Greater Tuberosity Fracture: Expert Diagnosis and Treatment Strategies
Introduction & Epidemiology
Greater tuberosity (GT) fractures of the proximal humerus represent a distinct subset of shoulder injuries, often overlooked but critical in their potential impact on glenohumeral function. While proximal humerus fractures overall account for approximately 4-5% of all fractures, GT fractures specifically comprise about 15-20% of these, making them the second most common proximal humerus fracture pattern after surgical neck fractures. They typically result from high-energy trauma in younger, active individuals (e.g., direct blow, fall onto an outstretched hand, motor vehicle accidents) or a fall onto the shoulder in older osteopenic patients. Indirect mechanisms, such as sudden muscle contraction (e.g., during seizure or electrocution) or a violent abduction-external rotation injury with avulsion by the rotator cuff, are also recognized.
The greater tuberosity serves as the insertion site for the supraspinatus, infraspinatus, and teres minor tendons, making its integrity paramount for normal rotator cuff function and glenohumeral kinematics. Consequently, displaced fractures can lead to significant pain, weakness, and restricted range of motion, particularly abduction and external rotation, if not appropriately managed. These fractures are frequently associated with other shoulder injuries, most notably anterior glenohumeral dislocations (occurring in 20-30% of cases), which often result in a reduction-induced avulsion fracture. Other associated injuries include rotator cuff tears (which may either cause the avulsion or be concomitant), brachial plexus injury, and humeral head impression fractures.
Accurate diagnosis is paramount, distinguishing between minimally displaced fractures that may respond to non-operative management and displaced fractures requiring surgical intervention. Displacement is often dictated by the unopposed pull of the rotator cuff muscles, primarily the supraspinatus, which can lead to superior and posterior migration of the fragment, resulting in subacromial impingement and functional deficit. Classification systems, while general for proximal humerus fractures (e.g., Neer classification as a two-part fracture), also consider specific GT fracture characteristics such as fragment size, number of fragments (single vs. comminuted), and the degree of displacement (superior, posterior, or anterior migration). The threshold for displacement requiring surgical intervention remains a subject of ongoing debate, typically ranging from 3mm to 5mm.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the greater tuberosity and surrounding structures is fundamental for effective diagnosis and treatment planning.
Surgical Anatomy
The greater tuberosity is a prominent bony projection located on the superolateral aspect of the humeral head, distal to the articular surface. It serves as the primary insertion point for three of the four rotator cuff muscles:
*
Supraspinatus:
Inserts on the superior facet of the greater tuberosity. Its primary action is abduction of the humerus, and its unopposed pull is the main driver of superior displacement in GT fractures.
*
Infraspinatus:
Inserts on the middle facet of the greater tuberosity. It is a primary external rotator of the humerus.
*
Teres Minor:
Inserts on the inferior facet of the greater tuberosity. It also contributes to external rotation.
The subscapularis tendon inserts on the lesser tuberosity, which is anteromedial to the greater tuberosity.
The integrity of the rotator cuff footprint on the greater tuberosity is crucial for maintaining the precise muscle-tendon length-tension relationships required for normal shoulder kinematics. Fracture of the GT disrupts this footprint, potentially leading to retraction of the attached rotator cuff tendons. The fragment size can vary from a small avulsion off a single facet to a large, comminuted piece involving all three facets.
Vascular Supply: The proximal humerus receives its blood supply predominantly from branches of the anterior and posterior circumflex humeral arteries, which form an arcuate artery and ascend into the humeral head. While avascular necrosis (AVN) is a significant concern with humeral head fractures, isolated GT fractures typically have a lower risk of AVN due to their peripheral location and robust soft tissue attachments. However, extensive soft tissue stripping during surgical approaches can compromise local vascularity to the fragment.
Neural Proximity: The axillary nerve is a critical anatomical structure in close proximity to the greater tuberosity. It wraps around the surgical neck of the humerus, approximately 5-7 cm distal to the lateral acromial border, supplying the deltoid and teres minor muscles. Surgical approaches, particularly the deltoid-splitting approach, require careful attention to avoid iatrogenic injury to this nerve. The cephalic vein lies within the deltopectoral interval and is a key landmark for the deltopectoral approach.
Biomechanics
The greater tuberosity and its attached rotator cuff tendons are integral to glenohumeral joint stability, motion, and force transmission.
*
Rotator Cuff Function:
The supraspinatus initiates abduction and, along with the infraspinatus and teres minor, acts to depress and center the humeral head within the glenoid fossa during elevation, counteracting the upward pull of the deltoid.
*
Fracture Displacement:
The pattern of GT fracture displacement is largely dictated by the forces exerted by the attached rotator cuff muscles.
