APPROACHES TO THE KNEE
Ten
The Knee

---
*
*
The knee is a synovial hinge joint, supported and stabilized by powerful
muscular and ligamentous forces. It is superficial on three sides (anterior, medial, and lateral), and approaches to it are comparatively straightforward. Because the knee joint is only covered by skin and retinacula on three of its four sides, the joint is ideal for arthroscopic approaches. Arthroscopy of the knee is also facilitated by the large size of the joint cavity. Arthroscopic approaches have largely replaced open surgical approaches for the treatment of meniscal pathology, anterior cruciate ligament reconstruction, and removal of loose bodies.
Two
arthroscopic approaches
are described that allow complete exploration of the knee joint.
Seven open approaches to the knee are described. These approaches are useful where arthroscopic equipment is not available. They are also of great importance when dealing with trauma of the knee joint associated with open wounds. Because the major neurovascular structures of the leg all pass posterior to the joint, the posterior approach is used mainly for exploration of these structures.
The
medial parapatellar approach,
the most common knee incision, can be used for a variety of procedures. The length of the incision depends on the pathology to be treated; when it is used fully, this approach gives an unrivaled exposure of the whole joint. It is suitable for total joint replacement.
The
approach for medial meniscectomy
is much more restricted. The introduction of the operative arthroscope has almost ended its use. The approach can be found in the electronic version of this book.
The
medial approach to the knee joint
affords easier access to the medial supporting structures of the knee. Because of its slightly more posterior placement and the curving nature of the approach, a flap can be developed that allows better visualization of the posteromedial corner of the joint.
The anatomy of the medial side of the knee is considered in a separate section after these approaches are described.
The
approach for lateral meniscectomy
provides adequate exposure, but its use is limited. The introduction of the operative arthroscope has almost ended its use. The approach can be found in the electronic version of this book. The
lateral approach
is used for ligamentous reconstruction of the knee’s lateral supporting structures. The anatomy of the knee’s lateral side is considered after these two approaches are outlined.
The
lateral approach to the distal femur,
an adjunct to the medial parapatellar incision, is used for repairs of ruptured anterior cruciate
ligaments. The approach enters the intercondylar notch from behind, allowing reattachment of the distal stump of a torn anterior cruciate ligament or the insertion of a graft. It usually is used in conjunction with an anteromedial approach to the knee.
The
posterior approach
to the knee is performed rarely, and when it is, it is usually for the repair of neurovascular structures and reconstruction of the tibial insertion of the posterior cruciate ligament. Open reduction and internal fixation of fractures of the posterior column of the tibial plateau is best carried out using the posterior approach to the tibial plateau (see Chapter 11). Its anatomy is considered after this approach is described.
General Principles of Arthroscopy
See Chapter 1, General Principles of Arthroscopy, Figs. 1-73 to 1-75.
Arthroscopic Approaches to the Knee
The knee is a large unconstrained hinge joint that is often described as subcutaneous. Its anteromedial and anterolateral coverings consist largely of fibrous tissue—the patellar retinaculum and joint capsule (see Figs. 10-32 and 10-33). Incisions through these coverings can be safely made without endangering any vital structures.
Arthroscopy of the knee has largely replaced open procedures for the following:
1. Meniscal resection or repair
2. Removal of loose bodies
3. Anterior or posterior cruciate ligament reconstruction
4. Synovial biopsy
5. Synovectomy
6. Debridement of early osteoarthritic knees, including microfracture
7. Treatment of osteochondritis dissecans
8. Arthroscopically assisted repair of tibial plateau fractures
12 The two most frequently used will be described.
The anterolateral portal is the one most commonly used for diagnostic
purposes; it is nearly always used in conjunction with the anteromedial portal. The combination of these approaches allows the use of the arthroscope along with arthroscopic instruments. Usually the arthroscope is inserted via the anterolateral portal and instruments are inserted via the anteromedial portal. However, either portal can be used for either purpose. These two approaches are described in this section.
Position of the Patient
10-1; see Figs. 10-9 and 10-41). Prep and drape the limb so that you are able to manipulate the knee during surgery. The use of an arthroscopic clamp placed around the tourniquet allows the surgeon to apply a valgus and external rotation force to the knee, facilitating access to the medial compartment. The use of a clamp, however, makes it more difficult to place the knee in the figure-of-eight position (placing the lateral malleolus of the involved extremity on the opposite thigh; see Figs. 10-8,
inset
to allow access to the lateral compartment of the knee. If a surgical assistant is available to provide the appropriate forces, the use of a clamp is not indicated.


 Figure 10-1 Place the patient supine on the operating table. Remove the end of the table so that you are able to manipulate the knee during surgery.
Landmarks and Incision
#### Lateral
Figure 10-1 Place the patient supine on the operating table. Remove the end of the table so that you are able to manipulate the knee during surgery.
Landmarks and Incision
#### Lateral
Flex and extend the knee and use your thumb to palpate the
lateral joint line.
Move your thumb toward the midline. You will feel the resistance of the lateral edge of the
patellar tendon.
Flex the knee to 90 degrees. Place your forefinger in the recess created by the lateral border of the patellar tendon and the lateral joint space. This is the so-called soft spot. Make an 8-mm transverse stab incision approximately 5 mm proximal to your finger, 1 cm to 1½ cm above the joint line (Fig. 10-2).
Medial
Move your finger to palpate the
medial joint line
and the medial edge of the _patellar tendon._10-2).


 Figure 10-2 Lateral incision: make a small 8-mm transverse stab incision 1½ cm above the lateral joint line. Medial incision: make an 8-mm stab incision 1½ cm above the medial joint line. Internervous Plane There is no internervous plane in these surgical approaches, which consist of incisions made in the medial and lateral patellar retinacula and joint capsule. No major nerves are present in these areas.
Surgical Dissection
With the knee flexed to 90 degrees, deepen the anterolateral skin incision using a sharp-ended blade. As you incise the retinaculum, you will suddenly feel a decrease in resistance. Withdraw the blade and insert the arthroscopic sheath and blunt trochar. Push the sheath and trochar into the anterolateral portion of the knee, taking care not to hit the underlying femur; then carefully extend the knee while advancing the arthroscopic sheath up into the suprapatellar pouch. Remove the trochar. Insert the 30-degree arthroscopic telescope. Switch on the irrigation fluid before switching on the light source to avoid thermal damage to the synovium.
Arthroscopic Exploration of the Knee
Figure 10-2 Lateral incision: make a small 8-mm transverse stab incision 1½ cm above the lateral joint line. Medial incision: make an 8-mm stab incision 1½ cm above the medial joint line. Internervous Plane There is no internervous plane in these surgical approaches, which consist of incisions made in the medial and lateral patellar retinacula and joint capsule. No major nerves are present in these areas.
Surgical Dissection
With the knee flexed to 90 degrees, deepen the anterolateral skin incision using a sharp-ended blade. As you incise the retinaculum, you will suddenly feel a decrease in resistance. Withdraw the blade and insert the arthroscopic sheath and blunt trochar. Push the sheath and trochar into the anterolateral portion of the knee, taking care not to hit the underlying femur; then carefully extend the knee while advancing the arthroscopic sheath up into the suprapatellar pouch. Remove the trochar. Insert the 30-degree arthroscopic telescope. Switch on the irrigation fluid before switching on the light source to avoid thermal damage to the synovium.
Arthroscopic Exploration of the Knee
Although the use of a preoperative MRI identifies most pathologies within the knee, it is important to ensure that each arthroscopic exploration examines all portions of the knee and not merely the site of the presumed pathology.
Order of Scoping
Begin with placing a 30-degree arthroscope in the suprapatellar pouch (Fig. 10-3, view 1). The arthroscope should be easily mobile, allowing you to examine all portions of the suprapatellar pouch, noting especially the synovium and checking for the presence of any loose bodies.
Keeping the knee fully extended, withdraw the arthroscope into the patellofemoral joint, rotating the telescope to allow examination of both the femoral and patellar aspects of the joint (see Fig. 10-3, view 2). Manipulating the patella medially and laterally facilitates this procedure.
Keeping the leg extended, slide the tip of the arthroscope into the lateral recess or gutter of the knee, passing the scope between the lateral aspect of the femur and the lateral capsule of the joint (see Fig. 10-3, view 3). Observe the lateral surface of the femur, and ensure that you can see
Fig. 10-3, view 4). The popliteal hiatus is a common recess for the presence of loose bodies.
10-4, view 6).
Withdraw the arthroscope into the center of the knee and gently flex to
10-510-6, view 8).
Fig. 10-7, view 9).
10-8, view 10).
To allow inspection of the undersurface of the menisci and to assess the integrity of the cruciate ligaments, insert the arthroscopic hook through the anteromedial portal and use it under direct vision of the arthroscope to palpate these structures.
Dang
Articular Cartilage
The
articular cartilage
of the knee may be damaged at two stages during arthroscopy: By the incision into the joint capsule or by the forceful insertion of an arthroscope. If the incision is made carefully, this problem should not occur. Remember that if you meet with resistance when manipulating the arthroscope within the knee, then it is certain that you are damaging the articular cartilage. More posteriorly based incisions on the
medial side may easily damage the articular surface of the medial femoral condyle if performed blind. Therefore, it is recommended that more posterior medial or lateral incisions, if needed, should be made under direct arthroscopic control. Ten seconds of careless use of an arthroscope within the knee may create the equivalent of 10 years of wear in that joint.



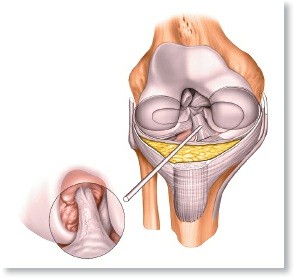
 Figure 10-3View 1: Begin with the arthroscope in the suprapatellar pouch and observe the synovium, checking for the presence of loose bodies. View 2: Withdraw the arthroscope into the patellofemoral joint. To observe the full extent of the joint, rotate the scope in both directions and move the patella medially and laterally. View 3: Slide the scope into the lateral recess of the knee and observe the lateral aspect of the lateral femoral condyle. View 4: Advance the arthroscope into the lateral gutter to view the insertion of the popliteal muscle.
Figure 10-3View 1: Begin with the arthroscope in the suprapatellar pouch and observe the synovium, checking for the presence of loose bodies. View 2: Withdraw the arthroscope into the patellofemoral joint. To observe the full extent of the joint, rotate the scope in both directions and move the patella medially and laterally. View 3: Slide the scope into the lateral recess of the knee and observe the lateral aspect of the lateral femoral condyle. View 4: Advance the arthroscope into the lateral gutter to view the insertion of the popliteal muscle.


