Complex Pilon Fracture Case: High-Energy Trauma, Diagnosis & Initial Management
Key Takeaway
A Ruedi-Allgöwer Type III pilon fracture is a complex, high-energy distal tibial injury involving severe articular comminution and impaction. Diagnosis mandates detailed clinical examination and initial radiographs. Crucially, a CT scan with 3D reconstruction provides definitive classification, precise articular fragment mapping, and comprehensive data essential for surgical planning.
Patient Presentation & History
A 38-year-old male, a keen amateur cyclist with no significant past medical history, presented to the emergency department following a high-energy trauma. He sustained a fall from a height of approximately 4 meters while working on a ladder, landing directly on his right foot. The patient immediately experienced severe pain, gross deformity of the right ankle, and complete inability to bear weight. He denied any head injury, loss of consciousness, or other associated injuries.
In the pre-hospital setting, paramedics applied a temporary splint, administered intravenous analgesia, and ensured neurovascular integrity before transport. On arrival, the patient was hemodynamically stable. His only regular medication was a multivitamin, and he had no known allergies. He reported no history of previous ankle injuries or surgeries. Social history was unremarkable, with no smoking or excessive alcohol consumption. This patient's high activity level and lack of comorbidities made him an excellent candidate for aggressive surgical management, provided soft tissue conditions allowed.
Clinical Examination
Upon arrival in the emergency department, a thorough clinical examination of the right lower extremity was performed.
Inspection
The right ankle demonstrated marked swelling, significant ecchymosis extending from the midfoot to the distal leg, and a gross varus deformity of the hindfoot with internal rotation of the foot relative to the tibia. There was notable skin tenting over the anteromedial aspect of the distal tibia, indicating impending skin compromise, though the skin itself remained intact with no open wounds or fracture blisters present initially. Capillary refill was brisk in all toes, and the foot appeared well-perfused. No signs of an open fracture were noted.
Palpation
Palpation revealed exquisite tenderness circumferentially around the ankle joint, particularly over the distal tibia, medial malleolus, and lateral malleolus. Significant crepitus was elicited with any attempt at passive motion. The fibular head was non-tender, ruling out a high fibular fracture associated with a Maisonneuve injury. Dorsalis pedis and posterior tibial pulses were palpable and strong bilaterally, though palpation was challenging due to the severe swelling. Sensation was intact in the distribution of the superficial peroneal, deep peroneal, saphenous, and sural nerves. No tenderness was noted along the course of the Achilles tendon. Assessment for compartment syndrome was performed given the high-energy mechanism, and at this initial presentation, no signs of increased compartment pressure were evident; however, this remained a critical consideration for ongoing monitoring.
Range of Motion
Active and passive range of motion of the ankle was severely restricted due to pain and mechanical blockade. Gross instability was noted, consistent with a severely disrupted ankle mortise and distal tibia. Subtalar joint motion was also severely limited.
Neurological & Vascular Assessment
As detailed above, the neurovascular status of the foot was intact at presentation. Sensory function was preserved in all dermatomes of the foot. Motor function of the ankle (dorsiflexion, plantarflexion, inversion, eversion) could not be reliably assessed due to pain and mechanical instability but toe movements were present and strong. Given the high-energy nature of the injury, serial neurovascular examinations were instituted, and the patient was closely monitored for any signs of evolving compartment syndrome or neurological deficit.
Imaging & Diagnostics
Initial Radiographs
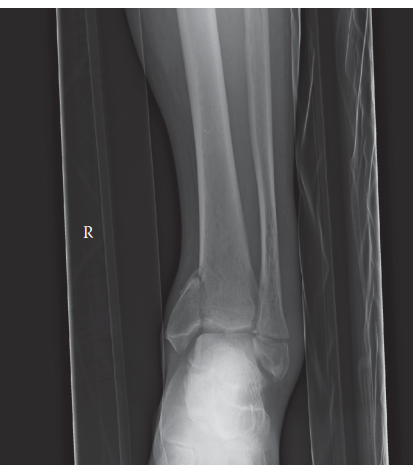
Standard anteroposterior (AP), lateral, and mortise views of the right ankle were obtained immediately in the emergency department. These revealed a complex fracture pattern involving the distal tibia (pilon fracture), the fibula, and the medial malleolus.
- AP View: Demonstrated significant comminution of the distal tibial plafond, with articular depression and metaphyseal extension. The talus was superiorly displaced and impacted into the tibial plafond. There was widening of the syndesmosis. A transverse fracture of the distal fibula was visible, approximately 4 cm proximal to the tip of the lateral malleolus.
