Mastering Forefoot and Midfoot Reconstruction: PIPJ Deformities, Sesamoidectomy, and Lisfranc Stability
Key Takeaway
Flexion deformities of the proximal interphalangeal joints (PIPJ), commonly presenting as hammertoes, require meticulous surgical correction to restore forefoot biomechanics. This comprehensive guide details the dorsal elliptical incision approach, phalangeal head resection, and K-wire stabilization. Furthermore, it explores the critical anatomy of the Lisfranc complex, midfoot column stability, and adjunctive procedures such as fibular sesamoidectomy, providing orthopedic surgeons with an evidence-based framework for complex forefoot and midfoot reconstruction.
INTRODUCTION TO FOREFOOT AND MIDFOOT RECONSTRUCTION
The surgical management of the forefoot and midfoot requires a profound understanding of intricate biomechanical relationships, soft-tissue balancing, and osseous architecture. Deformities in this region rarely exist in isolation; a flexion deformity of the proximal interphalangeal joint (PIPJ), commonly known as a hammertoe, is frequently associated with first ray pathology, such as hallux valgus or hallux rigidus, and underlying midfoot instability.
This comprehensive academic guide delineates the evidence-based surgical techniques for correcting PIPJ flexion deformities, performing a safe fibular sesamoidectomy, executing first metatarsophalangeal (MTP) joint arthrodesis, and understanding the complex stabilizing mechanisms of the midfoot and Lisfranc articulation.
CORRECTION OF FLEXION DEFORMITIES OF THE PROXIMAL INTERPHALANGEAL JOINTS
Flexion deformities of the lesser toe PIPJs are primarily driven by an imbalance between the intrinsic and extrinsic musculature of the foot. When conservative measures—such as extra-depth footwear, crest pads, and taping—fail to alleviate painful dorsal callosities or tip-of-toe ulcerations, surgical intervention is indicated. The cornerstone of rigid hammertoe correction is the resection arthroplasty or arthrodesis of the PIPJ.
Pathomechanics and Preoperative Considerations
A rigid PIPJ flexion deformity occurs when the plantar plate and collateral ligaments contract, tethering the joint in a flexed posture. The extensor digitorum longus (EDL) loses its mechanical advantage at the PIPJ, while the flexor digitorum longus (FDL) exerts an unopposed deforming force. Surgical correction must address both the bony deformity and the contracted soft tissue envelope.
Surgical Technique: PIPJ Resection Arthroplasty
The goal of this procedure is to decompress the joint, realign the digit, and provide a stable, functional toe that clears the toe box of standard footwear.
- Incision and Exposure:
Begin with a dorsal elliptical incision centered over the PIPJ. The ellipse should be oriented transversely or longitudinally depending on the redundancy of the dorsal skin. Excision of this skin wedge is critical; it removes the hyperkeratotic lesion (corn) and utilizes the subsequent skin closure to mechanically splint the toe in extension.
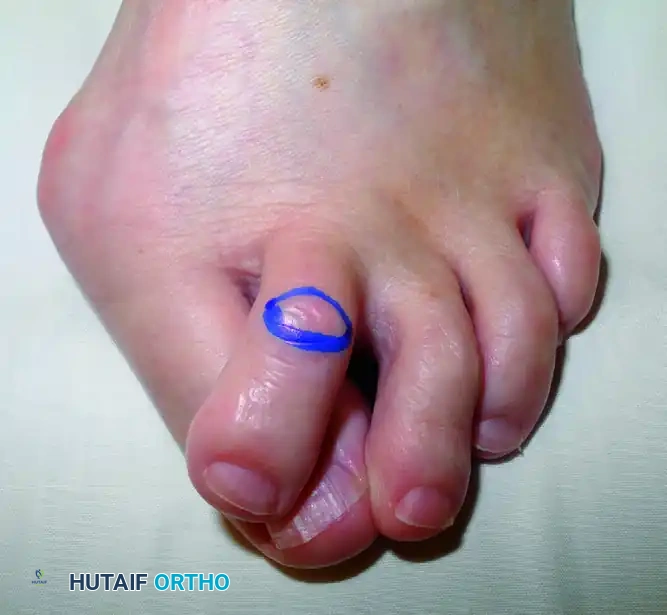
-
Capsulotomy and Ligament Release:
Deepen the incision through the subcutaneous tissue, taking care to retract the dorsal cutaneous nerves. Perform a transverse tenotomy of the extensor tendon over the joint, or split it longitudinally to expose the PIPJ capsule. Perform a thorough collateral ligament release to allow the proximal phalanx head to be delivered into the wound. -
Bone Resection:
Using a microsaw or sharp bone-cutting forceps, excise the head and neck of the proximal phalanx. The resection must be perpendicular to the long axis of the phalanx. Ensure sufficient bone is removed to allow the toe to rest in a neutral position without tension.
