Anatomic Gracilis Autograft Reconstruction for Chronic Lateral Ankle Instability: A Masterclass
Key Takeaway
Join us in the OR for an immersive masterclass on anatomic lateral ankle ligament reconstruction. We'll meticulously guide you through gracilis autograft harvest, precise fibular and talar tunnel creation, graft tensioning, and fixation for chronic instability. This comprehensive session emphasizes critical anatomy, intraoperative pearls, and detailed post-operative management.
Alright, fellows, welcome to the operating theater. Today, we're tackling a challenging but highly rewarding case: chronic lateral ankle instability requiring an anatomic reconstruction. This patient has exhausted nonoperative measures, and we're here to restore stability and function using a gracilis autograft. Pay close attention; this procedure demands precision and a deep understanding of ankle biomechanics and anatomy.
Understanding Lateral Ankle Instability: Preoperative Assessment and Planning
Before we even consider making an incision, a thorough understanding of the patient's history, physical findings, and imaging is paramount. This informs our decision-making and allows us to anticipate and address any concomitant pathologies.
Patient History and Physical Examination
Lateral ligament instability typically follows an inversion injury, often in plantarflexion. While common, only a subset of patients, perhaps 15% to 48%, develop persistent, debilitating instability requiring surgical intervention.
- Symptom Localization: Always ask the patient to remove their socks and shoes. Have them pinpoint the exact area of discomfort with one finger. This helps focus your examination and confirm the primary complaint.
- Activity-Related Instability: Inquire about the relationship between pain and activity, and the specific circumstances of instability episodes. Does the ankle "give way"? When? During running, cutting, or even ambulation on uneven ground? The more detail, the better.
-
Concomitant Pathologies: Lateral ligament disruption rarely occurs in isolation. We must actively seek out associated conditions, such as:
- Osteochondral defects (OCDs) of the talus.
- Hindfoot varus or cavus alignment.
- Peroneal tendon tears or tendinopathy.
- Anterolateral joint impingement.
- Equinus contracture (tight heel cord).
- Tarsal coalition.
- Medial ankle instability (deltoid ligament).
Any significant co-pathology must be addressed concurrently to ensure a successful outcome.
-
Standing and Walking Examination: Observe the patient's gait, looking for subtle signs of instability or compensatory mechanisms. Ask them to heel walk and toe walk.
- Cavus Foot Assessment: Look for a cavus alignment. A "peek-a-boo" heel sign can be diagnostic. If a cavus foot is present, perform a Coleman block test.
- Flexible Cavus: If the heel varus corrects with the block, the hindfoot is flexible, and the cavus is often secondary to a forefoot varus. Correcting the forefoot can then correct the hindfoot through the mobile midfoot.
- Rigid Cavus: If the heel varus does not correct, it's a rigid deformity, potentially requiring a calcaneal osteotomy in addition to forefoot correction.
Comprehensive Surgical Anatomy: The Lateral Ankle Ligamentous Complex
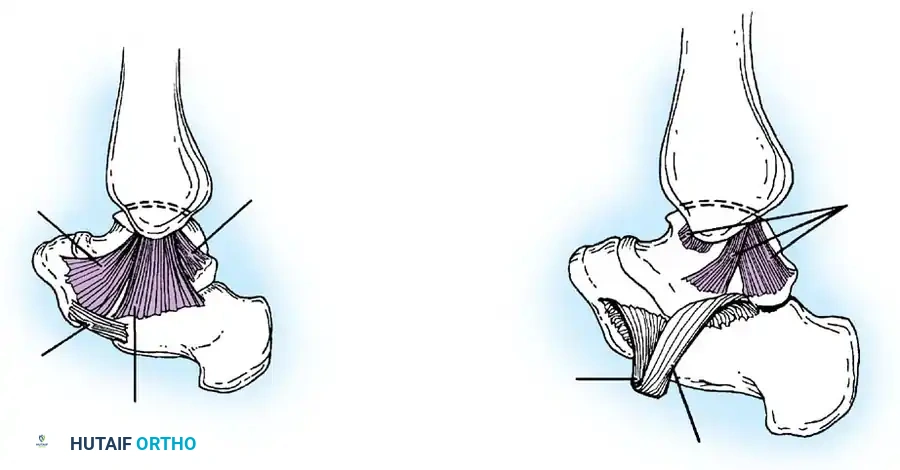
Let's quickly review the key players here, fellows. The lateral collateral ligament complex consists primarily of two distinct ligaments:
- Anterior Talofibular Ligament (ATFL): This is the most commonly injured ligament.
