COMPLICATIONS OF FRACTURES
Complications which may occur in a patient who has suffered a fracture or dislocation may be grouped in the following way:
1 COMPLICATIONS OF MAJOR TRAUMA
These include:
1 Internal and external haemorrhage, oligaemic shock, etc.
2 Infection (in open or compound injuries)
3 Metabolic responses of trauma including electrolyte shifts and protein breakdown
4
Acute respiratory distress syndrome (ARDS)/fat embolism syndrome (FES).
Major tissue trauma activates cell defence mechanisms which combat infection, remove damaged tissue and facilitate tissue repair. These processes may be affected by systemic mediators which might cause an imbalance. This may be towards a generalised pro-inflammatory state (systemic inflammatory response syndrome or SIRS) accompanied by cell damage with increased cell wall permeability, or to suppression of inflammation (compensatory anti-inflammatory response syndrome or CARS) which may lead to a susceptibility to infection. Such imbalances are said to be the result either of particularly severe trauma or a particular individual response.
3
The
acute respiratory distress syndrome
(ARDS) is regarded as being a local manifestation of SIRS, and in those who survive, the cause of multiple organ dysfunction (MODS). This may include cardiac, gastrointestinal, renal, hepatic, haematological and cerebral failure.
Hypoxia and acute respiratory insufficiency are common after trauma, and the causes include upper airway obstruction, chest injury (e.g. due to pneumothorax) and circulatory failure. Most respond to treatment of the underlying cause and the administration of oxygen, but if this fails other reasons, ARDS or the
fat embolism syndrome
(FES) must be suspected.
After most fractures some fat is released into the circulation and causes no problem. In FES however, the situation is different, and this may be related to the quantity of fat involved. The presence of fat in the pulmonary circulation may result in respiratory problems similar to those found in ARDS. Fat particles may, however, also enter the systemic circulation through pulmonary capillaries and shunts, or through a patent foramen ovale, producing very distinctive features which merit the title ‘fat embolus’. This is seen most often after fractures of the femoral shaft and pelvis.
In both ARDS and FES there is no evidence of cardiac failure; chest radiographs show bilateral ‘snowstorm’ lungs, and there is disturbance of the PaO
2
/FiO
2
ratio (the arterial oxygen concentration divided by the fractional inspired oxygen concentration). Where there has been a fat embolism the most distinctive features (which may appear 2 or 3 days after the injury) are:
• an increased frequency of respiration of more than 35, sustained after sedation dyspnoea; the use of the accessory muscles of respiration; a PaO
2
of less than 60 mmHg; a PaCO2 of more than 55 mmHg, or a pH of less than 7.3
• petechial haemorrhages in the skin of the axilla, anterior chest wall and conjunctiva
• neurological disturbances with the patient becoming confused, aggressive or comatose, and there may be focal neurological signs (e.g. epileptiform seizures)
• evidence of renal, cardiac, hepatic and gastrointestinal involvement.
Prevention:
The risks of these complications are reduced when (1) fluid replacement during and after surgery is impeccable; (2) when in cases of multiple injury, and assuming the principles of damage control orthopaedics are closely followed, any femoral fracture is rigidly fixed: in practice this generally implies intramedullary nailing, but an external fixator may be used; (3) all efforts must be made to reduce the occurrence of infection in any open injury.
Treatment:
(1) Aggressively carry out all routine resuscitative measures such as the administration of humidified oxygen and intravenous fluids. If indicated by the blood gas levels, proceed to endotracheal intubation and the use of a ventilator, with transfer to an intensive therapy unit. In rare cases a cardiopulmonary by-pass pump may be required. Where possible, active physiotherapy is advised. (2) If there is progressive deterioration in blood gas levels, surgical stabilisation of any femoral fracture is advocated. After such a procedure the patient should be left on a ventilator for not less than 24 hours; this may be discontinued when the blood gases improve, and there is an improvement in the tidal volume and the patient’s level of consciousness. (3) The administration of methylprednisolone in cases where the PaO 2 is less than 60 mm Hg, whether discovered before the onset of frank symptoms or later, has been shown to have a beneficial effect. (A dose of 30 mg per kg body weight on admission and repeated after 4 hours has been recommended.)
2 COMPLICATIONS OF PROLONGED RECUMBENCY
These include:
1 Hypostatic pneumonia
2 Pressure sores
3
Deep venous thrombosis and pulmonary embolism.
This complication may be serious or even fatal, and a careful risk assessment of the patient and his circumstances must be made in every case of major trauma or when the possibility of prolonged immobilisation arises. The measures which may be pursued in treatment or prevention must take account of the possibility of bleeding into the wound, or where a spinal or epidural anaesthetic has been used, the risks of a spinal haematoma developing.
Factors in risk assessment include:
• a previous history of deep vein thrombosis
• a family history of deep vein thrombosis
• the presence of malignancy
• the nature and site of the trauma (e.g. patients with pelvic and lower limb injuries being at particular risk)
• the need for prolonged immobilisation and recumbency.
