Patient Presentation & History
A 45-year-old male presented to the Emergency Department following a high-energy motor vehicle collision. He was an unrestrained driver involved in a frontal impact at highway speeds, resulting in significant lower extremity trauma. Specifically, his right lower leg bore the brunt of the impact, consistent with an axial loading mechanism to the ankle plafond.
Past medical history was significant for well-controlled Type 2 Diabetes Mellitus managed with oral hypoglycemics, and a 20-pack-year smoking history, with cessation 5 years prior. He had no prior history of lower extremity trauma or surgical intervention. Socially, he was employed as a construction worker, indicating a physically demanding occupation.
Upon initial assessment, the patient reported excruciating pain in his right ankle, rendering him unable to bear weight. He endorsed rapid swelling and a sensation of deformity. No other immediately life-threatening injuries were identified during the primary survey, and his hemodynamic status was stable.
Clinical Examination
Initial clinical examination revealed a severely swollen, tense, and ecchymotic right ankle. Gross deformity of the distal tibia and ankle joint was evident.
-
Inspection:
- Significant edema extending from the mid-tibia distally to the foot, with palpable tenseness.
- Blistering noted over the anterior and medial aspects of the ankle, indicative of severe soft tissue injury and impending skin necrosis due to swelling. Tscherne and Oestern grade II-III closed soft tissue injury was suspected.
- No open wounds were present, classifying it as a closed fracture.
- The skin appeared blanched in areas of maximal swelling, raising concern for compartment syndrome.
-
Palpation:
- Extreme tenderness localized to the distal tibia and ankle joint.
- Gross crepitus was elicited with minimal manipulation.
- Compartments of the lower leg were tense, particularly the anterior and deep posterior compartments.
- Distal pulses: Dorsalis pedis and posterior tibial pulses were diminished but palpable bilaterally. Capillary refill was sluggish in the injured foot (approximately 3-4 seconds), but eventually present.
-
Range of Motion (ROM):
- Grossly limited due to pain and swelling. Active and passive ankle ROM was severely restricted.
-
Neurological Assessment:
- Motor function: Gross assessment revealed intact plantarflexion and dorsiflexion, though severely limited by pain. Toe flexion and extension were grossly intact.
- Sensation: Intact light touch sensation in the distribution of the superficial and deep peroneal nerves, and the tibial nerve. No clear neurological deficit was identified, but the patient's pain level made a precise assessment challenging.
Given the clinical picture of severe swelling, deformity, and diminished pulses, urgent imaging and further assessment for potential compartment syndrome were initiated.
Imaging & Diagnostics
Immediate radiographic assessment of the right ankle and tibia/fibula was performed.
-
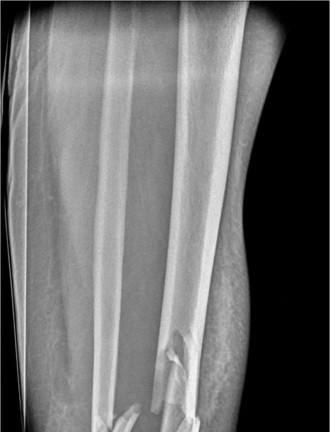
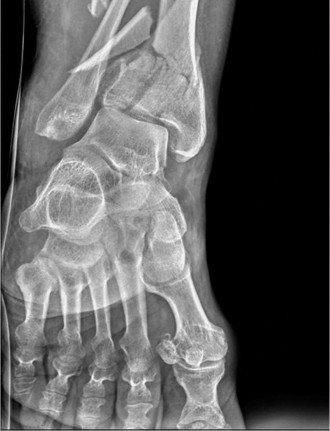
Initial X-rays (AP, lateral, mortise views):
- Demonstrated a highly comminuted, displaced intra-articular fracture of the distal tibia (pilon fracture).
- The articular surface of the tibial plafond was severely disrupted and impacted.
- Significant metaphyseal comminution was present, with shortening of the tibia.
- A comminuted fracture of the distal fibula was also noted, contributing to the instability and loss of ankle mortise integrity.
