Pes Planus and Tarsal Coalition: A Comprehensive Surgical Guide
Key Takeaway
Tarsal coalition represents a congenital failure of mesenchymal segmentation, often presenting as rigid pes planus and secondary peroneal spasticity. While calcaneonavicular and talocalcaneal coalitions are most common, accurate diagnosis requires rigorous clinical and radiographic evaluation. This guide details the biomechanics, conservative management, and step-by-step surgical techniques—including bar resection with interposition and arthrodesis—to optimize functional outcomes in both adolescent and adult patients.
INTRODUCTION AND PATHOPHYSIOLOGY
Although tarsal coalition has historically been cited as the primary etiology of congenital rigid pes planus, this association requires nuanced clinical understanding. The presence of a tarsal coalition—particularly a calcaneonavicular coalition—does not uniformly result in a severe pes planus deformity. Many patients exhibit only slight heel valgus and minimal loss of the medial longitudinal arch, which frequently remain asymptomatic and are not the patient’s primary complaint. Furthermore, the deformity associated with tarsal coalition is not always entirely rigid. Calcaneonavicular coalitions, in particular, may permit sufficient subtalar motion to deceive the unwary examiner prior to definitive radiographic evaluation.
Despite these variations, the majority of symptomatic patients with tarsal coalition do present with a fixed hindfoot valgus of varying severity and a concomitant loss of the normal longitudinal arch. It is for this reason that tarsal coalition remains a cornerstone in the academic discussion of rigid pes planus.
Genetic and Embryologic Origins
The true incidence of tarsal coalition is widely considered to be greater than the traditionally quoted 1% of the general population, largely due to the high prevalence of asymptomatic cases.
Clinical Pearl: Tarsal coalition is an inherited condition, manifesting as a unifactorial disorder of autosomal dominant inheritance with nearly full penetrance.
Embryologically, the specific type of coalition represents a genetic mutation responsible for the failure of the primitive mesenchyme to segment properly during the development of the peritalar complex. This failure of cavitation leads to abnormal bridging between adjacent tarsal bones, which may present as:
* Synostosis: A complete bony bridge.
* Synchondrosis: A cartilaginous bridge.
* Syndesmosis: A fibrous bridge.
Symptomatic tarsal coalitions other than calcaneonavicular and talocalcaneal are exceedingly rare. Talonavicular coalition, while more common than calcaneocuboid, naviculocuboid, naviculocuneiform, or massive pan-tarsal coalitions, remains an uncommon clinical entity.
BIOMECHANICS AND THE "PERONEAL SPASTIC" PHENOMENON
Tarsal coalition, rigid pes planus, and peroneal muscle spasm are frequently grouped together under the historical diagnostic umbrella of "peroneal spastic pes planus." However, the term "spastic" is a misnomer.
The Mechanism of Peroneal Tightness
Peroneal spasm is not a true upper motor neuron spasticity; rather, it is an acquired or adaptive shortening of the muscle-tendon units of the peroneal musculature. When an examiner applies an inversion stress to the affected foot, it often produces an unsustained three-beat or four-beat clonus of the peroneal muscles. This is simply the stretch reflex of a chronically shortened muscle-tendon unit.
Surgical Warning: It must be emphatically stressed that peroneal muscle tightness is the result of the tarsal coalition, not the cause of the deformity.
According to Lapidus, the relaxed position of the subtalar joint is in valgus, which places the least biomechanical strain on the talocalcaneal interosseous ligament. In the presence of a coalition, the peroneal muscles are reflexively stimulated to evert the hindfoot, effectively "decompressing" the subtalar joint. Over time, this adaptive positioning becomes a fixed contracture.
Differential Diagnosis of Peroneal Spasm
Peroneal muscle tightness is not pathognomonic for tarsal coalition. It is observed in numerous other clinical disorders that irritate the subtalar joint complex. The differential diagnosis must include:
* Inflammatory Arthropathies: Rheumatoid arthritis or juvenile idiopathic arthritis.
