Hand Injury Case: Is it Degloving or Complete Amputation?
Grand Rounds Clinical Case Presentation
Patient Presentation & History
A 38-year-old, right-hand dominant male presented to the Emergency Department following an industrial accident involving his dominant right upper extremity. The mechanism of injury involved his hand being forcibly pulled into a heavy-duty roller press at a manufacturing facility. The machine was reportedly stopped within seconds by a coworker. Emergency Medical Services (EMS) applied a provisional tourniquet proximally on the arm, initiated intravenous access, administered fentanyl for pain control, and applied a sterile dressing to the wound prior to transport. The total time from injury to arrival at our Level I Trauma Center was approximately 45 minutes.
The patient reported no significant past medical history, including diabetes mellitus, hypertension, or peripheral vascular disease. He denied current tobacco use, alcohol abuse, or recreational drug use. No known allergies. He is employed as a machinist, with significant reliance on fine motor control and strength in his right hand for his profession. He has no prior hand injuries or surgeries. Tetanus immunization status was unknown, prompting immediate prophylactic administration upon arrival.
Clinical Examination
Upon arrival, the patient was alert and oriented, hemodynamically stable (BP 130/80 mmHg, HR 88 bpm, RR 16, SpO2 98% on room air). He was in significant distress due to pain despite pre-hospital analgesia.
Inspection:
The entire right upper extremity was exposed. A pneumatic tourniquet was noted on the proximal arm, which was immediately released following initial assessment to evaluate vascularity and bleeding. Gross inspection of the right hand revealed extensive, circumferential soft tissue avulsion extending from the distal forearm, across the wrist, dorsum and palm of the hand, and all five digits. The skin envelope was severely compromised, appearing stretched, torn, and devitalized in large areas, consistent with a high-energy degloving injury.
Specifically, the dorsal skin of the hand was avulsed proximally to the level of the distal forearm, exposing the extensor tendons, metacarpal shafts, and carpal bones. The palmar skin of the hand and digits was also significantly avulsed, particularly over the thenar and hypothenar eminences, and extending distally along all digits. The avulsed skin appeared dusky, mottled, and cold, with areas of ecchymosis and pallor, suggesting significant vascular compromise to the detached flap.
Contamination with grease, hydraulic fluid, and small metallic fragments was evident throughout the wound bed. A partial amputation of the right thumb at the metacarpophalangeal (MCP) joint level was noted, with the thumb remaining attached by a narrow bridge of volar skin and soft tissue, lacking any palpable pulse. The index finger exhibited near-total degloving, with exposed flexor tendons, neurovascular bundles, and the proximal phalanx. Similar, albeit less extensive, degloving injuries were present on the middle, ring, and small fingers. Significant swelling was developing rapidly.
Palpation:
Palpation revealed a cold, clammy hand with significant tenderness and crepitus over the metacarpals and phalanges. Capillary refill was absent in the avulsed skin flap and the partially amputated thumb. The remaining distal portions of the index, middle, ring, and small fingers had markedly delayed capillary refill (>5 seconds) and were cool to touch.
Peripheral pulses: Radial and ulnar pulses were weakly palpable at the wrist but diminished compared to the contralateral limb. Digital pulses were absent in all digits by palpation and handheld Doppler, including the partially amputated thumb.
Range of Motion (ROM):
Active range of motion of the wrist and hand was impossible due to severe pain, gross instability, and presumed tendon transections. Passive ROM was extremely limited due to pain and soft tissue disruption. Gross instability was noted at the right thumb MCP joint and at the base of the index proximal phalanx.
Neurological Assessment:
Sensory examination was performed carefully, given the extensive soft tissue damage.
*
Median Nerve:
Sensation was grossly diminished to absent in the distribution of the median nerve (thumb, index, middle, radial half of ring finger) due to probable transection or severe stretch injury of digital nerves, and potential insult to the main trunk.
