Introduction & Epidemiology
Pelvic ring fractures represent severe skeletal trauma, frequently associated with high-energy mechanisms such as motor vehicle collisions, falls from height, and crush injuries. These injuries are complex, often involving significant hemorrhage, neurovascular damage, and visceral injury, contributing to high morbidity and mortality rates. The Advanced Trauma Life Support (ATLS) protocol forms the bedrock of initial assessment and management, emphasizing a systematic approach to identify and address life-threatening conditions.
Epidemiologically, pelvic fractures account for approximately 2-9% of all skeletal fractures in trauma patients. While the overall incidence is relatively low, the mortality rate can range from 5% in stable fractures to over 30% in hemodynamically unstable patients, particularly those with open fractures or severe associated injuries. The retroperitoneal space, with its extensive venous plexus and major arterial branches (internal iliac system), can accommodate large volumes of blood, making hemorrhage the leading cause of early mortality. Approximately 80-90% of significant pelvic hemorrhage is venous in origin, with arterial bleeding accounting for the remaining 10-20%, often from branches of the internal iliac artery (e.g., superior gluteal, obturator arteries).
Understanding the ATLS paradigm is critical for orthopedic surgeons. The primary survey (Airway, Breathing, Circulation, Disability, Exposure) prioritizes life-saving interventions, including rapid identification and control of hemorrhage. The secondary survey involves a more detailed head-to-toe examination, often identifying associated injuries that mandate specific management strategies. Adjuncts to the primary and secondary surveys, such as focused assessment with sonography for trauma (FAST) and plain radiographs (AP pelvis, chest X-ray), are integral for timely decision-making.
Pelvic fractures are typically classified using systems like Young-Burgess (based on mechanism of injury: Anteroposterior Compression, Lateral Compression, Vertical Shear, Combined Mechanism) or Tile (based on stability: Type A - stable, Type B - rotationally unstable but vertically stable, Type C - rotationally and vertically unstable). These classifications guide initial assessment, prognostication, and definitive management strategies. The immediate goal within the ATLS framework is not definitive fixation, but rather hemodynamic stabilization and mechanical stabilization of the pelvic ring to tamponade bleeding.
Surgical Anatomy & Biomechanics
A thorough understanding of pelvic anatomy and biomechanics is paramount for effective management of pelvic ring injuries. The pelvis is a bony ring comprising the sacrum posteriorly and the two innominate bones (ilium, ischium, pubis) anteriorly, joined by the pubic symphysis and sacroiliac (SI) joints.
Bony Anatomy
- Sacrum: A key component of the posterior pelvic ring, articulating with the ilia. Fractures here (Denis zones I, II, III) significantly impact stability and carry neurological risks.
- Ilium: Forms the superior and posterior part of the innominate bone.
- Ischium: Forms the inferior and posterior part, including the ischial tuberosity.
- Pubis: Forms the anterior part, articulating at the pubic symphysis.
Ligamentous Structures
The stability of the pelvic ring is critically dependent on its robust ligamentous complex.
*
Anterior Ligamentous Complex:
*
Pubic Symphysis:
Stabilized by superior, inferior (arcuate), anterior, and posterior pubic ligaments. Diastasis here indicates significant anterior disruption.
*
Posterior Ligamentous Complex:
These are the strongest ligaments and are crucial for vertical and rotational stability.
*
Sacroiliac Ligaments:
*
Anterior Sacroiliac Ligaments:
Weaker, contribute to rotational stability.
*
Posterior Sacroiliac Ligaments (Short and Long):
Strongest, resist vertical and rotational forces. Injury to these implies significant instability.
*
Interosseous Sacroiliac Ligaments:
Deep to the posterior ligaments, very strong, resist all movements. Disruption indicates severe injury.
*
Sacrotuberous and Sacrospinous Ligaments:
These accessory ligaments connect the sacrum/coccyx to the ischial tuberosity and ischial spine, respectively. They convert the greater and lesser sciatic notches into foramina and provide important rotational and vertical stability.
Neurovascular Structures
The retroperitoneum within the confines of the bony pelvis harbors critical neurovascular structures susceptible to injury from fractures or iatrogenic damage during fixation.
*
Arterial Supply:
The internal iliac arteries and their branches (superior gluteal, inferior gluteal, obturator, internal pudendal, lateral sacral) are primary sources of arterial hemorrhage.
*
Venous Plexus:
The presacral venous plexus and internal iliac veins are extensive and lack valves, making them a common source of high-volume, low-pressure venous bleeding that is difficult to tamponade without mechanical stabilization.