* Trauma: Osteochondral fractures of the talus or calcaneus.
* Infection: Tuberculous, mycotic, or pyogenic infections within the subtalar joint.
* Neoplasm: Osteoid osteoma, osteochondroma, Trevor disease (dysplasia epiphysealis hemimelica), or fibrosarcoma adjacent to the subtalar joint.
RADIOGRAPHIC EVALUATION OF TARSAL COALITION
Accurate diagnosis relies heavily on high-quality, weight-bearing radiographic imaging. While CT and MRI have become the gold standards for complex peritalar anatomy, standard radiography remains the first-line diagnostic tool.
Talonavicular Coalition Imaging
Though rare, congenital talonavicular coalition presents with distinct radiographic features. The failure of segmentation between the talar head and the navicular is readily apparent on standard views.
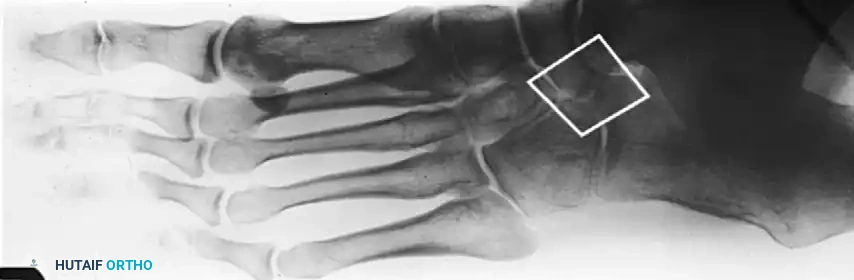
FIGURE 82-76 A: Congenital talonavicular tarsal coalition (Anteroposterior view).
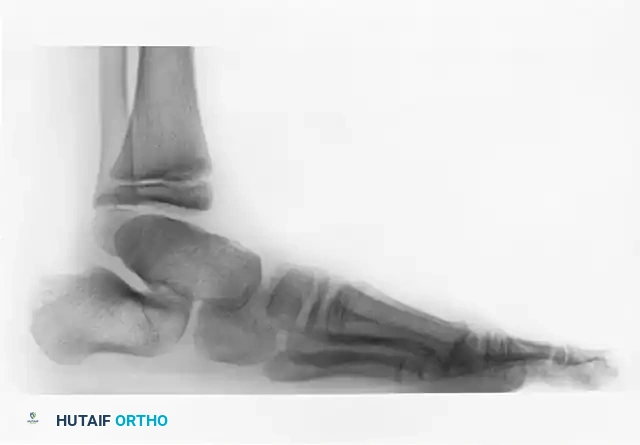
FIGURE 82-76 B: Congenital talonavicular tarsal coalition (Lateral view).
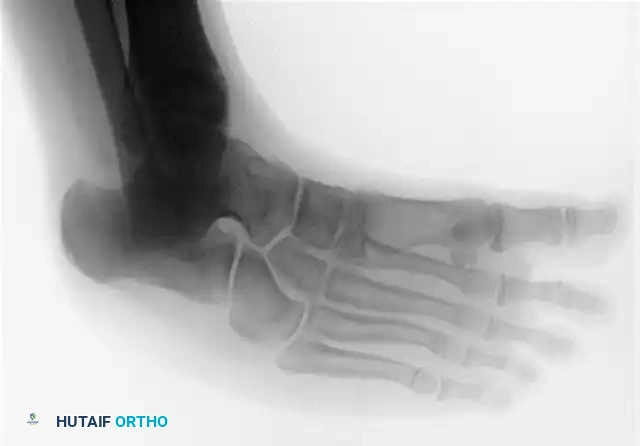
FIGURE 82-76 C: Congenital talonavicular tarsal coalition (Oblique view).
CALCANEONAVICULAR COALITION
Pathoanatomy and Ossification Timeline
Although the calcaneonavicular bar is present from birth, it does not ossify until the patient reaches 8 to 12 years of age. Prior to this period, the malleability of the cartilage surrounding the primary ossification centers of the peritalar complex absorbs mechanical stress, rendering significant symptoms rare.