*
Superior displacement:
Most commonly caused by the unopposed pull of the supraspinatus.
*
Posterior retraction:
Can occur if the infraspinatus and teres minor are intact and exert traction.
*
Anterior displacement:
Less common, but can occur with associated anterior dislocation.
*
Consequences of Displacement:
A superiorly displaced GT fragment can lead to mechanical impingement against the acromion during abduction, causing pain and limiting range of motion. Malunion or non-union can result in a permanent defect in the rotator cuff footprint, leading to chronic weakness, pain, and potentially degenerative changes in the glenohumeral joint. A displaced fragment effectively lengthens the rotator cuff unit, altering its length-tension relationship and reducing its mechanical efficiency.
Indications & Contraindications
The decision-making process for greater tuberosity fractures hinges on numerous factors, primarily the degree of displacement, patient age, activity level, bone quality, and the presence of associated injuries. The goal is to restore anatomical alignment and function while minimizing complications.
Non-Operative Management
Non-operative treatment is typically reserved for minimally displaced, stable fractures.
Indications for Non-Operative Management:
*
Minimally Displaced Fractures:
Displacement threshold is a critical determinant. Generally, fractures with less than 3-5 mm of superior or posterior displacement and minimal angulation (< 45 degrees) are considered candidates for conservative treatment. The exact threshold often varies based on surgeon preference and the patient's functional demands.
*
Stable Fracture Patterns:
Fractures that demonstrate stability on dynamic radiographic assessment (e.g., no further displacement with gravity or gentle ROM).
*
Elderly, Low-Demand Patients:
Individuals with significant comorbidities, low functional expectations, or poor bone quality where the risks of surgery outweigh the potential benefits.
*
Non-Engaging Impingement:
If the fragment does not mechanically impinge on the acromion during passive range of motion.
Non-Operative Protocol:
* Initial immobilization in a sling (often with an abduction pillow for comfort and to reduce supraspinatus tension) for 2-4 weeks.
* Early initiation of pendulum exercises and passive range of motion (PROM) for elbow, wrist, and hand to prevent stiffness.
* Gradual progression to assisted active range of motion (AAROM) and then active range of motion (AROM) as pain subsides and radiographic healing progresses.
* Emphasis on pain control and preventing adhesive capsulitis.
Operative Management
Operative intervention aims to achieve anatomical reduction and stable internal fixation to restore rotator cuff integrity and function, thereby preventing impingement, malunion, and chronic pain.
Indications for Operative Management:
*
Displaced Fractures:
*
Superior Displacement:
Greater than 3-5 mm (depending on literature and surgeon preference), which can lead to subacromial impingement and functional deficit.
*
Posterior Displacement:
Greater than 3-5 mm, which can alter rotator cuff mechanics and lead to external rotation weakness.
*
Anterior Displacement:
Often associated with anterior dislocation and requires reduction and fixation to prevent recurrent instability.
*
Associated Glenohumeral Dislocation:
Especially if the GT fragment displaces after reduction, indicating instability, or if closed reduction is unobtainable due to the interposed fragment.
*
Young, Active Patients:
Individuals with high functional demands where optimal restoration of shoulder mechanics is paramount.
*
Persistent Impingement:
Even with lesser displacement, if the fragment causes mechanical impingement on the acromion or glenoid during range of motion.
*
Significant Comminution:
While challenging, comminuted fragments may still require stabilization if significantly displaced.
*
Failure of Non-Operative Treatment:
Progressive displacement or persistent symptoms despite adequate non-operative care.
Contraindications
Absolute Contraindications:
*
Active Infection:
Systemic or local infection at the surgical site.
*
Severe Comorbidities:
Medical instability precluding safe anesthesia and surgery.
*
Extensive Soft Tissue Compromise:
Open fractures with significant contamination or devitalized tissue (though immediate debridement and stabilization may be indicated).
Relative Contraindications:
*
Poor Bone Quality:
Severe osteoporosis may make stable fixation challenging, though it may not completely contraindicate surgery if displacement is significant.
*
Non-Displaced or Minimally Displaced Fractures:
Where non-operative management is a safe and effective alternative.
Summary Table: Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Displacement | < 3-5 mm (superior/posterior) | > 3-5 mm (superior/posterior); any anterior displacement |
| Angulation | < 45 degrees | > 45 degrees |
| Functional Impact | Minimal pain, no significant impingement, good passive ROM | Significant impingement, loss of ROM, weakness, pain with activity |
| Patient Factors | Elderly, low functional demand, significant comorbidities, poor bone quality | Young, active, high functional demand, good bone quality, compliant patient |
| Associated Injury | Isolated GT fracture (uncomplicated) | Glenohumeral dislocation, significant rotator cuff tear, nerve injury |
| Fracture Pattern | Stable, minimally comminuted, no articular involvement | Unstable, single displaced fragment, comminuted, displaced avulsion |
| Imaging Findings | Concentric reduction, no impingement on abduction, stable | Non-concentric reduction, clear impingement, fragment migration |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing surgical outcomes and anticipating potential challenges.
