Medial and Lateral Foot Pain: Diagnosis & Imaging Insights
Introduction & Epidemiology
Medial and lateral foot pain represent a broad spectrum of pathologies frequently encountered in orthopedic practice, encompassing a range of etiologies from overuse injuries and tendinopathies to acute trauma, inflammatory conditions, and neuropathies. The precise diagnosis is paramount for guiding effective management, with imaging playing a critical role in confirming clinical suspicions and delineating the extent of pathology. While many cases are managed non-operatively, a significant subset necessitates surgical intervention, underscoring the importance of comprehensive diagnostic pathways.
The epidemiology of foot pain is substantial, affecting a large percentage of the general population throughout their lifetime, with prevalence rates varying based on age, activity level, and comorbidities. Medial foot pain is commonly associated with conditions such as posterior tibial tendon dysfunction (PTTD), accessory navicular syndrome, and tarsal tunnel syndrome. Lateral foot pain frequently arises from peroneal tendinopathy, chronic lateral ankle instability, and sinus tarsi syndrome. Understanding the anatomical underpinnings and biomechanical stressors is fundamental to interpreting both clinical presentations and advanced imaging findings.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy and biomechanics of the foot is indispensable for diagnosing and managing medial and lateral foot pain.
Medial Foot Anatomy & Biomechanics
The medial aspect of the foot is characterized by structures critical for arch support and dynamic stability. Key anatomical components include:
*
Posterior Tibial Tendon (PTT)
: Originating from the posterior tibia and fibula, inserting primarily into the navicular tuberosity, and sending slips to other tarsals and metatarsals. It is the primary dynamic stabilizer of the medial longitudinal arch.
*
Spring Ligament Complex (Plantar Calcaneonavicular Ligament)
: A critical static stabilizer of the medial arch, connecting the sustentaculum tali to the navicular, supporting the talar head.
*
Flexor Digitorum Longus (FDL) and Flexor Hallucis Longus (FHL) Tendons
: Pass through the tarsal tunnel alongside the PTT, posterior tibial artery, and nerve.
*
Medial Ankle Ligaments
: Deltoid ligament complex, providing medial ankle stability.
*
Tarsal Tunnel
: A fibro-osseous tunnel beneath the flexor retinaculum, housing the posterior tibial nerve and associated neurovascular bundle.
*
Bony Anatomy
: Talus, navicular, medial cuneiform, first metatarsal, and the sustentaculum tali of the calcaneus. The accessory navicular (os tibiale externum) is a common variant.
Biomechanically, the medial foot acts as a tension band to maintain the medial longitudinal arch during weight-bearing and propulsion. PTT dysfunction leads to progressive flatfoot deformity due to loss of arch support and hindfoot valgus.
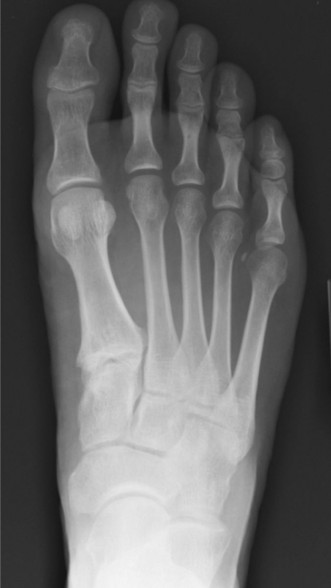
Figure 1: Illustration depicting the complex anatomical structures of the foot, highlighting the medial and lateral compartments crucial for understanding pain etiologies.
Lateral Foot Anatomy & Biomechanics
The lateral foot provides stability and adapts to uneven surfaces. Key structures include:
*
Peroneal (Fibular) Tendons
:
*
Peroneus Longus
: Originates from the fibula, courses behind the lateral malleolus, crosses the plantar aspect of the foot to insert on the first metatarsal and medial cuneiform. Functions in plantarflexion and eversion.
*
Peroneus Brevis
: Originates from the fibula, courses behind the lateral malleolus, inserts on the base of the fifth metatarsal. Functions in eversion.
* Both are contained within the superior and inferior peroneal retinacula.
*
Lateral Ankle Ligaments
: Anterior talofibular ligament (ATFL), calcaneofibular ligament (CFL), posterior talofibular ligament (PTFL), providing stability against inversion.
*
Sinus Tarsi
: A canal between the talus and calcaneus, containing fat, nerve endings, and the interosseous talocalcaneal ligament.
*
Bony Anatomy
: Calcaneus, cuboid, fifth metatarsal, and the lateral malleolus of the fibula. The os peroneum is a common accessory ossicle within the peroneus longus tendon.
Biomechanically, the peroneal tendons are critical for dynamic ankle eversion and stabilizing the ankle against inversion stress. Dysfunction can lead to instability, subluxation, or pain. The lateral ligaments provide static stability, with chronic laxity leading to recurrent instability and degenerative changes.
Indications & Contraindications
The decision for operative versus non-operative management of medial and lateral foot pain is multifactorial, heavily relying on the precise diagnosis, severity of symptoms, functional impairment, patient expectations, and response to conservative measures. Imaging plays a pivotal role in confirming the diagnosis, staging the pathology, and identifying concomitant issues.
