Rheumatoid Forefoot Reconstruction
Introduction and Epidemiology
Rheumatoid arthritis (RA) is a chronic, systemic inflammatory disorder characterized by a symmetric polyarthropathy predominantly affecting synovial joints. The foot and ankle are frequently involved, with upalaman epidemiological studies indicating that up to 90% of patients with chronic rheumatoid arthritis will develop foot symptoms over the course of their disease. The forefoot is the most commonly affected anatomical region, often presenting as the initial site of symptomatic disease in approximately 17% of patients.
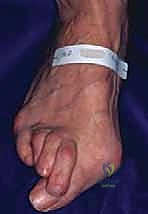
Historically, the natural history of rheumatoid forefoot deformity followed a predictable and relentless course of progressive joint destruction. Unrelenting synovitis leads to capsular distension, ligamentous attenuation, and eventual joint subluxation or dislocation. The classic rheumatoid forefoot triad consists of severe hallux valgus, lesser metatarsophalangeal (MTP) joint dorsal dislocations with associated claw toe deformities, and distal migration of the plantar fat pad resulting in intractable plantar keratosis (IPK).

While the advent of disease-modifying antirheumatic drugs (DMARDs) and biologic agents (e.g., TNF-alpha inhibitors) has significantly altered the disease trajectory—reducing the incidence of severe, end-stage destructive arthropathy—a substantial cohort of patients still requires surgical intervention. The paradigm of surgical management has evolved from pan-metatarsal head resections to a more nuanced approach, often favoring first MTP arthrodesis combined with lesser MTP joint resection arthroplasties or joint-preserving osteotomies in less advanced cases.

Surgical Anatomy and Biomechanics
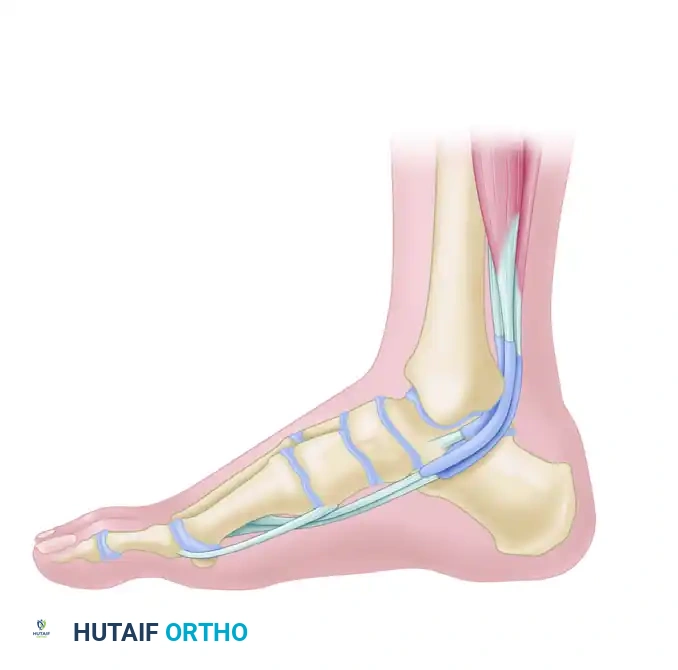
A thorough understanding of forefoot biomechanics and the pathomechanics of rheumatoid disease is essential for successful reconstruction. The MTP joint is a complex diarthrodial articulation stabilized by static and dynamic restraints.
Static and Dynamic Stabilizers
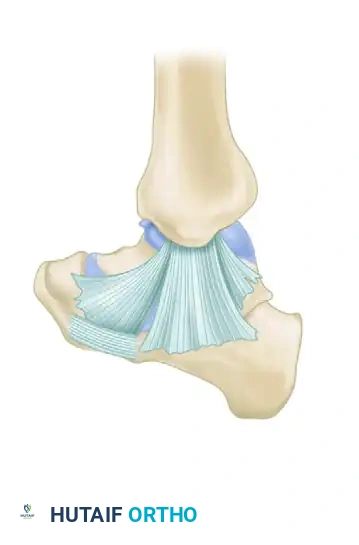
The primary static stabilizers of the lesser MTP joints include the plantar plate, the collateral ligaments (proper and accessory), and the joint capsule. The plantar plate is a thick, fibrocartilaginous structure that resists dorsal translation of the proximal phalanx. The dynamic stabilizers consist of a delicate balance between the extrinsic musculature (extensor digitorum longus, extensor digitorum brevis, flexor digitorum longus, flexor digitorum brevis) and the intrinsic musculature (lumbricals and interossei).

