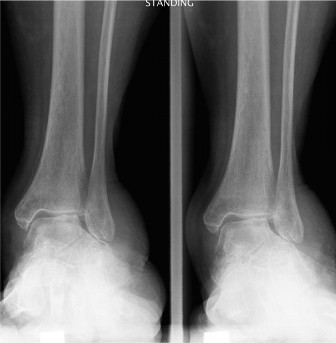
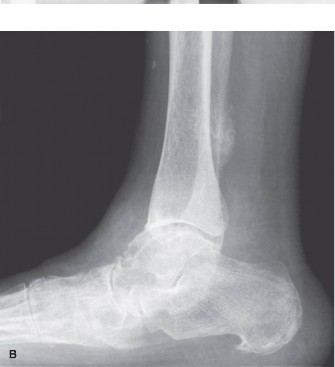
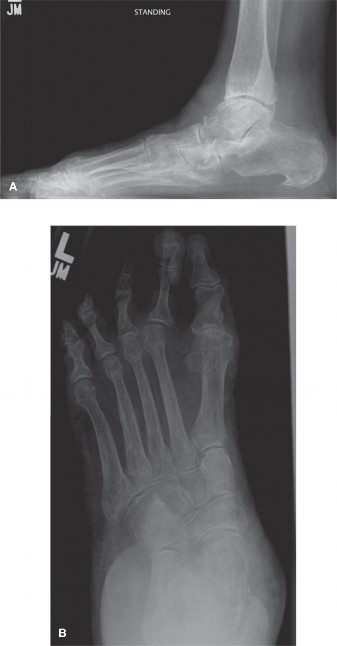
Introduction & Epidemiology
Foot and ankle pain represents a significant proportion of musculoskeletal complaints encountered in orthopedic practice, affecting individuals across all age demographics and activity levels. The etiology is remarkably diverse, ranging from acute traumatic injuries to chronic degenerative conditions, inflammatory processes, and biomechanical dysfunctions. Given the complexity of the 26 bones, 33 joints, and over 100 muscles, tendons, and ligaments comprising the foot and ankle, a systematic diagnostic approach is imperative.
Initial clinical evaluation, encompassing a detailed history and thorough physical examination, guides the necessity and focus of diagnostic imaging. Radiographs, specifically plain film radiography, serve as the foundational imaging modality in the assessment of foot and ankle pain. They are readily accessible, cost-effective, and provide critical information regarding osseous structures, joint alignment, and the presence of significant pathologies.
When radiographs are obtained, they primarily reveal alterations in bone architecture, joint space integrity, and overall structural alignment. These findings are instrumental in:
*
Diagnosing acute fractures and dislocations:
Identifying the location, pattern, displacement, and comminution of fractures.
*
Assessing degenerative joint disease (osteoarthritis):
Revealing joint space narrowing, osteophyte formation, subchondral sclerosis, and cyst formation.
*
Evaluating inflammatory arthropathies:
Detecting erosions, soft tissue swelling, and specific patterns of joint involvement.
*
Identifying deformities:
Such as pes planus (flatfoot), pes cavus (high arch), hallux valgus, and other forefoot, midfoot, or hindfoot malalignments.
*
Detecting stress fractures, avascular necrosis, or osteochondral lesions:
Though often requiring advanced imaging for confirmation, subtle changes can sometimes be appreciated.
*
Screening for tumors or infections:
Revealing osteolytic or osteoblastic lesions, periosteal reaction, or soft tissue gas.
*
Post-operative assessment:
Monitoring fracture healing, implant position, and arthrodesis consolidation.
Epidemiologically, ankle sprains are among the most common musculoskeletal injuries, with a high proportion of patients presenting for radiographic evaluation to rule out fracture. Foot fractures, particularly metatarsal and phalangeal fractures, are also frequent. Chronic foot and ankle pain due to conditions like osteoarthritis, tendinopathy, and plantar fasciitis also regularly necessitate radiographic assessment to exclude structural abnormalities or advanced degenerative changes that might warrant surgical intervention. The appropriate interpretation of radiographs, in conjunction with clinical findings, dictates the subsequent management strategy, often guiding the decision toward non-operative versus operative pathways.
