Ankle Arthroscopy: Indications, Surgical Anatomy, and Portal Planning

Key Takeaway
Ankle arthroscopy is a minimally invasive surgical technique for diagnosing and treating various ankle pathologies, offering reduced morbidity and faster recovery. Key indications include anterior/posterior impingement syndromes, osteochondral lesions of the talus (OCLTs), synovitis, and loose body removal. Precise surgical anatomy understanding and portal planning are crucial for safe, effective outcomes.
Introduction & Epidemiology
Ankle arthroscopy has evolved from a diagnostic tool to a cornerstone of minimally invasive ankle joint surgery. Its application has expanded significantly since its initial description, offering a distinct advantage over open procedures through reduced morbidity, accelerated recovery, and superior visualization of intra-articular pathology. The prevalence of ankle injuries and degenerative conditions necessitating surgical intervention underscores the importance of efficient and effective treatment modalities.
Ankle arthroscopy is primarily indicated for pathologies involving the tibiotalar joint, although its utility extends to the posterior ankle compartment, subtalar joint, and surrounding tendon sheaths (tendoscopy). Common indications include anterior and posterior impingement syndromes, osteochondral lesions of the talus (OCLTs), synovitis, removal of loose bodies, arthrofibrosis, and septic arthritis. Advances in instrumentation and surgical technique have broadened its scope, allowing for increasingly complex procedures to be performed arthroscopically.
Epidemiologically, ankle pathologies are frequent occurrences, particularly in athletic populations. Ankle sprains, often leading to chronic pain, instability, and impingement, affect millions annually. Osteochondral lesions, while less common than soft tissue injuries, represent a significant source of morbidity, often stemming from trauma. The minimally invasive nature of arthroscopy provides a viable treatment option for many of these conditions, minimizing soft tissue disruption inherent to open approaches.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy and biomechanics of the ankle is paramount for safe and effective arthroscopic intervention. The ankle joint, or tibiotalar joint, is a highly congruent hinge joint primarily responsible for dorsiflexion and plantarflexion. The subtalar joint, immediately inferior, provides inversion and eversion.
Tibiotalar Joint Anatomy
The tibiotalar joint is formed by the distal tibia (plafond and malleoli) and the talar dome. Key anatomical structures include:
*
Articular Cartilage:
Covers the talar dome and tibial plafond. OCLTs typically affect the talar dome.
*
Capsule:
A relatively thin, fibrous capsule encloses the joint.
*
Ligaments:
*
Lateral Collateral Ligament Complex:
Anterior talofibular ligament (ATFL), calcaneofibular ligament (CFL), and posterior talofibular ligament (PTFL). The ATFL is most commonly injured.
*
Medial (Deltoid) Ligament Complex:
Strong fan-shaped ligament providing medial stability.
*
Synovium:
Lines the non-articular surfaces of the joint capsule.
Neurovascular Structures and Portal Planning
Precise portal placement is critical to avoid iatrogenic injury to neurovascular structures.
*
Anterior Ankle:
*
Superficial Peroneal Nerve (SPN):
Courses superficially over the extensor retinaculum, typically found between the peroneus tertius and extensor digitorum longus tendons. At risk during anterolateral portal placement.
*
Saphenous Nerve and Great Saphenous Vein:
Located anteromedially, anterior to the medial malleolus. At risk during anteromedial portal placement.
*
Dorsalis Pedis Artery and Deep Peroneal Nerve:
Deep to the extensor hallucis longus and extensor digitorum longus tendons, between the tibialis anterior and extensor hallucis longus. At risk with central anterior portals.

*
Anatomical Correlates:
The tibialis anterior, extensor hallucis longus, and extensor digitorum longus tendons serve as important landmarks for anterior portal placement. The anteromedial portal is typically placed just medial to the tibialis anterior tendon. The anterolateral portal is placed lateral to the peroneus tertius or extensor digitorum longus tendons.


