Introduction & Epidemiology
Supracondylar humeral fractures (SCHFs) represent the most common elbow fracture in the pediatric population, accounting for approximately 60-80% of all elbow fractures in children. The peak incidence occurs between 5 and 7 years of age, with a slight male predominance. The vast majority (95-98%) are extension-type injuries, resulting from a fall onto an outstretched hand with the elbow in hyperextension, leading to posterior displacement of the distal fragment relative to the proximal humerus. Less commonly, flexion-type injuries occur from a direct blow to the posterior aspect of the elbow with the elbow in flexion.
The Gartland classification system is widely used to categorize these fractures based on radiographic displacement:
*
Type I:
Nondisplaced or minimally displaced.
*
Type II:
Displaced with an intact posterior cortex or a plastic deformation of the posterior cortex, maintaining some periosteal hinge.
*
Type III:
Completely displaced with no cortical contact, lacking a stable posterior periosteal hinge. These are further subclassified as Type IIIA (posteromedial displacement) or Type IIIB (posterolateral displacement), which has implications for nerve injury risk and reduction technique.
*
Type IV (recently added by Wilkins):
Multidirectionally unstable in flexion and extension.
While Gartland Type I fractures are typically managed non-operatively, Type II fractures often require closed reduction and casting, or closed reduction and percutaneous pinning (CRPP) if unstable after reduction. Gartland Type III and IV fractures, due to their significant displacement and instability, almost universally necessitate operative management via closed reduction and percutaneous pinning to restore anatomical alignment, prevent neurovascular compromise, and optimize long-term functional outcomes, avoiding complications such as cubitus varus deformity. The precision of reduction and stabilization is paramount to minimize subsequent morbidity.
Surgical Anatomy & Biomechanics
Understanding the complex anatomy and biomechanics of the distal humerus is critical for effective management of supracondylar fractures.
Surgical Anatomy
The distal humerus forms a triangular structure consisting of the medial and lateral columns.
*
Medial Column:
Composed of the medial supracondylar ridge, medial epicondyle, and trochlea. It articulates with the ulna.
*
Lateral Column:
Composed of the lateral supracondylar ridge, lateral epicondyle, and capitellum. It articulates with the radial head.
*
Supracondylar Region:
The narrowest part of the humerus, located just proximal to the flare of the condyles, making it a common site for fracture. The proximal fragment typically displaces anteriorly, while the distal fragment displaces posteriorly, superiorly, and often medially or laterally with varying degrees of rotation.
*
Fossae:
The coronoid fossa anteriorly and the olecranon fossa posteriorly accommodate the coronoid process and olecranon, respectively, during elbow flexion and extension. These fossae provide inherent stability to the elbow joint.
Neurovascular Structures:
The close proximity of vital neurovascular structures to the distal humerus makes these fractures particularly challenging.
*
Brachial Artery:
Lies anterior to the distal humerus, passing through the cubital fossa. It is highly susceptible to injury or entrapment, particularly with anterior displacement of the proximal fragment or significant hemorrhage.
*
Median Nerve:
Travels alongside the brachial artery. It can be injured by direct trauma, stretch, or entrapment within the fracture site, especially with posteromedial displacement of the distal fragment. Entrapment in the brachialis muscle or within the fracture fragments is a significant concern.
*
Radial Nerve:
Located laterally, it is less commonly injured in extension-type SCHFs but can be affected by direct trauma or iatrogenic injury during lateral pin placement if not careful. The posterior interosseous nerve (PIN) is its motor branch, vulnerable distally.
*
Ulnar Nerve:
Located posterior to the medial epicondyle, it is at significant risk of iatrogenic injury during medial pin placement or with severe medial displacement of the distal fragment. Awareness of its anatomical course, especially during elbow flexion, is paramount.
Musculature:
*
Brachialis Muscle:
Originates from the anterior surface of the humerus and inserts onto the coronoid process and ulnar tuberosity. Its deep fibers can become interposed between fracture fragments, particularly in severely displaced fractures, making closed reduction difficult ("milking maneuver" addresses this).
*
Triceps:
Inserts on the olecranon, contributing to the proximal displacement of the distal fragment in extension-type fractures.
*
Forearm Flexors/Extensors:
Originate from the medial and lateral epicondyles respectively, and their contracture can contribute to displacement and difficulty in reduction.
Biomechanics of Injury
The typical mechanism for an extension-type supracondylar fracture is a fall onto an outstretched hand with the elbow in hyperextension.
*
Hyperextension Force:
The olecranon impinges in the olecranon fossa, acting as a fulcrum, transmitting the axial load proximally.
*
Shear Force:
The continued force creates a shear stress across the supracondylar region, which is the weakest point.