Surgical Anatomy & Biomechanics
A profound understanding of the surgical anatomy and biomechanics of the foot and ankle is paramount for any surgeon contemplating intervention. Radiographs provide a two-dimensional representation of a complex three-dimensional structure, requiring the interpreter to mentally reconstruct the anatomy and appreciate the dynamic interplay of forces.
The ankle joint, a hinge joint, is formed by the distal tibia, fibula, and talus. Key radiographic assessments include:
*
Ankle mortise integrity:
Measured by the tibiofibular clear space, medial clear space, and talocrural angle on AP views, indicating syndesmotic stability.
*
Tillaux and Volkmann fragments:
Posterior and anterior tibial rim fractures often seen with rotational ankle injuries.
*
Pilon fractures:
High-energy axial load injuries to the distal tibia involving the plafond.
The hindfoot comprises the talus and calcaneus. Crucial radiographic parameters include:
*
Talar declination angle and calcaneal pitch angle:
Indicating arch height.
*
Kite's angle (talonavicular coverage angle):
Assessing midfoot abduction/adduction.
*
Böhler's angle and Gissane's angle:
Critical for evaluating calcaneal fractures.
*
Subtalar joint alignment:
Best assessed on hindfoot alignment views or CT, revealing varus or valgus deformities.
The midfoot consists of the navicular, cuboid, and three cuneiform bones, forming the transverse arch and contributing to longitudinal arch stability. Common pathologies here include:
*
Lisfranc injuries:
Disruption of the tarsometatarsal joint complex, often subtle on plain radiographs but critical to diagnose. Radiographic signs include widening between the first and second metatarsal bases, loss of alignment between the medial cuneiform and second metatarsal, or avulsion fractures at the Lisfranc ligament insertion.
*
Midfoot arthritis:
Affecting the talonavicular, calcaneocuboid, or cuneiform-metatarsal joints, often visualized as joint space narrowing and osteophytes.
The forefoot includes the metatarsals and phalanges. Radiographs are essential for:
*
Metatarsal fractures:
Common, especially stress fractures (often subtle or invisible on initial radiographs).
*
Hallux valgus:
Characterized by increased intermetatarsal angle (1-2), hallux valgus angle, and distal metatarsal articular angle.
*
Lesser toe deformities:
Hammertoe, claw toe, mallet toe, where joint subluxation or dislocation can be seen.
Biomechanically, the foot and ankle function as a mobile adaptor and a rigid lever. Radiographs assist in understanding static deformities that compromise these functions. For instance, in pes planus, a decreased calcaneal pitch and talonavicular uncoverage contribute to a rigid flatfoot. In arthritis, loss of joint space alters load transmission and motion. Understanding these relationships is critical for surgical planning, whether the goal is fracture reduction, arthrodesis, or osteotomy to restore alignment.
Indications & Contraindications
The decision for operative intervention in foot and ankle pain is a complex interplay between clinical assessment, radiographic findings, patient comorbidities, and functional demands. Radiographs are often the initial step in identifying pathologies that may necessitate surgery.
Indications for Operative Intervention (Often guided by radiographic findings):
*
Fractures with significant displacement, intra-articular involvement, or instability:
*
Ankle fractures:
Bimalleolar, trimalleolar, or syndesmotic injuries (e.g., widened medial clear space, tibiofibular clear space > 6mm on AP/mortise views).
*
Pilon fractures:
Articular incongruity, comminution.
*
Calcaneal fractures:
Displaced intra-articular fractures (e.g., depressed Böhler's angle), significant subtalar joint involvement.
*
Talus fractures:
Displaced neck/body fractures, particularly Hawkins types II-IV with risk of AVN.
*
Lisfranc injuries:
Any demonstrable dorsal subluxation, widening between M1/M2, or loss of medial cuneiform-M2 alignment.
*
Fifth metatarsal fractures:
Displaced Jones fractures (proximal diaphyseal-metaphyseal junction), often with high nonunion rates.
*
Severe degenerative arthritis refractory to non-operative management:
*
Ankle arthritis:
End-stage disease with bone-on-bone changes, significant pain and functional limitation.
*
Subtalar, talonavicular, calcaneocuboid arthritis:
Severe joint space narrowing, significant osteophyte formation.
*
First MTP joint arthritis (hallux rigidus):
Advanced Grade III/IV disease with severe dorsal osteophytes and joint destruction.