- Origin: Arises from the anterior portion of the distal fibula.
- Insertion: Inserts onto the lateral side of the talar neck.
- Function: Resists anterior translation and medial rotation of the talus on the tibia, especially in plantarflexion.
- Clinical Pearl: Because the ATFL is often injured in plantarflexion, an anterior drawer test is most sensitive in this position.

FIG 1 • Anatomy of the calcaneofibular and anterior talofibular ligaments. (This image would typically show the ATFL and CFL.)
- Calcaneofibular Ligament (CFL):
- Origin: Runs from the anterior tip of the fibula.
- Insertion: Courses deep to the peroneal tendons to insert via a broad base onto the lateral wall of the calcaneus.
- Relationship: Passes superficial to the lateral margin of the posterior facet of the subtalar joint.
- Function: Resists inversion of the talus and calcaneus, particularly in neutral or dorsiflexion.
These ligaments are condensations within the lateral capsule. Understanding their precise origins and insertions is critical for anatomic reconstruction.
- Neurovascular Structures:
- Superficial Peroneal Nerve (SPN): This nerve is a significant risk during lateral ankle approaches. It typically emerges from the deep fascia in the distal leg, approximately 10-15 cm proximal to the tip of the lateral malleolus, and then branches into intermediate dorsal cutaneous and medial dorsal cutaneous nerves. It lies superficial to the peroneal tendons and deep to the skin. Always identify and protect it.
- Deep Peroneal Nerve: While generally anterior and deeper, its terminal branches can be encountered in the anterolateral aspect, especially when dissecting towards the sinus tarsi. Its variable anatomy means we must be vigilant.
- Sural Nerve: Located more posteriorly, it generally supplies sensation to the lateral foot. While less at risk with an anterolateral incision, care must be taken during posterior dissection or if the incision extends too far posteriorly.
- Peroneal Tendons: The peroneus longus and brevis tendons run in a groove posterior to the lateral malleolus. They are dynamic stabilizers of the ankle and foot. Their sheath and retinaculum must be carefully managed to avoid damage or impingement.
Imaging and Other Diagnostic Studies
Our diagnostic workup is comprehensive.
- Plain Radiographs: We routinely obtain weight-bearing AP, lateral, and mortise views of the ankle. These are crucial for identifying:
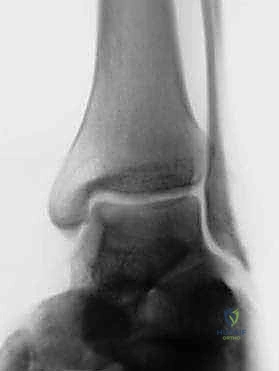
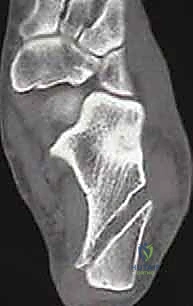
FIG 2 • Radiologic finding of osteochondral lesion of talar dome.
- Specialized Views:
- Calcaneal Axial View/Saltzman View: Useful for assessing hindfoot alignment, especially if a tarsal coalition is suspected due to a stiff hindfoot on exam.
- Tibial Views: For overall limb alignment if malalignment is suspected.
- CT Scan: Provides superior detail for complex osteochondral defects, osteophytes, arthritis, and tarsal coalition, especially if suggested by plain radiographs.
- MRI/MRI Arthrography: The gold standard for soft tissue evaluation. It can detail deficient ligaments, associated chondral and osteochondral lesions, and soft tissue impingement.
- Diagnostic Blocks: Selective local anesthetic blocks of the ankle, subtalar, or talonavicular joints can help localize the source of pain if it's unclear.
- Fluoroscopic Stress Tests: When diagnosis is uncertain, an inversion stress test under fluoroscopy, compared to the contralateral ankle, provides objective evidence of instability.
- Bone Scans: Can assist in determining associated pathology, such as stress fractures or inflammatory conditions.
Differential Diagnosis
Always consider the following:
* Loose body in the ankle joint
* Osteochondral defect of the talus
* Syndesmotic instability (high ankle sprain)
* Peroneal tendinopathy or rupture
* Medial ankle instability
* Cavus foot deformity
* Tarsal coalition
Nonoperative Management
We don't jump to surgery, fellows. Nonoperative treatment is always the first line.
