Introduction & Epidemiology
Hip fractures represent a critical public health concern, frequently occurring in the elderly population and associated with significant morbidity, mortality, and socioeconomic burden. Defined as a fracture of the proximal femur, these injuries are broadly categorized as intracapsular (femoral neck) or extracapsular (intertrochanteric and subtrochanteric). The distinction is paramount due to differences in vascularity, biomechanics, and consequently, treatment strategies and prognosis.
Epidemiologically, hip fractures predominantly affect individuals over 65 years of age, with incidence rates rising exponentially with advancing age. Women are disproportionately affected, largely due to higher rates of osteoporosis and longer life expectancy. Falls are the primary mechanism of injury in this demographic, often precipitated by age-related factors such as impaired balance, sarcopenia, visual deficits, polypharmacy, and environmental hazards. Osteoporosis is the predominant underlying pathology, rendering bones susceptible to fracture even with low-energy trauma. The annual incidence in the United States is approximately 300,000, with projections indicating a substantial increase due to an aging global population.
The clinical ramifications are severe: one-year mortality rates following a hip fracture range from 18% to 33%, with men typically having higher mortality than women. Furthermore, only about 50% of patients regain their pre-injury functional status, and a significant proportion require long-term institutional care. The economic burden is substantial, encompassing acute surgical care, rehabilitation, and long-term support services. Early diagnosis, prompt surgical intervention, and a comprehensive multidisciplinary approach are crucial to mitigate these adverse outcomes.
Classification systems are integral for guiding treatment and predicting outcomes. For femoral neck fractures, the Garden classification categorizes fractures based on displacement and impaction (Type I: incomplete/impacted, stable; Type II: complete, non-displaced; Type III: complete, partially displaced; Type IV: complete, fully displaced). The Pauwels classification focuses on the angle of the fracture line relative to the horizontal, reflecting shear forces and stability (Type I: <30°, Type II: 30-50°, Type III: >50°). For intertrochanteric fractures, the AO/OTA classification provides a comprehensive alphanumeric system, while the simpler Evans-Jensen classification (stable vs. unstable based on posteromedial comminution) is often used clinically. Subtrochanteric fractures are also classified by AO/OTA, often based on comminution and extension.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the proximal femur is fundamental to successful hip fracture management, dictating surgical approaches, implant selection, and anticipated outcomes.
Surgical Anatomy:
-
Proximal Femur:
- Femoral Head: Articulates with the acetabulum. Its vascular supply is critical and vulnerable in femoral neck fractures.
- Femoral Neck: Connects the head to the shaft. Its anteversion (average 15°) and inclination (neck-shaft angle, average 125-135°) are important biomechanical considerations.
- Greater Trochanter: The most lateral prominence, serving as the insertion point for the gluteus medius and minimus, and piriformis. A key landmark for intramedullary nail entry.
- Lesser Trochanter: Medial and posterior prominence, serving as the insertion point for the iliopsoas muscle. Its integrity is crucial for stability in intertrochanteric fractures.
- Intertrochanteric Line/Crest: Anteriorly, the intertrochanteric line connects the greater and lesser trochanters. Posteriorly, the intertrochanteric crest connects them. These are critical in intertrochanteric fracture patterns.
- Subtrochanteric Region: The area extending approximately 5 cm distal to the lesser trochanter. Fractures here are highly susceptible to deforming forces from powerful muscle attachments (gluteals, iliopsoas, adductors).
-
Blood Supply to the Femoral Head: This is a major determinant of avascular necrosis (AVN) risk in femoral neck fractures. The primary supply is derived from the medial and lateral circumflex femoral arteries, branches of the profunda femoris artery (or directly from the femoral artery).
- Lateral Epiphyseal Vessels: The dominant supply, arising from the lateral circumflex femoral artery, ascend on the posterior-superior aspect of the femoral neck within the retinaculum (Weitbrecht's retinaculum). These are most vulnerable to disruption in displaced femoral neck fractures.
- Medial Epiphyseal Vessels: From the medial circumflex femoral artery, contribute to the superior and inferior retinacular vessels.
- Artery of the Ligamentum Teres: A branch of the obturator artery, providing a minor and variable supply, particularly in children. Its contribution in adults is generally considered insufficient to prevent AVN if other supplies are compromised.
- Metaphyseal Vessels: From the nutrient artery of the femur and perforating branches, contributing to the neck and basal head.
-
Capsule and Ligaments: The hip joint capsule is strong, reinforced by the iliofemoral (strongest), pubofemoral, and ischiofemoral ligaments. Intracapsular fractures expose the hematoma to synovial fluid, potentially impairing fracture healing, and disrupt the retinacular vessels.
-
Musculature: The powerful muscles surrounding the hip (gluteals, quadriceps, hamstrings, adductors, iliopsoas, deep external rotators) exert significant deforming forces on fracture fragments, complicating reduction and contributing to instability, particularly in subtrochanteric fractures.
-
Nerve Supply: The femoral nerve (L2-L4) innervates the quadriceps and provides sensation to the anterior thigh. The obturator nerve (L2-L4) innervates adductors. The sciatic nerve (L4-S3) passes posterior to the hip joint, providing innervation to posterior thigh and leg muscles. These nerves are at risk during surgical approaches, particularly the sciatic nerve in posterior approaches and the femoral nerve in anterior approaches or with prolonged traction.
Biomechanics:
- Weight-bearing Axis: The forces across the hip joint are substantial, reaching 2.5-3 times body weight during single-leg stance and even higher during activities like stair climbing.
