Introduction & Epidemiology
Traumatic hip dislocations (THD) represent a true orthopedic emergency, demanding prompt recognition and expert management. These high-energy injuries, predominantly resulting from motor vehicle collisions, falls from height, or athletic trauma, threaten the vascularity of the femoral head and portend significant long-term morbidity if not addressed expeditiously. The hip joint, inherently stable due to its deep ball-and-socket configuration, robust capsuloligamentous complex, and surrounding musculature, requires substantial force to dislocate. Consequently, associated injuries are common and often dictate the complexity of treatment.
Classifications typically categorize dislocations based on the direction of femoral head displacement relative to the acetabulum:
*
Posterior Dislocations:
Account for approximately 85-90% of all THD. These commonly occur with a flexed, adducted, and internally rotated hip (e.g., "dashboard injury" where the knee strikes the dashboard, driving the femoral head posteriorly).
*
Anterior Dislocations:
Less common (5-10%), resulting from forced abduction and external rotation. These are further subdivided into obturator, pubic, and iliac types.
*
Central Dislocations:
A less precise term, usually indicating a fracture of the acetabulum with medial protrusion of the femoral head.
The incidence of THD is relatively low but clinically significant. While prompt closed reduction is the initial critical step, the subsequent evaluation for associated injuries – including acetabular fractures, femoral head or neck fractures, sciatic nerve injury, and incarcerated fragments – is paramount. Delayed reduction significantly increases the risk of complications such as avascular necrosis (AVN) of the femoral head and post-traumatic arthritis (PTA). A comprehensive understanding of the injury pattern, precise anatomical knowledge, and a systematic approach to treatment are essential for optimizing patient outcomes.
Surgical Anatomy & Biomechanics
A thorough understanding of the regional anatomy and biomechanics is foundational to the successful management of traumatic hip dislocations and their associated injuries.
The hip joint is a diarthrodial, enarthrodial (ball-and-socket) joint designed for stability and mobility. Key anatomical components include:
*
Femoral Head:
A spherical structure, two-thirds of which is covered by articular cartilage, articulating with the acetabulum. Its blood supply is critical and vulnerable to injury. The primary supply is via the medial and lateral circumflex femoral arteries, forming an extracapsular ring that gives rise to retinacular vessels. The artery of the ligamentum teres provides a minor contribution, particularly in children.
*
Acetabulum:
A cup-shaped cavity in the pelvis, formed by the ilium, ischium, and pubis. The lunate surface, covered by articular cartilage, is the primary weight-bearing area. The acetabular labrum, a fibrocartilaginous ring, deepens the socket and contributes to joint stability. The acetabular notch is bridged by the transverse acetabular ligament.
*
Joint Capsule:
A strong fibrous capsule reinforced by several powerful ligaments.
*
Ligamentous Stabilizers:
*
Iliofemoral Ligament (Y-ligament of Bigelow):
The strongest ligament in the body, anterior to the joint, preventing hyperextension.
*
Pubofemoral Ligament:
Anteroinferiorly, preventing hyperabduction and some external rotation.
*
Ischiofemoral Ligament:
Posteriorly, preventing hyperextension and internal rotation.
*
Ligamentum Teres:
Intracapsular, connecting the fovea of the femoral head to the transverse acetabular ligament, providing minor stability and vascular supply.
*
Muscular Stabilizers:
The powerful gluteal muscles (maximus, medius, minimus) and the short external rotators (piriformis, superior and inferior gemelli, obturator internus, quadratus femoris) provide dynamic stability. The psoas and iliacus contribute anteriorly.
*
Neurovascular Structures:
*
Sciatic Nerve:
Lies posterior to the hip joint, vulnerable in posterior dislocations, particularly at its point of exit below the piriformis.
*
Femoral Nerve:
Lies anterior to the hip joint, lateral to the femoral artery.
*
Femoral Artery and Vein:
Pass anterior to the hip capsule.
*
Obturator Nerve:
Medial to the joint.
Biomechanics of Dislocation:
Dislocation occurs when external forces overcome the static (capsuloligamentous, bony congruence, labrum) and dynamic (muscular) stabilizers.
*
Posterior Dislocation:
Typically involves an axial load applied to a flexed, adducted, and internally rotated knee/hip. The femoral head is driven posteriorly, often tearing the posterior capsule and occasionally the short external rotators.
