A Distal Femur Case: Mastering Fracture Evaluation
Patient Presentation & History
A 72-year-old female presented to the emergency department following a ground-level fall at home. She reported tripping over a rug and landing directly on her right knee. She immediately experienced severe pain, deformity, and an inability to bear weight on the affected limb.
Her past medical history included:
* Osteoporosis, diagnosed 10 years prior, managed with oral alendronate.
* Hypertension, well-controlled with a diuretic.
* Type 2 Diabetes Mellitus, managed with metformin, HbA1c 7.1%.
* History of smoking (1 pack-year for 20 years, quit 5 years ago).
* No prior surgeries to the affected limb.
The patient lives independently, is ambulating without aids prior to the fall, and reports a good functional status. Her social history reveals no current alcohol or illicit drug use. The mechanism of injury, a low-energy fall in an osteoporotic patient, is highly suggestive of a fragility fracture. Immediate onset of severe pain and deformity pointed towards a significant skeletal injury rather than a soft tissue contusion or sprain. Initial assessment in the emergency department noted an isolated injury to the right lower extremity, with no signs of head trauma, chest trauma, or abdominal trauma, thus fulfilling ATLS primary survey parameters.
Clinical Examination
Upon initial assessment, the patient was hemodynamically stable and alert.
Local Examination of the Right Lower Extremity:
*
Inspection:
The right thigh presented with significant swelling, ecchymosis extending from the mid-thigh to the knee joint. A noticeable varus deformity was appreciated at the distal femur, accompanied by apparent shortening of the limb. No open wounds, skin tenting, or signs of impending compartment syndrome were observed. The skin overlying the knee appeared intact, though distended by effusion.
*
Palpation:
Diffuse tenderness was elicited across the distal femur, particularly over the supracondylar and intercondylar regions. Gross crepitus was palpable with gentle manipulation, confirming skeletal disruption. The knee joint itself was tense and exquisitely tender to palpation, indicating a hemarthrosis. Distal pulses (dorsalis pedis and posterior tibial) were present and strong bilaterally. Capillary refill in the toes was brisk (<2 seconds).
*
Range of Motion (ROM):
Active range of motion of the right knee was not possible due to pain. Passive range of motion was severely restricted and painful, estimated to be from 0 to 15 degrees of flexion. The hip joint demonstrated pain-free, full range of motion, suggesting no associated proximal femoral or acetabular injury.
*
Neurological Assessment:
Sensation was intact to light touch in all dermatomes of the foot (L4, L5, S1, S2). Motor function of the ankle and toes was preserved; the patient was able to actively dorsiflex and plantarflex her ankle, and wiggle her toes against resistance. Specifically, the common fibular nerve (peroneal nerve) function was intact, with no foot drop or sensory deficit in the first web space. Tibial nerve function was also intact.
*
Associated Injuries:
A thorough examination of the ipsilateral hip, ankle, and foot revealed no additional deformities or focal tenderness. The contralateral limb was unremarkable. Given the isolated nature of the injury and low-energy mechanism, extensive screening for polytrauma was not indicated beyond the primary survey.
The clinical presentation, characterized by severe pain, gross deformity, and crepitus, strongly indicated an unstable fracture of the distal femur. The preserved neurovascular status was a positive prognostic sign, however, ongoing monitoring for compartment syndrome or secondary vascular compromise remained crucial.
Imaging & Diagnostics
Initial Radiographs:
Standard anteroposterior (AP) and lateral radiographs of the right femur, including the knee joint, were obtained upon presentation. Additionally, a full-length AP and lateral view of the entire femur was performed to rule out any skip lesions or pre-existing hardware. AP and lateral views of the ipsilateral hip and ankle were also obtained as part of a routine trauma series for lower extremity injuries to exclude concurrent injuries.
Findings:
*
AP View:
Demonstrated a comminuted, intra-articular fracture involving both the medial and lateral femoral condyles. There was significant varus angulation and shortening. A large metaphyseal component was evident, with extension proximally into the femoral shaft. Articular incongruity, marked by a step-off and gap, was clearly visible in the trochlear groove and condylar surfaces.
