Tibial Nonunion Management: Bone Marrow Injection and Fixation
Key Takeaway
The management of tibial nonunions requires a meticulous balance of mechanical stability and biological optimization. Treatment modalities range from percutaneous bone marrow aspirate concentrate injections for delayed unions to complex exchange nailing, tension-band plating, and circular external fixation. This guide details the indications, surgical techniques, and biomechanical principles essential for achieving successful osseous union in compromised tibial fractures.
INTRODUCTION TO TIBIAL NONUNION MANAGEMENT
The treatment of tibial nonunions and delayed unions remains one of the most challenging paradigms in orthopaedic trauma surgery. Because of its precarious anteromedial soft tissue envelope and high susceptibility to high-energy open trauma, the tibia exhibits a disproportionately high rate of impaired fracture healing. Successful management requires a comprehensive understanding of the "diamond concept" of fracture healing: optimizing osteoprogenitor cells, providing an osteoconductive scaffold, ensuring osteoinductive signaling, and establishing a stable mechanical environment.
The Role of Advanced Imaging
Computed Tomography (CT) is highly valuable in determining the presence and morphology of a tibial nonunion, particularly in the presence of complex fracture patterns or obscuring hardware. It is imperative to distinguish a delayed union—which may proceed to clinical union without invasive surgical intervention—from a true nonunion, which requires surgical intervention to achieve healing.
Clinical Pearl: While CT has an excellent ability to evaluate fracture healing even when metallic implants are present, it suffers from a surprisingly low specificity (approximately 62%). The orthopaedic surgeon must remain cognizant that a CT scan may suggest a nonunion even when the fracture has achieved functional clinical union. In equivocal cases, definitive confirmation may only be achieved through direct surgical exploration.
PERCUTANEOUS BONE MARROW INJECTION
The utilization of autologous bone marrow in treating a variety of osseous defects has revolutionized the biological management of nonunions. Percutaneous bone marrow injection is a minimally invasive method of performing autologous bone grafting, offering significantly less donor-site morbidity than standard open iliac crest bone graft (ICBG) harvesting techniques.
It is critical to note that biological augmentation is not a substitute for adequate mechanical stabilization. Casting, functional bracing, external fixation, or closed intramedullary nailing must be utilized concurrently if the fracture lacks intrinsic stability. When combined with appropriate mechanical support, percutaneous marrow injections have demonstrated union rates approaching 80%.
Biological Rationale and Stem Cell Concentration
According to landmark studies by Hernigou et al., the efficacy of bone marrow aspirate concentrate (BMAC) relies on the presence of pluripotent hematopoietic and mesenchymal stem cells capable of osteogenic differentiation. However, the absolute number and viability of these pluripotent cells are significantly decreased in patients with a history of smoking, chronic alcohol consumption, or systemic corticosteroid use.
To maximize osteogenic potential, the donor marrow sample must be centrifuged (spun down) to isolate and concentrate the pluripotent cells located within the buffy coat. Success is directly dependent on the absolute number and concentration of stem cells available for injection at the nonunion site.
Surgical Warning: Injecting unconcentrated bone marrow aspirate yields suboptimal results due to the low baseline concentration of mesenchymal stem cells in peripheral marrow. Always utilize a dedicated aspiration/injection kit (e.g., the Ignite system) to concentrate the aspirate. Furthermore, combining the concentrated marrow with Demineralized Bone Matrix (DBM) provides an excellent osteoconductive scaffold to complement the osteogenic cells.
🔪 Surgical Technique: Percutaneous Bone Marrow Aspiration and Injection (Connolly et al.)
This procedure is typically performed as an outpatient surgery under general anesthesia or deep regional blockade.
- Patient Positioning: Place the patient prone on a radiolucent operating table to allow simultaneous access to the posterior iliac crests and the posterior aspect of the tibia.
- Aspiration Site Preparation: Prep and drape the posterior pelvis and the affected lower extremity in a standard sterile fashion.