*
Ulnar Nerve:
Sensation was also significantly impaired to absent in the ulnar half of the ring finger and small finger distribution, indicating probable digital nerve transections and possible ulnar nerve involvement.
*
Radial Nerve:
Sensation over the dorsal thumb web space was markedly diminished, suggesting potential superficial radial nerve involvement.
Motor function could not be reliably assessed due to pain and skeletal/tendon disruption, but gross inability to actively flex or extend digits was apparent.
Vascular Assessment:
Doppler assessment confirmed absent flow in the digital arteries of all digits, including the partially amputated thumb. Radial and ulnar artery Doppler signals were present but weak and triphasic, suggesting significant spasm or partial injury. Given the extent of degloving and the compromised vascular status of the digits and the avulsed skin flap, immediate revascularization assessment was paramount.
The clinical picture was highly concerning for a near-total degloving injury of the entire hand and digits, coupled with a partial amputation of the thumb and likely multiple open fractures and severe neurovascular disruption.
Imaging & Diagnostics
Plain Radiographs:
AP, oblique, and lateral radiographs of the right hand and wrist were obtained in the trauma bay. These images revealed:
* Comminuted, displaced fractures of the second and third metacarpal shafts, with associated dorsal cortical defects.
* A severely comminuted fracture-dislocation of the right thumb metacarpophalangeal (MCP) joint, consistent with the partial amputation clinically observed. The articular surface of the metacarpal head was severely damaged.
* A comminuted, intra-articular fracture of the base of the right index finger proximal phalanx, with dorsal dislocation of the MCP joint.
* A spiral fracture of the middle phalanx of the small finger.
* Multiple small radiopaque foreign bodies (metallic shards) dispersed throughout the soft tissues, particularly on the dorsal aspect of the hand.
* Significant soft tissue swelling and gas shadows indicative of an open wound.
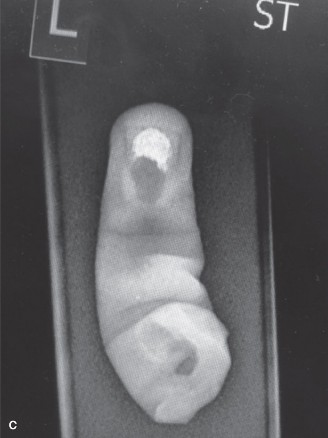
Figure 1: Initial AP radiograph of the right hand demonstrating comminuted fractures of the 2nd and 3rd metacarpals, a comminuted fracture-dislocation of the thumb MCP joint, and an intra-articular fracture of the index proximal phalanx base with MCP dislocation. Note multiple metallic foreign bodies and soft tissue swelling.
Computed Tomography (CT):
A CT scan of the hand and wrist was performed to better delineate the fracture patterns, assess for intra-articular involvement, and identify retained foreign bodies given the high-energy mechanism and industrial contamination. The CT confirmed the extensive comminution of the metacarpal and phalangeal fractures. It also provided a more precise localization of multiple small metallic fragments within the soft tissues, some in close proximity to neurovascular bundles. While not a primary modality for acute vascular assessment, the CT suggested significant soft tissue disruption surrounding the main neurovascular structures.
Other Diagnostics:
- Laboratory Investigations: Complete blood count (CBC), coagulation panel, basic metabolic panel, and type and screen were obtained immediately. All were within normal limits except for a mild leukocytosis (12.5 x 10^9/L), likely a stress response.
- Tetanus Prophylaxis: Administered due to unknown vaccination status and the nature of the wound.
- Antibiotics: Broad-spectrum intravenous antibiotics (Cefazolin 2g IV and Gentamicin 5mg/kg IV) were initiated in the ED, per institutional protocol for severe open fractures and contaminated injuries.