- Femoral Neck: The neck-shaft angle and anteversion create significant bending and shear forces across the femoral neck. Fractures here are subjected to large forces, making stable fixation challenging. Pauwels classification highlights the importance of the fracture angle – a steeper angle (Type III) indicates higher shear forces and a greater propensity for nonunion or fixation failure.
- Intertrochanteric Region: This region is cancellous bone and subject to complex loading. Fractures here often involve comminution of the posteromedial cortex, which is critical for stability. Loss of posteromedial cortical support converts compressive forces into varus-producing bending moments on the fixation device, leading to cutout.
- Subtrochanteric Region: This is a high-stress area located at the junction of cancellous and cortical bone. Fractures here are subjected to strong deforming forces from the gluteus medius/minimus (abduction), iliopsoas (flexion and external rotation of the proximal fragment), and adductors/hamstrings (adduction and extension of the distal fragment). This often leads to severe displacement and renders reduction challenging.
-
Implant Biomechanics:
- Dynamic Hip Screw (DHS): A sliding hip screw allows controlled impaction, converting shear forces into compressive forces at the fracture site, promoting healing. It is most effective for stable intertrochanteric fractures with an intact lateral wall.
- Intramedullary Nail (IMN): Provides central load sharing and is biomechanically superior for unstable intertrochanteric fractures (e.g., reverse obliquity, posteromedial comminution) and subtrochanteric fractures. It provides a shorter lever arm, reducing bending stress on the implant.
- Arthroplasty (Hemiarthroplasty/THA): Replaces the femoral head, eliminating the fracture fragments. The stability of the construct depends on stem fixation (cemented vs. uncemented) and prosthetic head articulation.
Indications & Contraindications
The management of hip fractures is predominantly surgical, with the primary goals being pain relief, early mobilization, and restoration of function. Non-operative management is reserved for a select few cases due to the high rates of morbidity and mortality associated with prolonged recumbency.
Indications for Operative Management:
- Nearly all hip fractures are candidates for surgical stabilization, given the severe complications of non-operative care (decubitus ulcers, pneumonia, DVT/PE, muscle atrophy, contractures, psychological distress).
-
Femoral Neck Fractures:
-
Displaced (Garden III/IV, Pauwels II/III):
- Hemiarthroplasty (HA): Typically for elderly, low-demand patients, especially those with pre-existing cognitive impairment or limited ambulation. Offers rapid mobilization and pain relief. Bipolar or unipolar components may be used.
- Total Hip Arthroplasty (THA): Considered for active, physiologically younger patients with displaced femoral neck fractures, particularly if they have pre-existing hip arthritis, to achieve superior long-term functional outcomes and reduce revision rates compared to HA.
- Open Reduction Internal Fixation (ORIF): Reserved for young patients (<55-60 years, varying by surgeon) with displaced femoral neck fractures, aiming to preserve the native femoral head. However, carries a high risk of avascular necrosis and nonunion.
-
Non-Displaced or Impacted (Garden I/II, Pauwels I):
- ORIF with cannulated screws: The standard for stable, non-displaced femoral neck fractures in patients of all ages, as it offers good healing potential and preserves the femoral head.
-
Displaced (Garden III/IV, Pauwels II/III):
-
Intertrochanteric Fractures:
- Dynamic Hip Screw (DHS): Indicated for stable, simple intertrochanteric fractures (e.g., Evans-Jensen Type I or AO/OTA A1) with an intact lateral wall and minimal posteromedial comminution.
- Intramedullary Nailing (IMN) - Cephalomedullary Nail: The preferred treatment for most intertrochanteric fractures, particularly unstable patterns (e.g., reverse obliquity, extensive comminution, lateral wall compromise, subtrochanteric extension). Offers superior biomechanical stability and reduced reoperation rates compared to DHS in unstable fractures.
-
Subtrochanteric Fractures:
- Intramedullary Nailing (IMN): The gold standard for subtrochanteric fractures due to their high-energy nature and significant deforming muscle forces. Long intramedullary nails provide load-sharing and effective neutralization of these forces. Plate fixation is generally reserved for situations where IMN is contraindicated or not feasible (e.g., extremely wide medullary canal, periprosthetic fractures adjacent to existing hardware).
Contraindications for Operative Management:
Absolute contraindications are rare and typically relate to the patient's immediate physiological status.
- Prohibitive Medical Comorbidities: Patients with severe, uncontrolled medical conditions (e.g., acute myocardial infarction, unstable angina, severe uncontrolled cardiac arrhythmia, decompensated heart failure, severe sepsis, active stroke) that render the anesthetic and surgical risks unacceptably high. These patients may be managed with supportive care, analgesia, and mobility aids if pain is tolerable.
- Expected Survival Less Than a Few Weeks: In rare instances of terminal illness or severe multi-organ failure where the patient's life expectancy is extremely short and surgery would only add to their suffering.
- Non-Ambulatory, Bed-Bound Patients with Minimal Pain: In patients who are already completely non-ambulatory, bed-bound, and have minimal pain from a stable, non-displaced fracture, non-operative management with meticulous nursing care may be considered. This is exceedingly rare for most fracture types.
- Moribund Patient: A patient who is actively dying, where surgical intervention would offer no significant benefit to comfort or longevity.
- Severe Local Infection: An active infection at the surgical site might necessitate delaying definitive fixation until the infection is controlled, although temporary external fixation might be considered.
