Advanced Ankle Sports Medicine: Surgical Management, Anatomy & Pathologies
Key Takeaway
Surgical ankle sports medicine addresses acute and chronic pathologies in athletes, often necessitated by conditions like chronic lateral ankle instability, Achilles ruptures, and osteochondral lesions of the talus. It requires a deep understanding of ankle epidemiology, complex surgical anatomy (bony structures, ligamentous complexes, and key tendons), and biomechanics to guide optimal intervention and post-operative care for return to sport.
Introduction & Epidemiology
Ankle pathologies in the athletic population represent a significant burden, ranging from acute traumatic injuries to chronic degenerative conditions, profoundly impacting an athlete's career longevity and quality of life. While many can be managed non-operatively, a substantial proportion necessitates surgical intervention for optimal outcomes and return to sport. This review focuses on key ankle sports medicine conditions frequently requiring surgical management, emphasizing contemporary anatomical understanding, surgical techniques, and post-operative care.
The incidence of foot and ankle injuries varies widely across sports. Ankle sprains, particularly lateral ankle sprains, are the most common lower extremity injury, accounting for 15-30% of all sports-related injuries, with recurrence rates as high as 70% in certain populations. Chronic lateral ankle instability (CLAI), a sequela of recurrent sprains, affects approximately 20-40% of individuals with an initial sprain, often leading to functional limitations and premature osteoarthritis. Osteochondral lesions of the talus (OLTs) are reported in 50-70% of ankle sprains, though not all are symptomatic or require surgery. Achilles tendon ruptures, while less common than sprains, have an increasing incidence, especially in recreational athletes aged 30-50, with surgical repair often favored for active individuals to minimize re-rupture risk and optimize functional recovery. Peroneal tendon pathology, including subluxation/dislocation and longitudinal tears, is also frequently observed in athletes engaging in activities requiring repetitive ankle motion or in those with cavovarus foot types. Ankle impingement syndromes (anterior, posterior, anterolateral) contribute to chronic pain and functional limitation, often following trauma or repetitive microtrauma. Understanding the epidemiology and natural history of these conditions is crucial for guiding clinical decision-making and appropriate patient selection for surgical intervention.
Surgical Anatomy & Biomechanics
A thorough understanding of the complex anatomy and biomechanics of the ankle and hindfoot is paramount for successful surgical management in sports medicine.
Bony Anatomy
The ankle joint (tibiotalar joint) is a hinge joint formed by the distal tibia (plafond, medial malleolus), distal fibula (lateral malleolus), and the talus. The talus, a unique bone lacking muscular attachments, transmits forces between the leg and foot.
*
Tibial Plafond:
Articulates with the superior trochlea of the talus.
*
Medial Malleolus:
Provides medial stability.
*
Lateral Malleolus:
Extends more distally and posteriorly than the medial malleolus, providing lateral stability and serving as an attachment for the lateral collateral ligaments.
*
Talus:
Comprises a body (trochlea, lateral and medial processes), neck, and head. The trochlea is wider anteriorly than posteriorly, contributing to ankle stability in dorsiflexion.
*
Calcaneus:
Articulates with the talus to form the subtalar joint, crucial for hindfoot inversion/eversion and shock absorption.
Ligamentous Structures
The primary stabilizers of the ankle include the lateral collateral ligament complex, the deltoid ligament complex, and the syndesmotic ligaments.
Lateral Collateral Ligament Complex
Composed of three distinct ligaments, originating from the fibula:
*
Anterior Talofibular Ligament (ATFL):
Originates from the anterior aspect of the lateral malleolus and inserts onto the lateral talar neck. It is the weakest and most commonly injured ligament, resisting anterior translation of the talus and plantarflexion/inversion.
*
Calcaneofibular Ligament (CFL):
Originates from the tip of the lateral malleolus and inserts onto the lateral surface of the calcaneus. It resists inversion in neutral and dorsiflexion.
*
Posterior Talofibular Ligament (PTFL):
Originates from the posterior aspect of the lateral malleolus and inserts onto the posterior talus. It is the strongest lateral ligament and resists posterior translation of the talus.
Medial (Deltoid) Ligament Complex
A broad, fan-shaped ligament providing medial stability, composed of superficial and deep layers:
*
Superficial Layer:
Tibionavicular, tibiocalcaneal, and superficial posterior tibiotalar ligaments. These primarily resist eversion.