*
Posterior Ankle:
*
Sural Nerve:
Courses posterolaterally, superficial to the Achilles tendon. At risk with posterolateral portal.
*
Tibial Nerve and Posterior Tibial Artery/Veins:
Located posteromedially, deep to the flexor hallucis longus tendon. At risk with posteromedial portal.

Biomechanics and Distraction
The ankle joint requires distraction to create adequate working space for arthroscopic instruments and to prevent iatrogenic cartilage damage. Distraction can be achieved through:
*
Non-invasive methods:
Manual traction, traction tower with straps (often used for anterior ankle arthroscopy).
*
Invasive methods:
Pin distraction (e.g., Schanz pin in the distal tibia and calcaneus, less common for ankle proper due to risk of iatrogenic injury but sometimes used for subtalar).
Adequate distraction helps widen the joint space, allowing for safe introduction of instruments and preventing scuffing of articular cartilage by the scope or shaver.
Indications & Contraindications
Indications for Ankle Arthroscopy
Arthroscopic management is considered for a variety of ankle pathologies when conservative measures have failed.
*
Anterior Impingement Syndrome:
*
Osseous Impingement:
Removal of osteophytes from the distal tibia and/or dorsal talar neck.
*
Soft Tissue Impingement:
Debridement of hypertrophic synovium, scarred capsular tissue, or meniscoid lesions.
*
Osteochondral Lesions of the Talus (OCLTs):
Debridement, microfracture, drilling, or fixation of stable fragments.
*
Synovitis:
Arthroscopic synovectomy for chronic inflammatory or infectious synovitis.
*
Loose Bodies:
Identification and removal of intra-articular osteochondral fragments or calcified bodies.
*
Arthrofibrosis:
Lysis of adhesions to restore range of motion.
*
Ankle Instability:
Diagnostic arthroscopy to assess intra-articular pathology accompanying instability, and occasionally for assisted ligament repair or reconstruction.
*
Septic Arthritis:
Arthroscopic lavage and debridement of infected joint fluid and synovium.
*
Posterior Ankle Pathology:
*
Os Trigonum Syndrome:
Excision of a symptomatic os trigonum.
*
Posterior Impingement:
Debridement of soft tissue or osseous impingement.
*
Flexor Hallucis Longus (FHL) Tendinopathy:
Debridement of tenosynovitis or release of stenosing lesions.
*
Subtalar Arthroscopy:
Synovectomy, debridement, loose body removal, and arthrodesis for subtalar pathology.
*
Tendoscopy:
Diagnostic and therapeutic management of peroneal or FHL tendinopathies.
Contraindications for Ankle Arthroscopy
While minimally invasive, ankle arthroscopy is not without contraindications.
*
Absolute Contraindications:
* Active local skin infection at planned portal sites.
* Severe vascular compromise in the extremity.
* Uncontrolled coagulopathy.
*
Relative Contraindications:
*
Severe Degenerative Arthritis:
While some debridement is possible, severe osteoarthritis often requires open arthrodesis or arthroplasty.
*
Significant Soft Tissue Compromise:
Extensive scarring from previous surgeries or trauma, severe edema, or poor skin quality can complicate portal placement and healing.
*
Extreme Ankle Stiffness:
Limited joint motion can hinder instrument maneuverability and increase risk of iatrogenic damage.