- Lateral View: Confirmed the severe comminution and impaction of the tibial plafond, with marked posterior displacement of the talus relative to the tibial shaft. A large posterior fragment of the distal tibia was appreciated, involving a significant portion of the posterior malleolus. The fibular fracture was also visible.
- Mortise View: Highlighted the loss of ankle mortise congruity, with an increased medial clear space and disruption of the lateral clear space. The fibular fracture was evident, and a vertically oriented fracture of the medial malleolus was clearly visualized.
Further radiographs including AP and lateral views of the entire lower leg were performed to rule out a proximal fibular fracture (Maisonneuve injury) and any other ipsilateral lower limb trauma, all of which were negative. Foot radiographs were also obtained to exclude subtalar or midfoot injuries.
Computed Tomography (CT) Scan
Given the complexity of the fracture pattern and the involvement of the articular surface, a computed tomography (CT) scan of the right ankle with 3D reconstructions was deemed essential for definitive characterization and pre-operative planning. The CT scan was performed after initial stabilization and splinting.
The CT scan provided invaluable detail:
*
Articular Involvement:
Confirmed severe comminution and impaction of the distal tibial plafond, consistent with a Ruedi-Allgöwer Type III pilon fracture. Multiple articular fragments were identified, including a significant anterolateral fragment, a posteromedial fragment, and a large posterior malleolar fragment encompassing approximately 30% of the articular surface. There was substantial central impaction of the subchondral bone and articular cartilage.
*
Metaphyseal Comminution:
Extensive comminution of the distal tibial metaphysis was noted, extending proximally approximately 6-7 cm from the plafond. This created a highly unstable metaphyseal region with significant bone loss.
*
Fibular Fracture:
The distal fibular fracture was confirmed as a spiral oblique fracture, approximately 4 cm proximal to the tip of the lateral malleolus, with mild shortening and internal rotation.
*
Medial Malleolus:
The vertical fracture of the medial malleolus was better delineated, demonstrating displacement and extending proximally into the tibial metaphysis.
*
Syndesmosis:
Evidence of syndesmotic disruption was clear, with widening of the tibiofibular clear space and overlap. The posterior inferior tibiofibular ligament (PITFL) and anterior inferior tibiofibular ligament (AITFL) were avulsed from their attachments, suggested by small avulsion fragments.
*
Talus:
The talus was found to be laterally shifted and impacted into the comminuted plafond. No obvious talar osteochondral lesions were identified acutely, but this remains a long-term concern.
The detailed images from the CT scan were crucial for understanding the three-dimensional anatomy of the fracture, the number and size of fragments, the extent of articular depression, and the degree of metaphyseal comminution, all of which informed the surgical strategy.

(Representative CT scan image illustrating the complex pilon fracture with significant articular comminution and metaphyseal involvement.)
MRI Scan
An MRI was not indicated in the acute setting for this particular complex pilon fracture, as the CT scan provided sufficient detail for surgical planning regarding bone and articular injuries. MRI might be considered in cases of suspected severe deltoid ligament injury without a medial malleolus fracture, or to assess for osteochondral lesions or chronic soft tissue injuries later in the recovery phase if symptoms persist.
Pre-operative Templating
Based on the CT images, pre-operative templating was performed to anticipate implant size, plate length, screw trajectories, and potential need for bone graft substitutes. The strategy focused on fibular reconstruction first to restore length and rotation, followed by meticulous articular reduction of the tibial plafond, and then stabilization of the medial malleolus and syndesmosis. The significant metaphyseal comminution mandated a bridge plating construct for the distal tibia.
Differential Diagnosis
Given the presented clinical picture and initial imaging, a differential diagnosis was formulated, focusing on other high-energy ankle and distal tibial injuries.