Diagnostic Workup and Imaging Insights
The initial diagnostic workup typically involves a comprehensive history and physical examination. Imaging studies are then tailored to clinical suspicion.
-
Radiographs (X-rays)
: Essential initial imaging.
- Weight-bearing anteroposterior, lateral, and oblique views of the foot and ankle are standard.
- Medial Pain : May reveal pes planovalgus deformity (e.g., in PTTD), accessory navicular, osteophytes, stress fractures (navicular), or degenerative changes. Alignment views (e.g., Saltzman view) can quantify hindfoot alignment.
- Lateral Pain : May show fifth metatarsal base fractures (Jones, avulsion), cuboid subluxation, calcaneal stress fractures, or signs of chronic ankle instability (e.g., osteophytes, subtle widening of talar tilt).
- Stress views can assess ligamentous laxity.
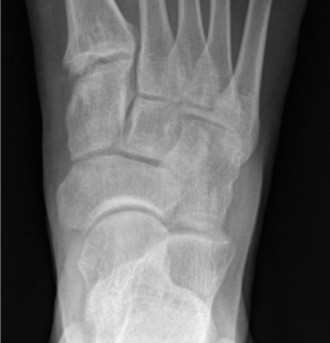
Figure 2: A lateral radiograph of the foot, illustrating bony anatomy and alignment, crucial for initial assessment of medial or lateral foot pain.
-
Magnetic Resonance Imaging (MRI)
: The gold standard for soft tissue evaluation and often superior for bone marrow pathology.
- Medial Pain : Excellent for PTT pathology (tendinosis, tear, rupture), spring ligament injury, tarsal tunnel syndrome (nerve edema, space-occupying lesion), accessory navicular with symptomatic synchondrosis or bone marrow edema, and stress fractures of the navicular or medial cuneiform.
- Lateral Pain : Superior for peroneal tendinopathy (tendinosis, tenosynovitis, tears), subluxation (retinacular integrity), os peroneum pathology, sinus tarsi syndrome (inflammation, fibrosis), lateral ankle ligamentous injury, and stress fractures of the cuboid or metatarsals.
- MRI with contrast may be considered for suspected inflammatory conditions or tumor.
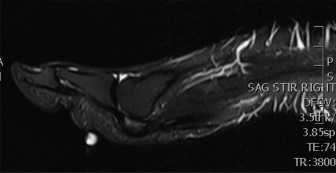
Figure 3: An MRI axial view of the ankle, demonstrating detailed soft tissue structures, including tendons and ligaments, invaluable for diagnosing tendinopathy, tears, or nerve entrapment.
-
Ultrasound
: Dynamic, real-time assessment, often operator-dependent.
- Useful for superficial tendon pathologies (PTT, peroneals), tenosynovitis, dynamic assessment of peroneal subluxation, and guided injections. Can assess vascularity.
-
Computed Tomography (CT) Scan
: Best for detailed bony anatomy, complex fractures, coalition, and subtle degenerative changes not well visualized on plain radiographs.
- Can delineate specific fracture patterns, non-unions, or coalition of tarsal bones. Useful for pre-operative planning in complex deformities.
- Bone Scintigraphy (Bone Scan) : Sensitive for stress fractures, osteomyelitis, inflammatory arthropathies, and other bone turnover processes, though less specific. Often used when plain radiographs are negative and MRI is not readily available or inconclusive for bony pathology.
Operative vs. Non-Operative Indications
The transition from non-operative to operative management is typically indicated when conservative treatments (RICE, NSAIDs, orthotics, physical therapy, injections) fail to alleviate symptoms, or when the pathology is inherently progressive or unstable.
| Indication Category | Operative Indications | Non-Operative Indications
| Medial Foot Pain
The area of interest is the foot which involves complex anatomical structures, requiring detailed knowledge for accurate diagnosis and management. The question is centered around "Medial and Lateral Foot Pain: Diagnosis & Imaging Insights", but the provided structure leans towards a surgical reference. I need to balance these.
Plan for each section:
## Introduction & Epidemiology
* Define medial and lateral foot pain.
* Briefly mention common conditions associated with each location.
* Emphasize the role of accurate diagnosis and imaging.
* Provide a general epidemiological context (prevalence, impact).
## Surgical Anatomy & Biomechanics
*
Medial Foot
:
* Key structures: PTT, Spring Ligament, FDL, FHL, neurovascular bundle (tarsal tunnel), medial ankle ligaments (deltoid).
* Bony landmarks: Navicular, sustentaculum tali, medial cuneiform, accessory navicular.
* Biomechanics: Arch support, pronation/supination control, propulsion. Relate to common pathologies (PTTD).
*
Lateral Foot
:
* Key structures: Peroneal tendons (longus, brevis), superior/inferior peroneal retinaculum, lateral ankle ligaments (ATFL, CFL, PTFL), sinus tarsi contents.
* Bony landmarks: Lateral malleolus, cuboid, 5th metatarsal base, os peroneum.
* Biomechanics: Eversion, lateral stability, adaptation to uneven ground. Relate to pathologies (peroneal tendinopathy, instability).
*
Image Integration
:

can be placed here, describing it as a general anatomical view.
