Dorsal Closing Wedge Osteotomy of the Metatarsals for Intractable Plantar Keratosis
Key Takeaway
Intractable plantar keratosis often results from altered forefoot biomechanics and localized metatarsal overload. The dorsal closing wedge osteotomy is a powerful joint-sparing procedure designed to elevate the offending metatarsal head, thereby redistributing plantar pressures. This comprehensive guide details the precise surgical technique, anatomical considerations, and fixation strategies required to achieve optimal clinical outcomes while minimizing complications such as transfer metatarsalgia or nonunion.
Introduction to Intractable Plantar Keratosis (IPK)
Intractable plantar keratosis (IPK) represents a focal, hyperkeratotic lesion on the plantar aspect of the foot, typically occurring beneath one or more of the lesser metatarsal heads. Unlike diffuse callosities, an IPK is a discrete, highly symptomatic lesion driven by localized mechanical overload during the stance phase of the gait cycle. This pathologic pressure distribution is frequently the result of a structurally plantarflexed metatarsal, an excessively long metatarsal, or retrograde buckling from a hammertoe deformity.
When conservative measures—such as custom orthoses with metatarsal offloading pads, callus debridement, and footwear modifications—fail to provide durable relief, surgical intervention is indicated. The dorsal closing wedge osteotomy of the proximal metatarsal is a highly effective, joint-sparing procedure designed to elevate the offending metatarsal head, thereby normalizing the metatarsal cascade and redistributing plantar forefoot pressures.
Biomechanics and Surgical Anatomy
A profound understanding of forefoot osteology and the neurovascular topography of the dorsum of the foot is mandatory to execute this procedure safely and effectively.
The Metatarsal Cascade and the "Keystone" Second Metatarsal
The second metatarsal is the longest and most rigidly fixed ray in the foot, acting as the keystone of the Lisfranc articulation.
* Proximal Articulation: The base of the second metatarsal articulates with the intermediate cuneiform.
* Recessed Anatomy: This articulation is recessed proximally by approximately 0.5 cm relative to the third metatarsal base and 1.0 cm relative to the first metatarsal base. This mortise-like configuration confers immense structural stability but makes surgical exposure technically demanding.
Osteology of the Metatarsal Base
The osteology of the base of the second metatarsal is highly specific. Its plantar surface is shaped remarkably like the keel of a boat.
* The apex of this plantar keel is situated slightly lateral to the midline of the dorsal base.
* The dorsal-to-plantar height of the base of the second metatarsal is approximately 1.5 cm.
Understanding this "keel" geometry is critical during the osteotomy to ensure the plantar hinge remains intact while allowing symmetric dorsal closure.
Neurovascular Structures at Risk
The dorsal approach to the lesser metatarsals traverses a complex neurovascular network.
* Superficial Peroneal Nerve: Branches of the intermediate dorsal cutaneous nerve cross the surgical field superficially.
* Deep Peroneal Nerve & Dorsalis Pedis Artery: These structures course through the first intermetatarsal space and dive plantarly between the first and second metatarsal bases. Aggressive deep dissection or errant retractor placement on the medial aspect of the second metatarsal base can result in catastrophic vascular injury or debilitating neuromas.
* Extensor Hallucis Brevis (EHB): The muscle belly of the EHB crosses obliquely over the base of the second and third metatarsals.
Surgical Warning: Incise only the skin during the initial approach. The superficial peroneal nerve branches, the extensor hallucis brevis, the deep peroneal nerve, and the accompanying dorsalis pedis artery may all be encountered or compromised if deep dissection is performed hastily.
Preoperative Clinical and Radiographic Evaluation
A meticulous preoperative assessment is required to confirm that the IPK is driven by a structural metatarsal abnormality rather than a primary dermatologic condition (e.g., verruca plantaris).
Standard weight-bearing radiographs of the foot—including dorsoplantar (DP), lateral, and oblique views—must be obtained. These views allow the surgeon to assess the metatarsal parabola, evaluate for concomitant deformities (such as hallux valgus or bunionettes), and measure critical angles.