*
Displacement:
The distal fragment typically displaces posteromedially or posterolaterally, with varying degrees of rotation and overriding. Muscle forces, particularly the triceps pulling on the olecranon, contribute to the proximal migration of the distal fragment, further complicating reduction.
*
Soft Tissue Injury:
The periosteum is often torn, particularly anteriorly. The anterior displacement of the proximal fragment can tether the brachial artery and median nerve against the sharp edge of the proximal fragment, leading to neurovascular compromise.
Indications & Contraindications
The decision for operative versus non-operative management of supracondylar humeral fractures is guided by the Gartland classification, stability, and the presence of neurovascular compromise.
Indications for Closed Reduction and Percutaneous Pinning (CRPP)
CRPP is the preferred treatment for displaced and unstable supracondylar humeral fractures in children.
*
Gartland Type II Fractures:
* Significant displacement that cannot be adequately reduced and held in a cast.
* Fractures that are unstable after attempted closed reduction and prone to redisplacement within a cast.
* Fractures with a compromised anterior periosteal hinge.
*
Gartland Type III Fractures:
* Complete displacement, loss of cortical contact, and absence of a stable posterior periosteal hinge. This is the primary indication for CRPP. Both Type IIIA (posteromedial displacement) and Type IIIB (posterolateral displacement) require CRPP.
* These fractures are inherently unstable and require internal fixation to maintain reduction.
*
Gartland Type IV Fractures:
* Multidirectionally unstable fractures in both flexion and extension, necessitating stable internal fixation.
*
Vascular Compromise (Pulseless but perfusing hand):
* Even if the hand is perfused, a pulseless extremity mandates urgent closed reduction. If reduction restores the pulse, observation may be considered, but pinning is crucial to maintain reduction and prevent recurrence of vascular compromise.
*
Associated Nerve Injury (neurapraxia):
* While many nerve injuries resolve with reduction, pinning ensures stability and prevents further irritation. Persistent or worsening deficits may warrant open exploration.
*
Swelling:
* In cases of significant swelling that precludes safe casting or increases the risk of compartment syndrome, CRPP allows for stable fixation in a reduced position without the compressive effects of a tight cast, potentially followed by a loose splint.
Contraindications for Closed Reduction and Percutaneous Pinning (CRPP)
Certain situations may necessitate an alternative approach, such as open reduction, or delay surgical intervention.
*
Absolute Contraindications (for closed reduction):
*
Open Fractures:
Require immediate surgical debridement and often necessitate an open approach for thorough wound management and reduction.
*
Irreducible Closed Fractures:
If repeated attempts at closed reduction under fluoroscopy fail to achieve acceptable alignment, soft tissue interposition (e.g., brachialis muscle, median nerve, brachial artery) or severe comminution may necessitate an open reduction.
*
Definite Vascular Injury Requiring Repair (Pulseless, non-perfused hand):
This is an emergency requiring immediate surgical exploration and repair of the brachial artery, which will be performed via an open approach.
*
Relative Contraindications:
*
Severe Local Edema/Blistering:
While CRPP can still be performed, aggressive manipulation in an already compromised soft tissue envelope must be cautious. Staging (external fixation initially, followed by delayed CRPP) or careful, minimal manipulation may be considered.
*
Pre-existing Skin Infection:
May require delay or antibiotic treatment prior to pinning.
*
Older, larger children or very obese children:
The increased soft tissue and bone density may make closed reduction and percutaneous pinning more challenging, sometimes leading to consideration of a mini-open approach.
The following table summarizes the indications for operative vs. non-operative management:
| Indication Category | Operative Management (CRPP) | Non-Operative Management (Casting) |
|---|---|---|
| Gartland Classification | Type II (unstable/displaced post-reduction), Type III, Type IV | Type I, Type II (stable after reduction and casting) |
| Fracture Stability | Unstable, prone to redisplacement | Stable, maintains reduction in cast |
| Neurovascular Status | Pulseless but perfused hand (urgent reduction), Associated nerve injury | Intact neurovascular status |
| Soft Tissue Issues | Significant swelling precluding safe casting, irreducible fractures (if open reduction considered) | Minimal swelling, no skin compromise |
| Associated Injuries | Open fractures (require debridement, often open reduction) | Isolated supracondylar fracture without other significant injuries |
| Reduction Attempts | Failed attempts at acceptable closed reduction | Successful closed reduction and stable immobilization |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are crucial for successful closed reduction and percutaneous pinning (CRPP) of supracondylar humeral fractures.
Pre-Operative Planning
-
Clinical Assessment:
- Neurovascular Status: Thorough assessment of radial, ulnar, and median nerve function (motor and sensory). Palpation of radial and ulnar pulses, capillary refill, and assessment of hand perfusion (color, temperature). Document any pre-existing deficits meticulously.
