Mastering Proximal Humeral Resection with Allograft Prosthetic Composite Arthroplasty

Key Takeaway
This masterclass details proximal humeral resection with allograft prosthetic composite arthroplasty. We'll meticulously cover surgical anatomy, preoperative planning, and intraoperative execution from incision to reconstruction. Learn critical techniques for neurovascular preservation, tumor margin control, and hardware application. Gain insights into pearls, pitfalls, and comprehensive postoperative management for optimal patient outcomes, ensuring functional recovery and long-term stability.
Alright, team, gather 'round. Welcome to the operating theater. Today, we're tackling a challenging but incredibly rewarding procedure: a proximal humeral resection with allograft prosthetic composite (APC) arthroplasty. This isn't just about removing a tumor; it's about meticulous reconstruction, preserving function, and giving our patient the best possible quality of life. The APC technique is a powerful tool, potentially mitigating the long-term complications we sometimes see with frozen osteoarticular allografts, such as fracture, joint collapse, and secondary arthritis.
Comprehensive Surgical Anatomy: Navigating the Shoulder Girdle
Before we make a single incision, let's refresh our understanding of this critical anatomical region. The shoulder girdle is a complex interplay of bone, muscle, and neurovascular structures, and our success hinges on respecting these relationships.
Osteology and Resection Types
We're performing an intra-articular resection today, a Type 1, which means we're preserving the glenoid and the crucial abductor mechanism.

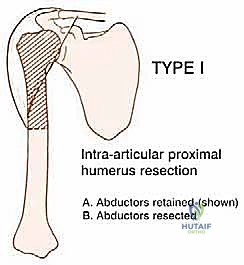
Figure 1: Type 1 (intra-articular) resection, emphasizing retained abductors.
This is a key distinction from more extensive extra-articular resections that might involve parts of the scapula, which would drastically alter our reconstructive options. The proximal humerus itself is a common site for primary bone tumors, and understanding its cortical and medullary architecture is paramount for achieving adequate margins.
Muscular Intervals and Attachments
The critical musculature of the upper humerus includes:
* Deltoid: The primary abductor of the arm, innervated by the axillary nerve. Its preservation, along with its innervation, is directly correlated with functional recovery. We'll be detaching it from the deltoid tuberosity.
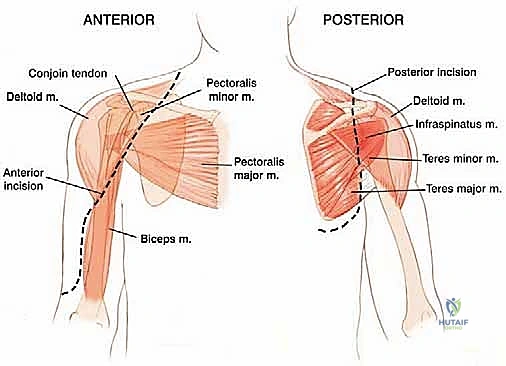
* Rotator Cuff: Comprising the supraspinatus, infraspinatus, teres minor (attaching to the greater tuberosity), and subscapularis (attaching to the lesser tuberosity). These tendons are essential for shoulder stability and rotation. The supraspinatus and infraspinatus are innervated by the suprascapular nerve.
* Pectoralis Major: Inserts onto the lateral lip of the bicipital groove.
* Latissimus Dorsi and Teres Major: Insert into the medial lip and floor of the bicipital groove, respectively. These muscles will need to be meticulously detached.
* Biceps and Coracobrachialis: These muscles, along with the musculocutaneous nerve that pierces the coracobrachialis, usually can be preserved through careful dissection and retraction, as they originate from the coracoid process.
Neurovascular Structures: Our Watchwords
This is where our attention to detail becomes absolutely non-negotiable.
* Axillary Nerve and Posterior Humeral Circumflex Artery: These structures pass through the quadrangular space (bounded by the teres minor superiorly, teres major inferiorly, surgical neck of the humerus laterally, and long head of the triceps medially) before innervating the deltoid. Preserving this neurovascular bundle is critical for maintaining abductor function.