*
Anterior Dislocation:
Results from forceful abduction and external rotation, often with extension. The femoral head is driven anteriorly, tearing the anterior capsule.
*
Associated Fractures:
The forces involved can also cause fractures.
*
Femoral Head Fractures (Pipkin):
Occur as the head impacts the acetabular rim during dislocation or reduction.
*
Femoral Neck Fractures:
Rare but severe, further compromising femoral head vascularity.
*
Acetabular Fractures:
Result from the femoral head impacting the acetabular dome or rim, or directly from the displacing force.
Understanding these anatomical relationships, particularly the proximity of the sciatic nerve posteriorly and the vascular supply to the femoral head, underscores the urgency of reduction and meticulous surgical planning.
Indications & Contraindications
The management of traumatic hip dislocations necessitates a rapid assessment to differentiate between dislocations requiring urgent closed reduction and those necessitating open reduction or operative fixation due to associated injuries or irreducible status.
Indications for Non-Operative Management (Closed Reduction):
The primary indication for closed reduction is an
uncomplicated traumatic hip dislocation without associated fractures or entrapped fragments.
This is the immediate, critical step in nearly all traumatic hip dislocations.
*
Uncomplicated posterior dislocation:
No evidence of femoral head fracture, acetabular fracture, or incarcerated intra-articular fragments on initial radiographs.
*
Uncomplicated anterior dislocation:
Similar to posterior, without associated bony injury or incarceration.
*
Successful reduction achieved within the critical timeframe:
Ideally within 6 hours of injury, with many advocating for reduction within 2 hours to minimize the risk of avascular necrosis (AVN).
Indications for Operative Management (Open Reduction and/or Internal Fixation):
Operative intervention is indicated in situations where closed reduction is unsuccessful, or when associated injuries compromise joint stability, congruity, or neurovascular status.
- Irreducible Dislocation: Failure to achieve concentric reduction after one or two attempts at closed reduction. This often suggests soft tissue interposition (e.g., labrum, capsule, piriformis tendon) or bony obstruction (e.g., osteochondral fragment).
-
Associated Femoral Head Fractures (Pipkin Classification):
- Type I: Fracture of the femoral head inferior to the fovea. If small and non-displaced, excision may be considered; larger or displaced fragments require ORIF.
- Type II: Fracture of the femoral head superior to the fovea (weight-bearing portion). Requires ORIF to restore articular congruity and prevent post-traumatic arthritis.
- Type III: Type I or II fracture with an associated femoral neck fracture. This is a severe injury, often necessitating ORIF of the femoral head fracture and management of the neck fracture (e.g., screws, hemiarthroplasty, or total hip arthroplasty, depending on patient age, fracture displacement, and surgeon preference).
- Type IV: Type I or II fracture with an associated acetabular fracture. Requires ORIF of both the femoral head and the acetabular fracture components.
-
Associated Acetabular Fractures:
- Fractures of the posterior wall or column causing instability after reduction.
- Displaced acetabular dome (weight-bearing) fractures.
- Intra-articular fragments identified after reduction (e.g., on post-reduction CT scan).
- Bony incarceration preventing concentric reduction.
- Concomitant Femoral Neck Fracture: Even without a femoral head fracture, a displaced femoral neck fracture in conjunction with a hip dislocation requires operative stabilization. The dislocation should be reduced first if possible, then the neck fracture addressed.
- Vascular Impairment or Nerve Entrapment: While rare, if a neurovascular compromise is directly attributable to the dislocation and cannot be resolved by closed reduction, open exploration and reduction are indicated.
- Concomitant Ipsilateral Lower Extremity Injuries: In polytrauma patients, early definitive fixation of the hip may be preferred to facilitate mobilization and overall management.
Contraindications to Closed Reduction:
*
Absolute:
None, in terms of initial attempt, if it's an isolated dislocation without obvious signs of irreducible fragments. However, if initial imaging clearly shows incarcerated bone or prosthetic components, open reduction may be prioritized.
*
Relative:
Pre-existing severe comorbidities that make immediate surgical intervention exceedingly high risk, though the urgency of reduction often outweighs many relative contraindications. The key is to manage the patient's physiological status concurrently with orthopedic management.
