Patient Presentation & History
A 32-year-old male, semi-professional soccer player, presented to the emergency department following a high-energy rotational injury to his left ankle during a competitive match. He reported being tackled from behind while his foot was planted and externally rotated, resulting in an immediate onset of severe pain, inability to bear weight, and rapid swelling. He was unable to continue play and required assistance off the field.
His chief complaint was exquisite pain in the left ankle and foot, rated 9/10 on the Visual Analogue Scale. He denied any prior significant ankle injuries or surgeries. His past medical history was unremarkable, with no known allergies and no regular medications. He was a non-smoker and consumed alcohol socially. Given his athletic background, a prompt and effective return to high-level function was a primary consideration for management.
The mechanism described, a pronation-external rotation force, is highly suggestive of a syndesmotic injury, often accompanied by associated fractures. The energy of the injury implies a potential for significant soft tissue damage, necessitating careful evaluation for impending compartment syndrome or open wounds. The patient's age and activity level underscore the importance of anatomical reduction and stable fixation to optimize long-term outcomes and prevent chronic instability or post-traumatic arthritis.
Clinical Examination
Upon initial assessment in the emergency department, the patient was alert and oriented.
His left ankle presented with marked swelling encompassing the entire ankle joint, extending into the foot and distal leg. Significant ecchymosis was evident circumferentially around the ankle, particularly prominent on the lateral aspect. There was no obvious gross deformity or skin tenting, but palpable tension in the soft tissues suggested considerable oedema. Crucially, no open wounds or skin blisters were present at this initial evaluation.
Palpation:
* Exquisite tenderness was elicited along the anterior inferior tibiofibular ligament (AITFL) and posterior inferior tibiofibular ligament (PITFL) regions, consistent with syndesmotic involvement.
* Tenderness was also noted over the distal fibula and the medial malleolus.
* The entire length of the fibula was palpated to rule out a proximal fibular fracture (Maisonneuve injury), which was negative.
* The base of the fifth metatarsal and navicular bone were also carefully palpated to exclude midfoot injuries.
Range of Motion (ROM):
* Active and passive ankle dorsiflexion and plantarflexion were severely limited due to pain and swelling. Eversion and inversion were similarly restricted.
Special Tests for Syndesmotic Instability (performed gently due to acute pain):
*
Squeeze Test:
Compression of the tibia and fibula at the mid-calf elicited sharp pain distally at the syndesmosis, suggestive of interosseous membrane disruption.
*
External Rotation Stress Test:
With the patient's knee flexed to 90 degrees and the ankle in neutral dorsiflexion, gentle external rotation of the foot on a stabilized tibia reproduced severe pain over the distal tibiofibular joint. Frank instability was difficult to ascertain clinically due to guarding and soft tissue swelling, emphasizing the need for imaging.
*
Cotton Test:
Lateral translation of the talus within the mortise was attempted but limited by patient discomfort.
Neurological Assessment:
* Dorsalis pedis and posterior tibial pulses were palpable and strong bilaterally.
* Capillary refill was brisk (< 2 seconds) in all toes.
* Sensory examination revealed intact light touch sensation in the superficial and deep peroneal, saphenous, sural, and tibial nerve distributions.
* Motor function was difficult to fully assess due to pain but showed gross ability to dorsiflex and plantarflex, with some weakness in toe extension and ankle eversion.
Vascular Assessment:
* Pulses, capillary refill, and skin temperature were normal, with no signs of impending compartment syndrome. However, given the high-energy mechanism and rapidly developing swelling, compartment pressures would have been measured if clinical suspicion was higher.
Overall, the clinical picture strongly suggested an unstable ankle fracture with significant syndesmotic involvement, necessitating urgent diagnostic imaging and definitive management.
Imaging & Diagnostics
Immediate radiographic evaluation of the left ankle was performed.
Initial Radiographs (AP, Lateral, Mortise Views):
*
AP View:
Revealed a distal fibular fracture extending proximally approximately 5 cm from the tip of the lateral malleolus, consistent with a Weber C fracture. Importantly, a widening of the clear space between the medial malleolus and the talus was noted, suggesting a deltoid ligament injury or medial malleolus fracture.
*
Lateral View:
Showed mild posterior displacement of the talus relative to the tibia and no obvious posterior malleolus fracture, though detailed assessment was limited by overlapping structures and soft tissue swelling.
