Introduction to Chronic Unreduced Dislocations
Old, unreduced dislocations of the major joints of the upper extremity—specifically the elbow and the shoulder—are relatively rare in modern orthopedic practice within developed nations, largely due to the advent of advanced imaging and accessible emergency care. However, they remain a significant source of morbidity in developing countries and in cases of polytrauma or delayed presentation.
The management of chronic unreduced dislocations requires a profound understanding of altered pathoanatomy, severe soft tissue contractures, and the biomechanical consequences of prolonged joint incongruity. Operative intervention is fraught with complications, including iatrogenic fractures of osteopenic bone, neurovascular compromise, and recurrent instability. This comprehensive guide details the evidence-based surgical management of both chronic unreduced posterior elbow dislocations and chronic locked posterior shoulder dislocations.
Chronic Unreduced Posterior Elbow Dislocations
Posterior dislocations are the most common variant of elbow dislocations. When left unreduced for weeks or months, the joint undergoes severe fibrotic and osseous changes that render closed reduction impossible and open reduction highly complex.
Pathoanatomy and Biomechanics
In a chronic unreduced posterior elbow dislocation, the arm is typically fixed in extension or slight flexion with a severely restricted arc of motion. The biomechanical alterations are profound:
* Rotational Block: Pronation is characteristically more limited than supination. Because the distal humerus is displaced anteriorly, the biceps brachii tendon is bowstrung and placed under immense tension as it angulates around the humeral condyles. This tension forcefully pulls the radial tuberosity, locking the forearm into supination.
* Myositis Ossificans: Extensive heterotopic ossification frequently develops within the brachialis and triceps brachii muscles due to the initial trauma and subsequent hematoma organization.
* Soft Tissue Contracture: There is marked shortening and fibrosis of the triceps muscle, the anterior capsule, and the medial and lateral collateral ligament (MCL and LCL) complexes.
* Fossa Obliteration: The olecranon and coronoid fossae become completely obliterated by dense, organized fibrous tissue, preventing the seating of the ulnar articular surfaces even if the joint is mobilized.
* The "Radial Humeral Horn": A classic radiographic and intraoperative finding in chronic cases is the "radial humeral horn." This is an osseous prominence resulting from the ossification of a localized hematoma near the periosteum, which adheres to the capsule adjacent to the radial head.
* Neurological Tethering: The ulnar nerve becomes encased in scar tissue and is tightly tethered behind the medial epicondyle. Any attempt at forceful flexion without prior neurolysis places the nerve at high risk for traction neuropraxia or axonotmesis.
Surgical Warning: Closed reduction of an elbow dislocation that is more than 3 weeks old is virtually impossible and strictly contraindicated. The combination of severe soft tissue contracture and profound disuse osteopenia makes closed manipulation exceedingly hazardous, carrying a high risk of iatrogenic distal humerus fractures or devastating sheer injuries to the articular cartilage.
Preoperative Evaluation and Indications
Standard anteroposterior (AP) and lateral radiographs are mandatory, but a fine-cut Computed Tomography (CT) scan with 3D reconstructions is the gold standard for preoperative planning. The CT scan delineates the extent of myositis ossificans, the presence of the radial humeral horn, and the degree of articular cartilage preservation.
Treatment Options:
1. Open Reduction: The treatment of choice for functional restoration, particularly if undertaken within 3 months of the injury. While a completely normal elbow should not be expected, functional arcs of motion can be restored.
2. Pediatric Considerations: In children, open reduction is always warranted regardless of the chronicity of the dislocation (provided it is not a congenital dislocation). Children possess remarkable remodeling potential and frequently regain highly useful ranges of flexion and extension.
3. Salvage Procedures: For extremely neglected cases with severe joint destruction, options include excision arthroplasty, interposition arthroplasty, total elbow arthroplasty (in older, low-demand patients), or arthrodesis.
Surgical Approach: Open Reduction of the Elbow
The surgical reconstruction of a chronic elbow dislocation demands meticulous soft tissue handling and a stepwise approach to joint mobilization.
1. Positioning and Anesthesia:
The patient is placed in the lateral decubitus position with the arm draped over a padded bolster, allowing for 120 degrees of elbow flexion. General anesthesia with complete neuromuscular blockade is essential to eliminate muscle tone. A sterile tourniquet is applied high on the arm.
2. Incision and Ulnar Nerve Management:
A universal posterior midline incision is utilized, curving slightly lateral to the tip of the olecranon.
* Step 1: The ulnar nerve must be identified proximally in the triceps interval and traced distally into the cubital tunnel.