- The talus appeared displaced proximally, consistent with the axial loading mechanism.
- No obvious syndesmotic widening was initially appreciated, but full assessment would require CT.
-
Computed Tomography (CT) Scan:
- An urgent CT scan of the ankle (with 3D reconstructions) was performed to fully delineate the fracture pattern, assess articular involvement, and aid in pre-operative planning.
-
Findings:
- Confirmed a highly comminuted Type C3 pilon fracture according to the AO/OTA classification, involving significant articular fragmentation and metaphyseal comminution.
- Four main articular fragments were identified: anteromedial, anterolateral, posteromedial, and a large posterolateral fragment comprising approximately 30% of the articular surface.
- Significant central impaction of the articular plafond was present, with a large metaphyseal void inferior to the reconstructed plafond.
- The distal fibula fracture was multi-fragmentary, with shortening and rotation.
- The syndesmosis appeared stable, however, subtle widening was observed on stress views, necessitating intra-operative assessment.
- No evidence of talar osteochondral injury was noted acutely.
- The CT scan was crucial for fragment mapping, determining surgical approach strategies, and templating appropriate fixation. Specifically, the presence of a large posterolateral fragment suggested the need for a posterolateral or combined approach.
-
Magnetic Resonance Imaging (MRI):
- Not indicated in the acute setting for primary fracture assessment due to the dominance of bony injury and need for immediate surgical intervention. MRI would be considered for assessing significant ligamentous injury (e.g., deltoid), occult osteochondral lesions, or avascular necrosis of the talus if complications arose later.
-
Templating:
- Based on the CT images, pre-operative templating was performed to estimate implant sizes and types. This included selecting appropriate spanning external fixators for initial stabilization and considering locking plates (e.g., pre-contoured pilon plates) for definitive fixation, along with various lag screws and potentially bone graft substitutes for metaphyseal defects.
Differential Diagnosis
While the imaging clearly identified a pilon fracture, it's important to consider other diagnoses in the initial assessment of ankle and distal leg trauma, especially before definitive imaging. A detailed differential diagnosis helps ensure no concurrent injuries are missed.
| Condition | Key Features (Clinical) | Key Features (Imaging) | Distinguishing Factors (from Pilon Fracture) |
|---|---|---|---|
| Pilon Fracture (AO/OTA 43-C) | Severe pain, gross deformity, rapid swelling, often high-energy mechanism, tense skin. | Comminuted intra-articular distal tibia fracture, metaphyseal comminution, talar impaction, fibular fracture common. | Direct impact/axial load to plafond, intra-articular extension is defining feature. |
| Trimalleolar Ankle Fracture | Pain, swelling, deformity. Often inversion/eversion mechanism. Less severe soft tissue swelling typically. | Fractures of medial malleolus, lateral malleolus (fibula), and posterior malleolus. Less or no articular plafond comminution/impaction. | Articular surface of tibial plafond often intact or minimally involved. Mechanism often rotational. |
| Talar Neck Fracture | Pain in ankle/hindfoot, inability to bear weight. May have associated ankle or subtalar dislocation. | Fracture line through talar neck, usually sagittal. May have associated body or head fractures. | Fracture is primarily of the talus, not the distal tibia. Often associated with dorsiflexion injury. |
| Calcaneal Fracture | Hindfoot pain, heel widening, inability to bear weight. Mechanism often fall from height. | Fracture of the calcaneus, often involving the subtalar joint. May have decreased Böhler's angle. | Pain is localized to the heel. Ankle joint (tibiotalar) often intact, though may have associated injuries. |
| High Ankle Sprain / Syndesmotic Disruption | Pain above ankle, swelling. Instability with external rotation stress. | Widening of tibiofibular clear space, increased tibiofibular overlap on mortise view. No obvious fracture or subtle avulsion. | Absence of significant bony fracture. Ligamentous injury is primary. Pain is often proximal to the ankle joint. |
Surgical Decision Making & Classification
Given the patient's presentation with a high-energy, severely comminuted and displaced intra-articular pilon fracture (AO/OTA 43-C3) and significant soft tissue compromise (Tscherne Grade II-III with blistering), a staged management approach was unequivocally indicated.
