CONGENITAL PSEUDARTHROSIS OF THE CLAVICLE: PATHOGENESIS AND CLINICAL EVALUATION
Congenital pseudarthrosis of the clavicle is a rare, highly specific pediatric orthopedic anomaly characterized by a failure of the clavicle to form a continuous bony structure during embryogenesis. Unlike traumatic nonunions, this condition is present at birth and possesses a distinct natural history, anatomical presentation, and biomechanical profile that demands specialized surgical management.
Embryology and Etiological Theories
The clavicle is the first bone in the human body to begin ossification, initiating during the fifth week of gestation. It is unique in that it develops via membranous ossification from two separate primary ossification centers—one medial and one lateral. These two centers typically fuse by the seventh week of gestation, forming a precartilaginous bridge that subsequently ossifies.
Congenital pseudarthrosis is fundamentally a failure of this precartilaginous bridge to ossify. Several theories have been proposed to explain this localized developmental arrest:
* The Vascular Pulsation Theory (Lloyd-Roberts): The most widely accepted biomechanical theory suggests that the lesion is caused by direct, repetitive pressure from the subclavian artery on the immature clavicle.
* Anatomical Asymmetry: The right subclavian artery normally arches higher than the left, placing it in closer proximity to the developing right clavicle. This anatomical relationship perfectly correlates with the clinical observation that congenital pseudarthrosis of the clavicle occurs almost invariably on the right side.
* The Dextrocardia Phenomenon: In a landmark series of 60 unilateral lesions, 59 were located on the right side. In the single patient presenting with a left-sided pseudarthrosis, dextrocardia was discovered. This finding strongly corroborates the subclavian artery pulsation theory, as dextrocardia reverses the vascular anatomy, placing the higher-arching subclavian artery on the left.
* Bilateral Involvement: Bilateral pseudarthrosis occurs in approximately 10% of patients and is often associated with more systemic developmental anomalies or cervical rib presence.
Clinical Presentation
The condition is present at birth and is typically noticed by parents or pediatricians as a painless, subcutaneous prominence over the middle third of the clavicle.
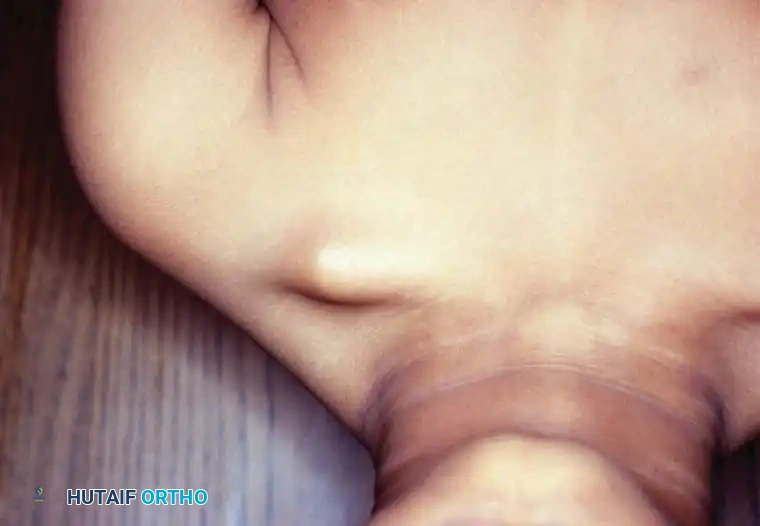
Fig. 28-10 Congenital pseudarthrosis of clavicle. A, Subcutaneous prominence in the middle third of the right clavicle in a 4-year-old child.

Fig. 28-10 Congenital pseudarthrosis of clavicle. B, Lateral view demonstrating the superior displacement of the medial fragment.
The medial fragment is typically displaced superiorly due to the unopposed pull of the sternocleidomastoid muscle, while the lateral fragment is pulled inferiorly by the weight of the upper extremity and the action of the pectoralis major and deltoid muscles. The overlying skin is normal, and there is no history of birth trauma. The shoulder girdle may exhibit hypermobility, allowing the child to bring the shoulders together anteriorly, though not to the extreme extent seen in cleidocranial dysplasia.
Differential Diagnosis and Associated Pediatric Deformities
The differential diagnosis for a mid-clavicular mass in an infant or young child includes:
1. Obstetric Clavicle Fracture: Usually associated with a difficult delivery, presents with pain, crepitus, and a lack of pseudarthrosis on early radiographs. It heals rapidly with abundant callus formation.
2. Cleidocranial Dysostosis (Dysplasia): A systemic condition characterized by bilateral clavicular hypoplasia or aplasia, delayed closure of cranial sutures, and dental anomalies.