| Feature | Pilon Fracture (Ruedi-Allgöwer Type III, AO/OTA 43-C3) | Trimalleolar Ankle Fracture (AO/OTA 44-C3) | Maisonneuve Fracture (AO/OTA 44-C1, -C2 variant) | Talar Neck Fracture (Hawkins Type II) |
|---|---|---|---|---|
| Pathoanatomy | High-energy axial load; distal tibial plafond comminution, articular impaction, often associated fibular and medial malleolar fx. Extensive metaphyseal comminution. | Rotational/abduction/adduction injury; fractures of lateral, medial, and posterior malleoli. Intact tibial plafond. | External rotation; high spiral fibular fx (proximal 1/3), syndesmotic disruption, often deltoid ligament rupture. Tibial plafond usually intact. | High-energy dorsiflexion; fracture of talar neck, often with subtalar dislocation. Risk of avascular necrosis (AVN). |
| Mechanism | Fall from height, motor vehicle accident (MVA) – axial loading + rotation. | Twisting injury, sports. | Pronation-external rotation. | High-energy ankle dorsiflexion with axial load. |
| Articular Surface | Always involved , significant impaction and comminution of tibial plafond. Subchondral bone depression. | Involved by malleolar fractures, but tibial plafond is intact . The talus remains congruent within the mortise. | Tibial plafond typically intact; syndesmosis disrupted. No direct plafond impaction. | Articular involvement of subtalar and ankle joints. Damage to vascular supply. |
| Imaging | Significant distal tibial comminution, impaction, displacement on AP/Lat X-rays. CT crucial for articular mapping and fragment analysis. Often involves multiple columns of the plafond. | Tri-malleolar fractures (lateral, medial, posterior). Mortise widening. No significant tibial plafond comminution. | High fibular fracture (proximal to ankle), wide mortise on X-ray, potentially positive stress views. Full-leg X-ray mandatory. CT may confirm syndesmotic injury. | Fracture line through talar neck; subtalar dislocation. Careful assessment for ankle joint involvement. Risk of AVN seen on later MRI. |
| Soft Tissue Injury | Severe , high risk of blistering, skin necrosis, compartment syndrome due to high energy. | Moderate to severe swelling, but typically less severe than pilon. | Moderate swelling, potential for compartment syndrome in severe cases. | Variable, can be severe, potential for open injury. |
| Treatment Principle | Restore articular congruity meticulously, stable fixation, address soft tissues. Often staged (external fixation then definitive ORIF). | Open reduction and internal fixation (ORIF) of malleoli to restore mortise congruity and stability. | ORIF of syndesmosis (high fibula may be non-op). Address deltoid and syndesmosis. | ORIF to restore alignment and prevent AVN. Early reduction is critical. |
For the presented case, the extensive articular comminution and impaction of the distal tibial plafond, as clearly demonstrated on both plain radiographs and the CT scan, unequivocally pointed towards a complex pilon fracture. The associated fibular and medial malleolar fractures, combined with syndesmotic disruption, further reinforced the diagnosis of a high-energy ankle injury involving the plafond.
Surgical Decision Making & Classification
Rationale for Operative Management
The decision for operative management was straightforward given the nature of the injury. Non-operative treatment for such a displaced, comminuted, and intra-articular pilon fracture (Ruedi-Allgöwer Type III, AO/OTA 43-C3) would invariably lead to severe malunion, chronic pain, significant functional disability, and accelerated post-traumatic arthritis. The goals of surgery were to:
1. Restore articular congruity of the tibial plafond.
2. Re-establish the length, rotation, and alignment of the fibula.
3. Stabilize the medial column via medial malleolus fixation.
4. Reduce and stabilize the syndesmosis.
5. Provide stable fixation allowing for early range of motion to minimize stiffness.
Classification Systems Applied
Several classification systems are relevant for understanding this complex ankle fracture:
-
Ruedi-Allgöwer Classification (for Pilon Fractures):
- Type I: Non-displaced articular fracture.
- Type II: Displaced articular fracture with minimal comminution.
-
Type III:
Severely comminuted and impacted articular fracture.
This patient's fracture, with extensive articular comminution, depression, and impaction, definitively falls into Ruedi-Allgöwer Type III . This classification highlights the difficulty of achieving anatomical reduction and the high risk of post-traumatic arthritis.
-
AO/OTA Classification (for Distal Tibia):
- The AO/OTA classification for distal tibia fractures is 43-A (extra-articular), 43-B (partial articular), or 43-C (complete articular).
- For this case, with complete articular involvement and severe comminution, the fracture is classified as 43-C3 . This signifies a multifragmentary articular and multifragmentary metaphyseal fracture, reflecting the highest severity within the complete articular category.
-
Danis-Weber Classification (for Fibular Fractures):
- Type A: Below the syndesmosis.
- Type B: At the level of the syndesmosis.
-
Type C:
Above the level of the syndesmosis.
The fibular fracture in this case was transverse/spiral oblique, approximately 4 cm proximal to the tip of the lateral malleolus, classifying it as a Weber B equivalent, indicating potential syndesmotic involvement. The associated syndesmotic disruption further supports this.