The decision-making process is summarized in the table below:
| Feature | Non-Operative Management (Closed Reduction) | Operative Management (Open Reduction & Internal Fixation) |
|---|---|---|
| Dislocation Status | Uncomplicated, first-time dislocation | Irreducible (failed closed reduction attempts) |
| Associated Fractures | No significant associated femoral head, neck, or acetabular fractures | Displaced femoral head fractures (Pipkin Type II-IV) |
| Displaced femoral neck fractures | ||
| Unstable acetabular fractures (e.g., posterior wall/column, displaced dome) | ||
| Intra-Articular Fragments | No evidence of incarcerated bony or cartilaginous fragments post-reduction | Evidence of incarcerated fragments (bony, labral, soft tissue) preventing concentric reduction |
| Post-Reduction Stability | Concentric and stable after closed reduction | Unstable or recurrent dislocation after closed reduction |
| Neurovascular Status | No persistent neurovascular deficit after reduction | Persistent or worsening neurovascular deficit related to dislocation/incarcerated fragments |
| Timing | Ideally within < 6 hours (target < 2 hours) of injury | Indicated after failure of closed reduction or for specific fracture patterns once patient stable |
Pre-Operative Planning & Patient Positioning
Once the decision for operative management is made, meticulous pre-operative planning and appropriate patient positioning are critical for a successful outcome and to minimize complications.
Pre-Operative Planning
-
Comprehensive Patient Assessment:
- History & Physical Examination: Confirm mechanism of injury, assess for polytrauma. A thorough neurovascular examination of the affected extremity is paramount, specifically evaluating for sciatic nerve function (peroneal and tibial divisions) in posterior dislocations and femoral nerve function in anterior dislocations. Document any pre-existing comorbidities.
-
Imaging Review:
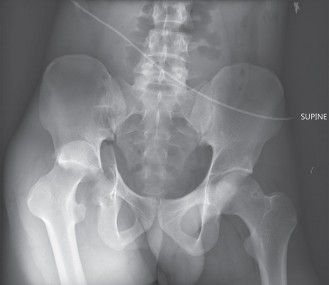
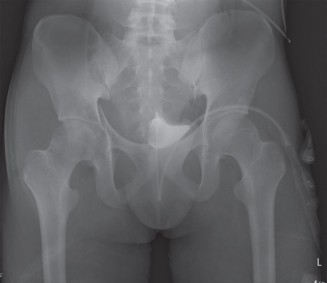
- Initial AP Pelvis and Cross-Table Lateral Hip Radiographs: These are crucial for confirming the diagnosis, classifying the dislocation type, and identifying gross associated fractures.
- Post-Reduction Radiographs: Essential to confirm concentric reduction.
-
Computed Tomography (CT) Scan:
This is the gold standard post-reduction imaging modality.
A fine-cut CT scan of the hip (with 3D reconstructions) is indispensable for:
- Identifying subtle or non-displaced acetabular fractures.
- Detecting intra-articular fragments (bony or labral) that may have been incarcerated during reduction.
- Precisely classifying femoral head fractures (Pipkin type) and assessing their displacement.
- Evaluating for femoral neck fracture patterns.
-
Assessing joint congruity post-reduction.
- Magnetic Resonance Imaging (MRI): Generally not acute pre-operative, but may be useful in cases of suspected labral injury without bony fragments, or later for assessment of avascular necrosis.
- Anesthesia Consultation: Assess patient's fitness for surgery, plan for appropriate pain management, and consider potential blood loss.
- Informed Consent: Discuss the inherent risks of surgery, including infection, neurovascular injury (especially sciatic nerve), avascular necrosis, post-traumatic arthritis, heterotopic ossification, nonunion, malunion, and the need for potential future surgery (e.g., total hip arthroplasty).
- Blood Management: Type and screen/crossmatch blood as significant blood loss can occur, particularly with complex acetabular or femoral head fracture fixation.
- Antibiotic Prophylaxis: Administer pre-operative broad-spectrum antibiotics.
- Deep Vein Thrombosis (DVT) Prophylaxis: Initiate DVT prophylaxis protocol.
- Surgical Approach Planning: Based on the injury pattern, determine the optimal surgical approach (e.g., Kocher-Langenbeck for posterior, Hueter or Smith-Petersen for anterior). Identify specific fracture patterns (e.g., acetabular posterior wall, femoral head Pipkin type) and plan the fixation strategy (implants, screw trajectories).