*
Progressive deformities causing pain or functional limitation:
*
Hallux valgus:
Severe deformity (e.g., HVA > 40°, IMA > 16°) with painful bunion, MTP joint arthrosis, or crossover toes.
*
Adult Acquired Flatfoot Deformity (AAFD) with significant radiographic parameters:
Talonavicular uncoverage, increased talar declination, hindfoot valgus.
*
Pes Cavus:
Fixed deformity leading to metatarsalgia, claw toes, or lateral ankle instability.
*
Chronic instability:
*
Chronic ankle instability:
Failed conservative treatment, positive anterior drawer/talar tilt on stress radiographs.
*
Peroneal tendon subluxation/dislocation:
Often associated with fibular groove shallowing.
*
Nonunion or malunion of fractures:
Documented by persistent fracture lines on radiographs and clinical symptoms.
*
Osteochondral lesions (OCL) of the talus:
Large or unstable lesions (e.g., Stage III/IV Berndt and Harty) refractory to conservative care.
*
Infections (osteomyelitis):
Radiographic evidence of bone destruction, periosteal reaction, sequestrum, involucrum, requiring debridement.
*
Tumors:
Radiographic features suggestive of aggressive or symptomatic bone lesions requiring biopsy/resection.
Contraindications for Operative Intervention:
*
Absolute:
* Acute local or systemic infection (relative contraindication for elective cases, absolute for hardware placement).
* Severe vascular compromise limiting healing potential.
* Uncontrolled diabetes with severe neuropathy or poor glycemic control.
* Severe, uncorrectable medical comorbidities that preclude safe anesthesia or surgery.
* Charcot neuroarthropathy in an acute, active (rocker-bottom) phase.
*
Relative:
* Mild symptoms responsive to non-operative management.
* Significant smoking history (increases complication rates, especially nonunion).
* Poor skin integrity or soft tissue envelope.
* Patient non-compliance or unrealistic expectations.
* Psychiatric comorbidities that may hinder recovery.
* Early degenerative changes with minimal pain.
Operative vs. Non-Operative Indications in Foot & Ankle Pain
| Condition/Radiographic Finding | Operative Indications (Radiographic Emphasis) | Non-Operative Indications (Radiographic Emphasis) |
|---|---|---|
| Ankle Fractures | Displaced (>2mm) articular incongruity, bimalleolar/trimalleolar, syndesmotic disruption (medial clear space >4mm, tibiofibular clear space >6mm, talar shift) | Non-displaced unimalleolar (stable), avulsion fractures not involving weight-bearing surface, stable stress fractures. |
| Pilon Fractures | Any significant articular displacement or comminution, particularly if impacting weight-bearing surface. | Rare; typically limited to truly non-displaced (Type I) or low-energy, stable fractures without articular disruption. |
| Calcaneal Fractures | Displaced intra-articular fractures (e.g., Böhler's angle <20° or depressed posterior facet), significant subtalar incongruity. | Extra-articular, non-displaced intra-articular, or stable posterior facet fractures. |
| Talus Fractures | Displaced neck fractures (Hawkins II-IV), body fractures with articular incongruity or significant displacement. | Non-displaced neck fractures (Hawkins I), stable avulsion fractures. |
| Lisfranc Injuries | Any diastasis (>2mm) between 1st & 2nd MTP base, loss of alignment between medial cuneiform and 2nd MTP, dorsal subluxation of metatarsal bases. | Ligamentous sprains without instability (rarely true for Lisfranc if diagnosed accurately), non-displaced avulsion fragments with intact alignment. |
| Hallux Valgus | Severe deformity (HVA >40°, IMA >16°), painful bunion, subluxation of sesamoids, MTP joint arthrosis. | Mild deformity, asymptomatic, pain responsive to wider shoes or orthotics, no significant MTP joint arthrosis. |
| Ankle Arthritis | End-stage joint space narrowing (bone-on-bone), significant osteophytes, subchondral sclerosis, cyst formation, disabling pain refractory to conservative care. | Mild to moderate joint space narrowing, early osteophytes, pain responsive to NSAIDs, activity modification, injections, bracing. |
| Adult Acquired Flatfoot | Progressive deformity with significant hindfoot valgus, talonavicular uncoverage (>30%), midfoot collapse, irreducible deformity, refractory pain. | Flexible deformity responsive to orthotics, early stage disease, mild symptoms, reducible flatfoot. |
| Stress Fractures | Displaced fractures, delayed union/nonunion after prolonged conservative care, high-risk locations (e.g., femoral neck, anterior tibia, displaced Jones fracture). | Most metatarsal stress fractures (e.g., 2nd-4th), navicular (non-displaced), calcaneus, distal tibia with appropriate offloading and activity modification. |
| Osteochondral Lesions | Large (>10-15mm), deep, unstable lesions (Stage III/IV Berndt & Harty), loose bodies, persistent pain after adequate conservative trial. | Small, stable, asymptomatic lesions, or symptomatic lesions responsive to initial activity modification, bracing, and injections. |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is the cornerstone of successful foot and ankle surgery, directly informed by comprehensive radiographic evaluation. Beyond standard anteroposterior (AP), lateral, and oblique views, specific stress views or weight-bearing radiographs are often critical. For complex deformities or intra-articular fractures, advanced imaging such as computed tomography (CT) with 3D reconstructions and magnetic resonance imaging (MRI) may be indispensable to delineate fracture patterns, assess articular congruity, quantify deformity, and evaluate soft tissue injury (e.g., ligamentous tears, cartilage damage).