*
Nerve Roots and Plexus:
The lumbosacral plexus (L4-S4 nerve roots) lies immediately anterior to the sacrum, susceptible to direct impingement from sacral fractures or iatrogenic injury during iliosacral screw placement. The L5 nerve root is particularly vulnerable. The sciatic nerve exits the pelvis via the greater sciatic foramen, also at risk.
Biomechanics and Injury Mechanisms
Pelvic ring injuries are classified by the mechanism of force application, dictating the pattern of instability and potential associated injuries.
*
Anteroposterior Compression (APC):
Typically from head-on collisions or direct blows to the anterior pelvis.
*
APC I:
Pubic symphysis diastasis < 2.5 cm, intact posterior ligaments. Rotationally stable.
*
APC II:
Pubic symphysis diastasis > 2.5 cm, anterior SI ligament disruption, intact posterior SI ligaments. Rotationally unstable, vertically stable ("open book" injury).
*
APC III:
Complete disruption of pubic symphysis, anterior and posterior SI ligaments, often with sacrotuberous and sacrospinous ligament tearing. Rotationally and vertically unstable.
*
Lateral Compression (LC):
Most common mechanism, often from side-impact collisions.
*
LC I:
Posterior arch intact. Pubic rami fractures and ipsilateral sacral compression fracture. Stable.
*
LC II:
Pubic rami fractures, posterior arch fracture/dislocation (ipsilateral or contralateral "bucket handle" injury) with posterior iliac wing fracture or SI joint disruption. Rotationally unstable, vertically stable.
*
LC III (Windswept Pelvis):
LC II injury on one side with contralateral APC II or III injury. Rotationally and vertically unstable.
*
Vertical Shear (VS):
High-energy axial load (e.g., fall from height landing on feet). Complete disruption of anterior and posterior pelvic rings with vertical displacement. Highly unstable, very high morbidity/mortality.
The integrity of the posterior pelvic ring (sacrum, SI joints, strong posterior ligaments) is the primary determinant of pelvic stability. Disruption of these structures leads to both rotational and vertical instability, increasing hemorrhage risk and requiring definitive stabilization.
Indications & Contraindications
The decision for operative versus non-operative management of pelvic fractures is complex, balancing hemodynamic stability, mechanical stability, and associated injuries. The ATLS protocol emphasizes initial stabilization, which may include temporary operative interventions, before proceeding to definitive fixation.
Indications for Operative Management
Operative management is primarily indicated for patients with pelvic ring instability or ongoing hemorrhage refractory to non-surgical measures.
*
Hemodynamic Instability:
* Ongoing hemorrhage from pelvic sources, despite fluid resuscitation, blood product transfusion, and external pelvic compression (e.g., binder). This often necessitates emergent angiography/embolization, preperitoneal packing, or external fixation.
*
Mechanical Instability:
*
Vertical Shear (Tile C, Young-Burgess VS):
Always require operative stabilization due to complete disruption of both anterior and posterior rings.
*
Rotationally Unstable (Tile B, Young-Burgess APC II/III, LC II/III):
* Pubic symphysis diastasis > 2.5 cm (APC II/III).
* Disruption of posterior sacroiliac ligaments (APC III, LC II/III).
* Significantly displaced sacral fractures (Denis zones II/III, U-type or H-type fractures).
*
Open Pelvic Fractures:
Require emergent debridement and often diverting colostomy in addition to fracture stabilization due to high infection risk and mortality.
*
Neurological Deficits:
Associated with sacral fractures where bony fragments impinge on nerve roots (L5, S1-S4). Decompression and fixation are indicated.
*
Associated Acetabular Fractures:
Often dictate the surgical approach and overall management strategy.
*
Failure of Non-Operative Management:
Progressive displacement, intractable pain, or inability to mobilize.
Indications for Non-Operative Management
Non-operative management is reserved for stable pelvic ring injuries.
*
Hemodynamically Stable Patients:
Without ongoing hemorrhage attributed to the pelvis.
*
Mechanically Stable Pelvic Ring (Tile A, Young-Burgess APC I, LC I):
* Isolated pubic rami fractures (unilateral or bilateral), nondisplaced.
* Minimally displaced iliac wing fractures.
* Avulsion fractures (e.g., ASIS, AIIS, ischial tuberosity) with minimal displacement and no functional deficit.
* Stable sacral fractures (Denis zone I) without significant displacement or neurological deficit.
*
Patient Comorbidities:
In rare circumstances, severe underlying comorbidities may temporarily or permanently contraindicate surgical intervention, especially in frail elderly patients with low-energy fractures. However, instability and hemorrhage typically override these concerns.