 Figure 10-4View 5: With the knee in full extension, sweep the arthroscope into the lateral portion of the knee and observe the anterior horn of the lateral meniscus and the anterior part of the lateral femoral condyle. View 6: Advance the arthroscope medially and rotate it to look posteriorly. Observe the medial femoral recess.
Figure 10-4View 5: With the knee in full extension, sweep the arthroscope into the lateral portion of the knee and observe the anterior horn of the lateral meniscus and the anterior part of the lateral femoral condyle. View 6: Advance the arthroscope medially and rotate it to look posteriorly. Observe the medial femoral recess.


 Figure 10-5 View 7: Withdraw the arthroscope into the center of the joint, and then flex the knee to allow the arthroscope to enter the medial compartment. Observe the rim of the medial meniscus, the medial femoral condyle, and the medial tibial plateau. #### Meniscus
Figure 10-5 View 7: Withdraw the arthroscope into the center of the joint, and then flex the knee to allow the arthroscope to enter the medial compartment. Observe the rim of the medial meniscus, the medial femoral condyle, and the medial tibial plateau. #### Meniscus
The
meniscus
may be damaged by the scalpel or the arthroscope if the incisions are made too close to the joint line.
How to Enlarge the Approach
#### Local Measures
Manipulation of the knee is the key to success in visualizing all portions of the joint. To allow complete inspection of the knee, apply a valgus external rotation force to assess the posterior aspect of the medial compartment of the knee. You will also need to apply a varus internal rotation stress to examine the lateral portions of the knee. Remember that the telescope you
use is angled at 30 degrees. Changing the direction of the telescope will therefore significantly change the view that you obtain (see Figs. 1-73 to 1-75). This is most important when examining the posterior third of the medial compartment of the knee.


 Figure 10-6 View 8: Apply a valgus/external rotation force to the knee, and rotate the arthroscope so that it is looking laterally. Observe the posterior horn of the medial meniscus.
Figure 10-6 View 8: Apply a valgus/external rotation force to the knee, and rotate the arthroscope so that it is looking laterally. Observe the posterior horn of the medial meniscus.



 Figure 10-7 View 9: Withdraw the arthroscope into the intercondylar notch to observe the cruciate ligaments.
Figure 10-7 View 9: Withdraw the arthroscope into the intercondylar notch to observe the cruciate ligaments.


 Figure 10-8
(
Inset
) Flex the knee 90 degrees above the hip, and place the lateral malleolus of the operative side on the anterior aspect of the contralateral knee (figure-of-eight position).
View 10:
Advance the arthroscope into the lateral compartment of the knee to observe the lateral meniscus in its entirety.
Medial Parapatellar Approach
Figure 10-8
(
Inset
) Flex the knee 90 degrees above the hip, and place the lateral malleolus of the operative side on the anterior aspect of the contralateral knee (figure-of-eight position).
View 10:
Advance the arthroscope into the lateral compartment of the knee to observe the lateral meniscus in its entirety.
Medial Parapatellar Approach
The medial parapatellar approach3 is the workhorse approach to the knee. Extended to its full length, it allows excellent access to most structures.
Portions of the incision can be used to gain access to the suprapatellar pouch, the patella, and the medial side of the joint. When a straight, midline, longitudinal skin incision is used in conjunction with a medial parapatellar capsular approach, the incision offers an exposure large enough for total knee arthroplasty.
Minimally invasive approaches have been described for the insertion of total knee replacements where the patella is not dislocated. Such approaches may significantly reduce the damage done to the extensor mechanism by the surgery and reduce the amount of postoperative scarring that occurs in the suprapatellar pouch. Such approaches, however, limit visualization of the distal femur, making accurate positioning of implants more difficult. Additional imaging, especially computer-assisted surgery, may be helpful if these approaches are used for total knee replacement.
The uses of the medial parapatellar approach include the following:
1. 4
2. 12
3. Ligamentous reconstructions
4. Patellectomy
5. Drainage of the knee joint in cases of sepsis
6. Open reduction and internal fixation of distal femoral fractures when a medial plate is to be used
Medial meniscectomy, removal of loose bodies and anterior cruciate reconstruction is nearly always carried out using arthroscopic approaches.
Position of the Patient
Place the patient in a supine position on the operating table. The approach can be made with or without the use of a tourniquet. Operating without a tourniquet slows the surgical approach, but bleeding points are easy to pick up in the superficial surgical dissection. If you are using a tourniquet, it will need to be removed prior to closure of the wound to allow you to obtain hemostasis of the wound. If you are using a tourniquet, exsanguinate the leg by applying a compressive bandage or by elevating the limb for 5 minutes; then, inflate a tourniquet (Fig. 10-9).
Place a sandbag on the table in such a position that it supports the heel when the knee is flexed to 90 degrees. This sandbag will help maintain the knee in a flexed position during joint replacement surgery. Position a table support on the outer aspect of the upper thigh to prevent the leg from
falling into abduction when the knee is flexed.
Landmarks and Incision
#### Landmarks
Palpate the patella. Run fingers down to the
patellar ligament
(ligamentum patellae) which runs from the inferior border of the patella and is palpable to its insertion into the tibial tubercle.
Incision
Make a longitudinal straight midline incision, extending from a point 5 cm above the superior pole of the patella to below the level of the tibial tubercle (see Fig. 10-10).
Internervous Plane
There is no internervous plane in this approach, even when the incision is extended superiorly into the intermuscular plane between the vastus medialis and rectus femoris muscles. Because both of these muscles are supplied by the femoral nerve well proximal to this dissection the intermuscular plane is safe for knee surgery.
Superficial Surgical Dissection
Divide the subcutaneous tissues in the line of the skin incision, ensuring hemostasis. Develop a medial skin flap to expose the quadriceps tendon, the medial border of the patella, and the medial border of the patellar tendon. Enter the joint by cutting through the joint capsule. Begin on the medial side of the patella, taking care to leave a cuff of capsular tissue medial to the patella and lateral to the quadriceps muscle to facilitate closure. Divide the quadriceps tendon in the midline to enter the suprapatellar pouch. Finally, complete the capsule incision by dividing the fibrous tissue on the medial aspect of the patellar tendon. The capsular incision will almost certainly also cut through the synovium, since the capsule and synovium are intimately related.
10-10 10-12).
Deep Surgical Dissection
If the approach is to be used for reconstruction of a fracture of the medial femoral condyle retract the patella laterally and the cut edge of the knee joint capsule medially to expose the anterior and medial aspects of the condyle.
10-910-13).

 Figure 10-9 Position of the patient for the medial parapatellar approach. Begin with the straight leg position, and then flex the knee for the deeper dissection.
Figure 10-9 Position of the patient for the medial parapatellar approach. Begin with the straight leg position, and then flex the knee for the deeper dissection.

 Figure 10-10 Make a longitudinal, straight, midline incision.
Figure 10-10 Make a longitudinal, straight, midline incision.


 Figure 10-11 Make a medial parapatellar capsular incision.
Figure 10-11 Make a medial parapatellar capsular incision.



 Figure 10-12 Continue the incision through the joint capsule and along the patellar ligament and quadriceps tendon to gain access to the joint. In the case of revision surgery, the suprapatellar pouch is reduced in size or may actually be obliterated. Careful sharp dissection through the scar tissue may significantly improve the mobility of the patella, which allows greater flexion of the knee and eversion of the patella.
Figure 10-12 Continue the incision through the joint capsule and along the patellar ligament and quadriceps tendon to gain access to the joint. In the case of revision surgery, the suprapatellar pouch is reduced in size or may actually be obliterated. Careful sharp dissection through the scar tissue may significantly improve the mobility of the patella, which allows greater flexion of the knee and eversion of the patella.
In those rare cases in which the patella still does not dislocate,
s incorporate a central peg that makes reattachment of a bone block impossible if a screw is to be used. In such cases, a staple fixation may be indicated.
When the patella is dislocated and the knee is flexed fully, this incision provides the widest possible exposure of the entire knee joint.
Dang
Nerves
The
infrapatellar branch of the saphenous nerve
often is cut during this approach. The major danger in cutting the nerve is the development of a postoperative painful neuroma. Because the area of anesthesia produced usually is not troublesome, do not repair the nerve if it is cut. Instead, resect it and bury its end in fat to decrease the chances that a painful neuroma will form (see Figs. 10-32 and 10-35).




 Figure 10-13 Dislocate the patella laterally, and flex the knee to 90 degrees.
Figure 10-13 Dislocate the patella laterally, and flex the knee to 90 degrees.

--- Figure 10-14 Detach the patellar ligament attachment with an underlying block of bone. #### Muscles and Ligaments
If the patellar ligament becomes avulsed from its insertion on the tibia, it is difficult to reattach. Postoperative mobilization of the knee is delayed and residual stiffness is common.
How to Enlarge the Approach
#### Local Measures
Superior Extension.
Extend the approach proximally between the rectus femoris and vastus medialis muscles. Then, split the underlying vastus intermedius muscle to expose the distal two-thirds of the femur. Stay in the distal third of the thigh; more proximally, the branches of the femoral nerve may become involved, resulting in partial denervation (see Anteromedial Approach to the Distal Two-thirds of the Femur in Chapter 9, see Figs. 9-16 to 9-20).
Inferior Extension. Mobilize the upper part of the attachment of the patellar ligament to the tibia or remove the patellar ligament with an
underlying block of bone. This extension may be useful in dealing with complex intra-articular fractures of the knee joint. (See the section detailing the lateral approach to the distal femur for combined use in repair of the cruciate ligament.)
Approach for Medial Meniscectomy
14 was a common formal incision for the knee. It is quite flexible, with several acceptable locations for incision and many different ways to position the patient. Some surgeons advocate a transverse skin incision over the joint line; although this limits the view of the knee, it provides better access to the meniscus itself. Others prefer longitudinal or oblique incisions, which offer a better view of such other intra-articular structures as the cruciate ligaments. Although operative arthroscopy has almost abolished the need for this approach, it remains a useful one in those parts of the world where arthroscopy is not available.
The uses of the anteromedial approach include the following:
1. Medial meniscectomy
2. Partial meniscectomy
3. Removal of loose bodies
4. Removal of foreign bodies
5.
Position of the Patient
10-15). Remove the end of the table so that the knee can be flexed beyond a right angle.
This position requires good lighting so that the meniscus can be seen during surgery. The light must be adjusted continually to keep it shining directly into the depths of the wound. A headlamp is the best light source.
Exsanguinate the limb by elevating it for 2 to 5 minutes or by applying
a soft rubber bandage. Then, inflate a tourniquet.
Landmarks and Incision
#### Landmarks
The
medial joint line
must be accurately identified because incisions can easily be made too high. To allow the line to be palpated with certainty flex and extend the knee.
Locate the inferomedial corner of the patella.