*
Mortise View (15 degrees internal rotation):
This view was critical for evaluating the syndesmosis. It demonstrated a clear widening of the tibiofibular clear space (TFCS) to 9 mm (normal < 6 mm) and a significant reduction in the tibiofibular overlap (TFO) to 0 mm (normal > 1 mm). There was also evidence of a displaced medial malleolus fracture.
Weight-Bearing Stress Radiographs: Due to the clear radiographic signs of instability and associated fractures, formal weight-bearing stress radiographs were not deemed necessary at this initial stage, as operative intervention was already indicated. However, intraoperative stress fluoroscopy would be performed.
Full-Length Tibia and Fibula Radiographs: These were obtained to definitively rule out a Maisonneuve fracture, which was confirmed negative.
Computed Tomography (CT) Scan:
A CT scan of the left ankle was ordered to further characterize the fibular fracture, assess the extent of the medial malleolus fracture, and meticulously evaluate the syndesmosis and for any subtle posterior malleolus involvement that might not be evident on plain films.
*
Findings:
* The CT confirmed the spiral oblique fracture of the distal fibula, extending approximately 5 cm proximal to the ankle joint line, consistent with a Weber C classification.
* A significant, comminuted, obliquely oriented fracture of the medial malleolus was present, involving the articular surface.
* The syndesmosis was clearly disrupted, with marked diastasis measuring up to 10 mm on axial cuts and loss of congruity between the fibula and the incisura fibularis of the tibia.
* A small, undisplaced posterior malleolus fragment (approximately 15% of the articular surface) was identified, deemed stable and not requiring primary fixation.
* No intra-articular loose bodies or significant chondral defects were observed acutely.
* 3D reconstructions were helpful for visualizing the overall fracture pattern and planning the reduction of the fibula relative to the tibia.
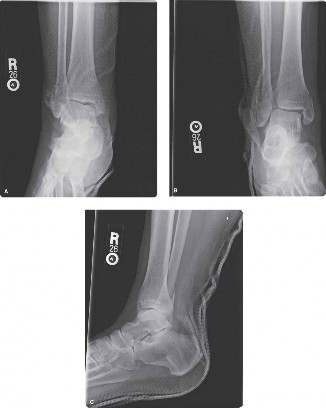
Figure 1: Illustration demonstrating key radiographic measurements for syndesmotic integrity. Note the Tibiofibular Clear Space (TFCS) and Tibiofibular Overlap (TFO) as assessed on the mortise view.
Magnetic Resonance Imaging (MRI) Scan:
Given the unequivocal findings on plain radiographs and CT, an MRI was not required pre-operatively. MRI is typically reserved for cases with ambiguous syndesmotic instability despite stress radiographs, or for evaluating chronic syndesmotic sprains, occult soft tissue injuries (e.g., deltoid ligament integrity in cases without medial malleolus fracture), or chondral pathology not well visualized on CT. In an acute, unstable fracture scenario with clear radiographic diastasis, the additional information from MRI rarely changes the immediate surgical plan.
Pre-operative Templating:
Based on the radiographs and CT, templating was performed.
* The fibular fracture dictated plate and screw choice (e.g., 1/3 tubular plate or specifically contoured fibular plate, 3.5 mm screws).
* The medial malleolus fracture indicated two parallel 3.5 mm cortical screws or tension band wiring.
* For syndesmotic fixation, the choice was narrowed to a 3.5 mm quad-cortical syndesmotic screw or a suture-button device. Given the patient's high demand for return to sport and the desire for dynamic stability, a suture-button system was favored for the syndesmosis. This decision would also influence the post-operative rehabilitation protocol, potentially allowing for earlier weight-bearing.
