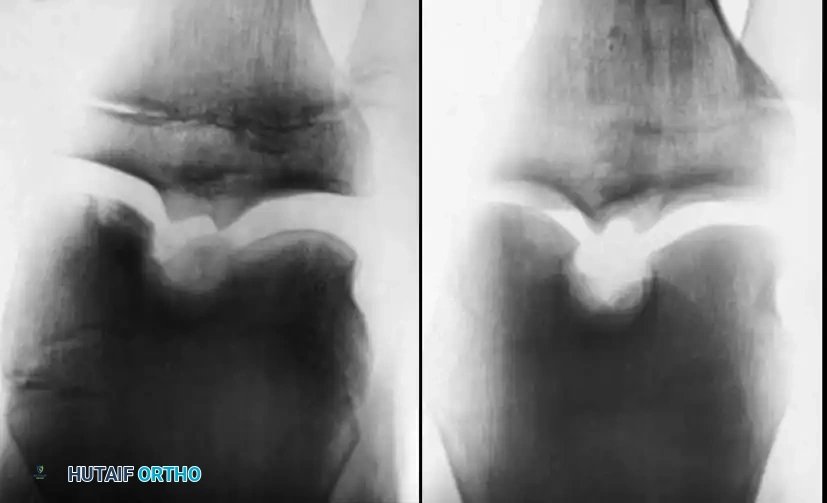
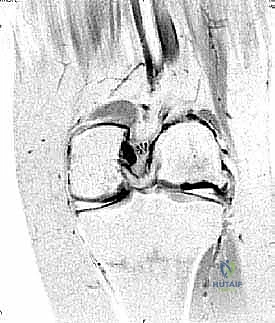
Arthroscopic Management of Osteochondritis Dissecans: An Intraoperative Masterclass
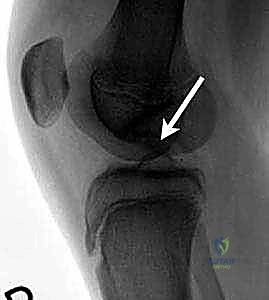
Key Takeaway
This masterclass provides an exhaustive, step-by-step guide to arthroscopic drilling for osteochondritis dissecans (OCD) of the knee. From meticulous preoperative planning and patient positioning to the granular intraoperative execution of transarticular, epiphyseal, hinged, and unstable lesion management, fellows will gain critical insights. We cover essential surgical anatomy, instrumentation, pearls, pitfalls, and comprehensive postoperative care, ensuring optimal patient outcomes.
Introduction and Epidemiology
Osteochondritis dissecans (OCD) represents a focal, idiopathic alteration of subchondral bone with risk for secondary disruption of the adjacent articular cartilage, resulting in delamination, sequestration, and potential articular instability. It is a relatively common cause of knee pain and mechanical dysfunction in children, adolescents, and young adults. The condition is classically subdivided into juvenile osteochondritis dissecans (JOCD), occurring in patients with open physes, and adult osteochondritis dissecans (AOCD), occurring in those with closed physes. The distinction is critical, as JOCD carries a significantly more favorable prognosis for spontaneous healing or healing following minimally invasive interventions such as arthroscopic drilling.

The exact pathogenesis of OCD remains a subject of ongoing debate, though contemporary consensus favors a multifactorial etiology heavily weighted toward chronic repetitive microtrauma. Historically, multiple factors have been implicated, including ischemia, inflammation, accessory centers of ossification, and genetic predisposition. The nomenclature "osteochondritis dissecans" historically implied an inflammatory etiology; however, extensive histological evaluation has failed to demonstrate acute or chronic inflammatory infiltrates as a primary driver, rendering the term somewhat of a misnomer.