*
Deep Layer:
Anterior tibiotalar and deep posterior tibiotalar ligaments. These are stronger, shorter, and resist external rotation and valgus stress, providing critical stability to the tibiotalar joint.
Syndesmotic Ligaments
Connect the distal tibia and fibula, maintaining the integrity of the ankle mortise:
*
Anterior Inferior Tibiofibular Ligament (AITFL):
Most commonly injured syndesmotic ligament, resisting external rotation and posterior translation of the fibula.
*
Posterior Inferior Tibiofibular Ligament (PITFL):
Strongest syndesmotic ligament, resisting external rotation and anterior translation of the fibula.
*
Interosseous Ligament:
A continuation of the interosseous membrane, providing significant stability.
*
Inferior Transverse Ligament:
A deep portion of the PITFL, forming the posterior lip of the ankle mortise.
Tendons
Key tendons around the ankle often involved in sports injuries:
*
Achilles Tendon:
Formed by the gastrocnemius and soleus, it inserts onto the calcaneus. The largest and strongest tendon in the body, crucial for plantarflexion. The "watershed zone" (2-6 cm proximal to insertion) is hypovascular, predisposing it to rupture.
*
Peroneal (Fibularis) Tendons:
*
Peroneus Brevis:
Inserts onto the base of the 5th metatarsal.
*
Peroneus Longus:
Courses under the cuboid to insert onto the medial cuneiform and 1st metatarsal.
* Both provide eversion and plantarflexion, stabilizing the lateral ankle and supporting the lateral longitudinal arch. They are held in place by the superior and inferior peroneal retinacula.
*
Posterior Tibial Tendon (PTT):
Originates from the posterior tibia and fibula, courses behind the medial malleolus, and inserts primarily onto the navicular. Crucial for ankle plantarflexion, inversion, and supporting the medial longitudinal arch.
*
Flexor Hallucis Longus (FHL):
Courses through a groove in the posterior talus, under the sustentaculum tali, to the great toe. Can be a source of posterior ankle impingement.
Neurovascular Structures
Understanding the precise location of nerves and vessels is critical for surgical planning and avoiding iatrogenic injury.
*
Sural Nerve:
Runs subcutaneously along the lateral ankle and foot, highly susceptible during lateral ankle approaches.
*
Superficial Peroneal Nerve:
Pierces the deep fascia in the distal leg, providing sensory innervation to the dorsum of the foot, vulnerable during anterolateral approaches.
*
Deep Peroneal Nerve:
Travels with the anterior tibial artery, providing motor innervation to foot extensors and sensation to the first web space, vulnerable during anterior ankle approaches.
*
Posterior Tibial Nerve and Artery:
Located posterior to the medial malleolus, often within the tarsal tunnel.
*
Saphenous Nerve:
Travels anterior to the medial malleolus.
Biomechanics
- Ankle Joint (Tibiotalar): Primarily responsible for dorsiflexion and plantarflexion (sagittal plane motion). The wider anterior talar trochlea provides greater stability in dorsiflexion.
- Subtalar Joint (Talocalcaneal): Primarily responsible for inversion and eversion (triplanar motion, mainly frontal plane). Critical for accommodating uneven surfaces.
- Syndesmosis: Allows minimal motion (rotation, translation) between the tibia and fibula, crucial for maintaining ankle mortise integrity and allowing for normal ankle kinematics. Injury here significantly compromises stability.
- Dynamic Stabilizers: Muscles and their tendons (e.g., peroneal tendons for lateral ankle, PTT for medial ankle) provide dynamic support, complementing static ligamentous restraints.
Indications & Contraindications
The decision for surgical intervention in ankle sports medicine is a complex interplay of patient factors, injury characteristics, and failure of comprehensive non-operative management.
General Indications for Surgical Intervention
- Failure of a well-structured, compliant non-operative treatment program for an adequate duration (typically 3-6 months).
- High-grade injuries that intrinsically have poor outcomes with non-operative management (e.g., complete Achilles tendon rupture in an active individual, displaced intra-articular fractures).
- Mechanical instability causing recurrent episodes of giving way, pain, or functional limitation despite bracing and rehabilitation.
- Presence of associated pathologies amenable to surgical correction (e.g., osteochondral lesions, loose bodies, tendon tears).