Differential Diagnosis
The comprehensive evaluation allowed for a precise diagnosis, distinguishing this complex injury from other potential ankle pathologies. The primary diagnosis was an unstable trimalleolar equivalent ankle fracture with syndesmotic disruption (Weber C fibular fracture, medial malleolus fracture, and posterior syndesmotic instability).
| Feature | Syndesmotic Injury (Unstable with Fracture) | High Ankle Sprain (Stable Syndesmotic Sprain) | Lateral Ankle Sprain (Grade III) | Maisonneuve Fracture |
|---|---|---|---|---|
| MOI | Pronation-ER, Supination-ER, high-energy axial load with rotation | Similar to unstable, but less severe force, often chronic microtrauma | Inversion, plantarflexion | Pronation-ER with axial load, often indirect fibular injury |
| Pain Location | Distal tibiofibular joint, medial malleolus, lateral malleolus, diffuse | Distal tibiofibular joint, anterior/posterior aspect | Anterolateral ankle (ATFL/CFL), swelling often localized | Proximal fibula (fibular head/neck), medial ankle, syndesmosis |
| Swelling/Ecchymosis | Significant, diffuse, rapid onset | Moderate, localized to syndesmosis, slower onset | Moderate to severe, localized to lateral ankle, rapid onset | Significant, often involving proximal leg and entire ankle, rapid |
| Tenderness | AITFL, PITFL, deltoid, fibula, medial malleolus | AITFL, PITFL, interosseous membrane | ATFL, CFL, sinus tarsi | Proximal fibula, medial ankle (deltoid), syndesmosis |
| Special Tests | Positive Squeeze, External Rotation Stress, Cotton (often too painful to assess fully) | Positive Squeeze, positive External Rotation Stress (mild to moderate), Cotton negative/equivocal | Anterior Drawer (positive), Talar Tilt (positive) | Positive Squeeze, External Rotation Stress (strong positive). Pain/tenderness at proximal fibula. |
| X-ray Findings | Widened TFCS (>6mm), decreased TFO (<1mm), fibular fracture (Weber B/C), medial malleolus fracture, +/- posterior malleolus fracture. Talar shift. | Normal TFCS/TFO on static views. Subtle widening on stress views. | Normal. No bony injury. | Proximal fibula fracture. Widened TFCS, decreased TFO. Talar shift. Often medial malleolus fracture or deltoid rupture. |
| CT Scan Findings | Confirms diastasis, fracture morphology, articular involvement. | Subtle disruption of syndesmotic ligaments (osseous avulsions). | Normal bony anatomy. | Confirms proximal fibular fracture, syndesmotic diastasis, associated medial injury. |
| MRI Scan Findings | Not always required acutely if X-ray/CT clear. Shows ligament tears (AITFL, PITFL, deltoid). | Direct visualization of ligamentous injury (AITFL, PITFL, interosseous membrane). | Clear visualization of ATFL, CFL, PTFL rupture. Edema. | Confirms ligamentous injury at syndesmosis and deltoid. |
| Stability | Grossly unstable, requiring operative stabilization | Stable or mildly unstable, can often be managed non-operatively | Mechanically unstable, but non-operative management often successful | Unstable, requiring operative stabilization |
| Management | Operative fixation of all components: fractures + syndesmosis | Non-operative (RICE, bracing, PT, gradual return to activity) | Non-operative (RICE, bracing, PT, proprioception) | Operative fixation of syndesmosis (and medial side if applicable). Proximal fibula often left alone. |
Surgical Decision Making & Classification
The patient's presentation, combined with the comprehensive imaging findings, left no ambiguity regarding the necessity for surgical intervention. The constellation of a Weber C fibular fracture, a displaced medial malleolus fracture, and confirmed syndesmotic diastasis constituted an unstable ankle injury. Non-operative management for such an injury would inevitably lead to chronic pain, instability, malunion, and premature post-traumatic arthritis due.
Indications for Operative Intervention in this Case:
1.
Unstable Fibular Fracture:
The Weber C fibular fracture is inherently unstable and requires ORIF for anatomical alignment and stability.
2.
Displaced Medial Malleolus Fracture:
Articular involvement and displacement mandate ORIF to restore joint congruity and prevent long-term arthrosis.
3.
Confirmed Syndesmotic Instability:
The widened tibiofibular clear space and absent tibiofibular overlap on radiographs and CT, coupled with a positive external rotation stress test clinically, indicated complete disruption of the syndesmotic ligaments, requiring formal fixation. Talar shift also confirmed instability.
4.
Patient's Activity Level:
As a semi-professional athlete, the goal was to restore maximal function and stability for a safe return to sport, which is best achieved through anatomical reduction and stable internal fixation.