Why operative vs non-operative?
Non-operative management for such a complex, displaced, and intra-articular pilon fracture is associated with predictably poor outcomes, including severe post-traumatic arthritis, malunion, limb shortening, and chronic pain. The goals of operative management are:
1. Anatomical reduction of the articular surface.
2. Restoration of overall limb length and alignment.
3. Stable fixation to allow early range of motion.
4. Preservation of the soft tissue envelope.
Staged Management Rationale:
The critical factor dictating surgical timing and approach for pilon fractures, particularly those with high-energy mechanisms, is the condition of the surrounding soft tissue envelope. Direct, immediate definitive open reduction and internal fixation (ORIF) in the presence of severe swelling and skin compromise (e.g., tension blisters, "wrinkle sign" absent) carries an unacceptably high risk of catastrophic wound complications, including wound dehiscence, deep infection, and soft tissue necrosis, which can jeopardize limb salvage.
Classification:
*
Rüedi and Allgöwer Classification:
This patient's fracture would be classified as a
Type III
(severe comminution with impaction and displacement of the articular surface), indicating a poor prognosis without meticulous surgical reconstruction.
*
AO/OTA Classification:
The most comprehensive classification, this fracture was clearly a
43-C3
, denoting a complete articular fracture of the distal tibia with both articular and metaphyseal comminution, consistent with the high-energy mechanism. This classification directly guided surgical planning, emphasizing the need for anatomical articular reconstruction and robust metaphyseal support.
*
Gustilo-Anderson Classification:
The fracture was
closed
, thankfully, but the severity of the soft tissue injury was significant, warranting careful consideration.
*
Tscherne and Oestern Classification:
Clinically, the ankle presented as a Tscherne Grade II-III, with significant swelling, blistering, and the absence of a "wrinkle sign" over the skin. This dictated the necessity of delayed definitive fixation.
Decision for Staged Management:
Based on these factors, the decision was made for staged management:
1.
Stage 1 (Emergency):
Urgent application of a spanning external fixator to restore length, provide temporary stability, decompress the soft tissues, and allow the soft tissue envelope to recover. Fibular fixation was considered in this stage as a crucial step for achieving length.
2.
Interval Period:
Close monitoring of the soft tissue condition, elevation, pain management, and medical optimization (e.g., glycemic control).
3.
Stage 2 (Delayed Definitive):
Once the "wrinkle sign" returned, blisters had resolved, and the soft tissue envelope was deemed quiescent (typically 7-14 days post-injury), definitive open reduction and internal fixation (ORIF) would be performed.
Surgical Technique / Intervention
Stage 1: Temporary External Fixation & Fibular Fixation
Goal: Restore length, realign gross deformity, provide stability, protect soft tissues, and facilitate soft tissue recovery.
- Patient Positioning & Anesthesia: Supine on a radiolucent table. General anesthesia.
-
Approach:
- Initially, percutaneous pins for the external fixator.
- A small incision over the distal fibula for direct reduction and plating.
-
Procedure:
- Fibular Fixation (Crucial First Step): The fibula was anatomically reduced and fixed with a 1/3 tubular plate and screws via a posterolateral approach. Restoring fibular length, rotation, and alignment is paramount as it serves as a "template" for tibial reduction, restoring the overall width and rotation of the ankle mortise. This was performed carefully to avoid excessive soft tissue stripping.
-
Spanning External Fixator Application:
- Proximal pins: Two Schanz pins (5mm) were inserted into the subcutaneous border of the tibia, approximately 10-15 cm proximal to the fracture site, ensuring they were well away from the planned definitive fixation zones.
- Distal pins: Two Schanz pins (5mm) were inserted into the calcaneus, avoiding the subtalar joint and neurovascular structures. Alternatively, a combination of calcaneal and first metatarsal pins can be used for stronger distraction and control.
- A modular external fixator frame was constructed, connecting the proximal and distal pins.