- Skin Integrity: Check for open wounds, abrasions, or developing blisters.
- Swelling: Evaluate the extent of edema. Severe swelling may influence timing or necessitate a more gentle approach.
-
Radiographic Assessment:
- Standard Views: Obtain true anteroposterior (AP) and lateral radiographs of the elbow. These are essential for assessing fracture morphology, displacement, angulation, and rotation.
-
Key Radiographic Lines:
- Anterior Humeral Line (AHL): A line drawn along the anterior cortex of the humerus, which should pass through the middle third of the capitellum on a true lateral view. Deviations indicate flexion/extension malunion.
- Capitellar-Trochlear Axis: Assess for rotational deformity.
- Baumann's Angle (Humeral Capitellar Angle): Formed by a line drawn along the lateral humeral shaft and a line drawn along the lateral condylar physis. Normal range is 70-75 degrees (or 9-15 degrees relative to perpendicular to the humeral shaft). Comparison to the contralateral side is often helpful. An increased angle suggests varus malalignment, while a decreased angle suggests valgus.
- Assess Displacement: Quantify superior/inferior displacement, medial/lateral translation, varus/valgus angulation, and rotational deformity. Identify any comminution.
-
Equipment Preparation:
- Fluoroscopy Unit (C-arm): Essential for intraoperative visualization and confirmation of reduction and pin placement. Ensure it is functioning correctly and positioned for easy maneuverability to obtain true AP and lateral views.
- K-wires: Assorted sizes (typically 1.6mm (0.062 inch) and 2.0mm (0.078 inch)) for fixation. Have extra on hand.
- Pin Driver: Oscillating or rotary, suitable for K-wires.
- Reduction Instruments: Non-toothed clamps (e.g., small Lane, mini-Hohmann), bone hooks, periosteal elevators, smooth-tipped bone holding forceps (e.g., Verbrugge) for precise manipulation if needed.
- Sterile Drapes, Gowns, Gloves: Standard sterile surgical setup.
- Tourniquet: Pneumatic tourniquet for upper arm, ensuring a bloodless field to aid visualization and prevent nerve irritation from pins.
- Splinting Materials: Plaster or fiberglass splint materials for post-operative immobilization.
- Ulnar Nerve Protector/Retractor (optional): For medial pin placement if a mini-open approach is used.
- Power Drill and Drill Bits (for open reduction, if anticipated): Although this is a closed reduction guide, have this ready in case conversion to open reduction is necessary.
- Informed Consent: Thorough discussion with parents/guardians regarding the procedure, expected outcomes, potential complications (nerve injury, vascular injury, malunion, stiffness, infection, need for revision surgery/open reduction), and post-operative care.
Patient Positioning
- Operating Table: The patient is placed supine on a radiolucent operating table.
-
Arm Positioning:
- The affected arm is typically supported on a sterile hand table or an arm board that allows full range of motion of the elbow and unimpeded fluoroscopic imaging.
- The shoulder is abducted and externally rotated, allowing the elbow to be flexed and extended freely.
- C-arm Access: Ensure the C-arm can be brought in perpendicularly to the arm to obtain true AP and lateral views without repositioning the patient. The C-arm monitor should be clearly visible to the surgeon.
- Tourniquet: A pneumatic tourniquet is applied high on the upper arm, proximal to the fracture site, after padding the skin. The arm is exsanguinated, and the tourniquet is inflated to the appropriate pressure (e.g., 250 mmHg for a child) to create a bloodless field.
- Sterile Preparation and Draping: The entire arm, from the shoulder to the fingertips, is prepped with an antiseptic solution and sterilely draped. Care is taken to ensure the axilla and shoulder joint are adequately prepped for full manipulation during reduction. The tourniquet cuff is typically excluded from the sterile field using a stockinette or separate drape.
Detailed Surgical Approach / Technique
The goal of closed reduction and percutaneous pinning (CRPP) is to achieve anatomical reduction of the fracture and stabilize it with K-wires, while minimizing iatrogenic injury to neurovascular structures. This is a highly systematic approach, heavily reliant on fluoroscopic guidance.
Reduction Maneuvers
The reduction of extension-type supracondylar humeral fractures (the majority) typically involves a sequence of maneuvers to restore length, correct rotational deformity, realign the medial and lateral columns, and then flex the elbow to engage the fragments.