* Physiotherapy: Proprioceptive training and strengthening of dynamic stabilizers (especially peroneal tendons) are crucial. Instability often leads to peroneal weakness and loss of proprioception.
* Bracing: Ankle bracing can aid recovery and prevent future sprains by providing external support and facilitating strengthening.
* Orthotics: For flexible hindfoot varus, a lateral wedge orthotic can be beneficial. If driven by a plantarflexed first ray (Coleman block positive), the orthotic should be "welled out" under the first metatarsal head to allow physiologic valgus progression.
Nonoperative treatment is less effective in the presence of fixed hindfoot varus.
Surgical Management: Indications and Principles
The indication for surgical management is chronic, symptomatic lateral ligament instability despite a diligent course of appropriate nonoperative treatment, including physiotherapy and bracing.
We differentiate between repair and reconstruction:
* Repair: Anatomic tightening of the existing lateral ankle ligaments (e.g., Brostrom procedure). This is preferred when the native ligaments are repairable, not scarred or attenuated, and have sufficient length.
* Reconstruction: Reconstitution of the lateral ankle ligaments using tissue beyond the local physiologic complex.
* Anatomic Reconstruction: Rebuilds the ligaments in their physiologically occurring orientation, mimicking the ATFL and CFL. This is our preference.
* Nonanatomic Reconstruction: Uses tendon transfers (e.g., Evans, Watson-Jones procedures) that do not follow the physiologic orientation. The literature generally favors anatomic over nonanatomic reconstruction due to better biomechanical outcomes.
Today, we're performing an anatomic reconstruction using a gracilis autograft, anchored via drill holes. Our goals are immediate stable fixation, eventual biologic ingrowth to bone, and a truly anatomic reconstruction.
Preoperative Planning and Patient Positioning
This is where we set ourselves up for success.
Patient Positioning
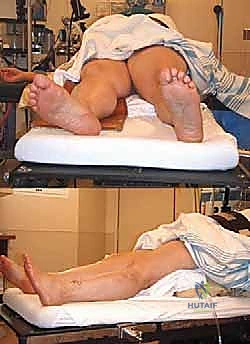
- OR Table Setup: We'll position the patient supine on the operating table.
- Hip Bump/Beanbag: Crucially, we use a beanbag or a large bump placed under the ipsilateral hip (the side we're operating on). This externally rotates the entire extremity, providing excellent access to the lateral ankle.
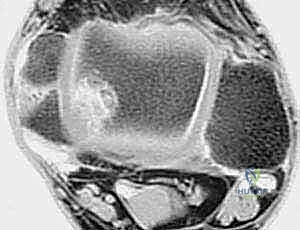
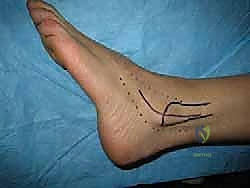
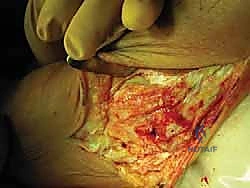
FIG 4 • Patient positioned using bean bag to allow good exposure to the lateral aspect of the ankle.
* Avoiding Full Lateral: A full lateral position is generally avoided as it can restrict access to the proximal medial tibia, which we'll need for gracilis tendon harvest.
* Tourniquet: A wide pneumatic thigh tourniquet is applied to ensure a bloodless field, which is essential for meticulous dissection and nerve protection.
* Preparation and Draping: The entire leg, from just above the knee down to the toes, is meticulously prepared and draped in a sterile fashion. This allows for both the lateral ankle approach and the medial knee incision for gracilis harvest.
* Regional Anesthetic Blocks: If possible, a regional anesthetic block (e.g., popliteal block) is administered preoperatively to ensure appropriate postoperative pain relief.
Final Preoperative Checks
-
Stress Testing Under Anesthesia: Before any incision, with the patient fully relaxed under anesthesia, we perform definitive stress tests. This is our gold standard for confirming the diagnosis and assessing the true extent of instability.
- Open Anterior Drawer Test: With the ankle in slight plantarflexion, we stabilize the tibia posteriorly and translate the calcaneus anteriorly while internally rotating the foot. This assesses ATFL integrity.
- Inversion Stress Test: This assesses CFL integrity.
We compare these findings to the contralateral, physiologically stable ankle.