*
Large OCLTs Requiring Cartilage Restoration:
Larger lesions (e.g., >1.5-2 cm²) or those requiring osteochondral autograft/allograft transplantation may be better addressed with open approaches.
*
Prior Extensive Surgery:
Can alter neurovascular anatomy and create dense adhesions, increasing surgical difficulty and risk.
Indications: Operative vs. Non-Operative Management
| Indication | Operative Management (Arthroscopy) | Non-Operative Management |
|---|---|---|
| Anterior Impingement (Osseous/Soft Tissue) | Failure of conservative care (physical therapy, NSAIDs, injections) for 3-6 months. Symptomatic restriction of dorsiflexion. | Initial conservative treatment for 3-6 months. Activity modification, NSAIDs, physical therapy, corticosteroid injections. |
| Osteochondral Lesions of the Talus (OCLTs) | Symptomatic lesions (pain, swelling, mechanical symptoms) unresponsive to conservative treatment. Unstable lesions. | Asymptomatic lesions. Small, stable lesions. Initial immobilization, protected weight-bearing, physical therapy, injections. |
| Chronic Synovitis/Arthrofibrosis | Persistent symptoms (pain, swelling, stiffness) despite conservative management. | NSAIDs, physical therapy, corticosteroid injections. |
| Loose Bodies | Symptomatic (pain, locking, catching). Large or multiple fragments. | Asymptomatic. |
| Septic Arthritis | Joint lavage and debridement (often urgent). | Systemic antibiotics (may be sufficient for early, mild cases or adjunct to surgery). |
| Posterior Impingement/Os Trigonum | Persistent posterior ankle pain with forced plantarflexion after adequate conservative treatment. | Activity modification, NSAIDs, physical therapy, corticosteroid injections. |
| Flexor Hallucis Longus Tendinopathy | Chronic pain and snapping, unresponsive to conservative treatment. | Rest, activity modification, NSAIDs, physical therapy, corticosteroid injections. |
| Subtalar Synovitis/Loose Bodies | Persistent symptoms after conservative measures. | NSAIDs, physical therapy, injections. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical to successful ankle arthroscopy, facilitating optimal visualization and safe instrument access.
Pre-operative Evaluation
- History and Physical Examination: Detailed assessment of pain characteristics, mechanical symptoms (clicking, locking), swelling, and instability. Range of motion (ROM) assessment and palpation for specific tenderness (e.g., anterior ankle for impingement). Neurovascular status is documented.
-
Imaging:
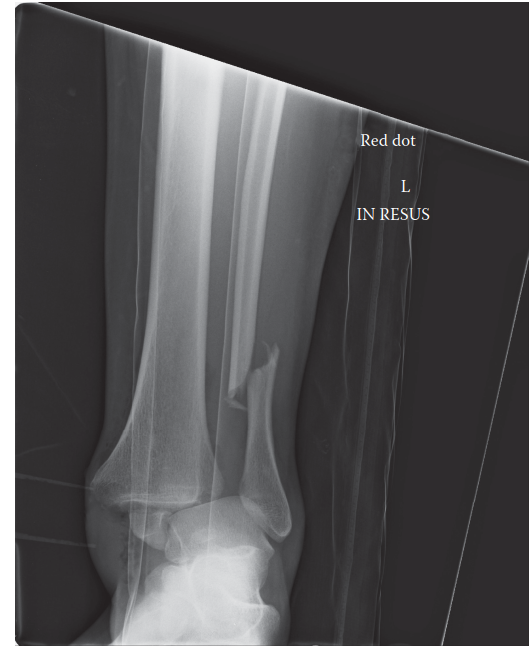
- Radiographs: Weight-bearing anteroposterior (AP), lateral, and mortise views are standard. Oblique views or stress views may be helpful. These identify osteophytes, joint space narrowing, and bony lesions.
- Magnetic Resonance Imaging (MRI): Essential for evaluating soft tissue pathology (synovitis, capsular hypertrophy, ligamentous injury) and especially for characterizing OCLTs (size, depth, subchondral edema, cyst formation).
-
Computed Tomography (CT) Scan:
Superior for delineating osseous morphology, especially for complex osteophytes, fractures, or evaluation of bony fusion in subtalar arthrodesis.