-
Initial Traction and Disengagement:
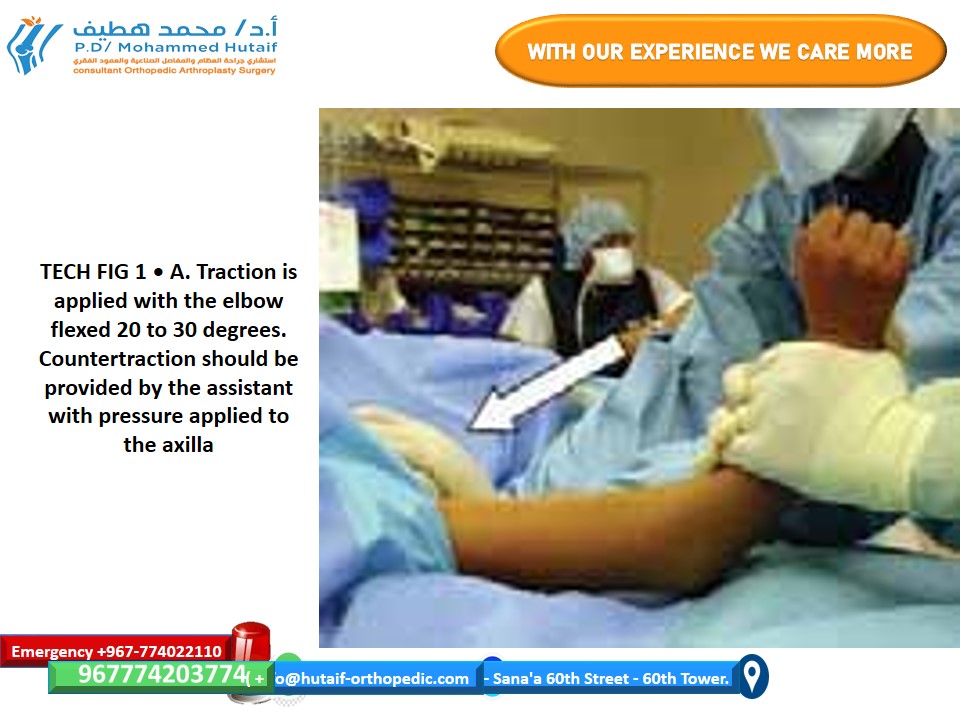
- With the patient supine and arm prepped, the surgeon applies gentle, continuous longitudinal traction to the forearm.
- The elbow is maintained in 20 to 30 degrees of flexion during this initial traction. This slight flexion is critical to prevent tethering and impingement of the neurovascular structures (brachial artery and median nerve) over the sharp, anteriorly displaced proximal fragment. Traction disengages the overriding fracture fragments.
-

- Simultaneously, an assistant or second surgeon provides counter-traction at the shoulder/upper arm. The goal is to restore the anatomical length of the humerus.
-
Milking Maneuver (for entrapped fragments):
- For severely displaced fractures, particularly those with significant anterior displacement of the proximal fragment or soft tissue swelling, the brachialis muscle can become entrapped between the fracture fragments, hindering reduction. In such cases, the "milking maneuver" is performed.
- While maintaining traction, the surgeon uses both hands to manipulate the soft tissue overlying the fracture in a proximal-to-distal direction . This technique aims to dislodge the entrapped brachialis muscle and other soft tissues from the fracture site, facilitating fragment translation.
-

-
Correction of Translation, Angulation, and Rotation:
- Once length is restored (verified by fluoroscopy), the focus shifts to correcting remaining deformities.
- Medial/Lateral Translation: The distal fragment is translated to align with the proximal fragment under AP fluoroscopic guidance.
- Varus/Valgus Angulation: The medial and lateral columns are realigned to restore the normal carrying angle. This is assessed on the AP fluoroscopic image, ensuring the condyles are perpendicular to the long axis of the humerus. Baumann's angle will be evaluated post-reduction.
- Rotation: This is the most challenging and frequently missed deformity, leading to cubitus varus malunion. In extension-type fractures, the distal fragment is typically internally rotated relative to the proximal fragment. Correcting this involves gently externally rotating the forearm and distal fragment . True lateral fluoroscopic views are essential to confirm rotational alignment (e.g., parallel olecranon and coronoid fossae, symmetric condyles). If the fracture is posteromedially displaced, the forearm is often externally rotated; if posterolaterally displaced, the forearm is internally rotated relative to the humerus to derotate the distal fragment.
-
Flexion Reduction Maneuver:
- For the vast majority of extension-type fractures, after length, translation, and rotation are corrected, the final step involves locking the fragments into reduction.
- The elbow is gradually flexed from the initial 20-30 degrees of flexion.
- Simultaneously, the surgeon applies anterior pressure on the olecranon (and thereby the distal humeral condyles) with the thumbs. This counteracts the posterior displacement tendency of the distal fragment and pushes it anteriorly, engaging the posterior cortex of the proximal fragment.