* Radial Nerve: This nerve passes posteriorly around the humerus in the spiral groove, distal to the deltoid insertion. It's highly vulnerable during distal humeral dissection and bone division, especially when retracting the humeral shaft.
* Brachial Plexus and Axillary Artery/Vein: Located medially in the axilla, these vital structures transition into the brachial artery and vein as they move distally. They are in close proximity to the coracoid and require careful dissection, identification, and protection, particularly during medial retraction.
* Musculocutaneous Nerve: As mentioned, it supplies the biceps and coracobrachialis. It's usually safe if we maintain our dissection plane correctly.
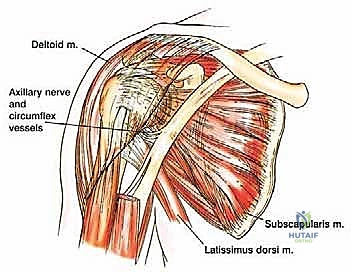
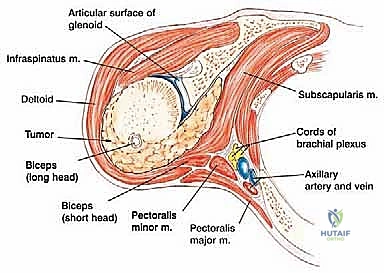
Figure 2: Coronal and transverse diagrams illustrating the intricate anatomy of the shoulder and upper humerus.
Preoperative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of a successful oncologic resection and reconstruction. It’s not just about the surgery itself, but every step leading up to it.
Patient Assessment and Indications
Our patient presents with pain, restricted range of motion, and a mass in the proximal humerus. Imaging confirms a low-grade sarcoma, specifically a chondrosarcoma, which has been pretreated with neoadjuvant chemotherapy, showing a good response. This intra-articular resection is indicated for such benign but aggressive tumors or well-responded sarcomas, where preservation of the abductor mechanism is feasible.
We've performed a meticulous neurologic examination, confirming intact function of the axillary, radial, median, ulnar, and musculocutaneous nerves. Any significant preoperative deficit in these nerves would necessitate a re-evaluation of our plan for an intra-articular resection and functional arthroplasty.
Imaging and Staging Studies
We've reviewed a comprehensive suite of imaging:
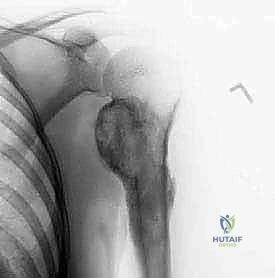
* Plain Radiographs (AP, lateral, axillary views): These were our initial diagnostic tools, providing crucial clues to the nature of the neoplasm – note the bone expansion and cortical thickening characteristic of chondrosarcoma.
Figure 3: Preoperative AP and lateral radiographs of the proximal humerus showing a chondrosarcoma.
* MRI (T1-weighted, coronal): Invaluable for delineating the soft tissue extent of the tumor and its precise relationship to the neurovascular bundle. Crucially, it defines the intramedullary extent, especially vital for tumors like chondrosarcoma where plain radiographs can underestimate involvement.
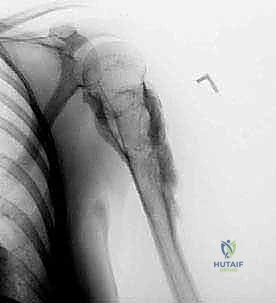
Figure 3: Preoperative coronal T1-weighted MRI scan showing a lesion with intramedullary involvement.
* CT Scans: Provided superior detail on bone involvement and cortical integrity.