Pre-Operative Imaging
- Standard Radiographs: An initial series including true AP (Grashey), scapular Y, and axillary lateral views provides basic information on displacement and associated dislocation. The axillary view is particularly useful for assessing superior/inferior and anterior/posterior displacement.
-
Computed Tomography (CT) Scan:
Essential
for displaced greater tuberosity fractures. A CT scan with 3D reconstructions provides detailed information regarding:
- The exact size, shape, and number of fragments.
- The precise degree and direction of displacement (superior, posterior, anterior).
- Articular involvement or impression fractures of the humeral head.
- Degree of comminution.
- Relationship of the fragment to the glenoid and acromion, especially with respect to potential impingement.
- Magnetic Resonance Imaging (MRI): Indicated if there is suspicion of concomitant rotator cuff pathology (beyond the avulsed tendons), labral tears, or other soft tissue injuries that might influence the surgical plan. While the rotator cuff tendons are inherently involved in the avulsion fracture, MRI can assess the integrity of the remaining cuff or the quality of the tendon attached to the fragment.
Surgical Planning
- Fragment Morphology: Based on CT, determine if it is a single large fragment, a multifragmentary fracture, or a small avulsion.
- Displacement Analysis: Quantify the displacement in millimeters and degrees of angulation. This guides reduction strategy.
-
Implant Selection:
- Sutures/Suture Anchors: Often preferred for smaller avulsion fractures or where bone quality is poor. Transosseous sutures provide broad compression.
- Cannulated/Non-Cannulated Screws: Suitable for larger, stable fragments, allowing for lag screw fixation.
- Plates: Locking plates (e.g., proximal humerus plates) may be considered for comminuted fractures, very large fragments, or when associated with surgical neck fractures, though direct plating of the tuberosity can be cumbersome and may irritate the subacromial space.
- Combination: Suture fixation augmented with screws for increased stability.
- Surgical Approach: Pre-determine the most appropriate surgical approach (deltopectoral vs. anterolateral/deltoid-splitting) based on fragment location, degree of displacement, and associated injuries.
Patient Positioning & Anesthesia
- Anesthesia: General anesthesia is standard. An interscalene regional block can be very effective for peri-operative pain management, minimizing narcotic requirements.
-
Patient Positioning:
-
Beach Chair Position (Semi-Fowler's):
This is the most common and versatile position for shoulder surgery. The patient is semi-recumbent with the head and torso elevated approximately 45-70 degrees.
- Advantages: Allows for easy visualization of the superior aspect of the shoulder, facilitates intraoperative assessment of range of motion, and can be converted to arthroscopy easily.
- Setup: The torso is secured to the table, and the head is supported in a headrest (e.g., 'Mayfield' type). The operative arm is draped free to allow for full circumduction and manipulation. Ensure the patient is positioned far enough to the side of the table to allow for instrument access without obstruction. The legs are supported, typically flexed at the hips and knees, with sequential compression devices.
-
Lateral Decubitus Position:
An alternative, less commonly used for isolated GT fractures, but may be preferred for specific associated injuries or surgeon preference.
- Advantages: Provides excellent access to the posterior aspect of the shoulder, useful for arthroscopic portals.
- Setup: Patient lies on the non-operative side, secured with bean bags or bolsters. The operative arm is suspended in traction, typically with 10-15 pounds of weight.
-
Beach Chair Position (Semi-Fowler's):
This is the most common and versatile position for shoulder surgery. The patient is semi-recumbent with the head and torso elevated approximately 45-70 degrees.
-
Sterile Prep and Drape: The entire shoulder, arm, and axilla are prepped and draped to allow for full mobility of the limb and to permit extension of the incision if necessary. The arm is typically placed in a sterile stockinette.
Detailed Surgical Approach / Technique
The goal of surgical fixation for displaced greater tuberosity fractures is anatomical reduction of the fragment to its original bed and stable internal fixation, restoring the rotator cuff footprint and preventing impingement.
Surgical Approach Selection
The choice of surgical approach depends on the fracture characteristics, surgeon preference, and associated injuries.
-
Anterolateral (Deltoid-Splitting) Approach:
- Indications: Primarily for isolated greater tuberosity fractures with superior or posterior displacement. Provides direct access to the GT.