Where the risks are judged to be more than trivial, the following may be considered:
Mechanical measures, such as:
• anti-embolus stockings
• lower limb supports incorporating automatic cyclical limb compression and relaxation
• powered mechanical devices producing cyclical limb motion
• prophylactic insertion of intravenous cava filters, indicated in patients with pelvic and/or multiple injuries.
Chemical prophylaxis:
Where the risks are considered to be high, chemical prophylaxis should be considered. It would seem advantageous to continue this for 4–5 weeks, even although the patient has been allowed home in the interim. Careful consideration must be given as to when the medication should be commenced: the earlier it is started, the more effective it is – but too early, and haemorrhage may ensue. A number of agents, of varying efficacy, are in current use. These include:
•
Aspirin:
this is of little efficacy in the trauma situation, and its side effects render it of little value
•
warfarin
: although its familiarity and comparative safety renders it attractive the regular monitoring required is time-consuming and expensive, and if started too early will lead to undesirable haemorrhage
•
low molecular weight heparin:
this is highly effective and comparatively safe, but has to be given by daily injection which may cause logistic difficulties when the patient is discharged. It should not be started until at least 6 hours after surgery or stabilisation after trauma, and not until at least 12 hours after removal of a spinal or epidural catheter
•
Pentasaccharide
(e.g.
Fondaparinux
) is given daily subcutaneously. It is also very effective and relatively safe, but has been noted to be associated with minor bleeding. It also should not be started until at least 6 hours after surgery or stabilisation after trauma, and not until at least 12 hours, and preferably longer after removal of a spinal or epidural catheter
•
Melagatran:
this comparatively new oral preparation, given as a fixed, twice-daily dose, is under evaluation, but appears to be more effective than Warfarin; it gives promise, as no monitoring is required and it would seem to be highly effective.
4 Muscle wasting and stiffening of joints, making subsequent mobilisation more difficult and prolonged
5 Skeletal decalcification and the formation of urinary tract calculi
6 Urinary tract infections
7 Neurological complications such as (i) common peroneal nerve palsy: this sometimes results from a less than ideal posture of the leg when external rotation leads to pressure in the region of the fibular neck; or it sometimes occurs from pressure against a splint; (ii) or ulnar neuropathy, from the patient repeatedly trying to change his position using downwards pressure of the elbows against the bed when use of a so-called monkey pole would avoid this
8 Cardiovascular complications, such as cardiac failure due to weakening of the cardiac muscle and poor venous return
9 Psychiatric complications such as depression.
Avoiding these complications as well as the costs of protracted in-patient treatment are the main reasons for the continuing trend towards the operative management of many fractures. In the case of multiple injuries, internal fixation is of considerable help to the nursing staff in their care of the patient.
3 COMPLICATION OF ANAESTHESIA AND SURGERY
These include:
1 Atelectasis and pneumonia
2 Blood loss leading to anaemia or shock with their secondary effects
3 Iatrogenic nerve palsies
4 Wound infection, mechanical failure of internal fixation devices, etc.
4 COMPLICATIONS PECULIAR TO FRACTURES
These include:
1 Disorders involving the rate and quality of union
2 Joint stiffness
3 Sudeck’s atrophy (complex regional pain syndrome)
4 Avascular necrosis
5 Myositis ossificans
6 Bone infections
7 Neurological, vascular and visceral complications
8 Implant complications.
This last group will be considered in more detail.
Slow Union
In slow union, the fracture takes longer than usual to unite, but passes through the stages of healing without any departure from normal, clinically or radiologically.
Delayed union
In delayed union, union fails to occur within the expected time. As distinct from slow union, radiographs of the part may show abnormal bone changes. Typically there is absorption of bone at the level of the fracture, with the production of a gap between the bone ends. External bridging callus may be restricted to a localised area and be of poor quality. There is, however, no sclerosis of the bone ends.
Non-Union
In non-union, the fracture has failed to unite, and there are radiological changes which indicate that this situation will be permanent, i.e. the fracture will never unite, unless there is some fundamental alteration in the line of treatment. Two types of non-union are recognised:
(a)
In hypertrophic non-union
the bone ends appear sclerotic, and are flared out so that the diameter of the bone fragments at the level of the fracture is increased (‘elephant’s foot’ appearance). The fracture line is clearly visible, the gap being filled with cartilage and fibrous tissue cells. The increase in bone density is somewhat misleading, and conceals the fact that the blood supply is good.
(b)
In atrophic non-union
there is no evidence of cellular activity at the level of the fracture. The bone ends are narrow, rounded and osteoporotic; they are frequently avascular. Non-union occurring in the presence of infection
(infective non-union)
is normally of this type. It has been shown that the rates of non-union are higher in smokers.
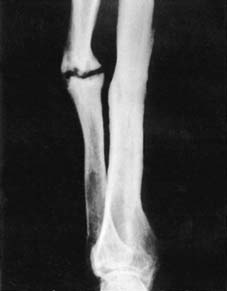
3
Hypertrophic non-union of the ulna.
<h3 class="head3" style