Classification:
*
Lauge-Hansen Classification:
Based on the mechanism of injury (pronation-external rotation), the injury pattern was consistent with a
Pronation-External Rotation (PER) type IV
. This involves a medial malleolus fracture or deltoid rupture, an anterior inferior tibiofibular ligament avulsion or tear, a spiral or comminuted fibular fracture extending above the ankle joint, and finally, a posterior inferior tibiofibular ligament tear and disruption of the interosseous membrane, leading to syndesmotic diastasis.
*
AO/OTA Classification:
The fibular fracture was classified as a
44-C3
fracture, indicating a fracture of the fibula proximal to the syndesmosis with significant syndesmotic disruption and associated medial injury. The medial malleolus fracture would be a 44-A type.
Timing of Surgery:
Given the absence of open wounds, severe blistering, or signs of impending compartment syndrome, the surgery was scheduled within 48 hours to minimize soft tissue swelling and scar tissue formation, which can complicate reduction. Delaying beyond 7-10 days can significantly increase the difficulty of achieving anatomical reduction of the syndesmosis. The current soft tissue envelope was deemed amenable to immediate surgical intervention.
Surgical Technique / Intervention
The patient underwent Open Reduction Internal Fixation (ORIF) of the left ankle with syndesmotic stabilization.
1. Patient Positioning and Anesthesia:
* The patient was positioned supine on a radiolucent operating table.
* A bump was placed under the ipsilateral hip to internally rotate the leg, presenting the lateral aspect of the ankle for optimal access to the fibula.
* A tourniquet was applied to the thigh, and an inflatable foot pump was used for DVT prophylaxis on the contralateral limb.
* General anesthesia was administered, along with a regional popliteal nerve block for post-operative analgesia.
* The limb was prepped and draped in a sterile fashion from the knee to the toes.
2. Surgical Approaches:
*
Lateral Approach:
A standard curvilinear incision was made along the posterior border of the distal fibula, centered over the fibular fracture site. This provided direct access to the fibula and allowed visualization of the lateral ankle joint and syndesmosis.
*
Medial Approach:
A separate straight incision was made over the medial malleolus to address the medial malleolar fracture.
3. Fixation of the Fibular Fracture:
* The fibular fracture fragments were carefully exposed, cleared of hematoma, and anatomically reduced.
* Reduction was initially maintained with pointed reduction clamps.
* A 3.5 mm contoured stainless steel locking plate (e.g., LCP Fibula Plate) was applied to the lateral aspect of the fibula.
* Lag screws were inserted through the plate for interfragmentary compression where feasible, followed by cortical screws to secure the plate proximally and distally, restoring fibular length, rotation, and alignment.
* Intraoperative fluoroscopy (AP, lateral, mortise views) confirmed anatomical reduction of the fibula and restoration of the lateral clear space.
4. Fixation of the Medial Malleolus Fracture:
* Through the medial incision, the medial malleolus fracture was exposed.
* Hematoma was evacuated, and the fracture fragments were meticulously reduced.
* The fracture was stabilized with two 3.5 mm fully threaded cancellous screws oriented from the tip of the malleolus into the tibial metaphysis, providing stable compression and fixation. A small fragment clamp was used to maintain reduction during drilling and screw insertion.
* Fluoroscopy confirmed satisfactory reduction and appropriate screw placement.
5. Syndesmotic Reduction and Stabilization:
* This is the most critical step. With both malleolar fractures fixed, the syndesmosis was addressed.
* The ankle was positioned in 0-5 degrees of dorsiflexion to open the widest part of the talar dome within the mortise, thus preventing iatrogenic over-compression of the syndesmosis.
* A pointed reduction clamp (e.g., Verbrugge clamp or an anterior-to-posterior pointed reduction clamp) was applied percutaneously or through the lateral incision. One tip was placed on the medial fibular cortex just proximal to the joint line, and the other on the posterolateral tibial cortex. Gentle compression was applied to reduce the fibula into the incisura fibularis.
*
Intraoperative Fluoroscopy for Syndesmotic Reduction Assessment:
Crucial fluoroscopic views (AP, mortise, and lateral) were taken with the clamp in place to confirm accurate reduction. The key parameters were:
*
Mortise View:
Restoration of the tibiofibular clear space (<6mm) and tibiofibular overlap (>1mm).
*
Lateral View:
The fibula should be centered in the incisura without anterior or posterior translation.
*
Dynamic Stress Testing:
Once static reduction was confirmed, an external rotation stress test was performed under fluoroscopy with the reduction clamp removed. If any widening was noted, reduction was re-attempted.