Anesthesia
A combination of general anesthesia with a regional anesthetic block (e.g., popliteal or sciatic block) is often preferred. The regional block provides excellent post-operative pain control, reducing the need for systemic opioids and facilitating earlier rehabilitation.
Tourniquet Application
A pneumatic tourniquet is typically applied to the proximal thigh or calf to ensure a bloodless field, which significantly improves visualization. Inflation pressure should be set at the minimum required to achieve ischemia, usually 100-150 mmHg above systolic blood pressure. Tourniquet time should be closely monitored.
Patient Positioning and Distraction Setup
For anterior ankle arthroscopy, the patient is usually positioned supine on the operating table.
*
Leg Holder:
The operative leg is placed in a thigh holder with the knee flexed to 90 degrees, allowing the ankle to be positioned freely off the end of the table. This facilitates ankle manipulation and application of traction.
*
Distraction:
*
Non-invasive Distraction:
The most common method. A sterile traction tower is positioned at the foot of the table. A sterile gauze wrap or cast padding is applied circumferentially around the midfoot, superior to the metatarsal heads, without encircling the toes. This is then connected to a spreader bar and the traction tower via sterile rope, applying longitudinal traction to the ankle joint. Approximately 20-30 lbs (9-14 kg) of traction is typically sufficient to open the joint space by 3-5 mm. Careful padding is essential to prevent pressure injury to the dorsum of the foot.