- Distraction and Ligamentotaxis: The frame was gradually distracted to restore appropriate length to the tibia, indirectly reducing the pilon fracture fragments via ligamentotaxis. This helped to de-impact the articular surface and create space for future definitive reduction. The tension on the soft tissues was significantly reduced.
- Fluoroscopy was used to confirm adequate distraction, restoration of length, and general alignment in AP and lateral views.
Interval Management
The patient was admitted, limb elevated, and managed with aggressive pain control, DVT prophylaxis, and careful wound care for the blisters. The external fixator provided stability, allowing the soft tissue swelling to resolve. Daily assessment of the skin condition, particularly the "wrinkle sign" (the reappearance of skin folds around the ankle when gently squeezed), was crucial. This phase lasted 10 days until the soft tissue envelope was deemed optimal for definitive surgery.
Stage 2: Definitive Open Reduction and Internal Fixation (ORIF)
Goal: Achieve anatomical reduction of the articular surface, restore mechanical axis, provide stable fixation, and allow for early mobilization.
- Timing: 10 days post-injury, "wrinkle sign" positive, blisters epithelialized, minimal edema.
- Patient Positioning & Anesthesia: Supine on a radiolucent table with a bolster under the ipsilateral hip for internal rotation. A small bump under the knee for slight flexion. The external fixator was left in place until surgical prep and draping were complete, then carefully removed to maintain stability until definitive plating. Fluoroscopy unit was positioned for AP, lateral, and mortise views.
-
Surgical Approaches: Given the extensive comminution and the large posterolateral fragment, a dual approach was selected:
- Anteromedial approach: For direct visualization and reduction of the medial and anteromedial plafond fragments.
- Posterolateral approach (modified extensile): To address the posterolateral fragment and facilitate access to the fibula (if needed for further adjustment) and posterior tibial metaphysis.
-
Procedure Details:
-
Articular Surface Reconstruction (Anteromedial Approach):
- A longitudinal incision was made over the anteromedial aspect of the distal tibia, extending proximal to the fracture and distally to the ankle joint.
- The skin and subcutaneous tissues were carefully reflected, protecting the saphenous nerve and vein.
- The fracture hematoma was evacuated.
- The primary focus was the articular surface. The fragments were meticulously identified.
-
Reduction Techniques:
- Using small pointed reduction clamps, K-wires as joysticks, and dental picks, the articular fragments were anatomically reduced under direct visualization.
- Particular attention was paid to restoring the congruence of the articular surface with the talus.
- Temporary fixation was achieved with multiple 1.5mm or 2.0mm K-wires.
- Fluoroscopy was used frequently to confirm reduction in all planes, especially ruling out residual joint step-off or gap.
- Impaction: The central impaction of the articular surface was elevated using blunt elevators (e.g., Freer elevator, bone tamp). The resulting metaphyseal void was filled with structural allograft (cancellous bone chips) to provide subchondral support and prevent collapse.
-
Metaphyseal Reconstruction & Plate Application (Anteromedial):
- Once the articular surface was reduced and temporarily stabilized, a pre-contoured anteromedial locking plate (e.g., specifically designed pilon plate) was selected.
- The plate was meticulously positioned to buttress the articular fragments and span the metaphyseal comminution, ensuring screws were directed into the most substantial bone fragments and subchondral bone, avoiding the joint space.
- Lag screws were used where appropriate to compress articular fragments prior to plate application, if possible.
- Proximal screws were placed to ensure solid purchase in the tibial diaphysis.
- The plate was carefully contoured to match the anatomy and provide adequate stability.
-
Posterolateral Approach & Fragment Fixation:
- A separate posterolateral incision was made, typically between the peroneus brevis and tertius tendons, avoiding the sural nerve.
- The large posterolateral fragment, which was not adequately visualized or reduced via the anteromedial approach, was directly accessed.
- This fragment was reduced under direct visualization using reduction clamps and K-wires.
- Fixation was achieved with lag screws placed anteriorly-to-posteriorly or with a small fragment plate (e.g., 1/3 tubular or small locking plate) applied to the posterior aspect, if space allowed and soft tissues permitted. In this case, due to the size and critical role of the fragment, a small locking plate was utilized for robust fixation.