*
Fixation with Suture-Button Device:
* After achieving anatomical and stable reduction, a double suture-button device (e.g., TightRope™) was chosen for dynamic stabilization.
* A targeting guide was used to drill a 3.7 mm hole through the lateral fibular plate (if applicable, otherwise directly through the fibula), then through the fibula, across the syndesmosis, and through the medial tibial cortex. The drill trajectory was approximately 2-3 cm proximal to the tibiofibular joint line, directed 25-30 degrees anteriorly from posterior-lateral to anterior-medial.
* The suture-button construct was passed through the drilled hole. The medial button was seated flush against the medial tibial cortex, and the lateral button against the lateral fibular cortex (or plate).
* The sutures were then tensioned gradually using a tensioning device to achieve appropriate stability without over-compression, confirmed by repeat fluoroscopic stress views. The ankle was cycled through a full range of motion while tensioning to ensure dynamic stability.
* A second suture-button device was placed approximately 1 cm proximal to the first, using the same technique, to provide additional rotational stability.
* The chosen fixation method was deliberately dynamic to allow physiological movement, reducing the need for hardware removal and potentially permitting earlier weight-bearing.
6. Wound Closure:
* Both incisions were irrigated thoroughly.
* Layered closure of the subcutaneous tissues and skin was performed.
* A sterile dressing and a posterior plaster splint were applied in a neutral position for initial immobilization and swelling control.
Post-Operative Protocol & Rehabilitation
The post-operative protocol was designed to protect the fixation, manage pain and swelling, and facilitate a progressive return to function, with considerations for the use of dynamic syndesmotic fixation.
Phase 1: Acute Protection (Weeks 0-2)
*
Immobilization:
Short-leg posterior plaster splint for the first few days, transitioned to a removable short-leg CAM (Controlled Ankle Motion) boot once swelling subsided and wound checked.
*
Weight-bearing:
Strictly Non-Weight Bearing (NWB) on the operative limb, using crutches or a knee scooter.
*
Pain & Swelling Management:
Elevation, ice, oral analgesics.
*
Wound Care:
Regular wound checks, dressing changes. Prophylactic antibiotics for 24-48 hours.
*
Early Mobilization:
Gentle active range of motion (AROM) of toes. No active or passive ankle ROM permitted in the first 2 weeks to protect the soft tissue healing.
Phase 2: Early Mobilization & Gradual Loading (Weeks 2-6)
*
Weight-bearing:
*
Suture-Button:
Progressive weight-bearing (PWB) initiated at week 2-3, gradually increasing to Full Weight Bearing (FWB) by week 6 in the CAM boot, as tolerated. The dynamic nature of the suture-button allows for earlier, controlled loading.
*
Syndesmotic Screws (if used):
NWB typically maintained for 6 weeks, then PWB to FWB in the boot.
*
Rehabilitation:
* Begin gentle AROM exercises for the ankle (dorsiflexion, plantarflexion, inversion, eversion) within a pain-free range, initially without resistance.
* Soft tissue mobilization to address scar tissue around the incisions.
* Stationary bike with light resistance (seated, no standing).
* Core and hip strengthening exercises to maintain overall fitness.
Phase 3: Strengthening & Proprioception (Weeks 6-12)
*
Weight-bearing:
Wean out of CAM boot and transition to supportive lace-up ankle brace (e.g., ASO) as pain allows, typically by week 8. FWB without restrictions.
*
Rehabilitation:
* Progressive strengthening: Calf raises (bilateral to unilateral), resistance band exercises (all planes), eccentric calf work.
* Proprioception and balance training: Single-leg stance, wobble board, unstable surfaces.
* Gait training to normalize walking pattern.
* Swimming and elliptical trainer for cardiovascular fitness.
Phase 4: Return to Activity/Sport (Weeks 12-6 months+)
*
Advanced Strengthening & Agility:
* Plyometric exercises, sport-specific drills (e.g., cutting, jumping, sprinting progression).
* Gradual return to running program.
* Agility ladder drills.
* Continue ankle strengthening and proprioceptive exercises.
*
Return to Sport:
* A stepwise, monitored return to sport program, typically not before 4-6 months, contingent on achieving full strength, range of motion, and confidence, and passing functional testing.
* The ankle may be protected with taping or a brace for several months upon return to sport.