Differential Diagnosis
The clinical presentation of this case highlights the critical distinction between severe degloving injuries and near-total amputations, which often coexist in complex mangled hand trauma.
| Feature | Extensive Degloving Injury (Open) | Near-Total Amputation (Hand/Digits) | Severe Open Crush Injury with Complex Fractures and Soft Tissue Loss |
|---|---|---|---|
| Definition | Skin and subcutaneous tissue avulsed from underlying fascia, creating a large, often compromised, flap. Underlying structures are exposed but usually remain attached. | Limb or digit remains attached by a tenuous bridge of non-functional tissue (e.g., skin bridge) with complete or near-complete transection of skeletal, neurovascular, and tendinous structures. | Diffuse, high-energy impact causing extensive, multifactorial damage to skin, muscle, bone, nerves, and vessels. Characterized by widespread tissue destruction, contusion, and laceration, without a distinct large "flap" or clear separation plane. |
| Primary Concern | Viability of the avulsed skin flap due to vascular compromise; prevention of infection in exposed tissues. | Replantation/revascularization potential and long-term functional outcome, given the complete structural disruption. | Infection control, debridement of diffusely devitalized tissue, staged reconstruction of multiple tissue types, and salvage of viable structures. |
| Vascular Status | Circulation to the avulsed skin flap is typically severely compromised, often relying on a narrow, stretched pedicle. Underlying major vessels may be intact but exposed, or locally damaged. | Major arteries and veins are typically completely severed or functionally non-patent. Revascularization is required for survival of the distal part. | Diffuse microvascular damage, thrombosis, and segmental tears of vessels. Large vessel transection may occur but is not a defining characteristic. |
| Nerve Involvement | Nerves are often exposed, stretched, or contused; potential for partial or complete transection if avulsion is severe and traction forces high. | Typically complete transection of major nerves (median, ulnar, radial) and/or multiple digital nerves. | Contusion, stretching, or transection of multiple nerves, often with irregular injury patterns due to the diffuse nature of the crush. |
| Skeletal Involvement | May have associated fractures or dislocations, often open. Bones are generally continuous with the proximal limb. | Often includes skeletal transection or severe, comminuted fractures that render the skeletal continuity precarious or absent. | Complex, comminuted, segmental, and highly contaminated open fractures; bone loss is common. |
| Reconstruction Focus | Flap salvage (e.g., de-fatting and re-grafting), robust wound closure via grafts or local/regional flaps, fracture fixation, tendon/nerve protection. | Microsurgical revascularization/replantation, meticulous nerve and tendon repair, stable skeletal stabilization (often external fixation initially). | Staged debridement, skeletal fixation (external or internal), and robust soft tissue coverage using local, regional, or free flaps. |
| Prognosis | Highly variable, depending on flap viability, contamination, and extent of underlying tissue damage. Can lead to significant scarring and functional deficits if coverage is delayed or inadequate. | Guarded for functional outcome, high risk of flap/digit loss if revascularization fails. Often requires multiple secondary procedures. | Often poor functional outcome due to diffuse tissue destruction, extensive scarring, and potential for chronic pain and stiffness. Higher rate of delayed amputation compared to isolated injuries. |
In our patient's case, the presentation combines features of an extensive degloving injury with a near-total amputation (of the thumb) and significant crush components across the hand. The main avulsed skin flap over the dorsum and palm, appearing dusky, cold, and avascular, presents as a classic degloving injury. The thumb, tenuously attached, fulfills the criteria for a near-total amputation requiring microsurgical revascularization for survival. The comminuted fractures and diffuse soft tissue contamination are hallmarks of a severe open crush injury. This complex presentation necessitates a comprehensive approach addressing all these components simultaneously.
Surgical Decision Making & Classification
Given the extent of tissue destruction, gross instability, contamination, and vascular compromise, this case was unequivocally deemed an emergent operative intervention . Non-operative management would invariably lead to widespread tissue necrosis, overwhelming infection, and eventual limb loss. The primary goals were limb salvage, revascularization of compromised tissues, stabilization of the skeletal architecture, definitive soft tissue coverage, and optimization of long-term functional outcome.
Key Classifications Applied:
-
Gustilo-Anderson Classification for Open Fractures: This system is critical for assessing the severity of soft tissue injury and guiding management, particularly regarding debridement and antibiotic regimens.
