Hallucal Sesamoid Fractures: Diagnosis & Surgical Management
Key Takeaway
Hallucal sesamoid fractures present a complex diagnostic and therapeutic challenge, often requiring differentiation from symptomatic bipartite sesamoids. Injuries occur via direct axial loading or indirect hyperextension, commonly affecting athletes. Management ranges from conservative offloading to surgical interventions, including mini-fragment screw fixation, bone grafting, or partial/complete sesamoidectomy. Precise surgical technique and meticulous soft tissue repair are paramount to prevent postoperative complications such as hallux varus or valgus deformities.
INTRODUCTION TO HALLUCAL SESAMOID FRACTURES
Fractures of the hallucal sesamoids represent a unique and often challenging pathology within foot and ankle orthopaedics. These injuries are most frequently encountered in two distinct clinical scenarios: acute high-energy trauma, often associated with dislocations of the first metatarsophalangeal (MTP) joint, and chronic stress fractures. The latter is predominantly seen in high-demand athletic populations, particularly long-distance runners, ballet dancers, and turf-sport athletes.
The diagnostic complexity of sesamoid fractures lies in differentiating true osseous failure from other pathologies affecting the sesamoid complex, most notably the symptomatic bipartite sesamoid, osteochondritis dissecans, and osteonecrosis. Misdiagnosis or delayed treatment can lead to chronic debilitating pain, altered gait mechanics, and progressive degenerative joint disease of the first ray.
SURGICAL ANATOMY AND BIOMECHANICS
To fully grasp the implications of sesamoid fractures and their surgical management, a profound understanding of the first MTP joint's biomechanics is mandatory. The hallucal sesamoids—medial (tibial) and lateral (fibular)—are embedded within the tendinous insertions of the flexor hallucis brevis (FHB) muscle.
The Sesamoid Complex
The sesamoids articulate dorsally with the plantar facets of the first metatarsal head, separated by the metatarsal crista. They are interconnected by the robust intersesamoidal ligament and are integral components of the plantar plate.
- Tibial (Medial) Sesamoid: Generally larger, longer, and bears a significantly higher load during the stance phase of gait. It is seated more directly beneath the medial facet of the metatarsal head, making it the more commonly injured of the two sesamoids.
- Fibular (Lateral) Sesamoid: Smaller, more circular, and slightly more mobile. It is less frequently fractured but is highly susceptible to injury during violent hyperextension or lateral dislocation events.
Clinical Pearl: The sesamoids function as a fulcrum, increasing the mechanical advantage of the FHB tendon, much like the patella does for the quadriceps. They absorb weight-bearing forces, reduce friction, and protect the flexor hallucis longus (FHL) tendon, which glides smoothly between them.
PATHOPHYSIOLOGY AND MECHANISM OF INJURY
The mechanism of injury dictates the fracture pattern and guides subsequent management. Injuries are broadly categorized into direct and indirect mechanisms.
Direct Trauma
Direct injury typically involves a sudden, high-energy axial loading force applied directly to the plantar aspect of the sesamoid. Examples include a fall from a height landing on the forefoot or a direct crush injury.
* Fracture Pattern: This mechanism generally produces a comminuted, multifragmented fracture, often with significant cartilaginous damage to both the sesamoid and the overlying metatarsal head.
Indirect Trauma
Indirect injuries are more common in athletic settings (e.g., football, soccer, rugby) and occur when the first MTP joint is violently hyperextended. This is often a variant of the classic "turf toe" injury.
* Fracture Pattern: The violent tensile force transmitted through the FHB and plantar plate typically results in a transverse fracture or an avulsion-type injury.
CLINICAL EVALUATION
History and Physical Examination
Patients typically present with localized pain, swelling, and ecchymosis over the plantar aspect of the first MTP joint. In chronic stress fractures, the onset is insidious, with pain exacerbating during push-off activities.
Key physical examination findings include:
* Pinpoint Tenderness: Exquisite tenderness directly over the affected sesamoid (tibial or fibular).
* Range of Motion Deficits: Limited active extension of the great toe. Passive extension of the hallux will reliably reproduce sharp pain due to the tension placed on the fractured sesamoid via the FHB complex.
* Gait Alterations: Patients often exhibit an antalgic gait, characterized by a shortened stance phase on the affected side. When descending stairs, the patient will characteristically lead with the injured foot to avoid the terminal stance push-off phase.
DIAGNOSTIC IMAGING AND THE BIPARTITE DILEMMA
Standard Radiographic Evaluation
A comprehensive radiographic series is the first line of investigation. Standard weight-bearing anteroposterior (AP) and lateral views of the foot should be obtained.
- Lateral View in Pronation: The forefoot should be placed in slight pronation while obtaining the lateral radiograph. This specific positioning helps to profile the sesamoids and project them away from the overlapping metatarsal head.