Contraindications
Absolute contraindications to life-saving pelvic fracture surgery are rare and usually relate to the patient's overall medical status precluding anesthesia. Relative contraindications may include:
* Overwhelming polytrauma with non-salvageable neurological injury or other life-threatening conditions where pelvic fixation would divert resources from more critical interventions.
* Severe contamination of an open fracture site, requiring initial damage control before definitive fixation.
Table: Operative vs. Non-Operative Indications for Pelvic Ring Fractures
| Feature/Condition | Operative Management | Non-Operative Management |
|---|---|---|
| Hemodynamic Status | Hemodynamically unstable due to pelvic hemorrhage (refractory to initial resuscitation) | Hemodynamically stable, no ongoing significant hemorrhage |
| Mechanical Stability | Rotationally AND vertically unstable (e.g., VS, APC III, LC III) | Stable or minimally rotationally unstable (e.g., APC I, LC I) |
| Pubic Symphysis Diastasis | > 2.5 cm | < 2.5 cm |
| Posterior Arch Integrity | Disrupted (e.g., SI joint disruption, displaced sacral fracture) | Intact or minimally disrupted (e.g., stable sacral fracture) |
| Fracture Type (Young-Burgess) | VS, APC II/III, LC II/III with posterior injury | APC I, LC I (isolated rami, stable sacral ala) |
| Fracture Type (Tile) | B2, B3, C1, C2, C3 | A1, A2, B1 |
| Open Fracture | Yes | No |
| Neurological Deficit | Present and related to fracture impingement | Absent or unrelated |
| Associated Injuries | Significant visceral/vascular injury requiring surgical exploration/repair | Minor or controlled associated injuries |
| Progression/Pain | Progressive displacement or intractable pain on non-op management | Stable, manageable pain |
Pre-Operative Planning & Patient Positioning
Comprehensive pre-operative planning is essential for optimizing outcomes in pelvic fracture management, encompassing resuscitation, imaging, consultations, and meticulous surgical setup.
ATLS Principles and Initial Resuscitation
-
Primary Survey (ABCDE):
- Airway: Ensure patency, consider intubation if GCS < 8 or respiratory compromise.
- Breathing: Address pneumothorax, hemothorax.
-
Circulation:
The most critical component for pelvic fractures. Rapid identification of hypovolemic shock.
- Fluid Resuscitation: Initial boluses of crystalloids, but transition rapidly to blood products (pRBCs, FFP, platelets) as per massive transfusion protocols.
- Pelvic Binder/Sheet: Application around the greater trochanters and symphysis pubis to reduce pelvic volume, internally compress bleeding vessels, and provide temporary mechanical stability. This is a critical early intervention.
- FAST Exam: To identify intra-abdominal hemorrhage.
-
Secondary Survey:
Detailed head-to-toe examination to identify all injuries.
- Log-roll: Carefully assess the posterior pelvis for open wounds, sacral tenderness, or crepitus.
- Rectal/Vaginal Exam: Assess for open fractures, gross blood, sphincter tone, prostate position (in males).
Imaging Modalities
-
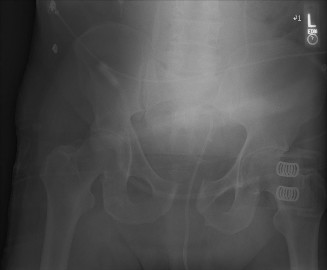
Plain Radiographs:
- AP Pelvis: Initial mandatory view, assesses overall ring integrity, symphysis diastasis, pubic rami fractures, gross SI joint displacement, sacral fractures.
- Inlet View: Projects posterior structures (sacrum, SI joints) without superimposition. Useful for assessing sacral kyphosis/angulation and anterior-posterior displacement of the posterior ring.
-
Outlet View:
Projects superiorly displaced hemipelvis, assessing vertical migration of the hemipelvis and sacral lordosis/angulation.
-
Computed Tomography (CT) Scan:
The gold standard for definitive fracture characterization.
- Pelvic CT with Contrast: Provides detailed bony anatomy, identifies small fractures, assesses SI joint integrity, detects retroperitoneal hemorrhage volume, identifies arterial blush (indicative of active arterial bleeding), and evaluates associated visceral injuries (bladder, urethra, bowel).
- CT Angiography: If active arterial bleeding is suspected or identified, for localization prior to embolization.
- Urethrogram/Cystogram: Indicated for suspected genitourinary injuries (blood at meatus, scrotal/perineal hematoma, high-riding prostate, gross hematuria).
Hemorrhage Control Strategies
Beyond pelvic binders:
*
Angiography and Embolization:
Indicated for active arterial extravasation identified on CT angiography, or persistent hemodynamic instability despite adequate resuscitation and mechanical stabilization, where an arterial source is suspected. Effective for arterial bleeds, less so for venous.