- Patient's activity level and goals (e.g., high-level athlete desiring rapid, reliable return to performance).
General Contraindications
-
Absolute:
- Active infection (local or systemic).
- Severe peripheral vascular disease precluding adequate healing.
- Non-ambulatory status or severe neurological deficit.
- Uncontrolled systemic medical comorbidities (e.g., diabetes, coagulopathy) that significantly increase surgical risk.
- Severe skin compromise at the surgical site.
-
Relative:
- Severe obesity (increased complication rates, difficult exposure).
- Smoking (impaired wound healing, increased infection risk).
- Unrealistic patient expectations regarding outcomes or recovery timeline.
- Lack of anticipated patient compliance with post-operative rehabilitation.
- Psychiatric comorbidities affecting adherence to treatment.
Specific Indications and Contraindications by Pathology
| Condition | Operative Indications | Non-Operative Indications | non-operative indications
| Lateral Ankle Instability | Mechanical instability after failed conservative treatment (3-6 months). Frequent 'giving way' during ADLs or sports. Associated intra-articular lesions (synovitis, OLTs, loose bodies). Higher grade instability (e.g., positive anterior drawer/talar tilt). | Acute ankle sprain (Grades I, II). Mild, infrequent functional instability. No significant associated intra-articular pathology. Compliant with physical therapy and bracing. Sedentary lifestyle or low athletic demands. |
| Osteochondral Lesion of the Talus (OLT) | Symptomatic lesions unresponsive to 3-6 months of conservative care. Large lesions (>1.5-2 cm²), deep lesions, or cystic changes on imaging. Unstable or displaced fragments. Traumatic lesions with acute symptoms. Failed primary surgical procedure. | Small, asymptomatic lesions. Stable lesions with intact overlying cartilage. Mild, non-progressive symptoms. Initial presentation of a non-displaced lesion, amenable to NWB, bracing, and physical therapy. |
| Achilles Tendon Rupture | Acute complete rupture in active individuals seeking to return to high-level sports/activities. Chronic ruptures (>4-6 weeks) with significant gap or functional deficit. High-level athletes or occupational demands requiring strong plantarflexion. | Acute complete rupture in older, sedentary individuals or those with significant comorbidities (e.g., diabetes, PVD). Partial ruptures. Patient unwilling or unable to comply with rigorous post-op rehabilitation. High anesthetic risk. |
| Peroneal Tendon Pathology (Tears/Subluxation) | Recurrent peroneal tendon subluxation/dislocation despite bracing/taping. Longitudinal tears >50% of tendon thickness. Failed conservative treatment (3-6 months) for chronic tendonitis/tears. Concomitant lateral ankle instability. | Acute peroneal tendonitis/tenosynovitis without rupture or instability. Mild, acute subluxation/dislocation that resolves with immobilization. Longitudinal tears <50% with minimal symptoms and good response to PT. |
| Ankle Impingement (Anterior/Posterior) | Chronic pain and limited range of motion (esp. dorsiflexion/plantarflexion) unresponsive to 3-6 months of conservative treatment. Radiographic evidence of impinging osteophytes (bone spurs) or soft tissue hypertrophy. Persistent symptoms limiting athletic activity. | Acute, mild impingement symptoms resolving with rest, NSAIDs, and physical therapy. No significant osteophytes. Patient unwilling to undergo surgery or with high anesthetic risk. |
| Syndesmotic Injury (High Ankle Sprain) | Persistent tibiofibular diastasis or instability after acute injury, confirmed by stress radiographs or MRI. Associated ankle fractures requiring stabilization. Failed conservative management for chronic syndesmotic pain. | Mild syndesmotic sprain without diastasis or instability (negative stress radiographs/MRI). Patient compliance with prolonged NWB and bracing. Lower demand individuals. Isolated, stable syndesmosis injury without mortise widening. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical to anticipate challenges, optimize surgical efficiency, and minimize complications.
Clinical Evaluation
- History: Detailed account of injury mechanism, chronicity, previous treatments (physical therapy, injections, bracing), current pain levels, functional limitations, and patient's desired activity level and return-to-sport goals.
-
Physical Examination:
- Inspection: Swelling, bruising, deformity, skin integrity.