*
Lateral View:
Revealed significant posterior displacement of the distal fragment relative to the femoral shaft, creating a posterior apex angulation. The articular involvement was confirmed, with disruption of the normal trochlear anatomy.
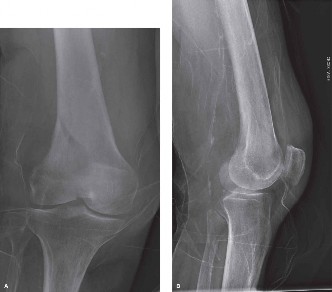
Figure 1: Initial lateral radiograph of the distal right femur demonstrating a comminuted supracondylar and intercondylar fracture with posterior displacement.
Computed Tomography (CT) Scan:
Given the complexity and intra-articular involvement noted on plain radiographs, a CT scan of the right knee with 3D reconstructions was indicated and performed immediately after initial radiographs. This provided invaluable detailed information for preoperative planning.
CT Scan Findings:
*
Fracture Morphology:
Confirmed a highly comminuted, complete articular fracture (AO/OTA Type 33-C3) of the distal femur.
*
Articular Involvement:
Detailed precise locations and sizes of articular fragments, including a significant split in the medial femoral condyle and comminution of the lateral condyle. The step-off in the weight-bearing axis was measured at 5 mm on the lateral condyle and 3 mm on the medial condyle. The articular gap was approximately 4 mm laterally.
*
Metaphyseal Comminution:
Extensive comminution of the metaphysis was observed, with cortical defects and bone loss posteriorly. This highlighted the challenge for achieving stable fixation in osteoporotic bone.
*
Diaphyseal Extension:
The fracture propagated proximally into the diaphysis, extending approximately 7 cm above the condyles, but remaining within the metaphyseal-diaphyseal junction zone.
*
Fragment Displacement:
Further delineated rotational and angular displacement of fragments, crucial for reduction strategies.
*
Bone Stock:
The overall bone density appeared reduced, consistent with the patient's known osteoporosis, implying challenges for screw purchase.
Magnetic Resonance Imaging (MRI):
An MRI was not indicated acutely in this case due to the clear fracture pattern identified on CT and the urgency for surgical planning. MRI is typically reserved for cases where soft tissue injuries (e.g., ligamentous ruptures, meniscal tears, chondral lesions) are suspected to significantly impact management, or if occult fractures are considered in the absence of clear radiographic findings, which was not the case here.
Templating:
Preoperative templating was performed using the contralateral intact femur's radiographs and the CT scan data. This involved:
*
Implant Selection:
Determining the appropriate length and type of locking plate (e.g., LISS/LCP Distal Femur Plate). The comminuted nature and osteoporotic bone mandated a locked plating construct.
*
Plate Contour:
Estimating the necessary plate contour and length to adequately bridge the comminution and achieve at least 6-8 cortices of screw purchase in the diaphysis proximally and sufficient fixation in the distal fragments.
*
Screw Trajectories:
Mapping potential screw trajectories to maximize bone purchase in the small, osteoporotic articular fragments.
*
Reduction Strategy:
Anticipating the order of reduction (articular first, then metaphysis, then diaphysis) and specific reduction aids (e.g., femoral distractor, clamps, K-wires).
*
Bone Grafting:
Planning for potential autograft or allograft augmentation for metaphyseal defects, given the patient's age and osteoporosis.
The comprehensive imaging allowed for an accurate AO/OTA classification of 33-C3 , indicating a complete articular fracture with severe comminution. This detailed understanding of the fracture pattern was paramount for developing a robust surgical plan.