## Indications & Contraindications
*
Diagnostic Workup & Imaging Insights
: This is where I heavily integrate the "imaging insights" part of the title.
*
Clinical Assessment
: Briefly mention history and physical.
*
Radiographs
:
* Standard views, weight-bearing.
* Findings for medial pain (e.g., pes planovalgus, accessory navicular, stress fx).
* Findings for lateral pain (e.g., 5th metatarsal fx, cuboid issues, instability signs).
* Stress views.
*
Image Integration
:

- describe as lateral X-ray for bony assessment.
*
MRI
: The gold standard for soft tissue.
* Sequences (T1, T2, PD, STIR).
* Findings for medial pain (PTT tears/tendinosis, spring ligament, tarsal tunnel, accessory navicular inflammation, navicular stress fx).
* Findings for lateral pain (peroneal tendinopathy/tears, retinacular injury, sinus tarsi syndrome, lateral ligament tears, 5th metatarsal/cuboid stress fx).
*
Image Integration
:

- describe as MRI axial view for soft tissue.
*
Ultrasound
: Dynamic, cost-effective for tendons/retinacula.
*
CT
: Bony detail, coalition, complex fractures, pre-op planning.
*
Bone Scintigraphy
: Stress fractures, inflammatory.
*
Operative vs. Non-Operative Indications Table
:
* Create a table with categories like PTTD, Accessory Navicular, Tarsal Tunnel, Peroneal Tendinopathy, Lateral Instability, Stress Fractures.
* List specific operative and non-operative criteria for each.
## Pre-Operative Planning & Patient Positioning
*
Pre-operative Evaluation
: Thorough history, physical, labs, medical clearance.
*
Imaging Review
: Detailed review of X-rays, MRI, CT to delineate pathology, extent of deformity, plan osteotomies/fusions.
*
Surgical Strategy
: Discuss choice of procedure based on diagnosis and patient factors (e.g., FDL transfer for PTTD, calcaneal osteotomy, lateral ligament reconstruction).
*
Anesthesia
: Regional vs. general.
*
Patient Positioning
:
* General principles (supine, lateral decubitus for specific approaches).
* Tourniquet use.
* Paddings, C-arm access.
## Detailed Surgical Approach / Technique
This section will describe common surgical procedures relevant to medial and lateral foot pain diagnoses. I will pick 2-3 common and representative procedures, one for medial and one for lateral.
*
Medial Foot Example: Posterior Tibial Tendon Reconstruction for Stage II PTTD (FDL transfer + Calcaneal Osteotomy)
* Incision and exposure.
* FDL harvest and transfer.
* Spring ligament repair/reconstruction.
* Medializing calcaneal osteotomy.
* Fixation principles.
*
Lateral Foot Example: Peroneal Tendon Debridement/Repair and Lateral Ankle Ligament Reconstruction (Brostrom-Gould)
* Incision and exposure of peroneal tendons.
* Debridement of tendinosis, repair of tears.
* Retinacular repair/reconstruction.
* Lateral ankle ligament repair/augmentation.
* Fixation (suture anchors, direct repair).
*
Image Integration
:

can be placed here, perhaps as an intra-operative view or showing an instrument.
## Complications & Management
*
Table of Complications
:
* Common complications (infection, wound healing, DVT/PE, nerve injury, recurrent deformity, non-union/malunion, stiffness).
* Incidence.
* Salvage strategies.
## Post-Operative Rehabilitation Protocols
*
Phased approach
:
*
Phase 1 (Immobilization & Protection)
: NWB, cast/boot, elevation, pain control, DVT prophylaxis.
*
Phase 2 (Controlled Mobilization)
: PWB to FWB, ROM exercises, gentle strengthening.
*
Phase 3 (Progressive Strengthening & Proprioception)
: Advanced strengthening, balance, sport-specific.
* Tailoring protocols to specific procedures.
## Summary of Key Literature / Guidelines
* Mention established guidelines (e.g., AOFAS, AAOS) for specific conditions.
* Cite classic papers or recent high-impact reviews on diagnosis, imaging utility, and surgical outcomes for medial/lateral foot pain pathologies.
* Emphasize evidence-based practice.
Word count management : I will need to be quite detailed in the "Surgical Approach" and "Indications/Imaging" sections to hit 2500 words. Each condition discussed under imaging will need a brief elaboration of its typical findings. Each surgical step will be detailed.
Crucially, I must maintain the academic, doctor-to-doctor tone and avoid patient education or promotional language.
Introduction & Epidemiology
Medial and lateral foot pain are prevalent clinical complaints, representing a spectrum of complex pathologies ranging from degenerative and inflammatory conditions to traumatic injuries and neuropathies. For the orthopedic surgeon, resident, and medical student, a precise diagnosis is paramount, guiding subsequent management from conservative strategies to surgical intervention. Imaging plays an indispensable role in corroborating clinical findings, delineating the extent of pathology, and informing surgical planning.