- The comminuted fractures of the metacarpals and phalanges, combined with the extensive soft tissue avulsion, periosteal stripping, and significant contamination from industrial machinery, classify these as Gustilo-Anderson Type IIIB open fractures . This implies extensive soft tissue damage precluding primary wound closure, requiring local or free flap coverage.
- The complete absence of digital pulses and the compromise of the radial/ulnar artery flow would further elevate this to Gustilo-Anderson Type IIIC if major arterial repair was definitively required to save the limb (which it was for the thumb and potentially other digits).
-
Mangled Extremity Severity Score (MESS): While predominantly used for lower limb trauma, the principles of the MESS score are applicable to assess the overall severity and predict the likelihood of limb salvage in mangled upper extremities.
- Skeletal/Soft-tissue injury: High score (e.g., severe crush, degloving, multiple fractures).
- Limb Ischemia: Moderate to severe (absent digital pulses, delayed capillary refill).
- Shock: Not present initially (patient was hemodynamically stable).
-
Age:
Patient is 38 (favorable).
A high MESS score would strongly suggest that primary amputation might be considered; however, in the upper extremity, especially the hand, the threshold for salvage is significantly lower due to the immense functional value, even with limited return of function. The decision in this case was to attempt salvage given the patient's age and high functional demand.
Surgical Strategy:
The surgical approach was planned as a staged procedure, commencing with immediate definitive debridement and skeletal stabilization, followed by microvascular assessment and repair, and finally, soft tissue coverage. The primary goal was to achieve a clean wound bed, stable bone architecture, and re-establish vascularity to the hand and digits. The decision to proceed with replantation of the thumb and revascularization of other digits was made intraoperatively after meticulous assessment of the structures and the potential for a functional outcome.
Surgical Technique / Intervention
The patient was taken to the operating theater emergently.
Pre-operative Preparation:
- Antibiotics: Cefazolin and Gentamicin doses were repeated.
- Anesthesia: General endotracheal anesthesia was administered.
- Positioning: Patient was positioned supine with the right arm abducted on a specialized radiolucent hand table, allowing for full access and C-arm fluoroscopy.
- Exsanguination and Tourniquet: The arm was exsanguinated, and a pneumatic tourniquet was inflated to 250 mmHg on the proximal arm.
Stage 1: Initial Debridement and Assessment
- Tourniquet Off Assessment: The tourniquet was temporarily deflated to assess the extent of active bleeding and further delineate viable versus non-viable tissue. Significant venous ooze and sluggish arterial flow were noted from multiple lacerated vessels. The avulsed skin flap appeared non-viable, dusky, and cold, with no capillary refill. The partially amputated thumb remained without perfusion.
- Copious Irrigation and Meticulous Debridement: The wound was copiously irrigated with 9 liters of warm normal saline using a high-pressure pulsatile lavage system. This was followed by meticulous sharp debridement. All foreign bodies (grease, metallic shards) were painstakingly removed. All devitalized skin, subcutaneous fat, muscle, and fascial tissue were excised until viable bleeding edges were encountered. The avulsed skin flap was deemed non-viable and was excised. This left extensive areas of exposed bone, tendons, and neurovascular structures. The decision was made to discard the avulsed skin flap due to irreversible damage and convert it to a full-thickness skin graft ex vivo if deemed suitable after defatting, which was later determined not feasible due to severe tissue maceration and contamination.
- Vascular Re-assessment: After debridement, the hand remained globally ischemic. The radial and ulnar arteries were identified and found to have segmental intimal tears and partial transections near the wrist, consistent with traction injury. All digital arteries and veins were transected or avulsed, particularly for the thumb and index finger.
Stage 2: Skeletal Stabilization
- Fracture Reduction: All fractures and dislocations were reduced under fluoroscopic guidance.
