Internal Fixation of Fifth Metatarsal Fractures: A Masterclass Surgical Guide
Key Takeaway
Internal fixation of fifth metatarsal fractures, particularly Jones and diaphyseal stress fractures, requires precise intramedullary screw placement. This technique provides robust biomechanical stability, facilitating early rehabilitation in high-demand athletes. Critical steps include protecting the sural nerve, achieving an optimal starting trajectory parallel to the hindfoot, and addressing medullary sclerosis with inlay bone grafting in cases of nonunion to ensure reliable osseous consolidation.
INTRODUCTION TO FIFTH METATARSAL FRACTURES
Fractures of the fifth metatarsal represent a complex spectrum of injuries that demand a nuanced understanding of foot biomechanics, vascular anatomy, and patient-specific functional demands. Historically categorized by Lawrence and Botte into three distinct anatomic zones, fractures occurring at the metaphyseal-diaphyseal junction (Zone 2, the classic Jones fracture) and the proximal diaphysis (Zone 3, stress fractures) are notoriously prone to delayed union and nonunion. This vulnerability is primarily attributed to a vascular "watershed" area and the immense repetitive tensile forces exerted by the plantar fascia and peroneus brevis during the heel-off phase of gait.
For high-demand patients, professional athletes, and cases of established nonunion, conservative management often yields unacceptable rates of clinical failure. Consequently, internal fixation with a solid or cannulated intramedullary malleolar screw has become the gold standard. This masterclass details the evidence-based surgical techniques, anatomical considerations, and postoperative protocols required to achieve reliable osseous consolidation.
SURGICAL ANATOMY AND BIOMECHANICS
The Vascular Watershed
The proximal fifth metatarsal receives its blood supply from three primary sources: the nutrient artery, metaphyseal perforators, and periosteal vessels. The nutrient artery enters the medial cortex in the middle third of the diaphysis and sends branches proximally. The metaphyseal vessels supply the tuberosity. Between these two distinct vascular networks lies a relative avascular zone at the metaphyseal-diaphyseal junction—the exact location of the Jones fracture. Disruption of this tenuous blood supply during injury significantly impairs the biologic healing potential.
Neurologic Considerations: The Sural Nerve
As demonstrated by Donley et al., the surgical approach to the base of the fifth metatarsal places the sural nerve at significant risk. The sural nerve bifurcates into a dorsal and a straight lateral branch. The dorsolateral branch, in particular, courses dangerously close to the optimal percutaneous insertion point for an intramedullary screw. Iatrogenic injury or entrapment of this nerve can lead to debilitating postoperative neuromas, which often overshadow the successful union of the fracture.
⚠️ Surgical Warning: Sural Nerve Protection
Never use sharp dissection down to the bone. Incise the skin only, followed by meticulous blunt dissection using a hemostat to spread the subcutaneous tissues down to the periosteum. The dorsal and lateral branches of the sural nerve must be directly visualized or gently swept away from the drill portal.
PREOPERATIVE PLANNING AND IMAGING
Standard weight-bearing anteroposterior (AP), lateral, and oblique radiographs of the foot are mandatory. The oblique view is particularly useful for profiling the fracture line at the metaphyseal-diaphyseal junction.
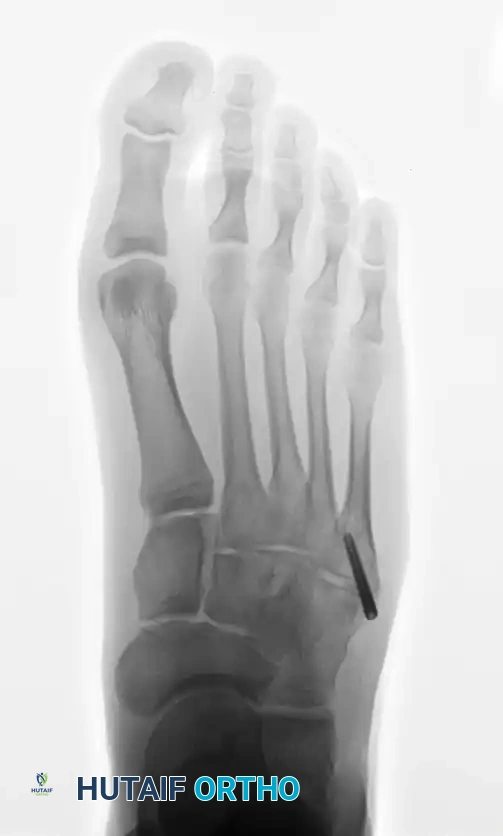
In cases of delayed union or nonunion, advanced imaging such as a Computed Tomography (CT) scan may be warranted to assess the extent of medullary sclerosis and to precisely measure the canal diameter. The medullary canal of the fifth metatarsal is not perfectly straight; it exhibits a lateral and plantar bow. Preoperative templating is critical to select a screw diameter that achieves cortical purchase without causing iatrogenic lateral cortical blowout.