- Oblique Views: The medial oblique view is highly sensitive for evaluating the tibial sesamoid, whereas the lateral oblique view is optimal for isolating the fibular sesamoid.
- Axial Sesamoid View: This specialized view is critical. It allows for direct visualization of the sesamoid-metatarsal articulation, revealing joint space narrowing, subchondral sclerosis, or osteochondral defects associated with osteochondritis.
Differentiating Fracture from Bipartite Sesamoid
The most significant diagnostic hurdle is distinguishing an acute fracture from a bipartite sesamoid. The sesamoids are reported to be multipartite in 5% to 30% of asymptomatic individuals, with the bipartite condition occurring far more frequently in the tibial sesamoid.
Diagnostic Pitfall: While a bipartite sesamoid can be bilateral, the presence of a singular, unipartite sesamoid in the contralateral foot does not absolutely confirm that the symptomatic foot has a fracture. The symptomatic foot may simply have a painful synchondrosis separation of a unilateral bipartite sesamoid.
Key Distinguishing Features:
1. Fragment Size: Fractured sesamoid bones tend to divide roughly into equally sized sections. Conversely, bipartite sesamoids typically present with one dominant, larger fragment and one smaller accessory fragment.
2. Edge Morphology: Bipartite sesamoids exhibit smooth, well-corticated, and rounded edges. Fractured sesamoids display irregular, jagged, and uncorticated margins.
Advanced Imaging Modalities
When plain radiographs are equivocal, advanced imaging is warranted.
* Computed Tomography (CT): High-resolution CT scans (or tomograms) are excellent for delineating subtle fracture lines, assessing comminution, and evaluating the articular surface.
* Radionuclide Bone Scanning (Technetium-99m): Highly sensitive for detecting stress fractures or acute osseous injury. However, extreme caution is recommended during interpretation. Studies indicate that 26% to 29% of completely asymptomatic individuals exhibit increased radiotracer uptake in the sesamoids, and significant side-to-side asymmetry is common even in healthy patients.
* Magnetic Resonance Imaging (MRI): MRI is increasingly utilized to assess bone marrow edema, osteonecrosis, and concomitant soft tissue injuries (e.g., plantar plate ruptures).
DIFFERENTIAL DIAGNOSIS
If the fracture is not widely displaced, the differential diagnosis must include:
* Symptomatic bipartite sesamoid (synchondrosis injury)
* Osteochondritis dissecans of the sesamoid
* Osteonecrosis (avascular necrosis) of the sesamoid
* Plantar plate rupture
* Flexor hallucis longus (FHL) tenosynovitis
SURGICAL MANAGEMENT
While many non-displaced or stress fractures can be managed conservatively with strict immobilization, offloading, and extended rest, surgical intervention is indicated for widely displaced fractures, fractures associated with MTP dislocation, highly comminuted fractures, and symptomatic nonunions that have failed exhaustive conservative care.
The primary surgical options include Open Reduction and Internal Fixation (ORIF), bone grafting, partial sesamoidectomy, and complete sesamoidectomy. Regardless of the chosen method, meticulous restoration of the flexor mechanism is crucial.
1. Open Reduction and Internal Fixation (ORIF)
ORIF is the gold standard for acute, displaced transverse fractures of the sesamoid, particularly in young, athletic patients where preservation of the sesamoid's biomechanical function is paramount.
Surgical Technique:
* Approach: For the tibial sesamoid, a medial longitudinal incision is utilized, staying plantar to the medial eminence to avoid the medial dorsal cutaneous nerve, while carefully protecting the medial plantar proper digital nerve.
* Preparation: The fracture site is exposed by longitudinally incising the medial capsule and the FHB expansion. The fracture hematoma is evacuated, and the jagged edges are debrided to expose bleeding cancellous bone.
* Fixation: The fracture is reduced using a pointed reduction clamp. Fixation is typically achieved using a mini-fragment screw system (1.5 mm to 2.0 mm). A cannulated or solid headless compression screw is directed from proximal to distal (or distal to proximal, depending on fragment size) to achieve rigid interfragmentary compression.
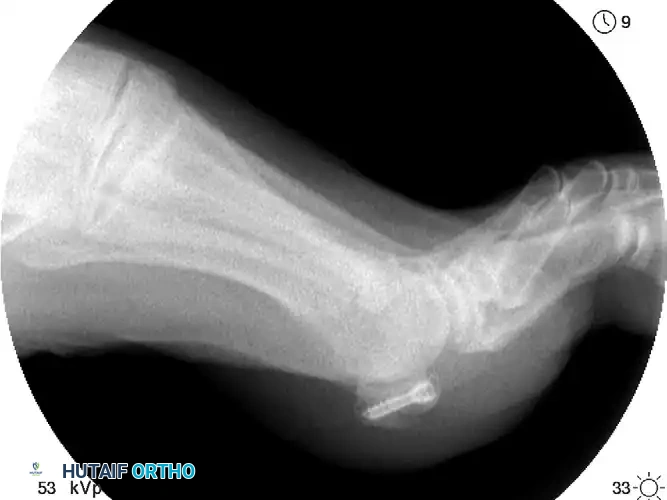
FIGURE 88-80: Mini-fragment screw fixation of a sesamoid fracture, demonstrating precise intra-osseous placement to achieve compression while avoiding the articular surface.