-
Internal Fixation:
- Thumb MCP Joint: Given the comminuted fracture-dislocation and near-total amputation, a meticulous attempt was made to reconstruct the articular surface. The thumb proximal phalanx was reduced and fixed to the first metacarpal with two 1.2 mm Kirschner wires (K-wires) in a cross-pin configuration. The comminuted metacarpal head fragment was re-aligned and secured with additional fine K-wires.
- Index Proximal Phalanx/MCP Joint: The intra-articular fracture of the index proximal phalanx base was reduced and stabilized with two 0.8 mm K-wires. The dorsal MCP joint dislocation was reduced and temporarily stabilized with an additional K-wire through the metacarpal head into the proximal phalanx.
- Metacarpal Fractures (2nd and 3rd): The comminuted, displaced fractures of the 2nd and 3rd metacarpal shafts were anatomically reduced. Due to the extensive soft tissue loss and contamination, internal fixation with 2.0 mm mini-plates and screws was performed for definitive stability. This provided a rigid framework for subsequent soft tissue and neurovascular repairs.
- Small Finger: The spiral fracture of the small finger middle phalanx was reduced and stabilized with a single 0.8 mm K-wire.
- Final fluoroscopic images confirmed satisfactory reduction and stable fixation of all fractures.
Stage 3: Microvascular Repair and Tendon Repair
-
Vascular Repair:
- Main Vessels: The tourniquet was released. The radial and ulnar arteries were explored. A 1.5 cm segmental defect was noted in the radial artery, and a 0.8 cm intimal tear with thrombosis was present in the ulnar artery. Given the critical need for inflow, both vessels were repaired. The radial artery was reconstructed using a reverse interposition vein graft harvested from the ipsilateral forearm (a non-critical superficial vein). The ulnar artery received a primary end-to-end repair after thrombectomy and debridement of damaged intima.
- Digital Vessels (Thumb and Index): Using micro-surgical techniques under 10x magnification, the ulnar digital artery of the thumb was identified, debrided, and re-anastomosed end-to-end. Multiple digital veins for the thumb were also repaired. For the index finger, one dorsal digital artery and two digital veins were repaired. This re-established inflow and outflow to the replanted thumb and revascularized index finger.
-
Tendon Repair:
- Extensor Tendons: Multiple extensor tendons (to thumb, index, middle, ring, small fingers) were found to be lacerated and retracted. These were identified and primarily repaired using modified Kessler sutures reinforced with epitendinous sutures.
- Flexor Tendons: Similarly, lacerated flexor digitorum superficialis and profundus tendons for all digits, and flexor pollicis longus for the thumb, were identified and repaired using similar techniques. Care was taken to ensure gliding surfaces were preserved as much as possible, given the exposed nature of the repairs.
-
Nerve Repair:
- Digital Nerves: Transected digital nerves to the thumb and index finger were identified. Given the clean ends, primary epineurial repair was performed under magnification. The extent of nerve injury to other digits and main nerves required further assessment for potential delayed grafting.
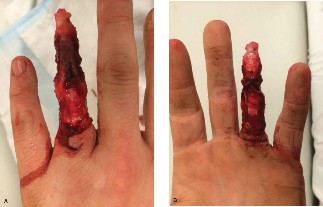
Figure 2: Intraoperative view following meticulous debridement, skeletal stabilization with K-wires and mini-plates, and microvascular anastomosis of the digital vessels. Note the exposed tendons and bone, awaiting soft tissue coverage.
Stage 4: Soft Tissue Coverage
Following stabilization and vascular repair, the extensive soft tissue defect presented a significant challenge.
1.
Temporary Coverage:
Due to the large size of the defect, contamination, and the need to monitor vascular repairs, immediate definitive soft tissue coverage was deferred for a planned "second look" surgery in 48 hours. The wound was temporarily covered with sterile, non-adherent dressings and a vacuum-assisted closure (VAC) device to promote wound bed preparation and manage exudate. The hand was splinted in an intrinsic plus position.