- Internervous Plane: This approach essentially splits the deltoid muscle fibers. It is crucial to limit the split to approximately 5 cm distal to the acromial border to avoid injury to the axillary nerve, which typically courses horizontally around the humerus at this level.
-
Steps:
- Incision: A curvilinear incision, 5-8 cm in length, centered over the greater tuberosity, typically originating from the anterolateral acromial edge and extending distally.
- Subcutaneous dissection to the deltoid fascia.
- Split the deltoid fibers in line with their orientation (anterior or middle deltoid, depending on fragment location).
- Careful blunt dissection beneath the deltoid to visualize the fracture site. Protect the axillary nerve by staying proximal and using careful retraction.
- Bursectomy: The subacromial bursa is incised and resected to improve visualization.
-
Deltopectoral Approach:
- Indications: Often preferred when there is an associated anterior glenohumeral dislocation, comminution, or when broader exposure of the proximal humerus is required. It provides excellent visualization of the anterior aspect of the shoulder.
- Internervous Plane: This approach utilizes the interval between the deltoid muscle (innervated by the axillary nerve) laterally and the pectoralis major muscle (innervated by the medial and lateral pectoral nerves) medially. The cephalic vein typically runs in this interval and can be retracted medially or laterally.
-
Steps:
- Incision: A curvilinear incision, typically 8-12 cm, extending from the coracoid process inferiorly along the deltopectoral groove.
- Identification and isolation of the cephalic vein, which is usually retracted medially.
- Development of the deltopectoral interval.
- Retraction of the deltoid laterally and the pectoralis major medially.
- The clavipectoral fascia is incised, and the underlying structures (conjoined tendon, subscapularis) are identified.
- For greater tuberosity access, the deltoid may need to be carefully elevated from the humeral shaft or a limited superior split may be required, again minding the axillary nerve.
Reduction of the Fracture Fragment
Once the fracture site is exposed, the fragment must be anatomically reduced.
1.
Release of Retracting Forces:
Often, the rotator cuff tendons attached to the fragment are under significant tension, causing superior and posterior retraction. Gentle traction on the arm, often in abduction and external rotation, can help relax these forces.
2.
Direct Reduction:
* Use a bone hook, K-wire (as a joystick), or a blunt periosteal elevator to directly manipulate the fragment back into its anatomical position on the humeral head.
* Visualize the rotator cuff footprint. The goal is to align the fracture edges precisely.
* Associated rotator cuff tears (e.g., partial-thickness tears of the remaining cuff) should be identified and addressed.
3.
Temporary Fixation:
Once reduced, the fragment can be temporarily stabilized with K-wires to maintain position while definitive fixation is applied. Ensure K-wires do not interfere with subsequent implant placement.
Fixation Strategies
The choice of fixation method depends on fragment size, bone quality, comminution, and surgeon preference.
-
Suture Fixation (Transosseous Sutures / Suture Anchors):
- Indications: Small avulsion fragments, comminuted fragments where screw purchase is unreliable, or in osteoporotic bone. Excellent for reattaching the rotator cuff footprint.
-
Technique:
- Transosseous sutures: Non-absorbable sutures (e.g., #2 FiberWire) are passed through drill holes in the humeral shaft cortex distal to the fracture and then through the attached rotator cuff/fracture fragment. This creates a tension-band effect. Typically, 3-4 sutures are used.
- Suture anchors: One or more suture anchors are placed into the humeral head just medial to the fracture bed. The sutures are then retrieved and passed through the attached rotator cuff/fracture fragment in a mattress or modified Mason-Allen fashion.
- Advantages: Atraumatic to the bone, provides broad load distribution, strong fixation for tendon-bone healing.
- Disadvantages: Requires careful soft tissue handling; knots can irritate soft tissues.
-
Screw Fixation:
- Indications: Larger, single, well-corticated fragments where good screw purchase can be achieved.
-
Technique:
- Lag Screw Principle: Often, 2-3 cannulated or non-cannulated screws (e.g., 3.5mm or 4.0mm cortical or cancellous screws) are placed across the fracture site in a lag fashion to achieve interfragmentary compression.
- The screws are inserted perpendicular to the fracture plane for optimal compression.
- Pre-drilling, measuring, tapping (if non-cannulated), and careful screw insertion are critical to avoid stripping and ensure good purchase.
- Ensure screws do not penetrate the articular surface. Intraoperative fluoroscopy is essential to confirm screw length and position.
- Advantages: Rigid fixation, can provide excellent compression.