Pre-Operative Planning Steps:
1.
Diagnosis Confirmation:
Correlate clinical findings with imaging to confirm the primary diagnosis and exclude concomitant pathologies.
2.
Deformity Analysis:
For reconstructive cases (e.g., flatfoot, hallux valgus), precise measurements from weight-bearing radiographs (e.g., Meary's angle, Talar-1st Metatarsal angle, calcaneal pitch, talonavicular coverage, Intermetatarsal angle, Hallux Valgus Angle) guide osteotomy planning and fusion angles.
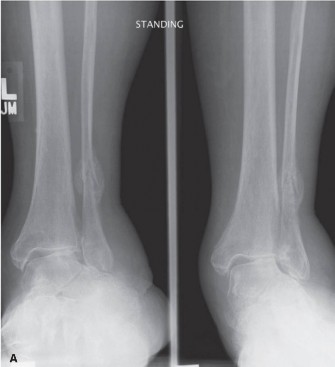
3.
Fracture Pattern Delineation:
For fractures, radiographs identify displacement, comminution, articular involvement, and stability. CT scans further characterize these, aiding in fragment reduction strategy and implant selection.
4.
Implant Selection and Templating:
Radiographs are used to template appropriate implant size and type (e.g., plates, screws, external fixators, fusion nails). This ensures the correct instrumentation is available and reduces operative time.
5.
Surgical Approach Selection:
Based on the pathology and desired reduction/fixation, the optimal surgical approach is chosen to minimize soft tissue compromise and maximize exposure.
6.
Potential Complications Mitigation:
Anticipate challenges such as poor bone quality, neurovascular structures at risk, or compromised soft tissues based on imaging.
Patient Positioning:
Patient positioning varies significantly depending on the anatomical region and surgical procedure.
*
Supine Position:
Most common for forefoot, midfoot, and anterior ankle approaches. A bump under the ipsilateral hip can internally rotate the limb for better access to the medial ankle or dorsal foot. A tourniquet is typically applied to the thigh.
*
Lateral Decubitus Position:
Used for lateral ankle approaches (e.g., fibular fracture fixation, peroneal tendon repair) or medial approaches to the hindfoot, providing unrestricted access.
*
Prone Position:
Essential for posterior ankle and hindfoot approaches (e.g., calcaneal osteotomy, Achilles repair, posterior ankle arthroscopy). Ensure adequate padding and pressure relief.
*
Semi-lateral (beach chair):
Can be useful for certain posterior-medial or posterior-lateral approaches to the ankle/hindfoot.
In all positions, careful padding of bony prominences, monitoring of neurovascular status, and appropriate limb draping are essential. The image intensifier (fluoroscopy) is positioned to allow for immediate intra-operative radiographic assessment of reduction and fixation.
Detailed Surgical Approach / Technique
Given the broad scope of "Foot & Ankle Pain," a comprehensive step-by-step description for every possible surgical intervention is not feasible. Instead, this section will outline general principles and common techniques, highlighting how radiographic findings directly influence intraoperative decision-making, reduction, and fixation. We will focus on key aspects relevant to fracture fixation, arthrodesis, and osteotomy.