-
Ankle Arthroscopy (if indicated): If preoperative imaging (MRI) suggests intra-articular pathology such as osteochondral defects, loose bodies, or impingement lesions, we will address these with ankle arthroscopy before proceeding with the open ligament reconstruction. This ensures a comprehensive treatment.
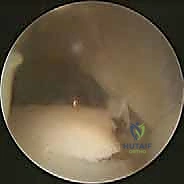
TECH FIG 2 • Osteochondral defect of the talus found on arthroscopy before ligament reconstruction. (This image would show an OCD lesion.)
Intraoperative Execution: The Anatomic Gracilis Reconstruction
Now, let's scrub in.
Step 1: Gracilis Tendon Harvest
We'll start with the autograft harvest, as this takes a bit of time and ensures the graft is ready when we need it.
- Incision: Make a small, longitudinal incision, typically 2-3 cm in length, over the medial aspect of the tibial tubercle, directly over the pes anserinus insertion. This is a well-known anatomical landmark.
- Dissection: Carefully carry the dissection down through the sartorius fascia. You'll then identify the gracilis tendon, which is the most posterior and medial of the pes anserinus tendons.
- Isolation: With the knee flexed to relax the hamstring muscles, meticulously isolate the gracilis tendon. Use a hemostat to gently separate it from the sartorius and semitendinosus tendons.
- Proximal Release: Use a specialized tendon stripper to release the gracilis from its muscular belly proximally. Be careful to ensure a clean harvest and avoid damaging the muscle.
- Distal Division and Preparation: Divide the tendon at its insertion into the bone. Measure the length and diameter of the harvested tendon.
- Whipstitch: Using a No. 2 braided nonabsorbable polyester suture, meticulously reef the tendon with a baseball whipstitch on both ends. This provides strong, secure ends for graft passage and fixation.
- Pearl: Keep the harvested tendon moist in a saline-soaked sponge while we prepare the ankle.
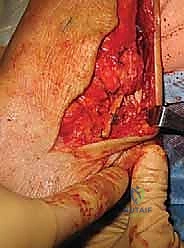
Step 2: Lateral Ankle Approach and Exposure
Now, let's turn our attention to the ankle.
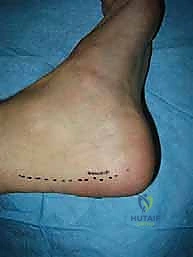
- Skin Incision: We'll use an extensile longitudinal curvilinear approach, which offers superior exposure compared to the traditional J-shaped incision.
- Start: Begin the incision on the distal fibula.
- Course: Continue it over the lateral malleolus.
- Curve: Gently curve it anteriorly towards the sinus tarsi.
- Rationale: This extensile approach not only provides excellent access to the lateral ankle ligaments but also allows for visualization of the distal tibia, peroneal tendons, sinus tarsi, and lateral calcaneus, enabling us to address any adjuvant procedures if warranted.
- Subcutaneous Dissection and Flap Elevation: Carefully elevate full-thickness skin flaps.
- CRITICAL: Superficial Peroneal Nerve Protection: Identify and protect the branches of the superficial peroneal nerve. This nerve has variable anatomy, and meticulous dissection is key. Use blunt dissection and gentle retraction.
- Surgical Warning:
> Surgical Warning: The superficial peroneal nerve is highly susceptible to injury during lateral ankle approaches. Always visualize, isolate, and protect its branches. Injury can lead to distressing neuropathic pain or numbness.
- Deep Dissection - Anterior to Fibula:
- Superior Extensor Retinaculum: Expose the superior extensor retinaculum anterior to the fibula. Carefully strip it off the fibula.
- Extensor Compartment: This dissection exposes the extensor compartment.
- Distal Dissection: Carry the dissection distally towards the ankle joint, reaching the junction between the tibia, talus, and fibula.
- Joint Opening: Carefully open the joint at this level. This controlled dissection ensures that no ligaments are inadvertently damaged during the initial exposure.
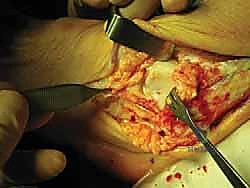
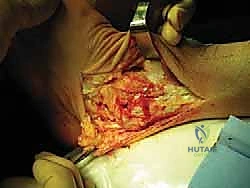
TECH FIG 4 • Lateral dissection anterior to the fibula, sparing the anterior talofibular ligament. (These images would show the dissection anterior to the fibula.)