-
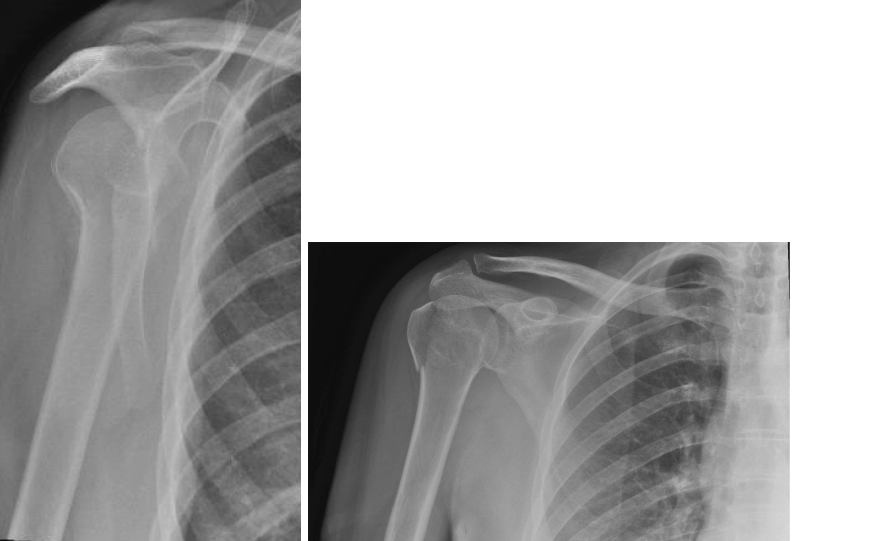[Note: The image, if it showed screws in a GT fracture, would fit well here.] - Disadvantages: Risk of screw pullout in osteoporotic bone, hardware prominence, potential for articular penetration.
-
Plate Fixation:
- Indications: Less common for isolated GT fractures. May be considered for very large or comminuted fragments, or when combined with a surgical neck fracture where a proximal humerus locking plate is already being used.
- Technique: Small fragment plates or specialized proximal humerus plates. Requires meticulous contouring to avoid soft tissue irritation.
- Advantages: Strong construct, especially in comminuted situations.
- Disadvantages: Larger dissection, greater soft tissue irritation, potential for hardware impingement subacromially.
Intraoperative Assessment
- After fixation, perform a gentle, controlled range of motion to confirm stability of the construct, assess for any impingement, and ensure no articular penetration of hardware.
- Confirm fragment position and hardware placement with fluoroscopy in multiple planes (AP, Y, axillary).
Closure
- Irrigate the wound thoroughly.
- Close the deltoid fascia (if split) or the deltopectoral interval.
- Layered closure of subcutaneous tissue and skin.
- Apply a sterile dressing. The arm is typically placed in a sling, often with an abduction pillow, for initial immobilization.
Complications & Management
Despite meticulous surgical technique, complications can arise following operative management of greater tuberosity fractures. Understanding these potential issues and their management strategies is crucial for academic orthopedic surgeons.
Common Complications
-
Non-union or Malunion:
- Description: Failure of the fracture fragments to heal or healing in a non-anatomical position. Malunion often results in a displaced fragment that impinges on the acromion or alters rotator cuff mechanics.
- Incidence: Varies widely, but reported between 5-15% depending on fracture complexity, fixation method, and patient factors.
- Symptoms: Persistent pain, weakness, limited range of motion (especially abduction and external rotation), and crepitus.
-
Management:
- Conservative: Physical therapy, NSAIDs, steroid injections for mild symptoms without severe impingement.
-
Surgical:
- Revision ORIF with Bone Grafting: For symptomatic non-union, debridement of fibrous tissue, fresh reduction, and stable fixation augmented with autogenous or allogenous bone graft.
- Osteotomy: For significant malunion causing impingement, corrective osteotomy to restore anatomical contour.
- Hardware Removal: If prominent hardware is causing impingement.
- Arthroplasty: In severe, chronic cases with associated glenohumeral arthrosis or irreparable rotator cuff dysfunction (e.g., hemiarthroplasty, total shoulder arthroplasty, or reverse shoulder arthroplasty).
-
Adhesive Capsulitis (Frozen Shoulder):
- Description: A common complication after shoulder trauma and surgery, characterized by progressive pain and stiffness due to capsular inflammation and fibrosis.
- Incidence: High, reported between 10-30%, particularly if rehabilitation is delayed or inadequate.
- Symptoms: Gradual onset of diffuse shoulder pain followed by global loss of active and passive range of motion.
-
Management:
- Aggressive Physical Therapy: The cornerstone of treatment, focusing on restoring range of motion.
- Corticosteroid Injections: Intra-articular injections can reduce inflammation and pain, aiding rehabilitation.