-
Lauge-Hansen Classification:
- While primarily for rotational ankle fractures, some components of this classification might be inferred. Given the axial load and rotational component from the fall, elements of Pronation-External Rotation (PER) or Pronation-Dorsiflexion (PDF) could be present, contributing to the fibular fracture and syndesmotic disruption, as well as the posterior malleolus fracture. However, the dominant feature is the axial impaction of the plafond, which is not fully captured by Lauge-Hansen.
Staging of Surgical Intervention
Due to the severe soft tissue swelling and impending skin compromise observed on initial presentation, a staged approach was deemed mandatory.
Stage 1 (Acute):
Immediate closed reduction and application of a spanning external fixator. This allowed for joint distraction, de-tensioning of the soft tissues, and restoration of overall limb alignment, while waiting for the "wrinkle sign" to appear, indicating resolution of soft tissue edema. During this period, diligent elevation, ice application, and serial soft tissue checks were performed. DVT prophylaxis was initiated.
Stage 2 (Definitive ORIF):
Performed 7 days post-injury, once the soft tissue envelope had significantly improved, as evidenced by the presence of skin wrinkles and reduced swelling. This delay significantly reduces the risk of wound complications, infection, and subsequent hardware exposure.
Surgical Technique / Intervention
Patient Positioning and Preparation
The patient was positioned supine on a radiolucent operating table, allowing unrestricted access for both anteromedial and anterolateral approaches, and for intraoperative fluoroscopy. A sterile tourniquet was applied to the thigh. The entire limb was prepped and draped in a standard sterile fashion. The external fixator, applied in Stage 1, was left in situ during prepping and draping and removed only after the definitive sterile field was established.
Surgical Approaches
A dual-incision approach was planned to address the fibula, the distal tibia (plafond and metaphysis), and the medial malleolus.
- Anterolateral Approach: An oblique incision, approximately 10-12 cm in length, was made between the fibula and the tibialis anterior tendon. This provided access to the lateral aspect of the distal tibia, the syndesmosis, and the fibular fracture. Care was taken to protect the superficial peroneal nerve.
- Anteromedial Approach: A curvilinear incision, approximately 8-10 cm in length, was made over the medial aspect of the ankle, centered over the medial malleolus and extending proximally along the tibial shaft. This provided access to the medial malleolus and the anteromedial aspect of the tibial plafond. Care was taken to protect the saphenous nerve and vein.
Reduction and Fixation Sequence
-
Fibular Fixation:
- The fibular fracture was exposed via the anterolateral approach.
- Reduction was achieved by direct manipulation, restoring length and rotation using small bone clamps. This step is critical as the fibula acts as a template for the overall length and rotation of the ankle mortise.
- A 1/3 tubular plate (7-hole, 3.5mm) was contoured and applied to the lateral aspect of the fibula, secured with cortical screws. One lag screw was placed across the spiral fracture component for interfragmentary compression. Fluoroscopy confirmed restoration of fibular length and rotation.
-
Articular Reduction of Tibial Plafond:
- The anterolateral approach allowed access to the anterolateral tibial plafond. Through the anteromedial approach, the medial aspect of the plafond was visualized.
- The main articular fragments were carefully identified using the CT scan as a roadmap. The central impacted fragments were elevated using bone tampers and dental picks through limited cortical windows in the metaphysis and direct visualization.
- The depressed articular surface was meticulously restored. Any underlying metaphyseal void was filled with an allograft bone chip matrix to provide structural support for the elevated articular surface.
- Temporary K-wires (1.5mm) were used to provisionally hold the articular fragments in anatomical position, particularly the large anterolateral and posteromedial fragments. Intraoperative fluoroscopy was crucial to confirm articular congruity in both AP and lateral planes.
-
Medial Malleolus Fixation:
- The medial malleolus fracture, being vertically oriented and displaced, was reduced under direct visualization through the anteromedial incision.
- Two 4.0mm partially threaded cancellous screws were inserted in an anterior-to-posterior direction, providing stable compression and fixation of the medial malleolus. In some cases, a small medial plate or tension band wiring might be used depending on the fragment size and fracture configuration.
-
Distal Tibial Metaphyseal Fixation (Bridge Plating):
- With the articular surface reduced and temporarily pinned, and the fibula and medial malleolus fixed, attention turned to the comminuted tibial metaphysis.