Patient Positioning
Correct patient positioning is crucial for surgical access, fluoroscopic visualization, and patient safety.
-
Supine Position:
- Used for: Anterior approaches (Hueter, Smith-Petersen), often for anterior dislocations or specific acetabular fracture patterns (e.g., anterior column).
- Setup: Patient supine on a radiolucent table. Ensure adequate padding at pressure points. The affected limb should be free-draped for full range of motion. Fluoroscopy C-arm access is typically from the contralateral side or perpendicular for AP/lateral views.
-
Lateral Decubitus Position:
- Used for: Posterior approach (Kocher-Langenbeck), commonly for posterior dislocations with associated posterior wall/column acetabular fractures or femoral head fractures.
- Setup: Patient is placed on the unaffected side, typically using a beanbag or sacral and anterior iliac wing supports. The chest and pelvis are secured. The affected hip is flexed approximately 30-45 degrees. The limb is draped free to allow for controlled manipulation. Ensure adequate padding, especially axillary and peroneal nerve protection. Fluoroscopy access from above the patient for AP and lateral views.
-
Prone Position:
- Used for: Less common for acute dislocations, but may be used for specific posterior column or transverse acetabular fractures when a posterior approach is favored.
- Setup: Patient prone, chest rolls or a Jackson table ensures abdominal free-hang, reducing epidural venous pressure. Padding of face, shoulders, and knees.
Regardless of position, ensure:
*
Sterile Field:
Broad preparation and draping to allow for extension of the incision if necessary and manipulation of the limb.
*
Fluoroscopy Access:
Unobstructed access for intraoperative imaging in at least two planes.
*
Surgeon Comfort:
Optimize ergonomics for the surgical team.
Detailed Surgical Approach / Technique
The surgical technique for traumatic hip dislocations, especially those complicated by fractures or irreducibility, requires precision, anatomical knowledge, and careful attention to minimize iatrogenic injury. The choice of approach is dictated by the dislocation type, associated fracture pattern, and surgeon preference.
General Principles
- Urgency: While not as critical as the initial closed reduction, operative intervention for irreducible dislocations or significant intra-articular fractures should be performed expeditiously once the patient is medically stable and imaging is complete.
- Gentle Tissue Handling: Minimize retraction and blunt dissection to protect neurovascular structures and preserve soft tissues.
- Anatomical Reduction: Achieve an anatomical reduction of the femoral head and any associated fractures.
- Stable Fixation: Provide stable internal fixation of fractures to allow early mobilization.
Posterior Dislocations (Kocher-Langenbeck Approach)
This is the workhorse approach for posterior dislocations, posterior wall/column acetabular fractures, and femoral head fractures.
- Incision: A curvilinear or straight incision centered over the greater trochanter, extending proximally towards the posterior superior iliac spine (PSIS) and distally along the femur. The length depends on the extent of exposure required.
-
Muscle Dissection:
- Fascia Lata: Incise the fascia lata in line with the skin incision.
- Gluteus Maximus: Split the gluteus maximus fibers bluntly in line with their orientation. Avoid excessive denervation of the muscle.
- Identification of Sciatic Nerve: The sciatic nerve lies deep to the gluteus maximus, superficial to the short external rotators. It must be carefully identified and protected throughout the procedure. Gentle retraction with vessel loops can assist.
-
Short External Rotators:
The piriformis, superior gemellus, obturator internus, inferior gemellus, and quadratus femoris are encountered. These muscles (typically piriformis and obturator internus with gemelli) are sharply detached from their insertions on the greater trochanter. Tags of tissue should be left for later repair. This exposes the posterior capsule.

- Capsulotomy: A T-shaped or H-shaped capsulotomy is performed. The transverse limb is made along the posterior acetabular rim, and the vertical limb extends towards the femoral neck, allowing wide exposure of the joint.
-
Joint Assessment & Fragment Removal:
- Visually inspect the femoral head for chondral lesions or fractures.
- Carefully inspect the acetabulum for fracture patterns and incarcerated fragments (bone, labrum). Remove all loose fragments. This may require irrigation and meticulous searching.
- Assess the integrity of the labrum.