As the cartilaginous precursor ossifies, hindfoot stiffness ensues. Consequently, the patient’s ability to withstand the repetitive stress of vigorous childhood and adolescent activities declines rapidly.
Clinical Pearl: Incomplete coalitions (cartilaginous or fibrous) are frequently more symptomatic than complete bony synostoses. This is due to the painful micromotion and micro-tearing that occurs at the syndesmotic or synchondrotic interface during weight-bearing activities.
Radiographic Diagnosis of Calcaneonavicular Coalition
The 45-degree lateral oblique radiograph is the most sensitive and specific plain film view for diagnosing a calcaneonavicular coalition, whether complete or incomplete.
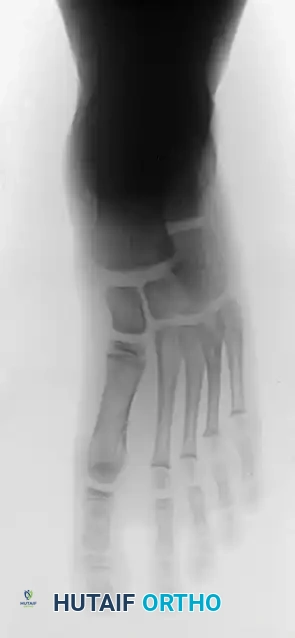
FIGURE 82-76 D: Calcaneonavicular incomplete tarsal coalition, demonstrating the classic "anteater nose" sign.
The abnormal bar typically runs from the anterior process of the calcaneus (just lateral to the anterior facet) dorsally and medially to the lateral and dorsolateral extra-articular surface of the navicular.
* Dimensions: The bar is usually 1.0 to 2.0 cm in length and 1.0 to 1.2 cm in width.
* Interface Characteristics: In a bar with a cartilaginous or fibrous interface, the adjacent bony margins appear irregular, sclerotic, and indistinct.
* Associated Findings: The talar head may appear small and underdeveloped. Notably, the dorsal talar "beaking" commonly seen in talocalcaneal coalitions is uncommon in isolated calcaneonavicular coalitions.
The "Pseudocoalition" Pitfall: In older adolescents and adults, a prominent anterior tuberosity of the calcaneus may be radiographically confused with an incomplete calcaneonavicular coalition. This "pseudocoalition" must be correlated with clinical examination (specifically assessing subtalar motion) and additional lateral oblique radiographs taken at varying angles. Standard tomography and CT are rarely required to diagnose a standard calcaneonavicular coalition but are invaluable if a concomitant talocalcaneal coalition is suspected.
Clinical Presentation
Patients typically present with:
* Vague dorsolateral foot pain centering around the sinus tarsi.
* Difficulty walking on uneven surfaces (due to loss of subtalar inversion/eversion).
* Premature foot fatigue.
* An occasional painful limp.
Most commonly, the patient is an active adolescent. Physical examination may or may not show significant reduction of subtalar motion or flattening of the longitudinal arch; thus, a high index of suspicion is mandatory. In unilateral cases, careful comparative examination of subtalar motion almost always reveals a definite restriction on the affected side. Tenderness is usually localized to the sinus tarsi and directly along the anatomical course of the bar.
CONSERVATIVE MANAGEMENT
Although a calcaneonavicular coalition may not become symptomatic until adulthood, the peak age of presentation is 8 to 12 years, corresponding directly to the ossification of the cartilaginous precursor.
Patient and Family Education
Education is the first line of treatment. Parents must be informed regarding:
1. The congenital and hereditary nature of the disorder.
2. The biomechanical reason for the delay in symptoms until adolescence.
3. The fact that many coalitions remain asymptomatic throughout life.
Immobilization and Orthotics
A trial of reduced activity and/or cast immobilization is highly recommended before considering surgical intervention.