Chronic repetitive microtrauma is hypothesized to induce subchondral microfractures, which subsequently fail to heal due to focal ischemia or alterations in endochondral ossification, ultimately leading to a localized avascular segment. Green and Banks historically proposed that ischemia was the primary factor, postulating an ischemic watershed region at the lateral aspect of the medial femoral condyle. However, subsequent anatomical studies have failed to corroborate a relative ischemic watershed in this specific topography, suggesting ischemia is secondary to microfracture rather than the primary inciting event.
Familial and genetic tendencies exist but are rare. Petrie identified OCD in only 1 of 86 first-degree relatives, whereas Mubarak and Carroll reported a highly penetrant familial cluster spanning four generations. While specific genetic, biochemical, or behavioral predispositions may exist in isolated cohorts, the most common form of OCD is sporadic and strongly associated with athletic participation involving repetitive impact loading.
Surgical Anatomy and Biomechanics
The anatomical distribution of OCD lesions in the knee is highly predictable. Approximately 70% to 80% of lesions occur on the medial femoral condyle, specifically on the lateral aspect of the medial femoral condyle (often remembered by the mnemonic LAME). Another 15% to 20% involve the lateral femoral condyle (typically the inferocentral weight-bearing region), and 5% to 10% involve the patella, predominantly the inferior pole or medial facet.

The predilection for the lateral aspect of the medial femoral condyle has significant biomechanical implications. In 1933, Fairbanks suggested that OCD might result from a "violent rotation inwards of the tibia, driving the tibial spine against the inner condyle." While isolated acute trauma and anterior tibial spine impingement may not fully explain the etiology of all posterolateral medial femoral condyle lesions, the frequent occurrence of OCD in patients involved in cutting, pivoting, and impact sports heavily supports a repetitive microtrauma model driven by cyclic shear and compressive forces.

Initially, the subchondral bone undergoes softening and focal necrosis, while the overlying articular cartilage remains grossly intact, sustained by synovial fluid diffusion. This intact cartilage stage represents the optimal window for arthroscopic drilling. As the subchondral structural support fails, the lesion progresses to early articular cartilage separation, fissuring, and eventually complete osteochondral separation, creating a loose body and a corresponding defect.

The vascular anatomy of the distal femur is derived from the genicular anastomoses. The epiphyseal blood supply is robust, but the subchondral capillary loops are end-arterioles. When cyclic loading exceeds the remodeling capacity of the subchondral bone, a stress fracture ensues. The resulting micromotion at the fracture site prevents neoangiogenesis, leading to a sclerotic margin that isolates the fragment biologically. Arthroscopic drilling aims to penetrate this sclerotic boundary, creating vascular channels that allow the influx of mesenchymal stem cells, angiogenic factors, and pluripotential marrow elements to facilitate creeping substitution and osseous union.
Indications and Contraindications
The management of OCD is dictated by patient age (physeal status), lesion stability, and clinical symptoms. Non-operative management, consisting of activity modification, protected weight-bearing, and immobilization, is the first-line treatment for stable JOCD lesions. However, surgical intervention is warranted when non-operative measures fail or when specific clinical and radiographic criteria are met.

Arthroscopic drilling is specifically indicated for stable OCD lesions (intact overlying cartilage) that have failed a minimum of 3 to 6 months of conservative management. It is also considered as a primary intervention in older adolescents nearing physeal closure or young adults with stable lesions, as their potential for spontaneous healing is markedly diminished.

Contraindications to isolated arthroscopic drilling include unstable lesions (characterized by articular cartilage fissuring, fluid tracking behind the lesion on MRI, or a discrete loose body), advanced osteoarthritis, and active intra-articular infection. Unstable lesions require fixation (e.g., bioabsorbable implants, variable pitch screws) with or without bone grafting, while unsalvageable detached fragments necessitate cartilage restoration procedures (e.g., microfracture, osteochondral autograft/allograft transfer, or autologous chondrocyte implantation).
Table of Indications for OCD Management
| Clinical Scenario | Lesion Stability | Physeal Status | Recommended Management Strategy |
|---|---|---|---|
| Asymptomatic incidental finding | Stable | Open | Observation, routine follow-up |
| Symptomatic, initial presentation | Stable | Open | Trial of non-operative management (activity modification, bracing) for 3-6 months |
| Symptomatic, failed conservative | Stable | Open | Arthroscopic extra-articular (retroarticular) or transarticular drilling |
| Symptomatic, initial presentation | Stable | Closed | Arthroscopic drilling (low threshold for early surgical intervention) |
| Symptomatic, fluid cleft on MRI | Unstable in situ | Open or Closed | Arthroscopic drilling with internal fixation (screws, darts) |
| Symptomatic, loose body | Detached | Open or Closed | Loose body removal/fixation, base debridement, bone grafting if necessary |
| Symptomatic, unsalvageable fragment | Detached | Open or Closed | Fragment excision, cartilage restoration (OATS, ACI, MACI) |
Pre Operative Planning and Patient Positioning
Thorough clinical evaluation and advanced imaging are prerequisites for operative planning. Physical examination findings in stable OCD are often subtle. Children and adolescents may present with a vague, poorly localized ache exacerbated by exercise and a slight antalgic gait. In late presentations with an osteochondral flap or loose body, classic mechanical symptoms such as locking, catching, buckling, and giving way emerge.