 Figure 10-15A: Position of the patient for medial meniscectomy. B: Improper placement of the sandbag pushes the popliteal artery against the posterior joint capsule. C: Proper placement of the sandbag under the affected thigh. #### Incision
Figure 10-15A: Position of the patient for medial meniscectomy. B: Improper placement of the sandbag pushes the popliteal artery against the posterior joint capsule. C: Proper placement of the sandbag under the affected thigh. #### Incision
Begin the incision at the inferomedial corner of the patella. Angle it inferiorly and posteriorly, ending about 1 cm below the joint line. Incisions
10-1710-18).
Deep Surgical Dissection
20 10-21).
Dang
Nerves
The
infrapatellar branch of the saphenous nerve
Fig. 10-16).

 Figure 10-16 Incision for anteromedial approach for medial meniscectomy.
Figure 10-16 Incision for anteromedial approach for medial meniscectomy.

---
Figure 10-17 Incise down to the anteromedial aspect of the joint capsule.

 Figure 10-18 Incise the joint capsule in line with the incision to reveal the extrasynovial fat. #### Vessels
Figure 10-18 Incise the joint capsule in line with the incision to reveal the extrasynovial fat. #### Vessels
Because the
popliteal artery
is immediately behind the posterior joint capsule, any injury to the posterior joint capsule may damage the artery. If the knee is flexed, the posterior joint capsule falls away from the tibia and femur, taking the artery with it. A sandbag placed directly under the
popliteal fossa prevents the capsule from moving posteriorly and must be avoided at all costs (see Fig. 10-15B,C).
Muscles and Ligaments
The
coronary ligament
(the meniscotibial element of the deep medial ligament) connects the periphery of the meniscus with the joint capsule and tibia, and may be damaged if the incision through the synovium is made at the joint line (see Figs. 10-33 and 10-34).
Incisions made too far posteriorly may cut the
superficial medial ligament
(the tibial collateral ligament) as it runs from the medial epicondyle of the femur to its insertion on the tibia under cover of the pes anserinus (see Figs. 10-27 and 10-28).
Special Structures
The
fat pad
occupies varying amounts of the anterior portion of the knee joint and should not be damaged. Damage may produce adhesions within the joint and, in theory, can interfere with the blood supply to the patella (see Fig. 10-12).
The
medial meniscus
may be incised accidentally during the opening of the synovium unless the knee joint is entered well above the joint line.
How to Enlarge the Approach
#### Local Measures
Three factors may improve the exposure offered by this approach:

 Figure 10-19 Incise the synovium to gain access to the joint.
Figure 10-19 Incise the synovium to gain access to the joint.

 Figure 10-20 Open the joint capsule and synovium to the joint line to prevent damage to the meniscus and synovial fat pad.
Figure 10-20 Open the joint capsule and synovium to the joint line to prevent damage to the meniscus and synovial fat pad.

 Figure 10-21 Flex the knee and use retractors to gain further access to the meniscus. 1.
Retraction. Retractors must be positioned and repositioned carefully to ensure the best possible view of the intra-articular structures.
Figure 10-21 Flex the knee and use retractors to gain further access to the meniscus. 1.
Retraction. Retractors must be positioned and repositioned carefully to ensure the best possible view of the intra-articular structures.
2.
Position of light. Light should shine directly into the wound, usually from over the surgeon’s shoulder. Constant readjustment is necessary, and the use of a headlamp is invaluable.
3. A valgus stress will open up the medial side of the joint. Flexion of the knee allows better access to the back of the medial side of the joint. If the posterior horn of the medial meniscus must be seen, however, a better view is obtained by putting the leg into full extension and
applying a distraction and valgus force. However, visualization of the peripheral parts of the posterior horn is always very limited in this surgical approach when compared to arthroscopic approaches.
Extensile Measures
Posterior Extension. The dissection is limited posteriorly by the superficial medial ligament, which crosses the joint just in front of the midpoint of the femur. For better access to the posterior half of the joint, a second incision must be made behind this ligament. This is usually only required for excision of a retained posterior horn.
10-2210-23).


 Figure 10-22 Insert a blunt instrument into the joint, and push it backward along the inside of the medial joint capsule. Palpate posteriorly until the instrument can be felt beneath the skin.
Figure 10-22 Insert a blunt instrument into the joint, and push it backward along the inside of the medial joint capsule. Palpate posteriorly until the instrument can be felt beneath the skin.

 Figure 10-23 Make a second longitudinal posterior incision to enter the posteromedial aspect of the joint.
Superior Extension. To extend the incision superiorly, continue incising the skin along the medial border of the patella. Then, incise the medial patellar retinaculum and the underlying joint capsule in the same line to reach the back of the patella. Further superior extension exposes the suprapatellar pouch, which is a frequent site of loose bodies in the knee.
Figure 10-23 Make a second longitudinal posterior incision to enter the posteromedial aspect of the joint.
Superior Extension. To extend the incision superiorly, continue incising the skin along the medial border of the patella. Then, incise the medial patellar retinaculum and the underlying joint capsule in the same line to reach the back of the patella. Further superior extension exposes the suprapatellar pouch, which is a frequent site of loose bodies in the knee.
The incision may be extended still farther proximally in the muscular plane between the vastus medialis and rectus femoris muscles, exposing the distal two-thirds of the femur.
Inferior Extension. Inferior extension can cut the infrapatellar branch
of the saphenous nerve and is not recommended.
Medial Approach to the Knee and Its Supporting Structures
16 provides the widest possible exposure of the ligamentous structures on the medial side of the knee. Although it is used mainly for the exploration and treatment of damage to the superficial medial (collateral) ligament and medial joint capsule, the approach also can be used for a medial meniscectomy in conjunction with ligamentous repair and for the repair of a torn anterior cruciate ligament. (See the section regarding the lateral approach to the distal femur.)
Position of the Patient
10-24).
Landmark and Incision
#### Landmark
Palpate the
adductor tubercle
on the medial surface of the medial femoral condyle. It lies on the posterior part of the condyle in the distal end of the natural depression between the vastus medialis and hamstring muscles.
Incision
10-25).
Internervous Plane
There is no true internervous plane in this approach. Because the nerves at the level of the knee pass posterior to the approach in the popliteal fossa,
dissection is quite safe. The only cutaneous nerve that may be damaged is the saphenous nerve and its branches.
Superficial Surgical Dissection
Raise the skin flaps to expose the fascia. The exposure should extend from the midline anteriorly to the posteromedial corner of the knee posteriorly (Fig. 10-26).

 Figure 10-24 Position for the medial approach to the knee.
Figure 10-24 Position for the medial approach to the knee.

 Figure 10-25 Make a long, curved incision. The middle of this incision runs parallel and about 3 cm medial to the medial border of the patella. The infrapatellar branch of the saphenous nerve crosses the operative field transversely and is sacrificed; however, the saphenous nerve itself, which emerges from between the gracilis and sartorius muscles, must be preserved, as must the long saphenous vein in the posteromedial aspect of
Figure 10-25 Make a long, curved incision. The middle of this incision runs parallel and about 3 cm medial to the medial border of the patella. The infrapatellar branch of the saphenous nerve crosses the operative field transversely and is sacrificed; however, the saphenous nerve itself, which emerges from between the gracilis and sartorius muscles, must be preserved, as must the long saphenous vein in the posteromedial aspect of
the dissection. (The infrapatellar branch of the saphenous nerve should be cut and the end buried in fat to diminish the chances of the formation of a painful neuroma.)
Deep Surgical Dissection
Exposing the deep structures within the knee involves incising the layers that cover them, either in front of or behind the superficial medial ligament (the medial collateral ligament). These separate incisions provide access to the anterior and posterior parts of the medial side of the joint, respectively.
Anterior to the Superficial Medial Ligament
Use the anterior approach to expose the superficial medial ligament, the anterior part of the medial meniscus, and the cruciate ligament.
10-2610-27).


 Figure 10-26 Retract the skin flaps to expose the fascia of the knee. Note that the infrapatellar branch of the saphenous nerve crosses the operative field transversely. Incise the fascia along the anterior border of the sartorius. Retract all three muscles posteriorly to expose the tibial insertion of the superficial medial ligament, which lies deep and distal to the anterior edge of the sartorius. Note that the ligament inserts some 6 to 7 cm below the
Figure 10-26 Retract the skin flaps to expose the fascia of the knee. Note that the infrapatellar branch of the saphenous nerve crosses the operative field transversely. Incise the fascia along the anterior border of the sartorius. Retract all three muscles posteriorly to expose the tibial insertion of the superficial medial ligament, which lies deep and distal to the anterior edge of the sartorius. Note that the ligament inserts some 6 to 7 cm below the
10-28). Apply a gentle valgus force to the superficial medial ligament to reveal its point of injury.
10-29).
Posterior to the Superficial Medial Ligament
The posterior approach exposes the posterior third of the meniscus and the posteromedial corner of the knee.
of the medial femoral condyle usually will be seen, with its underlying meniscus visible through the torn posteromedial joint capsule. If the capsule is intact, expose the posteromedial corner of the joint by separating the medial head of the gastrocnemius muscle from the semimembranosus muscle. Although both muscles are supplied by the tibial nerve, this intermuscular plane is a safe area for dissection, because the semimembranosus receives its nerve supply well proximal to the approach and the gastrocnemius receives it well distal.


 Figure 10-27 Flex the knee and retract the sartorius posteriorly to uncover the remaining components to the pes anserinus. Finally, separate the medial head of the gastrocnemius muscle from the posterior capsule of the knee joint almost to the midline by blunt dissection (permits inspection or treatment of posterior intra-articular or periarticular
Figure 10-27 Flex the knee and retract the sartorius posteriorly to uncover the remaining components to the pes anserinus. Finally, separate the medial head of the gastrocnemius muscle from the posterior capsule of the knee joint almost to the midline by blunt dissection (permits inspection or treatment of posterior intra-articular or periarticular
Fig. 10-31). Repair of the posteromedial comer of the joint also is possible.