* Casting: A short-leg walking cast applied for 4 to 6 weeks can render a patient asymptomatic for varying periods, sometimes indefinitely. Intermittent casting for short durations, interspersed with lengthy intervals of non-casting, may be sufficient.
* Orthotics: Following cast removal, a custom-molded, firm medial longitudinal arch support or a University of California Biomechanics Laboratory (UCBL) orthosis can help control hindfoot valgus and reduce stress across the peritalar complex.
Surgical Warning: The mere radiographic presence of a tarsal coalition is not an absolute indication for surgery. If patients reach their twenties with minimal symptoms, they frequently remain asymptomatic for life. Surgery is reserved for those who fail conservative management and are unable to participate in desired activities.
SURGICAL MANAGEMENT: CALCANEONAVICULAR BAR RESECTION
If a rigorous trial of casting and orthotic management fails to relieve symptoms, surgical intervention is indicated. The most commonly accepted primary surgical treatment for an isolated, symptomatic calcaneonavicular coalition in an adolescent without advanced degenerative changes is resection of the calcaneonavicular bar with interposition of muscle or fat.
Preoperative Planning and Indications
- Indications: Symptomatic calcaneonavicular coalition failing conservative therapy; absence of advanced degenerative arthritis in the subtalar or talonavicular joints; absence of a secondary talocalcaneal coalition.
- Adult Considerations: The literature is conflicting regarding the efficacy of bar excision in adults. While some studies report good results in 68% to 92% of adult patients, others report recurrence rates up to 67% and progressive osteoarthritic changes in 96%. However, many modern authors report excellent restoration of subtalar motion and functional improvement after aggressive resection and interposition in adults, provided joint arthrosis is minimal.
Surgical Technique: Step-by-Step
1. Positioning and Anesthesia
- The patient is placed in the lateral decubitus position or supine with a substantial bump under the ipsilateral hip to internally rotate the leg, providing excellent exposure to the lateral aspect of the foot.
- A well-padded thigh or calf tourniquet is applied for hemostasis.
- Regional anesthesia (popliteal block) combined with general anesthesia is preferred for optimal postoperative pain control.
2. Surgical Approach (Ollier Incision)
- A transverse or slightly oblique lateral incision (Ollier approach) is made over the sinus tarsi. The incision begins just inferior to the lateral malleolus and extends distally and medially toward the talonavicular joint.
- Superficial Dissection: Careful subcutaneous dissection is performed to identify and protect the intermediate dorsal cutaneous nerve (a branch of the superficial peroneal nerve) dorsally, and the sural nerve branches plantarly.
3. Deep Dissection and Exposure
- The inferior extensor retinaculum is incised and tagged for later repair.
- The muscle belly of the Extensor Digitorum Brevis (EDB) is identified. The EDB is sharply elevated from its origin on the lateral and anterior calcaneus and reflected distally.
- This reflection exposes the sinus tarsi, the anterior process of the calcaneus, the calcaneocuboid joint, and the lateral aspect of the navicular.
4. Identification and Resection of the Bar
- The calcaneonavicular bar is visually and palpably identified. In incomplete coalitions, the fibrous or cartilaginous interface may appear as a thickened, irregular cleft.
- Using a combination of osteotomes, rongeurs, and a high-speed burr, the bar is resected.
- Critical Step: The resection must be generous. A rectangular block of bone measuring at least 1.0 to 1.5 cm in width must be removed to prevent recurrence. The resection should extend from the anterior process of the calcaneus to the lateral margin of the navicular.
- The surgeon must ensure that the resection does not inadvertently violate the articular surfaces of the adjacent talonavicular or calcaneocuboid joints.
- Following resection, the subtalar joint is taken through a full range of motion. A dramatic improvement in inversion and eversion should be immediately palpable on the operating table.
5. Interposition to Prevent Recurrence
To prevent osteogenic recurrence across the resected gap, biological interposition is mandatory.
* Muscle Interposition (EDB): The previously elevated EDB muscle belly is mobilized and rotated into the defect. It is secured in place using absorbable sutures passed through drill holes in the navicular or cuboid, or anchored to the deep plantar fascia.