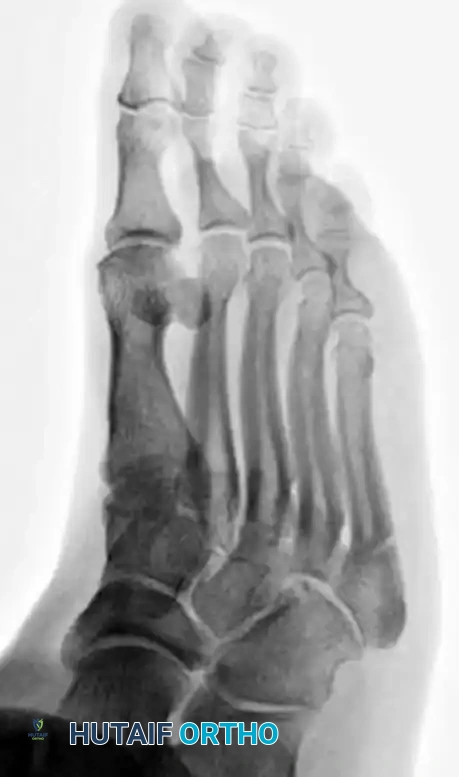
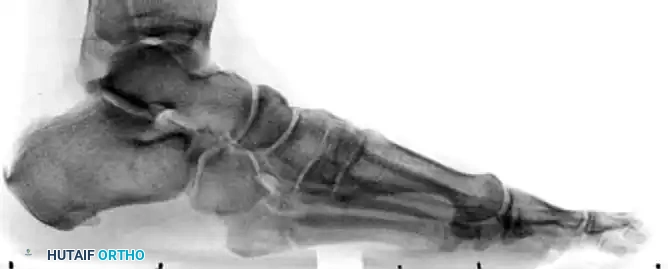
SURGICAL TECHNIQUE: INTRAMEDULLARY SCREW FIXATION
The technique described herein builds upon the foundational principles established by Kavanaugh, Brower, and Mann, optimized for modern cannulated and solid screw systems.
1. Patient Positioning and Anesthesia
The patient is placed in the lateral decubitus position, or supine with a large bump under the ipsilateral hip to internally rotate the leg, bringing the lateral border of the foot directly toward the ceiling. A radiolucent table is mandatory to allow unobstructed fluoroscopic imaging in multiple planes. A thigh or calf tourniquet is applied.
2. Surgical Approach
- Incision: Make a 1.5 to 2.0 cm longitudinal incision starting at the tip of the fifth metatarsal tuberosity and extending proximally.
- Dissection: Expose the base of the fifth metatarsal on its dorsolateral surface. Incise the skin only. Observe and protect the two branches of the sural nerve (one dorsal and one straight lateral) that are highly vulnerable in this field.
- Peroneus Brevis Management: The tendon of the peroneus brevis inserts onto the tuberosity and may obscure the ideal starting portal. If necessary, longitudinally split the tendon or elevate a small dorsal portion of it off the bone to gain clear access to the starting point.
