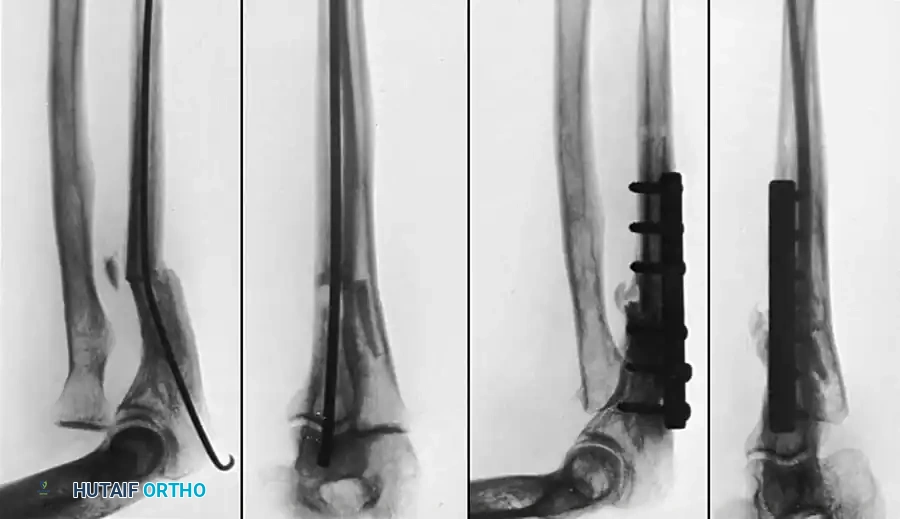
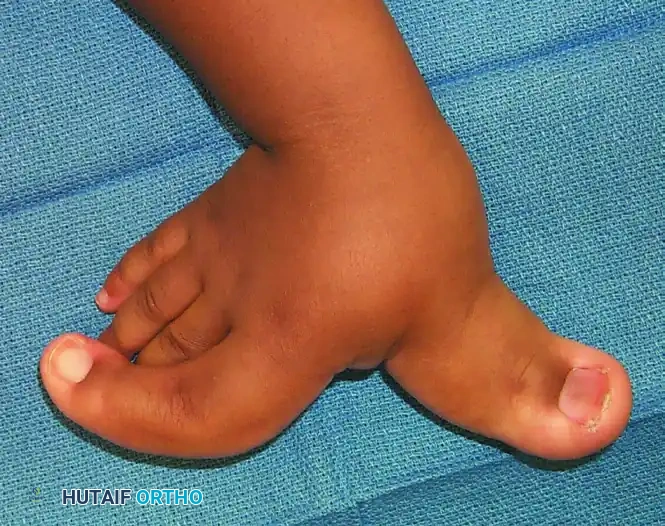
Operative Management of Pronation Contracture of the Forearm
Key Takeaway
Pronation contracture of the forearm is a disabling deformity frequently encountered in spastic cerebral palsy, primarily driven by spasticity of the pronator teres and pronator quadratus. Surgical intervention is guided by the Gschwind classification, balancing active and passive supination deficits. Procedures range from simple pronator teres tenotomy to complex rerouting transfers. Careful preoperative assessment is critical to prevent devastating iatrogenic supination deformities.
INTRODUCTION AND CLINICAL SIGNIFICANCE
Pronation deformity of the forearm is one of the most common and functionally disabling upper extremity contractures encountered in children and adults with spastic cerebral palsy. The classic hemiplegic upper extremity posture consists of shoulder internal rotation, elbow flexion, forearm pronation, wrist flexion, and thumb-in-palm deformity. Among these, the pronation contracture severely limits the patient's ability to position the hand in space, accept objects, perform two-handed activities, and manage personal hygiene or feeding.
The primary pathoanatomic drivers of this deformity are spasticity and subsequent myostatic contracture of the pronator teres (PT) and, frequently, the pronator quadratus (PQ). Over time, dynamic spasticity transitions into fixed fibrotic contracture, altering the biomechanics of the forearm axis and potentially leading to secondary skeletal changes, such as radial head subluxation or bowing of the radius.
CLINICAL PEARL:
A pronation contracture can be unmasked or aggravated by the surgical lengthening of the biceps tendon when addressing a concurrent elbow flexion contracture. The biceps brachii is a powerful supinator; weakening it through lengthening diminishes the primary antagonist to the spastic pronator group, thereby exacerbating the pronation deformity.
PATHOANATOMY AND BIOMECHANICS
The forearm rotates around a longitudinal axis extending from the center of the radial head to the fovea of the distal ulna. Normal pronation is achieved through the synergistic action of the pronator teres (median nerve) and the pronator quadratus (anterior interosseous nerve).