It is important to emphasize that advanced age alone is not a contraindication to surgery. The patient's physiological status and comorbidities, rather than chronological age, dictate suitability for operative intervention.
Table: Operative vs. Non-Operative Indications for Hip Fractures
| Indication Type | Operative Indications | Non-Operative Indications (Rare)
Elderly (>75-80 years) or low-demand patient with displaced femoral neck fracture.
* Young patients (<55-60 years) with non-displaced femoral neck fracture (Garden I/II).
* Elderly, high-demand patient (active, healthy) with displaced femoral neck fracture.
* Most intertrochanteric fractures, especially unstable patterns (e.g., reverse obliquity, posteromedial comminution).
* Subtrochanteric fractures.
* Stable intertrochanteric fractures (e.g., intact lateral wall).
* Pathologic hip fractures (tumor or metastasis), depending on prognosis and bone quality. |
| Non-Operative |
*
Prohibitive Medical Comorbidities:
Patient deemed too unstable or frail for surgery by medical/anesthesia teams (e.g., severe acute cardiac event, uncontrolled sepsis, imminent death).
*
Non-Ambulatory, Bed-Bound Patient with Minimal Pain:
Extremely rare. Only if the patient has no functional goals, minimal pain from a stable fracture, and surgery would likely reduce quality of life more than conservative care.
*
Expected Survival < Weeks:
Terminal illness with minimal life expectancy where surgery provides no benefit to comfort.
*
Severe Dementia with No Ambulation Potential:
If pain can be managed adequately with analgesics and there is no benefit to improving mobility.
*
Stable Impacted Femoral Neck Fracture in a Very Frail Patient (Rare):
* Exceptionally rare, typically requiring careful assessment of pain and mobility. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical for optimizing surgical outcomes, minimizing complications, and ensuring efficient execution of the surgical procedure.
Pre-Operative Planning
-
Medical Optimization:
- Comprehensive Medical Evaluation: Immediate assessment by internal medicine or geriatric co-management teams (orthogeriatrics) to identify and optimize comorbidities (cardiac disease, pulmonary insufficiency, renal dysfunction, diabetes mellitus, anemia).
- Anemia Management: Transfusion if hemoglobin is <8 g/dL or if patient is symptomatic/has cardiac comorbidities. Consider pre-operative iron supplementation or erythropoietin in select cases.
- Anticoagulation Management: Develop a clear plan with cardiology/hematology for bridging or holding anticoagulants to minimize bleeding risk while mitigating thrombotic risk.
- Nutritional Assessment: Malnutrition is common in elderly hip fracture patients and is associated with poorer outcomes. Nutritional support may be initiated pre-operatively if time permits.
- Delirium Screening: Baseline cognitive assessment and implementation of delirium prevention strategies (e.g., early mobilization, pain control, hydration, sleep hygiene).
-
Imaging Review and Templating:
- Standard Radiographs: AP pelvis, AP and lateral views of the injured hip are mandatory. Full-length femur radiographs may be useful for subtrochanteric fractures to assess bowing and plan nail length/diameter.
- CT Scan: Indicated for complex fracture patterns, occult fractures not visible on plain radiographs but suspected clinically, or for detailed assessment of comminution and fragment orientation, particularly for subtrochanteric fractures or periprosthetic fractures.
- Templating (for Arthroplasty): Use calibrated AP pelvic radiographs to template femoral stem size and offset, as well as acetabular component size (for THA). This aids in predicting leg length and stability.
- Fracture Table Setup: Anticipate the specific requirements for C-arm access, traction, and patient rotation based on the chosen surgical technique.
-
Timing of Surgery:
- Current evidence supports surgery within 24-48 hours of injury, provided the patient is medically stable, to reduce rates of pneumonia, pressure ulcers, and mortality. Delays beyond 48 hours should be justified by compelling medical reasons.
-
Infection Prophylaxis:
- Administer broad-spectrum intravenous antibiotics (e.g., Cefazolin 2g) within 60 minutes prior to incision.
-
DVT Prophylaxis:
- Initiate mechanical prophylaxis (sequential compression devices) pre-operatively. Pharmacological prophylaxis (e.g., LMWH) is typically started post-operatively, once hemostasis is controlled, or pre-operatively if there is a significant delay to surgery and bleeding risk is low.
Patient Positioning
The choice of patient positioning is dictated by the specific fracture type and planned surgical approach.
-
Supine on a Fracture Table (Most Common for ORIF):
- Indications: Intramedullary nailing (IMN) for intertrochanteric and subtrochanteric fractures, Dynamic Hip Screw (DHS), and cannulated screw fixation for femoral neck fractures.
-
Setup:
- Patient is placed supine on a radiolucent fracture table.
- The uninjured leg is placed in an abduction-flexion-external rotation position to facilitate C-arm access to the injured hip.
- The injured leg is placed in traction via a boot or ankle hitch. The perineal post should be well-padded and positioned laterally to avoid neurovascular compression (pudendal nerve, skin necrosis).
- Traction and Rotation: Traction is applied to restore length and align the fracture fragments. The leg is typically internally rotated 10-15 degrees to correct the external rotation deformity commonly seen in hip fractures and to align the femoral neck in its anatomical anteversion for proper guide wire placement.
- C-arm Access: Ensure unrestricted anteroposterior (AP) and lateral fluoroscopic views of the hip and proximal femur. The C-arm should be able to sweep freely from the knee to above the greater trochanter. This usually involves adducting the uninjured leg and ensuring the perineal post and table supports do not obstruct the beam.