4. Osteophyte Removal (if present): If anterior osteophytes are present, use a small osteotome and mallet to carefully remove them, addressing any potential anterior impingement.
5. Open Stress Tests (Final Confirmation): With the joint now open, we perform the open anterior drawer and inversion stress tests again. This is our final, definitive assessment of the integrity of the lateral collateral ligaments in situ.
TECH FIG 5 • Open anterior drawer test. Talus is anterior and internally rotated relative to fibula, indicating a positive test and insufficiency of the anterior talofibular ligament.
* Decision Point: At this stage, we reassess. If the ligaments are clearly torn off bone, not excessively scarred or thickened, and have sufficient length, a direct repair (Brostrom) might be considered. However, in this patient, with chronic, severe instability and attenuated ligaments, reconstruction is warranted.
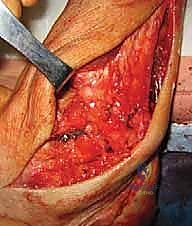
Step 3: Fibular Exposure and Peroneal Tendon Assessment
- Peroneal Fascia Incision: Expose the fibula by carefully incising part of the peroneal fascia. This will expose the peroneal tendons (longus and brevis) and the posterior fibula.
- Peroneal Tendon Assessment: This is an opportune moment to thoroughly examine the peroneal tendons.
- Inspection: Look for signs of tendinopathy, tears, or subluxation.
- Palpation: Gently palpate the tendons for any thickening or crepitus.
- Retinaculum: If peroneal pathology is identified, the peroneal retinaculum may need to be incised, ideally with a step-cut, to allow for complete exposure, debridement, or repair of the tendons. This step-cut allows for a stronger repair later.
- Surgical Warning:
> Surgical Warning: Always assess the peroneal tendons. Missed peroneal pathology is a common cause of persistent symptoms after lateral ankle ligament surgery.
Step 4: Preparing the Ligamentous Insertions and Osseous Tunnels
Now, we prepare the bone for our new ligaments.
- Ligament Incision and Bone Exposure: Carefully incise the remnants of the native collateral ligaments (ATFL and CFL). Dissect down to the origins of both ligaments on the calcaneus and talus, clearing these areas meticulously onto bone.
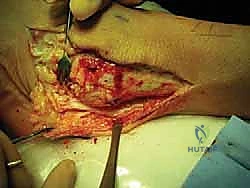
TECH FIG 6 • Dissection of the talus with exposure of the insertion of the anterior talofibular ligament.
-
Graft Sizing: Recall the diameter of your harvested gracilis tendon. Select a drill bit that matches this size (typically 3.5 mm, 4.5 mm, or 6 mm). This ensures a snug fit for the graft. Alternatively, if using an interference screw system, select the screw and drill bit size matched to the tendon's diameter.
-
Fibular Drill Holes: This is where precision is key to recreate the anatomic paths of the ATFL and CFL.
- CFL Tunnel (Inferior Fibular Hole):
- Entry Point: Make the first fibular drill hole starting at the precise anatomical insertion of the CFL on the fibula.
- Trajectory: Drill obliquely, aiming to exit the posterior fibula.
- Surgical Warning:
> Surgical Warning: Ensure the drill trajectory avoids damaging the peroneal tendons or their sheath posteriorly. Use a drill guide or protect the posterior structures with a blunt elevator.
- ATFL Tunnel (Superior Fibular Hole):
- Entry Point: Make the second fibular drill hole starting at the precise anatomical insertion of the ATFL on the anterior fibula.
- Trajectory: Drill obliquely, aiming to exit the posterior fibula, approximately 1 cm above the exit point of the previous CFL fibular drill hole. This maintains the distinct anatomic separation of the two ligaments.
- CFL Tunnel (Inferior Fibular Hole):
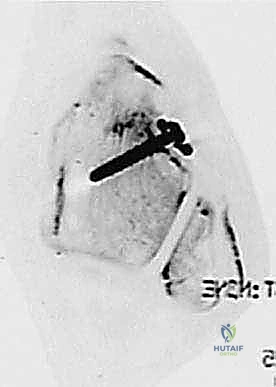
TECH FIG 10 • (This image would show the two distinct drill holes in the fibula, exiting posteriorly.)
- Talar Drill Hole:
- Entry Point: Create a 2.5 mm pilot drill hole precisely in the center of the junction between the talar body and neck – this is the anatomical insertion site of the ATFL on the talus.