- The elbow is often brought into hyperflexion (as much as 120-130 degrees, if tolerated) to lock the fracture in place by tensioning the triceps and anterior capsule.
-

Assessment of Reduction (Fluoroscopic Criteria)
Once the reduction is achieved and the elbow is held in hyperflexion, its adequacy is meticulously assessed using fluoroscopy in multiple planes.
*
True Lateral View:
*
Anterior Humeral Line (AHL):
A line drawn along the anterior cortex of the humerus must pass through the
middle third of the capitellum
. If it passes anterior to the capitellum, residual hyperextension deformity (extension malunion) is present. If it passes posterior to the capitellum, a flexion malunion exists.
*
Posterior Cortex:
Should be smooth and continuous, indicating sagittal plane alignment.
*
Rotational Alignment:
Assessed by the superimposition of the medial and lateral condyles, making the capitellum and trochlea appear as a single, rounded structure. The olecranon and coronoid fossae should also appear well aligned.
*
True AP View:
*
Baumann's Angle (Humeral Capitellar Angle):
This angle, formed by the shaft of the humerus and the physis of the capitellum, should be within the normal range of
10-15 degrees
relative to the contralateral side (or 70-75 degrees relative to the humeral shaft). An increased angle indicates cubitus varus, and a decreased angle indicates cubitus valgus.
*
Medial and Lateral Columns:
Should be realigned, correcting any varus or valgus angulation.
*
Translation:
Medial and lateral translation should be corrected.
*
Oblique Views:
* Confirm intact medial and lateral columns and rule out subtle rotational malalignment or comminution not visible on true AP/lateral views.
Pinning Strategy
Once an anatomically acceptable reduction is confirmed, K-wires are inserted percutaneously to stabilize the fracture. The elbow is typically maintained in hyperflexion during pin placement to tension the posterior capsule and reduce the risk of iatrogenic ulnar nerve injury with medial pin insertion. The forearm is held in pronation for medial pinning (moves the ulnar nerve anteriorly), and in supination for lateral pinning (moves radial nerve away).
The choice of pinning configuration remains a subject of debate, with lateral-entry pins and cross-pins being the most common.
-
Lateral Entry Pins (Two divergent lateral pins):
-
Technique:
Two K-wires (typically 1.6mm or 2.0mm) are inserted from the lateral epicondyle region. The entry points should be far enough apart to create a broad base.
- The first pin is directed proximally and medially, aiming to engage the medial cortex of the proximal humeral shaft, ideally crossing the fracture site twice.
- The second pin is inserted more proximally and directed proximally and medially but in a slightly different trajectory, often parallel or slightly divergent to the first pin. It should also engage the medial cortex of the proximal fragment.
- Advantages: Significantly lower risk of iatrogenic ulnar nerve injury as no medial skin incision or pin is used.
- Disadvantages: Biomechanically less stable than cross-pins, especially in highly comminuted or unstable fractures. If both pins exit posteriorly, they may be less stable.
-
Technique:
Two K-wires (typically 1.6mm or 2.0mm) are inserted from the lateral epicondyle region. The entry points should be far enough apart to create a broad base.
-
Cross-Pins (One medial, one lateral):
-
Technique:
- A medial pin is typically inserted first. With the elbow hyperflexed and forearm pronated (to protect the ulnar nerve by moving it anteriorly), a K-wire is inserted from the medial epicondyle. It is directed proximally and laterally, aiming to engage the lateral cortex of the proximal humeral shaft. A mini-open approach with direct visualization and retraction of the ulnar nerve is recommended for the medial pin by many surgeons to minimize nerve injury risk.
- A lateral pin is then inserted from the lateral epicondyle, directed proximally and medially, aiming to engage the medial cortex of the proximal humeral shaft.
- Advantages: Biomechanically the most stable construct, providing superior resistance to rotational and varus/valgus forces due to the crossing nature and wide spread of the pins.
- Disadvantages: Highest risk of iatrogenic ulnar nerve injury due to the proximity of the medial epicondyle to the nerve. This risk is mitigated by careful technique (hyperflexion, pronation, mini-open approach).
-
Technique:
-
Hybrid Constructs:
- Some surgeons advocate for two lateral pins and one medial pin, aiming to combine the stability of cross-pins with a reduced risk profile for the ulnar nerve by making the medial pin less critical for overall stability.
General Pinning Principles:
* All pins should achieve a good purchase in both the distal and proximal fragments, ideally engaging the opposite cortex.
* Avoid entering the olecranon fossa or articular surface.
* Check pin placement and fracture stability under fluoroscopy in AP, lateral, and oblique views.