Normally, the intrinsic muscles pass plantar to the transverse axis of the MTP joint, generating a plantarflexion moment at the MTP joint and an extension moment at the interphalangeal (IP) joints. The proximal phalanx of the hallux normally exhibits a physiologic valgus orientation of 0 to 15 degrees at the first MTP joint, supported by the medial capsule, medial sesamoid complex, and the abductor hallucis.
Pathomechanics of Rheumatoid Deformity
The pathogenesis of the rheumatoid forefoot is driven by chronic, hyperplastic synovitis (pannus formation). This inflammatory tissue produces proteolytic enzymes and cytokines that degrade articular cartilage and subchondral bone, leading to marginal erosions and subchondral cysts. Concurrently, the mechanical distension of the joint capsule by synovial hypertrophy and effusions causes attenuation of the collateral ligaments and the plantar plate.

As the plantar plate fails, the proximal phalanx subluxates dorsally under the continuous pull of the extensor tendons during the terminal stance phase of gait. Once the proximal phalanx translates dorsally, the line of pull of the intrinsic muscles shifts dorsal to the transverse axis of the MTP joint. This critical biomechanical alteration converts the intrinsics from MTP plantarflexors to MTP dorsiflexors. This exacerbates the dorsal dislocation of the MTP joint and leads to reciprocal plantarflexion of the proximal interphalangeal (PIP) joint, resulting in a fixed claw toe deformity.

At the first ray, the medial capsule attenuates, allowing the abductor hallucis to slide plantarward. The adductor hallucis then acts unopposed, pulling the hallux into severe valgus and pronation. As the lesser MTP joints dislocate, the metatarsal heads are driven plantarly. The protective plantar fat pad, which normally resides beneath the metatarsal heads, is drawn distally by the dislocating proximal phalanges. This leaves the prominent, often eroded lesser metatarsal heads directly subcutaneous, creating focal areas of extreme high pressure, intractable pain, and potential ulceration.

Indications and Contraindications
Surgical intervention is indicated when patients experience intractable pain, progressive deformity, or impending skin breakdown that fails to respond to comprehensive conservative management. Non-operative modalities include custom orthoses with metatarsal offloading pads, extra-depth footwear with wide toe boxes, rocker-bottom modifications, and pharmacological optimization.

When conservative measures are exhausted, the decision to proceed with operative reconstruction must be carefully weighed against the patient's vascular status, medical comorbidities, and systemic disease control.
| Clinical Scenario | Operative Indications | Non-Operative Indications |
|---|---|---|
| Pain Level | Intractable forefoot pain limiting ADLs despite orthotics | Mild to moderate pain managed with shoe modifications |
| Deformity Status | Rigid, fixed hallux valgus with dislocated lesser MTP joints | Flexible deformities without frank dislocation |
| Skin Integrity | Impending ulceration over medial eminence or plantar MT heads | Intact skin, manageable callosities |
| Vascular Status | Palpable pulses, ABI > 0.9, adequate capillary refill | ABI < 0.5, ischemic rest pain, absent pulses (Contraindication) |
| Medical Status | Medically optimized, cleared by rheumatology | Active systemic infection, unmanaged cardiopulmonary disease |
| Patient Goals | Desire for pain relief and functional ambulation | Non-ambulatory patient, minimal functional demands |

Pre Operative Planning and Patient Positioning
Comprehensive preoperative planning requires a multidisciplinary approach involving the orthopedic surgeon, rheumatologist, and primary care physician.
Clinical and Radiographic Evaluation
Physical examination must include a rigorous assessment of the vascular supply. Given the high prevalence of peripheral vascular disease and microvascular compromised in RA patients, an ankle-brachial index (ABI) and potentially non-invasive arterial Doppler studies should be obtained if pedal pulses are diminished. Neurologic examination should screen for peripheral neuropathy, which may alter postoperative weight-bearing compliance.

Standard weight-bearing radiographs of the foot (anteroposterior, lateral, and oblique views) are mandatory. The examiner must evaluate for periarticular osteopenia, symmetric joint space narrowing, marginal cortical erosions, and subchondral cysts. The AP view is utilized to assess the intermetatarsal angle, hallux valgus angle, and the degree of lesser MTP subluxation or dislocation. The lateral view aids in assessing the dorsal displacement of the proximal phalanges and the plantar prominence of the metatarsal heads.

Perioperative Medical Management
Perioperative management of DMARDs and biologic agents is guided by the American College of Rheumatology (ACR) and the American Association of Hip and Knee Surgeons (AAHKS) guidelines. Generally, non-biologic DMARDs (e.g., methotrexate) can be continued perioperatively. However, biologic agents (e.g., adalimumab, etanercept) should typically be withheld prior to surgery for an interval based on the drug's dosing cycle to mitigate infection risk, resuming postoperatively once wound healing is assured (typically 14 days).