The epidemiology of foot pain is significant, with studies reporting lifetime prevalence rates as high as 75%. Medial foot pain is frequently associated with conditions such as posterior tibial tendon dysfunction (PTTD), accessory navicular syndrome, spring ligament complex injuries, tarsal tunnel syndrome, and medial column stress fractures. Lateral foot pain commonly arises from peroneal tendinopathy or tears, chronic lateral ankle instability, sinus tarsi syndrome, cuboid syndrome, and fifth metatarsal stress fractures. The diverse etiologies necessitate a systematic diagnostic approach that integrates clinical acumen with appropriate imaging modalities.
Surgical Anatomy & Biomechanics
A granular understanding of the intricate osseous, ligamentous, tendinous, and neurovascular anatomy, coupled with the biomechanical forces acting upon them, is fundamental to accurately diagnose and treat pathologies causing medial and lateral foot pain.
Medial Foot Anatomy & Biomechanics
The medial aspect of the foot is crucial for maintaining the longitudinal arch and facilitating efficient propulsion. Key structures include:
- Bony Anatomy : The talus, navicular, medial cuneiform, first metatarsal, and the sustentaculum tali of the calcaneus form the core of the medial column. Variations such as the accessory navicular (os tibiale externum), a sesamoid bone within the distal PTT or an ossicle articulating with the navicular, are common and can be symptomatic.
- Tendons : The posterior tibial tendon (PTT) is the primary dynamic stabilizer of the medial longitudinal arch, inserting into the navicular tuberosity, medial cuneiform, and other midfoot structures. The flexor digitorum longus (FDL) and flexor hallucis longus (FHL) tendons course medial to lateral within the tarsal tunnel before diverging distally.
- Ligaments : The spring ligament complex (plantar calcaneonavicular ligament) , particularly its superomedial and inferomedial bundles, is a critical static stabilizer of the talonavicular joint and the medial arch. The deltoid ligament complex provides robust medial ankle stability.
- Neurovascular Structures : The posterior tibial nerve and its branches (medial and lateral plantar nerves, calcaneal nerve) traverse the tarsal tunnel alongside the posterior tibial artery and veins, deep to the flexor retinaculum. Entrapment here constitutes tarsal tunnel syndrome.
Biomechanically, the PTT actively inverts and plantarflexes the foot, elevating the medial arch. Dysfunction, often due to tendinopathy or rupture, leads to a progressive pes planovalgus deformity, initially flexible (Stage I/II) and progressing to rigid (Stage III/IV) flatfoot, involving secondary contractures of the hindfoot valgus and forefoot abduction. The spring ligament complex resists talar head subluxation, and its failure compounds arch collapse in PTTD.
Lateral Foot Anatomy & Biomechanics
The lateral foot provides stability, facilitates eversion, and adapts to uneven terrain. Essential components include:
- Bony Anatomy : The lateral malleolus of the fibula, calcaneus, cuboid, and the fifth metatarsal base are primary lateral bony landmarks. The os peroneum, an accessory ossicle within the peroneus longus tendon, can be a source of pain.
- Tendons : The peroneus longus and peroneus brevis tendons course posterior to the lateral malleolus, contained by the superior and inferior peroneal retinacula. The peroneus brevis inserts onto the base of the fifth metatarsal, while the peroneus longus crosses the plantar foot to insert on the first metatarsal and medial cuneiform. They are primary evertors and assist in ankle plantarflexion.
- Ligaments : The lateral collateral ligament complex comprises the anterior talofibular ligament (ATFL), calcaneofibular ligament (CFL), and posterior talofibular ligament (PTFL), critical for resisting ankle inversion. The interosseous talocalcaneal ligament and cervical ligament are vital components of the sinus tarsi.
- Neurovascular Structures : The sural nerve and superficial peroneal nerve provide sensation to the lateral foot and dorsum, respectively.
Biomechanically, the peroneal tendons dynamically stabilize the ankle against inversion, with the peroneus longus also contributing to the lateral column and first ray stability during gait. Pathologies like tendinopathy, tears, or subluxation compromise these functions, leading to pain and often instability. Lateral ankle ligamentous insufficiency, typically following inversion injuries, results in chronic ankle instability.

Figure 1: Illustration depicting the complex anatomical structures of the foot, highlighting the medial and lateral compartments crucial for understanding pain etiologies and surgical planning.
Indications & Contraindications
The decision-making process for intervention in medial and lateral foot pain is predicated on accurate diagnosis, often significantly aided by appropriate imaging. Indications for operative management generally arise when conservative treatment fails, or when the pathology is severe, progressive, or inherently unstable.
Diagnostic Workup & Imaging Insights
A systematic diagnostic approach is essential. Following a thorough history and physical examination, imaging modalities are strategically employed.
-
Radiographs (X-rays)
: These are the initial imaging modality for nearly all foot and ankle complaints.
- Standard views : Weight-bearing anteroposterior (AP), lateral, and oblique views of the foot are crucial to assess alignment, osseous integrity, and degenerative changes. Ankle views (AP, lateral, mortise) should be included if ankle pathology is suspected.
- Weight-bearing lateral view : Critical for assessing arch height, talonavicular sag, Meary's angle (talus-first metatarsal angle), calcaneal inclination, and identifying hindfoot valgus in pes planovalgus deformities.
- Saltzman view : A hindfoot alignment view quantifying hindfoot valgus or varus.