3. Neurofibromatosis: Can present with pseudarthrosis, though more commonly in the tibia or forearm.
4. Congenital Muscular Torticollis: While a distinct pathology involving the sternocleidomastoid muscle, severe torticollis can present with profound neck and shoulder asymmetry, mimicking or complicating the clinical picture of clavicular anomalies.

Fig. 28-9 Bipolar release for congenital torticollis. A, Severe congenital torticollis (right) in an 8-year-old girl, demonstrating profound cervical asymmetry.

Fig. 28-9 Bipolar release for congenital torticollis. B, Postoperative appearance after bipolar release, restoring normal cervical alignment.
Clinical Pearl: Always evaluate the cervical spine and sternocleidomastoid in patients presenting with shoulder asymmetry. A missed congenital torticollis can lead to permanent facial hemihypoplasia and secondary cervical scoliosis.
INDICATIONS FOR SURGICAL INTERVENTION
Spontaneous union of a congenital pseudarthrosis of the clavicle is unknown in the orthopedic literature. Consequently, any desired union requires operative intervention.
Historically, surgery was indicated primarily for cosmetic reasons (unacceptable appearance of the prominent bone ends) or for mild hypermobility. However, modern indications have expanded to include functional preservation and the prevention of late-onset neurovascular complications.
Thoracic Outlet Syndrome (TOS)
Sales de Gauzy et al. described thoracic outlet syndrome in adolescent patients with untreated congenital pseudarthrosis of the clavicle. During hyperabduction of the arm, the medial end of the lateral clavicular fragment acts as a fulcrum, compressing the subclavian artery and brachial plexus against the first rib.
* Surgical Rationale: Although the condition is largely asymptomatic in early childhood, surgical treatment is highly recommended to restore normal clavicular morphology, stabilize the shoulder girdle, and prevent debilitating functional or vascular problems in adolescence and adulthood.
Timing of Surgery
The consensus among pediatric orthopedic surgeons is that the ideal time for surgical intervention is between ages 3 and 5 years.
* Early Intervention (< 3 years): Grogan et al. reported successful treatment in children younger than 3 years using a simplified technique: resection of the fibrous pseudarthrosis and sclerotic bone ends, careful dissection and preservation of the periosteal sleeve, and direct approximation of the bone ends without bone grafting or internal fixation. All patients achieved bridging ossification by 6 to 8 weeks. Lorente Molto et al. also recommended early surgery (18 months to 4 years) using excision, bone grafting, and simple intramedullary Kirschner wire (K-wire) fixation.
* Standard Intervention (> 4 years): As the child ages, the deforming forces increase, and the pseudarthrosis becomes more rigid. In older children and adolescents, simple resection or K-wire fixation is insufficient. Open reduction, rigid internal fixation with a plate and screws, and autogenous iliac crest bone grafting are mandatory to achieve union.
Surgical Warning: Simple resection of the prominent bone ends without achieving union is strictly contraindicated. It invariably results in persistent pain, recurrent prominence during shoulder movement, and permanent asymmetry of the shoulder girdle.
PREOPERATIVE PLANNING AND BIOMECHANICS
Successful reconstruction requires overcoming the inherent biomechanical forces acting on the clavicle. The sternocleidomastoid pulls the medial fragment posterosuperiorly, while the weight of the arm and the pectoralis major pull the lateral fragment anteroinferiorly.
Preoperative imaging should include standard anteroposterior (AP) and 20-degree cephalad tilt radiographs of both clavicles for comparison. In older adolescents with suspected TOS, dynamic Doppler ultrasound or MR angiography with the arm in hyperabduction may be indicated to assess subclavian vessel compression.
SURGICAL TECHNIQUE: OPEN REDUCTION AND ILIAC BONE GRAFTING
The following technique describes the gold-standard approach for children aged 4 years and older, utilizing rigid plate fixation and autogenous iliac crest bone grafting.
1. Patient Positioning and Setup
- Place the patient in the beach-chair position with the head secured in a neutral position.
- Place a small bump between the scapulae to allow the shoulders to fall posteriorly, aiding in the reduction of the clavicle.
- The entire forequarter, including the neck, chest, shoulder, and arm, must be prepped and draped free to allow intraoperative manipulation of the upper extremity.
- Simultaneously prep and drape the ipsilateral anterior iliac crest for bone graft harvesting.
2. Incision and Superficial Dissection
- Make a transverse 3-inch (7.5-cm) incision centered over the body of the clavicle.
- Crucial Step: Place the incision approximately one fingerbreadth above the superior border of the bone (in Langer’s lines). This prevents the final surgical scar from resting directly over the prominent hardware, reducing postoperative irritation and improving cosmesis.