*
Invasive Distraction (Less Common for Ankle Proper):
Involves inserting a Steinmann pin into the distal tibia and another into the calcaneus, then connecting them to an external distraction frame. While providing very stable distraction, this carries a risk of pin tract infection and nerve injury. It is more commonly considered for subtalar arthroscopy or complex cases.
Sterilization and Draping
Standard sterile preparation and draping are performed. The entire limb from above the tourniquet to the toes is prepped and draped to allow full range of motion of the ankle and access for portal creation.

Landmarking and Portal Planning
Before inflation of the tourniquet, key anatomical landmarks and neurovascular structures are meticulously identified and marked on the skin with a surgical pen. This includes:
* Tip of medial and lateral malleoli.
* Ankle joint line (palpated during dorsiflexion/plantarflexion).
* Tibialis anterior tendon, extensor hallucis longus tendon, extensor digitorum longus tendons, peroneus tertius tendon.
* Estimated course of the superficial peroneal nerve (SPN), saphenous nerve and vein, dorsalis pedis artery.


















Portal sites are then carefully planned in relation to these landmarks.
Detailed Surgical Approach / Technique
Successful ankle arthroscopy relies on systematic execution, from equipment setup to portal creation and precise intra-articular work.
Equipment
A standard arthroscopy setup is employed, tailored for ankle dimensions.
*
Sterile Instruments/Equipment:
All instruments, including cannulas, trocars, shavers, burrs, grasping forceps, and radiofrequency wands, must be sterile.

*
Arthroscope:

The
2.7-mm scope
is most frequently used and is our preference. This size is ideal for the ankle joint, allowing for both anterior ankle arthroscopy and comprehensive intra-articular evaluation. Furthermore, the 2.7-mm scope can be safely utilized for posterior ankle arthroscopy, subtalar arthroscopy, and tendoscopy, offering versatility across different regions of the foot and ankle. Occasionally, the
1.9-mm scope
is employed in cases of exceptionally tight ankles, for pediatric patients, or when visualization through standard portals is challenging. Some surgeons advocate for the
4.0-mm scope
, which can be useful in anterior ankle arthroscopy, particularly for larger working areas, but may pose a challenge for detailed intra-articular evaluation in confined spaces or when attempting to visualize recesses.
*
Arthroscope Angle:

The
30-degree scope
is adequate in most situations, providing a good balance of direct and angled views. However, a
70-degree scope
is particularly useful for viewing the posterior joint compartment, posterior talar dome, and posterior tibial plafond from anterior portals, especially when a dedicated posterior approach is not planned or when assessing the extent of posterior impingement from the anterior aspect.