Stage 5: Second Look and Definitive Coverage (48 hours later)
The patient returned to the operating room.
1.
Re-debridement:
The wound was re-explored. All tissues appeared viable, and the re-vascularized digits demonstrated good perfusion. A small area of questionable tissue was re-debrided.
2.
Definitive Soft Tissue Coverage:
*
Dorsal Hand/Metacarpals:
Given the large defect over the dorsum of the hand with exposed metacarpals and extensor tendons, a
free anterolateral thigh (ALT) flap
was harvested from the left thigh. This flap provided robust, vascularized tissue. The flap was anastomosed microsurgically to the radial artery (distal to the repair) and a concomitant vein, or to a branch of the ulnar artery and a superficial dorsal vein of the hand.
*
Palmar Hand/Digits:
For the palmar defects and the thumb/index finger, full-thickness skin grafts were harvested from the groin and applied to areas with adequate underlying vascularized tissue, after careful fenestration. Areas where skin graft take was questionable due to exposed tendon or bone required more durable coverage which was addressed by carefully mobilizing local tissue or extending the ALT flap.
Post-operative Course:
The patient was transferred to the intensive care unit for close monitoring of flap and replant viability, with continuous monitoring of temperature, Doppler signals, and capillary refill. Systemic anticoagulation with intravenous heparin was initiated for the first 5 days, followed by oral aspirin (81mg daily) for 6 weeks. Broad-spectrum antibiotics were continued for 7 days.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Period (Day 0-7):
- Protection: The hand was immobilized in a well-padded, volar plaster splint, maintaining the wrist in 30 degrees of extension, MCP joints in 70 degrees of flexion, and IP joints in slight flexion (intrinsic plus position) to protect the repairs and prevent collateral ligament contracture. The thumb was positioned in palmar abduction.
- Elevation: Strict elevation of the hand above the level of the heart was maintained to minimize edema.
- Vascular Monitoring: Hourly checks of replanted digits and flap viability (color, temperature, capillary refill, Doppler signals). Any signs of vascular compromise (pallor, cyanosis, coldness, absence of Doppler signal) would necessitate immediate return to the operating room.
- Pain Management: Multimodal analgesia including opioids, NSAIDs, and regional nerve blocks (e.g., interscalene block initially, followed by continuous peripheral nerve block via catheter if needed).
- Antibiotics & Anticoagulation: IV antibiotics continued for 7 days. Systemic heparin infusion for 5 days, then transitioned to low-dose aspirin (81mg daily) for 6 weeks.
- Wound Care: Daily dressing changes with careful inspection of suture lines and flap integrity.
Early Mobilization Phase (Weeks 1-6):
- Certified Hand Therapy: Initiation of a supervised, structured hand therapy program by a certified hand therapist (CHT) at week 1-2, once wound stability was confirmed.
- Edema Control: Continued elevation, light compression wraps, gentle retrograde massage.
- Controlled Passive Range of Motion (PROM): Gentle, protected PROM of all involved joints, strictly within the limits prescribed by the surgeon to protect tendon and fracture repairs. Dynamic splinting may be introduced to assist with finger flexion or extension.
- Scar Management: Initiation of scar massage, silicone gel sheets, and gentle stretching to prevent adhesions and reduce hypertrophic scarring.
- Neuropathic Pain: Management of any developing neuropathic pain with gabapentinoids or tricyclic antidepressants.
Intermediate Mobilization and Strengthening Phase (Weeks 6-12):
- Progressive Active Range of Motion (AROM): Gradually increasing AROM exercises for all joints as tendon healing progresses.
- Strengthening: Introduction of light resistance exercises for grip, pinch, and individual digit strength.
- Sensory Re-education: For the replanted thumb and revascularized digits, specific sensory re-education protocols were initiated to promote nerve regeneration and cortical remapping.
- Functional Activities: Integration of hand into light daily activities.
Advanced Rehabilitation and Functional Return (Weeks 12+):
- Advanced Strengthening: Progressive resistive exercises tailored to the patient's occupational demands.