-
Syndesmotic Assessment and Fixation:
- After definitive plating of the tibia and fibula, the stability of the distal tibiofibular syndesmosis was reassessed.
- With the foot in dorsiflexion, an external rotation stress test and a "hook test" (using a bone hook on the fibula) were performed under fluoroscopy.
- Minor instability was noted, warranting a single 3.5mm cortical syndesmotic screw placed through four cortices, approximately 2-3 cm proximal to the ankle joint. The screw was placed in a neutral position to maintain reduction.
-
Final Checks:
-
Final fluoroscopic images (AP, lateral, mortise) were obtained to confirm:
- Anatomical articular reduction (no step-off >1mm).
- Appropriate plate and screw position (no intra-articular hardware).
- Restoration of limb length and alignment.
- Adequate syndesmotic reduction.
- The ankle joint was gently taken through a full range of motion to ensure no impingement and stability.
-
Final fluoroscopic images (AP, lateral, mortise) were obtained to confirm:
-
Wound Closure:
- Meticulous, layered closure of both incisions was performed, paying close attention to avoiding tension.
- Skin staples or non-absorbable sutures were used for the skin.
- Sterile dressing applied.
-

Post-Operative Protocol & Rehabilitation
The post-operative management focused on protecting the meticulous surgical reconstruction, promoting soft tissue healing, and gradually restoring function.
-
Immediate Post-Operative Period (Day 0-14):
- Immobilization: The limb was placed in a well-padded splint (posterior or sugar-tong) in a neutral position.
- Elevation: Strict elevation of the limb above heart level was maintained to minimize swelling.
- Pain Management: Multimodal analgesia including opioids, NSAIDs (if no contraindications), and gabapentinoids.
- Wound Care: Daily dressing changes were performed, monitoring for signs of infection, dehiscence, or skin necrosis. Staples/sutures were typically removed at 2 weeks.
- Weight-Bearing: Strictly non-weight bearing (NWB) on the operative limb.
- DVT Prophylaxis: Chemical prophylaxis (e.g., LMWH) was initiated and continued for 4-6 weeks.
-
Early Rehabilitation (Week 2-8):
- Immobilization: Transition to a removable walking boot (CAM walker) or hinged ankle-foot orthosis (AFO).
- Range of Motion (ROM): Gentle, active and passive range of motion exercises for the ankle and subtalar joint were initiated, limited by pain and soft tissue healing. This typically involved dorsiflexion and plantarflexion, inversion, and eversion, avoiding aggressive stretches.
- Weight-Bearing: Remained NWB . Emphasis on maintaining quadriceps strength, hip, and knee ROM.
- Physical Therapy: Focus on scar management, edema control, and maintaining mobility of unaffected joints. Gentle ankle ROM within the boot's range.
-
Intermediate Rehabilitation (Week 8-12):
- Imaging: Repeat radiographs (AP, lateral, mortise) were obtained to assess fracture healing.
- Weight-Bearing: If radiographs showed early signs of healing and no loss of reduction, gradual progression to partial weight-bearing (PWB) was initiated. This began with toe-touch weight-bearing with crutches/walker, gradually increasing the load as tolerated and guided by pain and radiographic progression.
- Physical Therapy: Intensified. Focus on improving ankle and subtalar joint ROM, initiating strengthening exercises (isometric, then isotonic with resistance bands), balance and proprioception training. Gait training with assistive devices.
-
Advanced Rehabilitation (Week 12+):
- Weight-Bearing: Progression to full weight-bearing (FWB) as tolerated, typically without assistive devices, once radiographic union was evident.
- Physical Therapy: Advanced strengthening of all lower extremity muscle groups, plyometrics, agility drills, and sport-specific training as appropriate for the patient's functional goals.
- Return to Work/Activity: Phased return to activities. For a construction worker, a full return to pre-injury function might take 9-12 months or longer, and often involves job modification.