General Principles of Surgical Exposure:
*
Incision Planning:
Incisions are planned to optimize exposure, avoid vital neurovascular structures, and ensure adequate soft tissue coverage. Radiographs help identify underlying bony landmarks and potential displacement patterns.
*
Soft Tissue Dissection:
Careful, atraumatic dissection is crucial to preserve skin flaps, tendons, nerves, and vessels. Knowledge of internervous planes is vital (e.g., between the tibialis anterior and extensor hallucis longus for dorsal ankle access, or between the Achilles tendon and flexor hallucis longus for posterior access).
*
Hemostasis:
A tourniquet is almost universally employed to achieve a bloodless field, enhancing visualization.
Fracture Reduction and Fixation (e.g., Ankle, Pilon, Calcaneus, Talus, Lisfranc):
Radiographs are paramount for understanding the initial fracture pattern and guiding reduction maneuvers.
1.
Exposure:
An appropriate approach is chosen (e.g., anterolateral for pilon, posterolateral for calcaneus, medial and lateral for bimalleolar ankle).
2.
Debridement:
Hematoma and small, non-articular bone fragments may be removed to facilitate visualization.
3.
Anatomical Reduction:
This is the primary goal, especially for articular fractures.
*
Direct Reduction:
Using bone clamps, dental picks, or joy sticks to manipulate fragments under direct visualization.
*
Indirect Reduction:
Ligamentotaxis or external fixator application may be used to restore length and alignment.
*
Radiographic Guidance:
Fluoroscopy is used continuously to assess reduction in multiple planes (AP, lateral, oblique views). For instance, in an ankle fracture, reduction is confirmed by restoring the ankle mortise integrity. In pilon fractures, articular congruity is meticulously checked.

4.
Temporary Fixation:
K-wires are frequently used to temporarily hold reduced fragments.
5.
Definitive Fixation:
*
Plates and Screws:
Commonly used for metaphyseal and diaphyseal fractures, providing rigid fixation. Contoured plates adapted to the bone's anatomy are preferred.
*
Lag Screws:
Applied for interfragmentary compression in spiral or oblique fractures, crucial for articular stability.
*
Screws:
Used alone for non-displaced fractures or to provide compression across an articular surface.
*
Syndesmotic Screws:
For unstable ankle syndesmosis injuries, fixed after anatomical reduction of the fibula to the tibia. Post-operative radiographs confirm reduction and screw placement.
*
Intramedullary Nails:
Less common in the foot/ankle but used for certain calcaneal or talar body fractures, or metatarsal fractures.
*
External Fixation:
Employed for high-energy injuries with significant soft tissue compromise (e.g., open fractures, pilon fractures with swelling) as a staged procedure or definitive fixation in certain situations.
6.
Final Radiographic Check:
Ensure all hardware is appropriately placed, reduction is maintained, and no iatrogenic damage has occurred.
Arthrodesis (Fusion) Techniques (e.g., Ankle, Subtalar, TMT Joints):
Used for end-stage arthritis, severe deformity, or instability. Radiographs guide joint preparation and hardware placement.
1.
Joint Exposure:
Appropriate approach to the specific joint (e.g., anterior for ankle, lateral for subtalar, dorsal for TMT joints).
2.
Cartilage Resection:
All articular cartilage and subchondral bone is removed down to bleeding cancellous bone to promote fusion. Deformity correction is performed at this stage.

3.
Bone Grafting:
Autograft or allograft may be used to enhance fusion rates, especially in cases of bone loss or revision surgery.
4.
Compression and Fixation:
*
Screws:
Most common for intertarsal and ankle fusions, providing interfragmentary compression.
*
Plates:
Useful for providing rigid fixation across larger joints or in the presence of significant bone loss (e.g., ankle fusion plates, locking plates for TMT fusions).
*
Intramedullary Nails:
Increasingly popular for hindfoot and ankle fusions, particularly in patients with poor bone quality, neuropathy, or revision cases, offering substantial stability.
5.
Radiographic Confirmation:
Ensure anatomical alignment is restored (e.g., neutral ankle dorsiflexion, 5-7° hindfoot valgus for subtalar fusion), and hardware is well-positioned for optimal compression.
Osteotomy Techniques (e.g., Calcaneal, Metatarsal, Tibial):
Used to correct bony deformities, re-align joints, or redistribute load. Radiographs guide the location and amount of correction.