Differential Diagnosis
When evaluating a patient with acute knee pain and deformity following trauma, several differential diagnoses must be considered beyond an isolated distal femur fracture. A structured approach ensures no critical injury is overlooked.
| Feature | Distal Femur Fracture (e.g., AO/OTA 33-C3) | Proximal Tibia Fracture (Tibial Plateau, e.g., Schatzker VI) | Patellar Fracture (e.g., Stellate/Comminuted) | Acute Knee Dislocation (Multiligamentous Injury) |
|---|---|---|---|---|
| Mechanism of Injury | High-energy direct trauma (MVA, fall from height) or low-energy fall in osteoporotic bone. Axial loading with valgus/varus stress. | High-energy axial loading with valgus/varus stress, direct impact to proximal tibia. | Direct impact to patella (e.g., dashboard injury, direct fall onto knee). | Very high-energy trauma (MVA, sports injuries), hyperextension, rotation, direct blow. |
| Clinical Presentation |
- Severe pain, gross deformity (varus/valgus, shortening), palpable crepitus over distal femur.
- Swelling, ecchymosis, tense hemarthrosis. - Inability to bear weight. |
- Severe pain, palpable crepitus over proximal tibia/knee.
- Swelling (effusion often significant), ecchymosis over knee and proximal tibia. - Inability to bear weight. |
- Severe pain directly over patella.
- Palpable gap in patella (transverse fractures). - Swelling, hemarthrosis. - Inability to actively extend knee against gravity (extensor mechanism disruption). |
- Severe pain, gross deformity (if persistent dislocation).
- Rapid and profound swelling/hemarthrosis. - Key: Gross instability of the knee joint. - High risk of neurovascular injury (popliteal artery, peroneal nerve). |
| Key Radiographic Features |
- Fracture line extending into articular surface of distal femur.
- Comminution of condyles and metaphysis. - Displacement, angulation, rotation of distal fragment. - CT scan crucial for intra-articular detail. |
- Fracture line extending into tibial plateau.
- Depression and/or split of articular surface. - Varus/valgus collapse of plateau. - Subluxation of knee joint often present. - CT scan crucial for intra-articular detail. |
- Fracture line traversing the patella (transverse, stellate, vertical).
- Patella alta (if extensor mechanism disrupted and patellar ligament intact) or patella baja (if quadriceps tendon ruptured). - Retinacular tears often associated. |
- Often subtle or normal X-rays if spontaneously reduced.
- Dislocation of tibiofemoral joint (rarely persistent). - Stress views may show gross instability. - MRI is the gold standard for ligamentous assessment. Angiogram for vascular. |
| Management Implications |
-
Operative:
ORIF with locking plate (LISS/LCP) for displaced, intra-articular fractures.
- NWB for 6-12 weeks. - High risk of malunion, non-union, stiffness. |
-
Operative:
ORIF with plate and screws for displaced articular fractures, bone graft often needed.
- NWB for 6-12 weeks. - High risk of post-traumatic arthritis, stiffness, compartment syndrome. |
-
Operative:
Tension band wiring (transverse), partial or total patellectomy (comminuted) for extensor mechanism disruption.
- NWB with immobilization in extension. - Risk of extensor lag, stiffness, hardware prominence. |
-
Urgent:
Vascular assessment (ABI, CTA).
- Immediate reduction (if dislocated). - External fixation for stability, then staged ligamentous reconstruction. - High risk of limb loss or permanent disability. |
In the presented case, the clinical and radiographic findings overwhelmingly pointed to a distal femur fracture, specifically a highly comminuted, complete articular injury. The distinct location of pain, deformity, and the clear fracture lines observed on radiographs and CT scan differentiated it from other potential injuries around the knee. The absence of a palpable patellar defect or inability to extend the knee ruled out a patellar fracture as the primary injury, although it could be a concomitant finding in poly-trauma. The specific location of crepitus and deformity, proximally to the knee joint line, helped distinguish it from a primary tibial plateau fracture. While knee instability is a feature of multi-ligamentous injuries, the obvious bone injury superseded this differential as the main pathology. However, a comprehensive neurovascular assessment remains critical for all severe knee injuries, including distal femur fractures, due to the proximity of the popliteal neurovascular bundle.
