary of Key Literature and Guidelines
The academic literature robustly supports the efficacy of posterior cervical foraminotomy for the treatment of cervical radiculopathy. Systematic reviews and meta analyses comparing posterior cervical foraminotomy to anterior cervical discectomy and fusion (ACDF) consistently demonstrate equivalent long term outcomes regarding arm pain relief and neurological recovery.
Posterior foraminotomy offers distinct advantages, including the avoidance of anterior approach related complications such as dysphagia, recurrent laryngeal nerve palsy, and esophageal perforation. Furthermore, by preserving the intervertebral disc and avoiding arthrodesis, posterior foraminotomy eliminates the risk of pseudarthrosis and theoretically reduces the incidence of adjacent segment disease associated with rigid fusion constructs.
The advent of minimally invasive surgical (MIS) techniques utilizing tubular retractors has further refined the procedure. MIS posterior cervical foraminotomy has been shown to significantly reduce intraoperative blood loss, minimize paraspinal muscle crush injury, and decrease postoperative axial neck pain compared to traditional open approaches, while maintaining identical decompression efficacy. Guidelines from major spine societies endorse posterior cervical foraminotomy as a first line surgical option for patients with unilateral cervical radiculopathy secondary to foraminal stenosis or lateral disc herniation who have failed exhaustive nonoperative management.
Clinical & Radiographic Imaging



















You Might Also Like