- Manipulation Under Anesthesia (MUA): For recalcitrant cases, carefully performed MUA can release adhesions.
- Arthroscopic Capsular Release: For severe, unresponsive cases, arthroscopic release of the thickened capsule.
-
Rotator Cuff Re-tear (if associated repair):
- Description: If the GT fracture was associated with a larger rotator cuff tear that was repaired, failure of that repair can occur.
- Incidence: Varies with the complexity of the initial tear and repair, often 5-20%.
- Symptoms: Persistent pain, weakness, specific deficits in abduction or rotation.
-
Management:
- Conservative: Physical therapy, activity modification for asymptomatic tears.
- Revision Rotator Cuff Repair: For symptomatic, repairable re-tears, often with augmentation (e.g., patch grafts).
- Superior Capsular Reconstruction (SCR): For irreparable tears in younger, active patients.
- Reverse Shoulder Arthroplasty (RSA): For older, low-demand patients with symptomatic, irreparable rotator cuff deficiency (cuff tear arthropathy).
-
Hardware Related Issues:
- Description: Prominent hardware causing irritation or impingement, hardware loosening, migration, or failure.
- Incidence: 5-10%.
- Symptoms: Localized pain, crepitus, palpable hardware.
-
Management:
- Hardware Removal: The most common solution for symptomatic hardware, typically performed after radiographic evidence of fracture union.
- Revision Fixation: If hardware failure leads to loss of reduction, revision surgery with a different fixation strategy may be required.
-
Axillary Nerve Injury:
- Description: Damage to the axillary nerve during the surgical approach (particularly deltoid-splitting) or due to direct trauma during injury.
- Incidence: Relatively low (1-5%), often transient neurapraxia.
- Symptoms: Deltoid weakness or paralysis, sensory deficit over the lateral shoulder (regimental badge area).
-
Management:
- Observation: Most neurapraxias recover spontaneously within 3-6 months.
- Electromyography (EMG) studies: To assess nerve function and prognosis.
- Neurolysis/Nerve Grafting: In severe cases of transection or persistent deficits.
- Tendon Transfers: For permanent deltoid paralysis to restore some abduction function (e.g., latissimus dorsi transfer).
-
Infection:
- Description: Superficial or deep surgical site infection.
- Incidence: Low, <1-2% for clean orthopedic procedures.
- Symptoms: Pain, redness, swelling, fever, purulent discharge.
-
Management:
- Antibiotics: Targeted intravenous antibiotics based on culture results.
- Surgical Debridement and Irrigation: For deep infections, often multiple debridements are required.
- Hardware Removal: If the infection persists despite debridement and antibiotics, especially for deep infections.
- Staged Reconstruction: For chronic infections requiring hardware removal, a staged approach to reimplantation.
-
Avascular Necrosis (AVN) of the Humeral Head:
- Description: Death of bone tissue due to interruption of blood supply to the humeral head.
- Incidence: Rare for isolated greater tuberosity fractures, more commonly associated with displaced humeral head fractures (anatomical neck or surgical neck with significant displacement).
- Symptoms: Progressive pain, stiffness, collapse of the humeral head leading to arthrosis.
-
Management:
- Observation: For asymptomatic early stages.
- Core Decompression: For pre-collapse lesions.
- Arthroplasty: Hemiarthroplasty or total shoulder arthroplasty for symptomatic collapse and arthrosis.
Summary Table: Common Complications & Management
| Complication | Incidence (approx.) | Salvage / Management Strategies |
|---|---|---|
| Non-union / Malunion | 5-15% | Revision ORIF with bone grafting, corrective osteotomy, hardware removal for impingement, arthroplasty for severe sequelae |
| Adhesive Capsulitis | 10-30% | Aggressive physical therapy, steroid injections, manipulation under anesthesia, arthroscopic capsular release |
| Rotator Cuff Re-tear | 5-20% | Revision rotator cuff repair, superior capsular reconstruction, reverse shoulder arthroplasty (if irreparable, symptomatic) |
| Hardware Related Issues | 5-10% | Hardware removal for pain/impingement, revision fixation for failure |
| Axillary Nerve Injury | 1-5% (transient) | Observation, EMG studies, neurolysis/nerve graft, tendon transfers for permanent deficit |
| Infection | <1-2% | Debridement, irrigation, targeted antibiotics, hardware removal (if necessary) |
| Avascular Necrosis (AVN) | Rare for isolated GT | Observation, core decompression (early stages), hemiarthroplasty, total shoulder arthroplasty, reverse shoulder arthroplasty |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as surgical fixation for optimizing functional outcomes following greater tuberosity fracture repair. Protocols are typically structured in phases, with progression based on fracture stability, fixation strength, bone healing, and individual patient response. Close communication between the surgeon and physical therapist is essential.