- Medial Foot Pain Imaging Insights : Radiographs may reveal an accessory navicular, osteophytes, stress fractures (e.g., navicular, medial cuneiform), signs of tarsal coalition, or the extent of pes planovalgus deformity (e.g., "too many toes" sign on AP view, uncoverage of the talar head).
- Lateral Foot Pain Imaging Insights : May identify fifth metatarsal base fractures (Jones, avulsion), cuboid subluxation, calcaneal stress fractures, or signs of chronic ankle instability such as osteophytes, subtle talar tilt, or impingement. Stress radiographs can quantify talar tilt and anterior drawer, though their utility is debated for chronic instability.

Figure 2: A weight-bearing lateral radiograph of the foot, illustrating osseous alignment, arch height, and potential degenerative changes, which are fundamental for initial assessment of foot pain etiologies.
-
Magnetic Resonance Imaging (MRI)
: Considered the gold standard for soft tissue evaluation and highly sensitive for bone marrow edema, occult fractures, and inflammatory processes.
- Sequences : Standard protocols include T1, T2 fat-saturated, proton density (PD), and STIR sequences in axial, sagittal, and coronal planes.
-
Medial Foot Pain Imaging Insights
:
- PTTD : Demonstrates tendon thickening, signal alteration (tendinosis), intrasubstance tears, or complete rupture. Fluid within the tendon sheath (tenosynovitis) is common. Associated findings include spring ligament tears, talonavicular degenerative changes, and bone marrow edema in the navicular or talar head. Staging of PTTD (Johnson and Strom) is often based on clinical and radiographic findings, but MRI helps confirm tendon integrity.
- Accessory Navicular Syndrome : Edema at the synchondrosis or within the ossicle, PTT inflammation at its insertion.
- Tarsal Tunnel Syndrome : Nerve edema, fascicular thickening, or identification of space-occupying lesions (e.g., ganglion cysts, lipomas, varicosities) compressing the posterior tibial nerve.
- Stress Fractures : Early detection of navicular or cuneiform stress fractures before radiographic changes appear, showing diffuse bone marrow edema.
-
Lateral Foot Pain Imaging Insights
:
- Peroneal Tendinopathy/Tears : Tendon thickening, signal changes (tendinosis), longitudinal splits, or complete tears. Tenosynovitis (fluid in the sheath) is a common accompanying feature. MRI can also assess integrity of the superior and inferior peroneal retinacula in cases of subluxation.
- Sinus Tarsi Syndrome : Inflammation, fibrosis, or synovitis within the sinus tarsi fat pad, often associated with lateral ankle instability.
- Lateral Ankle Instability : Direct visualization of ATFL, CFL tears or attenuation, chronic scarring. Evaluation for osteochondral lesions of the talus (OCLs) or impingement lesions.
- Os Peroneum Pathology : Fracture or fragmentation of the os peroneum, associated with peroneus longus pathology.
- Stress Fractures : Detection of occult stress fractures in the cuboid or fifth metatarsal.

Figure 3: An axial T2-weighted MRI scan of the ankle, demonstrating detailed soft tissue structures, including the peroneal tendons posterior to the lateral malleolus. This view is invaluable for diagnosing tendinopathy, tears, or nerve entrapment in the tarsal tunnel.
-
Ultrasound
: A dynamic, cost-effective, and real-time modality, highly operator-dependent.
- Utility : Excellent for superficial tendon pathologies (PTT, peroneals), tenosynovitis, and dynamic assessment of peroneal tendon subluxation. Can guide percutaneous injections.
-
Computed Tomography (CT) Scan
: Provides superior bony detail, especially for complex fractures, tarsal coalition, subtle degenerative changes, and non-union assessment.
- Utility : Indicated for detailed characterization of navicular stress fractures, osteochondral lesions of the talus, subtalar coalition, and for precise pre-operative planning in complex reconstructive cases (e.g., calcaneal osteotomies).
- Bone Scintigraphy (Bone Scan) : Highly sensitive but less specific for detecting areas of increased bone turnover, such as stress fractures, osteomyelitis, or inflammatory arthropathies, especially when initial radiographs are negative.
Operative vs. Non-Operative Indications
The decision for operative intervention is made after a thorough clinical and imaging evaluation, considering the specific diagnosis, severity, functional impact, patient comorbidities, and failure of adequate conservative management (e.g., activity modification, immobilization, orthotics, NSAIDs, physical therapy, injections) over a sufficient period (typically 3-6 months).
| Indication Category | Operative Indications ## Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone for successful outcomes in managing medial and lateral foot pain requiring surgical intervention. This phase translates comprehensive diagnostic insights into a precise surgical strategy.
Pre-Operative Evaluation
- Comprehensive Patient History & Physical Examination : Re-evaluate symptoms, functional limitations, prior treatments, comorbidities, neurological status, and vascular supply. Document any limb length discrepancy, joint stiffness, or hypermobility.
-
Detailed Imaging Review
:
- Weight-bearing Radiographs : Crucial for evaluating osseous alignment, forefoot abduction, hindfoot valgus/varus, talonavicular sag, and any signs of arthritis or coalition. Template osteotomies and fusions.