* Fat Interposition: Alternatively, a free fat graft (harvested from the gluteal fold or local subcutaneous tissue) can be packed tightly into the defect.
* Bone wax may be applied to the raw cancellous bone surfaces of the calcaneus and navicular as an adjunct to prevent hematoma ossification.
6. Closure
- The inferior extensor retinaculum is loosely approximated over the EDB (if not fully transposed).
- The subcutaneous tissue and skin are closed in layers.
- A sterile compressive dressing and a well-padded short-leg splint are applied in a neutral position.
SALVAGE PROCEDURES: ARTHRODESIS
In cases where bar resection is contraindicated—such as in the presence of advanced peritalar osteoarthritis, massive pan-tarsal coalitions, failed prior resections, or severe, rigid, long-standing deformity in older adults—arthrodesis is the treatment of choice.
Subtalar Arthrodesis
Isolated subtalar (talocalcaneal) arthrodesis may be indicated if the degenerative changes are strictly confined to the subtalar joint, though this is less common in the setting of a primary calcaneonavicular coalition.
Triple Arthrodesis
Triple arthrodesis (fusion of the subtalar, talonavicular, and calcaneocuboid joints) remains the most frequently recommended salvage procedure.
* Biomechanics: It definitively eliminates painful peritalar motion, corrects the fixed hindfoot valgus, and restores a stable, plantigrade foot.
* Technique Overview: The articular cartilage of all three joints is aggressively denuded. The deformity is corrected by manipulating the transverse tarsal joint and subtalar joint into neutral alignment. Rigid internal fixation is achieved using large-fragment cannulated screws or specialized midfoot plating systems. Bone grafting (autograft or allograft) is frequently utilized to fill structural voids and promote robust osteogenesis.
POSTOPERATIVE PROTOCOL AND REHABILITATION
Following Bar Resection
- Phase I (0-3 Weeks): The patient is maintained strictly non-weight-bearing in a short-leg cast or rigid splint to allow the soft tissues and interpositional graft to heal.
- Phase II (3-6 Weeks): The cast is removed. The patient is transitioned to a controlled ankle motion (CAM) boot. Progressive weight-bearing is initiated. Aggressive physical therapy begins, focusing heavily on active and active-assisted subtalar inversion and eversion to prevent scar tissue tethering.
- Phase III (6+ Weeks): Transition to regular footwear, often with a supportive orthotic. Return to sports and high-impact activities is permitted once full, painless range of motion and baseline strength are achieved (typically 3 to 4 months postoperatively).
Following Arthrodesis
Recovery is significantly more protracted. Patients require 6 to 8 weeks of strict non-weight-bearing immobilization, followed by progressive weight-bearing in a CAM boot until radiographic union is confirmed (typically 10 to 12 weeks). Physical therapy focuses on strengthening the extrinsic foot musculature and optimizing gait mechanics, as peritalar motion is permanently eliminated.
CONCLUSION
The management of pes planus secondary to tarsal coalition requires a profound understanding of peritalar biomechanics and the natural history of the disease. While conservative measures remain the first line of defense, meticulous surgical resection of the calcaneonavicular bar with biological interposition offers excellent functional restoration for the active patient. In cases of advanced arthrosis or rigid adult deformity, triple arthrodesis remains a powerful and reliable tool to restore a painless, plantigrade foot. Thorough preoperative imaging and precise surgical execution are paramount to minimizing recurrence and optimizing long-term patient outcomes.
📚 Medical References
- Conway JJ, Cowell HR: Tarsal coalition: clinical signifi cance and radiographic demonstration, Radiology 92:799, 1969.
- Cowell HR: Tarsal coalition: review and update, Instr Course Lect 31:264, 1982.
- Cowell HR, Elener V: Rigid painful fl atfoot secondary to tarsal coalition, Clin Orthop Relat Res 177:54, 1983.
You Might Also Like