- Precautions: Monitor neurovascular status of both lower extremities. Ensure adequate padding at pressure points. Be mindful of potential traction injuries to the foot/ankle.
-
Supine on a Radiography-Permeable Operating Table (for DAA THA/HA or some ORIF):
- Indications: Direct anterior approach (DAA) total hip arthroplasty or hemiarthroplasty, or certain ORIF procedures where a fracture table is not required or desired.
- Setup: Patient supine on a standard operating table, often with a bump under the ipsilateral hip for some approaches (e.g., to externally rotate the femur for lateral approaches). Adequate space for C-arm is still essential.
- Precautions: Less common for typical hip fracture ORIF unless specific equipment or a specialized table (e.g., hana table for DAA) is used.
-
Lateral Decubitus Position (for Posterior or Direct Lateral Approach Arthroplasty):
- Indications: Total hip arthroplasty or hemiarthroplasty via a posterior (Kocher-Langenbeck) or direct lateral (Hardinge) approach.
-
Setup:
- Patient is positioned on their unaffected side.
- A beanbag or specialized positioning device is used to stabilize the torso.
- An axillary roll is placed in the dependent axilla to prevent brachial plexus compression.
- Pillows are placed between the knees and ankles.
- The dependent arm is flexed at the shoulder and elbow; the superior arm rests on an arm board.
- Ensure the greater trochanter is near the edge of the table to allow for full range of motion of the hip during surgery.
- Precautions: Careful padding of all pressure points, especially the dependent ear, eye, and malleoli. Monitor for signs of nerve compression (brachial plexus, peroneal nerve).
Regardless of the chosen position, meticulous attention to detail regarding padding, neurovascular status, and surgical field exposure is paramount.
Detailed Surgical Approach / Technique
The detailed surgical technique varies significantly based on the fracture type and chosen implant. Below, we outline common approaches for the most prevalent hip fracture patterns. General principles include judicious soft tissue handling, accurate reduction, and rigid internal fixation.
General Intra-Operative Principles:
- Timing: Aim for surgery within 24-48 hours once medically optimized.
- Antibiotics: Administer pre-operatively and consider post-operative doses as per institutional guidelines.
- DVT Prophylaxis: Continue mechanical prophylaxis; initiate chemical prophylaxis post-operatively.
- Anesthesia: General anesthesia or spinal/epidural anesthesia, often with regional nerve blocks for post-operative pain control.
- Fluoroscopy: Essential for all hip fracture ORIF procedures to confirm reduction and implant placement.
- Blood Loss: Anticipate and manage blood loss effectively. Cell Saver may be considered for high-risk arthroplasty cases.
A. Displaced Femoral Neck Fractures in the Elderly: Hemiarthroplasty / Total Hip Arthroplasty
1. Posterior Approach (Kocher-Langenbeck) for Hemiarthroplasty / THA:
*
Patient Positioning:
Lateral decubitus, injured hip superior.
*
Incision:
Curvilinear incision centered over the greater trochanter, extending 8-10 cm proximally along the gluteus maximus fibers and 8-10 cm distally along the femur.
*
Muscle Dissection:
* Incise skin and subcutaneous tissue.
* Split the gluteus maximus bluntly along its fibers.
* Identify and incise the fascia lata just posterior to the greater trochanter.
* Retract the gluteus medius and minimus anteriorly.
*
Internervous Plane:
No true internervous plane is utilized; rather, muscles are split or released. The key is to protect the sciatic nerve, which lies deep and posterior to the short external rotators.
* Identify the short external rotators (piriformis, superior/inferior gemelli, obturator internus, quadratus femoris) inserting on the greater trochanter and intertrochanteric crest. Tag and release these from their femoral insertions. The piriformis is often released first.
* Perform a posterior capsulotomy (T-shaped or inverted T) to expose the femoral head.
*
Head Excision & Femoral Preparation:
* Dislocate the femoral head posteriorly. Remove the fractured femoral head.
* Ream the femoral canal proximally to accommodate the chosen stem size.
* Perform progressive broaching to prepare the metaphysis and diaphysis for the stem.
* Insert the trial stem and evaluate leg length, offset, and stability.
* For hemiarthroplasty, a unipolar or bipolar head is assembled onto the stem. For THA, an acetabular reaming and cup insertion precede femoral stem insertion.
*
Stem Insertion:
* Cemented stem: Insert with cement after canal preparation.
* Uncemented stem: Impact into a precisely prepared canal for press-fit fixation.
*
Reduction & Closure:
* Reduce the femoral head (or prosthetic head) into the acetabulum.
* Repair the capsule and reattach the short external rotators to the greater trochanter through drill holes or sutures in the soft tissue sleeve. This is crucial for posterior stability.
* Close the deep fascia, subcutaneous tissue, and skin in layers.

Figure 1: Intraoperative image demonstrating a prosthetic femoral component, likely during hemiarthroplasty or total hip arthroplasty.
2. Direct Lateral Approach (Hardinge) for Hemiarthroplasty / THA:
*
Patient Positioning:
Lateral decubitus.
*
Incision:
Straight lateral incision, centered over the greater trochanter.
*
Muscle Dissection:
* Incise skin, subcutaneous tissue, and fascia lata.
* Elevate the anterior portion of the gluteus medius and vastus lateralis from the greater trochanter, reflecting them anteriorly (often partially splitting the gluteus medius). This avoids complete detachment of the abductor mechanism.
* Perform an anterior capsulotomy.
*
Head Excision & Femoral Preparation:
Similar to posterior approach.