*
Standard Arthroscopy Tower:
Comprises a high-definition monitor, a powerful light source, a shaver motor, and often a printer for capturing still images.
*
Fluid Management:
We do not routinely use an arthroscopic pump for fluid inflow. Instead, we rely on
gravity flow
of sterile saline solution (normal saline or lactated Ringer's solution) from an elevated bag. This minimizes the risk of fluid extravasation and compartment syndrome, while still providing adequate distention and washout. For cases requiring aggressive debridement or with significant bleeding, a low-pressure pump may be selectively used with careful monitoring of inflow and outflow.
Portal Placement (Anterior Ankle)
The creation of portals requires meticulous attention to anatomical landmarks to prevent neurovascular injury. A "mini-open" technique is generally preferred, involving skin incision, followed by blunt dissection.
- Joint Distension: Prior to portal creation, the joint is distended with 10-20 mL of sterile saline using an 18-gauge needle, typically inserted just lateral to the tibialis anterior tendon. This separates articular surfaces and pushes neurovascular structures away from the joint capsule.
-
Anteromedial (AM) Portal:
- Location: Approximately 1 cm medial to the tibialis anterior tendon, at the level of the ankle joint line.
- Risk: Saphenous nerve and great saphenous vein.
-
Technique:
A small (5 mm) longitudinal skin incision is made. A mosquito clamp or blunt obturator is used for careful blunt dissection, spreading soft tissues down to the joint capsule. The capsule is then penetrated with the clamp, creating a path for the inflow cannula or arthroscope.

-
Anterolateral (AL) Portal:
- Location: Approximately 1 cm lateral to the peroneus tertius or extensor digitorum longus tendons, at the level of the ankle joint line.
- Risk: Superficial peroneal nerve (SPN). Care must be taken to avoid the nerve, which often courses near this portal.
-
Technique:
Similar blunt dissection technique as for the AM portal. This is often the primary viewing portal, with the AM portal used for instrumentation or vice versa.


-
Accessory Portals:
- Anterocentral Accessory Portal: Less frequently used, positioned between the EHL and EDL tendons. Increased risk to dorsalis pedis artery and deep peroneal nerve.
- Peroneal Portal: Placed slightly more distally and laterally than the AL portal, anterior to the lateral malleolus. Useful for visualizing the lateral gutter and accessing lateral impingement lesions.
- Cannulation: Once a portal is established, a clear cannula with a blunt trocar is inserted. The blunt trocar is then exchanged for the arthroscope. Inflow is established through the viewing cannula or a separate inflow portal (e.g., AM portal for inflow, AL portal for scope).
Systematic Intra-Articular Examination (Anterior)
Once the arthroscope is in place and inflow is established, a systematic examination of the joint is performed.
*
Anterior Gutter:
Inspect for synovitis, scar tissue, and osteophytes.
*
Medial Gutter:
Visualize the deltoid ligament, medial talar dome, and medial aspect of the tibial plafond.
*
Lateral Gutter:
Evaluate the ATFL, lateral talar dome, and lateral aspect of the tibial plafond. This area is commonly affected by impingement.
*
Central Joint:
Examine the anterior aspect of the talar dome and tibial plafond. Assess for OCLTs, cartilage defects, and loose bodies. The use of a probe is essential for assessing cartilage integrity.






Portal Placement (Posterior Ankle)
Posterior ankle arthroscopy is typically performed with the patient in a prone or lateral decubitus position. Non-invasive distraction is often preferred, but gravity can be sufficient in some cases. Careful marking of the sural nerve and the posteromedial neurovascular bundle (tibial nerve, posterior tibial artery) is crucial.
-
Posterolateral (PL) Portal:
- Location: Approximately 1 cm lateral to the Achilles tendon, at the level of the ankle joint line.
- Risk: Sural nerve.
- Technique: A small skin incision is made. Blunt dissection is directed towards the interval between the Achilles tendon and the peroneal tendons. The capsule is carefully penetrated. This is commonly the viewing portal.
-
Posteromedial (PM) Portal:
- Location: Approximately 1 cm medial to the Achilles tendon, at the level of the ankle joint line.
- Risk: Tibial nerve and posterior tibial artery/veins, flexor hallucis longus tendon.
- Technique: Blunt dissection is performed carefully, staying lateral to the FHL tendon and avoiding the neurovascular bundle. This serves as the working portal.
Specific Arthroscopic Procedures
- Anterior Impingement: Resection of anterior tibial and/or talar osteophytes using a shaver or burr. Debridement of hypertrophic synovium or soft tissue impinging lesions.
- OCLT Management: Debridement of unstable cartilage, removal of loose fragments. Microfracture is performed by creating multiple perforations (1-2 mm deep, 3-4 mm apart) in the subchondral bone using an awl to promote fibrocartilage formation.
- Loose Body Removal: Identified and grasped with pituitary forceps or retrieved with a shaver.
-
Posterior Impingement/Os Trigonum Excision:
Identification of the os trigonum or posterior osteophytes. Resection using a burr and shaver, taking care to protect the FHL tendon and neurovascular structures.