Evaluating the Lateral Column: The Bunionette Deformity
In many patients presenting with forefoot overload, a splay foot or bunionette deformity may coexist, altering the global biomechanics of the forefoot. The lateral prominence of the fifth metatarsal head must be evaluated.

Figure 83-38 A and B: Clinical presentation of a bunionette with metatarsus quintus valgus and fifth toe varus.
Measurement of the 4-5 Intermetatarsal Angle (4-5 IMA) is standard practice. This angle is formed by two lines that bisect the diaphyseal shafts of the fourth and fifth metatarsals.
* Normal 4-5 IMA: Less than 6.5 to 8 degrees (Average is 6.5 degrees in normal feet).
* Pathologic 4-5 IMA: Averages 9.6 degrees in feet with a symptomatic bunionette.
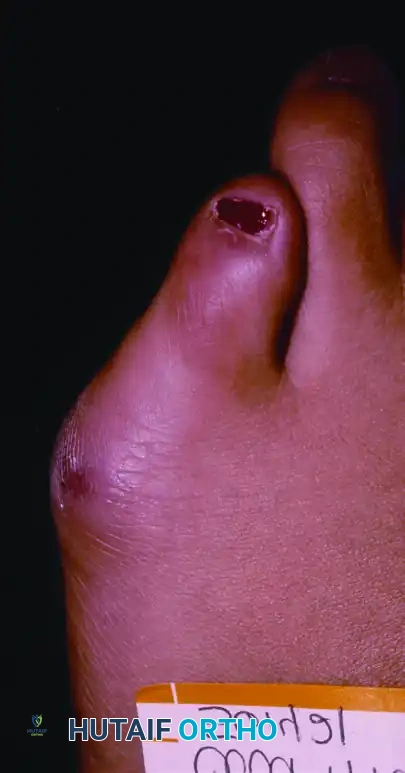
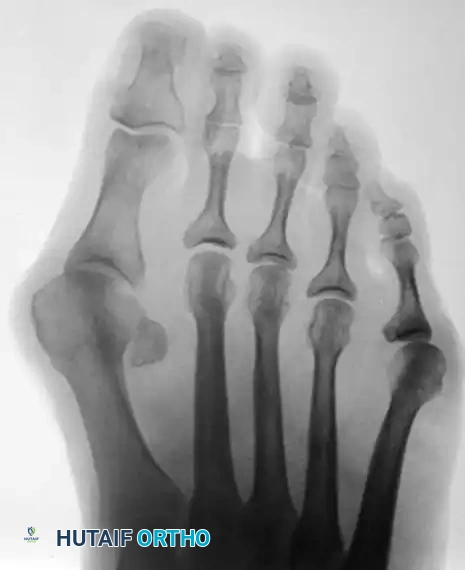
Figure 83-39: Bunionette–hallux valgus–splay foot complex. Note the lateral angulation of the shaft of the fifth metatarsal at the distal third (arrows).
Bunionettes are classified based on these weight-bearing radiographs to guide concurrent surgical decision-making:
* Type I: Enlargement of the fifth metatarsal head or a prominent lateral exostosis.
* Type II: Lateral bowing of the fifth metatarsal shaft with a normal 4-5 IMA.
* Type III: An abnormally widened 4-5 IMA (divergent fifth metatarsal).
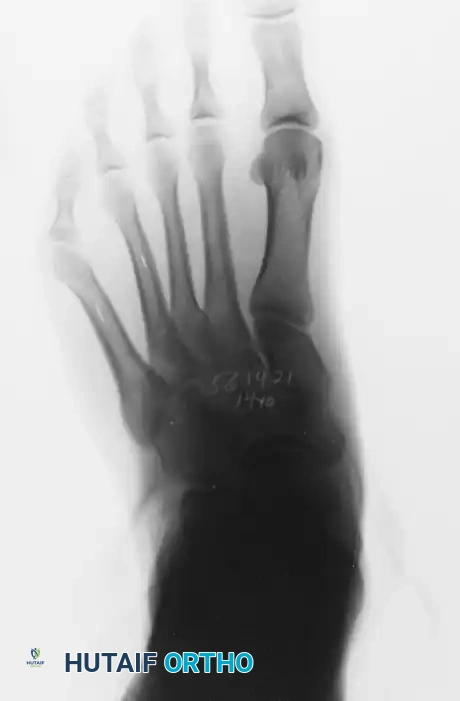
Figure 83-41: Weight-bearing radiographic classification of bunionette deformities.