*
Stem Insertion & Closure:
Similar to posterior approach, with repair of the abductor mechanism to the greater trochanter.
B. Non-Displaced Femoral Neck Fractures: Cannulated Screw Fixation (ORIF)
- Patient Positioning: Supine on fracture table, injured leg in internal rotation and traction.
- Reduction: Confirm anatomical reduction with fluoroscopy (AP and lateral views). If displaced (even slightly), apply manual traction and internal rotation. A percutaneous K-wire or joystick can aid reduction.
-
Guide Wire Placement:
- Typically three parallel cannulated screws are used in a "inverted triangle" or "triangle" configuration for optimal biomechanical stability.
- Aim for subchondral bone purchase in the femoral head.
- Insert the first guide wire centrally in the femoral neck on the lateral view and slightly inferior on the AP view.
- Confirm position with fluoroscopy. The guide wires should penetrate the subchondral bone of the femoral head. Avoid penetration into the joint space.
- Insert additional guide wires parallel to the first, ensuring good spread in both AP and lateral planes. The posteroinferior screw is crucial for stability.
-
Screw Insertion:
- Measure the length of each guide wire.
- Pre-drill (if required by system) and tap the cortical bone laterally.
- Insert fully threaded or partially threaded cannulated screws (depending on fracture type and surgeon preference) over the guide wires.
- Compress the fracture by ensuring the partially threaded screws gain purchase in the distal fragment while sliding through the proximal fragment.
- Final Check: Confirm screw position and fracture reduction with fluoroscopy. Ensure screws do not protrude into the joint.
C. Intertrochanteric Fractures: Cephalomedullary Nailing (IMN) or Dynamic Hip Screw (DHS)
1. Cephalomedullary Nailing (IMN):
*
Patient Positioning:
Supine on fracture table with internal rotation and traction. C-arm access is critical.
*
Reduction:
Apply traction, internal rotation, and sometimes slight abduction to achieve reduction. Fluoroscopic confirmation in AP and lateral views. For unstable or comminuted fractures, manual manipulation, joysticks (percutaneous K-wires), or a large bone hook may be needed.
*
Entry Point:
* Make a longitudinal incision (approx. 5-7 cm) proximal to the greater trochanter.
* Incise fascia and split the gluteus medius fibers bluntly.
* Locate the tip of the greater trochanter.
* Using an awl or starting reamer, create an entry portal at the tip or slightly medial to the tip of the greater trochanter. The starting point must be in line with the femoral canal in both AP and lateral planes. Malpositioning can lead to varus or valgus malalignment or iatrogenic fracture.
*
Reaming & Nail Insertion:
* Pass a guide wire down the medullary canal.
* Ream the canal over the guide wire to the appropriate diameter, allowing for nail insertion.
* Insert the cephalomedullary nail, ensuring proper depth such that the lag screw/blade insertion site is aligned with the center of the femoral head/neck junction.
*
Lag Screw/Blade Insertion:
* Determine the appropriate length for the lag screw or blade, aiming for the center of the femoral head, approximately 1 cm from the subchondral bone, in both AP and lateral views.
* Drill and insert the lag screw or blade. For two-screw systems (e.g., reconstructive nails), insert both in the femoral head/neck. For single-screw systems, compress the fracture if possible.
*
Distal Locking:
* Perform distal locking with two screws via a targeting jig or freehand technique using fluoroscopy. This prevents rotation and shortening.
*
Final Check:
Confirm nail and screw positions, fracture reduction, and rotational alignment with AP and lateral fluoroscopy.
*
Closure:
Close wounds in layers.
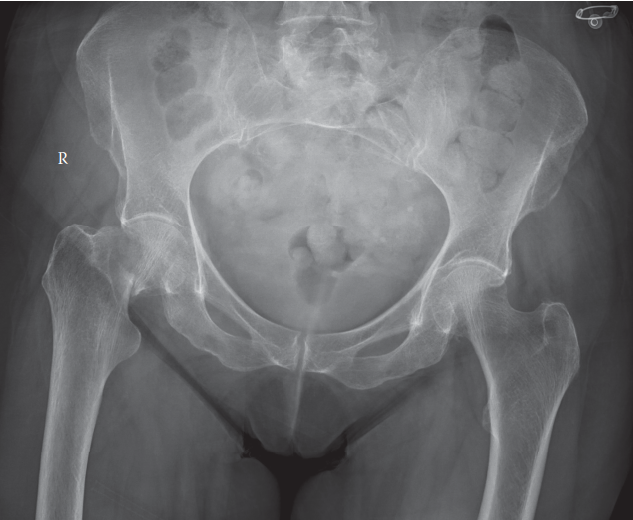
Figure 2: AP radiograph showing a cephalomedullary nail in situ for an intertrochanteric hip fracture, demonstrating the lag screw in the femoral head and distal locking screws in the femoral shaft.
2. Dynamic Hip Screw (DHS):
*
Patient Positioning:
Supine on fracture table with internal rotation and traction.
*
Reduction:
Essential for DHS. Traction, internal rotation, and abduction/adduction maneuvers to achieve anatomical or near-anatomical reduction. Fluoroscopic confirmation.
*
Incision:
Longitudinal incision (8-10 cm) over the lateral aspect of the proximal femur, centered on the greater trochanter and extending distally.
*
Plate Placement:
* Expose the lateral femoral cortex.
* Place a guide wire (usually 135° angle) into the femoral head, aiming for the center of the head in both AP and lateral views, 1-2 cm from the subchondral bone.