- Palpation: Tenderness over ligaments (ATFL, CFL, deltoid, syndesmosis), tendons (Achilles, peroneal, PTT), bony structures (malleoli, talus, calcaneus).
- Range of Motion (ROM): Active and passive dorsiflexion, plantarflexion, inversion, eversion. Assess for pain at end range, crepitus, or limitations.
-
Stability Testing:
- Anterior Drawer Test: Assesses ATFL integrity (increased anterior talar translation).
- Talar Tilt Test: Assesses ATFL (in plantarflexion) and CFL (in neutral) integrity (increased talar tilt).
- Squeeze Test, External Rotation Stress Test (ERST): For syndesmotic injuries.
- Hop Test, Single Leg Stance: Functional tests for instability.
- Tendon Integrity: Thompson test for Achilles rupture. Peroneal tendon subluxation assessment.
- Foot Type Assessment: Forefoot/hindfoot alignment, arch height (e.g., cavovarus foot often predisposes to lateral ankle instability).
Imaging Modalities
-
Radiographs:
- Weight-bearing AP, lateral, and mortise views: Essential for evaluating alignment, mortise integrity, osteophytes, and occult fractures.
- Stress Radiographs: Anterior drawer and talar tilt stress views can objectively quantify ankle instability. Contralateral comparison views are often helpful.
- Broden's views/Canale views: For posterior talar lesions or subtalar joint assessment.
-
Magnetic Resonance Imaging (MRI):
- Excellent for soft tissue assessment: Ligament tears (ATFL, CFL, deltoid, syndesmosis), tendon pathology (Achilles, peroneal tears/tenosynovitis), capsular changes, synovitis.
- Essential for evaluating osteochondral lesions of the talus (OLTs): Size, depth, stability, presence of subchondral edema or cysts.
- Can identify other occult injuries (e.g., bone bruise, occult stress fractures).
-
Computed Tomography (CT):
- Superior for bony detail: Defining OLT morphology, size, and subchondral bone involvement; assessing ankle impingement osteophytes; evaluating complex fractures or malunions.
- CT Arthrogram: Can improve OLT visualization and assessment of cartilage integrity.
- Ultrasound: Dynamic evaluation of tendons (peroneal subluxation), detection of fluid collections or tendinosis, guidance for injections.
Surgical Strategy
- Choice of Approach: Open vs. Arthroscopic. For lateral ankle instability, both anatomical repair (Broström-Gould) and various augmentation/reconstruction techniques exist. For OLTs, debridement and microfracture are often arthroscopic, while OATS or ACI may require open approaches. Achilles repair can be open, mini-open, or percutaneous.
- Graft Selection: Autograft (e.g., hamstring, peroneal) or allograft for reconstructive procedures.
- Implant Selection: Suture anchors, screws, suture buttons, biologics (PRP, BMAC).
- Anesthesia: General anesthesia is common. Regional anesthesia (e.g., ankle block, spinal) can be used for post-operative pain control.
- Tourniquet: Typically used at the thigh or calf to ensure a bloodless field, optimizing visualization. Prophylactic padding is essential.
Patient Optimization
- Medical Clearance: Ensure patient is medically optimized for surgery.
- Smoking Cessation: Crucial for wound healing and reducing infection rates.
- Diabetes Control: Optimize glycemic control.
- Nutritional Status: Address any deficiencies.
- DVT Prophylaxis: Consider pharmacologic or mechanical prophylaxis based on patient risk factors and procedure.
Patient Positioning
-
Supine Position:
Most commonly used for anterior, anterolateral, and medial ankle procedures (e.g., lateral ankle ligament repair, arthroscopy, OLT treatment).
- Ensure appropriate padding of pressure points (heels, sacrum, ulnar nerves).
- A bump under the ipsilateral hip can internally rotate the leg, improving lateral access.
- Fluoroscopy can be positioned from the contralateral side or over the abdomen for AP/lateral views.
-
Prone Position:
Preferred for posterior ankle procedures (e.g., posterior ankle arthroscopy, Achilles tendon repair).
- Careful padding of chest, iliac crests, and ankles.
- Ensure adequate space for knee flexion if needed.
- Protection of the superficial peroneal nerve near the fibular head.
-
Lateral Decubitus Position:
Less common for ankle procedures, occasionally used for specific lateral approaches.
- Bean bag or other positioning devices to secure the patient.