- A longer, pre-contoured locking plate (e.g., a specific pilon plate or a long periarticular locking plate, 10-hole, 3.5mm) was selected. The plate was applied to the anterolateral aspect of the distal tibia, bridging the comminuted metaphyseal segment.
- Proximally, the plate was secured to the intact tibial shaft with multiple locking screws. Distally, non-locking cortical screws were used to compress the plate to the anatomically reduced articular fragments, followed by locking screws for angular stability, ensuring subchondral support. The principle here was biological bridge plating, avoiding direct manipulation of the comminuted diaphyseal fragments.
- Fluoroscopy confirmed satisfactory plate position and screw length, ensuring no intra-articular screw penetration.
-
Syndesmotic Fixation:
- After all bone fragments were fixed, the stability of the syndesmosis was reassessed. Under fluoroscopic guidance, a cotton hook test was performed, and external rotation stress views were taken to check for any residual widening or instability.
- Given the clear syndesmotic disruption and ongoing instability, fixation was performed. A single 3.5mm tricortical syndesmotic screw was placed approximately 2 cm proximal to the ankle joint line, oriented 30 degrees posterior to the coronal plane, engaging three cortices (fibular and medial tibial). The ankle was held in neutral dorsiflexion during screw insertion to avoid overtightening.
- Alternatively, a flexible syndesmotic fixation device (e.g., TightRope) could have been considered, offering dynamic stability. For this case, due to the severe instability and comminution, a screw was chosen to provide robust initial stability.
Wound Closure
After final fluoroscopic confirmation of reduction and fixation, the surgical sites were thoroughly irrigated. Hemostasis was achieved. The incisions were closed in layers: deep fascia, subcutaneous tissue, and skin with absorbable sutures and staples respectively. Sterile dressings were applied, and a well-padded posterior splint was applied with the ankle in neutral dorsiflexion.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Period (Day 0-14)
- Immobilization: The ankle was maintained in a well-padded posterior splint, with the ankle in neutral dorsiflexion, for 2 weeks.
- Weight Bearing: Strict non-weight bearing (NWB) on the operative leg. Crutch or walker ambulation was initiated immediately.
- Elevation & Ice: Continuous elevation above the level of the heart was paramount to control swelling. Regular ice application was encouraged.
- Pain Management: Multimodal analgesia including NSAIDs, acetaminophen, and opioid pain medication as needed.
- DVT Prophylaxis: Low molecular weight heparin (LMWH) or oral anticoagulants for 4-6 weeks, or until full weight bearing is achieved.
- Wound Care: Dressings changed as per protocol. Close monitoring for signs of infection or wound complications.
Early Rehabilitation Phase (Weeks 2-8)
- Immobilization: At 2 weeks, sutures/staples were removed. The splint was replaced with a removable controlled ankle motion (CAM) boot.
- Weight Bearing: Continued strict NWB.
- Range of Motion (ROM): Gentle, protected active and passive ankle dorsiflexion/plantarflexion and inversion/eversion were initiated out of the boot, within the pain-free range. Emphasis on non-impact activities. Physical therapy sessions commenced, focusing on soft tissue mobilization and maintaining joint mobility.
- Exercises: Isometric exercises for the surrounding musculature (quadriceps, hamstrings, gluteals) to maintain strength and proprioception.
Progressive Loading Phase (Weeks 8-16)
-
Weight Bearing:
- At 8-10 weeks post-surgery, radiographic assessment (AP, lateral, mortise views) was performed to assess fracture healing. If sufficient healing was demonstrated (e.g., bridging callus), protected partial weight bearing (PWB) in the CAM boot was initiated, gradually increasing tolerance.
- By 12-14 weeks, progression to full weight bearing (FWB) in the CAM boot, and then transitioning out of the boot into supportive footwear, was anticipated, contingent on clinical and radiographic progression.
- Range of Motion & Strengthening: Aggressive physical therapy focused on restoring full ankle and subtalar joint ROM, improving strength of all lower extremity muscle groups, and addressing any gait abnormalities. Proprioceptive training (e.g., wobble board) was introduced.
- Hardware Consideration: The syndesmotic screw was typically considered for removal at 10-12 weeks post-op, especially for an active patient or if symptoms develop. In this case, it was removed at 12 weeks to allow for more physiological syndesmotic motion. Other hardware removal was reserved for symptomatic cases only.
Advanced Rehabilitation Phase (Months 4-12+)
- Functional Training: Progression to sport-specific training for the cyclist, including balance, agility, plyometrics, and cardiovascular conditioning.