1.
Exposure:
Approach is tailored to the specific bone and osteotomy site.
2.
Osteotomy Creation:
Precise bone cuts are made using oscillating saws, ensuring controlled translation, rotation, or angular correction.
3.
Correction:
The bony fragments are manipulated to achieve the desired alignment.
4.
Fixation:
Screws, plates, or K-wires are used to stabilize the corrected osteotomy.

5.
Radiographic Assessment:
Intraoperative fluoroscopy confirms the desired correction and stable fixation. Postoperative radiographs monitor healing and maintenance of correction.
Complications & Management
Despite meticulous surgical technique and thorough pre-operative planning, complications can arise in foot and ankle surgery. Radiographs play a critical role in diagnosing and monitoring many of these issues.
Common Complications in Foot & Ankle Surgery:
| Complication | Incidence (Approx.) | Radiographic Findings & Management | Salvage Strategies |
|---|---|---|---|
| Nonunion | 5-15% (variable by site & patient factors) | Persistent fracture line or absent trabecular bridging after 6-9 months on plain radiographs, often confirmed by CT. Sclerosis at fracture margins. Hardware loosening or failure. | Revision ORIF with debridement, bone grafting (autograft/allograft), electrical/ultrasound stimulation, more rigid fixation (e.g., IM nail). For fusions, repeat fusion with aggressive decortication and grafting. |
| Malunion | 5-20% (variable by site) | Radiographs show angular or rotational deformity, shortening, or articular step-off that significantly alters biomechanics. Often causes pain, secondary arthritis, or altered gait. | Corrective osteotomy (e.g., supramalleolar osteotomy for ankle malunion, calcaneal osteotomy), arthrodesis for severe secondary arthritis. |
| Infection (SSI) | 1-5% (superficial), <1% (deep) | Early: Soft tissue swelling, cellulitis (clinically). Late (osteomyelitis): Periosteal reaction, cortical destruction, sequestrum/involucrum on radiographs (late finding, often requires MRI/CT/bone scan for earlier diagnosis). Radiolucency around hardware suggests loosening. | Superficial: Oral antibiotics, wound care. Deep (SSI/osteomyelitis): Surgical debridement, irrigation, IV antibiotics, hardware removal (if stable union), staged reconstruction, plastic surgery consultation for soft tissue coverage. Arthrodesis in severe cases of joint infection. |
| Hardware Failure | 2-10% (can be higher with nonunion) | Radiographs show broken plates/screws, screw pull-out, or bending. Often indicative of nonunion or inadequate initial fixation. | Revision fixation with stronger implants, bone grafting if nonunion is present, removal of symptomatic hardware after healing. If due to nonunion, address nonunion simultaneously. |
| Nerve Injury | 1-5% (e.g., superficial peroneal, sural nerve) | No direct radiographic findings. Clinically presents as numbness, paresthesia, or motor weakness. | Observation, nerve protection, gabapentin/pregabalin for neuropathic pain. Surgical exploration and neurolysis/repair for persistent or severe symptoms (rarely required for iatrogenic injury). |
| Vascular Injury | Rare (<0.1%) | No direct radiographic findings (unless angiogram performed). Clinically presents as absent pulses, pallor, cold extremity. | Immediate surgical exploration, vascular repair/grafting. May lead to limb loss if untreated. |
| Avascular Necrosis (AVN) | Variable (e.g., Talus 10-50% with displaced neck fractures, Navicular 5-10% with certain fractures) | Increased bone density (sclerosis) or collapse of the bone fragment on radiographs. Fragmentation and joint collapse in late stages. MRI is more sensitive for early detection. | For talar AVN, early: core decompression, bone grafting. Late: arthrodesis (talonavicular, tibiotalar), prosthetic replacement. Navicular AVN: naviculectomy, fusion. |
| Thromboembolic Events (DVT/PE) | 1-5% (without prophylaxis), <1% (with prophylaxis) | No direct radiographic findings. Chest X-ray for PE may show pleural effusion or atelectasis, but CTPA is diagnostic. | Prophylactic anticoagulation is key. Treatment: full anticoagulation. |
| Reflex Sympathetic Dystrophy (CRPS) | <1-5% | Early: Normal. Later: Patchy osteopenia (Sudeck's atrophy) on radiographs, often with periarticular soft tissue swelling. Bone scan can show diffuse uptake. | Multimodal approach: physical therapy, pain management (nerve blocks, neuromodulators), pharmacological agents (NSAIDs, gabapentinoids, calcitonin). Referral to pain clinic. |
| Stiffness/Arthrofibrosis | Common (variable) | Radiographs may show joint space narrowing, heterotopic ossification, or soft tissue calcification around joints. | Aggressive physical therapy, manipulation under anesthesia. Arthroscopic or open arthrolysis/capsulectomy for recalcitrant cases. |
Management Principles:
*
Early Recognition:
Vigilant post-operative monitoring and prompt investigation of symptoms are crucial.