🔪 Surgical Pearl: Bone Resection
Inadequate bone resection is the leading cause of recurrent deformity and vascular compromise upon straightening the digit. The toe should easily rest in neutral alignment; if tension persists, resect an additional 1 to 2 mm of the proximal phalanx.
- Internal Fixation (Optional but Recommended):
While some surgeons rely solely on the elliptical skin closure and a meticulously applied forefoot dressing for stability, internal fixation is highly recommended for rigid deformities. - Insert a 0.054-inch Kirschner wire (K-wire) in a retrograde fashion.
- Drive the wire from the resected surface of the middle phalanx, through the distal phalanx, exiting the tip of the toe.
- Reduce the PIPJ and drive the K-wire proximally into the medullary canal of the proximal phalanx and into the lesser metatarsal remnant.
-
Ensure the MTP joint is held in neutral or slight plantarflexion during wire advancement to prevent iatrogenic MTP joint hyperextension.
-
Closure:
Close the dorsal wound over the lesser toe PIPJs using 3-0 or 4-0 nonabsorbable monofilament suture (e.g., nylon). If K-wires are utilized, bend the distal ends to prevent proximal migration and cap them with commercially supplied protective balls to prevent snagging.
ADJUNCTIVE FIRST RAY PROCEDURES: FIBULAR SESAMOIDECTOMY AND MTP ARTHRODESIS
Severe forefoot deformities often necessitate concurrent management of the first ray. In cases of advanced hallux valgus with severe lateral subluxation of the sesamoid apparatus, or during a first MTP joint arthrodesis, a fibular sesamoidectomy may be required.
Surgical Technique: Fibular Sesamoidectomy
The fibular (lateral) sesamoid is embedded within the lateral head of the flexor hallucis brevis (FHB) tendon. Its removal must be performed with meticulous attention to the surrounding neurovascular structures.
-
Identification and Grasping:
Through the primary surgical approach (often a dorsal or medial incision depending on the concurrent procedure), identify the fibular sesamoid. Clasp the sesamoid firmly with a Kocher clamp and apply medial traction. -
Dissection:
Free the soft tissue surrounding the fibular sesamoid using blunt dissection. Proceed with sharp dissection to release the intersesamoidal ligament and the lateral head of the FHB.
🚨 Surgical Warning: Neurovascular Bundle
Extreme caution must be exercised at the proximal lateral border of the fibular sesamoid. The neurovascular bundle supplying the first web space is highly vulnerable in this region. Keep the scalpel blade directed strictly toward the bone of the sesamoid to avoid catastrophic nerve injury.
- Hemostasis and Tendon Inspection:
Once the sesamoid is excised, thoroughly inspect the flexor hallucis longus (FHL) tendon to ensure it has not been inadvertently lacerated. Cauterize any bleeding vessels immediately, as the highly vascular bed of the sesamoid apparatus can lead to significant postoperative hematoma.
First MTP Joint Arthrodesis Fixation
When performing a first MTP joint arthrodesis (often indicated for hallux rigidus or severe, recurrent hallux valgus), the method of internal fixation dictates the biomechanical stability of the construct.