 Figure 10-28 Retract all three muscles (sartorius, semitendinosus, and gracilis) posteriorly to expose the tibial insertion of the superficial medial ligament. ### Dang
Figure 10-28 Retract all three muscles (sartorius, semitendinosus, and gracilis) posteriorly to expose the tibial insertion of the superficial medial ligament. ### Dang
Nerves
The cut end of the
infrapatellar branch of the saphenous nerve
should be buried in fat to prevent the formation of a painful postoperative neuroma.
10-32; see Fig. 10-35).
Vessels
The
saphenous vein
appears in the posterior corner of the superficial dissection. Because it may be required for future vascular procedures, it should be preserved (see Fig. 10-35).
The
medial inferior genicular artery
curves around the upper end of the tibia. It may be damaged when the medial belly of the gastrocnemius muscle is lifted off the posterior capsule: The damage may go unnoticed until the wound is closed and the tourniquet is released (see Figs. 10-38 and 10-39).

 Figure 10-29 Make a longitudinal medial parapatellar incision to gain access to the inside of the front of the knee joint. The
popliteal artery
lies against the posterior joint capsule in the midline and is adjacent to the medial head of the gastrocnemius muscle. Take care to avoid injuring the vessel during separation of the gastrocnemius from the joint capsule (see Figs. 10-58 and 10-61).
Special Problems
Hematomas under the skin flap that develop postoperatively can cause skin necrosis. Therefore, the large skin flaps that are created in this approach should be drained well.
How to Enlarge the Approach
The incision already is extensive, providing exposure to all the medial structures of the knee, and cannot be extended usefully in either direction. (For repair of the anterior cruciate ligament, see the section describing the lateral approach to the distal femur.)
Figure 10-29 Make a longitudinal medial parapatellar incision to gain access to the inside of the front of the knee joint. The
popliteal artery
lies against the posterior joint capsule in the midline and is adjacent to the medial head of the gastrocnemius muscle. Take care to avoid injuring the vessel during separation of the gastrocnemius from the joint capsule (see Figs. 10-58 and 10-61).
Special Problems
Hematomas under the skin flap that develop postoperatively can cause skin necrosis. Therefore, the large skin flaps that are created in this approach should be drained well.
How to Enlarge the Approach
The incision already is extensive, providing exposure to all the medial structures of the knee, and cannot be extended usefully in either direction. (For repair of the anterior cruciate ligament, see the section describing the lateral approach to the distal femur.)


 Figure 10-30
Retract the sartorius, semitendinosus, and gracilis posteriorly to expose the posteromedial corner of the joint. Orientation of the knee (
inset
).
Figure 10-30
Retract the sartorius, semitendinosus, and gracilis posteriorly to expose the posteromedial corner of the joint. Orientation of the knee (
inset
).


 Figure 10-31 Expose the posteromedial corner of the knee joint by first separating the gastrocnemius muscle and the posterior capsule of the joint, and then performing a capsulotomy posterior to the tibial collateral ligament.
Figure 10-31 Expose the posteromedial corner of the knee joint by first separating the gastrocnemius muscle and the posterior capsule of the joint, and then performing a capsulotomy posterior to the tibial collateral ligament.




 Figure 10-32 The outer layer of the anteromedial aspect of the knee joint. ## Applied Surgical Anatomy of the Medial Side of the Knee
Overview
As Warren and Marshall pointed out, the ligaments on the medial side of the knee are merely “condensations within tissue planes.”17 he medial side of the knee.
Figure 10-32 The outer layer of the anteromedial aspect of the knee joint. ## Applied Surgical Anatomy of the Medial Side of the Knee
Overview
As Warren and Marshall pointed out, the ligaments on the medial side of the knee are merely “condensations within tissue planes.”17 he medial side of the knee.
17 Approaches to the knee enter the joint by incising these layers sequentially, from outside to inside.
Outer Layer
The outer layer consists of the proximal continuation of the deep fascia of the thigh. It encloses the sartorius muscle, whose fibers blend with the fascial layer before they insert into the tibia.
Anteriorly, the outer layer blends with fibrous tissue derived from the vastus medialis muscle to form the medial patellar retinaculum. Posteriorly, the layer is continuous with the deep fascia, which covers the gastrocnemius muscle and the roof of the popliteal fossa (Fig. 10-35; see Fig. 10-32).
Middle Layer
10-33 and 10-34).
Above the superficial medial ligament, fibrous tissue from the middle layer passes to the medial side of the patella, forming the medial patellofemoral ligament (see Fig. 10-34).
Posterior to the superficial medial ligament, the fibrous tissue of the middle layer merges with that of the true joint capsule (deep layer) and the tendon of the semimembranosus muscle (Fig. 10-36).
The semimembranosus muscle runs down across the popliteal fossa before it inserts into the back of the medial condyle of the tibia. Three expansions of fibrous tissue come from the muscle’s tendon to reinforce the supporting structures of the knee. The tough
oblique poplite_ _al ligament,
one of the expansions, crosses the popliteal fossa, extending upward and laterally before attaching to the lateral femoral condyle (
10-3810-38). These muscular insertions are thought to be very important for the dynamic stabilization of the knee. In cases of damage to the posteromedial corner of the knee, they should be reattached in their anatomic position, if possible.
The
semitendinosus
and
gracilis
muscles run between the superficial and middle layers of the supporting structures of the knee. They insert into the tibia under the tendon of the sartorius muscle (in the outer layer), where they become part of the outer layer (see Figs. 10-34 and 10-36).
Deep Layer
The deep layer consists of the joint capsule itself as it attaches just above and below the margins of the articular surfaces of the tibia and femur. Anteriorly, the true capsule lies over the fat pad; it is not part of the medial retinaculum that covers it.
10-39).
Incision
The relaxed skin tension lines run roughly transversely across the knee joint. Therefore, the more transverse the incision, the more cosmetic the resulting scar. Longitudinal incisions, such as those that are used for the medial parapatellar approaches, often leave broad, obvious scars, which are distressing, especially in young women.
Superficial and Deep Surgical Dissections
The three-layer pattern offers a step-by-step approach to the medial exposure of the knee that is consistent with the anatomy.
1.
Medial exposure of the knee and its supporting structures
1. With anterior arthrotomy
1. The
outer layer_Fig. 10-35).
2. Retraction of the sartorius muscle posteriorly uncovers the two structures lying between the superficial and middle layers: The semitendinosus and gracilis muscles (see Fig. 10-36).
3. Retraction of all three muscles of the pes anserinus reveals the
_middle layer,the superficial medial ligament (see Fig. 10-36).
4. Vertical incision through the medial patellar retinaculum exposes the thin underlying capsule, the _deep layer_Fig. 10-36).
5. Fig. 10-34).
2. With posterior arthrotomy
1. Incision of the _outer layer_Fig. 10-37).





 Figure 10-33 The sartorius and the medial patellar retinaculum (outer layer) have been resected to reveal the superficial medial ligament of the middle layer. The true joint capsule (deep layer) also is exposed.
Figure 10-33 The sartorius and the medial patellar retinaculum (outer layer) have been resected to reveal the superficial medial ligament of the middle layer. The true joint capsule (deep layer) also is exposed.






 Figure 10-34 The joint cavity of the knee, with all the more superficial structures removed.
Figure 10-34 The joint cavity of the knee, with all the more superficial structures removed.





 Figure 10-35 The outer layer of the medial aspect of the knee joint consists of the sartorius, the fascia of the thigh, and the medial patellar retinaculum.
Figure 10-35 The outer layer of the medial aspect of the knee joint consists of the sartorius, the fascia of the thigh, and the medial patellar retinaculum.





 Figure 10-36 The outer layer has been resected to reveal the intermediate layer, consisting of the superficial medial ligament. Between the superficial and middle layers run the semitendinosus and gracilis muscles. The deep medial ligament (meniscofemoral ligament) of the deep layer is visible. The true joint capsule anterior to the superficial medial ligament also is visible.
Figure 10-36 The outer layer has been resected to reveal the intermediate layer, consisting of the superficial medial ligament. Between the superficial and middle layers run the semitendinosus and gracilis muscles. The deep medial ligament (meniscofemoral ligament) of the deep layer is visible. The true joint capsule anterior to the superficial medial ligament also is visible.




 Figure 10-37 A more posteromedial view of the knee joint. The sartorius, the deep fascia of the outer layer, the gracilis, the semitendinosus, and the semimembranosus have been resected to reveal the superficial medial ligament (middle layer), the posteromedial joint capsule (deep layer), and the medial head of the gastrocnemius.
Figure 10-37 A more posteromedial view of the knee joint. The sartorius, the deep fascia of the outer layer, the gracilis, the semitendinosus, and the semimembranosus have been resected to reveal the superficial medial ligament (middle layer), the posteromedial joint capsule (deep layer), and the medial head of the gastrocnemius.




 Figure 10-38 The medial head of the gastrocnemius has been resected to reveal the three expansions of the semimembranosus.
Figure 10-38 The medial head of the gastrocnemius has been resected to reveal the three expansions of the semimembranosus.