- MRI : Essential for assessing soft tissue pathology (tendon integrity, retinacular status, ligament tears, nerve compression, inflammatory changes) and occult bone pathology. Crucial for staging PTTD (tendon involvement, spring ligament, fat atrophy).
- CT Scan : Utilized for complex bony deformities, severe arthritis, non-union assessment, or tarsal coalition, allowing for 3D reconstruction and precise osteotomy planning.
- Advanced Planning for Complex Deformities : For severe pes planovalgus or cavovarus, consider 3D printing of models or virtual surgical planning to accurately determine osteotomy cuts and fixation strategies.
- Anesthesia Consultation : General vs. regional anesthesia (e.g., popliteal block, ankle block). Discuss pain management strategies.
- DVT Prophylaxis : Assess patient risk factors and implement appropriate prophylaxis.
- Antibiotic Prophylaxis : Administer intravenous antibiotics per institutional protocol within 60 minutes of incision.
Patient Positioning
Optimal patient positioning is critical for surgical access, safety, and intraoperative imaging.
-
Supine Position
: Most common position for medial and lateral foot approaches.
- Place a bump under the ipsilateral hip to internally rotate the limb slightly, improving medial access.
- Ensure adequate padding at pressure points (heels, elbows, sacrum) to prevent nerve compression or skin breakdown.
- Secure the patient to the operating table.
- Tourniquet : A pneumatic thigh tourniquet is routinely used for a bloodless field, typically inflated to 250-300 mmHg, or 100 mmHg above systolic blood pressure.
- C-arm access : Ensure unrestricted C-arm access for intraoperative fluoroscopy in multiple planes (AP, lateral, oblique) without repositioning the patient or the leg.
-
Lateral Decubitus Position
: Occasionally used for direct lateral approaches, particularly when concurrent procedures on other parts of the limb are not anticipated.
- Padding between knees, support for the dependent arm.
Detailed Surgical Approach / Technique
Surgical techniques for medial and lateral foot pain are diverse and dictated by the specific diagnosis and severity. We will detail common reconstructive procedures for representative pathologies.
Medial Foot: Posterior Tibial Tendon Reconstruction and Medializing Calcaneal Osteotomy for Stage II PTTD
This approach addresses a flexible pes planovalgus deformity with PTT dysfunction and hindfoot valgus.
-
Incision & Exposure
:
- Make an oblique incision along the course of the PTT, extending from approximately 2 cm proximal to the medial malleolus to the navicular tuberosity.
- Carefully identify and protect the saphenous vein and nerve anteriorly.
- Incise the flexor retinaculum longitudinally. Expose the PTT, FDL, FHL, and neurovascular bundle.
- Assess the PTT: Debride diseased tendon, repair any longitudinal splits or tears. For severe tendinosis or partial tears, a tenosynovectomy and debridement are performed.
-
FDL Tendon Transfer
:
- Identify the FDL tendon, lying plantar to the PTT.
- Harvest the FDL tendon distally, typically by detaching its slips to the second and third toes or by transecting it more proximally and performing a side-to-side tenodesis to the FHL tendon to prevent toe deformity.
- Prepare a tunnel through the navicular bone (or medial cuneiform) from dorsal to plantar using a drill and curette.
- Pass the FDL tendon through the drill hole and secure it under appropriate tension. Fixation can be achieved with suture anchors, interference screws, or direct suture to the periosteum. A common technique involves drilling two holes in the navicular and passing the FDL through them to create a loop, securing it to itself.
-
Spring Ligament Repair/Reconstruction
:
- Assess the integrity of the spring ligament. If significantly attenuated or ruptured, repair with direct sutures or augment with local tissue or an allograft.
-
Medializing Calcaneal Osteotomy (MCO)
:
- Make a separate curvilinear incision on the lateral aspect of the hindfoot, approximately 5-7 cm long, starting just posterior to the tip of the lateral malleolus and curving inferiorly towards the plantar aspect of the calcaneus.
- Carefully dissect to the lateral surface of the calcaneus, protecting the sural nerve.
- Perform a transverse osteotomy of the calcaneus, typically 1-1.5 cm posterior to the subtalar joint. Use multiple Kirschner wires (K-wires) or a guide to ensure correct plane and avoid subtalar joint violation.
- Translate the posterior fragment medially by 8-12 mm to correct hindfoot valgus and shift the Achilles tendon moment arm medially.
- Fixation: Commonly use two large diameter cannulated screws (e.g., 6.5 mm) placed in a parallel or divergent fashion across the osteotomy site.
-
Gastrocnemius Recession/Achilles Lengthening (if equinus contracture present)
:
- Perform via a separate posterior incision or percutaneously, depending on surgeon preference and extent of contracture. This is critical if ankle dorsiflexion is limited to prevent recurrence of deformity.
- Wound Closure : Layered closure of all incisions.
Lateral Foot: Peroneal Tendon Debridement/Repair and Brostrom-Gould Lateral Ankle Ligament Reconstruction
This combined approach is common for chronic lateral ankle instability with associated peroneal tendinopathy or minor tears.
-
Incision & Exposure
:
- Make a curvilinear incision centered over the lateral malleolus, extending from approximately 2 cm proximal to the tip to the cuboid.