Step-by-Step Surgical Technique: Dorsal Closing Wedge Osteotomy
The following technique describes the procedure for an IPK located beneath the second metatarsal head, which is the most common anatomical site for this pathology.
1. Anesthesia and Hemostasis
- Administer an ankle block regional anesthetic. This provides excellent intraoperative hemostasis (when combined with a tourniquet) and robust postoperative analgesia.
- Apply an Esmarch wrap to exsanguinate the foot up to the ankle level, securing it to function as an ankle tourniquet.
2. Incision and Exposure
- Begin the longitudinal incision 1 cm proximal to the articulation of the second metatarsal with the intermediate cuneiform.
- Continue the incision distally over the dorsal shaft of the second metatarsal for approximately 3 cm.
- Clinical Pearl: The tarsometatarsal articulation is easily palpable by lifting up and down on the second metatarsal head while simultaneously palpating the base of the metatarsal.
- Superficial Dissection: Incise just the skin. Carefully bluntly dissect the subcutaneous tissues to identify and retract branches of the superficial peroneal nerve.
- Retract the extensor tendons laterally or medially depending on the exact exposure needed, taking great care to protect the deep peroneal nerve and dorsalis pedis artery situated medially.
- Note: If the IPK is beneath the third or fourth metatarsal, the same incision placed more laterally is significantly less anatomically encumbered by critical neurovascular structures.
- Identify the tarsometatarsal joint capsule and perform a limited subperiosteal dissection to expose the proximal metatarsal metaphysis.
3. Executing the Osteotomy
- Using a straight needle or a marking pen under fluoroscopic guidance, measure exactly 6 to 7 mm distal to the joint line. Score the dorsal bone at this precise point.
- Utilize a microsagittal power saw equipped with a 4-mm blade (or a sharp osteotome) to create the osteotomy.
- The Wedge Resection: Remove a dorsal wedge of bone exactly 2 mm wide.
- The Plantar Hinge: It is imperative not to complete the osteotomy through the plantar cortex. Penetrate the plantar cortex just enough to weaken it, allowing the wedge to be closed by applying upward (dorsal) pressure on the second metatarsal head. This creates a greenstick fracture of the plantar cortex, which acts as a stabilizing tension-band hinge.
Biomechanical Pearl: The "Keel" Cut
Because the plantar surface of the second metatarsal base is shaped like a boat's keel with its apex slightly lateral to the midline, a straight dorsal-to-plantar cut may inadvertently completely sever the medial plantar cortex while leaving the lateral cortex too thick to hinge. To accommodate this anatomy, aim the saw blade slightly lateral (10 to 20 degrees) when making the dorsal-to-plantar cut.
4. Closure of the Osteotomy and Fixation
- Apply firm dorsal pressure to the plantar aspect of the metatarsal head to close the dorsal wedge. Ensure bone-on-bone apposition at the osteotomy site.
- Fixation Options: The osteotomy must be rigidly held to prevent dorsal malunion or nonunion.
- 2.7-mm Cortical Lag Screw (Preferred): If a screw is utilized, drill the near (dorsal) cortex before completing the osteotomy to prevent displacement. Place the screw in a dorsomedial to plantar-lateral trajectory. This specific vector ensures maximum bony purchase across the thickest portion of the plantar "keel."
- Crossed Kirschner Wires: Alternatively, two crossed 0.045-inch or 0.062-inch K-wires can be used to stabilize the osteotomy.
- Confirm the elevation of the metatarsal head and the position of the hardware using intraoperative fluoroscopy.
5. Closure
- Deflate and remove the Esmarch tourniquet wrap.
- Obtain meticulous hemostasis using bipolar electrocautery.
- Close the periosteum and extensor retinaculum with absorbable sutures, followed by standard skin closure.