-
Hip Reduction:
- If the hip is still dislocated (irreducible via closed means), gentle traction and manipulation are performed under direct vision. The limb is typically flexed, adducted, and internally rotated to clear the posterior rim, then externally rotated while applying traction. Avoid forceful maneuvers to prevent iatrogenic damage.
- Once reduced, assess for stability through a range of motion.
-
Fracture Management (e.g., Pipkin Fractures):
-
Femoral Head Fractures (Pipkin Types I-IV):
- Reduction: The femoral head fracture fragments must be meticulously reduced to restore articular congruity. Often, the hip is temporarily dislocated or distracted to gain better visualization.
- Fixation: Small, low-profile headless compression screws (e.g., Herbert screws) or absorbable pins are typically used. Screws should be placed perpendicular to the fracture plane but parallel to the joint surface to avoid articular penetration and minimize prominence. Ensure smooth articular surface. Fluoroscopy is essential to confirm screw placement.
-
Acetabular Fractures (e.g., Posterior Wall):
- Reduction: Posterior wall fragments are reduced anatomically and held with reduction clamps.
- Fixation: Fixation is typically achieved with buttress plates and screws, contouring the plate to the posterior column. Ensure adequate screw length and avoidance of intra-articular penetration.
-
Femoral Head Fractures (Pipkin Types I-IV):
-
Capsular Repair & Closure:
- Repair the posterior capsule where possible, particularly for stable constructs.
- Reattach the short external rotators to the greater trochanter using non-absorbable sutures through drill holes or transosseous tunnels. This helps restore posterolateral stability.
- Close the gluteus maximus fascia, fascia lata, and skin layers. Place a drain if significant dead space or bleeding is anticipated.
Anterior Dislocations (Modified Hueter/Anterolateral Approach)
Less common for open reduction of anterior dislocations unless irreducible or associated with specific fractures. Often, closed reduction is successful.
- Incision: A longitudinal incision centered over the anterior superior iliac spine (ASIS), extending distally along the anterior aspect of the thigh.
- Internervous Plane: The interval between the sartorius (medially, femoral nerve innervation) and tensor fascia latae (laterally, superior gluteal nerve innervation) is developed.
-
Deep Dissection:
- Retract the rectus femoris medially (femoral nerve innervation).
- Identify and protect the ascending branch of the lateral circumflex femoral artery and vein.
- The anterior hip capsule is exposed.
- Capsulotomy: A T-shaped capsulotomy is made in the anterior capsule.
- Joint Assessment & Reduction: Remove any incarcerated fragments. Manipulate the hip under direct visualization to achieve reduction.
- Fracture Management: Address any associated anterior column or specific anterior femoral head fractures.
- Closure: Repair the capsule, reapproximate muscles, close fascia and skin.
Post-Reduction Assessment
- Clinical: Re-examine neurovascular status.
- Radiological: Intraoperative fluoroscopy and post-operative radiographs (AP pelvis, cross-table lateral) are essential to confirm concentric reduction and satisfactory fracture fixation.
- Stability: Range of motion assessment to ensure stability of the joint and implant.
Complications & Management
Traumatic hip dislocations, particularly those requiring operative intervention, are associated with a significant risk of both early and late complications. Proactive recognition and appropriate management are crucial for mitigating adverse outcomes.