*
Imaging:
Routine post-operative radiographs assess implant position and bone healing. Additional views (stress views, oblique) or advanced imaging (CT, MRI) are used to investigate suspected complications.
*
Conservative Measures:
For mild complications (e.g., minor wound issues, mild stiffness), non-operative treatment with wound care, physical therapy, or medication may suffice.
*
Surgical Intervention:
For significant complications such as nonunion, severe malunion, deep infection, or hardware failure, re-operation is often required. This may involve revision fixation, debridement, bone grafting, or reconstructive procedures.
*
Multidisciplinary Approach:
Collaboration with infectious disease specialists, pain management, physical therapists, and plastic surgeons is often necessary for complex complications.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an integral component of the surgical journey, crucial for restoring function, preventing complications, and achieving optimal long-term outcomes. Protocols are tailored to the specific surgery, patient factors, and the stability of fixation, with radiographs guiding progression.
General Principles:
1.
Protection of Repair/Reconstruction:
The primary goal initially is to protect the surgical site. This often involves immobilization in a cast or boot, and strict weight-bearing restrictions.
*
Radiographic confirmation of stable fixation
is essential before initiating any weight-bearing.
*
Weight-bearing radiographs
may be taken to ensure stability under load.
2.
Pain and Edema Control:
Elevation, cryotherapy, compression, and analgesia are critical in the immediate post-operative period.
3.
Gradual Restoration of Range of Motion (ROM):
Once stable, early, controlled motion (passive or active-assisted) is initiated to prevent stiffness and improve joint nutrition, as determined by the surgeon and physical therapist.
* For fracture fixation, ROM typically begins once callus formation is evident on radiographs.
* For fusions, ROM is typically restricted at the fused joint, focusing on adjacent joint mobility.
4.
Progressive Weight-Bearing:
This is often the most critical aspect, dictated by the stability of fixation and evidence of healing on radiographs.
*
Non-weight-bearing (NWB):
Often for 4-8 weeks for fractures, and up to 12 weeks for fusions, particularly hindfoot.
*
Touch-down weight-bearing (TDWB) / Partial weight-bearing (PWB):
Progression is based on radiographic signs of early callus and clinical pain tolerance.
*
Full weight-bearing (FWB):
Allowed once solid radiographic union or fusion is confirmed, and the patient demonstrates adequate strength and balance.
5.
Strengthening and Proprioception:
Once weight-bearing is initiated, progressive strengthening exercises for ankle dorsiflexors, plantarflexors, invertors, and evertors, along with balance and proprioceptive training, are introduced.
6.
Functional Activities and Return to Sport/Work:
Tailored to individual goals, involving sport-specific drills, occupational therapy, and gradual return to previous activities. This phase requires significant patience and compliance.
* Return to high-impact activities typically requires solid radiographic union and excellent functional recovery, often 6-12 months post-surgery.
Radiographic Monitoring in Rehabilitation:
*
Initial Post-op:
To confirm hardware position and reduction.
*
2-week / 6-week / 12-week intervals:
To assess early callus formation, maintenance of reduction, signs of infection, or hardware issues.
*
3-6 month post-op:
To confirm union/fusion and guide transition to full activity. For fusions, bridging trabeculae across the joint space is the primary sign. For fractures, cortical bridging across at least three cortices is often considered sufficient.
*
As needed:
For new pain, swelling, or suspected complications.
Specific Considerations:
*
Ankle Fractures:
NWB for 4-6 weeks in a boot/cast, followed by progressive weight-bearing and ROM. Syndesmotic injuries often require longer protection.