Patient Positioning
The patient is positioned supine on the operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the foot to a neutral, directly anterior-facing position. A well-padded thigh tourniquet or calf tourniquet is utilized to provide a bloodless surgical field, provided there are no vascular contraindications. Prophylactic intravenous antibiotics are administered prior to tourniquet inflation.

Detailed Surgical Approach and Technique
The gold standard for end-stage rheumatoid forefoot deformity is the first MTP arthrodesis combined with lesser metatarsal head resection arthroplasties (often referred to as a modified Hoffman procedure). This provides a stable, plantigrade medial column and decompresses the lesser rays.

Incisional Strategy
A three-incision dorsal approach is generally preferred to minimize the risk of skin necrosis, maintaining adequate skin bridges (minimum of 1.5 to 2 cm).
1. First Incision: A dorsal longitudinal incision centered over the first MTP joint, medial to the extensor hallucis longus (EHL) tendon.
2. Second Incision: A dorsal longitudinal incision centered over the second webspace, allowing access to the second and third MTP joints.
3. Third Incision: A dorsal longitudinal incision centered over the fourth webspace, providing access to the fourth and fifth MTP joints.

Step 1 First MTP Arthrodesis
The first MTP joint is exposed via the medial dorsal incision. The EHL is retracted laterally, and the extensor hallucis brevis (EHB) is identified and transected if necessary. A longitudinal capsulotomy is performed, and full-thickness flaps are elevated to expose the articular surfaces. Aggressive synovectomy is undertaken.

The articular cartilage and subchondral bone of the metatarsal head and the base of the proximal phalanx are removed. While flat cuts can be utilized, cup-and-cone reamers are preferred as they allow for multi-planar adjustment of the arthrodesis position without compromising bony contact. The subchondral bone is meticulously prepared to bleeding cancellous bone.
Positioning of the arthrodesis is the most critical step. The hallux must be positioned in:
* Valgus: 10 to 15 degrees relative to the first metatarsal shaft (parallel to the lesser toes).
* Dorsiflexion: 10 to 15 degrees relative to the first metatarsal shaft, or 15 to 20 degrees relative to the floor, allowing for shoe clearance and rollover during gait.
* Rotation: Neutral rotation, ensuring the toenail faces directly dorsal.

Once provisional fixation with K-wires confirms optimal alignment, definitive fixation is achieved. A low-profile dorsal titanium plate with a compression screw (either integrated into the plate or placed separately as an interfragmentary lag screw) provides excellent biomechanical stability.

Step 2 Lesser Metatarsal Head Resections
Attention is directed to the lesser rays via the second and third incisions. The extensor tendons are identified. An extensor tenotomy or Z-lengthening is performed to relieve dorsal tension. A dorsal capsulotomy is performed at each MTP joint. The collateral ligaments are released to allow plantarflexion of the metatarsal shaft and dorsal translation of the proximal phalanx, exposing the metatarsal head.

Using an oscillating saw, the metatarsal heads are resected at the level of the surgical neck. The cut is typically made in a dorsal-distal to plantar-proximal direction to prevent a prominent plantar bony spike.

A meticulous metatarsal cascade must be created to prevent transfer metatarsalgia. The second metatarsal should be the longest, with a smooth, progressive shortening of the third, fourth, and fifth metatarsals. The surgeon must palpate the plantar aspect of the foot to ensure no residual bony prominences exist.

Step 3 Soft Tissue Balancing and Stabilization
Once the bony resection is complete, the toes are manually reduced. The plantar fat pad, previously migrated distally, must be drawn proximally beneath the resected metatarsal necks. To maintain this reduction and stabilize the flail joints during early soft tissue healing, smooth Kirschner wires (typically 0.045 or 0.062 inch) are driven antegrade through the tip of the toe, across the IP joints, and retrograde into the medullary canal of the remaining metatarsal shaft.

The incisions are irrigated copiously. Closure is performed in layers, utilizing absorbable suture for the deep tissues and non-absorbable monofilament for the skin. A bulky, compressive forefoot dressing is applied to control edema and maintain the alignment of the lesser toes.

Complications and Management
Rheumatoid forefoot reconstruction is fraught with potential complications due to poor host tissue quality, immunosuppressive medications, and altered biomechanics. Close postoperative surveillance is imperative.