2. Bone Grafting
In cases of chronic nonunion where the fragments are viable but fail to unite, autologous bone grafting (often harvested from the distal tibia or calcaneus) can be utilized. This is advocated as a joint-preserving alternative to excision in select, highly compliant patients. The graft is packed into the debrided nonunion site, often augmented with internal fixation.
3. Partial Sesamoidectomy
Excision of the fractured pole (usually the smaller proximal or distal fragment) is indicated when the fragment is too small for rigid fixation or in cases of localized osteonecrosis.
* Technique: The fragment is carefully shelled out of the FHB tendon using sharp dissection.
* Critical Step: The resulting defect in the FHB tendon must be meticulously repaired using heavy non-absorbable sutures (e.g., #2-0 FiberWire) to restore the tension and continuity of the flexor apparatus. Failure to do so will result in weakness and potential deformity. Literature indicates excellent outcomes, with athletes frequently returning to sports after excision of the proximal pole.
4. Complete Sesamoidectomy
Complete excision of the sesamoid is reserved as a salvage procedure.
* Indications: Highly comminuted fractures with no reconstructable large fragments, severe osteonecrosis, or profound loss of articulating cartilage on either the sesamoid or the overlying metatarsal head.
* Technique: The entire sesamoid is enucleated from its tendinous envelope. The surgeon must take extreme care not to violate the FHL tendon or the intersesamoidal ligament unnecessarily.
Surgical Warning: Complete excision of both the tibial and fibular sesamoids is strongly contraindicated. Bilateral excision completely destroys the intrinsic flexor mechanism of the hallux, inevitably resulting in a severe, rigid claw toe deformity (cock-up deformity) that is exceedingly difficult to salvage.
POSTOPERATIVE PROTOCOL AND REHABILITATION
Postoperative management is tailored to the specific procedure performed:
* Following ORIF or Bone Grafting: Patients are typically placed in a non-weight-bearing cast or rigid boot for 4 to 6 weeks to allow for osseous union. Gradual weight-bearing in a stiff-soled shoe follows, with progressive range-of-motion exercises.
* Following Sesamoidectomy: Patients may begin protected heel-weight-bearing in a postoperative shoe immediately or within the first week. Active and passive MTP joint mobilization is initiated early (at 2-3 weeks) to prevent capsular scarring and stiffness.
Return to Play:
In a comprehensive review of sesamoidectomies in athletically active patients, athletes were able to return to competitive sports at a mean time of 7.5 weeks. The remainder of the "active" non-competitive patients returned to full activity at 12 weeks.
COMPLICATIONS AND OUTCOMES
While outcomes following sesamoid surgery are generally favorable—with reports indicating up to 90% of patients returning to their preoperative activity levels—complications can be severe if surgical principles are violated.
Deformity
The most feared complications relate to biomechanical imbalance following sesamoid excision:
* Hallux Valgus: Can develop late after a tibial sesamoidectomy. Excision of the medial sesamoid weakens the medial head of the FHB, allowing the unresisted lateral structures (adductor hallucis and lateral FHB) to pull the hallux into valgus.
* Hallux Varus: Can develop after a fibular sesamoidectomy due to the unresisted pull of the medial structures (abductor hallucis).
Clinical Pearl: The prevention of postoperative hallux varus or valgus relies entirely on the careful, robust soft tissue repair of the tendinous defect left after excision. The remaining capsulotendinous structures must be imbricated and sutured tightly.
Neurological and Soft Tissue Complications
- Neuroma Formation: Postoperative scarring and iatrogenic injury to the plantar proper digital nerves can result in painful neuroma-like symptoms. This is particularly noted after plantar approaches to the fibular sesamoid.
- Plantar Keratosis: Altered weight-bearing mechanics can lead to intractable plantar keratosis under the remaining sesamoid or adjacent metatarsal heads.
In conclusion, hallucal sesamoid fractures demand a high index of suspicion, precise radiographic interpretation, and a nuanced approach to surgical intervention. Whether undertaking internal fixation or excision, the orthopaedic surgeon must prioritize the anatomical restoration of the first ray's complex soft-tissue envelope to ensure optimal functional recovery.
You Might Also Like