- Depth Measurement: Measure the depth of this pilot hole.
- Screw Preparation: A fully threaded cancellous small-fragment screw, along with small and large-fragment washers, should be readily available on the back table, sized appropriately for the talar bone. This screw will serve as the anchor for the talar limb of the graft.
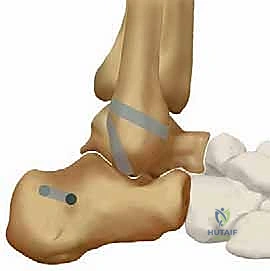
TECH FIG 11 • (This image would show the drill hole in the talar neck.)
Step 5: Graft Passage and Fixation
Now, we bring our prepared gracilis graft into the field and begin the reconstruction.
- Graft Preparation: Our gracilis tendon, whipstitched on both ends, is now ready. We'll fold it in half, creating a loop.
- Fibular Tunnel Passage:
- Passage through Superior Fibular Hole: Pass the looped end of the gracilis graft through the superior fibular drill hole (the ATFL tunnel) from anterior to posterior.
- Retrieval: Retrieve the two free ends of the graft from the posterior fibular exit points.
- Surgical Warning:
> Surgical Warning: Ensure the graft passes smoothly without kinking or excessive friction. Use a passing suture or a small curved clamp if needed. Avoid damaging the graft during passage.
- Talus and Calcaneus Attachment (The "Y" Configuration):
- Talar Limb: Take one of the free ends of the graft and pass it through the 2.5 mm talar drill hole.
TECH FIG 12 • (This image would show the graft passed through the fibula and one limb secured in the talus.)
* Calcaneal Limb: Take the remaining free end of the graft. This will form our reconstructed CFL.
* Calcaneal Tunnel Creation (if needed): A calcaneal drill hole is typically made from the anatomical insertion of the CFL on the lateral calcaneus, aiming medially. The drill hole should be sized to match the graft.
* Graft Passage: Pass the free end of the graft through this calcaneal tunnel.
TECH FIG 13 • (This image would show the graft passed into the calcaneus.)
- Tensioning and Final Fixation: This is arguably the most critical step for restoring stability.
- Ankle Position: Position the ankle in slight plantarflexion and neutral inversion/eversion. This is the optimal position for tensioning the lateral ligaments.
- Tensioning: Apply appropriate tension to both the talar (ATFL) and calcaneal (CFL) limbs of the graft. The goal is to restore normal anatomical tension without overtightening, which could lead to stiffness or impingement.
- Fixation: Secure the calcaneal limb of the graft. This can be done with an interference screw within the calcaneal tunnel, or by suturing the graft limb back onto itself or to the periosteum/soft tissues around the calcaneus.
TECH FIG 14 • (This image would show the final tensioning and fixation of the calcaneal limb.)
* Surgical Warning:
> Surgical Warning: Overtensioning can lead to an iatrogenic varus deformity or restrict ankle motion. Undertensioning will result in persistent instability. Aim for a firm, anatomical feel. Perform gentle stress tests to confirm stability.
- Reinforcement (Optional): The remnants of the native lateral ankle capsule and retinaculum can be imbricated over the reconstructed ligaments to further reinforce the repair.
Step 6: Wound Closure
- Irrigation: Thoroughly irrigate the surgical site with sterile saline.
- Peroneal Retinaculum Repair (if incised): If the peroneal retinaculum was incised with a step-cut, meticulously repair it using non-absorbable sutures. This prevents peroneal tendon subluxation.
- Fascial Closure: Close the subcutaneous layers using absorbable sutures.
- Skin Closure: Close the skin incision with staples or non-absorbable sutures.
- Dressing: Apply a sterile dressing and a well-padded splint (e.g., posterior splint) to maintain the ankle in a neutral or slightly dorsiflexed position, protecting the reconstruction.
Pearls and Pitfalls
- Nerve Injury: The superficial peroneal nerve is the most common iatrogenic injury. Always identify, protect, and gently retract. If symptoms of nerve irritation arise post-op, consider conservative measures initially, but be prepared for exploration if severe or persistent.
- Missed Concomitant Pathology: Failing to address OCDs, peroneal tears, or hindfoot malalignment will lead to persistent symptoms. A thorough preoperative workup and intraoperative vigilance are key.
- Graft Tunnel Placement: Inaccurate drill hole placement will result in a non-anatomic reconstruction and biomechanical failure. Use anatomical landmarks and consider fluoroscopic guidance for challenging cases.