Common Complications
Wound healing issues and superficial infections are the most common early complications, exacerbated by thin rheumatoid skin and systemic steroids. Nonunion of the first MTP arthrodesis occurs in approximately 5-10% of cases but is often asymptomatic. Symptomatic nonunions require revision with structural bone grafting and robust fixation.
Transfer metatarsalgia is a significant late complication, arising if the lesser metatarsal resection cascade is uneven, leaving a relatively long metatarsal stump that bears excessive plantar pressure.

| Complication | Estimated Incidence | Etiology | Prevention and Salvage Strategy |
|---|---|---|---|
| Wound Dehiscence / Infection | 5 - 15% | Thin skin, DMARDs, excessive retraction | Maintain wide skin bridges. Withhold biologics pre-op. Salvage: Local wound care, oral/IV antibiotics, rarely flap coverage. |
| First MTP Nonunion | 5 - 10% | Poor bone stock, inadequate fixation, smoking | Use cup-and-cone reamers for maximal bone contact. Rigid plate fixation. Salvage: Revision arthrodesis with autograft/allograft. |
| Transfer Metatarsalgia | 10 - 20% | Disrupted metatarsal cascade (uneven resection) | Meticulous intraoperative assessment of the length cascade. Salvage: Custom orthotics with offloading; revision osteotomy/resection. |
| Recurrent Lesser Toe Deformity | 15 - 25% | Inadequate soft tissue release, early pin removal | Ensure complete collateral release and adequate bony resection. Leave K-wires in for 4-6 weeks. Salvage: Revision resection, syndactylization. |
| Hardware Prominence | 5 - 10% | Thin dorsal soft tissue envelope over 1st MTP | Use low-profile plates. Salvage: Hardware removal after clinical and radiographic union is achieved. |

Post Operative Rehabilitation Protocols
The postoperative protocol is designed to protect the first MTP arthrodesis and maintain the alignment of the lesser rays while allowing soft tissues to heal.
Phase 1 Acute Healing (Weeks 0 to 2)
The patient is placed in a bulky Jones dressing and a rigid postoperative shoe or fracture boot. Weight-bearing is typically restricted to heel-touch or non-weight-bearing with crutches/walker to prevent bending forces across the first MTP joint and to avoid pin tract irritation. Elevation is critical to mitigate edema.
Phase 2 Intermediate Phase (Weeks 2 to 6)
At the 2-week mark, sutures are removed. The percutaneous K-wires in the lesser toes require routine pin care (e.g., alcohol or betadine swabs) to prevent pin tract infections. The patient may transition to protected weight-bearing through the heel and lateral border of the foot in a stiff-soled surgical shoe.
Phase 3 Pin Removal and Progression (Weeks 4 to 8)
The lesser toe K-wires are typically removed in the clinic between 4 and 6 weeks postoperatively, depending on the stability of the soft tissues. Following pin removal, toe taping or strapping may be utilized to maintain alignment. Radiographs are obtained at 6 to 8 weeks to assess the consolidation of the first MTP arthrodesis. Once clinical and radiographic union is progressing, the patient is transitioned into a wide-toe box, accommodative shoe.
Phase 4 Long Term Management (Months 3 and Beyond)
Maximal medical improvement may take 6 to 12 months. Patients are highly encouraged to utilize custom-molded orthotics with metatarsal pads to distribute plantar pressures evenly and protect the resected lesser metatarsal stumps. Continued rheumatologic follow-up is necessary for systemic disease control.
Summary of Key Literature and Guidelines
The evolution of rheumatoid forefoot reconstruction is well documented in orthopedic literature. Early procedures, such as the Clayton procedure (pan-metatarsal head resection including the first metatarsal) and the Mayo procedure, often resulted in a shortened, unstable medial column and high rates of recurrent deformity.
The shift towards preserving the medial column via first MTP arthrodesis was championed by Coughlin et al., whose long-term outcome studies demonstrated superior functional scores, better weight-bearing distribution, and higher patient satisfaction when the first ray was rigidly fused compared to resection arthroplasty. The arthrodesis provides a rigid medial buttress that prevents the lateral drift of the lesser toes.
In the modern era of biologic DMARDs, joint-preserving techniques for the lesser rays (such as Weil osteotomies combined with plantar plate repairs) have gained traction for patients with mild to moderate disease without severe articular destruction. Barouk and others have described the utility of metatarsal shortening osteotomies to restore the cascade without sacrificing the joint. However, for the classic, severe rheumatoid forefoot with dislocated, eroded MTP joints, the consensus remains that first MTP arthrodesis coupled with lesser metatarsal head resection represents the most reliable, durable, and definitive surgical solution.
Perioperative guidelines published jointly by the ACR and AAHKS provide critical algorithms for medication management, significantly reducing the incidence of postoperative surgical site infections while preventing acute systemic disease flares. Adherence to these guidelines, combined with meticulous surgical technique and rigid biomechanical principles, ensures optimal outcomes in this challenging patient population.
Clinical & Radiographic Imaging

























You Might Also Like