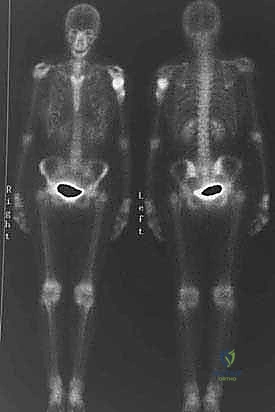
* Technetium Tc 99m Bone Scan: Confirmed an isolated humeral lesion, ruling out skip lesions or polyostotic disease, which is essential for staging and ensuring we're not missing multicentric disease.
* Chest CT: Performed pre-biopsy for sarcoma staging.
Biopsy Planning: The Critical First Step
The biopsy, performed previously, was meticulously planned. We collaborated with our pathologist to ensure adequate tissue for diagnosis. The biopsy site itself was strategically placed, avoiding the deltopectoral groove, instead passing through either the deltoid or pectoralis muscle. This ensures the biopsy tract can be excised en bloc with the definitive tumor specimen, preventing contamination.
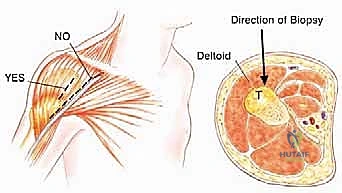
Figure 4: Diagram of the correct biopsy incision for tumors of the upper humerus, avoiding the deltopectoral groove.
Allograft and Prosthesis Procurement
We've already contacted an AATB-accredited tissue bank to secure our frozen humeral allograft. Its radiograph has been templated against our patient's anatomy and the chosen long-stem humeral prosthetic hemiarthroplasty device. We ensured the allograft is sufficiently long to replace the resected bone and has an appropriate soft tissue cuff for later repair. We also templated the glenoid to confirm the appropriate metallic hemiarthroplasty size.
Positioning and OR Setup
Our patient is positioned in a semi-Fowler's (beach chair) position. This allows for extensile exposure of the shoulder girdle, both anteriorly and posteriorly if needed.
* A towel roll is placed longitudinally behind the medial border of the scapula. This elevates and stabilizes the scapula and glenoid, making our anterior approach more direct and preventing the scapula from "winging" posteriorly.
* The entire upper limb, from the hand to the neck, is prepped and draped in a sterile fashion, allowing for complete free manipulation of the arm throughout the procedure. This is crucial for exposing different aspects of the humerus and for facilitating dislocation and reduction.
* We have a C-arm fluoroscopy unit readily available, draped and positioned for intraoperative imaging, particularly for confirming our bone cuts and hardware placement.
* An arm board is attached to the table, providing a stable platform for the arm during initial dissection and for resting the limb when not actively being manipulated.
Step-by-Step Intraoperative Execution: The Surgeon's View
Alright team, we've done our time-out. Patient, procedure, site confirmed. Let's begin.
1. Incision and Biopsy Site Excision
"Scalpel, please. We'll start with a standard utilitarian deltopectoral incision, extending from the clavicle down to the deltoid insertion, approximately 15-20 cm in length. This curvilinear incision will allow us excellent exposure. Remember, the previous biopsy site was carefully planned to be excised en bloc with our definitive resection. So, we'll incorporate that elliptical skin incision into our primary approach, ensuring no tumor cells are left behind in the superficial tissues."
"Now, deepen the incision through the subcutaneous tissue and platysma. Control any bleeders with electrocautery. We're meticulously excising the biopsy tract down to the muscle layer."
2. Development of the Deltopectoral Groove
"Next, we identify the deltopectoral groove. Fellows, you can often see the cephalic vein running within this interval. We have two options for the vein: either carefully retract it laterally with the deltoid or, if necessary for exposure or if it's compromised by the tumor, ligate and divide it. For today, given its clear path, we will carefully retract it laterally."
"Using a combination of blunt and sharp dissection, we'll develop this interval from the clavicle proximally, where the deltoid originates, down to its insertion on the deltoid tuberosity. We're separating the anterior fibers of the deltoid laterally from the pectoralis major medially. Be precise here; we want to stay right in this natural plane."