Surgical Decision Making & Classification
Indications for Operative vs. Non-Operative Management:
Given the patient's functional status, the displaced and intra-articular nature of the fracture, and the significant comminution, operative management was unequivocally indicated.
Non-operative treatment
for distal femur fractures is generally reserved for:
* Non-displaced or minimally displaced, stable extra-articular fractures.
* Palliative care in non-ambulatory, severely comorbid patients where surgical risks outweigh potential benefits.
* Patients with extremely poor bone quality or significant medical contraindications to surgery, where limited weight-bearing for extended periods is feasible and acceptable.
* Certain stable periprosthetic fractures.
Operative treatment
was indicated in this case due to:
1.
Displaced Intra-articular Fracture:
Articular step-off and gap exceeding 2mm necessitate anatomical reduction to prevent post-traumatic arthritis.
2.
Unstable Fracture Pattern:
The extensive comminution and displacement rendered the fracture inherently unstable and impossible to manage non-operatively with good functional outcome.
3.
Patient's Functional Demands:
The patient was independently ambulating prior to injury, and restoring limb function was a high priority.
4.
Osteoporosis:
While challenging, osteoporotic bone often benefits from stable fixation to allow early controlled motion and facilitate healing, preventing further bone loss associated with prolonged immobilization.
Fracture Classification:
The AO/OTA (Arbeitsgemeinschaft für Osteosynthesefragen/Orthopaedic Trauma Association) classification system is the universally accepted standard for classifying long bone fractures, including those of the distal femur.
AO/OTA Classification for Distal Femur (33-):
*
33-A (Extra-articular):
Fractures proximal to the articular surface.
* 33-A1: Simple metaphyseal fracture.
* 33-A2: Metaphyseal wedge fracture.
* 33-A3: Complex metaphyseal fracture.
*
33-B (Partial Articular):
Fractures involving a portion of the articular surface.
* 33-B1: Unicondylar lateral sagittal fracture.
* 33-B2: Unicondylar medial sagittal fracture.
* 33-B3: Frontal (coronal) fracture (Hoffa fracture).
*
33-C (Complete Articular):
Fractures involving the entire articular surface and metaphyseal extension.
* 33-C1: Articular simple, metaphyseal simple.
* 33-C2: Articular simple, metaphyseal comminuted.
* 33-C3: Articular comminuted, metaphyseal comminuted.
Based on the detailed imaging, this case was classified as an AO/OTA 33-C3 fracture . This indicates a complete articular fracture with severe comminution involving both the articular surface and the metaphysis. This specific classification dictates a complex surgical approach requiring meticulous anatomical reduction of the articular fragments followed by stable fixation of the articular block to the femoral shaft, often utilizing locking plate technology. The extensive comminution also signifies a higher risk of non-union, malunion, and post-traumatic arthritis.
Pre-operative Considerations:
*
Timing:
The surgery was scheduled within 24-48 hours of presentation, allowing for adequate patient optimization (fluid resuscitation, pain control, DVT prophylaxis) and detailed surgical planning, while minimizing the risk of skin compromise from swelling.
*
Medical Optimization:
Given the patient's comorbidities (osteoporosis, hypertension, diabetes), a thorough medical evaluation was performed by an internal medicine consultant. Blood glucose was optimized, and cardiovascular stability confirmed.
*
Antibiotic Prophylaxis:
Standard broad-spectrum IV antibiotics were administered pre-operatively.
*
Informed Consent:
Detailed discussion with the patient regarding the operative plan, potential risks (infection, non-union, malunion, hardware failure, neurovascular injury, stiffness, post-traumatic arthritis), and expected post-operative course.
The decision for operative intervention was straightforward due to the fracture's inherent instability and intra-articular involvement, necessitating Open Reduction Internal Fixation (ORIF) to restore anatomical alignment and stability.
Surgical Technique / Intervention
The surgical goal was anatomical reduction of the articular surface, restoration of mechanical axis, length, and rotation, followed by stable fixation that permitted early range of motion.