- Graft Tensioning: This is an art. Too loose, and instability persists. Too tight, and stiffness, pain, or even iatrogenic varus can occur. Practice makes perfect.
- Hardware Failure/Prominence: Ensure screws are flush and not prominent, particularly in the talus, to avoid impingement or irritation.
- Infection: Standard surgical precautions. A bloodless field and meticulous technique minimize infection risk.
- Stiffness:
Additional Intraoperative Imaging & Surgical Steps
REFERENCES
-
Juliano PJ, Jordan JD, Lippert FG, et al. Persistent postoperative pain after the Chrisman-Snook ankle reconstruction. Am J Orthop 2000; 29:449.
-
Kaikkonen A, Kannus P, Jarvinen M. Surgery versus functional treatment in ankle ligament tears: a prospective study. Clin Orthop Relat Res 1996;326:194–202.
-
Kaikkonen A, Lehtonen H, Kannus P, et al. Long-term functional outcome after surgery of chronic ankle instability: a 5-year follow-up study of the modified Evans procedure. Scand J Med Sci Sports 1999;9:239.
-
Karlsson J, Bergsten T, Lansinger O, et al. Lateral instability of the ankle treated by the Evans procedure: a long-term clinical and radiological follow-up. J Bone Joint Surg Br 1988;70B:476.
-
Karlsson J, Brandsson S, Kalebo P, et al. Surgical treatment of concomitant chronic ankle instability and longitudinal rupture of the peroneus brevis tendon. Scand J Med Sci Sports 1998;8:42.
-
Karlsson J, Lansinger O. Chronic lateral instability of the ankle in athletes. Sports Med 1993;16:355.
-
Karlsson J, Lansinger O. Lateral instability of the ankle joint. Clin Orthop Relat Res 1992;276:253–261.
-
Karlsson J, Lansinger O: Lateral instability of the ankle joint (1). Non-surgical treatment is the first choice—20 per cent may need ligament surgery. Lakartidningen 1991;88:1399.
-
Karlsson J, Wiger P. Longitudinal split of the peroneus brevis tendon and lateral ankle instability: treatment of concomitant lesions. J Athlet Train 2002;37:463.
-
Kennedy MP, Coughlin MJ. Peroneus longus rupture following a modified Evans lateral ankle ligament reconstruction. Orthopedics 2003;26:1059.
-
Krips R, Brandsson S, Swensson C, et al. Anatomical reconstruction and Evans tenodesis of the lateral ligaments of the ankle: clinical and radiological findings after follow-up for 15 to 30 years. J Bone Joint Surg Br 2002;84B:232.
-
Labs K, Perka C, Lang T. Clinical and gait-analytical results of the modified Evans tenodesis in chronic fibulotalar ligament instability. Knee Surg Sports Traumatol Arthrosc 2001;9:116.
-
Larsen E, Lund PM. Peroneal muscle function in chronically unstable ankles: a prospective preoperative and postoperative electromyographic study. Clin Orthop Relat Res 1991;272:219–226.
-
Mack RP. Ankle injuries in athletics. Clin Sports Med 1982;1:71.
-
Nimon GA, Dobson PJ, Angel KR, et al. A long-term review of a modified Evans procedure. J Bone Joint Surg Br 2001;83B:14.
-
Orava S, Jaroma H, Weitz H, et al. Radiographic instability of the ankle joint after Evans repair. Acta Orthop Scand 1983;54:734.
-
Paterson R, Cohen B, Taylor D, et al. Reconstruction of the lateral ligaments of the ankle using semi-tendinosis graft. Foot Ankle Int 2000; 21:413.
-
Rosenbaum D, Becker H, Sterk J, et al. Functional evaluation of the 10-year outcome after modified Evans repair for chronic ankle instability. Foot Ankle Int 1997;18:765.
-
Rubin A, Sallis R. Evaluation and diagnosis of ankle injuries. Am Fam Physician 1996;54:1609.
-
Sammarco GJ, DiRaimondo CV. Surgical treatment of lateral ankle instability syndrome. Am J Sports Med 1988;16:501.
-
Sammarco VJ. Complications of lateral ankle ligament reconstruction. Clin Orthop Relat Res 2001;391:123–132.