* Measure the guide wire length and ream the path for the lag screw.
* Insert the lag screw into the femoral head.
* Place the DHS side plate over the lag screw barrel and impact it onto the lateral femoral cortex. Ensure the plate is centered and flush.
* Insert the cortical screws distally to fix the plate to the femoral shaft.
*
Compression (Optional):
If fracture geometry allows, apply compression across the fracture site using a compression screw to promote impaction.
*
Final Check:
Confirm lag screw position, plate alignment, and fracture reduction.
*
Closure:
Close wounds in layers.
D. Subtrochanteric Fractures: Cephalomedullary Nailing (IMN)
- Patient Positioning: Supine on fracture table with traction. Reduction of these fractures is often difficult due to strong muscle forces.
-
Reduction:
This is the most challenging aspect.
- The proximal fragment often flexes, abducts, and externally rotates due to iliopsoas and gluteal muscle pull.
- The distal fragment tends to adduct.
- Techniques: Manual manipulation, large pointed reduction clamps (e.g., Verbrugge clamps), percutaneous bone hooks, "joysticks" (K-wires or Steinman pins inserted into fragments), or even a temporary external fixator can be employed.
- The goal is to align the proximal and distal fragments to allow nail passage.
- Entry Point & Reaming: Similar to intertrochanteric nailing, but the entry point must be precise to accommodate the often larger diameter and longer subtrochanteric nail. The tip of the greater trochanter is the usual starting point.
- Nail Insertion: Insert a long cephalomedullary nail (often extending beyond the fracture site by several cortical diameters).
- Lag Screw/Blade Insertion: Insert a lag screw or blade into the femoral head/neck, ensuring good purchase.
- Distal Locking: Two distal locking screws are essential to prevent rotation and shortening.
- Final Check: Confirm reduction, nail position, and locking screw placement in both AP and lateral views. Assess for leg length discrepancy.
- Closure: Close wounds in layers.
Complications & Management
Despite meticulous surgical technique, hip fractures are associated with a range of complications, particularly given the advanced age and comorbidities of affected patients. Recognizing and managing these complications is paramount to improving patient outcomes.
General Complications:
-
Medical Complications:
- Delirium (15-50%): Post-operative confusion. Management: early mobilization, adequate pain control, fluid balance, sleep hygiene, minimizing polypharmacy.
- Pneumonia (10-20%): Aspiration or hypostatic. Management: early mobilization, incentive spirometry, chest physiotherapy, appropriate antibiotics.
- Urinary Tract Infection (UTI) (10-20%): Especially with indwelling catheters. Management: early catheter removal, hydration, appropriate antibiotics.
- Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) (DVT 40-60% without prophylaxis, PE 1-5%): Risk factors include age, immobility, surgery. Management: mechanical and pharmacological prophylaxis, early mobilization. Symptomatic PE requires anticoagulation.
- Cardiac Events (5-10%): Myocardial infarction, arrhythmias, heart failure. Management: aggressive pre-operative medical optimization, careful intraoperative monitoring, appropriate post-operative cardiac care.
- Pressure Ulcers (5-20%): Due to prolonged immobility. Management: early mobilization, frequent turning, specialized mattresses, meticulous skin care.
-
Surgical Complications:
- Infection (1-5%): Superficial or deep surgical site infection. Management: debridement, antibiotics, implant retention vs. removal (based on organism, host factors, and chronicity). Girdlestone resection arthroplasty may be necessary for severe, refractory infections in arthroplasty.
- Blood Loss/Transfusion Requirements: Manage with careful hemostasis, cell saver, and blood product transfusion as indicated.
Specific Fracture and Fixation Complications:
| Complication | Incidence (Approx.) | Salvage Strategies & Management |
| Complication | Incidence (Approx.) | Salvage Strategies & Management |
| Nonunion (with persistent pain) | 10-20% | Revision surgery (ORIF to HA/THA, revision IMN). For recalcitrant nonunion in unstable patients, Girdlestone or resection arthroplasty. Consider bone grafting, biologics. |
| Avascular Necrosis (AVN) of Femoral Head | 10-30% (femoral neck) | Early AVN without collapse: watchful waiting. Symptomatic AVN with collapse: THA (gold standard), HA (for lower demand). Salvage: core decompression, vascularized fibula graft (young patients). |
| Implant Cutout/Failure | 5-15% | Revision to arthroplasty (HA/THA), revision ORIF with stronger implant (e.g., DHS to IMN), or Girdlestone. Optimize bone density. |
| Malunion (deformity/pain) | 5-10% | Corrective osteotomy (for significant pain or functional deficit), revision to arthroplasty if severe and symptomatic. |
| Leg Length Discrepancy | 5-20% | Shoe lift for minor discrepancies (<2cm). For larger, symptomatic discrepancies: revision arthroplasty (lengthening/shortening osteotomy of femur). |
| Dislocation (Arthroplasty) | 1-10% | Closed reduction. Recurrent dislocations: component revision (liner, head, stem/cup repositioning), constraint liners, bipolar head. |
| Periprosthetic Fracture (Arthroplasty) | 1-5% | Management depends on Vancouver classification. ORIF (plates/wires) vs. revision arthroplasty (long stem), or a combination. |
| Z-effect/Reverse Z-effect (IMN) | <5% | Occurs in IMN with dual screws where one backs out. Usually indicates unstable fracture/poor reduction. Revision IMN or arthroplasty. |
| Screw Migration/Back-out | <5% | Excision of hardware if symptomatic and fracture healed. Revision fixation if fracture not healed or implant failure is imminent. |
| Hardware Prominence | 5-10% | Hardware removal after fracture healing if symptomatic. |
| Nerve Injury (Sciatic, Femoral) | <1% | Prevention through careful surgical technique and positioning. Management: observation, nerve repair (if indicated and recognized early), pain management. |
Management Principles:
- Early Recognition: Vigilant post-operative monitoring for signs and symptoms of complications.