 Figure 10-39 The posterior aspect of the superficial medial ligament (middle layer) has been excised to reveal the true joint capsule and its thickening, the deep medial ligament (the meniscofemoral ligament and the coronary ligaments). The posteromedial joint capsule has been excised to reveal the corner of the joint. The insertion of the semimembranosus and a portion of its expansion are visible. 2. Further posterior retraction brings the posteromedial corner of the joint into view. The cover consists of fibrous tissue derived from the semimembranosus muscle (the
middle layer
), which has fused with the true joint capsule (the
deep layer;
see Fig. 10-38).
Figure 10-39 The posterior aspect of the superficial medial ligament (middle layer) has been excised to reveal the true joint capsule and its thickening, the deep medial ligament (the meniscofemoral ligament and the coronary ligaments). The posteromedial joint capsule has been excised to reveal the corner of the joint. The insertion of the semimembranosus and a portion of its expansion are visible. 2. Further posterior retraction brings the posteromedial corner of the joint into view. The cover consists of fibrous tissue derived from the semimembranosus muscle (the
middle layer
), which has fused with the true joint capsule (the
deep layer;
see Fig. 10-38).
3. Covering the medial side of the posterior joint capsule is the
medial head of the gastrocnemius muscle. This head can be reflected backward off the capsule to extend the exposure posteriorly (see Figs. 10-37 and 10-39).
4. Arthrotomy posterior to the superficial medial ligament consists of incising the deep and middle layers together, exposing the intra-articular structures in the posterior half of the joint (
2.
Approach for medial meniscectomy
1. Incising the medial patellar retinaculum exposes the true capsule of the joint, which is very thin at this point.
2. The true capsule of the joint, incised with the synovium, allows access to the anteromedial portion of the joint (see Figs. 10-33 and 10-34).
3.
Medial parapatellar approach to the knee
1. The joint is dissected through the same fascial layers as in the approach for the medial meniscus.
Special Anatomic Points
Three muscles, the sartorius, semitendinosus, and gracilis, insert into the upper part of the subcutaneous surface of the tibia. Each muscle has a different nerve supply: The sartorius is innervated by the femoral nerve, the semitendinosus by the sciatic nerve, and the gracilis by the obturator nerve. In addition, each muscle crosses both the hip and the knee.
The actions of the three muscles are duplicated by other, more powerful, muscles. At their pelvic origins, the three attach to three points on the bony pelvis that are separated as widely as the pelvis allows: The anterior-superior iliac spine (sartorius), the ischial tuberosity (semitendinosus), and the inferior pubic ramus (gracilis). With these origins and insertions, the muscles are arranged ideally to stabilize the pelvis on the leg.
The sartorius, semitendinosus, and gracilis insert into the subcutaneous surface of the tibia at a point called the
pes anserinus
(goose foot). Acting together, they not only flex the knee, but also internally rotate the tibia.


 Figure 10-40 Osteology of the posteromedial aspect of the knee joint. Approach for Lateral Meniscectomy
Figure 10-40 Osteology of the posteromedial aspect of the knee joint. Approach for Lateral Meniscectomy
A lateral meniscectomy can be performed through several types of incisions. Longitudinal and oblique incisions provide better access to other structures within the joint, whereas a transverse incision provides limited access to the knee, but excellent exposure of the meniscus itself. All incisions enter the lateral compartment of the knee anterior to the superficial lateral ligament.
Open surgical approaches for lateral meniscectomy are now confined to parts of the world where arthroscopic equipment is not available.
The approach is used for the following:
2. Removal of loose bodies
3. Removal of foreign bodies
4. Treatment of osteochondritis of the lateral femoral condyle
Position of the Patient
Two positions can be used. For both positions, exsanguinate the limb either by elevating it for 2 minutes or by applying a soft rubber bandage. Next, inflate a tourniquet.
Table-Bent Position
The table-bent position is identical to that used for medial meniscectomy. Two points are critical:
1. The sandbag must be placed under the thigh, not under the knee, to keep the popliteal artery and the posterior capsule from being compressed against the back of the femur and tibia.
2. Fig. 10-41).
Crossed Leg Position
10-42).

---
Figure 10-41 Position for the lateral approach to the knee.

 Figure 10-42 With the patient supine on the operating table, drop the end of the table so the knee can flex. The crossed leg position allows a direct approach to the lateral aspect of the knee.
Landmarks and Incision
#### Landmarks
Figure 10-42 With the patient supine on the operating table, drop the end of the table so the knee can flex. The crossed leg position allows a direct approach to the lateral aspect of the knee.
Landmarks and Incision
#### Landmarks
Palpate the smooth anterior border of the
lateral femoral condyle
as far as the joint line.
The
head of the fibula
is situated at about the same level as the tibial tubercle. From the lateral femoral epicondyle, move a thumb inferiorly and posteriorly across the joint line to find it.
Palpate the lateral border of the patella.
To find the
lateral joint line,
flex and extend the knee; palpate the area with a thumb to feel the movement of the femur and the tibia.
To palpate the
superficial lateral ligament
(
fibular collateral ligament,
lateral collateral ligament), cross the patient’s leg so that his or her ankle rests on the opposite knee. When the knee is flexed to 90 degrees and the hip is abducted and externally rotated, the iliotibial tract relaxes and makes the superficial lateral ligament easier to isolate. The ligament stands away from the joint itself, stretching from the fibular head to the lateral femoral condyle. It is easily palpable and usually visible.
Incision
Fig. 10-43B).
Deep Surgical Dissection
10-44; see Fig. 10-43C).


 Figure 10-43 A: Incision for the lateral approach to the knee. The incision should remain considerably anterior to the superficial lateral (fibular collateral) ligament. B: Incise the knee joint capsule in line with the skin incision. C: Incise the synovium and extrasynovial fat pad to enter the joint. Avoid damaging the underlying meniscus.
Figure 10-43 A: Incision for the lateral approach to the knee. The incision should remain considerably anterior to the superficial lateral (fibular collateral) ligament. B: Incise the knee joint capsule in line with the skin incision. C: Incise the synovium and extrasynovial fat pad to enter the joint. Avoid damaging the underlying meniscus.

 Figure 10-44 Expose the meniscus. Place retractors to allow maximum exposure of the joint. ### Dang
Figure 10-44 Expose the meniscus. Place retractors to allow maximum exposure of the joint. ### Dang
Vessels
The lateral inferior genicular artery runs around the upper part of the tibia. The artery lies next to the peripheral attachment of the lateral meniscus; it may be damaged if the meniscus is detached along with a portion of the capsule during meniscectomy, leading to massive postoperative hemarthrosis. It is not in danger during the approach (see Fig. 10-50).
Muscles and Ligaments
The
superficial lateral ligament
(fibular collateral ligament) limits posterior extension at the incision. If it is cut and not repaired, it may affect lateral stability. Its position may be estimated by a line drawn from
the head of the fibula to the lateral femoral condyle (see Fig. 10-50).
Special Problems
The lateral meniscus may be damaged if the synovium is incised too close to the joint line.
How to Enlarge the Approach
This particular approach restricts the view of the inside of the joint because of the relative immobility of the structures that are incised and the difficulty in retracting them. The exposure may be improved in three ways without extending the incision:
1.
Retraction. Retractors should be readjusted frequently to allow the best possible view.
2.
Position of the joint. An inward stress opens up the lateral side of the joint (one advantage of the crossed leg position), which automatically puts an inward stress on the knee. Flexion of the knee allows better access to the back of the lateral side of the joint. If the very back of the joint must be seen, however, the best view may be obtained by putting the knee into extension and applying distraction and inward force.
3.
Lights. The direction of the light should be adjusted frequently so that it shines into the depths of the wound. A headlamp can be used to advantage for lateral meniscectomy.
Extensile Measures
Posterior Extension. The incision cannot be extended posteriorly because of the presence of the superficial lateral ligament._Superior Extension.
To extend the incision superiorly, incise the skin and lateral patellar retinaculum along the lateral border of the patella, increasing access to the back of the patella. To widen the exposure still further, extend the incision superiorly and open the plane between the posterior border of the vastus lateralis muscle and the lateral intramuscular septum. Extending this approach into a posterolateral approach to the femur offers the theoretic possibility of extending the exposure as far as the greater trochanter (see Posterolateral Approach in Chapter 9). This extended exposure is very useful in the treatment of supracondylar fractures of the femur with intra-articular components.
Inferior Extension. To extend the incision inferiorly, incise the skin
vertically downward, staying lateral to the tibial tubercle and running vertically down the leg about 1 cm from the subcutaneous border of the tibia. Incise the lateral patellar retinaculum, then carefully detach part of the origin of the tibialis anterior muscle from the lateral border of the tibia. This will allow access to the upper third of the tibia and good visualization of the inside of the joint. This extension can be used for the internal fixation of lateral tibial plateau fractures although the anterolateral approach to the lateral tibial plateau is most commonly used for treatment of these pathologies (see pages 585-588). In these fractures, it is critically important to achieve good visualization of the articular surface of the lateral tibial condyle to allow anatomic reconstruction of this surface.
Lateral Approach to the Knee and Its Supporting Structures
The lateral approach provides access to all the supporting structures on the lateral side of the knee. It may be extended for intra-articular exploration of the knee’s anterior and posterior structures as well.
Normally, only part of the exposure is needed for any single surgical procedure. Its major use is in the assessment of ligamentous damage, a type of pathology that is more common on the medial side because valgus stress is more common than varus stress.
Position of the Patient
Place the patient supine on the operating table with a sandbag under the buttock of the affected side. This position rotates the leg medially to expose better the lateral aspect of the knee. Exsanguinate the limb either by elevating it for 3 to 5 minutes or by applying a soft rubber bandage then inflate a tourniquet (see Fig. 10-41). Flex the knee to 90 degrees.
Landmarks and Incision
#### Landmarks
Locate the lateral border of the patella and the lateral joint line.
Gerdy tubercle(the lateral tubercle of the tibia), a smooth, circular facet on the anterior surface of the lateral condyle of the tibia, marks the inferior attachment of the iliotibial band. Palpate it just lateral to the
patellar ligament.
Incision
10-45).
Internervous Plane
The dissection exploits the plane between the
iliotibial band
and the
biceps femoris_10-46).
Superficial Surgical Dissection
Mobilize the skin flaps widely. Underneath are two major structures: The iliotibial band, sweeping down to attach to the anterolateral border of the tibia and Gerdy tubercle, and the biceps femoris muscle, passing downward and forward to attach to the head of the fibula. Both these structures may be avulsed from their insertions during severe varus stress to the knee.
Incise the fascia in the interval between the iliotibial band and the biceps femoris muscle, avoiding the common peroneal nerve on the posterior border of the biceps tendon (posteriorly, uncovering the superficial lateral ligament (fibular collateral ligament) as it runs from the lateral epicondyle of the femur to the head of the fibula. The posterolateral corner of the knee capsule also is visible (](content://com.xodo.pdf.reader.pdftron.fileprovider/external_files/Download/Actions/Chapter%20Ten%20The%20Knee
)Fig. 10-48).
Deep Surgical Dissection
Enter the joint either in front of or behind the superficial lateral ligament (see Fig. 10-48).