* The pins should be bent outside the skin and cut short, then capped or covered with sterile dressings. They should not be left flush with the skin, as this makes removal difficult and increases the risk of skin erosion.
* The forearm is generally held in pronation for the final immobilization to potentially reduce the tension on the ulnar nerve, particularly if a medial pin has been inserted.
*
 (This image can represent the final pinned construct with the forearm pronated, or demonstrate specific pin insertion technique if applicable).
(This image can represent the final pinned construct with the forearm pronated, or demonstrate specific pin insertion technique if applicable).
After successful pinning, the tourniquet is deflated. Neurovascular status of the hand is re-assessed immediately. A well-padded, long-arm posterior splint (sugar-tong or U-splint) is applied with the elbow at approximately 90 degrees of flexion and the forearm in pronation. This splint provides additional protection and stability without being overly constrictive.
Complications & Management
Despite meticulous surgical technique, complications can arise following closed reduction and percutaneous pinning (CRPP) of supracondylar humeral fractures. Recognition and prompt management are essential for optimal outcomes.
| Complication | Incidence | Etiology | Salvage / Management Strategy |
|---|---|---|---|
| Vascular Injury | 0.5-1% true arterial injury; 5-10% pulseless (perfused) | Brachial artery entrapment (proximal fragment), laceration, spasm, intimal tear. | Pulseless/Perfused: Urgent reduction and pinning. Observe. If pulse doesn't return, often resolves spontaneously. Pulseless/Ischemic: Immediate exploration. Reduction, pin stabilization. If no pulse restoration, consult vascular surgery for possible fasciotomy/repair/graft. |
| Nerve Injury | 10-20% pre-op (median > radial > ulnar); <5% iatrogenic (ulnar) | Stretch, direct trauma, entrapment (median nerve in brachialis), iatrogenic (ulnar nerve from medial pin). | Pre-op: Most resolve spontaneously (neurapraxia). Observe for 6-12 weeks. EMG/NCS if no improvement. Iatrogenic: If recognized intra-op, remove/reposition pin. If post-op, remove pin immediately. Persistent deficit: consider exploration after 3-6 months. Most resolve. |
| Malunion | |||
| * Cubitus Varus (Gunstock) | 10-30% (most common) | Inadequate reduction (medial column collapse, rotational malunion), growth disturbance. | Observation for mild cosmetic deformity. For significant functional or cosmetic concern, corrective osteotomy (e.g., dome osteotomy) after skeletal maturity. |
| * Cubitus Valgus | Rare | Medial column overgrowth, often associated with physeal injury. | Corrective osteotomy. |
| * Flexion/Extension Malunion | Variable | Inadequate sagittal plane reduction (AHL not crossing capitellum in middle third). | Minor impact on function. Rare indications for corrective osteotomy for severe functional deficit. |
| Elbow Stiffness/Loss of Motion | 5-10% (minor loss more common) | Prolonged immobilization, heterotopic ossification, intra-articular adhesions. | Early active range of motion post-pin removal. Avoid aggressive passive ROM. Physical therapy. For persistent severe stiffness, consider manipulation under anesthesia or arthrolysis (rare). |
| Compartment Syndrome | <0.1% | Increased intra-compartmental pressure due to hemorrhage/edema, tight cast. Risk increased with vascular injury. | Immediate diagnosis (5 Ps, intracompartmental pressure measurement). Urgent forearm fasciotomy. Remove tight dressings/cast. |
| Pin Tract Infection | 2-5% (superficial) | Poor pin site care, prolonged pin presence, inadequate asepsis. | Local wound care, oral antibiotics for superficial infection. For deep infection, debridement and IV antibiotics. Pin removal may be necessary. |
| Pin Migration/Breakage | Rare | Loosening of fixation, premature weight-bearing, trauma. | Surgical removal of migrated/broken pin. Re-fixation if fracture unstable. |
| Refracture | <1% | Premature removal of pins/splint, insufficient healing, trauma. | Re-reduction and re-pinning. |
| Physeal Arrest | Very rare | Direct pin injury to physis, severe trauma. | Potential for growth disturbance. May require corrective osteotomy if significant limb length discrepancy or angulation occurs. |
| Heterotopic Ossification | Rare, but can cause stiffness | Post-traumatic inflammation, aggressive early PROM. | Prophylaxis with NSAIDs (e.g., indomethacin) for high-risk patients. For established HO, physical therapy, sometimes surgical excision once mature. |
Specific Considerations:
- Pulseless Hand (Pink Pulseless Hand): This is a critical scenario. After closed reduction and pinning, if the radial pulse does not return but the hand remains well-perfused (pink, warm, good capillary refill), initial management typically involves observation. The vast majority (80-90%) of these cases are due to brachial artery spasm or dynamic entrapment and will recover spontaneously without exploration. However, the child must be closely monitored in a high-dependency unit for 24-48 hours. If there are signs of neurological deterioration (e.g., anterior interosseous nerve palsy) or impending ischemia, urgent vascular exploration is warranted.