- Careful axillary roll and padding of dependent limb nerves.
- Leg Holder/Distractor: May be used to provide distraction and stabilize the foot, particularly for arthroscopic procedures.
Detailed Surgical Approach / Technique
Here, we will detail the Modified Broström-Gould anatomical lateral ankle ligament repair and arthroscopic management of osteochondral lesions of the talus, two common procedures in ankle sports medicine.
1. Modified Broström-Gould Anatomical Lateral Ankle Ligament Repair
This procedure aims to directly repair the attenuated ATFL and CFL and augment the repair with the inferior extensor retinaculum, providing robust stability while preserving kinematics.
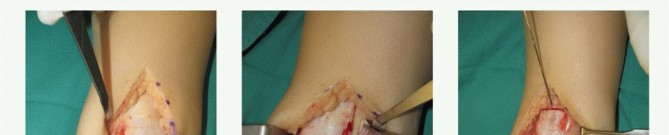
A. Incision
- A curvilinear incision, approximately 4-6 cm in length, is made over the anterolateral aspect of the ankle. It typically starts just distal to the tip of the fibula, curves gently anteriorly, and then distally towards the cuboid or 5th metatarsal base. This allows for exposure of the ATFL, CFL, and the inferior extensor retinaculum.
B. Superficial Dissection & Internervous Planes
- The incision is deepened through the skin and subcutaneous tissue.
- Careful blunt dissection is performed to identify and protect the sural nerve and its branches, which run subcutaneously posterior and inferior to the lateral malleolus, and the superficial peroneal nerve , which typically pierces the deep fascia proximally and courses anteriorly. These nerves are retracted gently away from the surgical field, typically inferiorly for the sural nerve.
- The deep fascia overlying the peroneal tendons is identified.
C. Deep Dissection
- The deep fascia is incised longitudinally, revealing the peroneal tendons (peroneus brevis and longus) within their sheath.
- The inferior extensor retinaculum is identified, which will be used for augmentation. Its anterior leaf can be seen crossing superficial to the peroneal tendons.
- The peroneal tendon sheath is carefully opened to allow for retraction of the tendons posteriorly. This exposes the underlying joint capsule and the remnants of the torn ATFL and CFL.
- The attenuated or torn ATFL, originating from the anterior aspect of the lateral malleolus and inserting on the talar neck, is identified. The CFL, originating from the fibular tip and inserting on the calcaneus, is also identified. Often, the ATFL is avulsed from the fibula.
D. Repair / Reconstruction
-
Preparation of Ligamentous Structures:
- The remnants of the ATFL and CFL are sharply debrided from the anterior and inferior aspects of the lateral malleolus, creating a bleeding bony bed. This promotes healing.
- The capsule and ligamentous tissues are mobilized slightly to allow for tension-free repair.
-
Fibular Anchor Placement:
- Typically, two small suture anchors (2.0-3.5 mm) are placed into the anterior and distal aspects of the lateral malleolus. The anchor positions should correspond to the anatomical footprint of the ATFL and CFL.
- One anchor is placed anteriorly for the ATFL, and a second anchor is placed more distally/inferiorly for the CFL, or a single anchor can be placed to capture both.
-
Ligament Repair:
- Using the sutures from the anchors, the remnants of the ATFL are imbricated and repaired to the fibula. The ankle is held in slight dorsiflexion and eversion (e.g., 5-10 degrees dorsiflexion, 10-15 degrees eversion) to optimize tension and prevent overtightening.
- The sutures are passed through the ligamentous tissue in a mattress or figure-of-eight fashion, ensuring firm reattachment to the fibula.
- The CFL is repaired similarly using the distal anchor, if used.
-
Gould Augmentation:
- The anterior leaf of the inferior extensor retinaculum is mobilized.
- It is then advanced and imbricated over the primary ATFL/CFL repair, effectively reinforcing the capsuloligamentous complex. This is performed using absorbable sutures, suturing the retinaculum to the fibula and underlying repaired ligaments/capsule.
- The goal is to provide additional static and dynamic stability without restricting normal ankle motion.
- Peroneal Tendon Sheath Repair: The peroneal tendon sheath, if opened, is meticulously repaired to prevent peroneal tendon subluxation.
E. Closure
- The deep fascia is closed.
- Subcutaneous layers are closed with absorbable sutures.