| Complication | Incidence | Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Sciatic Nerve Injury | 8-20% (posterior THD) | High-energy trauma, posterior dislocation, delayed reduction, associated posterior wall Fx, iatrogenic during surgery | Acute: Urgent reduction, nerve decompression if entrapped. Chronic: Observation for spontaneous recovery (up to 12-18 months), bracing, nerve transfer, tendon transfers for functional deficits. |
| Avascular Necrosis (AVN) of Femoral Head | 5-40% | Disruption of femoral head blood supply, time to reduction (>6 hours), severity of trauma, associated femoral head/neck fractures | Early: Protected weight-bearing, bisphosphonates, core decompression, vascularized fibular graft. Late: Total Hip Arthroplasty (THA) for collapse. |
| Post-Traumatic Arthritis (PTA) | Up to 60-80% (long-term) | Cartilage damage at injury, AVN, inadequate reduction, retained fragments, heterotopic ossification | Early: Activity modification, NSAIDs, intra-articular injections. Late: Joint preserving procedures (e.g., osteotomy), Arthrodesis (rare), THA for severe pain/dysfunction. |
| Heterotopic Ossification (HO) | 10-20% (clinical), higher radiographically | High-energy trauma, head injury, prolonged immobilization, associated fractures, open reduction | Prophylaxis: NSAIDs (Indomethacin) or radiation therapy post-op. Established: Observation, surgical excision if functionally limiting (after maturation). |
| Infection | 1-5% | Open wounds, prolonged surgery, patient comorbidities | Aggressive surgical debridement, organism-specific antibiotics, implant retention (if stable/early) vs. removal and staged reconstruction. |
| Redislocation | 1-5% | Inadequate reduction, associated unstable fractures, soft tissue laxity | Closed reduction if possible. If recurrent/unstable, open reduction and stabilization of underlying instability (e.g., capsular repair, acetabular fracture fixation). |
| Iatrogenic Injury | <1% | During closed reduction or open surgery (e.g., nerve, vessel, fracture) | Prevention through careful technique. Management specific to the injury (e.g., nerve repair, vascular repair, fracture fixation). |
| DVT / Pulmonary Embolism | 5-15% / 1-2% | Trauma, immobilization, hypercoagulable state | Prophylaxis: Chemical (LMWH, Factor Xa inhibitor) and mechanical (SCDs). Treatment: Anticoagulation. |
| Nonunion / Malunion of Fractures | Variable (depending on fracture type) | Inadequate fixation, severe comminution, vascular compromise | Revision internal fixation with bone grafting, conversion to arthroplasty (especially for femoral neck). |
Discussion of Key Complications:
-
Avascular Necrosis (AVN): This is arguably the most dreaded complication. Disruption of the retinacular vessels during dislocation, exacerbated by delayed reduction, is the primary etiology. The incidence is directly correlated with the time to reduction; studies consistently show a sharp increase in AVN rates when reduction is delayed beyond 6-12 hours. Associated femoral head or neck fractures also significantly elevate this risk. Management ranges from conservative (protected weight-bearing, bisphosphonates) for early, asymptomatic AVN, to joint-preserving surgeries (e.g., core decompression, vascularized fibular grafts) for pre-collapse stages, and ultimately to total hip arthroplasty (THA) once collapse and significant arthritis occur.
-
Post-Traumatic Arthritis (PTA): A very common long-term complication, occurring in a majority of patients regardless of initial management. Contributing factors include chondral damage at the time of injury, inadequate reduction of articular surfaces, retained intra-articular fragments, malunion of associated fractures, and AVN. Symptoms typically manifest years after the initial injury. Management initially involves conservative measures (NSAIDs, activity modification, physical therapy, injections). For end-stage PTA, surgical options include arthroscopy for debridement, osteotomies (rarely), or most commonly, THA.
-
Sciatic Nerve Injury: The sciatic nerve is particularly vulnerable in posterior dislocations. Injury can range from neuropraxia (most common, good prognosis for recovery) to axonotmesis or neurotmesis (poorer prognosis). Risk factors include severe trauma, posterior acetabular wall fractures, and delayed reduction. A thorough baseline neurological examination is critical, and any new or worsening deficit post-reduction warrants immediate re-evaluation and potentially surgical exploration to decompress the nerve or remove entrapped fragments. Recovery can take up to 18-24 months.
-
Heterotopic Ossification (HO): Ectopic bone formation in soft tissues around the hip is common after hip trauma and surgery. While often asymptomatic, severe HO can restrict range of motion and cause pain. Prophylaxis with non-steroidal anti-inflammatory drugs (NSAIDs, e.g., Indomethacin) or a single dose of post-operative radiation therapy is highly effective, especially in high-risk patients (e.g., head injury, polytrauma, previous HO). Surgical excision is reserved for mature, functionally limiting HO.
Early identification of these complications through diligent follow-up, appropriate imaging, and a low threshold for intervention is essential for optimizing long-term patient function and quality of life.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following traumatic hip dislocations, especially those requiring open reduction and internal fixation of associated fractures, is a critical component of successful recovery. Protocols must be individualized based on the stability of reduction, the type and stability of fracture fixation, the extent of soft tissue repair, and the presence of any complications. The overarching goals are to protect the repair, restore range of motion, regain strength, and facilitate a safe return to function.