Careful palpation through varying degrees of knee flexion may localize a point of maximal tenderness over the anterior medial aspect of the knee, corresponding to the classic lesion location on the lateral aspect of the distal medial femoral condyle. Effusion, crepitus, and extreme pain through a normal range of motion are rarely observed with stable lesions. The Wilson sign is a classic but inconsistently present diagnostic maneuver. The test is performed with the knee flexed to 90 degrees; the tibia is internally rotated, and the knee is actively extended. A positive test elicits pain at approximately 30 degrees of flexion, which is relieved by external rotation of the tibia, theoretically due to the tibial eminence impinging on the medial condyle lesion.

Standard radiographic evaluation includes weight-bearing anteroposterior (AP), lateral, Merchant/sunrise, and notch (tunnel) views. The notch view, taken with the knee flexed to 45 degrees, is particularly critical for visualizing the classic posterolateral aspect of the medial femoral condyle.
Magnetic Resonance Imaging (MRI) is the gold standard for assessing lesion size, depth, subchondral bone viability, and, most importantly, stability. Criteria for instability on MRI include a high T2 signal line (fluid cleft) completely surrounding the lesion, focal full-thickness cartilage defects, multiple subchondral cysts, and a high T2 signal line breaching the articular cartilage.

For patient positioning, the patient is placed supine on the operating table. A thorough examination under anesthesia (EUA) is performed to assess range of motion and ligamentous stability. A non-sterile tourniquet is applied to the proximal thigh. The operative leg is typically placed in a standard leg holder or positioned over a lateral post to allow for valgus stress and access to the medial compartment, while allowing full flexion to at least 120 degrees, which is often necessary to access posterior lesions. The contralateral leg is placed in a well-padded gynecologic stirrup or kept flat on the table. Standard surgical preparation and draping are performed.
Detailed Surgical Approach and Technique
The primary goal of arthroscopic drilling is to decompress the sclerotic bone and create channels for revascularization and cellular migration without compromising the structural integrity of the overlying articular cartilage. There are two primary techniques: transarticular drilling and retroarticular (extra-articular) drilling.
Diagnostic Arthroscopy and Lesion Assessment
Standard anterolateral and anteromedial portals are established. A comprehensive diagnostic arthroscopy is performed, evaluating all compartments. The OCD lesion is carefully visualized and probed. A tactile assessment is critical; stable lesions will feel firm with an intact articular surface, whereas unstable lesions may exhibit softening, ballotability, or frank fissuring.

The International Cartilage Repair Society (ICRS) classification is commonly utilized during arthroscopy:
* Grade I: Stable, continuous but softened cartilage.
* Grade II: Partial discontinuity, stable on probing.
* Grade III: Complete discontinuity, "dead in situ" (unstable but not dislocated).
* Grade IV: Empty defect or defect with a loose body.
Drilling alone is reserved for ICRS Grade I and select Grade II lesions.
Transarticular Drilling Technique
Transarticular drilling is technically straightforward and relies on direct arthroscopic visualization. The primary disadvantage is the iatrogenic violation of the intact articular cartilage.

- Portal Placement: Depending on the lesion's location, the standard anteromedial or anterolateral portal may be used. For extreme posterior lesions, an accessory medial or lateral portal, or even a trans-patellar tendon portal, may be required to achieve an orthogonal approach to the articular surface.
- K-Wire Selection: A smooth K-wire, typically 0.045-inch or 0.062-inch (1.1 mm or 1.5 mm), is utilized. Thinner wires minimize cartilage damage but are prone to bending or breaking.
- Drilling Execution: The knee is flexed to the appropriate angle to bring the lesion into view and allow perpendicular access. The K-wire is advanced through the cartilage, through the subchondral lesion, and into the healthy epiphyseal cancellous bone.
- Depth and Spacing: The drill depth should be approximately 10 to 15 mm, ensuring penetration through the sclerotic base of the lesion. Drilling is repeated systematically, creating a grid-like pattern with holes spaced 3 to 5 mm apart.
- Debris Clearance: Copious irrigation is utilized to clear osteochondral debris generated by the drilling process to prevent secondary loose body formation or third-body wear.