*
Hindfoot Fusions (Subtalar, Triple):
NWB for 8-12 weeks in a cast, then gradual PWB in a CAM boot for another 4-8 weeks.
*
Lisfranc Injuries (ORIF/Fusion):
NWB for 6-12 weeks, followed by controlled weight-bearing in a boot. Fusion typically requires longer NWB.
*
Achilles Tendon Repair:
Early protected motion with controlled dorsiflexion, NWB initially then gradual weight-bearing in a boot with heel lifts.
Effective communication between the surgeon, physical therapist, and patient is paramount to successful rehabilitation, ensuring compliance and optimizing outcomes.
Summary of Key Literature / Guidelines
The management of foot and ankle pain and its surgical sequelae is continually refined through evidence-based practice. Radiographs are consistently cited as the initial and most critical diagnostic tool across numerous guidelines and consensus statements.
Diagnostic Imaging Guidelines:
*
American Academy of Orthopaedic Surgeons (AAOS):
Emphasizes plain radiographs as the first-line imaging for acute ankle and foot injuries, guiding further advanced imaging like CT or MRI when fracture patterns are complex, intra-articular involvement is suspected, or soft tissue injury needs evaluation (e.g., Ottawa Ankle Rules for fracture exclusion).
*
Emergency Medicine Guidelines (e.g., Ottawa Ankle/Foot Rules):
These clinical decision rules, while primarily for reducing unnecessary radiographs, highlight scenarios where radiographs
are
indicated (e.g., inability to bear weight, bony tenderness over specific landmarks). When radiographs are obtained, their interpretation directly impacts management.
Surgical Management Principles:
*
Fractures:
Guidelines consistently advocate for anatomical reduction and stable internal fixation for displaced intra-articular fractures (e.g., ankle, pilon, calcaneus, talus, Lisfranc) to restore joint congruity and minimize post-traumatic arthritis. Evidence suggests superior outcomes with anatomical reduction versus non-anatomical for most articular injuries.
*
Lisfranc injuries:
Current consensus supports surgical stabilization for all true Lisfranc injuries with instability or displacement, with primary arthrodesis gaining favor over ORIF for severe ligamentous injuries or chronic instability due to potentially better long-term outcomes and lower rates of re-operation. Radiographic parameters (e.g., diastasis >2mm) are key diagnostic criteria.
*
Pilon fractures:
Staged management with initial external fixation for soft tissue healing followed by ORIF with meticulous articular reduction is the accepted standard for high-energy injuries. Radiographs and CT scans are indispensable for classification and surgical planning.
*
Arthritis:
Surgical management (arthrodesis or arthroplasty) is typically reserved for end-stage arthritis refractory to comprehensive non-operative management.
*
Ankle Arthrodesis vs. Total Ankle Arthroplasty (TAA):
Literature demonstrates comparable patient-reported outcomes for both, with TAA offering motion preservation. The choice is patient-specific, influenced by age, activity level, deformity, and bone quality. Radiographs are critical for assessing the extent of arthritis and bone stock.
*
Deformities:
Surgical correction of complex deformities like adult acquired flatfoot or severe hallux valgus is guided by comprehensive radiographic analysis (weight-bearing views) to understand the sagittal and coronal plane pathology. Evidence supports multi-planar correction combining soft tissue procedures with osteotomies and fusions to restore optimal foot alignment and function.
*
Adult Acquired Flatfoot Deformity (AAFD):
Progression from flexible to rigid deformity, as assessed clinically and radiographically, guides surgical choice from tendon transfers/osteotomies to fusions (e.g., subtalar, triple arthrodesis).
Evidence-Based Outcomes:
* Numerous studies highlight the strong correlation between accurate radiographic diagnosis, appropriate surgical planning, and positive patient outcomes.
* The importance of meticulous surgical technique, particularly achieving and maintaining anatomical reduction in fractures and fusions, is consistently reinforced by evidence.
* High-quality rehabilitation protocols, guided by radiographic healing, are shown to minimize stiffness, maximize functional recovery, and facilitate return to activity.
In conclusion, radiographs are not merely images; they are diagnostic windows into the complex biomechanics and pathologies of the foot and ankle. Their astute interpretation is foundational for guiding effective, evidence-based surgical decision-making and remains an indispensable tool for orthopedic surgeons in the comprehensive management of foot and ankle pain.
Clinical & Radiographic Imaging