- Multidisciplinary Approach: Collaboration with internal medicine, geriatrics, infectious disease, physical therapy, and occupational therapy.
- Patient Optimization: Address bone health (Vitamin D, calcium, anti-osteoporotic agents), nutrition, and fall prevention strategies.
- Reoperation Strategy: Based on fracture type, patient factors, and functional goals. Revision surgery often involves conversion to arthroplasty for failed osteosynthesis in the elderly.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a cornerstone of hip fracture management, aiming to restore mobility, strength, and independence while minimizing secondary complications. A coordinated multidisciplinary approach involving surgeons, nurses, physical therapists (PTs), occupational therapists (OTs), and social workers is essential.
Immediate Post-Operative Period (Days 0-7):
- Pain Management: Aggressive, multimodal analgesia (acetaminophen, NSAIDs if appropriate, opioids judiciously, regional nerve blocks like fascia iliaca or pericapsular nerve blocks). Effective pain control facilitates early mobilization.
-
Early Mobilization:
The cornerstone of recovery.
- Day 0-1: Out of bed to chair (if medically stable), initiation of sitting balance, deep breathing exercises, ankle pumps, and isometric gluteal/quadriceps contractions.
-
Weight-Bearing (WB) Status:
Dictated by fracture stability, fixation type, and surgeon preference.
- Hemiarthroplasty/Total Hip Arthroplasty (THA): Typically Weight-Bearing As Tolerated (WBAT) immediately.
- Stable ORIF (e.g., non-displaced femoral neck screws, stable intertrochanteric IMN/DHS): Often WBAT or Protected Weight-Bearing (PWB) (e.g., 25-50% body weight) for 6-12 weeks.
- Unstable Fractures/Complex ORIF (e.g., comminuted intertrochanteric, subtrochanteric, very unstable femoral neck): May require Touch-Down Weight-Bearing (TDWB) (foot to floor for balance, <10% body weight) or Non-Weight Bearing (NWB) for 6-12 weeks, progressing based on radiographic healing.
-
Physical Therapy (PT) Intervention:
- Initial Exercises: Gentle active and passive range of motion (ROM) of the hip and knee, ankle pumps, quad sets, glute sets.
- Gait Training: Progression with appropriate assistive devices (walker, crutches) as pain tolerates and weight-bearing status allows. Focus on proper gait mechanics and safety.
- Transfer Training: Bed to chair, chair to commode.
-
Occupational Therapy (OT) Intervention:
- Activities of Daily Living (ADLs): Training in self-care tasks (dressing, bathing, toileting) using adaptive equipment (e.g., long-handled reachers, sock aids, elevated toilet seats) to minimize hip flexion and rotation.
-
Hip Precautions (for Arthroplasty):
- Posterior approach: Avoid hip flexion >90°, internal rotation, and adduction past midline.
- Anterior approach/DAA: Avoid hip extension, external rotation, and adduction. (Precautions are often less restrictive, but still need to be followed).
- DVT/PE Prophylaxis: Continue mechanical and chemical prophylaxis.
Subacute Rehabilitation (Weeks 1-12):
-
Intensified PT:
- Progressive Strengthening: Focus on hip abductors, extensors, flexors, and quadriceps. Use resistance bands, light weights, and bodyweight exercises.
- Balance Training: Single-leg stance, tandem stance, dynamic balance exercises.
- Advanced Gait Training: Weaning from assistive devices, stair training, navigating uneven surfaces.
- Functional Mobility: Incorporate activities relevant to daily living and pre-injury hobbies.
- Radiographic Monitoring: Serial radiographs (e.g., at 6 weeks, 12 weeks) to assess fracture healing for ORIF cases. Weight-bearing progression is often guided by radiographic evidence of callus formation and stability.
- Nutritional Support: Continue to address any nutritional deficiencies.
- Bone Health: Initiate or continue appropriate osteoporosis management (Vitamin D, calcium, anti-resorptive or anabolic agents) as per guidelines.
- Fall Prevention: Comprehensive assessment of home environment and patient risk factors, including medication review, vision assessment, and balance training. Referral to community fall prevention programs.
Long-Term Rehabilitation (Beyond 12 Weeks):
- Continued Strengthening and Conditioning: Patients should engage in ongoing exercise programs to maintain strength, flexibility, and cardiovascular health.
- Return to Activities: Gradual return to recreational activities and hobbies, with guidance from PT. High-impact activities may be restricted in some arthroplasty patients.
- Psychological Support: Address fear of falling, depression, and anxiety, which are common after hip fracture.
- Follow-up: Regular follow-up with the orthopedic surgeon to monitor implant status, fracture healing, and functional recovery.
Special Considerations:
- Cognitive Impairment: Rehabilitation protocols need to be adapted for patients with dementia or cognitive impairment, focusing on simpler instructions, consistent routines, and caregiver involvement.
- Pre-Existing Disability: Rehabilitation goals should be individualized based on pre-injury functional status and realistic post-injury expectations.