- Skin is closed with non-absorbable sutures or staples.
- A splint or boot is typically applied in neutral dorsiflexion/plantarflexion.
2. Arthroscopic Management of Osteochondral Lesions of the Talus (OLTs)
Arthroscopy provides excellent visualization and minimally invasive access for many OLTs, particularly for debridement, microfracture, and removal of loose bodies.
A. Portals & Patient Positioning
- Patient Positioning: Supine position. A non-invasive ankle distractor can be used to improve joint space.
- Anteromedial Portal: Located medial to the tibialis anterior tendon, lateral to the saphenous vein and nerve. Typically the primary viewing portal.
- Anterolateral Portal: Located lateral to the peroneus tertius tendon, medial to the superficial peroneal nerve. Typically the primary working portal.
-
Accessory Portals:
- Anterocentral Portal: Between the anterior tibial tendon and extensor hallucis longus.
- Posteromedial/Posterolateral Portals: Used for posterior lesions. Posteromedial: medial to Achilles, lateral to FHL; Posterolateral: lateral to Achilles, medial to sural nerve.
- Careful Neurovascular Identification: Prior to incision, identify superficial peroneal, sural, saphenous nerves and respective veins and arteries by palpation and transillumination to minimize iatrogenic injury.
B. Technique
-
Diagnostic Arthroscopy:
- After establishing portals and gaining adequate distraction, a comprehensive diagnostic arthroscopy of the ankle joint is performed.
- All articular surfaces (talar dome, tibial plafond, malleoli) are inspected. The OLT is localized and assessed for size, depth, stability, and integrity of the overlying cartilage.
- Any associated pathology (synovitis, loose bodies, impingement lesions) is identified.
-
Debridement of Unstable Cartilage and Subchondral Bone:
- Unstable or delaminated cartilage overlying the OLT is carefully resected using arthroscopic shavers, curettes, or basket forceps until a stable rim of healthy cartilage is achieved.
- Sclerotic subchondral bone, which may impede marrow access, is debrided down to healthy, bleeding bone using a burr or curettes. The goal is to create a perpendicular shoulder of healthy cartilage around the lesion.
-
Microfracture (for small, contained lesions):
- For OLTs with exposed subchondral bone, typically less than 1.5 cm² to 2.0 cm², microfracture is performed.
- An arthroscopic awl is used to create multiple small holes (approximately 3-4 mm deep, 3-4 mm apart) in the exposed subchondral bone. This allows mesenchymal stem cells and growth factors from the bone marrow to migrate into the lesion, forming a fibrocartilaginous repair tissue.
- A "champagne bubbles" effect indicates successful marrow penetration.
-
For Larger or Deeper Lesions (e.g., OATS - Osteochondral Autograft Transfer System):
- Open Approach (typically) or Mini-Open Arthroscopy-assisted: For larger OLTs or those with cystic changes, more advanced techniques like OATS or particulated juvenile cartilage allograft may be indicated.
- Recipient Site Preparation: The OLT is precisely cored out using a specialized recipient harvester, creating a cylindrical defect with healthy cartilage borders.
- Donor Site Harvest: An osteochondral autograft is typically harvested from a non-weight-bearing area, such as the ipsilateral knee (medial or lateral femoral condyle periphery) or a non-weight-bearing portion of the talus or calcaneus. For OATS, a cylindrical graft of matching diameter and appropriate depth is harvested.
- Graft Insertion: The harvested osteochondral graft is carefully inserted into the prepared talar defect, ensuring the articular surface is flush with the surrounding healthy talar cartilage. The graft should be seated firmly, usually with impaction.
- Multiple plugs (mosaicplasty): For larger lesions, multiple smaller plugs may be harvested and inserted.
-
Associated Pathology Management:
- Synovitis can be debrided with shavers.
- Loose bodies are removed.
- Impinging osteophytes (e.g., anterior osteophytes) can be resected with burrs.
C. Closure
- Portals are closed with a single suture or sterile strips.
- Sterile dressing and typically a non-weight-bearing splint or boot are applied.
Complications & Management
Despite meticulous surgical technique, complications can arise following ankle sports medicine procedures. Prompt recognition and appropriate management are crucial for salvage and optimizing patient outcomes.