- Marrow Aspiration: Insert a heavy-duty 16-gauge marrow aspiration needle into multiple distinct areas of the posterior superior iliac spine (PSIS) and the posterior wing of the ilium.
- Volume Collection: Obtain 100 to 150 mL of marrow. Technique Tip: Aspirate in small aliquots (2-4 mL per pull) and frequently redirect the trocar to avoid diluting the sample with peripheral blood.
- Centrifugation: Process the aspirate using a commercial centrifuge system to isolate the stem-cell-rich buffy coat.
- Injection: Under multi-planar image intensification (fluoroscopy), insert a marrow needle directly into the site of the nonunion or delayed union.
- Targeting the Graft: The preferred location for injection is the well-vascularized posterior aspect of the tibia, mirroring the location where a standard open posterolateral bone graft would be placed. Inject the concentrated marrow slowly to allow tissue expansion and prevent backflow along the needle tract.
ANTERIOR CENTRAL BONE GRAFTING
When open bone grafting is required, the posterolateral approach is traditionally favored. However, severe soft tissue compromise may preclude this route. Ryzewicz et al. described an alternative "anterior central" bone grafting technique, creating a synostosis between the fibula and tibia.
Surgical Approach and Rationale
This technique utilizes the anatomical interval between the anterior compartment (containing the extensor digitorum longus) and the lateral compartment (containing the peroneus longus and brevis).
- Indications: Highly effective for patients where severe posterior or posterolateral soft tissue injury (e.g., prior degloving, skin grafting, or flap coverage) precludes a standard posterolateral approach.
- Outcomes: In a retrospective review of 24 patients, this anterior central approach was found to heal faster and require fewer subsequent operations than the traditional posterolateral approach. The creation of a robust tibiofibular synostosis provides excellent secondary stability and a massive surface area for biological incorporation.
INTERNAL FIXATION STRATEGIES
The primary advantages of internal fixation in the setting of nonunion are its ability to acutely correct multi-planar deformity and to provide the absolute or relative stability required to promote osseous healing. The selection of the specific device depends on the magnitude of the deformity, the size of the fracture gap, the presence or history of infection, and the vascularity of the fracture fragments (hypertrophic vs. atrophic).
Closed Reamed Tibial Interlocking Nailing
Closed, reamed tibial interlocking nailing is currently considered by most academic authors to be the procedure of choice for diaphyseal tibial nonunions. Reamed nailing can be utilized in the vast majority of diaphyseal nonunions, boasting union rates of up to 93%.
- Biomechanics: Dynamic locked nails—sometimes accompanied by a fibular osteotomy to allow compression—provide relatively rigid fixation while permitting controlled axial impaction of the fracture site during weight-bearing.
- Biological Advantages: If performed closed, the delicate extraosseous vascular status of the tibia is not further compromised. Furthermore, the act of intramedullary reaming generates morselized autograft that is deposited along the endosteal surface, stimulating a robust regional healing response.
- Indications: Best reserved for the treatment of closed fractures initially treated by casting, where the medullary canals remain in close anatomical proximity. If the fracture exhibits bayonet apposition or severe translation, an open reduction is mandatory prior to nail passage.
Pitfall: Particular caution must be exercised if the original injury was an open fracture (Gustilo-Anderson Type II or greater), and especially if external fixation was utilized for a significant duration. There is a markedly increased risk of deep intramedullary infection if reamed nailing is performed in a tibia that hosted external fixation pins for longer than 2 weeks. In previously infected fractures, antibiotic-coated intramedullary nails should be strongly considered.
Exchange Nailing for Nonunion
In cases where an initial unreamed nail was used and the fracture progresses to nonunion (often heralded by hardware failure such as broken interlocking screws), exchange nailing is highly effective. The process involves removing the existing nail, sequentially over-reaming the canal by 1.5 to 2.0 mm to stimulate bleeding and clear fibrous tissue, and inserting a larger diameter, stiffer nail.