Retroarticular Drilling Technique
Retroarticular drilling is technically more demanding and requires intraoperative fluoroscopy. Its primary advantage is the preservation of the articular cartilage, making it highly desirable for purely intact lesions.

- Targeting: The lesion is identified arthroscopically. An anterior cruciate ligament (ACL) tibial drill guide is frequently repurposed for this technique. The intra-articular tip of the guide is placed precisely on the center of the OCD lesion under direct arthroscopic visualization.
- Incision and Guide Placement: The extra-articular sleeve of the guide is positioned on the medial or lateral femoral epicondyle, taking care to avoid the medial patellofemoral ligament (MPFL) origin, the superficial medial collateral ligament (sMCL), or the lateral collateral ligament (LCL). A small stab incision is made down to the bone.
- Fluoroscopic Verification: Anteroposterior and lateral fluoroscopic views are obtained to confirm the trajectory of the guide. It is imperative to ensure the planned drill path does not violate the open distal femoral physis in JOCD patients, although central epiphyseal penetration is generally well-tolerated if necessary.
- Drilling: A 1.5 mm or 2.0 mm K-wire or drill bit is advanced through the guide sleeve. Fluoroscopy and arthroscopy are used concurrently. The drill is advanced until it breaches the sclerotic margin of the lesion without penetrating the articular cartilage.
- Multiple Channels: By slightly altering the angle of the extra-articular sleeve while keeping the intra-articular tip fixed (or moving it slightly), multiple divergent channels can be created into the lesion from a single extra-articular entry point.


Fixation of Unstable Lesions
If intraoperative probing reveals an unstable lesion (ICRS Grade III), drilling alone is insufficient. The lesion must be stabilized. The fibrous tissue at the base of the crater is debrided using a curette or arthroscopic shaver to expose bleeding subchondral bone. The fragment is then anatomically reduced.

Fixation can be achieved using various implants, including bioabsorbable pins, darts, or variable pitch compression screws. Metallic headless compression screws provide excellent biomechanical stability but require a secondary surgery for removal. Bioabsorbable implants eliminate the need for removal but have been associated with sterile sinus tract formation, osteolysis, and incomplete degradation. The choice of implant depends on the surgeon's preference, fragment size, and bone quality.


Complications and Management
While arthroscopic drilling is generally a safe and effective procedure, complications can arise, ranging from iatrogenic injury during the index procedure to failure of biological healing.

Iatrogenic cartilage damage is the most direct risk of transarticular drilling. Utilizing smooth K-wires rather than fluted drill bits and maintaining sharp instrumentation minimizes thermal necrosis and mechanical tearing of the chondral surface. In retroarticular drilling, the primary risk is inadvertent penetration of the articular surface or damage to the distal femoral physis. Careful fluoroscopic monitoring is mandatory to mitigate this risk.
Failure of healing or progression to fragment detachment occurs in a subset of patients, particularly older adolescents and adults. If follow-up MRI demonstrates persistent fluid clefts or the patient develops mechanical symptoms, revision surgery involving fixation, bone grafting, or cartilage restoration procedures is indicated.