3. Deep Dissection and Neurovascular Isolation
"Now, let's deepen our exposure. We'll begin by detaching the pectoralis major from its insertion on the lateral lip of the bicipital groove. Use a periosteal elevator to carefully lift it off the humerus, staying subperiosteal to preserve its integrity. Tag this tendon with a heavy non-absorbable suture, like a #5 Ethibond, for later repair. We'll retract the pectoralis major medially."
"Next, we need to address the deep neurovascular structures. Let's identify the musculocutaneous nerve. It typically pierces the coracobrachialis muscle. Carefully dissect around the biceps and coracobrachialis, retracting them medially along with the main brachial plexus and axillary vessels. Use broad, blunt retractors like a Hohmann or Army-Navy to protect these vital structures. We must maintain constant vigilance here."
"Now, let's turn our attention posteriorly and laterally. We need to identify the quadrangular space. Carefully dissect between the teres minor superiorly and teres major inferiorly, and the long head of the triceps medially. Here, you will find the axillary nerve and the posterior humeral circumflex vessels. These are paramount for deltoid function. Meticulously dissect them free from any surrounding tissue or tumor involvement, tracing them distally towards the deltoid. Use fine instruments and gentle technique. Once identified, carefully loop them with vessel loops for easy identification and protection."
"Next, we must protect the radial nerve. This nerve courses around the posterior aspect of the humerus in the spiral groove, distal to the deltoid insertion. As we manipulate the humerus, especially as we prepare for our bone cut, this nerve is highly vulnerable. We'll place Chandler retractors around the posterior aspect of the humerus, ensuring they are protecting the radial nerve from any direct injury or excessive tension during retraction."
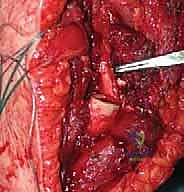
Figure 1: The radial nerve identified adjacent to the resected bone, highlighting the importance of its preservation.
4. Soft Tissue Detachment and Tagging
"With our neurovascular structures protected, we can proceed with detaching the remaining soft tissues from the proximal humerus, which will be part of our resected specimen."
- Rotator Cuff: "First, the subscapularis. We'll carefully detach it from the lesser tuberosity. Use a sharp scalpel or electrocautery, staying close to the bone to ensure a clean release. Tag it with a heavy suture. Now, move to the greater tuberosity. We'll detach the supraspinatus, infraspinatus, and teres minor tendons. Again, sharp dissection close to the bone. Tag each tendon individually with sutures for precise identification and repair later. This tagging is crucial for anatomical reconstruction."
- Deltoid: "Next, the deltoid. We've already developed our deltopectoral interval. Now, we'll detach the deltoid from its insertion on the deltoid tuberosity. This will allow us to mobilize the muscle superiorly and laterally."
- Latissimus Dorsi and Teres Major: "Finally, the latissimus dorsi and teres major muscles are detached from their insertions on the humeral shaft. Again, tag these with sutures."
5. Arthrotomy and Humeral Head Dislocation
"Now, we approach the joint capsule. We'll perform an anterior capsulotomy first. This allows us to inspect the joint for any gross tumor contamination. If there's any suspicion, we would send samples for frozen section. In our case, the joint appears clear."
"Once clear, we'll proceed with a circumferential arthrotomy. Release the superior and anterior capsule. As we move inferiorly, we must be exceptionally careful to protect the axillary nerve. To facilitate this, adduct the patient's arm and progressively externally rotate it. This maneuver relaxes the inferior capsule and moves the axillary nerve away from our surgical field, allowing us to safely incise the inferior capsule off the humeral neck."
"Once the capsule is fully released, we can gently dislocate the humeral head from the glenoid. Use an assistant to apply gentle traction and external rotation, while I use a bone hook to lever the humeral head out of the glenoid fossa. This will give us full access to the proximal humerus."