-
Sugimoto K, Takakura Y, Kumai T, et al. Reconstruction of the lateral ankle ligaments with bone-patellar tendon graft in patients with chronic ankle instability: a preliminary report. Am J Sports Med 2002;30:340. 47. van der Rijt AJ, Evans GA. The long-term results of Watson-Jones tenodesis. J Bone Joint Surg Br 1984;66B:371.
-
Vertullo C. Unresolved lateral ankle pain: it’s not always “just a sprain.” Aust Fam Physician 2002;31:247.
- Anderson ME. Reconstruction of the lateral ligaments of the ankle using the plantaris tendon. J Bone Joint Surg Am 1985;67A:930.
-
Baltopoulos P, Tzagarakis G, Kaseta M. Midterm results of a modified Evans repair for chronic lateral ankle instability. Clin Orthop Relat Res 2004;422:180.
-
Barbari S, Brevig K, Egge T. Reconstruction of the lateral ligamentous structures of the ankle with a modified Watson-Jones procedure. Foot Ankle 1987;7:362.
-
Baumhauer JF, O’Brien T. Surgical considerations in the treatment of ankle instability. J Athlet Train 2002;37:458.
-
Becker HP, Rosenbaum D. Chronic recurrent ligament instability on the lateral ankle. Orthopade 1999;28:483.
-
Becker HP, Rosenbaum D, Zeithammer G, et al. Gait pattern analysis after ankle ligament reconstruction (modified Evans procedure). Foot Ankle Int 1994;15:477.
-
Bosien WR, Staples OS, Russell SW. Residual disability following acute ankle sprains. J Bone Joint Surg Am 1955;37A:1237.
-
Boszotta H, Sauer G. Chronic fibular ligament insufficiency at the upper ankle joint: late results after modified Watson-Jones plastic surgery. Unfallchirurg 1989;92:11.
-
Boyer DS, Younger AS. Anatomic reconstruction of the lateral ligament complex of the ankle using a gracilis autograft. Foot Ankle Clin 2006;11:585.
-
Brostrom L. Sprained ankles. V. Treatment and prognosis in recent ligament ruptures. Acta Chir Scand 1966;132:537.
-
Colville MR. Surgical treatment of the unstable ankle. J Am Acad Orthop Surg 1998;6:368.
-
Colville MR, Grondel RJ. Anatomic reconstruction of the lateral ankle ligaments using a split peroneus brevis tendon graft. Am J Sports Med 1995;23:210.
-
Colville MR, Marder RA, Zarins B. Reconstruction of the lateral ankle ligaments: a biomechanical analysis. Am J Sports Med 1992;20:594.
-
Coughlin MJ, Matt V, Schenck RC Jr. Augmented lateral ankle reconstruction using a free gracilis graft. Orthopedics 2002;25:31.
-
Coughlin MJ, Schenck RC Jr, Grebing BR, et al. Comprehensive reconstruction of the lateral ankle for chronic instability using a free gracilis graft. Foot Ankle Int 2004;25:231.
-
Eskander M, Macdonald R. Watson-Jones tenodesis for chronic ankle joint instability. J Roy Army Med Corps 1993;139:115.
-
Evans DL. Recurrent instability of the ankle; a method of surgical treatment. Proc Roy Soc Med 1953;46:343.
-
Evans GA, Frenyo SD. The stress-tenogram in the diagnosis of ruptures of the lateral ligament of the ankle. J Bone Joint Surg Br 1979; 61B:347.
-
Evans GA, Hardcastle P, Frenyo AD. Acute rupture of the lateral ligament of the ankle: to suture or not to suture? J Bone Joint Surg Br 1984;66B:209.
-
Fujii T, Kitaoka HB, Watanabe K, et al. Comparison of modified Brostrom and Evans procedures in simulated lateral ankle injury. Med Sci Sports Exerc 2006;38:1025.
-
Girard P, Anderson RB, Davis WH, et al. Clinical evaluation of the modified Brostrom-Evans procedure to restore ankle stability. Foot Ankle Int 1999;20:246.
-
Hedeboe J, Johannsen A. Recurrent instability of the ankle joint: surgical repair by the Watson-Jones method. Acta Orthop Scand 1979; 50:337.
-
Hintermann B, Boss A, Schafer D. Arthroscopic findings in patients with chronic ankle instability. Am J Sports Med 2002;30:402.
-
Horstman JK, Kantor GS, Samuelson KM. Investigation of lateral ankle ligament reconstruction. Foot Ankle 1981;1:338.