*
Preperitoneal Pelvic Packing:
Performed via a suprapubic incision, often by general surgeons or orthopedic trauma surgeons. Direct packing of the retroperitoneal space to tamponade venous and small arterial bleeding. Highly effective for venous hemorrhage, particularly when embolization is unavailable or unsuccessful. Often combined with external fixation.
Consultations
A multidisciplinary approach is crucial.
*
General Surgery:
For abdominal/visceral injuries, open fractures, diagnostic peritoneal lavage (if indicated), preperitoneal packing.
*
Urology:
For genitourinary trauma (urethral/bladder rupture).
*
Vascular Surgery:
For major vascular injuries identified (rarely primary source of pelvic bleed, usually iatrogenic or associated).
*
Interventional Radiology:
For angiography and embolization.
*
Intensivist:
For critically ill patients, managing resuscitation and organ support.
Timing of Definitive Fixation
- Emergent (within hours): Hemodynamically unstable patients requiring external fixation, preperitoneal packing, or embolization. Open fractures (debridement).
- Urgent (within 24-48 hours): Mechanically unstable but hemodynamically stable patients, once resuscitation is optimized.
- Elective (days to weeks): Stable, minimally displaced fractures, or after initial damage control for complex polytrauma patients (often after external fixation). The "golden window" for definitive fixation is generally considered within 5-7 days.
Patient Positioning
- Supine: For initial resuscitation, external fixation, preperitoneal packing, anterior approaches to the pubic symphysis, and percutaneous iliosacral screw insertion. A radiolucent table is essential.
- Prone: For open posterior approaches to the sacrum or SI joint. Often requires a chest/thigh support frame (e.g., Jackson table) to allow the abdomen to hang free, reducing intra-abdominal pressure and venous bleeding.
- Lateral Decubitus: Less common, but may be used for specific unilateral posterior approaches.
- Traction Table: Can be used to aid reduction of vertical shear injuries or facilitate exposure for anterior approaches, but requires careful management of soft tissues and skin.
Detailed Surgical Approach / Technique
The surgical management of pelvic ring fractures involves both temporary stabilization for hemorrhage control and definitive internal or external fixation. The choice of technique depends on the fracture pattern, stability, patient status, and associated injuries.
Temporary Stabilization (ATLS Context)
-
Pelvic Binder/Sheet:
- Principle: Reduces pelvic volume and externally compresses bleeding vessels.
- Application: Applied circumferentially at the level of the greater trochanters, not the iliac crests, to achieve internal rotation and approximation of the anterior and posterior pelvic rings. The symphysis pubis is typically aligned with the center of the binder.
- Note: Should not be left on for prolonged periods (e.g., >24 hours) due to risk of skin breakdown and pressure sores.
-
External Fixation (Ex-Fix):
- Indications: Hemodynamically unstable APC and LC type fractures, gross symphyseal diastasis, to aid reduction, and as a temporary measure in polytrauma patients.
-
Anterior Frame (most common for temporary stabilization):
- Pin Placement: Typically two Schanz pins inserted into each iliac crest, either supra-acetabular (superior to the anterior inferior iliac spine (AIIS)) or infra-acetabular (into the supra-acetabular corridor). Supra-acetabular pins are easier and quicker but have less purchase. Infra-acetabular (e.g., Dyacrofix) pins offer better stability and purchase but require more surgical expertise. Pins are angled posteriorly 10-20 degrees and medially 20-30 degrees to avoid injury to neurovascular structures (lateral femoral cutaneous nerve, deep circumflex iliac artery/vein) and penetrate dense bone.
- Technique: Small incisions, blunt dissection down to the outer cortex of the ilium. Periosteum is incised, and a drill bit is used to create pilot holes. Schanz pins (e.g., 5-6mm diameter) are then inserted. Care must be taken to ensure pins are parallel and perpendicular to the axis of fracture reduction.
- Frame Assembly: Pins are connected by a carbon fiber rod or metal frame, compressed across the symphysis to reduce the "open book" injury and provide stability.
- Posterior Frame: Less commonly used for temporary stabilization but can be incorporated for definitive fixation.
-
Preperitoneal Pelvic Packing:
- Indications: Persistent hemodynamic instability despite resuscitation and external compression (binder/ex-fix), especially when venous bleeding is suspected or angiography has failed to identify/control arterial bleeding.
- Technique: A small suprapubic incision is made, and the preperitoneal space is bluntly dissected. Three laparotomy sponges are packed firmly into each side of the retroperitoneal space adjacent to the bladder and pelvic sidewalls. The incision is then closed temporarily. Patients are typically taken for repacking and exploration in 24-48 hours.