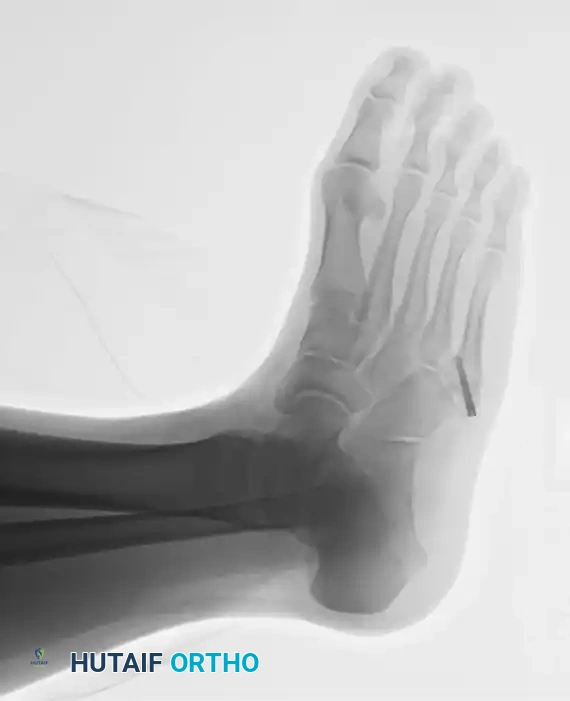
3. Establishing the Starting Point and Trajectory
Achieving the correct starting point is the most critical step of the operation. Because of the lateral bow of the metatarsal, starting directly on the tip of the tuberosity will result in a trajectory that breaches the medial cortex.
- The "High and Inside" Rule: The optimal starting point is slightly dorsal and medial to the anatomic center of the tuberosity.
- Guidewire Insertion: Use a stout guide wire (typically 1.4mm or 1.6mm) to find the medullary canal. This can be technically demanding. The wire must lie almost parallel to the hindfoot and the plantar aspect of the foot.
- Fluoroscopic Confirmation: Advance the wire under multi-planar fluoroscopy. Ensure the wire passes the fracture site and sits centrally within the narrowest portion of the diaphysis (the isthmus).
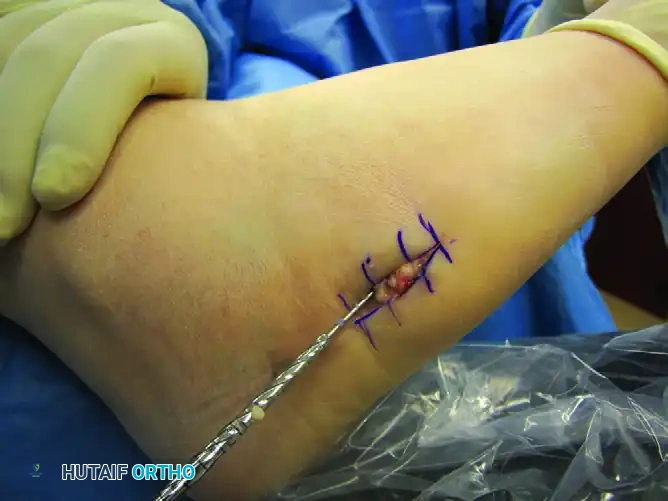
💡 Clinical Pearl: Avoiding Cortical Blowout
If the guidewire meets hard resistance before crossing the fracture, do not force it. You are likely abutting the medial or plantar cortex. Withdraw, adjust your starting point slightly more dorsal and medial, and redirect.
4. Drilling and Tapping
- Once the guidewire is perfectly positioned, drive a cannulated drill bit into the medullary canal.
- Confirm the drill's location via AP and lateral radiographs. The drill should cross the fracture site and engage the diaphyseal cortex without breaching it.
- If using a solid screw system, the canal is drilled and tapped over the wire trajectory. Tapping is highly recommended in young athletes with dense cortical bone to prevent screw breakage during insertion.
5. Screw Selection and Insertion
- Measurement: Estimate the length of the screw from the intraoperative radiographs. The screw must be long enough to bypass the fracture site and engage the diaphyseal isthmus, ensuring all threads are distal to the fracture line to allow for interfragmentary compression.
- Insertion: Place the screw over the guide wire. A 4.5mm to 5.5mm partially threaded screw is typically utilized, depending on the patient's canal diameter.