General Principles
- Protection: Initially, protect the surgical site and fracture fixation from excessive stress.
- Gradual Progression: Advance activity levels systematically, guided by clinical and radiographic healing.
- Pain Management: Effective pain control is essential for patient participation in therapy.
- Hip Precautions: Maintain specific hip precautions for a designated period to prevent redislocation or disruption of fixation.
Phased Rehabilitation Protocol
Phase 1: Immediate Post-Operative (Weeks 0-6)
- Goals: Protect fixation, minimize pain and swelling, initiate gentle range of motion (ROM), prevent complications.
-
Weight-Bearing (WB):
- Uncomplicated THD after closed reduction, stable joint: Touch-down weight-bearing (TDWB) to partial weight-bearing (PWB) as tolerated, progressing to full weight-bearing (FWB) over 6 weeks.
- Femoral Head or Unstable Acetabular Fractures requiring ORIF: Typically non-weight bearing (NWB) or TDWB (10-15 lbs) for 6-12 weeks, depending on fracture stability and surgeon preference. This is crucial to prevent failure of fixation or collapse of the femoral head.
-
Range of Motion (ROM):
-
Passive ROM (PROM):
Initiate gentle, controlled PROM within an arc of motion deemed safe by the surgeon. Avoid extremes of motion, especially those that reproduce the dislocation mechanism.
- Posterior approach/dislocation: Avoid hip flexion >90 degrees, adduction past neutral, and internal rotation.
- Anterior approach/dislocation: Avoid hip extension, extreme external rotation, and abduction.
- Active-Assistive ROM (AAROM): Progress to AAROM as pain allows.
-
Passive ROM (PROM):
Initiate gentle, controlled PROM within an arc of motion deemed safe by the surgeon. Avoid extremes of motion, especially those that reproduce the dislocation mechanism.
-
Strengthening:
- Isometric quadriceps and gluteal sets (e.g., glute squeezes).
- Ankle pumps to prevent DVT.
- Gentle core stabilization exercises.
- Other: DVT prophylaxis (pharmacological and mechanical), wound care, patient education on precautions and assistive device use.
Phase 2: Intermediate (Weeks 6-12)
- Goals: Increase ROM, gradually increase strength, progress weight-bearing.
- Weight-Bearing: Progress from TDWB/PWB to FWB as tolerated, based on radiographic evidence of healing and surgeon's assessment. Use of crutches or a walker initially, progressing to a single cane.
- Range of Motion: Gradually increase active ROM within safe limits. Incorporate gentle stretching.
-
Strengthening:
- Initiate light isotonic exercises for hip abductors, adductors, flexors, and extensors (e.g., clam shells, leg slides, hip abduction/adduction in sidelying).
- Progress core strengthening.
- Begin stationary cycling with minimal resistance.
- Proprioception: Begin balance and proprioception exercises (e.g., standing on one leg with support).
Phase 3: Advanced Strengthening & Return to Function (Weeks 12-24 and Beyond)
- Goals: Maximize strength, endurance, and proprioception; achieve functional independence; prepare for return to desired activities.
- Weight-Bearing: Full weight-bearing without assistive devices.
- Range of Motion: Full pain-free ROM.
-
Strengthening:
- Progress to more advanced resistance exercises (e.g., lunges, squats, step-ups, leg press).
- Sport-specific or work-specific exercises.
- Advanced balance and agility training.
- Swimming, elliptical.
- Functional Activities: Gradually reintroduce recreational and occupational activities. Return to high-impact sports should be delayed until 6-12 months post-surgery, with careful assessment of strength, stability, and absence of pain.
Important Considerations
- Radiographic Follow-up: Regular X-rays are crucial to monitor fracture healing, implant integrity, and assess for signs of AVN or early post-traumatic arthritis.
- Pain-Guided Progression: Progression should always be pain-limited. Any new or increasing pain should prompt re-evaluation.
- Patient Compliance: Emphasize the importance of adherence to precautions and exercises.
- Psychological Support: Address patient's concerns, fear of re-injury, and psychological impact of a major trauma.
The ultimate success of rehabilitation hinges on a collaborative approach between the surgeon, physical therapist, and the patient, ensuring a tailored program that respects the biological healing process and the specific surgical constructs.