Patient Positioning:
The patient was positioned supine on a radiolucent operating table. A deflatable beanbag was used to stabilize the torso. A sterile bump was placed under the ipsilateral hip to allow for slight internal rotation of the limb. The ipsilateral knee was flexed approximately 30 degrees over a sterile support (e.g., knee roll or sandbag) to facilitate posterior exposure and allow for full lateral and AP fluoroscopic imaging of the distal femur and knee joint without obstruction. A tourniquet was applied high on the thigh but not inflated unless required for severe hemorrhage or difficult visualization.
Surgical Approach:
A standard
lateral approach
to the distal femur was chosen.
1.
Incision:
A longitudinal incision was made, centered over the lateral femoral condyle, extending from approximately 10-12 cm proximal to the joint line distally to the level of the lateral epicondyle.
2.
Dissection:
The iliotibial band (ITB) was incised longitudinally. The vastus lateralis muscle was then identified. A subvastus approach or a limited vastus lateralis split was performed to expose the lateral aspect of the distal femur and femoral condyles. The subvastus approach, dissecting beneath the vastus lateralis from posterior to anterior, minimizes muscle damage and preserves vascularity.
3.
Exposure:
The periosteum was carefully elevated only where necessary for plate placement, adhering to principles of biological fixation. The fracture fragments were visualized. Care was taken to identify and protect the lateral superior genicular artery which runs deep to the vastus lateralis.
Reduction Techniques:
Reduction was performed in a methodical "distal-to-proximal" fashion:
1.
Articular Reduction:
The primary focus was the restoration of the articular congruity. Individual intra-articular fragments (medial and lateral condyles) were meticulously reduced under direct visualization and fluoroscopic guidance. Temporary fixation was achieved using 2.0 mm or 2.5 mm K-wires to stabilize the articular fragments, forming an "articular block." Intra-articular step-off and gap were verified both visually and with fluoroscopy (AP, lateral, and oblique views).
2.
Metaphyseal Reduction:
Once the articular block was reconstructed, it was reduced to the femoral shaft. This often required indirect reduction techniques due to the extensive metaphyseal comminution.
*
Distractor:
A femoral distractor was applied from the proximal tibia to the proximal femur to restore length and distract the fragments, facilitating reduction.
*
Ligamentotaxis:
Traction through the knee joint can aid in gross alignment of articular fragments.
*
Reduction Clamps:
Pointed reduction clamps (e.g., Weber clamps) were used cautiously to achieve initial apposition between the articular block and the femoral diaphysis.
*
Joystick K-wires:
K-wires inserted into the larger fragments were used as joysticks to manipulate them into anatomical position.
3.
Restoration of Length, Alignment, and Rotation:
Once gross reduction was achieved, mechanical axis, length, and rotation were meticulously checked using fluoroscopy. The patella should track centrally in the trochlear groove, and the femoral neck anteversion should align appropriately relative to the knee joint. The plate itself can be used as a template to aid in maintaining reduction during screw insertion.
Fixation Construct:
A
locking compression plate (LCP) distal femur plate
system was chosen due to its angular stability, which is particularly beneficial in comminuted and osteoporotic fractures.
1.
Plate Application:
The pre-contoured LCP plate was slid submuscularly via a minimally invasive plate osteosynthesis (MIPO) technique where feasible, or applied directly if more extensive exposure was necessary for complex reduction. The plate was centered on the lateral femoral shaft, ensuring it was appropriately positioned relative to the lateral condyle.
2.
Distal Fixation:
Initially, the articular block was secured to the plate with at least 3-4 locking screws. These screws were directed to engage the largest possible bone fragments in the distal condyles, avoiding the joint space. Screw length was critical to achieve bicortical purchase without violating the medial cortex or joint.
3.
Proximal Fixation:
After ensuring proper alignment, length, and rotation, the plate was secured to the femoral shaft with locking screws. A minimum of 6-8 cortices of screw purchase (e.g., 3-4 bicortical screws) were targeted proximally to provide adequate working length and stiffness. Dynamic compression holes were utilized if necessary for initial compression at the metaphysis in simple patterns, but in this C3 fracture, locking screws primarily provided fixed-angle stability.