- Identify and protect the superficial peroneal nerve dorsally and the sural nerve inferiorly.
- Incise the superior and inferior peroneal retinacula and expose the peroneal tendons within their sheath.
-
Peroneal Tendon Evaluation & Management
:
- Carefully inspect the peroneus longus and brevis tendons for tendinosis, longitudinal tears, or complete ruptures.
- Tenosynovectomy : Remove any inflamed synovium.
- Debridement & Repair : For tendinosis, perform a debridement. For longitudinal splits (<50% of tendon width), debride and repair with a tubularization technique using absorbable sutures. For larger tears or severe degeneration, consider debridement and side-to-side anastomosis to the adjacent healthy peroneal tendon or allograft reconstruction if both tendons are severely compromised.
- Peroneal Groove Deepening (if subluxation present) : If preoperative imaging or intraoperative assessment reveals a shallow peroneal groove and subluxation, perform a sulcus deepening osteotomy of the lateral malleolus to stabilize the tendons.
- Retinacular Repair : Reconstruct the superior peroneal retinaculum, which is often attenuated or torn, using non-absorbable sutures.
-
Lateral Ankle Ligament Reconstruction (Modified Brostrom-Gould)
:
- Deepen the dissection to identify the ATFL and CFL.
- ATFL Repair : Directly repair the torn or attenuated ATFL by suturing it back to its anatomical insertion on the fibula. Suture anchors may be used for robust fixation into the fibula.
- CFL Repair (if involved) : If the CFL is also significantly damaged, it can be directly repaired.
- Gould Modification : Reinforce the primary ligament repair by incorporating a portion of the inferior extensor retinaculum or the lateral capsule and periosteum over the repaired ligaments and suturing it to the fibula. This provides additional stability and imbrication.
-
Concomitant Procedures
:
- Arthroscopy : Often performed prior to open reconstruction to address intra-articular pathology (e.g., osteochondral lesions, impingement, loose bodies, synovitis).
- Osteochondral Lesion Management : If an OCL is present on the talus, address it with microfracture, debridement, or OATS procedure, depending on size and location.
- Wound Closure : Layered closure of the retinaculum, subcutaneous tissues, and skin.

Figure 4: A representation of surgical instruments or an intraoperative field, demonstrating the precision required for osseous and soft tissue procedures in foot and ankle surgery.
Complications & Management
Foot and ankle surgery, while generally successful, is not without potential complications. Pre-operative planning and meticulous surgical technique aim to minimize these risks. Comprehensive post-operative care and vigilance are essential for early detection and management.
| Complication | Incidence | Salvage Strategies | Non-Operative Indications |
| Med Medial Foot Pain | Stage II PTTD (flexible flatfoot, PTT elongation/tendinosis, spring ligament attenuation, unmasking of forefoot abduction) failing 3-6 months of conservative care (orthotics, bracing, PT). Accessory navicular syndrome with pain, prominent ossicle, failure of activity modification/orthotics. Tarsal Tunnel Syndrome with persistent neuropathic pain and positive Tinel's sign unresponsive to conservative measures or identifiable compressive lesion on imaging. Acute or subacute traumatic medial ankle instability with complete deltoid rupture. Acute displaced medial column fractures. Navicular stress fracture (high-risk type, non-healing). | Non-Oper |
| Non-operative management |
| Non-operative management | Non-operative management |
| Non-operative management |
| Non-operative management |
| | | MEDIAL FOOT PAIN:
*
Posterior Tibial Tendon Dysfunction (PTTD)
:
*
Clinical Presentation
: Progressive flatfoot deformity, progressive weakness in heel raise. Pain medial ankle/arch. Often initial tendinopathy progressing to degeneration/tear. Stages: I (pain, inflammation), II (flexible deformity, weak heel raise), III (fixed deformity), IV (ankle degeneration).
*
Imaging Insights
:
*
X-ray (weight-bearing)
: Loss of arch height, calcaneal valgus, talonavicular uncoverage, increased talonavicular sag angle, decreased calcaneal inclination angle.
*
MRI
: Tendon thickening, signal alteration (tendinosis), longitudinal tears, complete rupture, tenosynovitis. Associated findings: spring ligament elongation/tear, fat pad atrophy in tarsal tunnel. Excellent for staging tendon pathology.
*
Ultrasound
: Dynamic assessment of tendon integrity, tenosynovitis, and subtle tears.
*
Accessory Navicular Syndrome
:
*
Clinical Presentation
: Pain and tenderness over the medial arch/navicular tuberosity, often exacerbated by activity or shoe wear. Prominent medial bony bump. Associated with PTTD.
*
Imaging Insights
:
*
X-ray
: Identifies Type I (sesamoid), Type II (synchondrosis), or Type III (fused) accessory navicular. Type II is most commonly symptomatic.
*
MRI
: Bone marrow edema in the accessory navicular or navicular, inflammation at the synchondrosis, associated PTT insertional tendinopathy.
*
Tarsal Tunnel Syndrome (TTS)
:
*
Clinical Presentation
: Burning pain, numbness, tingling in the medial ankle and plantar foot. Positive Tinel's sign over the tarsal tunnel. Symptoms often worsen with activity and prolonged standing.