In the spastic upper extremity, the delicate balance between the pronators and supinators (biceps brachii and supinator muscle) is disrupted. The pronator teres, being a larger, biarticular muscle, is typically the primary deforming force. It often fires out of phase during attempted supination, acting as an active tether.
Furthermore, a pronation contracture may be aggravated by a contracted bicipital aponeurosis (lacertus fibrosus). This fascial band, which extends from the biceps tendon across the flexor mass, can become fibrotic and contracted in chronic elbow flexion and pronation deformities. Division of this structure alone can sometimes yield a measurable improvement in passive supination.
PREOPERATIVE EVALUATION
A meticulous clinical examination is paramount to differentiate between dynamic spasticity and fixed myostatic contracture.
Clinical Assessment Parameters
- Active Range of Motion (AROM): Assess the patient's ability to actively supinate the forearm. This must be tested with the elbow flexed to 90 degrees to eliminate shoulder rotation substitution.
- Passive Range of Motion (PROM): Determine the absolute limits of supination. A discrepancy between active and passive supination indicates dynamic spasticity or weakness of the supinators, whereas a lack of passive supination indicates a fixed contracture of the PT, PQ, or interosseous membrane.
- Phase of Firing: Dynamic electromyography (EMG) or careful palpation during active movement can determine if the pronator teres is firing out of phase (i.e., contracting during attempted supination).
SURGICAL WARNING:
Overcorrection resulting in a supination contracture is a devastating and highly disabling complication. A supinated hand is functionally useless for keyboard use, writing, and most activities of daily living. Surgical planning must be conservative, aiming for a functional arc of motion rather than absolute anatomical neutrality.
THE GSCHWIND CLASSIFICATION SYSTEM
Surgical decision-making is heavily reliant on the Gschwind Classification of Pronation Deformities. This system categorizes the deformity based on the presence and degree of active and passive supination, providing a direct algorithmic guide to surgical intervention.
Group 1: Active Supination Beyond Neutral
- Clinical Presentation: The patient maintains the ability to actively supinate the forearm past the neutral (zero-degree) position, despite a resting pronated posture.
- Surgical Recommendation: No specific surgery is indicated for the pronation deformity. Therapy and orthotic management are sufficient.
Group 2: Active Supination To or Less Than Neutral
- Clinical Presentation: The patient can actively supinate, but cannot move past the neutral position. Passive supination is generally preserved.
- Surgical Recommendation: Pronator quadratus release, with or without a flexor aponeurotic release. The PT is spared to prevent overcorrection, as the patient still possesses some active supinator function.
Group 3: No Active Supination, Free Passive Supination
- Clinical Presentation: The patient has completely lost active supination, but the examiner can passively supinate the forearm without significant resistance. This indicates severe dynamic spasticity or complete weakness of the supinators without fixed fibrotic contracture.
- Surgical Recommendation: Pronator teres rerouting procedure. This transfer converts the spastic PT from a deforming pronator into an active supinator, restoring the lost active motion while eliminating the dynamic tether.
Group 4: No Active Supination and Limited Passive Supination
- Clinical Presentation: The most severe category. The patient has neither active nor passive supination, indicating profound fixed contracture of the pronator musculature and potentially the interosseous membrane.
- Surgical Recommendation: Pronator quadratus release combined with a flexor aponeurotic release.
- Staged Approach: If, after these releases, no active supination is possible intraoperatively or postoperatively, a pronator teres rerouting may be added. However, Gschwind et al. strongly caution against performing a PT transfer at the same time as a PQ release, as an undesirable and irreversible supination deformity may ensue.
SURGICAL TECHNIQUES
1. Pronator Teres Tenotomy (Simple Release)
A simple pronator teres tenotomy is ideal for patients who lack supination just short of neutral, and in whom the pronator is contracted and fires out of phase with supination.
Operative Steps:
1. Incision: A 4- to 5-cm longitudinal incision is made over the middle third of the radial aspect of the volar forearm.
2. Dissection: The interval between the brachioradialis (retracted radially) and the flexor carpi radialis (retracted ulnarly) is developed.
3. Nerve Protection: The superficial branch of the radial nerve lies deep to the brachioradialis and must be identified and protected.
4. Identification of PT: The broad, flat tendinous insertion of the pronator teres is identified as it wraps around the lateral convexity of the radius.
5. Tenotomy: The tendon is sharply divided at its insertion. For a more controlled release, a Z-lengthening or step-cut lengthening can be performed, though a simple tenotomy is highly effective and standard for out-of-phase spasticity.