- Apply a soft, sterile compression dressing.
Postoperative Care and Rehabilitation Protocol
Strict adherence to postoperative weight-bearing restrictions is critical, as the proximal metaphysis of the lesser metatarsals is susceptible to delayed union or nonunion due to watershed vascularity and high bending moments during gait.
- Weeks 0 to 3: The patient is placed in a short-leg cast extending beyond the toes. Strict non-weight-bearing (NWB) is enforced.
- Weeks 3 to 6: The patient may transition to partial weight-bearing (PWB) in the cast or a rigid fracture boot, depending on radiographic progression.
- Week 6: Obtain weight-bearing radiographs. If clinical and radiographic union is apparent, the patient is transitioned to a stiff-soled postoperative shoe and may begin progressive weight-bearing as tolerated.
- Delayed Union: If union is not definitively apparent at 6 weeks, a short-leg walking cast or rigid boot must be worn for an additional 4 weeks. Complete radiographic union may require 3 to 5 months.
Alternative Pathology: Intractable Keratosis Beneath the Tibial Sesamoid
While lesser metatarsal IPKs are managed with the dorsal closing wedge osteotomy described above, an IPK located beneath the first metatarsophalangeal joint—specifically under the tibial sesamoid—requires a different anatomical approach.
The tibial sesamoid bears a massive load during the terminal stance phase. When a localized, intractable keratosis develops directly beneath it, conservative offloading is notoriously difficult.
Surgical Options for Tibial Sesamoid IPK
- Sesamoidectomy or Plantar Skiving (Mann and DuVries Technique):
- This involves either total excision of the tibial sesamoid or surgically "skiving" (shaving off) its plantar half to reduce its prominent profile.
- Caution: Total tibial sesamoidectomy carries a risk of iatrogenic hallux valgus due to the destabilization of the medial head of the flexor hallucis brevis.
- First Metatarsal Dorsal Closing Wedge Osteotomy:
- An alternative, joint-sparing treatment is a proximal dorsal closing wedge osteotomy of the first metatarsal.
- A 2 to 3 mm dorsal wedge is removed from the proximal metaphysis, and the osteotomy is stabilized with pin or screw fixation. This elevates the entire first ray, decompressing the sesamoid apparatus.
Postoperative Care for First Ray Procedures:
Regardless of whether a sesamoidectomy or a first metatarsal osteotomy is performed, a short-leg cast is recommended for a total of 6 weeks. The patient remains non-weight-bearing for the first 3 weeks, with partial weight-bearing allowed in the final 3 weeks prior to transitioning to a stiff-soled shoe.
Complications and Pitfalls
- Transfer Metatarsalgia: The most common complication of any metatarsal elevation osteotomy. If the 2-mm wedge over-elevates the second metatarsal, the load is transferred to the adjacent third metatarsal head, creating a new, iatrogenic IPK. Precise preoperative templating and intraoperative measurement (strictly adhering to the 2-mm wedge limit) are essential.
- Nonunion/Delayed Union: The proximal metaphysis has a tenuous blood supply. Excessive periosteal stripping or failure to maintain the plantar cortical hinge significantly increases the risk of nonunion.
- Plantar Hinge Fracture: If the plantar cortex is completely transected, the osteotomy becomes highly unstable. If this occurs, rigid internal fixation with a dorsal bridging plate may be required instead of a single lag screw.
- Neurovascular Injury: As emphasized, the deep peroneal nerve and dorsalis pedis artery are highly vulnerable during the approach to the second metatarsal base. Meticulous, superficial-only initial dissection is mandatory.
Conclusion
The dorsal closing wedge osteotomy of the metatarsals is a highly effective, biomechanically sound intervention for the eradication of intractable plantar keratosis. By respecting the unique "keel" osteology of the metatarsal base, preserving the plantar cortical hinge, and achieving rigid internal fixation, the orthopedic surgeon can successfully restore the normal forefoot pressure cascade. Rigorous adherence to postoperative non-weight-bearing protocols ensures high union rates and excellent long-term functional outcomes for patients suffering from debilitating forefoot overload.
You Might Also Like