- Irreducible Fractures: If repeated attempts at closed reduction fail, consider soft tissue interposition (e.g., brachialis muscle, median nerve, anterior capsule). Conversion to an open reduction (usually via an anterior approach) is indicated. This allows direct visualization and removal of entrapped tissues.
- Ulnar Nerve Injury: Iatrogenic ulnar nerve injury is a recognized risk of medial pin placement. If a deficit is noted post-operatively, especially motor weakness (e.g., intrinsic hand muscle weakness), the pin should be immediately removed or repositioned. Most iatrogenic injuries are neurapraxias and resolve. Prophylactic mini-open approach for medial pinning is increasingly popular to directly visualize and protect the ulnar nerve.
Post-Operative Rehabilitation Protocols
Post-operative management following CRPP for supracondylar humeral fractures is designed to protect the fracture fixation, prevent complications, and restore elbow function. The protocol typically progresses through several phases.
Phase 1: Immobilization and Protection (0-3/4 Weeks)
-
Immediate Post-Op:
- Splint: A well-padded, non-constrictive long-arm posterior splint (or U-splint, or sugar-tong splint) is applied immediately post-operatively. The elbow is typically positioned at approximately 90 degrees of flexion (or slightly less, e.g., 70-80 degrees, to avoid excessive ulnar nerve tension if a medial pin is present and hyperflexion was used for reduction) with the forearm in pronation . Pronation is thought to move the ulnar nerve away from the medial epicondyle and any medial pins.
- Monitoring: Continuous close monitoring of neurovascular status (pulses, capillary refill, sensation, motor function) is paramount, especially in the first 24-48 hours, due to the risk of swelling, vascular compromise, and compartment syndrome.
- Pain Management: Appropriate analgesia is provided.
- Pin Site Care: Pin sites are kept clean and dry. Parents/caregivers are instructed on signs of infection.
- Duration of Immobilization: The splint is usually maintained for 3-4 weeks . In younger children or those with less stable fractures, it may extend to 6 weeks.
- Activity: Strict activity restrictions are enforced. The child is encouraged to keep the arm elevated (e.g., in a sling) and avoid any strenuous activity or direct trauma to the elbow. Gentle finger and wrist active range of motion (AROM) is encouraged to prevent stiffness in the hand and wrist.
Phase 2: Pin Removal and Initiation of Motion (3/4-6 Weeks)
- Radiographic Assessment: At 3-4 weeks (or as clinically indicated), follow-up radiographs (AP and lateral) are obtained to assess fracture healing. Early callus formation and stability are usually evident.
- Pin Removal: Once adequate radiographic healing is observed and the fracture feels clinically stable, the K-wires are removed in an outpatient setting. This is a relatively quick procedure, often performed under local anesthesia or light sedation.
- Post-Removal Immobilization: After pin removal, the arm is often placed back into a removable posterior long-arm splint for an additional 1-2 weeks, particularly for younger children or if there is any concern for residual instability. Some surgeons may transition directly to active range of motion exercises without further splinting if healing is robust.
-
Initiation of Active Range of Motion (AROM):
- Crucial Principle: Gentle active range of motion (AROM) is initiated immediately after pin/splint removal.
- Avoid Passive Range of Motion (PROM): Aggressive passive stretching or forced motion is strictly discouraged in the early phases, as it can incite heterotopic ossification and increase pain and stiffness. The patient should be encouraged to use their own muscle power to move the elbow.
- Gravity-Assisted Exercises: Simple gravity-assisted exercises (e.g., leaning forward with the arm extended, using the weight of the hand to gently extend the elbow) are often beneficial.
- Play-Based Therapy: For children, incorporating therapeutic exercises into play activities (e.g., reaching for toys, stacking blocks) is highly effective.
- Discontinuation of Sling: As comfort and motion improve, the sling is gradually weaned.
Phase 3: Strengthening and Return to Activity (6+ Weeks)
- Gradual Strengthening: Once a good pain-free AROM is achieved, gentle strengthening exercises can be introduced. This typically begins with light isometric exercises and progresses to light resistance exercises using elastic bands or very light weights.
- Functional Activities: Progressive return to age-appropriate functional activities is encouraged.
-
Return to Sports:
- Contact sports and activities involving significant risk of re-injury (e.g., gymnastics, climbing, throwing) are usually restricted until full range of motion, strength, and confidence are restored, typically around 8-12 weeks post-injury.