- Fine Motor Skills: Training for dexterity and coordination.
- Return to Work Assessment: Gradual return to work with modifications as needed, emphasizing ergonomic principles and protective equipment.
- Secondary Procedures: Assessment for potential secondary procedures such as tenolysis (for tendon adhesions), arthrolysis (for joint stiffness), nerve grafting (if primary repairs failed or gaps were large), or flap debulking.
The rehabilitation process for such a complex injury is protracted, often lasting 12-18 months, with potential for lifelong limitations. Patient compliance and psychological support are crucial for optimal outcomes.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- "The Gold is in the Debridement": Meticulous and aggressive debridement of all devitalized tissue and foreign bodies is the single most critical step in open trauma and mangled extremity management. Inadequate debridement inevitably leads to infection, sepsis, and failure of all subsequent repairs. Do not hesitate to perform a "second look" debridement in 24-48 hours.
- Early, Stable Skeletal Fixation: Provides a rigid framework for accurate soft tissue, tendon, and neurovascular repairs. Without a stable skeleton, all other repairs are compromised. K-wires for smaller bone fragments and primary plates for metacarpals are often optimal.
- Prompt Soft Tissue Coverage: "No bone likes to be seen." Exposed bone, tendon, or neurovascular structures are a conduit for infection and desiccate rapidly. Obtain definitive vascularized soft tissue coverage within 72 hours (ideally 24-48 hours) using the simplest, most effective method (skin graft, local/regional flap, or free flap).
- Microsurgical Expertise is Paramount: Revascularization and replantation require skilled microsurgical teams for optimal outcomes. Do not compromise on arterial and venous repair; venous congestion is a common cause of flap failure.
- Staged Approach: Complex mangled extremities often benefit from a planned, staged operative approach. Prioritize debridement, stabilization, revascularization, then definitive coverage. This prevents prolonged single-stage procedures and allows for re-assessment.
- Aggressive Hand Therapy: Early and consistent involvement of a certified hand therapist is non-negotiable for maximizing functional recovery and mitigating complications like stiffness, contractures, and scar adhesions.
- Manage Expectations: Be brutally honest with the patient and family about the long, arduous road to recovery, the potential for multiple surgeries, and the likelihood of permanent functional deficits. This aids in patient compliance and realistic goal setting.
- Antibiotic and Tetanus Prophylaxis: Standard for all open injuries, especially contaminated ones.
Pitfalls:
- Incomplete Debridement: The most common cause of catastrophic failure. Failure to remove all devitalized tissue will lead to infection, osteomyelitis, and flap/replant failure.
- Delayed Soft Tissue Coverage: Increases infection risk, delays healing, and promotes exuberant scar formation leading to functional impairment.
- Compromised Vascular Repairs: Inadequate or tensioned microvascular anastomoses, or overlooked venous insufficiency, will result in flap or replant failure.
- Ignoring Venous Drainage: Often more challenging than arterial repair, but crucial for replant/flap survival. Prioritize adequate venous outflow.
- Unstable Skeletal Fixation: Leads to malunion, non-union, and breakdown of soft tissue repairs.
- Premature or Overly Aggressive Mobilization: Disrupts delicate tendon and nerve repairs, leading to re-rupture or inadequate healing.
- Underestimation of Contamination: Industrial injuries often involve polymicrobial contamination requiring specific antibiotic choices and diligent debridement.
- Failure to Address Nerve Injuries: While often secondary to limb salvage, identified nerve injuries must be repaired (primary) or planned for reconstruction (secondary) to restore meaningful function.
- Neglecting Patient Comorbidities: Diabetes, peripheral vascular disease, and smoking significantly impair wound healing, increase infection risk, and compromise vascular repairs. Smoking, in particular, is a strong contraindication for many flaps.
- Lack of Psychological Support: The profound impact of severe hand trauma extends beyond the physical; patients often require extensive psychological support and vocational rehabilitation.