*
Hardware Management (Syndesmotic Screws vs. Suture-Button):
*
Suture-Button:
Generally left in situ unless symptomatic (rare).
*
Syndesmotic Screws:
If screws were used, removal is typically considered at 8-12 weeks post-op, especially for active individuals or athletes, to prevent screw breakage and allow for physiological tibiofibular motion. For less active, asymptomatic patients, they may be left in.
Throughout all phases, close monitoring for complications such as infection, wound dehiscence, nerve injury, hardware irritation, and especially malunion or ongoing instability, is paramount. Regular clinical and radiographic follow-up is essential.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- High Index of Suspicion: Always suspect syndesmotic injury in any rotational ankle trauma, even if initial radiographs appear benign. A subtle increase in TFCS or decrease in TFO is significant.
- Stress Radiographs are Indispensable: If static radiographs are equivocal, obtain gravity stress views or, if necessary, fluoroscopic stress views under anesthesia to confirm instability. Never operate on an equivocal syndesmosis without confirming instability.
- Maisonneuve Rule-out: Always palpate the entire fibula and obtain full-length tibia-fibula radiographs to rule out a Maisonneuve fracture in any syndesmotic injury.
- Anatomic Reduction of the Fibula: This is the absolute cornerstone of successful syndesmotic fixation. The fibula must be reduced into its incisura, restoring its length, rotation, and translation. Fibular malreduction is the most common cause of poor long-term outcomes.
- Ankle Position During Fixation: Fix the syndesmosis in 0-5 degrees of dorsiflexion. This ensures the widest part of the talus is within the mortise, preventing iatrogenic over-compression and loss of motion post-operatively.
- Direct Visualization (If Possible): If an associated lateral malleolus fracture exposes the syndesmosis, use direct visualization to confirm fibular reduction into the incisura. Palpation of the anterior syndesmotic ligaments after reduction can confirm congruity.
- Syndesmotic Screw Trajectory: Typically 2-3 cm proximal to the joint line, angled 25-30 degrees anteriorly from posterior-lateral to anterior-medial, ensuring adequate purchase through all cortices (quad-cortical).
- Dynamic Fixation: Consider suture-button devices for athletes or patients requiring earlier return to function, as they allow physiological micromotion at the syndesmosis, potentially reducing reoperation for hardware removal.
- Posterior Malleolus: A significant posterior malleolus fracture (typically >25-30% of the articular surface or with gross posterior talar subluxation) should be fixed as it can contribute to syndesmotic instability and make fibular reduction difficult. It also represents a critical component of the "posterior wall" of the incisura.
Pitfalls
- Missed Diagnosis: Failure to diagnose and treat an unstable syndesmosis leads to chronic pain, instability, reduced athletic performance, and accelerated post-traumatic arthritis.
- Inadequate Reduction (Malreduction): This is the single most important pitfall. Persistent tibiofibular clear space widening, reduced overlap, or malrotation of the fibula will result in poor outcomes. Intraoperative fluoroscopy (AP, mortise, lateral views) with and without stress should confirm reduction.
- Over-compression: Over-tightening syndesmotic screws or fixing the ankle in plantarflexion can lead to a rigid syndesmosis, impingement, pain, loss of dorsiflexion, and premature arthritis.
- Hardware Failure/Breakage: Syndesmotic screws are subject to cyclic loading and can break, especially if left in active patients. This often necessitates hardware removal, but if asymptomatic, can be observed. Suture-button devices have a lower reported failure rate but are not immune.
- Nerve Injury: The superficial peroneal nerve (lateral incision) and saphenous nerve (medial incision) are at risk during approach and retraction. Careful dissection is crucial.
- Compartment Syndrome: High-energy ankle injuries carry a risk. Vigilant post-operative monitoring for increasing pain disproportionate to injury, tenseness of compartments, and paresthesias is vital.
- Wound Complications: Significant swelling and fracture blisters can delay surgery, and infection remains a concern with any open procedure.
- Leaving Screws In (when inappropriate): While leaving screws in can be acceptable for some, for active individuals, particularly athletes, routine removal of syndesmotic screws at 8-12 weeks is often recommended to allow physiological motion and prevent breakage.
- Poor Surgical Technique for Suture-Button: Incorrect drill trajectory, inadequate seating of buttons, or improper tensioning can lead to failure of the construct or persistent instability.