- Radiographic evidence of complete fracture consolidation is desired before return to high-impact activities.
- Expected Outcomes: Most children regain excellent to full range of motion and strength following supracondylar fracture treatment. Minor loss of full extension (up to 5-10 degrees) is common but rarely functionally limiting. Persistent stiffness or pain should prompt further investigation.
Important Rehabilitation Considerations:
*
Parent/Caregiver Education:
Comprehensive education for parents regarding activity restrictions, home exercise programs, and warning signs is vital for successful rehabilitation.
*
Therapist Involvement:
While many children recover well with home exercises, physical or occupational therapy may be beneficial for those experiencing significant stiffness, fear of movement, or persistent weakness.
*
Long-Term Follow-up:
Patients should be monitored for potential late complications such as cubitus varus, which may become more apparent with growth.
Summary of Key Literature / Guidelines
The management of displaced supracondylar humeral fractures has evolved over decades, with closed reduction and percutaneous pinning (CRPP) establishing itself as the gold standard for Gartland Type II (unstable), III, and IV fractures. Key literature and guidelines emphasize a few critical points:
-
CRPP as the Treatment of Choice: Numerous studies and systematic reviews consistently demonstrate that CRPP provides superior outcomes compared to casting alone for displaced supracondylar fractures, offering better maintenance of reduction, lower rates of malunion (especially cubitus varus), and acceptable complication rates.
-
Pin Configuration Debate (Lateral vs. Cross-Pins):
- Cross-Pins (medial and lateral): Biomechanically, cross-pins (medial and lateral) offer superior stability against all planes of displacement and rotation compared to lateral-only pins. This has been supported by various cadaveric and in vitro studies.
- Lateral-Entry Pins: Lateral-only pin constructs were introduced to mitigate the risk of iatrogenic ulnar nerve injury associated with medial pin placement. While biomechanically less robust than cross-pins, clinical studies have shown comparable outcomes in terms of maintaining reduction and avoiding cubitus varus when adequately divergent and engaged in the medial column.
- Clinical Outcomes: Many meta-analyses suggest that while cross-pins may provide slightly better stability, the clinical outcomes (e.g., range of motion, functional scores, incidence of cubitus varus) between cross-pinning and lateral-entry pinning are often not statistically different, particularly if the lateral pins are appropriately placed and divergent. The incidence of iatrogenic ulnar nerve injury is unequivocally higher with medial pins.
- Recommendation: The choice often comes down to surgeon preference, fracture pattern, and comfort with ulnar nerve protection. A mini-open approach for medial pin placement is increasingly advocated to directly visualize and protect the ulnar nerve, thus allowing surgeons to safely utilize the biomechanical advantages of cross-pinning. For challenging or highly unstable fractures, cross-pinning (with appropriate ulnar nerve precautions) may be favored.
-
Importance of Anatomical Reduction: Achieving anatomical reduction, particularly in terms of sagittal alignment (assessed by the anterior humeral line) and rotational alignment, is paramount. Persistent rotation is a significant contributor to cubitus varus, which, while often cosmetic, can be a source of functional concern. Baumann's angle remains a reliable indicator for varus/valgus alignment.
-
Management of Pulseless Extremity: The "pink pulseless hand" scenario is well-addressed in the literature. Current consensus supports urgent closed reduction and pinning. If the pulse does not return but the hand remains well-perfused, close observation in a high-dependency setting is generally recommended, as most cases resolve spontaneously. Surgical exploration for vascular repair is reserved for signs of frank ischemia or neurological deterioration.
-
Role of Open Reduction: While CRPP is preferred, literature supports conversion to open reduction when closed reduction attempts fail (often due to soft tissue interposition) or in the context of open fractures requiring debridement. The most common approach for open reduction is anterior (Henry approach) or medial.
-
Long-Term Outcomes and Cubitus Varus: Cubitus varus (gunstock deformity) is the most common long-term complication, occurring in 10-30% of cases, often due to inadequate reduction or medial column collapse. While primarily a cosmetic deformity, severe cases can alter elbow biomechanics. Corrective osteotomy is the salvage procedure, typically performed after skeletal maturity.
-
Evidence-Based Guidelines: Major orthopedic societies (e.g., AAOS) provide clinical practice guidelines that largely reinforce the principles of urgent reduction and stable fixation, tailored to the Gartland classification. Emphasis is placed on comprehensive neurovascular assessment both pre- and post-operatively, and meticulous fluoroscopic control during reduction and pinning.
In conclusion, the successful management of supracondylar humeral fractures hinges on a thorough understanding of the anatomy, precise closed reduction maneuvers, judicious application of percutaneous pinning, and vigilant post-operative monitoring and rehabilitation, all guided by a robust evidence base.