Summary of Key Literature / Guidelines
The management of traumatic hip dislocations has evolved over decades, with key principles remaining constant while adjunctive techniques and understanding of long-term sequelae have been refined through rigorous study.
-
Urgency of Reduction: The most critical determinant of long-term outcome, particularly regarding the risk of avascular necrosis (AVN), is the time to reduction. Classic literature, notably Stewart and Milford (1954) , established the correlation between delayed reduction and increased rates of AVN and post-traumatic arthritis. Modern reviews consistently reinforce this, with a strong recommendation for reduction within 6 hours , ideally within 2-4 hours , to minimize AVN risk.
- Conclusion: Immediate closed reduction is the paramount initial step for nearly all traumatic hip dislocations.
-
Role of Post-Reduction Imaging: While plain radiographs confirm reduction, a post-reduction Computed Tomography (CT) scan is widely considered mandatory. This consensus is driven by evidence that CT significantly improves the detection of associated injuries not visible on plain films.
- Ortho Trauma Association (OTA) and AAOS Guidelines: Strongly recommend CT imaging to identify incarcerated intra-articular fragments (bony or cartilaginous), femoral head fractures (Pipkin classification), and subtle acetabular fractures that dictate the need for open reduction and internal fixation. Failure to identify and address these fragments is a major contributor to post-traumatic arthritis.
-
Management of Associated Fractures:
-
Femoral Head Fractures (Pipkin Classification):
- Pipkin Type I and II: Non-displaced Type I fragments can sometimes be excised, but displaced Type II fragments consistently require anatomical open reduction and internal fixation (ORIF) with low-profile screws to restore articular congruity.
- Pipkin Type III and IV: These complex injuries, involving a concomitant femoral neck or acetabular fracture, often have a poorer prognosis. The decision between ORIF and arthroplasty (hemiarthroplasty or total hip arthroplasty) for older patients with femoral neck involvement remains debated and is often individualized based on fracture pattern, patient age, and activity level. The priority is to restore joint congruity and stability.
- Acetabular Fractures: The Judet and Letournel classification (1964) remains the gold standard for describing acetabular fracture patterns. Dislocations associated with unstable acetabular fractures (e.g., displaced posterior wall, posterior column, or complex patterns) necessitate ORIF. The goals are anatomical reduction, stable fixation, and restoration of the weight-bearing dome.
-
Femoral Head Fractures (Pipkin Classification):
-
Open vs. Closed Reduction: While closed reduction is the initial attempt, the literature supports open reduction for:
- Irreducible dislocations after two attempts at closed reduction.
- Dislocations with unequivocally identified incarcerated fragments on post-reduction CT.
- Associated unstable fractures that compromise hip stability or congruity.
- The surgical approach (e.g., Kocher-Langenbeck for posterior, Hueter for anterior) is chosen based on the dislocation type and fracture pattern to provide optimal visualization and access.
-
Complication Management and Prophylaxis:
- Avascular Necrosis (AVN) and Post-Traumatic Arthritis (PTA): These are the most common long-term complications. The best "treatment" is prevention through prompt, anatomical reduction. For established AVN leading to collapse or severe PTA, Total Hip Arthroplasty (THA) has become the salvage procedure of choice, offering predictable pain relief and functional restoration, though it can be technically challenging in younger patients with post-traumatic deformities.
- Sciatic Nerve Injury: Incidence ranges from 8-20% in posterior dislocations. Early neurological assessment is critical. Prognosis for recovery is generally good for neuropraxia. Persistent deficits may warrant neurophysiological studies or surgical exploration if nerve entrapment is suspected.
- Heterotopic Ossification (HO): Prophylaxis with NSAIDs (e.g., Indomethacin for 3-6 weeks) or a single low-dose radiotherapy session is effective in high-risk patients following open reduction of complicated dislocations.
In summary, current guidelines emphasize immediate closed reduction, comprehensive post-reduction CT assessment, and early, anatomical surgical intervention for irreducible dislocations or those complicated by unstable fractures or intra-articular fragments. Long-term follow-up is essential to monitor for and manage the common sequelae of AVN and PTA, which often necessitate further surgical intervention. The principles outlined ensure a systematic and evidence-based approach to optimizing outcomes for these challenging injuries.
Clinical & Radiographic Imaging