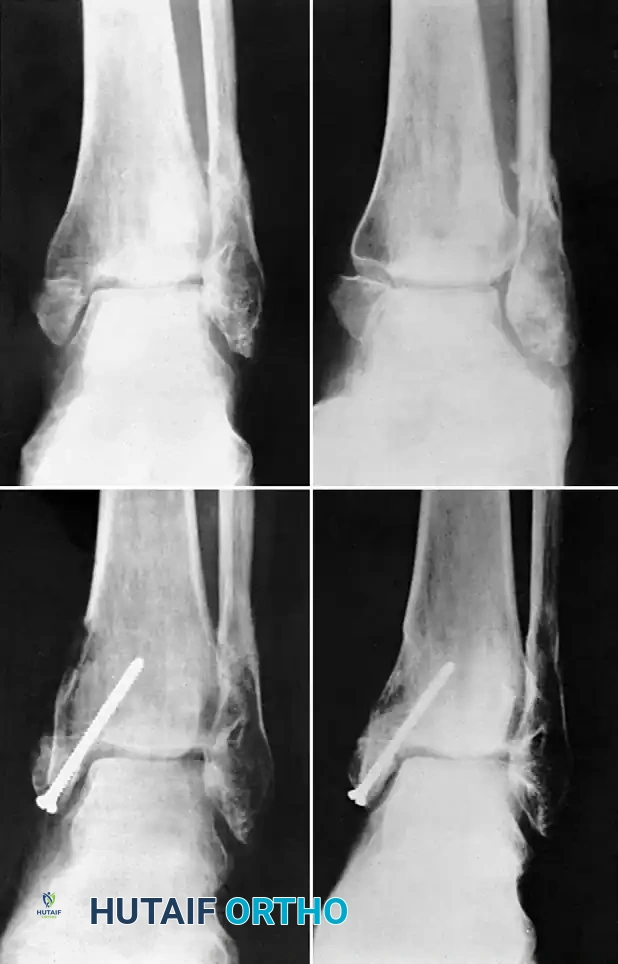
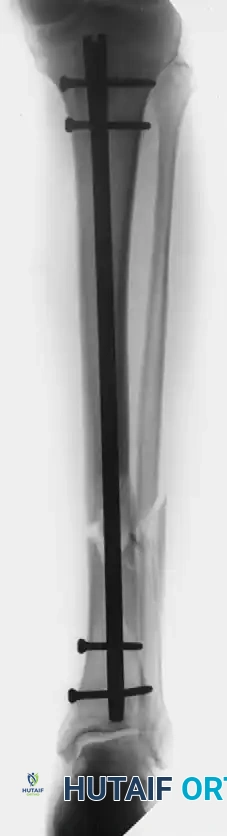
Figure A: Patient with an open tibial fracture treated initially with unreamed nailing. The broken distal interlocking screw is a clear radiographic indicator of nonunion and persistent mechanical instability despite prior attempts at dynamization.
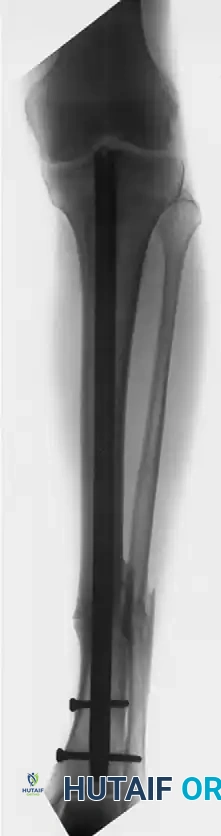
Figure B: Successful osseous union achieved after performing an exchange nailing procedure. The canal was reamed, and a larger diameter nail was inserted with new distal interlocking screws, providing the necessary stability and biological stimulation for healing.
Open Tibial Nailing
If there is no excessive bone loss that would lead to unacceptable limb shortening, open nailing of the tibia with direct anatomical restoration of alignment can be performed.
- Indications: This technique is primarily indicated for hypervascular (hypertrophic) nonunions of closed fractures where the overlying soft tissue coverage is pristine.