Definitive Fixation Approaches
Definitive fixation involves reducing fracture displacement and providing stable internal fixation. This often requires a combination of anterior and posterior stabilization.
1. Anterior Fixation (Pubic Symphysis / Pubic Rami)
-
Approach:
- Pfannenstiel Incision: A transverse curvilinear incision made suprapubically, dissecting down to the rectus fascia. The rectus muscles are split in the midline or elevated from the superior pubic ramus. The bladder is identified and retracted inferiorly.
- Modified Stoppa Approach: A wider, more extensile approach, allows for exposure of the pelvic brim and quadrilateral plate, useful for combined anterior and posterior ring injuries, often for intrapelvic plating.
-
Reduction:
- For symphyseal diastasis, reduction is achieved by applying direct anterior-posterior compression with bone clamps (e.g., Farabeuf, Weber) or by using the external fixator to gain preliminary reduction. Care must be taken to avoid over-reduction or tilting.
-
Fixation:
- Symphyseal Plating: A 3.5mm reconstruction plate (typically 2-4 holes) or a dedicated symphyseal plate is contoured and applied to the superior aspect of the pubic symphysis. Bicortical screws are used. For highly unstable injuries (APC III), a second plate can be applied anteriorly for increased stability, or an internal fixator (INFIX) device can be used as an alternative to external fixation.
- Pubic Rami Plating/Screws: Displaced pubic rami fractures can be fixed with small plates or intramedullary screws via a mini-open or percutaneous technique, though this is less common for isolated rami fractures without posterior instability.
2. Posterior Fixation (Sacroiliac Joint / Sacrum)
Posterior fixation is critical for vertical and rotational stability.
-
Percutaneous Iliosacral Screws:
- Indications: SI joint dislocation/fracture-dislocation, sacral fractures (Denis zones I, II, III). Preferred method due to minimal invasiveness.
-
Technique:
Performed under fluoroscopic guidance (inlet, outlet, lateral sacral views, +/- Judet views for SI joint). The patient is typically supine on a radiolucent table.
- Entry Point: Posterior superior iliac spine (PSIS) region, usually slightly inferior and anterior to the PSIS.
- Trajectory: Requires precise navigation through the dense bone of the ilium into the body of S1 and/or S2, avoiding the sacral foramina and neurovascular structures. A guide wire is placed, verified in multiple views, over-drilled, and a cannulated screw (typically 7.0-8.0 mm partially threaded) is inserted.
- S1 Screws: Common, aim for the S1 vertebral body.
- S2 Screws: Can be used for S2 fractures or to augment S1 fixation, but higher risk of nerve injury.
- Transsacral (Transforaminal) Screws: For sacral fractures, where the screw crosses the fracture line and gains purchase in the contralateral sacral ala or ilium.
- Bilateral Screws: Often required for unstable injuries.
- Complications: L5 nerve root injury is a significant risk with S1 screws if the trajectory is too anterior or caudal.
-
Open Reduction and Internal Fixation (ORIF) of the Posterior Pelvis:
- Indications: Significantly displaced SI joint injuries, complex sacral fractures (e.g., U-type, H-type), nerve root impingement requiring decompression, or when percutaneous techniques are not feasible or fail.
-
Approaches:
- Posterior Gluteal Approach (e.g., Galveston, Kocher-Langenbeck variant): Exposes the posterior ilium and SI joint. Can split gluteus maximus fibers. Allows for direct visualization, reduction, and plate fixation.
- Modified Stoppa (Intrapelvic) Approach: While primarily anterior, it can provide access to the anterior aspect of the SI joint and sacral ala for direct plating or buttressing.
- Reduction: Direct visualization and manipulation using bone hooks, clamps, and traction.
-
Fixation:
- SI Joint Plating: Plates can be applied across the SI joint (often an anterior plate or a posterior tension band plate) after direct reduction.
- Sacral Plate Fixation: Contoured plates can be used to bridge sacral fractures after direct reduction and decompression.
- Tension Band Plating: For specific sacral fractures or SI dislocations, a tension band construct can be created using plates or wires, transforming tensile forces into compression forces.
Combined Pelvic Fixation
Many unstable pelvic ring injuries (e.g., APC III, VS) require both anterior and posterior stabilization to restore full stability. The sequence often depends on the predominant instability and surgeon preference, but posterior fixation is paramount for vertical stability. Often, posterior percutaneous iliosacral screws are performed first, followed by anterior plating.