 Figure 10-45 Incision for the lateral approach to the knee joint. The incision should be made with the knee flexed. #### Anterior Arthrotomy
Figure 10-45 Incision for the lateral approach to the knee joint. The incision should be made with the knee flexed. #### Anterior Arthrotomy
To inspect the entire lateral meniscus, incise the capsule in front of the ligament. Make a separate fascial incision to create a lateral parapatellar
Fig. 10-47).
Posterior Arthrotomy
To inspect the posterior horn of the lateral meniscus, find the lateral head of the gastrocnemius muscle at its origin at the back of the lateral condyle of the femur. Dissect between it and the posterolateral corner of the joint capsule. The lateral inferior genicular arteries are in this area; they must be ligated or coagulated.
Note that the popliteus muscle inserts into the femur by way of a tendon that lies inside the joint capsule; the posterolateral corner of the knee may be hidden by the popliteus and its tendon. In cases of trauma, the dissection in this area already may have been done.
10-48).





 Figure 10-46
Internervous plane between the
iliotibial band
(which is supplied by the superior gluteal nerve) and the
biceps femoris
(which is supplied by the sciatic nerve).
Figure 10-46
Internervous plane between the
iliotibial band
(which is supplied by the superior gluteal nerve) and the
biceps femoris
(which is supplied by the sciatic nerve).
Dang
Nerves
The
common peroneal nerve
is the structure most at risk during this approach. It lies on the posterior border of the biceps tendon and must be found early in the approach, as the supporting structures of the lateral side of the knee are being dissected; thereafter, it must be protected, because it is easy to damage. To safely identify the nerve begin your dissection well
proximal to any damage and trace it from a normal area into an abnormal one (Fig. 10-49).
Vessels
The lateral inferior genicular artery runs between the lateral head of the gastrocnemius muscle and the posterolateral capsule, and requires ligation for full exposure of that corner of the joint (Fig. 10-51). Because this vessel may cause a significant postoperative hematoma if it is not ligated adequately, it is advisable to remove the tourniquet before closing the incision to check that adequate hemostasis has been achieved.
Muscles and Ligaments
The
popliteus tendon
is at risk as it travels within the joint before it attaches to the posterior aspect of the meniscus and the femur. Take care when opening the posterior half of the knee joint capsule to avoid cutting the tendon (see Fig. 10-51).
Special Problems
The
lateral meniscus
or its
coronary ligament
may be incised accidentally if arthrotomy is performed too close to the joint line.

 Figure 10-47 Incise the fascia in the interval between the iliotibial band and the biceps femoris to uncover the superficial lateral (fibular collateral) ligament and the posterior joint complex. Make a separate fascial incision anteriorly to create a lateral parapatellar approach.
How to Enlarge the Approach
#### Local Measures
Figure 10-47 Incise the fascia in the interval between the iliotibial band and the biceps femoris to uncover the superficial lateral (fibular collateral) ligament and the posterior joint complex. Make a separate fascial incision anteriorly to create a lateral parapatellar approach.
How to Enlarge the Approach
#### Local Measures
The approach as described gives a complete view of the lateral structures of the knee and cannot be improved usefully.
Extensile Measures
The exposure cannot be extended usefully.



 Figure 10-48 Make an incision into the joint capsule anterior to the superficial lateral ligament for a standard anterolateral approach. To enter the posterior portion of the joint, retract the iliotibial band anteriorly and the biceps femoris posteriorly, revealing the superficial lateral ligament and the posterolateral aspect of the joint. Incise the joint capsule posterior to the ligament to reveal the contents of the joint. ## Applied Surgical Anatomy of the Lateral Side of the Knee
Overview
The supporting structures on the lateral side of the knee fall into three layers. Because the anatomy can be distorted in pathologic states, a clear
Figure 10-48 Make an incision into the joint capsule anterior to the superficial lateral ligament for a standard anterolateral approach. To enter the posterior portion of the joint, retract the iliotibial band anteriorly and the biceps femoris posteriorly, revealing the superficial lateral ligament and the posterolateral aspect of the joint. Incise the joint capsule posterior to the ligament to reveal the contents of the joint. ## Applied Surgical Anatomy of the Lateral Side of the Knee
Overview
The supporting structures on the lateral side of the knee fall into three layers. Because the anatomy can be distorted in pathologic states, a clear
19 are carried out.
Outer Layer
e and gluteus maximus muscles, is a thickening in the deep fascia of the thigh. Its fibers run longitudinally.



 Figure 10-49 A slightly anterolateral view of the outer layer of the knee. The lateral patellar retinaculum, the biceps femoris, and the iliotibial band constitute the outer layer. The
biceps femoris
muscle, a part of the outer layer, is enclosed by the deep fascia, as is the sartorius muscle on the medial side.
Figure 10-49 A slightly anterolateral view of the outer layer of the knee. The lateral patellar retinaculum, the biceps femoris, and the iliotibial band constitute the outer layer. The
biceps femoris
muscle, a part of the outer layer, is enclosed by the deep fascia, as is the sartorius muscle on the medial side.
The
lateral patellar retinaculum
is a tough structure derived largely from the fascia covering the vastus lateralis muscle.
Middle Layer
The superficial lateral ligament (fibular collateral ligament) runs from the lateral epicondyle of the femur to the head of the fibula. The lateral inferior genicular vessels run between the ligament and the joint capsule itself. Because the ligament is attached to the femoral condyle behind the axis of rotation, it is tight in extension. When the ligament is damaged, subsequent functional problems are minimized by the existence of other
Fig. 10-50).
This structure passes anterodistally from an attachment proximal and posterior to the lateral femoral epicondyle to the margin of the lateral tibial plateau, approximately midway between Gerdy tubercle and the head of the fibula. The ligament is superficial to the lateral (fibular) collateral ligament proximally, from which it is distinct, and separate from the capsule of the knee.





 Figure 10-50 The lateral patellar retinaculum, the iliotibial band, and the deep
fascia (outer layer) have been excised to reveal the superficial lateral ligament (middle layer) and the joint capsule (deep layer). Note that the lateral inferior genicular artery runs along the joint line between the middle and deep layers.
Figure 10-50 The lateral patellar retinaculum, the iliotibial band, and the deep
fascia (outer layer) have been excised to reveal the superficial lateral ligament (middle layer) and the joint capsule (deep layer). Note that the lateral inferior genicular artery runs along the joint line between the middle and deep layers.
Deep Layer
The deep layer consists of the true capsule of the knee joint, the fibrous tissue attached just above and below the articular surfaces of the knee. Two other structures run with the capsule:
1. The
popliteus
muscle originates from the popliteal surface of the tibia above the soleal line. Its tendon, which lies within the joint capsule, attaches to the lateral condyle of the femur and the posterior aspect of the lateral meniscus.
2. The _short lateral ligament_10-51).





 Figure 10-51 A true lateral view of the knee joint. The biceps femoris, iliotibial band, and vastus lateralis have been excised to reveal the deeper layers. The joint capsule has been excised anterior and posterior to the superficial lateral ligament (fibular collateral ligament) to expose the intra-articular structures, notably the popliteus tendon and the lateral meniscus. Landmarks and Incision Oblique or longitudinal skin incisions cross the relaxed skin tension lines almost perpendicularly and may result in broad scars.
Superficial and Deep Dissections
1.
Approach for lateral meniscectomy
Figure 10-51 A true lateral view of the knee joint. The biceps femoris, iliotibial band, and vastus lateralis have been excised to reveal the deeper layers. The joint capsule has been excised anterior and posterior to the superficial lateral ligament (fibular collateral ligament) to expose the intra-articular structures, notably the popliteus tendon and the lateral meniscus. Landmarks and Incision Oblique or longitudinal skin incisions cross the relaxed skin tension lines almost perpendicularly and may result in broad scars.
Superficial and Deep Dissections
1.
Approach for lateral meniscectomy
1. Incise the
superficial
and
deep layers,
cutting the lateral patellar retinaculum (see Fig. 10-50).
2. The true capsule of the joint is very thin at this point. Incise it with its synovium to gain access to the joint surface.
2.
Lateral exposure of the knee and its supporting structures
1. Open the
superficial layer
in the plane between the biceps femoris muscle and the iliotibial band (see Fig. 10-50).
2. Incise the joint either in front of or behind the superficial lateral ligament, the
middle layer
of the lateral side (see Fig. 10-51).
3. Incise the capsule of the joint (the
deep layer
) in front of or behind the superficial lateral ligament. Do not damage the tendon of the popliteus muscle, which lies between the outer border of the lateral meniscus and the capsule of the joint (see Fig. 10-51).
Posterior Approach to the Knee
322 is primarily a neurovascular approach. Orthopedically, it rarely is needed because the medial and lateral approaches each provide good access to half the posterior capsule. Reconstruction of fractures of the posterior column of the tibial plateau is best carried out through the posterior approach to the tibial plateau (see Chapter 11). Its uses include the following:
1. Repair of the neurovascular structures that run behind the knee in cases of trauma
2. Repair of avulsion fractures of the site of attachment of the posterior cruciate ligament to the tibia
3. Recession of gastrocnemius muscle heads in cases of contracture
4. Lengthening of hamstring tendons
5. Excision of Baker cyst and other popliteal cysts
6. Access to the posterior capsule of the knee
Position of the Patient
Fig. 10-52).
Landmarks and Incision
#### Landmarks
Palpate the two heads of the
gastrocnemius muscle
at their origin on the posterior femoral surface just above the medial and lateral condyles. They are not as easy to feel as the hamstring tendons just above them.
Palpate the
semimembranosus
and
semitendinosus muscles
on the medial border of the popliteal fossa. The semitendinosus feels round; the semimembranosus is deeper and remains muscular to its insertion.
Because this approach is rarely performed by orthopedic surgeons and is carried out in the prone position palpate the head of the fibula and draw the letter L (lateral) over it using a skin marker. This will aid many surgeons with orientation during the surgical dissection.
Incision
10-53).

--- Figure 10-52 Position of the patient on the operating table for the posterior approach to the knee.

!10-54; see Fig. 10-57).
10-55).