6. Closure: The wound is irrigated and closed in layers.
2. Pronator Teres Rerouting Procedure
Indicated primarily for Gschwind Group 3 deformities, this procedure aims to convert the PT into a supinator.
Operative Steps:
1. Exposure: The approach is identical to the simple tenotomy, utilizing the interval between the brachioradialis and FCR.
2. Mobilization: The PT tendon is identified. To gain maximum length, the tendon is detached from the radius along with a contiguous strip of periosteum.
3. Rerouting: The muscle belly is mobilized proximally to the level of the median nerve branches (which must be meticulously protected). The tendon is then passed dorsally around the radius (from volar to dorsal) through the interosseous space or simply around the radial border, depending on the specific technique variation.
4. Reattachment: The tendon is passed back to the volar side and sutured to itself, or anchored into the radius via drill holes or suture anchors, with the forearm held in maximum supination.
5. Tensioning: The transfer is tensioned to hold the forearm in approximately 45 degrees of supination.
3. Pronator Quadratus Release
Indicated for Gschwind Group 2 and Group 4 deformities.
Operative Steps:
1. Incision: A distal volar longitudinal incision is made (distal Henry approach).
2. Dissection: The flexor tendons and the median nerve are retracted ulnarly. The radial artery is protected and retracted radially.
3. Release: The transverse fibers of the pronator quadratus are identified on the distal volar radius. The muscle is sharply elevated off the radius from radial to ulnar.
4. Hemostasis: The anterior interosseous artery and its branches lie deep to the PQ and must be carefully cauterized to prevent postoperative hematoma.
4. Flexor Carpi Ulnaris (FCU) Transfer for Supination
Supination can also be improved by the transfer of the flexor carpi ulnaris around the ulnar side of the forearm. This is typically performed during the augmentation of the extensor digitorum communis (EDC) or the extensor carpi radialis brevis (ECRB) for concurrent wrist/finger flexion deformities.
Operative Steps:
1. Harvest: The FCU is detached from its insertion on the pisiform.
2. Mobilization: The muscle is mobilized proximally, protecting the ulnar nerve and artery.
3. Routing: The tendon is routed subcutaneously around the ulnar border of the forearm to the dorsal aspect.
4. Attachment: It is woven into the EDC or ECRB tendons. The vector of this transfer provides a secondary supinating force to the forearm.
PITFALL:
Overcorrection with a supination contracture is a high-risk complication if an FCU transfer (routed for supination) is combined with a pronator teres release or transfer. These procedures should rarely be performed simultaneously.
5. Division of the Bicipital Aponeurosis
As an adjunctive procedure, division of a contracted bicipital aponeurosis (lacertus fibrosus) can yield immediate improvements in supination.
1. Incision: A transverse or curvilinear incision is made across the antecubital fossa.
2. Identification: The superficial veins and medial antebrachial cutaneous nerve are protected. The taut band of the aponeurosis is identified extending medially from the biceps tendon.
3. Division: The aponeurosis is sharply divided. Care must be taken to protect the underlying brachial artery and median nerve, which lie immediately deep to this structure.
POSTOPERATIVE MANAGEMENT
The success of forearm rebalancing procedures relies heavily on rigorous postoperative immobilization and subsequent rehabilitation.
- Immobilization: Immediately postoperatively, the upper extremity is immobilized in a long-arm cast. The elbow is flexed to 90 degrees, and the forearm is positioned in 45 to 60 degrees of supination (or maximum achieved supination if less than 45 degrees).
- Duration: The cast is maintained for 4 to 6 weeks to allow for tendon healing (in the case of rerouting or transfer) or to allow the released tissues to heal in an elongated position.
- Orthotic Transition: Following cast removal, a custom thermoplastic long-arm splint is fabricated. This is worn full-time for an additional 2 to 4 weeks, then transitioned to a nighttime-only wearing schedule for 6 to 12 months to prevent recurrence of the contracture.
- Rehabilitation: Intensive occupational therapy is initiated immediately upon cast removal. Therapy focuses on active supination exercises, bimanual activities, and integration of the newly positioned hand into activities of daily living.
COMPLICATIONS
- Supination Deformity (Overcorrection): The most dreaded complication. Caused by over-releasing the pronators (e.g., simultaneous PT rerouting and PQ release) or combining releases with supinating transfers (e.g., FCU transfer). Treatment is exceedingly difficult and may require supinator release or reverse transfers.
- Recurrence (Undercorrection): Common in growing children or those with severe, unmanaged spasticity. Often requires revision surgery or serial casting.
- Nerve Injury: The superficial radial nerve (during PT release), median nerve (during PT rerouting), and anterior interosseous nerve (during PQ release) are all at risk. Meticulous surgical technique and anatomical knowledge are mandatory.