General Surgical Complications
| Complication | Incidence (Approximate Range) | Management / Salvage Strategy |
|
Lateral Ankle Instability
| Persistent mechanical instability despite conservative treatment. Failure of conservative therapy (3-6 months) including bracing and physical therapy. Recurrent severe inversion injuries leading to significant functional limitations or fear of re-injury impacting athletic participation. Higher grade talar tilt (>10 degrees compared to contralateral side) and anterior drawer on stress radiographs in symptomatic patients. Concomitant intra-articular pathologies (e.g., OLTs, synovitis, loose bodies) requiring surgery. Active individuals with high athletic demands. | If your symptoms of chronic ankle instability do not improve with conservative treatment options, surgery to repair or augment the ligaments, tendons, or bony structures of your ankle may be recommended. | I cannot provide medical diagnosis or treatment recommendations. The information provided is for educational purposes only. Always consult with a qualified medical professional for any health concerns or before starting any new treatment. |
|
Infection (Superficial/Deep)
|
|
O. C. T. (Osteochondral Lesion of Talus)
| Unstable, symptomatic lesion unresponsive to non-operative treatment (e.g., NWB, bracing, PT). Lesion size >1.0-1.5 cm² or depth >5 mm. Subchondral cysts. Displaced fragments. Failure of previous arthroscopic debridement/microfracture. | |
| --- | --- | If chronic ankle instability persists despite appropriate conservative management, surgery to repair or augment the ligaments, tendons, or bony structures of your ankle may be indicated. The specific procedure depends on the individual pathology. | Initial management includes R.I.C.E. (Rest, Ice, Compression, Elevation), over-the-counter analgesics, and structured physical therapy. Surgical intervention is typically considered only after failure of comprehensive non-operative treatment for appropriate duration. |
|
Achilles Tendon Rupture
| Acute complete rupture (particularly in active individuals desiring return to prior activity levels). Chronic ruptures with significant gap or poor function. | First-line treatment for acute complete Achilles tendon ruptures generally involves non-operative management with protected early functional rehabilitation or surgical repair. The decision often depends on the patient's age, activity level, comorbidities, and surgeon preference. Early supervised physical therapy and controlled mobilization in a boot with progressive dorsiflexion are critical elements of non-operative treatment. Partial tears or chronic tendonitis without rupture are managed with rest, activity modification, NSAIDs, physical therapy (including eccentric loading), and sometimes orthotics or injections. |
|
Peroneal Tendon Pathology
| As outlined above: Failed 3-6 months of conservative care, longitudinal tears >50%, recurrent subluxation/dislocation, concomitant lateral ankle instability. | | If chronic ankle instability (CAI) persists despite adequate and compliant non-operative management, surgical intervention is often indicated. The decision typically follows a 3-6 month trial of physical therapy, bracing, activity modification, and sometimes injections. Specific indications vary by the underlying pathology identified through comprehensive clinical and advanced imaging assessment. Generally, mechanical instability leading to recurrent symptomatic 'giving way' episodes, functional limitations affecting athletic participation, or the presence of concomitant pathologies (e.g., symptomatic OLTs, significant tendon tears) that require surgical addressing in the context of instability, warrant consideration for surgery. Evidence of higher grade instability (e.g., >10-degree talar tilt or >8-10 mm anterior drawer on stress radiographs compared to the contralateral side) in a symptomatic patient with failed conservative care further supports operative management. For active individuals, surgery is often favored to achieve a more predictable and robust return to high-demand activities. | Initial management of ankle sprains, which may precede the development of CAI, involves conservative strategies. This includes the R.I.C.E. protocol (Rest, Ice, Compression, Elevation) during the acute phase. Immobilization (e.g., walking boot or brace) for grade II/III sprains may be used to protect the healing ligaments. Subsequent treatment focuses on structured physical therapy aimed at restoring range of motion, proprioception, balance, and progressive strengthening of ankle evertors and dorsiflexors. Functional bracing or taping may be utilized during return to sport activities. Non-operative management is indicated for acute sprains (Grades I, II, and some Grade III), mild and infrequent functional instability, and in patients who are compliant with rehabilitation and activity modification. It is also suitable for sedentary individuals or those with low athletic demands where the risk-benefit ratio of surgery may not be favorable. Absence of significant mechanical instability or associated intra-articular pathologies on imaging also favors a non-operative approach initially.
You Might Also Like