* Step 2: A meticulous neurolysis is performed. Because the nerve is often tightened and tethered by the altered anatomy, an anterior subcutaneous or submuscular transposition is routinely performed to protect it during subsequent joint flexion.
3. Triceps Lengthening and Joint Exposure:
Most authors agree that lengthening of the triceps mechanism is mandatory to achieve reduction without placing excessive compressive forces on the articular cartilage.
* Speed’s V-Y Technique: This is the most widely utilized method. An inverted V-shaped incision is made through the triceps aponeurosis, allowing the muscle to be reflected distally. After joint reduction, the aponeurosis is repaired in a Y-configuration, effectively lengthening the extensor mechanism.
* Alternative Techniques: Vangorder described a transverse tenotomy of the triceps, bridging the resulting gap with fascia lata or Achilles tendon allograft. Conversely, Krishnamoorthy et al. advocated for utilizing dual medial and lateral surgical windows without routinely dividing the triceps, though this limits exposure in severe cases.
4. Joint Debridement and Release:
* The dense fibrous tissue filling the olecranon and coronoid fossae must be radically excised using rongeurs and curettes.
* The "radial humeral horn" and any bridging myositis ossificans are resected.
* The contracted collateral ligaments often require sharp release from their epicondylar origins to mobilize the joint.
5. Reduction and Stabilization:
Once the fossae are cleared and the soft tissues released, gentle traction is applied. The joint is reduced under direct vision.
Clinical Pearl: Never use the forearm as a lever to force reduction. The osteopenic coronoid or distal humerus will fracture. Reduction must be achieved through adequate soft tissue release and direct, gentle translation of the articular surfaces.
The Role of Hinged External Fixation
Following open reduction, the elbow is inherently unstable due to the extensive release of the collateral ligaments and capsule. Historically, ligamentous repair alone yielded a 29% recurrent luxation rate (as noted by Duckworth et al.). Consequently, the modern standard of care involves the application of a hinged external fixator.
- Biomechanical Rationale: A hinged fixator (e.g., Compass hinge or similar dynamic frame) maintains concentric joint reduction while permitting early, protected active and passive range of motion. This enhances muscle-tendon stretching and cartilage nutrition.
- Application: The critical step is identifying the true axis of rotation of the elbow, which passes from the center of the capitellum to the anteroinferior aspect of the medial epicondyle. An axis pin is placed precisely along this line.
- Outcomes: Jupiter and Ring demonstrated stable, mobile joints using open reduction and hinged external fixation at an average of 11 weeks post-injury. They reattached the lateral soft tissues to the lateral epicondyle but relied on the fixator (left in place for 5 to 8 weeks) rather than complex ligamentous reconstructions to maintain stability. Hotchkiss similarly utilized hinged fixators for 8 weeks to maintain reduction and facilitate aggressive rehabilitation.
- Alternative Stabilization: Arafiles described a historical technique of creating an intraarticular "cruciate" ligament using local tissue to stabilize the joint, allowing flexion-extension exercises within 6 days of surgery. However, external fixation remains the contemporary gold standard.
Chronic Unreduced Posterior Shoulder Dislocations
While the elbow text transitions into shoulder pathology, the underlying principles of managing chronic dislocations remain consistent: addressing bone loss, soft tissue contracture, and altered joint kinematics. Chronic locked posterior shoulder dislocations are frequently missed on initial presentation and present months later with significant anterior humeral head defects (reverse Hill-Sachs or McLaughlin lesions).
Preoperative Planning and Defect Assessment
The duration of the dislocation and the size of the humeral head defect dictate the surgical algorithm. CT scanning is mandatory to quantify the percentage of articular surface involvement.
* Defects < 20%: Can often be managed with transfer of the subscapularis tendon or lesser tuberosity into the defect (McLaughlin procedure).
* Defects 20% - 45%: May require structural osteochondral allografting.
* Defects > 45% or Chronicity > 6 Months: Require arthroplasty or complex rotational osteotomies.
Hemiarthroplasty for Posterior Dislocations
For very old dislocations (longer than 6 months) or for massive head defects (larger than 45% to 50%), most authors suggest proceeding directly to arthroplasty. Hemiarthroplasty is indicated if the glenoid cartilage is preserved.
Version Control in Arthroplasty:
The most critical technical aspect of hemiarthroplasty for chronic posterior dislocations is the management of humeral component version. The native humerus typically has approximately 30 degrees of retroversion. However, in a chronic posterior dislocation, the posterior soft tissues are severely stretched, and the anterior tissues are contracted. Replicating native retroversion will lead to immediate posterior subluxation of the prosthesis.