- Hardware Removal: Syndesmotic screw removal (if present) typically at 3-6 months. Plate removal is often considered if symptomatic (pain, irritation), usually no sooner than 12-18 months post-operatively.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Soft Tissue Envelope Dictates Timing: The condition of the soft tissues is paramount. Never rush definitive fixation into a compromised soft tissue envelope (e.g., severe swelling, extensive blistering, absence of "wrinkle sign"). Staged management is the gold standard for high-energy pilon fractures.
- Fibular Reconstruction First: Always restore fibular length, rotation, and alignment first. The fibula acts as a "lateral template" for reduction of the tibial plafond, restoring the overall width and rotation of the ankle mortise. This can be performed during the initial external fixator stage if soft tissues permit.
- Anatomical Articular Reduction: This is the most critical step. A step-off or gap greater than 1mm on the articular surface significantly increases the risk of post-traumatic arthritis. Use direct visualization, small fragments as reduction keys, K-wires as joysticks, and confirm with intra-operative fluoroscopy.
- Metaphyseal Void Management: After elevating impacted articular fragments, the underlying metaphyseal void must be filled. Autogenous bone graft (iliac crest) is ideal, but allograft or bone graft substitutes can be used to provide structural support and prevent late collapse.
- Indirect Reduction and Ligamentotaxis: Utilize external fixators or femoral distractors to restore length and de-impact the articular fragments, which can indirectly aid in reduction and protect the soft tissues by relieving tension.
- Judicious Surgical Approaches: No single approach fits all pilon fractures. Be prepared for dual approaches (e.g., anteromedial and posterolateral) for complex fracture patterns, especially those with large posterior or posterolateral fragments. Always identify and protect neurovascular structures.
- Stable Fixation: Employ modern locking plate technology and anatomical pre-contoured plates to buttress articular fragments and provide angular stability in comminuted metaphyses. Lag screws are essential for interfragmentary compression of articular pieces.
- Syndesmotic Assessment: Always assess the syndesmosis after definitive plating of both the tibia and fibula. Perform external rotation stress tests and hook tests under fluoroscopy. Fixation (typically with one cortical screw) is necessary if instability is present.
- Early Motion: Once stable fixation is achieved and soft tissues permit, early, gentle, protected range of motion can help mitigate stiffness and improve functional outcomes.
Pitfalls
- Rushing Definitive Fixation: Performing ORIF too early in the setting of severe soft tissue swelling and blistering is a recipe for disaster, leading to wound dehiscence, infection, and potential limb loss.
- Inadequate Articular Reduction: Failure to achieve an anatomical reduction of the articular surface will almost inevitably lead to painful post-traumatic arthritis, requiring future arthrodesis or arthroplasty.
- Ignoring Fibular Fracture: Not adequately addressing the fibular fracture (length, rotation) will compromise the overall ankle mortise reduction and stability, making tibial reduction challenging and impacting long-term ankle mechanics.
- Inadequate Metaphyseal Support: If metaphyseal voids are left unaddressed or fixation is unstable, late collapse of the articular surface can occur, leading to malunion and post-traumatic arthritis.
- Over-Stripping Soft Tissues: Extensive soft tissue dissection, especially in compromised envelopes, can lead to devascularization, wound complications, and non-union. Utilize indirect reduction techniques and minimally invasive approaches when possible.
- Failure to Address Posterior Malleolar Fragments: Large posterior fragments (often posterolateral) can be critical to ankle stability and congruity. If unaddressed, they can lead to posterior subluxation of the talus and chronic pain.
- Premature Weight-Bearing: Applying weight to an ununited pilon fracture can cause loss of reduction, collapse, and implant failure. Strict non-weight bearing for the appropriate duration (typically 8-12 weeks) is crucial.
- Neurovascular Injury: Aggressive dissection or pin placement without careful consideration of neurovascular anatomy can lead to iatrogenic nerve or vessel damage.
- Post-Operative Compartment Syndrome: Though less common after external fixation, it can still occur. Vigilance for signs and symptoms is necessary.
Clinical & Radiographic Imaging