- Multidisciplinary Team Meetings: Regular team discussions to review patient progress, adjust goals, and coordinate discharge planning (home, subacute rehab facility, skilled nursing facility).
The ultimate goal of rehabilitation is to optimize functional recovery and quality of life for hip fracture patients, recognizing that many will not return to their pre-fracture functional level but can still achieve meaningful independence.
Summary of Key Literature / Guidelines
The management of hip fractures has evolved significantly, driven by robust clinical research and consensus guidelines from major orthopedic and geriatric societies. A summary of key literature and guidelines highlights evidence-based best practices.
1. Timing of Surgery:
*
Consensus:
Strong evidence supports performing hip fracture surgery within
24-48 hours
of injury.
*
Key Literature:
Meta-analyses and large cohort studies consistently demonstrate that delays beyond 48 hours are associated with increased rates of 30-day and 1-year mortality, medical complications (pneumonia, UTI, pressure ulcers), and longer hospital stays. While urgent medical optimization is paramount, prolonged delays for non-life-threatening comorbidities are generally discouraged.
2. Multidisciplinary Orthogeriatric Co-management:
*
Consensus:
A multidisciplinary approach, ideally involving formal orthogeriatric co-management (geriatricians, orthopedic surgeons, nurses, PT/OT, nutritionists, social workers), is strongly recommended.
*
Key Literature:
Randomized controlled trials and systematic reviews have shown that orthogeriatric models of care significantly reduce hospital length of stay, improve functional outcomes, lower rates of delirium and other medical complications, and reduce 30-day and 1-year mortality rates.
3. Femoral Neck Fractures:
*
Displaced Fractures (Garden III/IV):
*
Young/Active Patients (<55-60 years):
Open Reduction Internal Fixation (ORIF)
is the preferred treatment to preserve the native femoral head, despite the significant risk of avascular necrosis (AVN) and nonunion (up to 30-40%). Close follow-up for AVN is essential.
*
Elderly/Low-Demand Patients:
Hemiarthroplasty (HA)
(unipolar or bipolar) is the standard. HA provides reliable pain relief and early mobilization with a lower risk of reoperation compared to ORIF.
*
Active Elderly Patients (physiologically younger, high-demand, no severe comorbidities, pre-existing arthritis):
Total Hip Arthroplasty (THA)
is increasingly favored. Studies show THA provides superior long-term functional outcomes, less pain, and lower rates of reoperation compared to HA in this specific cohort.
*
Non-Displaced Fractures (Garden I/II):
*
Cannulated Screw Fixation (ORIF)
is the standard of care for all ages. It offers good healing potential with a lower risk of AVN compared to displaced fractures.
4. Intertrochanteric Fractures:
*
Consensus:
Intramedullary Nailing (IMN)
is generally considered the preferred implant, especially for unstable fracture patterns (e.g., reverse obliquity, extensive posteromedial comminution, lateral wall compromise, subtrochanteric extension).
*
Key Literature:
Meta-analyses indicate that IMN offers biomechanical advantages, lower rates of implant failure, and reduced reoperation rates compared to Dynamic Hip Screws (DHS) for unstable intertrochanteric fractures. DHS remains a viable option for stable, non-comminuted intertrochanteric fractures with an intact lateral wall, often demonstrating similar outcomes to IMN in these specific cases.
5. Subtrochanteric Fractures:
*
Consensus:
Long Cephalomedullary Nailing (IMN)
is the treatment of choice due to the high-energy nature of these fractures and the significant deforming forces of surrounding musculature.
*
Key Literature:
IMN provides central load-sharing and superior biomechanical stability compared to plate fixation, particularly for comminuted fractures. Plate osteosynthesis is generally reserved for situations where IMN is not feasible (e.g., extremely wide canal, existing hardware).
6. Bone Health Optimization:
*
Consensus:
All hip fracture patients should be evaluated for osteoporosis and initiated on appropriate medical management (e.g., Vitamin D, calcium, anti-osteoporotic medications) post-operatively to reduce the risk of subsequent fractures.
*
Key Literature:
Secondary fracture prevention programs demonstrating the effectiveness of pharmacological interventions in reducing re-fracture rates by 30-70%.
7. DVT Prophylaxis:
*
Consensus:
Mechanical prophylaxis (intermittent pneumatic compression devices) should be initiated pre-operatively and continued post-operatively. Pharmacological prophylaxis (e.g., LMWH, fondaparinux, aspirin) should be initiated post-operatively once hemostasis is controlled, and continued for several weeks.
*
Key Literature:
Guidelines from AAOS, ACCP, and NICE universally recommend both mechanical and pharmacological prophylaxis.
8. Pain Management:
*
Consensus:
Multimodal analgesia, including regional nerve blocks (e.g., fascia iliaca block, pericapsular nerve group (PENG) block), is recommended to reduce opioid consumption and facilitate early mobilization.
9. Rehabilitation:
*
Consensus:
Early mobilization and a structured, progressive rehabilitation program led by physical and occupational therapists are critical for functional recovery.
*
Key Literature:
Evidence supports early weight-bearing as tolerated for most stable fixations and arthroplasties to prevent deconditioning and reduce complications.
In summary, current guidelines emphasize prompt surgical intervention, a multidisciplinary approach focusing on orthogeriatric co-management, judicious implant selection based on fracture type and patient factors, aggressive pain management, robust DVT prophylaxis, and comprehensive post-operative rehabilitation including bone health optimization and fall prevention strategies. These principles collectively contribute to minimizing morbidity and mortality and improving functional outcomes for this vulnerable patient population.