* Dislocations < 6 Months Old: The humeral component should be placed in approximately 20 degrees of retroversion (reducing the normal retroversion by 10 degrees).
* Dislocations > 6 Months Old: The posterior capsular laxity is profound. The humeral component must be placed in neutral version (0 degrees) to provide anterior stability and prevent the head from subluxing posteriorly.
Surgical Warning: Occasionally, significant posterior instability may persist even after arthroplasty with altered version. In these cases, further soft tissue reconstruction is required, such as posterior capsule augmentation using a transplanted biceps tendon, as described by Kumar et al.
Total Shoulder Arthroplasty (TSA)
Total shoulder replacement is recommended if the glenoid articular surface has been destroyed by the chronic articulation of the dislocated humeral head, provided the dislocation is more than 6 months old or the humeral defect exceeds 45%.
Glenoid Reconstruction:
Extensive erosion of the posterior margin of the glenoid fossa is common. Preoperative CT scans are vital to assess this bone loss. If posterior glenoid wear is significant, asymmetric reaming may be insufficient, and a structural bone graft (often harvested from the resected humeral head) must be keyed into the posterior glenoid to restore a neutral version to the glenoid component.
Rotational Osteotomy of the Humerus
In select cases of locked posterior dislocations where joint preservation is desired but the anterior defect is substantial, a rotational osteotomy of the proximal humerus can be performed. This technique, described by Keppler et al., involves a transverse osteotomy of the surgical neck. The humeral shaft is internally rotated, which effectively rotates the anterior defect away from the glenoid rim, preventing it from engaging during internal rotation.
The osteotomy is rigidly fixed using an angled blade plate or a modern locking plate system.
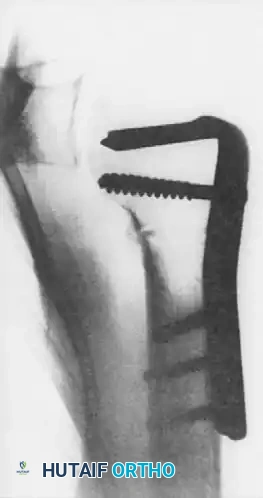
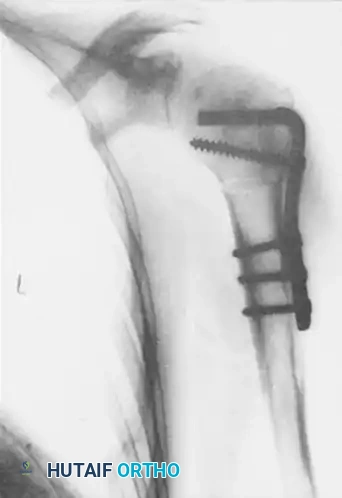
Figures above illustrate the internally fixed humerus after transverse osteotomy and internal rotation of the humeral shaft using an angled plate construct. This effectively alters the articular arc, preventing the reverse Hill-Sachs lesion from engaging the posterior glenoid rim.
Postoperative Rehabilitation Protocols
Whether addressing the elbow or the shoulder, the postoperative rehabilitation following reconstruction of a chronic dislocation is a delicate balance between preventing recurrent stiffness and protecting the surgical repair.
Elbow Rehabilitation (Hinged External Fixator)
- Phase I (0-2 Weeks): The hinged fixator is unlocked immediately or within 3-5 days postoperatively. Continuous Passive Motion (CPM) or active-assisted range of motion (AAROM) is initiated. The fixator protects the collateral ligaments while allowing the triceps to glide.
- Phase II (2-6 Weeks): Active range of motion is encouraged. The V-Y triceps repair is protected by avoiding forceful active extension against resistance.
- Phase III (6-8 Weeks): The external fixator is removed in the clinic. Progressive strengthening and terminal stretching are initiated. Night splinting in extension may be required if a flexion contracture begins to develop.
Shoulder Rehabilitation (Arthroplasty)
- Phase I (0-4 Weeks): The shoulder is immobilized in a neutral rotation sling (often an external rotation brace is used to protect the anterior subscapularis repair and prevent posterior subluxation). Passive forward elevation is allowed, but internal rotation is strictly limited.
- Phase II (4-8 Weeks): Active-assisted motion begins. The focus is on restoring forward elevation and gentle external rotation.
- Phase III (8-12+ Weeks): Strengthening of the rotator cuff and deltoid begins. Full functional recovery may take up to a year, and patients must be counseled that while pain relief is highly predictable, range of motion will likely remain less than that of a native, uninjured shoulder.