- Head Burial: It is imperative to countersink or bury the head of the screw into the tuberosity. A prominent screw head will cause severe irritation to the peroneus brevis tendon and overlying skin, often necessitating a second surgery for hardware removal.
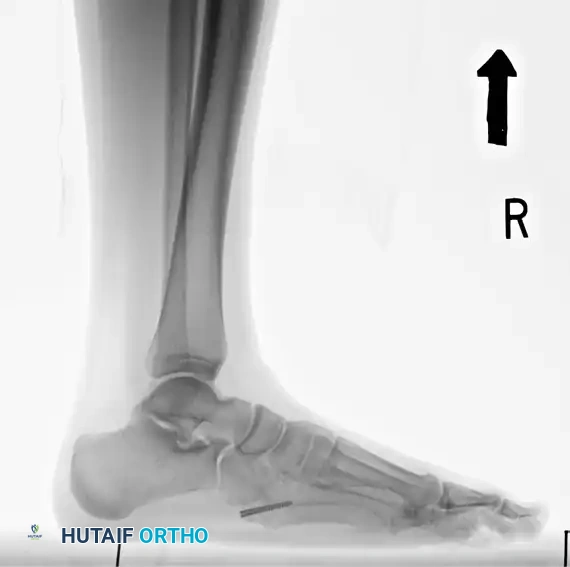
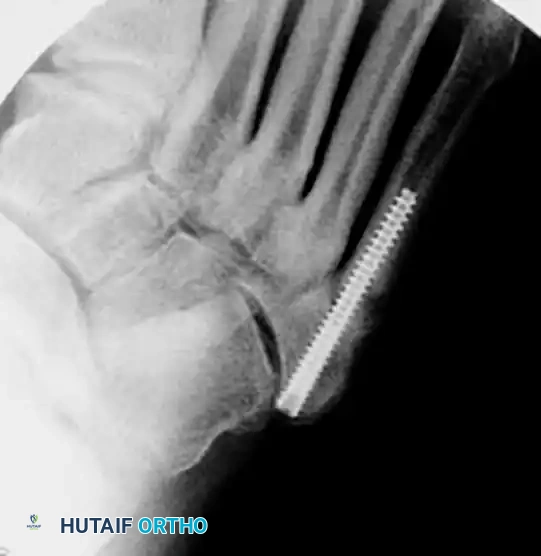
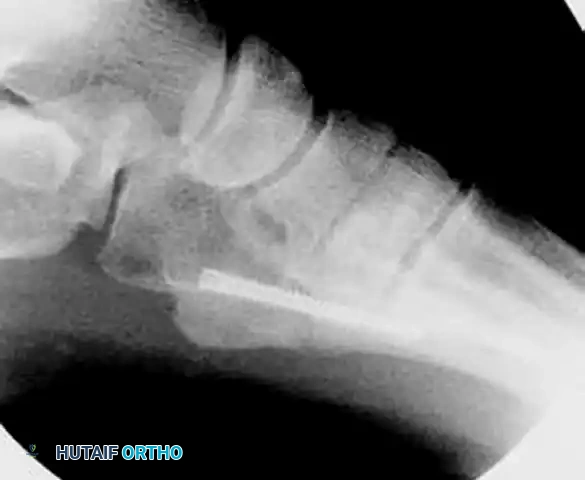
6. Final Verification and Closure
- Verify final screw placement, fracture reduction, and compression with orthogonal radiographs.
- Thoroughly irrigate the wound to remove bone debris.
- Close the subcutaneous tissue and skin meticulously.
MANAGEMENT OF NONUNIONS: THE INLAY BONE GRAFT TECHNIQUE
While acute fractures respond excellently to intramedullary screw fixation, chronic nonunions present a distinct biologic challenge. Exposing a nonunion and applying a small cancellous bone graft may or may not enhance union. However, if profound cortical thickening and medullary sclerosis are present, biologic augmentation is mandatory.