*
Imaging Insights
:
*
MRI
: Critical for identifying space-occupying lesions (e.g., ganglion cysts, lipomas, nerve sheath tumors, varicosities) compressing the posterior tibial nerve. Can show nerve edema or thickening.
*
Ultrasound
: Dynamic assessment of nerve, identification of extrinsic compression.
*
Medial Column Stress Fractures (Navicular, Medial Cuneiform)
:
*
Clinical Presentation
: Insidious onset of deep aching pain, often worse with weight-bearing and activity. Tenderness to palpation.
*
Imaging Insights
:
*
X-ray
: Often negative in early stages. May show subtle sclerosis or fracture line weeks after symptom onset.
*
MRI
: Gold standard for early detection, revealing bone marrow edema without definitive fracture line. Critical for distinguishing high-risk (dorsal cortex) navicular fractures from low-risk.
*
CT
: Useful for detailed assessment of fracture lines and extent for surgical planning, especially if non-healing.
LATERAL FOOT PAIN:
-
Peroneal Tendinopathy/Tears
:
- Clinical Presentation : Pain and tenderness posterior to the lateral malleolus or along the course of the peroneal tendons, often worse with activity, inversion, or eversion. Swelling. Can be associated with chronic ankle instability. Subluxation may present with a "snapping" sensation.
-
Imaging Insights
:
- X-ray : May be normal. Could show an os peroneum or signs of chronic ankle instability.
- MRI : Tendon thickening, signal changes (tendinosis), longitudinal splits (especially peroneus brevis near lateral malleolus), or frank ruptures. Tenosynovitis. Assesses integrity of superior/inferior peroneal retinacula. Fracture of os peroneum.
- Ultrasound : Dynamic assessment of tendon excursion, subluxation, tenosynovitis, and tears.
-
Chronic Lateral Ankle Instability (CLAI)
:
- Clinical Presentation : Recurrent ankle sprains, feeling of "giving way" or instability, persistent lateral ankle pain, stiffness, and weakness. History of multiple inversion injuries.
-
Imaging Insights
:
- X-ray (weight-bearing) : Often normal, but may show subtle signs of degenerative changes or osteophytes. Stress radiographs (talar tilt, anterior drawer) can quantify laxity but are often performed clinically.
- MRI : Direct visualization of ATFL and CFL tears, attenuation, or chronic scarring. Exclusion of other pathology like peroneal tears, OCLs, or sinus tarsi syndrome.
-
Sinus Tarsi Syndrome
:
- Clinical Presentation : Chronic lateral ankle pain and tenderness localized to the sinus tarsi, often exacerbated by activity or weight-bearing on uneven surfaces. History of inversion injury.
-
Imaging Insights
:
- MRI : Inflammation, edema, or fibrosis within the fat pad of the sinus tarsi. May show tears of the interosseous talocalcaneal ligament or cervical ligament. Often associated with concomitant lateral ankle ligamentous laxity.
-
Fifth Metatarsal Base Fractures
:
- Clinical Presentation : Acute lateral foot pain, swelling, and tenderness at the base of the fifth metatarsal following trauma (e.g., inversion injury). Location differentiates avulsion (Zone 1), Jones (Zone 2), and diaphyseal stress (Zone 3).
-
Imaging Insights
:
- X-ray : Typically diagnostic, revealing the fracture line. Important to differentiate from a normal apophysis in adolescents.
- CT : For complex fracture patterns or non-union assessment.
-
MRI
: For early detection of stress reactions or occult fractures in Zone 3. | PTTD Stage I/II (flexible deformity) with mild symptoms responsive to orthotics, bracing, physical therapy, NSAIDs, activity modification.
Accessory navicular with minimal symptoms, no significant PTT involvement, responsive to shoe modification/orthotics.
Tarsal Tunnel Syndrome with mild intermittent symptoms, negative imaging for compressive lesions, responsive to activity modification, shoe wear, oral NSAIDs, or corticosteroid injections.
Medial column stress fractures (low-risk type) with stable symptoms, responsive to activity modification and boot immobilization.
Peroneal tendinopathy/mild tenosynovitis without tears or instability, responsive to RICE, NSAIDs, physical therapy, orthotics, boot immobilization, corticosteroid injections.
Mild lateral ankle instability without functional impairment or recurrent sprains, responsive to bracing, physical therapy (proprioception, strengthening), activity modification.
Sinus Tarsi Syndrome responsive to activity modification, NSAIDs, corticosteroid injections, physical therapy.
Acute non-displaced or minimally displaced Zone 1 (avulsion) or Zone 2 (Jones) fifth metatarsal base fractures, or Zone 3 stress fractures, with appropriate non-weight bearing or protected weight-bearing immobilization. | Non-operative management |
| | Non-operative management: Activity modification, NSAIDs, physical therapy (stretching, strengthening), orthotics (medial arch support, hindfoot stability), bracing (AFO, CAM boot), corticosteroid injections (e.g., for plantar fasciitis, tarsal tunnel, peroneal tenosynovitis). |
| | | | |
Clinical & Radiographic Imaging