General Principles
- Protection of Fixation: The primary goal in the early phase is to protect the surgical repair, especially if an associated rotator cuff repair was performed.
- Gradual Progression: Rehabilitation progresses slowly and systematically, advancing only when specific milestones are met.
- Pain Management: Effective pain control is vital for patient compliance and early initiation of therapy.
- Individualization: Protocols should be tailored to the specific fracture pattern, quality of fixation, patient's age, bone quality, and functional goals.
Phase 1: Protection Phase (0-6 Weeks Post-Op)
- Goals: Control pain and inflammation, protect the healing fracture, prevent stiffness in adjacent joints, and avoid muscle atrophy in the elbow/wrist/hand.
- Immobilization: Arm immobilized in a sling, often with an abduction pillow, for 4-6 weeks. The duration depends on surgeon's assessment of fracture stability and fixation.
-
Activities:
- Pendulum Exercises (Codman's): Initiate early (within a few days post-op) to promote gentle joint nutrition and prevent stiffness without active muscle contraction.
- Passive Range of Motion (PROM): Elbow, wrist, and hand exercises to maintain mobility.
- Scapular Retractions: Gentle isometric scapular exercises to maintain scapular stability without stressing the shoulder.
- Gravity-Assisted PROM (limited): Gentle external rotation or flexion with gravity assistance may be initiated in a supine position, always under strict supervision and within pain-free limits. Avoid aggressive external rotation if the infraspinatus/teres minor footprint was involved.
- Restrictions: NO active shoulder range of motion (AROM). NO lifting, pushing, pulling, or supporting body weight with the operative arm. Avoid external rotation past neutral, especially if the infraspinatus/teres minor was involved. No driving.
Phase 2: Early Active Motion Phase (6-12 Weeks Post-Op)
- Goals: Gradually restore active range of motion, initiate gentle strengthening, improve neuromuscular control.
- Progression Criteria: Radiographic evidence of early fracture healing (callus formation), minimal pain, and satisfactory passive range of motion.
-
Activities:
- Discontinue Sling: As tolerated, usually around 6 weeks.
- Active Assisted Range of Motion (AAROM): Using the non-operative hand or a pulley system to assist with flexion, abduction, and rotation within pain-free limits.
- Active Range of Motion (AROM): Gradually progress to active shoulder movements as pain allows. Start with gravity-eliminated positions.
- Isometric Strengthening: Gentle isometric exercises for the rotator cuff and deltoid, performed in multiple directions, without resistance.
- Scapular Stabilization Exercises: Progress to more challenging exercises to enhance scapulohumeral rhythm.
- Restrictions: Still NO heavy lifting. Avoid sudden or forceful movements. No unassisted lifting of objects.
Phase 3: Strengthening Phase (12-24 Weeks Post-Op)
- Goals: Restore full shoulder strength, endurance, and advanced range of motion. Improve proprioception and functional movement patterns.
- Progression Criteria: Full, pain-free active range of motion, good muscle activation, and radiographic evidence of substantial fracture healing.
-
Activities:
-
Progressive Resistance Exercises (PREs):
- Theraband exercises for internal/external rotation, abduction, flexion.
- Light weights for deltoid and rotator cuff strengthening.
- Focus on eccentric control.
- Proprioceptive Training: Balance and stability exercises (e.g., using a stability ball or wobble board).
- Core Strengthening: To support overall body mechanics.
- Endurance Training: For shoulder musculature.
- Begin Functional Activities: Gradually introduce activities mimicking daily living.
-
Progressive Resistance Exercises (PREs):
- Restrictions: Avoid maximal lifting or high-impact overhead activities. Gradual increase in resistance and intensity.
Phase 4: Return to Activity Phase (24+ Weeks Post-Op)
- Goals: Full return to pre-injury activity levels, including sports or strenuous work.
- Progression Criteria: Full strength (often measured with isokinetic testing), endurance, and pain-free execution of sport-specific or work-specific movements.
-
Activities:
- Sport-Specific or Work-Specific Training: Gradually introduce activities requiring overhead movements, throwing, or heavy lifting.
- Plyometrics (if applicable): For athletes requiring power.
- Maintain Strength and Flexibility: Ongoing home exercise program.
- Restrictions: Close monitoring during return to high-demand activities.
Key Considerations:
*
Radiographic Follow-up:
Regular X-rays are crucial to monitor fracture healing and detect potential hardware complications or loss of reduction.
*
Patient Education:
Patients must understand the importance of adherence to the protocol and the potential consequences of premature return to activity.