 Figure 10-54 Reflect the skin flaps. Identify the small saphenous vein as it passes upward in the midline of the calf. On the lateral side of the vein is the medial sural cutaneous nerve. Incise the fascia of the fossa just lateral to the small saphenous vein. The apex of the popliteal fossa is formed by the semimembranosus
Figure 10-54 Reflect the skin flaps. Identify the small saphenous vein as it passes upward in the midline of the calf. On the lateral side of the vein is the medial sural cutaneous nerve. Incise the fascia of the fossa just lateral to the small saphenous vein. The apex of the popliteal fossa is formed by the semimembranosus
10-56; see Fig. 10-59).
Now, turn to the popliteal artery and vein, which lie deep and medial to the tibial nerve (Fig. 10-57). The artery has five branches around the knee: Two superior, two inferior, and one middle genicular artery. One or more of these branches may have to be ligated if the artery needs to be mobilized (see Fig. 10-60).
The popliteal vein lies medial to the artery as it enters the popliteal fossa from below. Then it curves, lying directly posterior to the artery while in the fossa. Above the knee joint, it moves to the posterolateral side of the artery. Be very careful in mobilizing this structure. Intimal damage may cause thrombosis.


 Figure 10-55 Incise the fascia of the popliteal fossa. Trace the medial sural cutaneous nerve proximally, back to its source, the tibial nerve. Deep Surgical Dissection Retracting the muscles that form the boundaries of the popliteal fossa exposes various parts of the posterior joint capsule. There are two ways to gain greater access to the joint if this is necessary:
Figure 10-55 Incise the fascia of the popliteal fossa. Trace the medial sural cutaneous nerve proximally, back to its source, the tibial nerve. Deep Surgical Dissection Retracting the muscles that form the boundaries of the popliteal fossa exposes various parts of the posterior joint capsule. There are two ways to gain greater access to the joint if this is necessary:
1. Posteromedial joint capsule. Detach the tendinous origin of the medial head of the gastrocnemius muscle from the back of the femur. Retract
the head laterally and inferiorly, retracting the nerves and vessels out of the way to reach the posteromedial corner of the joint. The exposure now is the same as that achieved by posterior extension of the medial approach to the knee (Fig. 10-58; see Fig. 10-57).
2. 10-57 and 10-58).


 Figure 10-56 Dissect out the common peroneal nerve in a proximal to distal direction as it runs along the posterior border of the biceps femoris muscle.
Figure 10-56 Dissect out the common peroneal nerve in a proximal to distal direction as it runs along the posterior border of the biceps femoris muscle.
Note that the posterior approach is no better than the lateral and medial approaches in dealing with pathology of the posteromedial and posterolateral corners of the knee joint. It should be used mainly for exploring structures within the popliteal fossa and for reattaching the avulsed tibial insertion of the posterior cruciate ligament.
Dang
Nerves
The
medial sural cutaneous nerve,
which lies lateral to the
small saphenous vein,
may be damaged as it travels beneath the deep fascia of the calf. Incising the deep fascia of the calf
medial
to the vein, therefore, will preserve the nerve. Cutting the medial sural cutaneous nerve may produce a painful neuroma, but the resulting anesthesia usually is not significant (Fig. 10-59; see Fig. 10-54).
The
tibial nerve
may be damaged in the popliteal fossa. Damage to the nerve at this level produces paralysis of all the flexors of the toes and feet (Fig. 10-60; see Fig. 10-58).
The
common peroneal nerve
also is susceptible to damage in the popliteal fossa. Damage to the nerve at this level produces paralysis of the extensors and the evertors of the foot (see Figs. 10-58 and 10-59).




 Figure 10-57 The popliteal vein lies lateral to the artery as it enters the popliteal fossa from below. Then it curves, lying directly posterior to the artery while in the fossa. #### Vessels
Figure 10-57 The popliteal vein lies lateral to the artery as it enters the popliteal fossa from below. Then it curves, lying directly posterior to the artery while in the fossa. #### Vessels
The
small saphenous vein
may need to be ligated; this is an uncomplicated procedure.
The _popliteal vessels_Fig. 10-58).
How to Enlarge the Approach
#### Local Measures
The exposure described gives an adequate view of the contents of the popliteal fossa. Retracting the muscles of the fossa improves the view. To expose the knee capsule itself, detach one or both of the heads of the gastrocnemius muscle.
Extend the approach inferiorly to expose the trifurcation of the popliteal artery. At that point, the anterior tibial artery passes forward above the upper border of the interosseous membrane into the extensor compartment of the leg tethering the artery. It is a common site for arterial pathology in association with fractures in this area. This pattern makes it difficult to mobilize the artery; anastomoses in these areas are quite challenging.




 Figure 10-58 Retract the muscles that form the boundaries of the popliteal fossa, exposing the various parts of the posterior joint capsule. Detach the tendinous origin of the medial head of the gastrocnemius in the back of the femur to expose the posteromedial portion of the joint capsule. Detach the origin of the lateral head of the gastrocnemius from the lateral femoral condyle to expose the posterolateral corner of the joint capsule. ## Applied Surgical Anatomy of the
Posterior Approach to the Knee Overview
The anatomy of the posterior approach to the knee is the anatomy of the popliteal fossa.
Figure 10-58 Retract the muscles that form the boundaries of the popliteal fossa, exposing the various parts of the posterior joint capsule. Detach the tendinous origin of the medial head of the gastrocnemius in the back of the femur to expose the posteromedial portion of the joint capsule. Detach the origin of the lateral head of the gastrocnemius from the lateral femoral condyle to expose the posterolateral corner of the joint capsule. ## Applied Surgical Anatomy of the
Posterior Approach to the Knee Overview
The anatomy of the posterior approach to the knee is the anatomy of the popliteal fossa.
The popliteal fossa is diamond shaped in cadavers. In live patients, the lower “V” of the diamond (the gap between the two heads of the gastrocnemius muscle) is nonexistent until the heads are retracted from one another.
The fossa is bounded on its superior border by the semimembranosus and semitendinosus muscles medially and by the biceps femoris muscle laterally. Its inferior boundaries are the two heads of the gastrocnemius muscle. The roof of the fossa is the popliteal fascia, which is formed by the outer layer of the knee’s supporting structures. The floor is the posterior aspect of the distal end of the femur, the posterior capsule of the joint, and the popliteus muscle, which overlies the proximal tibia (see Fig. 10-59).
Incision
The lines of cleavage in the skin run almost transversely across the back of the knee joint. The curved incision described, therefore, has a variable relation to these lines. The resultant scar usually is cosmetically acceptable.
The incision crosses a major flexor crease at the back of the knee, but because the incision is almost parallel to the skin crease at this level, a flexion contracture of the knee does not occur when the wound heals.
Superficial Surgical Dissection
Superficial surgical dissection involves incising the roof of the popliteal fossa, using the small (short) saphenous vein and the medial sural cutaneous nerve of the calf as guides.
The
roof
of the popliteal fossa consists of the popliteal fascia, a continuation of the deep fascia of the thigh, and part of the outer layer of the knee. Two key structures pierce it to form the basis for the dissection of the fossa itself:
1. The
small (short) saphenous vein
arises in the foot and runs behind the lateral malleolus into the back of the calf. It travels roughly along the
midline of the calf and penetrates the popliteal fascia before joining the popliteal vein.
2. The
medial sural cutaneous nerve
also runs in the midline of the calf beneath the deep fascia, just lateral to the small saphenous vein. This nerve, which is a branch of the tibial nerve, supplies varying amounts of skin on the back of the calf.
Fig. 10-59).
The
tibial nerve,
a continuation of the sciatic nerve, is lateral to the popliteal artery as it enters the popliteal fossa. Then, at the midpoint of the fossa, it crosses the artery and lies medial to it as they leave the fossa together. The tibial nerve passes vertically downward in the fossa, giving branches to the plantaris, gastrocnemius, soleus, and popliteus muscles. Its sole cutaneous branch, the sural nerve, is of surgical interest in nerve grafting. The tibial nerve leaves the fossa between the two heads of the gastrocnemius muscle. Tibial nerve palsy affects the plantar flexors of the toes and ankle (see Fig. 10-60).
The
common peroneal nerve
slopes downward across the fossa, running laterally toward the medial side of the tendon of the biceps muscle. It disappears into the peroneus longus muscle, usually under a fibrous arch, where it may be entrapped before it winds around the fibula. Because patients naturally lie with their legs externally rotated, the head of the fibula often is in contact with the bed and compression palsy of the nerve can occur. For this reason, it is critically important to pad the head of the fibula when the patient is placed on the operating table in such a position that the head of this bone may come in contact with the operating table surface. Its division into deep and superficial peroneal nerves occurs within the substance of the peroneus longus muscle. Common peroneal nerve palsy affects all the extensors and evertors of the foot (see
The vascular structures lie more deeply in the fossa. The popliteal artery runs obliquely through the fossa after entering on the medial side of the femur. It lies directly behind the posterior capsule of the knee joint, dividing into its terminal branches, the posterior tibial, anterior tibial, and peroneal arteries, behind the gastrocnemius muscle. In the fossa, it gives off five branches.
The
two superior genicular arteries
encircle the lower end of the femur. The lateral artery requires ligation in the posterolateral approach to the knee. The medial artery requires ligation if the medial head of the
gastrocnemius muscle has to be detached from the femur to expose the posteromedial corner of the knee.
The
middle genicular artery
passes forward in the knee and supplies the cruciate ligaments. Traumatic rupture of the cruciate ligaments, therefore, is associated with brisk intra-articular bleeding that usually manifests as an immediate posttraumatic effusion. The artery holds its parent trunk firmly to the posterior capsule of the joint. For this reason, it can be damaged easily in dislocations of the knee during trauma or surgery. It also may be damaged as the posterior structures in the knee are dissected out from medial or lateral approaches. To avoid endangering the artery, flex the knee to allow the joint capsule to fall away from the back of the femur and tibia.
The _two inferior genicular arteries_10-60).






 Figure 10-59 View of the superficial structures of the knee. Note the centrally located small (short) saphenous vein and medial sural cutaneous nerve.
Figure 10-59 View of the superficial structures of the knee. Note the centrally located small (short) saphenous vein and medial sural cutaneous nerve.