Table of Complications and Salvage Strategies
| Complication | Incidence / Risk Factors | Prevention and Management Strategy |
|---|---|---|
| Iatrogenic Cartilage Damage | Moderate (inherent to transarticular approach) | Use small diameter (1.1-1.5mm) smooth K-wires; avoid fluted drill bits; irrigate to remove debris. |
| Physeal Arrest | Low (primarily a risk in retroarticular drilling) | Use fluoroscopy; aim centrally in the epiphysis; avoid multiple passes across the peripheral physis. |
| Hardware Prominence/Failure | Variable (if fixation is used adjunctively) | Countersink screws 1-2mm below cartilage surface; plan for routine hardware removal if metallic screws are used. |
| Bioabsorbable Implant Reaction | 5-10% (osteolysis, sterile effusion) | Monitor clinically; may require arthroscopic debridement if a sterile cyst or synovitis develops. |
| Nonunion / Progression to Instability | 10-30% (higher in AOCD vs JOCD) | Serial MRI monitoring; salvage with internal fixation, autologous bone grafting, or OATS/MACI if fragment is non-viable. |
| Intra-articular Loose Body | Low (from broken K-wire or dislodged fragment) | Ensure K-wires are not bent during drilling; thorough arthroscopic sweep prior to closure. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol following arthroscopic drilling of OCD is designed to protect the healing subchondral bone while preventing joint stiffness and muscle atrophy. The biological process of creeping substitution and osseous union is protracted, necessitating a cautious and phased approach to rehabilitation.

Phase 1: Protection and Early Motion (Weeks 0-6)
Immediately postoperatively, the patient is placed in a hinged knee brace locked in extension for ambulation. Weight-bearing is typically restricted to toe-touch or non-weight-bearing with crutches for the first 4 to 6 weeks to minimize compressive and shear forces across the healing lesion. Passive and active-assisted range of motion (ROM) exercises are initiated early, often utilizing a continuous passive motion (CPM) machine or guided physical therapy, to promote cartilage nutrition and prevent arthrofibrosis. Isometric quadriceps strengthening and straight leg raises are encouraged.
Phase 2: Progressive Weight-Bearing (Weeks 6-12)
At approximately 6 weeks, if clinical symptoms have subsided, weight-bearing is progressively advanced by 25% increments weekly until full weight-bearing is achieved. The brace is gradually weaned. Closed kinetic chain exercises, such as mini-squats and leg presses, are introduced, ensuring the arc of motion avoids high contact pressures on the specific location of the OCD lesion.
Phase 3: Strengthening and Proprioception (Months 3-5)
Once full, pain-free ROM and normal gait are achieved, the focus shifts to advanced strengthening, proprioception, and core stability. Isokinetic exercises, stationary cycling, and swimming are excellent modalities. Impact loading and running are strictly avoided during this phase.
Phase 4: Return to Play (Months 6+)
Return to high-impact sports or pivoting activities is not permitted until radiographic or MRI evidence of osseous healing is confirmed, which typically takes 6 to 9 months, and sometimes longer. The patient must demonstrate 90% or greater limb symmetry index on functional testing (e.g., hop testing) and have no effusion or pain with sport-specific drills prior to full clearance.
Summary of Key Literature and Guidelines
The literature surrounding the surgical management of OCD heavily emphasizes the distinction between juvenile and adult forms, as well as the critical nature of lesion stability.

Crawfurd and associates provided foundational natural history data, following 21 patients with undetached lesions left in situ with an average follow-up of 7.5 years. They noted healing in the medial femoral condyle in only 3 of 10 patients, whereas healing elsewhere was noted in 10 of 11 patients, highlighting the recalcitrant nature of classic LAME lesions.
More recently, the Research in OsteoChondritis of the Knee (ROCK) study group has provided comprehensive guidelines and classification systems to standardize treatment. Their consensus statements emphasize that drilling is highly effective for stable JOCD lesions that fail non-operative management, with healing rates frequently reported between 80% and 95%.
Kocher et al. identified several predictors of healing following non-operative and operative management. Factors associated with a higher risk of failure and need for subsequent surgery include larger lesion size (greater than 400 mm²), presence of a fluid cleft on MRI, and advanced skeletal maturity (closed physes). For adult OCD, or lesions in adolescents nearing skeletal maturity, the threshold for surgical intervention is significantly lowered, and primary drilling or fixation is often favored over prolonged, likely futile, non-operative trials.
In conclusion, arthroscopic drilling—whether transarticular or retroarticular—remains a cornerstone in the orthopedic surgeon's armamentarium for the treatment of stable osteochondritis dissecans. Meticulous surgical technique, appropriate patient selection based on physeal status and MRI findings, and strict adherence to protracted rehabilitation protocols are essential to achieve successful biological joint preservation.
Clinical & Radiographic Imaging























You Might Also Like