4.
Adjuncts:
Due to significant metaphyseal comminution and concerns for bone healing in an osteoporotic patient,
autologous bone graft
(harvested from the ipsilateral iliac crest) was packed into the metaphyseal defect to promote union. Allograft or synthetic bone substitutes can also be considered.
5.
Final Checks:
Fluoroscopic images (AP, lateral, and oblique views) were taken to confirm anatomical reduction, appropriate implant position, and screw length. The range of motion of the knee was gently assessed to ensure no impingement of hardware and that motion was possible through a stable arc.
Wound Closure:
The surgical site was thoroughly irrigated. A drain was typically placed submuscularly. The vastus lateralis was repaired, followed by the ITB, subcutaneous tissue, and skin in layers.
Post-Operative Protocol & Rehabilitation
The post-operative management focused on pain control, wound care, early mobilization, and progressive weight-bearing tailored to fracture stability and healing.
Immediate Post-Operative Period (Day 0-7):
*
Pain Management:
Multimodal analgesia including regional nerve blocks (femoral nerve block), oral opioids, NSAIDs (if no contraindications), and acetaminophen.
*
Wound Care:
Regular dressing changes, monitoring for signs of infection. Drain removal when output significantly decreases.
*
DVT Prophylaxis:
Low molecular weight heparin (LMWH) or fondaparinux initiated immediately post-operatively and continued for 4-6 weeks, considering the patient's age and immobility.
*
Early Mobilization:
*
Continuous Passive Motion (CPM) Machine:
Initiated on Day 1, with a goal of achieving 0-90 degrees of knee flexion, as tolerated, to prevent stiffness and promote articular cartilage health.
*
Weight Bearing:
Strict
non-weight bearing (NWB)
on the operated limb was enforced for a minimum of 6-8 weeks, extending up to 12 weeks, depending on radiographic signs of healing and fracture stability. Crutches or a walker were provided.
*
Physical Therapy:
Bedside physical therapy initiated to teach isometric quadriceps contractions, gluteal sets, ankle pumps, and gentle active-assisted range of motion exercises for the knee (within the prescribed limits).
Phase 1: Controlled Mobilization & Protection (Weeks 1-6/8):
*
Weight Bearing:
Continued NWB.
*
Range of Motion:
Aggressive but pain-limited active and active-assisted knee flexion and extension exercises to gradually increase ROM. Target 0-110 degrees by 6 weeks.
*
Strengthening:
Isometrics for quadriceps, hamstrings, gluteals. Hip abduction/adduction in supine.
*
Transfer Training:
Education on safe transfers and activities of daily living (ADLs) while maintaining NWB.
Phase 2: Progressive Loading & Strengthening (Weeks 6/8 - 12):
*
Radiographic Assessment:
X-rays at 6-8 weeks to evaluate early signs of union (callus formation, blurring of fracture lines).
*
Weight Bearing Progression:
If radiographic healing is evident and the patient has good control, progression to
touch-down weight bearing (TDWB)
or
partial weight bearing (PWB)
(e.g., 25% body weight) may begin, using crutches or a walker. This is gradually increased based on pain tolerance and continued radiographic healing.
*
Strengthening:
Open and closed kinetic chain exercises for the knee (e.g., mini-squats, leg presses with minimal resistance), hip and ankle strengthening.
*
Balance & Proprioception:
Single leg stance with support, balance board exercises.
Phase 3: Return to Function (Weeks 12+):
*
Radiographic Assessment:
X-rays at 12 weeks to confirm bridging callus and continued union.
*
Weight Bearing:
Progression to
full weight bearing (FWB)
as tolerated, discarding gait aids.
*
Advanced Strengthening:
Progressive resistance exercises for all lower extremity muscle groups. Emphasis on functional movements, stair climbing, walking on uneven surfaces.
*
Activity Modification:
Patient educated on avoiding high-impact activities initially and for several months. Gradual return to prior activities, with consideration for the potential for hardware removal at 12-18 months post-op if symptoms warrant.