- Hematoma: Particularly common after PQ release due to the vascularity of the anterior interosseous system. Adequate hemostasis and potentially a drain are recommended.
📚 Medical References
- pronation contractures of the forearm in cerebral palsy by changing the insertion of the pronator radii teres, J Bone Joint Surg 63A:645, 1981.
- Sakellarides HT, Mital MA, Matza RA: The surgical treatment of the different types of “thumb-in-palm” deformities seen in cerebral palsy, Orthop Trans 4:9, 1980 (abstract). Samilson RL, Morris JM: Surgical improvement of the cerebralpalsied upper limb: electromyographic studies and results of 128 operations, J Bone Joint Surg 46A:1203, 1964.
- Skoff H, Woodbury DF: Current concepts review: management of the upper extremity in cerebral palsy, J Bone Joint Surg 67A:500, 1985.
- [Tachdjian MO: Affections of brain and spinal cord. In Pediatric orthopaedics, Philadelphia, 1972, Saunders.
Postnatal Cerebral Palsy Browne AO, McManus F: One-session surgery for bilateral correction of lower limb deformities in spastic diplegia, J Pediatr Orthop 7:259, 1987.](https://pubmed.ncbi.nlm.nih.gov/?term=Tachdjian%20MO%3A%20Affections%20of%20brain%20and%20spinal%20cord.%20In%20Pediatric%20orthopaedics%2C%20Philadelphia%2C%201972%2C%20Saunders.%0A%0APostnatal%20Cerebral%20Palsy%20Browne%20AO%2C%20McManus%20F%3A%20One-session%20surgery%20for%20bilateral%20correction%20of%20lower%20limb%20deformities%20in%20spastic%20diplegia%2C%20J%20Pediatr%20Orthop%207%3A259%2C%201987.)
- Dwyer FC: The treatment of relapsed club foot by the insertion of a wedge into the calcaneum, J Bone Joint Surg 45B:67, 1963.
- Jones ET, Knapp DR: Assessment and management of the lower extremity in cerebral palsy, Orthop Clin North Am 18:725, 1987.
- Lindsey RW, Drennan JC: Management of foot and knee deformities in the mentally retarded, Orthop Clin North Am 12:107, 1981.
- Norlin R, Tkaczuk H: One-session surgery for correction of lower extremity deformities in children with cerebral palsy, J Pediatr Orthop 5:208, 1985.
- Perry J, Hoffer MM, Antonelli D, et al: Electromyography before and after surgery for hip deformity in children with cerebral palsy: a comparison of clinical and electromyographic fi ndings, J Bone Joint Surg 58A:201, 1976.
- Samilson RL: Current concepts of surgical management of deformities of the lower extremities in cerebral palsy, Clin Orthop Relat Res 138:99, 1982.
- Samilson RL, Dillin L: Postural impositions on the foot and ankle from trunk, pelvis, hip, and knee in cerebral palsy, Foot Ankle 4:120, 1983.
- [Tachdjian MO: Affections of brain and spinal cord. In Pediatric orthopaedics, Philadelphia, 1972, Saunders.
Adults with Cerebral Palsy Andersson C, Mattsson E: Adults with cerebral palsy: a survey describing problems, needs, and resources, with special emphasis on locomotion, Dev Med Child Neurol 43:76, 2001.](https://pubmed.ncbi.nlm.nih.gov/?term=Tachdjian%20MO%3A%20Affections%20of%20brain%20and%20spinal%20cord.%20In%20Pediatric%20orthopaedics%2C%20Philadelphia%2C%201972%2C%20Saunders.%0A%0AAdults%20with%20Cerebral%20Palsy%20Andersson%20C%2C%20Mattsson%20E%3A%20Adults%20with%20cerebral%20palsy%3A%20a%20survey%20describing%20problems%2C%20needs%2C%20and%20resources%2C%20with%20special%20emphasis%20on%20locomotion%2C%20Dev%20Med%20Child%20Neurol%2043%3A76%2C%202001.)
- Ando N, Ueda S: Functional deterioration in adults with cerebral palsy, Clin Rehabil 14:300, 2000.
- Bottos M, Feliciangeli A, Sciuto L, et al: Functional status of adults with cerebral palsy and implications for treatment of children, Dev Med Child Neurol 43:516, 2001.
- Gallien P, Nicolas B, Petrilli S, et al: Role for botulinum toxin in back pain treatment in adults with cerebral palsy: report of a case, Joint Bone Spine 71:76, 2004.