- Return to Activity: Gradual return to cycling and other pre-injury activities, usually by 6-9 months, depending on functional recovery and radiographic union. High-impact activities may take longer, up to 12 months or more.
- Long-Term Follow-up: Regular clinical and radiographic follow-up for up to 2 years to monitor for post-traumatic arthritis, stiffness, or other complications. Patient education regarding potential long-term issues like stiffness and pain with weather changes was provided.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls (Key Takeaways for Success)
- Soft Tissue Envelope Dictates Timing: For high-energy pilon fractures, the dictum "the skin dictates the surgery" is paramount. A staged approach with initial external fixation and delayed definitive ORIF (waiting for the "wrinkle sign") is crucial to minimize wound complications, infection, and potential for hardware exposure.
- CT is Non-Negotiable: A pre-operative CT scan with 3D reconstructions is essential for understanding the complex fracture pattern, particularly the articular comminution, fragment size, impaction, and location of the large articular fragments (e.g., posterior malleolus). This allows for meticulous pre-operative planning and surgical templating.
- Fibular Length and Rotation First: The fibula is often considered the "ruler" of the ankle. Restoring its anatomical length, rotation, and alignment provides a stable lateral column and guides the subsequent reduction of the tibial plafond.
- Meticulous Articular Reduction: The primary goal is to restore anatomical congruity of the tibial plafond. This involves careful elevation of impacted fragments, subchondral bone graft or substitute for metaphyseal voids, and precise reduction of the articular fragments. Small, temporary K-wires are invaluable for provisional fixation.
- Biological Bridge Plating for Metaphysis: For comminuted metaphyseal segments, a bridge plating technique is preferred. This minimizes periosteal stripping and preserves biological viability, promoting healing while providing stable fixation. Locking plates are excellent for angular stability in comminuted areas.
- Address All Columns: Ensure all components of the fracture are addressed: lateral (fibula), medial (medial malleolus/deltoid), and posterior (posterior malleolus if significant).
- Syndesmotic Assessment and Fixation: Always reassess syndesmotic stability after fibular and tibial fixation. If unstable, fix it. The choice between tricortical screws and flexible fixation (e.g., TightRope) depends on surgeon preference, fracture pattern, and patient activity level.
- Early, Protected Motion: Once soft tissues allow and fixation is stable, initiate early protected range of motion to minimize stiffness, a common complication of pilon fractures.
Pitfalls (Common Mistakes and Complications to Avoid)
- Rushing Definitive Surgery: Operating on a "hot" ankle with severe swelling and skin compromise is a recipe for disaster, leading to high rates of wound dehiscence, infection, and potentially chronic osteomyelitis. Patience is key.
- Inadequate Imaging: Proceeding with surgery without a detailed CT scan for a complex pilon fracture can lead to surprises in the operating room, incomplete reduction, and poor outcomes.
- Ignoring Fibular Malreduction: Failing to restore anatomical fibular length, rotation, or alignment will inevitably lead to malreduction of the mortise and increased load on the medial ankle, resulting in poor biomechanics and accelerated arthritis.
- Incomplete Articular Reduction: Any residual step-off (>1-2 mm) or gap in the articular surface significantly increases the risk and severity of post-traumatic arthritis. Fluoroscopy alone is insufficient; direct visualization or mini-arthrotomy is often required.
- Overtightening the Syndesmosis: If using screws, overtightening the syndesmosis (especially with the ankle in plantarflexion) can restrict physiological ankle motion and lead to chronic pain or early screw breakage. Insert screws with the ankle in neutral or slight dorsiflexion.
- Premature Weight Bearing: Starting weight bearing too early, especially in a severely comminuted fracture with extensive metaphyseal bone loss, risks loss of reduction, hardware failure, and nonunion.
- Missing Compartment Syndrome: High-energy ankle fractures carry a risk of compartment syndrome. Maintain a high index of suspicion, perform serial clinical examinations, and consider compartment pressure monitoring if warranted.
- Inadequate Post-Operative Rehabilitation: Failure to engage in a structured and aggressive rehabilitation program will result in chronic stiffness, weakness, and functional limitations despite successful surgical fixation.
- Poor Patient Counseling: Pilon fractures are severe injuries with a high propensity for post-traumatic arthritis, even with optimal surgical management. Patients must be counselled appropriately regarding realistic expectations, potential long-term sequelae, and the prolonged recovery period.