Closure
After all procedures are completed, instruments are removed, and the joint is thoroughly irrigated. Portal incisions are typically closed with a single non-absorbable suture or sterile strips. A sterile dressing is applied, followed by a soft compressive dressing or splint, depending on the procedure performed.
Complications & Management
While ankle arthroscopy is generally safe, specific complications can occur. Vigilance and proper technique are essential for prevention and effective management.
Common Complications and Management
| Complication | Incidence | Prevention Strategies | Salvage Strategies |
|---|---|---|---|
| Neurovascular Injury | 2-10% (transient) | Meticulous landmarking, blunt dissection, adequate joint distension, "mini-open" portal technique. Avoid central portals. | Observation (most resolve spontaneously within weeks/months). Nerve conduction studies/EMG for persistent symptoms. Surgical exploration/nerve repair for severe, persistent deficits. |
| Superficial Peroneal Nerve (SPN) Damage | Most common, 3-8% | Anterolateral portal lateral to peroneus tertius, parallel to nerve course, blunt dissection. | As above. |
| Saphenous Nerve/Vein Injury | 1-3% | Anteromedial portal medial to tibialis anterior, blunt dissection. | As above. Vein ligation if persistent bleeding. |
| Infection | <1% (septic arthritis) | Strict aseptic technique, prophylactic antibiotics (per institutional protocol), thorough joint irrigation. | Arthroscopic lavage and debridement, systemic broad-spectrum antibiotics, culture-guided antibiotic adjustment. |
| Cartilage Damage (Iatrogenic) | Rare but significant | Adequate joint distraction, careful instrument manipulation (avoid levering), blunt tipped instruments. | Microfracture for small defects. Larger defects may require open procedures or specialized cartilage repair techniques. |
| Fluid Extravasation/Compartment Syndrome | Rare but emergent | Use of gravity flow or low-pressure pump, limit surgical time, monitor inflow/outflow, careful cannula placement. | Immediately discontinue inflow, remove all cannulas, apply compression. Urgent fasciotomy if compartment pressures are elevated. |
| Instrument Breakage | Very rare | Pre-operative instrument check, proper technique, avoid excessive force. | Intra-articular retrieval (arthroscopic or open). |
| Deep Venous Thrombosis (DVT)/Pulmonary Embolism (PE) | <1% | Early mobilization, regional anesthesia, mechanical prophylaxis (compression devices) for high-risk patients. | Anticoagulation (therapeutic). |
| Post-operative Pain/Stiffness | Common (mild to mod) | Adequate pain control (regional block), early initiation of physical therapy, proper rehabilitation protocol. | Aggressive physical therapy, pain management, injections. Consider lysis of adhesions if severe arthrofibrosis. |
| Recurrent Symptoms | Varies by pathology | Thorough debridement, address underlying pathology adequately. | Re-evaluation, repeat imaging, possible revision arthroscopy or open surgery. |
Neurovascular Injury
Injury to peripheral nerves is the most frequently reported complication. The superficial peroneal nerve is particularly vulnerable during anterolateral portal creation, presenting as numbness or dysesthesia in the dorsum of the foot. The saphenous nerve and vein are at risk with anteromedial portals. Prevention hinges on precise anatomical landmarking, generous skin incisions followed by careful blunt dissection down to the joint capsule, and adequate joint distension prior to instrumentation insertion. Most nerve injuries are neurapraxias and resolve spontaneously. Persistent symptoms warrant further investigation and potentially nerve repair or neurolysis.
Fluid Extravasation
Excessive fluid inflow or prolonged surgical time can lead to fluid extravasation into surrounding soft tissues, potentially causing pain, swelling, and in rare cases, compartment syndrome. Utilizing gravity feed for inflow and ensuring continuous outflow minimizes this risk. If a pump is used, pressures should be kept as low as possible. Meticulous closure of portal sites and a compressive dressing post-operatively also help. In the event of suspected compartment syndrome, immediate assessment of compartment pressures and emergent fasciotomy is indicated.
Iatrogenic Chondral Damage
Direct damage to articular cartilage can occur from impinging instruments, excessive levering of the scope, or inadequate joint distraction. This risk is minimized by maintaining optimal joint distension and using appropriate, blunt-tipped instruments when feasible.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing outcomes following ankle arthroscopy. Protocols are tailored to the specific procedure performed and individual patient factors, but general principles apply.
Immediate Post-Operative Phase (Days 0-7)
- Pain Management: Multimodal analgesia, often including regional nerve blocks, oral NSAIDs, and short-term opioids as needed.
- RICE: Rest, Ice, Compression, and Elevation to minimize swelling and pain.
-
Weight-Bearing:
Varies by procedure:
- Diagnostic arthroscopy, synovectomy, loose body removal, anterior impingement debridement: Typically immediate protected weight-bearing in a walking boot or progressive weight-bearing as tolerated.
- OCLT microfracture or repair, posterior impingement/os trigonum excision: Non-weight-bearing (NWB) for 2-6 weeks in a protective boot or cast to allow for healing and maturation of the repair tissue.
- Early Motion: Gentle, pain-free range of motion (ROM) exercises are encouraged, often initiated within days of surgery, especially for procedures not involving significant cartilage repair. Dorsiflexion, plantarflexion, inversion, and eversion within comfortable limits.
Early Rehabilitation Phase (Weeks 1-6)
- Edema Control: Continued RICE.
- Progressive ROM: Gradual increase in active and passive ROM exercises. Manual therapy techniques by a physical therapist may be beneficial.
-
Strengthening:
- Isometrics: Initiate non-weight-bearing isometric exercises for ankle musculature (dorsiflexors, plantarflexors, invertors, evertors).