Complications & Management
Pelvic fractures are associated with a wide array of early and late complications, reflecting the high-energy nature of the injury and the complex anatomy of the region. Prompt recognition and appropriate management are crucial.
Early Complications
-
Hemorrhage:
- Persistent Bleeding: Despite initial resuscitation, external compression, and potential embolization/packing.
- Management: Re-evaluation of hemodynamic status, repeat angiography, repeat preperitoneal packing, damage control laparotomy for intra-abdominal sources, or even open surgical exploration of the retroperitoneum (last resort).
-
Infection:
- Pin Site Infection (External Fixation): Common, particularly with prolonged use or inadequate pin care.
- Deep Wound Infection: Less common but more severe, especially in open fractures or after definitive internal fixation.
- Management: Prophylactic antibiotics, meticulous pin care, debridement, negative pressure wound therapy, culture-directed antibiotics, potential hardware removal once fracture stability allows.
-
Neurovascular Injury:
-
Neurological Deficit:
- Initial: Due to fracture fragment impingement (e.g., L5/S1 nerve root in sacral fractures).
- Iatrogenic: During screw placement (e.g., L5 nerve root with S1 iliosacral screws, sciatic nerve).
- Vascular Injury: Direct injury to major vessels (internal iliac, superior gluteal) from fracture fragments or iatrogenic during surgical dissection/fixation.
- Management: Careful pre-operative imaging review, intra-operative neuromonitoring (if available), fluoroscopic imaging verification for screws. For iatrogenic injury, immediate hardware removal/repositioning. For established deficits, observation, neurolysis, pain management. For vascular injury, urgent vascular surgery consultation for repair.
-
Neurological Deficit:
-
Visceral Injury:
Bladder, urethra, bowel, vagina.
- Management: Early identification (e.g., urethrogram, cystogram), primary repair by urology/general surgery, temporary urinary diversion (suprapubic catheter), diverting colostomy for open rectal injuries.
-
Compartment Syndrome:
Rare but possible in the gluteal compartment or thighs, especially with high-volume fluid resuscitation and prolonged immobilization.
- Management: Clinical suspicion, intracompartmental pressure measurement, urgent fasciotomy.
-
Deep Venous Thrombosis (DVT) and Pulmonary Embolism (PE):
High risk due to hypercoagulable state, immobilization, and direct vascular injury.
- Management: Aggressive prophylaxis (mechanical and pharmacological anticoagulation), early mobilization.
Late Complications
-
Malunion/Nonunion:
- Incidence: Higher in unstable patterns, inadequate fixation, or infection.
- Management: Corrective osteotomy and revision internal fixation, SI joint fusion, or salvage procedures for chronic pain and deformity.
-
Chronic Pain:
- Sources: Malunion, SI joint dysfunction, neuropathic pain (from nerve injury), symphyseal instability.
- Management: Multimodal pain management, physical therapy, nerve blocks, selective injections, SI joint fusion (if indicated).
-
Sexual and Urogenital Dysfunction:
- Causes: Pelvic nerve injury, urethral/bladder injury, chronic pain.
- Management: Urological/gynecological consultation, specific interventions as needed.
-
Gait Disturbance / Leg Length Discrepancy:
Resulting from malunion or persistent instability.
- Management: Physical therapy, shoe lifts, corrective osteotomy.
-
Heterotopic Ossification (HO):
Ectopic bone formation in soft tissues, especially around the hip.
- Management: Prophylaxis (NSAIDs, radiation), surgical excision if symptomatic and mature.
Table: Common Complications of Pelvic Ring Fractures
| Complication | Incidence (%) (approx.) | Salvage/Management Strategy |
|---|---|---|
| Hemorrhage (persistent) | 10-25 | Re-angiography/embolization, preperitoneal packing, repeat resuscitation/transfusion, damage control laparotomy for refractory cases, direct surgical exploration (rare) |
| Infection (pin site/deep) | 5-15 (pin site up to 30) | Meticulous pin care, antibiotics (culture-directed), debridement, negative pressure wound therapy, hardware removal (once stable) |
| Neurological Injury (iatrogenic) | 2-10 (e.g., L5/S1) | Immediate hardware removal/repositioning, precise anatomical knowledge, careful fluoroscopic guidance, neuromonitoring; for established deficits: observation, neurolysis, pain management, functional rehabilitation. |
| Malunion/Nonunion | 5-20 | Corrective osteotomy, revision internal fixation, SI joint fusion, pelvic osteotomy, targeted pain management. |
| Chronic Pain (SI joint, neuropathic) | 20-40 | Multimodal pain management, physical therapy, nerve blocks, SI joint injections/fusion (if instability/arthrosis), hardware removal if symptomatic, referral to pain specialist. |
| DVT/PE | 10-30 | Aggressive chemical and mechanical DVT prophylaxis (pharmacological agents, compression devices), early mobilization, inferior vena cava (IVC) filter in selected high-risk patients with contraindications to anticoagulation. |
| Heterotopic Ossification (HO) | 10-20 | Prophylactic NSAIDs or radiation, observation, surgical excision (if symptomatic and mature, typically 6-12 months post-injury), range of motion exercises. |
| Urogenital Dysfunction | Variable | Urological/gynecological consultation, specific medical or surgical interventions for erectile dysfunction, urinary incontinence, etc. |
| Pin Track Loosening/Failure | Up to 20 | Pin care optimization, antibiotics for infection, revision of pin placement, transition to internal fixation. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following pelvic ring fracture fixation is critical for optimizing functional outcomes, preventing secondary complications, and facilitating return to activity. Protocols must be individualized based on the fracture pattern, stability of fixation, presence of associated injuries, and patient comorbidities.