- Fibular Management: Osteotomy of the nonunion site can often be accomplished percutaneously under fluoroscopy. A fibular osteotomy is usually performed for diaphyseal fractures to allow the tibia to compress. However, resecting or osteotomizing the fibula in distal third fractures must be done with extreme caution, as it may allow the distal tibial fragment to displace into a valgus deformity.
Plate Osteosynthesis
Plate fixation remains a powerful tool, particularly when applied to the tension (convex) side of the deformity to achieve healing through dynamic compression.
- Surgical Technique: Anatomical reduction is typically achieved (accepting minor shortening if necessary to close gaps), and the fracture is sufficiently exposed to allow for the addition of autologous bone graft. Interfragmentary lag screws should be utilized whenever fracture geometry permits, and the plate must be meticulously contoured to the bone.
- Biological Preservation: Care must be taken not to devascularize the tibia. Avoid excessive periosteal stripping. Do not completely "take down" or aggressively debride the nonunion site unless you are treating a frankly infected nonunion.
- Indications & Advantages: Plating is highly advantageous over intramedullary nailing in patients who previously had external fixators, as the plate can be positioned to completely avoid the contaminated pin tracks. Additionally, low-profile locking plates or angled blade plates are the implants of choice when the distal fragment is highly osteoporotic or too distal to accommodate the requisite number of interlocking screws for an intramedullary nail.
- Risks: Deep infection and catastrophic implant failure remain the largest risks associated with open plating. It is generally contraindicated in patients with a history of active or latent osteomyelitis at the fracture site.
EXTERNAL FIXATION
Because of the high frequency of infection associated with tibial nonunions, external fixation remains an incredibly attractive and versatile option.
- Biological Preservation: The application of a circular or monolateral external fixator does not disturb the fragile fracture site biology, as the wires and half-pins are applied percutaneously away from the zone of injury.
- Deformity Correction: External fixation allows for the gradual correction of complex, multi-planar deformities. Furthermore, it permits the bridging of massive segmental bone defects through distraction osteogenesis and bone transport techniques (the Ilizarov method).
- Outcomes: Healing has been reported in up to 94% of nonunions utilizing dynamic axial external fixation. Exceptionally high rates of union are consistently reported with the Ilizarov method and hexapod systems, such as the Taylor Spatial Frame, especially in recalcitrant, infected, or highly complicated nonunions. When necessary, these frames can be combined with targeted bone grafting once the soft tissue envelope has been optimized.
POSTOPERATIVE PROTOCOLS
The postoperative rehabilitation protocol must be tailored to the specific fixation method utilized:
1. Intramedullary Nailing: Patients are typically allowed progressive weight-bearing as tolerated, which encourages axial micromotion and secondary bone healing.
2. Plate Fixation: Weight-bearing is generally restricted (toe-touch or non-weight-bearing) for 6 to 8 weeks until radiographic evidence of bridging callus is observed, preventing early fatigue failure of the plate.
3. External Fixation: Immediate weight-bearing is encouraged to stimulate the bone transport regenerate and the docking site, leveraging the dynamic axial micromotion permitted by the wire tension. Pin-site care protocols must be strictly enforced to prevent superficial infections.
📚 Medical References
- tibial nonunions, Clin Orthop Relat Res 266:259, 1991.
- Dahners LE, Mullis BH: Effects of nonsteroidal anti-infl ammatory drugs on bone formation and soft-tissue healing, J Am Acad Orthop Surg 12:139, 2004.
- Day L: Electrical stimulation in the treatment of ununited fractures, Clin Orthop Relat Res 161:54, 1981.
- DeHaas WG, Beaupré A, Cameron H, et al: The Canadian experience with pulsed magnetic fi elds in the treatment of ununited tibial fractures, Clin Orthop Relat Res 208:55, 1986.
- DeLee JC, Heckman JD, Lewis AG: Partial fi bulectomy for ununited fractures of the tibia, J Bone Joint Surg 63:1390, 1981.
- DiPasquale D, Ochsner MG, Kelly AM, et al: The Ilizarov method for complex
You Might Also Like