- Hemming K, Hutton JL, Pharoah PO: Long-term survival for a cohort of adults with cerebral palsy, Dev Med Child Neurol 48:90, 2006.
- Jahsen R, Villien L, Aamodt G, et al: Musculoskeletal pain in adults with cerebral palsy compared with the general population, J Rehabil Med 36:78, 2004.
- Michelsen SI, Uldall P, Hansen T, Madsen M: Social integration of adults with cerebral palsy, Dev Med Child Neurol 48:643, 2006.
- Murphy KP, Molnar GE, Lankasky K: Employment and social issues in adults with cerebral palsy, Arch Phys Med Rehabil 81:807, 2000.
- Nagoya S, Nagao M, Takada J, et al: Long-term results of rotational acetabular osteotomy for dysplasia of the hip in adult ambulatory patients with cerebral palsy, J Bone Joint Surg 87B:1627, 2005.
- Noonan KJ, Jones J, Pierson J, et al: Hip function in adults with severe cerebral palsy, J Bone Joint Surg 86A:2607, 2004.
- Strauss D, Ojdana K, Shavelle R, Rosenbloom L: Decline in function and life expectancy of older persons with cerebral palsy, Neurorehabilitation 19:69, 2004.
- Younger AS, Hansen ST Jr: Adult cavovarus foot, J Am Acad Orthop Surg 13:302, 2005.
- Adult Stroke Patient Braun RM, Hoffer MM, Mooney V, et al: Phenol nerve block in the treatment of acquired spastic hemiplegia in the upper limb, J Bone Joint Surg 55A:580, 1973.
- Braun RM, West F, Mooney V, et al: Surgical treatment of the painful shoulder contracture in the stroke patient, J Bone Joint Surg 53A:1307, 1971.
- Caldwell C, Braun RM: Spasticity in the upper extremity, Clin Orthop Relat Res 104:80, 1974.
- McCollough NC III: Orthopaedic evaluation and treatment of the stroke patient, I: incidence and functional prognosis of hemiplegia, Instr Course Lect 24:21, 1975.
- McCollough NC III: Orthopaedic evaluation and treatment of the stroke patient, II: lower extremity management: orthotic management, Instr Course Lect 24:29, 1975.
- McCollough NC III: Orthopaedic evaluation and treatment of the stroke patient, III: upper extremity management: evaluation and management, Instr Course Lect 24:45, 1975.
- McCollough NC III: Orthotic management in adult hemiplegia, Clin Orthop Relat Res 131:38, 1978.
- Mooney V, Perry J, Nickel VL: Surgical and non-surgical orthopaedic care of stroke, J Bone Joint Surg 49A:989, 1967.
- Perry J: Orthopaedic evaluation and treatment of the stroke patient, I: lower extremity management: examination—a neurologic basis for treatment, Instr Course Lect 24:26, 1975.
- Perry J, Giovan P, Harris LJ, et al: The determinants of muscle action in the hemiparetic lower extremity (and their effect on the examination procedure), Clin Orthop Relat Res 131:71, 1978.
- Perry J, Waters RL: Orthopaedic evaluation and treatment of the stroke patient, II: lower extremity management: surgery, Instr Course Lect 24:26, 1975.
- Perry J, Waters RL: Orthopaedic evaluation and treatment of the stroke patient, III: upper extremity management: surgery, Instr Course Lect 24:45, 1975.
- Perry J, Waters RL, Perrin T: Electromyographic analysis of equinovarus following stroke, Clin Orthop Relat Res 131:47, 1978.
- Roper BA: The orthopedic management of the stroke patient, Clin Orthop Relat Res 219:78, 1987.
- Solomonow M: Restoration of movement by electrical stimulation: a contemporary view of the basic problems, Orthopedics 7:245, 1984.
- Tracy HW: Operative treatment of the plantar-fl exed inverted foot in adult hemiplegia, J Bone Joint Surg 58A:1142, 1976.
- Waters RL: Stroke rehabilitation, Clin Orthop Relat Res 131:2, 1978 (editorial comment). Waters RL: Upper extremity surgery in stroke patients, Clin Orthop Relat Res 131:30, 1978.
- Waters RL, Frazier J, Garland DE, et al: Electromyographic gait analysis before and after operative treatment for hemiplegic equinus and equinovarus deformity, J Bone Joint Surg 64A:284, 1982.
- Waters RL, Garland DE, Perry J, et al: Stiff-legged gait in hemiplegia: surgical correction, J Bone Joint Surg 61A:927, 1979.
- Waters RL, Perry J, Garland D: Surgical correction of gait abnormalities following stroke, Clin Orthop Relat Res 131:54, 1978.
You Might Also Like