6. Bone Division
"Now for the critical bone cut. We've already isolated the humeral shaft distal to the tumor. Based on our preoperative MRI and templating, we've identified the
Additional Intraoperative Imaging & Surgical Steps
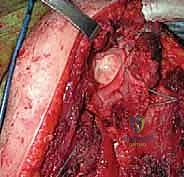
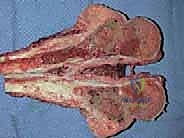
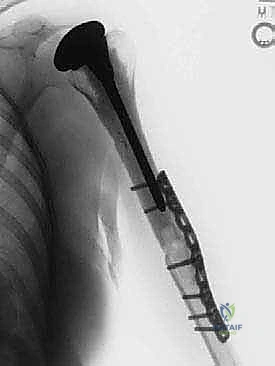
REFERENCES
-
Cheng EY, Gebhardt MC. Allograft reconstructions of the shoulder after bone tumor resections. Orthop Clin North Am 1991;22: 37–48.
-
Damron TA, Rock MG, O’Connor MI, et al. Functional laboratory assessment after oncologic shoulder joint resections. Clin Orthop Relat Res.1998;348:124–134.
-
DeGroot H, Donati D, Di Liddo M, et al. The use of cement in osteoarticular allografts for proximal humeral bone tumors. Clin Orthop Relat Res 2004 427:190–197.
-
Dudkiewicz I, Velkes S, Oran A, et al. Composite grafts in the treatment of osteosarcoma of the proximal humerus. Cell Tissue Bank 2003;4:37–41.
-
Getty PJ, Peabody TD. Complications and functional outcomes of reconstruction with an osteoarticular allograft after intra-articular resection of the proximal aspect of the humerus. J Bone Joint Surg Am 1999;81A:1138–1146.
-
Gitelis S, Malawer M, MacDonald D, Derman G. Principles of limb salvage surgery—tumors of the proximal humerus. In: Orthopaedic Surgery. Philadelphia: Lippincott Williams & Wilkins, 2001.
-
Jensen KL, Johnston JO. Proximal humeral reconstruction after excision of a primary sarcoma. Clin Orthop Relat Res 1995;311: 164–175.
-
Kassab M, Dumaine V, Babinet A, et al. [Twenty nine shoulder reconstructions after resection of the proximal humerus for neoplasm with mean 7-year follow-up]. Rev Chir Orthop Reparatrice Appar Mot 2005;91:15–23.
-
O’Connor MI, Sim FH, Chao EY. Limb salvage for neoplasms of the shoulder girdle. Intermediate reconstructive and functional results. J Bone Joint Surg Am 1996;78A:1872–1888.
-
Rodl RW, Gosheger G, Gebert C, et al. Reconstruction of the proximal humerus after wide resection of tumours. J Bone Joint Surg Br 2002;84B:1004–1008.
-
Wang J, Dickinson IC. [Functional outcome following shoulder tumor resection and reconstruction]. Zhonghua Wai Ke Za Zhi 2006; 44:809–12.
Jensen and Johnston 7 reported on four patients with an allograft prosthetic composite using the Neer prosthesis and found excellent outcomes.
In 2005, Kassab et al 8 reported on three patients with an allograft prosthetic composite of the humerus. The Musculoskeletal Tumor Society (MSTS) functional score for this small series was 76%.
Damron et al 2 functionally evaluated shoulder reconstruction and concluded that the osteoarticular allograft procedure had the best outcomes if the abductors of the shoulder are preserved.
O’Connor, Sim, and Chao 9 reported on one of the largest series of upper humerus reconstructions (57 patients). An osteoarticular allograft, which was used in eight patients, had the best functional outcomes in their cohort. Four of eight of these grafts fractured. Other authors reported outcomes with osteoarticular allograft reconstruction after an intra-articular resection. 1,10
DeGroot et al 3 reported a 37% allograft fracture rate and recommended the osteoarticular allograft be filled with cement to decrease this problem. Some of the fractured allografts were salvaged with an allograft prosthetic composite arthroplasty.
Wang et al 11 reported osteoarticular allograft fractures in 14 of their 20 patients.