- Preferred Construct: The gold standard in modern operative orthopedics is the use of an obliquely placed headless compression screw (crossing the arthrodesis site) augmented with a precontoured dorsal neutralization plate. This construct provides superior resistance to plantar gapping during the terminal stance phase of gait.
- Length Considerations: The final length of the hallux is critical for forefoot mechanics. The hallux should not be more than 6 to 8 mm longer than the second toe. Excessive length leads to shoe-wear difficulties and increased lever-arm forces on the arthrodesis site, while excessive shortening compromises the windlass mechanism.
MIDFOOT AND LISFRANC JOINT COMPLEX: ANATOMY AND INSTABILITY
The midfoot serves as the critical transition zone between the mobile forefoot and the rigid hindfoot. Instability of the tarsometatarsal (Lisfranc) joint complex can result from high-energy trauma, subtle athletic injuries, progressive osteoarthritis, or inflammatory arthropathies (such as rheumatoid arthritis or Charcot neuroarthropathy).
Regardless of the etiology, failure of the midfoot architecture leads to progressive collapse of the longitudinal arch, debilitating pain due to altered joint mechanics, and the formation of dorsal and plantar bony prominences that make shoe wear nearly impossible.
The Three Columns of the Midfoot
Biomechanically and anatomically, the midfoot is divided into three distinct functional columns:
- The Medial Column: Comprises the first metatarsal and the medial cuneiform. This column possesses a small degree of sagittal plane mobility, essential for accommodating uneven terrain and facilitating the windlass mechanism.
- The Middle Column: Comprises the second and third metatarsals articulating with the middle and lateral cuneiforms, respectively. This is the most rigid column, acting as the central stabilizing strut of the foot.
- The Lateral Column: Comprises the fourth and fifth metatarsals articulating with the cuboid. This column is highly mobile, allowing for triplanar accommodation during the contact phase of gait.
Radiographic Alignment Parameters
Proper alignment of the midfoot is assessed using specific radiographic parameters on weight-bearing anteroposterior (AP) and oblique views:
* The medial border of the first metatarsal base must align perfectly with the medial border of the medial cuneiform.
* The medial border of the second metatarsal base must align with the medial border of the middle cuneiform.
* The medial border of the fourth metatarsal base must align with the medial border of the cuboid.
The "Roman Arch" and Osseous Stability
The inherent stability of the midfoot is derived from its unique coronal plane architecture. The cuneiforms are wedge-shaped, being significantly wider dorsally than plantarly. When articulated, they form a structural "Roman arch."
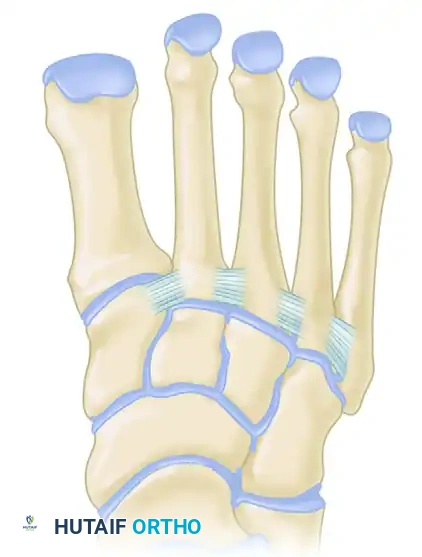
Furthermore, the base of the second metatarsal is recessed proximally between the medial and lateral cuneiforms, locking it into place like the keystone of an arch. This osseous mortise severely limits translation in the transverse and coronal planes.
Ligamentous Anatomy: The Lisfranc Complex
While the bony architecture provides static stability, the ligamentous network is the primary restraint against dynamic deforming forces.