*
Long-term Monitoring:
Regular follow-up for up to 1-2 years to monitor for late complications such as post-traumatic arthritis, non-union, or implant failure. Bone health management for osteoporosis continues.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Comprehensive Preoperative Planning: A thorough understanding of the fracture morphology via CT scan with 3D reconstructions is non-negotiable for complex intra-articular distal femur fractures. Templating for plate length, screw trajectories, and potential bone grafting is crucial.
- Anatomical Articular Reduction First: The articular surface must be meticulously reduced and provisionally fixed with K-wires or fine clamps. Achieving a perfect articular reduction (less than 1-2mm step-off/gap) is paramount for minimizing post-traumatic arthritis.
- Length, Alignment, and Rotation: After articular reduction, restore the mechanical axis, length, and rotation of the femur. Fluoroscopy with full-length views is essential to verify these parameters before final fixation.
- Biological Fixation Principles (MIPO): Utilize minimally invasive techniques (MIPO) where possible to preserve the soft tissue envelope and periosteal blood supply, enhancing healing, especially in comminuted and osteoporotic fractures. Limited stripping of the metaphyseal area.
- Locked Plating Technology: The angular stability provided by locking plates (LCP/LISS) is superior in comminuted and osteoporotic bone, offering improved screw purchase and construct stability compared to conventional plates.
- Adjunctive Fixation & Grafting: Don't hesitate to use additional K-wires, interfragmentary screws (if appropriate for non-locking), or bone graft (autograft or allograft) for metaphyseal defects or to augment healing in osteoporotic patients.
- Neurovascular Assessment: Meticulous pre- and post-operative neurovascular assessment is critical due to the proximity of the popliteal vessels and nerves. Document findings thoroughly.
- Early Controlled Mobilization: Once stable fixation is achieved, initiating early range of motion is vital to prevent knee stiffness, a common and debilitating complication. However, respect the stability of the construct and progression of bone healing.
- Osteoporosis Management: Address underlying osteoporosis concurrently. Medical management (bisphosphonates, PTH analogs, vitamin D, calcium) is essential for optimizing bone healing and preventing future fragility fractures.
Pitfalls:
- Inadequate Articular Reduction: Failure to achieve anatomical reduction of the articular surface will almost inevitably lead to post-traumatic osteoarthritis, pain, and functional limitations.
- Loss of Length, Alignment, or Rotation: Malunion (varus/valgus, flexion/extension, or rotational malalignment) can result in limb length discrepancy, gait disturbance, patellofemoral pain, and increased stress on the knee joint.
- Insufficient Fixation: Inadequate number or poor placement of screws, or using a non-locked plate in comminuted/osteoporotic bone, can lead to construct failure, loss of reduction, and non-union.
- Excessive Soft Tissue Stripping: Over-zealous exposure of fracture fragments devitalizes bone, compromises the blood supply, and significantly increases the risk of infection and non-union.
- Missed Associated Injuries: Overlooking ligamentous injuries (especially in high-energy trauma) or neurovascular compromise can lead to significant long-term morbidity.
- Premature Weight-Bearing: Allowing weight-bearing before sufficient radiographic healing and fracture stability can result in hardware failure, loss of reduction, and non-union. Patient education and strict adherence to protocol are vital.
- Post-Operative Stiffness: Despite early mobilization, knee stiffness remains a common complication. Aggressive physiotherapy and, in some cases, manipulation under anesthesia or arthrolysis may be required.
- Peroneal Nerve Palsy: Can occur due to traction, direct injury during approach, or compression from excessive swelling. Vigilant monitoring and early recognition are important.
- Non-Union/Delayed Union: Particularly in comminuted, open, or osteoporotic fractures. Requires careful monitoring, and may necessitate revision surgery with bone grafting and/or adjustment of fixation.
- Hardware Prominence/Irritation: Plates and screws can irritate overlying soft tissues, especially laterally. May necessitate hardware removal after fracture union, typically at 12-18 months.