- Carry sharp dissection through the subcutaneous tissue and the platysma muscle.
- Identify and carefully retract the supraclavicular nerves. Transection of these nerves leads to a bothersome patch of numbness over the anterior chest and carries a high risk of painful neuroma formation.
3. Deep Exposure and Pseudarthrosis Takedown
- Expose the clavicle medially and laterally in the central third, directly over the area of the pseudarthrosis.
- Incise the thick periosteum longitudinally along the superior aspect of the clavicle.
- Subperiosteal Dissection: Expose the bone subperiosteally using a Cobb elevator.
- Surgical Pitfall: Extreme caution must be exercised along the inferior and posterior borders of the clavicle. The subclavian vein and artery, as well as the brachial plexus, lie directly posterior to the subclavius muscle. Maintain the dissection strictly within the subperiosteal envelope to protect these critical neurovascular structures.
- Excise the dense, fibrous pseudarthrosis tissue.
4. Preparation of the Bone Ends
- The bone ends are typically bulbous, capped with cartilage, and highly sclerotic.
- Use a rongeur or an oscillating microsaw to resect the sclerotic bone ends until healthy, bleeding cortical bone is encountered (the "paprika sign").
- Use a small drill bit (e.g., 2.0 mm) to open the medullary canals of both the medial and lateral fragments. This establishes marrow continuity and allows for the migration of osteoprogenitor cells into the graft site.
5. Bone Grafting
- Harvest an autogenous corticocancellous bone block and supplementary cancellous chips from the anterior iliac crest.
- If a significant gap exists after resecting the sclerotic ends, shape the corticocancellous block to fit precisely into the defect as an interpositional strut.
- If the bone ends can be approximated without undue tension, pack the cancellous chips circumferentially around the decorticated junction.
6. Internal Fixation
- Reduce the clavicle by manipulating the arm and elevating the lateral fragment while depressing the medial fragment.
- Apply a pre-contoured pediatric clavicle plate or a 3.5-mm reconstruction plate along the superior or anterosuperior surface of the clavicle.
- Secure the plate with a minimum of three bicortical screws in both the medial and lateral fragments. In osteopenic bone or older children, locking screws may be utilized to enhance construct rigidity.
- Note on K-wires: While intramedullary K-wires have been described for very young children, they carry a well-documented risk of catastrophic intrathoracic migration and provide inferior rotational stability compared to plate fixation. If used, the lateral end must be bent and securely buried beneath the skin, with close radiographic follow-up.
7. Closure
- Meticulously close the thick periosteal sleeve over the bone graft and plate. This periosteal envelope is highly osteogenic in children and is critical for rapid union.
- Repair the platysma muscle as a distinct layer to prevent scar widening.
- Close the subcutaneous tissue with inverted absorbable sutures and the skin with a running subcuticular stitch or tissue adhesive.
POSTOPERATIVE PROTOCOL AND REHABILITATION
- Immobilization: Place the patient in a pediatric shoulder immobilizer or a well-padded sling for 4 to 6 weeks.
- Early Phase (0-4 weeks): Allow gentle, passive pendulum exercises of the shoulder and active range of motion of the elbow, wrist, and hand to prevent stiffness. Active elevation and abduction of the shoulder are strictly prohibited to prevent hardware failure or graft displacement.
- Intermediate Phase (4-8 weeks): Obtain follow-up radiographs at 4 and 8 weeks. Once bridging callus is visible, transition to active-assisted and active range of motion exercises.
- Return to Activity: Full unrestricted activity, including contact sports, is withheld until there is radiographic evidence of complete bony consolidation and remodeling, which typically occurs between 4 and 6 months postoperatively.
COMPLICATIONS AND MANAGEMENT
While union rates approach 100% with rigid plating and autogenous grafting, surgeons must be prepared to manage potential complications:
1. Hardware Prominence: The most common postoperative complaint. Due to the subcutaneous nature of the clavicle, plates often become palpable and irritating once the swelling subsides. Hardware removal is routinely offered 9 to 12 months postoperatively, after complete remodeling is confirmed.
2. Nonunion: Exceedingly rare with modern plating techniques but can occur if the sclerotic bone ends are inadequately resected or if fixation is tenuous. Management requires revision ORIF with structural bone grafting.
3. Neurovascular Injury: Injury to the subclavian vessels is a catastrophic complication. It is entirely preventable by maintaining a strict subperiosteal dissection plane and utilizing blunt retractors (e.g., malleable retractors) placed carefully behind the clavicle during drilling and screw insertion.
4. Infection: Superficial surgical site infections are managed with oral antibiotics. Deep infections require prompt surgical debridement, hardware retention (if stable) until union occurs, and culture-directed intravenous antibiotics.