Early Post-Operative Period (Days 0-14)
- Pain Management: Implement a multimodal approach including opioids, NSAIDs (if not contraindicated for HO prophylaxis), gabapentinoids, and regional nerve blocks to minimize narcotic dependence and facilitate early mobilization.
- DVT Prophylaxis: Continue pharmacological (e.g., LMWH) and mechanical (e.g., sequential compression devices) prophylaxis until full mobilization is achieved.
-
Early Mobilization:
As soon as pain is controlled and hemodynamic stability is ensured.
- Bed Mobility: Log-rolling for posterior access, passive and active-assisted range of motion (ROM) of unaffected limbs.
- Out-of-Bed Mobilization: Initial focus on sitting upright, then standing with assistance.
-
Weight-Bearing (WB) Status:
This is the most crucial decision point and is dictated by the stability of the fracture and fixation.
- Non-Weight Bearing (NWB) / Touch-Down Weight Bearing (TDWB): For highly unstable fractures (VS, APC III, LC III) or where fixation is considered less robust, typically for 6-12 weeks. Use of crutches or a walker.
- Partial Weight Bearing (PWB): Often prescribed for moderately stable fractures (e.g., LC II with good posterior fixation) or as a progression from NWB, typically 25-50% body weight.
- Weight-Bearing as Tolerated (WBAT): For stable fractures (e.g., APC I, LC I, or well-fixed B-type fractures) and highly stable posterior fixation, usually initiated early.
-
Physical Therapy (PT):
- Initial Focus: Education on WB restrictions, bed mobility, transfers, upper extremity strengthening for assistive device use, gentle ROM for lower extremities (within pain limits, avoiding extremes of hip rotation/abduction if SI joint involved).
- Respiratory Therapy: Especially for polytrauma patients, to prevent pneumonia.
- Wound Care: Meticulous pin site care for external fixators to prevent infection. Regular inspection of surgical incisions.
Intermediate Phase (Weeks 2-12)
- Progression of Weight-Bearing: Gradual increase in WB status as pain allows and radiographic healing progresses, under the guidance of the surgeon and physical therapist. This is often based on follow-up radiographs and clinical assessment of tenderness and stability.
-
Advanced Physical Therapy:
- Strengthening: Core stability exercises, gluteal strengthening (abductors, extensors), quadriceps, and hamstring strengthening.
- Balance and Proprioception: Exercises to restore neuromuscular control.
- Gait Training: Progression from assistive devices to independent ambulation.
- Range of Motion: Continue to work on hip and lumbar spine ROM to prevent stiffness. Avoid aggressive stretching of hip flexors or external rotators if an anterior approach was used or if posterior stability is questionable.
- Radiographic Follow-up: AP pelvis, inlet, and outlet radiographs are typically performed at 2, 6, and 12 weeks post-operatively to assess fracture alignment, hardware integrity, and early signs of union. CT scans may be used for more detailed assessment if union is delayed or if complications are suspected.
Late Phase (Beyond 12 Weeks)
- Full Weight-Bearing & Return to Activity: Once radiographic union is confirmed and clinical symptoms allow, patients can progress to full weight-bearing and gradually return to pre-injury activities.
- Advanced Rehabilitation: Sport-specific training, high-impact activities (if appropriate), and vocational rehabilitation.
- Addressing Residual Pain/Dysfunction: Continue targeted physical therapy, pain management, or consider further interventions for chronic pain, malunion, or hardware irritation.
-
Hardware Removal:
- Indications: Symptomatic hardware (e.g., prominent screws, plates causing irritation), persistent pain, deep infection, or as a prophylactic measure in young, active individuals (e.g., symphyseal plates).