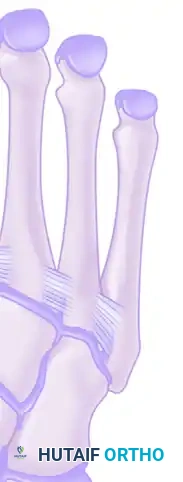

- The Lisfranc Ligament: Crucially, there is no intermetatarsal ligament connecting the base of the first metatarsal to the base of the second metatarsal. Instead, the critical stabilizing structure is the Lisfranc ligament, a robust plantar intra-articular ligament that originates on the lateral aspect of the medial cuneiform and inserts onto the medial aspect of the second metatarsal base.
- Secondary Stabilizers: Stability is further augmented by tight plantar ligamentous attachments, the plantar fascia, and dynamic stabilizers including the peroneus longus, adductor hallucis, flexor hallucis brevis, tibialis posterior, and tibialis anterior.
Disruption of the Lisfranc ligament, even without fracture, uncouples the medial and middle columns, leading to rapid diastasis, arch collapse, and severe degenerative joint disease if left untreated.
WOUND CLOSURE AND HEMOSTASIS PROTOCOLS
Meticulous soft tissue handling and hemostasis are paramount in forefoot surgery to prevent wound dehiscence, infection, and excessive scarring.
- Capsular and Skin Closure:
- Close the joint capsules with 2-0 or 3-0 absorbable sutures (e.g., Vicryl) to restore the soft tissue tension band.
- Close the dorsal skin with 3-0 or 4-0 monofilament nylon.
-
For plantar incisions (if utilized), close the thick plantar skin with 3-0 monofilament nylon, ensuring the edges are perfectly everted. Use 4-0 nylon for filler stitches if protruding plantar fat is a problem. Always try to preserve as much plantar fat pad as possible, as it is critical for weight-bearing cushioning.
-
Tourniquet Release and Hemostasis:
Release the pneumatic tourniquet or Esmarch wrap prior to final dressing application. Carefully inspect all wounds for pulsatile bleeding and cauterize vessels as needed.
💡 Clinical Pearl: Managing Diffuse Bleeding
Diffuse, non-pulsatile bleeding is exceedingly common in orthopedic foot and ankle patients due to the prolonged preoperative use of nonsteroidal anti-inflammatory drugs (NSAIDs), which inhibit platelet aggregation. Placing the patient in the Trendelenburg position during wound closure decreases venous hydrostatic pressure in the lower extremity and is usually sufficient to obtain hemostasis after major pulsatile vessels have been controlled.
- Dressing Application:
Apply a conforming, nonconstricting, bulky compression forefoot dressing. The dressing acts as a soft-tissue splint; it must hold the toes in their corrected alignment without causing vascular compromise.
POSTOPERATIVE CARE AND REHABILITATION
The success of forefoot and midfoot reconstruction relies heavily on strict adherence to postoperative protocols.
- Immediate Postoperative Phase (0-72 Hours):
Strict elevation of the operative extremity is mandatory for the first 72 hours to mitigate edema and prevent wound complications. Ambulation is strictly limited to bathroom privileges using a walker or with assistance. - Early Mobilization (72 Hours to 4 Weeks):
After 72 hours, ambulation to tolerance is permitted. The patient is transitioned to a firm-soled, rigid postoperative shoe to protect the osteotomies and arthrodesis sites from bending moments. Crutches or a walker are usually not required unless dictated by patient frailty or concurrent hindfoot procedures. - Intermediate Phase (4 to 12 Weeks):
At 4 weeks, assuming clinical and radiographic signs of healing are present, K-wires (if used for PIPJ correction) are removed in the clinic. The patient is transitioned to a deep, wide, jogging-type shoe for an additional 6 to 8 weeks to accommodate residual swelling. - Long-Term Management:
For long-term use, especially in patients with significant midfoot reconstruction or underlying systemic arthropathies, an extra-deep shoe with a soft, accommodating upper (such as deerskin) is highly recommended to prevent recurrent ulcerations and accommodate the altered biomechanics of the reconstructed foot.
You Might Also Like