*
Pain as a Guide:
While patients are encouraged to push gently, pain should generally be respected as a signal to slow progression.
Summary of Key Literature / Guidelines
Greater tuberosity fractures, particularly displaced ones, are increasingly recognized for their clinical significance. The current literature and evolving guidelines highlight several key principles and ongoing debates.
Consensus Principles
- Diagnosis: Advanced imaging, particularly CT scans with 3D reconstructions , is paramount for accurately characterizing fracture morphology, fragment displacement, and assessing for articular involvement, guiding operative planning. Standard radiographs often underestimate displacement.
- Displacement Threshold: While historically varied, a general consensus has emerged suggesting that displacement exceeding 3-5 mm (superior or posterior) in active patients warrants surgical intervention. This threshold is critical due to the high risk of subacromial impingement, rotator cuff dysfunction, and pain with greater displacement. Some authors argue for a 3mm threshold, particularly for superior displacement, given its direct impact on cuff function and impingement.
- Anatomic Reduction: The primary goal of operative treatment is the anatomical reduction of the greater tuberosity fragment to restore the rotator cuff footprint and maintain normal glenohumeral kinematics. Failure to achieve anatomical reduction is a leading cause of unsatisfactory outcomes.
- Associated Injuries: The high incidence of associated glenohumeral dislocation (up to 30%) and rotator cuff tears necessitates thorough evaluation for these concomitant injuries, as their management directly impacts the overall treatment strategy.
Controversies and Evolving Concepts
-
Optimal Fixation Method:
There is no single universally accepted "best" fixation method.
- Suture fixation (transosseous sutures, suture anchors): Is often preferred for smaller avulsion fragments or in osteoporotic bone, and by many for reattaching the rotator cuff footprint broadly. Systematic reviews often show good results with suture fixation, emphasizing biological healing.
- Screw fixation (lag screws): Is typically used for larger, sturdy fragments where adequate bone stock allows for rigid compression. Some studies suggest screws may offer more rigid immediate fixation but carry risks of hardware prominence or articular penetration.
- Plate fixation: Less common for isolated GT fractures but may be considered for larger, comminuted patterns or those extending into the surgical neck.
- The decision often comes down to surgeon preference, fragment characteristics, and bone quality. Combination techniques (screws augmented with sutures) are also utilized.
-
Role of Arthroscopy:
The use of arthroscopically assisted reduction and fixation is gaining traction.
- Advantages: Minimally invasive, allows for comprehensive intra-articular inspection (e.g., labral tears, articular surface), precise fragment reduction under direct visualization, and simultaneous treatment of associated rotator cuff or labral pathology.
- Disadvantages: Technically demanding, longer learning curve, specialized equipment, and may not be suitable for highly comminuted fractures. Some literature suggests comparable outcomes to open approaches but with potentially less soft tissue disruption.
-
Rehabilitation Protocols:
The timing and aggressiveness of post-operative rehabilitation remain areas of debate, particularly regarding early versus delayed range of motion.
- Early Motion: Generally favored to prevent stiffness and adhesive capsulitis, but must be balanced against the need to protect the healing fracture and soft tissue repair, especially if a rotator cuff repair was also performed.
- Delayed Motion: May be advocated for tenuous fixation or poor bone quality, but risks increased stiffness.
- Most protocols advocate for early passive and protected active motion, with gradual progression to strengthening, individualized to the patient and surgical construct.
Key Literature and Guidelines
- Neer Classification (1970): While general for proximal humerus fractures, it classifies displaced greater tuberosity fractures as two-part fractures.
- AO/OTA Classification: Provides a more detailed description of proximal humerus fractures, including specific types of greater tuberosity involvement.
- Systematic Reviews and Meta-Analyses: Recent reviews consistently demonstrate that operative management of significantly displaced greater tuberosity fractures leads to better functional outcomes compared to non-operative treatment, particularly in younger, active patients. They also highlight the importance of anatomical reduction and stable fixation.
- AAOS (American Academy of Orthopaedic Surgeons) Guidelines: While not specific to GT fractures, general guidelines for proximal humerus fractures emphasize shared decision-making, considering patient factors, fracture displacement, and surgeon expertise.
- Emphasis on Outcomes: Patient-reported outcome measures (PROMs) like the Constant-Murley score, ASES (American Shoulder and Elbow Surgeons) score, and UCLA shoulder score are widely used in literature to assess functional recovery, pain relief, and patient satisfaction, informing best practices.
In conclusion, the management of greater tuberosity fractures requires a nuanced approach, balancing anatomical reduction and stable fixation with personalized rehabilitation strategies. Ongoing research continues to refine our understanding of optimal surgical techniques and post-operative care.