- Resisted Exercises: Progress to light resistance band exercises as pain allows.
- Proprioception: Begin balance and proprioception exercises (e.g., single-leg stance, wobble board, unstable surfaces) once weight-bearing is initiated and tolerated.
- Gait Training: If NWB, progress to partial weight-bearing (PWB) and then full weight-bearing (FWB) as indicated. Focus on normal gait mechanics.
Intermediate Rehabilitation Phase (Weeks 6-12)
- Advanced Strengthening: Increase resistance and intensity of strengthening exercises. Incorporate functional exercises (calf raises, heel walks, toe walks).
- Proprioception & Balance: Advance balance training with dynamic movements and sport-specific drills.
- Cardiovascular Fitness: Low-impact activities (swimming, cycling) can be introduced.
- Specific considerations: For OCLTs, weight-bearing progression is crucial, with continued protection of the healing cartilage. For impingement cases, focus on restoring full pain-free ROM.
Advanced Rehabilitation & Return to Activity (Weeks 12+)
- Sport-Specific Training: Gradually introduce agility drills, plyometrics, and sport-specific activities.
- Return to Activity: Phased return to sport or full work activities, guided by functional assessment and patient readiness. This typically occurs between 3-6 months for most procedures, but may be longer (6-12 months or more) for complex OCLT repairs.
- Monitoring: Continued monitoring for pain, swelling, or recurrent symptoms.
Close collaboration between the surgeon, physical therapist, and patient is essential throughout the rehabilitation process to ensure optimal recovery and prevent re-injury.
Summary of Key Literature / Guidelines
Ankle arthroscopy has a robust and growing body of literature supporting its efficacy across a broad range of indications.
Evidence for Common Indications
- Anterior Ankle Impingement: Arthroscopic debridement of osseous and soft tissue impingement has demonstrated high rates of success (75-90% good-to-excellent results), particularly in cases unresponsive to conservative management. Outcomes are generally superior to open techniques due to less soft tissue disruption and faster recovery. Level I and II evidence supports its use for both osseous and soft tissue lesions.
- Osteochondral Lesions of the Talus (OCLTs): Arthroscopic debridement and microfracture remain a cornerstone for small to medium-sized OCLTs (typically <1.5-2 cm²). Long-term outcomes are generally favorable, with good-to-excellent results reported in 70-85% of patients. However, the quality of repair tissue (fibrocartilage) is inferior to native hyaline cartilage, which has driven research into biologic augmentation (e.g., PRP, bone marrow aspirate concentrate) and advanced cartilage restoration techniques (e.g., autologous chondrocyte implantation, osteochondral allografts) for larger or failed lesions. The optimal treatment for large or cystic OCLTs remains a subject of ongoing research and debate.
- Synovitis and Loose Body Removal: Arthroscopic synovectomy for chronic inflammatory synovitis (e.g., rheumatoid arthritis, pigmented villonodular synovitis) and removal of symptomatic loose bodies are highly effective, with rapid symptom resolution and low recurrence rates.
- Posterior Ankle Pathology: Posterior ankle arthroscopy for conditions like os trigonum syndrome, FHL tendinopathy, and posterior impingement is gaining increasing acceptance. Studies have shown comparable outcomes to open approaches with the benefits of minimally invasive surgery, though the technical demands are higher, and the risk of neurovascular injury remains a concern if not meticulous.
- Septic Arthritis: Arthroscopic lavage and debridement is considered the gold standard for management of septic arthritis of the ankle, allowing for thorough debridement, removal of purulent material, and tissue sampling for culture, leading to better outcomes and shorter hospital stays compared to aspiration alone.
Current Guidelines and Best Practices
- Diagnosis: Thorough clinical evaluation combined with appropriate imaging (MRI for soft tissue and cartilage, CT for bony pathology) is essential for accurate diagnosis and surgical planning.
- Portal Safety: Adherence to established portal landmarks and "mini-open" blunt dissection techniques is critical for minimizing neurovascular complications, particularly for the superficial peroneal nerve.
- Distraction: Adequate joint distraction, primarily non-invasive traction, is paramount for visualization and preventing iatrogenic chondral damage.
- Fluid Management: Gravity-fed inflow or low-pressure pumps are preferred to mitigate the risk of fluid extravasation and compartment syndrome.
- Rehabilitation: Procedure-specific, progressive rehabilitation protocols are vital for optimal functional recovery.
Future Directions
The field of ankle arthroscopy continues to evolve.
*
Biologics:
The integration of biologic adjuncts (e.g., platelet-rich plasma, bone marrow aspirate concentrate, mesenchymal stem cells) with microfracture or cartilage repair techniques for OCLTs is an active area of research aiming to improve the quality and durability of repair tissue.
*
Navigation and Robotics:
While less prevalent in ankle arthroscopy compared to other joints, advancements in surgical navigation systems and robotic assistance hold promise for enhancing precision in portal placement and complex intra-articular maneuvers, potentially reducing complication rates and improving outcomes.
*
Expanded Indications:
Ongoing research explores the role of arthroscopy in more complex pathologies, such as ankle instability with capsular plication or ligament repair, and even early stages of arthrodesis.
In conclusion, ankle arthroscopy represents an indispensable tool in the armamentarium of the orthopedic foot and ankle surgeon, offering a safe and effective approach for a multitude of intra-articular pathologies. A deep understanding of anatomy, meticulous technique, and appropriate post-operative care are the cornerstones for achieving optimal patient outcomes.
Clinical & Radiographic Imaging

You Might Also Like