 Figure 10-60 The gastrocnemius and the plantaris have been resected to reveal the neurovascular bundle in the popliteal fossa. The
popliteal vein
lies between the popliteal artery and the tibial nerve. The small saphenous vein pierces the popliteal fascia to enter the popliteal vein within the fossa.
Deep Surgical Dissection and Its Dangers
Deep surgical dissection consists of retracting and, sometimes, mobilizing the boundaries of the popliteal fossa. These boundaries are formed by the semimembranosus and semitendinosus muscles superomedially, by the biceps femoris muscle superolaterally, by the medial head of the gastrocnemius muscle inferomedially, and by the lateral head of the gastrocnemius muscle inferolaterally (see Fig. 10-60). For more information on these muscles, see Applied Surgical Anatomy of the Thigh in Chapter 9 and Posterolateral Approach to the Tibia in Chapter 11.
Figure 10-60 The gastrocnemius and the plantaris have been resected to reveal the neurovascular bundle in the popliteal fossa. The
popliteal vein
lies between the popliteal artery and the tibial nerve. The small saphenous vein pierces the popliteal fascia to enter the popliteal vein within the fossa.
Deep Surgical Dissection and Its Dangers
Deep surgical dissection consists of retracting and, sometimes, mobilizing the boundaries of the popliteal fossa. These boundaries are formed by the semimembranosus and semitendinosus muscles superomedially, by the biceps femoris muscle superolaterally, by the medial head of the gastrocnemius muscle inferomedially, and by the lateral head of the gastrocnemius muscle inferolaterally (see Fig. 10-60). For more information on these muscles, see Applied Surgical Anatomy of the Thigh in Chapter 9 and Posterolateral Approach to the Tibia in Chapter 11.
The floor of the popliteal fossa is formed by the _popliteus,_10-61 10-62).





 Figure 10-61 The medial and lateral hamstrings and the neurovascular bundle have been resected to reveal the posterior joint capsule of the knee. Note the three expansions of the semimembranosus sheath.
Figure 10-61 The medial and lateral hamstrings and the neurovascular bundle have been resected to reveal the posterior joint capsule of the knee. Note the three expansions of the semimembranosus sheath.



 Figure 10-62 The posterior joint capsule of the knee has been resected to reveal the intra-articular structures of the posterior aspect of the knee, most notably the posterior cruciate ligament and the popliteus.
Popliteus.
Origin. Popliteal surface of tibia above soleal line. Insertion. Lateral epicondyle of femur and posterior aspect of lateral meniscus. Action. Rotates femur laterally on tibia. Nerve supply. Tibial nerve.
Figure 10-62 The posterior joint capsule of the knee has been resected to reveal the intra-articular structures of the posterior aspect of the knee, most notably the posterior cruciate ligament and the popliteus.
Popliteus.
Origin. Popliteal surface of tibia above soleal line. Insertion. Lateral epicondyle of femur and posterior aspect of lateral meniscus. Action. Rotates femur laterally on tibia. Nerve supply. Tibial nerve.
The popliteus muscle unlocks the knee from its fully extended (screw home) position. It also draws the lateral femoral condyle backward on the tibia and pulls the lateral meniscus back, preventing it from being trapped between the tibia and femur. The convex rounded posterior aspect of the lateral tibial plateau allows this movement to take place.
Lateral Approach to the Distal Femur for Anterior Cruciate Ligament Surgery
The lateral approach to the distal femur, known as the “over-the-top” approach, is used in conjunction with the medial parapatellar approach for repair or reconstruction of the anterior cruciate ligament (see the section regarding the medial parapatellar approach). Therefore, it is not used as an isolated incision. The approach exposes the posterior aspect of the
intercondylar notch by passing over the top of the posterior aspect of the lateral femoral condyle.
The lateral approach to the distal femur also provides access to the lateral aspect of the lateral femoral condyle so that drill holes can be made in the condyle (if they are needed) for reattachment of the femoral end of the anterior cruciate ligament or attachment of the femoral end of an anterior cruciate substitute.
Position of the Patient
10-63).
Landmarks and Incision
#### Landmarks
Palpate the posterior lateral margin of the
lateral femoral condyle
as it flares out from the shaft of the femur.
Note the intersection between the
iliotibial band
and the
biceps femoris
muscle.
Incision
Fig. 10-64).

--- Figure 10-63 Position for the lateral approach to the distal femur. Internervous Plane The dissection exploits the internervous plane between the _vastus lateralis_muscle(which is supplied by the femoral nerve) and the biceps femoris muscle Fig. 10-65).
Deep Surgical Dissection
10-66 10-6710-6810-69).

 Figure 10-64 Make an incision 10 cm long parallel to and over the indentation between the biceps femoris and the iliotibial band.
Figure 10-64 Make an incision 10 cm long parallel to and over the indentation between the biceps femoris and the iliotibial band.

 Figure 10-65 Incise the iliotibial band just anterior to the lateral intermuscular septum, in line with the skin incision. ### Dang
Figure 10-65 Incise the iliotibial band just anterior to the lateral intermuscular septum, in line with the skin incision. ### Dang
Nerves and Vessels
The
peroneal nerve
may be injured if the dissection strays to the posterior side of the biceps femoris muscle.
The
lateral superior genicular artery
must be ligated. Otherwise, it can cause a large postoperative hematoma.
The
popliteal artery
may be injured if the surgical plane does not remain subperiosteal. As the intercondylar notch is felt, bend the knee to 90 degrees to allow the popliteal artery to fall posteriorly with the joint capsule.
How to Enlarge the Approach
#### Local Measures
Retract the vastus lateralis muscle vigorously toward the midline of the knee with a right-angled retractor.
Extensile Measures
This incision is very extensile. It can be extended as far proximally and distally as it has to be (see Lateral Approach in Chapter 9, see Fig. 9-14). In addition, the incision can be used in its more proximal extensions for an iliotibial-fascial graft.


 Figure 10-66 The vastus lateralis anterior to the intermuscular septum is retracted anteriorly and medially. Identify the lateral superior genicular artery.
Figure 10-66 The vastus lateralis anterior to the intermuscular septum is retracted anteriorly and medially. Identify the lateral superior genicular artery.

 Figure 10-67 Retract the muscles further, ligate the lateral superior genicular artery, and incise the periosteum at the junction of the shaft and the flare of the femur.
Figure 10-67 Retract the muscles further, ligate the lateral superior genicular artery, and incise the periosteum at the junction of the shaft and the flare of the femur.

 Figure 10-68A: Pass a small instrument behind the posterolateral flare of the lateral femoral condyle deep to the periosteum. B: Continue passing the instrument distally and medially over the top of the lateral femoral condyle until it can be felt entering the intercondylar notch.
Figure 10-68A: Pass a small instrument behind the posterolateral flare of the lateral femoral condyle deep to the periosteum. B: Continue passing the instrument distally and medially over the top of the lateral femoral condyle until it can be felt entering the intercondylar notch.

 Figure 10-69 Advance the tip of the instrument anteriorly until it is visible in the knee as viewed from the anteromedial incision.
Figure 10-69 Advance the tip of the instrument anteriorly until it is visible in the knee as viewed from the anteromedial incision.
Scientific References
- 1. SCOTT WN, INSALL JN, KELLY MA: Arthroscopy and meniscectomy; surgical approaches, anatomy and techniques. In: Insall JN, Windsor RE, Scott WN, Kelly MA, Aglietti P, eds. _Surgery of the Knee_. Vol. 1. 2nd ed. New York, NY: Churchill Livingstone; 1993:165–215.
- 2. INSALL JN, ed: _Surgery of the Knee_. 2nd ed. New York, NY: Churchill Livingstone; 1993.
- 3. ABBOTT LC, CARPENTER WF: Surgical approaches to the knee joint. _J Bone Joint Surg._ 1945;27:277–310.
- 4. COVERNTRY MB, UPSHAW JE, RILEY LH, ET AL: Geometric total knee arthroplasty, 1: conception, design, indications, and surgical technic. _Clin Orthop Relat Res._ 1973;94:171–184.
- 5. FREEMAN MA: Total replacement of the knee. _Orthop Rev._ 1974;3:21.
- 6. FREEMAN MA, TODD RC, BAMERT P, ET AL: ICLH arthroplasty of the knee, 1968–1977. _J Bone Joint Surg Br._ 1978;60:339.
- 7. GUNSTON FH, MACKENZIE RI: Complications of polycentric knee arthroplasty. _J Bone Joint Surg Br._ 1977;59:506.
- 8. HABERMAN ET, DEUTSCH SD, ROVERE GD: Knee arthroplasty with the use of the Walldius total knee prosthesis. _Clin Orthop Relat Res._ 1973;94:72–84.
- 9. INSALL IN, SCOTT WN, RANAWAT CS: The total condylar knee: a report of 220 cases. _J Bone Joint Surg Am._ 1979;61:173.
- 10. LAKSIN RS: Modular total knee replacement arthroplasty: a review of 89 patients. _J Bone Joint Surg Am._ 1978;58:766–773.
- 11. SHEEHAN JM: Arthroplasty of the knee. _J Bone Joint Surg Br._ 1978;60:333–338.
- 12. CONATY JP: Surgery of the hip and knee in patients with rheumatoid arthritis. _J Bone Joint Surg Am._ 1973;55:301–314.
- 13. MCMASTER M: Synovectomy of the knee in juvenile rheumatoid arthritis. _J Bone Joint Surg Br._ 1972;54:263–271.
- 14. SMILLIE IS: _Injuries of the Knee Joint_. 4th ed. Baltimore, MD: Williams & Wilkins; 1971.
- 15. AICHROTH P: Osteochondritis dissecans of the knee: a clinical survey. _J Bone Joint Surg Br._ 1971;53:440–447.
- 16. HUGHSTON JC: A surgical approach to the medial and posterior ligaments of the knee. _J Bone Joint Surg Am._ 1973;55:29–33.
- 17. WARREN LF, MARSHALL JL: The supporting structure and layers on the medial side of the knee. _J Bone Joint Surg Am_. 1979;61:56–62.
- 18. POGRUND H: A practical approach for lateral meniscectomy. _J Trauma._ 1976;16:365–367.
- 19. KAPLAN EB: Surgical approach to the lateral [peroneal] side of the knee joint. _Surg Gynecol Obstet_. 1957;104:346–356.
- 20. SLOCUM DB, JAMES SL, LARSEN RL, ET AL: Late reconstruction of ligament injuries to the medial compartment of the knee. _Clin Orthop Relat Res_. 1976;118:63.
- 21. DODDS AL, HALEWOOD C, GUPTE CM, ET AL: The anterolateral ligament: anatomy, length changes and association with the Segond fracture. _Bone Joint J Br._ 2014;96(3):325–331.
- 22. BRACKETT EG, OSGOOD RB: The popliteal incision for the removal of “joint mick” in the posterior capsule of the knee joint: a report of cases. _Boston J Med Surg._ 1911;165:975–976. #
Academic Citations & Sources
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding approaches-to-the-knee