- Timing: Typically 12-24 months post-operatively, after solid union is confirmed. Not all hardware needs to be removed. Percutaneous iliosacral screws are often left in situ if asymptomatic.
Summary of Key Literature / Guidelines
The management of pelvic ring fractures has evolved significantly, guided by accumulating evidence and consensus recommendations. The ATLS protocol remains the cornerstone for initial assessment and resuscitation, while subsequent definitive management relies on established orthopedic trauma principles.
ATLS Guidelines and Initial Resuscitation
- American College of Surgeons Committee on Trauma (ACS-COT) ATLS Manual: Emphasizes a standardized, systematic approach to trauma patients, prioritizing life-threatening injuries. For pelvic fractures, early recognition of hemodynamic instability, application of a pelvic binder, and rapid transition to hemorrhage control measures (e.g., angiography/embolization, preperitoneal packing) are critical. The "C" in ABCDE (Circulation) includes controlling external hemorrhage and assessing for internal bleeding.
- Damage Control Orthopedics (DCO): A widely adopted strategy for polytrauma patients, particularly those with pelvic fractures. It involves initial temporary stabilization (e.g., external fixation, pelvic packing) to stabilize the patient physiologically, followed by definitive fixation once the patient is resuscitated and out of the "physiologic abyss." This approach has been shown to reduce morbidity and mortality in critically injured patients.
Classification Systems and Stability
- Young-Burgess Classification (1990): Mechanistically based (APC, LC, VS). Correlates well with injury severity and predicted instability, guiding management decisions. Widely used for initial assessment and communication.
- Tile Classification (1988): Based on the stability of the posterior pelvic ring (Type A: stable, Type B: rotationally unstable, Type C: rotationally and vertically unstable). Emphasizes the critical role of posterior ligamentous integrity in overall pelvic stability.
Hemorrhage Control Strategies
- Pelvic Binders/Sheets: Numerous studies support the efficacy of early external pelvic compression in reducing pelvic volume and tamponading venous hemorrhage, improving hemodynamic stability in unstable fractures.
- Angiography and Embolization: The role of angiography is well-established for controlling arterial hemorrhage. Meta-analyses demonstrate its effectiveness in reducing mortality in patients with arterial bleeding, often identified by a "blush" on CT angiography.
- Preperitoneal Pelvic Packing: Increasingly recognized as a rapid and effective method, particularly for venous bleeding, especially in centers without immediate access to angiography or when embolization fails. Studies support its use, often in conjunction with external fixation, as a part of damage control strategies.
- Combined Modalities: The optimal management of pelvic hemorrhage often involves a combination of external compression, external fixation, preperitoneal packing, and angiography/embolization, in a sequential or concurrent manner based on patient response and available resources.
Definitive Fixation Principles
- Early vs. Delayed Fixation: While damage control orthopedics permits delayed definitive fixation, studies suggest that definitive stabilization of the pelvic ring within the first few days (e.g., 24-72 hours) for mechanically unstable injuries, once the patient is physiologically stable, can lead to improved outcomes and reduced complication rates compared to prolonged external fixation.
-
Anterior vs. Posterior Fixation:
- Posterior Fixation: Widely recognized as paramount for restoring vertical and rotational stability. Percutaneous iliosacral screws, applied under fluoroscopic guidance, are the preferred method for many SI joint dislocations and sacral fractures due to their minimally invasive nature and high biomechanical stability. Open posterior approaches are reserved for complex fractures or neural decompression.
- Anterior Fixation: Essential for symphyseal diastasis and pubic rami fractures. Plating of the symphysis (single or dual) is the standard.
- Multidisciplinary Approach: Consensus guidelines emphasize the importance of a trauma team approach involving orthopedic surgeons, general surgeons, intensivists, interventional radiologists, and urologists to optimize patient care and outcomes.
Outcomes and Rehabilitation
- Long-term studies on pelvic fracture outcomes highlight the high incidence of chronic pain (particularly SI joint related), gait disturbance, sexual dysfunction, and neurological deficits, even after successful fixation.
- Aggressive, individualized rehabilitation protocols are crucial to mitigate these long-term morbidities.
- The principles of weight-bearing progression are based on the biomechanical stability of the final fixation construct, with careful radiographic follow-up.
In conclusion, the management of pelvic ring fractures necessitates a systematic, evidence-based approach rooted in ATLS principles, combined with a deep understanding of pelvic anatomy, biomechanics, and contemporary surgical techniques. Continuous refinement of protocols and multidisciplinary collaboration are essential to improve the outcomes for these critically injured patients.