Pathophysiology of Sclerosis
A consistent finding in the presence of a chronic nonunion of this fracture is the complete obliteration of the medullary canal by dense, sclerotic bone along the margins of the fracture. Torg et al. suggested that the tendency of this fracture toward nonunion, delayed union, or refracture after healing is the direct result of this poorly organized, sclerotic bone, which acts as a mechanical and biologic barrier, impairing healing and the ultimate tensile strength of the union.
The Torg Inlay Graft Technique
To address this, Torg et al. described a highly effective technique to reestablish the continuity of the medullary canal and facilitate healing:
1. Approach: A longitudinal incision is made directly over the fracture site.
2. Resection: A rectangular window of bone (approximately 0.5 cm x 1.5 cm) is outlined across the nonunion site using a microsaw or fine osteotomes.
3. Canal Reconstitution: The sclerotic bone plug obliterating the medullary canal is meticulously removed using a high-speed burr or curettes until healthy, bleeding cancellous bone is encountered proximally and distally.
4. Graft Harvest and Inset: A corticocancellous inlay bone graft is harvested from the proximal or distal anteromedial tibia. The graft is contoured to precisely match the dimensions of the created window and is tamped into place. The cortical surface of the graft sits flush with the metatarsal cortex, while the cancellous portion bridges the medullary defect.
5. Fixation: This inlay graft can be utilized in isolation or, more commonly in modern practice, combined with intramedullary screw fixation for optimal biomechanical and biologic synergy.
DISTAL FIFTH METATARSAL FRACTURES (DANCER'S FRACTURE)
While proximal fractures dominate the literature, spiral fractures of the distal fifth metatarsal diaphysis and neck are common, occurring frequently in ballet dancers and professional athletes.
Mechanism of Injury
The mechanism of injury is almost exclusively rotational. It occurs when the athlete rolls over on the outer border of the foot while standing on the ball of the foot with the ankle fully plantar flexed—the classic demi-pointe position in ballet.
Evidence-Based Management
Unlike proximal Zone 2 and 3 fractures, distal spiral fractures possess a robust blood supply and a vast periosteal envelope. A comprehensive study of dancers with this injury, treated both operatively and nonoperatively, found that even in the presence of displacement, conservative management yields excellent outcomes.
Treatment typically consists of cast immobilization or symptomatic treatment with rigid bandaging and full weight bearing as tolerated. The literature reports that this approach has no long-term negative consequences. In the aforementioned study, there was only one delayed union and one refracture, both of which subsequently healed without further intervention. All ballet dancers returned to professional performance without limitations, and no patient reported pain with performance at long-term follow-up. Operative intervention for these distal fractures is strictly reserved for severe open injuries or extreme displacement threatening the soft tissue envelope.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol following intramedullary screw fixation of a proximal fifth metatarsal fracture must balance the need for rigid immobilization with the desire for early functional rehabilitation.
- Phase I: Immediate Postoperative (Weeks 0-2)
- A well-padded, short-leg, nonwalking cast or rigid fracture boot extending to the toes is applied in the operating room.
- The patient is strictly non-weight-bearing (NWB) on crutches or a knee scooter.
-
Elevation and cryotherapy are emphasized to minimize edema and protect the incision.
-
Phase II: Early Weight Bearing (Weeks 2-6)
- At 2 weeks postoperatively, sutures are removed.
- Weight bearing in a rigid cast or CAM boot may be initiated, progressing from partial to full weight bearing as tolerated.
-
Active range of motion (ROM) of the ankle and toes is encouraged out of the boot.
-
Phase III: Functional Rehabilitation (Weeks 6-10)
- The patient transitions to a stiff-soled shoe or a shoe with a carbon fiber insert.
-
Physical therapy focuses on peroneal strengthening, proprioception, and gait normalization.
-
Phase IV: Return to Play (Weeks 10-12+)
- Return to competitive sports is strictly discouraged until the fracture has healed both clinically (absence of point tenderness at the fracture site) and radiographically (bridging trabeculae across three out of four cortices).
- This consolidation process usually takes 10 to 12 weeks. Premature return to high-impact activities, especially in athletes with residual medullary sclerosis, significantly increases the risk of catastrophic hardware failure and refracture.
You Might Also Like
