Patient Presentation & History
A 78-year-old female presents to the emergency department following a ground-level fall at home. She tripped on a rug and landed directly onto her left hip. She immediately experienced severe left hip pain and was unable to bear weight or move her left lower extremity. She reports no loss of consciousness, head injury, or other acute injuries.
Her medical history is significant for:
* Osteoporosis, diagnosed 5 years prior, managed with weekly Alendronate.
* Hypertension, well-controlled on Lisinopril.
* Type 2 Diabetes Mellitus, managed with Metformin, HbA1c 7.1%.
* Atrial Fibrillation, on Apixaban for anticoagulation.
* Mild cognitive impairment, managed by her family. She is generally independent with activities of daily living (ADLs) with a cane for ambulation, and lives with her daughter.
* Previous falls: One fall in the past year, resulting in a wrist sprain.
* Surgical history: Cholecystectomy 15 years prior.
Upon arrival, she is alert but visibly distressed due to pain. Vital signs are stable. She is unable to stand or ambulate due to severe left hip pain. Her family confirms her pre-injury functional status was independent ambulation with a cane, able to manage stairs and community ambulation for short distances.
Clinical Examination
Inspection
The left lower extremity is slightly externally rotated and appears shortened compared to the right. There is moderate swelling over the left greater trochanter and lateral thigh. No obvious ecchymosis or open wounds are noted acutely. The skin is intact.
Palpation
Palpation elicits severe tenderness over the left greater trochanter, iliac crest, and pubic rami. There is crepitus noted with gentle rotation of the left hip. Distal palpation of the left femur and patella reveals no specific tenderness.
Range of Motion
Active range of motion of the left hip is severely limited and painful in all planes. Passive range of motion is also exquisitely painful and guarded, with only a few degrees of flexion and external rotation possible before muscle spasm and patient discomfort halt further movement. An attempt at internal rotation causes significant pain. The patient is unable to perform a straight leg raise. Right hip range of motion is full and pain-free.
Neurological Assessment
- Motor: Grossly, strength is 5/5 in the right lower extremity. In the left lower extremity, the patient is unable to lift against gravity due to pain, but she can demonstrate flicker strength in the quadriceps (L3-L4), tibialis anterior (L4-L5), extensor hallucis longus (L5), and gastrocnemius (S1) muscles when attempting minimal movement. Specific testing of individual muscle groups for sciatic or femoral nerve compromise is limited by pain and guarding, but no gross foot drop or quadriceps paralysis is evident.
- Sensory: Sensation to light touch is intact in the bilateral L2, L3, L4, L5, and S1 dermatomes.
- Reflexes: Bilateral patellar (L3-L4) and Achilles (S1) reflexes are 2+.
Vascular Assessment
Distal pulses (femoral, popliteal, dorsalis pedis, posterior tibial) are 2+ and symmetrical bilaterally. Capillary refill in the left toes is less than 2 seconds. The left lower extremity is warm to touch. There are no signs of acute ischemia or compartment syndrome.
Associated Injuries
A gentle assessment of the pelvic ring stability with AP and lateral compression reveals no overt instability, though this is limited by patient pain and muscle guarding. The bilateral knees and ankles are clinically stable with no signs of fracture or ligamentous injury. The lumbar spine is non-tender to palpation.
Imaging & Diagnostics
Initial Radiographs
Standard radiographs of the pelvis and left hip were obtained upon arrival.
*
Anteroposterior (AP) Pelvis View:
Demonstrates a comminuted fracture involving the left acetabulum, with extension into the anterior and posterior columns. There is significant superior migration and impaction of the femoral head. The integrity of the ipsilateral femoral neck is assessed and appears intact. Evidence of severe osteopenia is present.
*
Iliac Oblique View (Judet View):
Provides a profile of the anterior column and posterior wall. This view shows significant comminution of the posterior wall and superior portion of the posterior column. There is articular step-off and marginal impaction of the posterior wall fragment.
*
Obturator Oblique View (Judet View):
Profiles the posterior column and anterior wall. This view elucidates a fracture line extending through the obturator ring into the anterior column, with comminution.
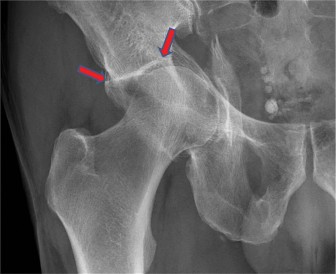
Figure 1: Initial Iliac Oblique (Judet) radiograph of the left acetabulum demonstrating a complex, comminuted fracture pattern.
The radiographic findings collectively indicate a complex acetabular fracture, likely an associated anterior column and posterior hemitransverse or a both column pattern, with significant comminution of the weight-bearing dome and articular surface impaction. The osteopenic bone quality is evident.
Computed Tomography (CT)
A dedicated CT scan of the pelvis with 1.25mm axial cuts and multiplanar reconstructions (coronal, sagittal) and 3D volume renderings was performed for detailed fracture characterization and pre-operative planning.
*
Axial Views:
Confirm extensive comminution involving the quadrilateral plate and medial wall, with intra-articular fragments and medial displacement of the femoral head. There is significant impaction of the superior dome.
*
Coronal Views:
Demonstrate vertical shear components and the extent of superior migration of the femoral head. Articular step-off and gapping are clearly visible.
*
Sagittal Views:
Further delineate impaction of the posterior wall and superior dome.
*
3D Reconstructions:
Provide an invaluable global understanding of the fracture pattern, confirming a highly comminuted associated anterior column and posterior hemitransverse fracture involving the weight-bearing dome, with significant impaction and osteochondral fragments. The posterior column is also comminuted. A large segment of the quadrilateral plate is displaced medially. There is no evidence of an acute femoral head fracture, but the head appears deeply impacted into the acetabulum. No clear signs of femoral head impaction fracture were identified, but cartilage damage is highly suspected.
Magnetic Resonance Imaging (MRI)
MRI was not deemed acutely necessary for primary fracture characterization, as CT provided sufficient detail for surgical planning. It would be indicated if an occult femoral neck fracture was suspected despite CT, or if there were concerns for extensive soft tissue injury not amenable to CT.
Templating
Pre-operative templating using the CT data was crucial. This involved:
* Assessing the size and morphology of the acetabulum for potential reconstruction rings or total hip arthroplasty (THA) components.
* Planning potential plate contours and screw trajectories.
* Identifying the extent of bone loss and potential need for bone grafting or specific augmentations (e.g., anti-protrusio cage).
* Determining the optimal surgical approach based on the specific fracture lines and displacement.
Other Diagnostics
Routine pre-operative blood work included complete blood count, basic metabolic panel, coagulation studies (PT/INR, PTT, given Apixaban use), and type and screen. ECG showed atrial fibrillation with controlled ventricular rate. Chest X-ray was clear. Cardiopulmonary clearance was obtained, with recommendations for peri-operative management of anticoagulation and diabetes. Apixaban was held for 48 hours pre-operatively.
Differential Diagnosis
The presentation of a geriatric patient with hip pain and inability to bear weight after a fall mandates a broad differential, particularly in the context of osteopenia.
| Diagnosis | Mechanism | Clinical Features | Imaging Findings (X-ray, CT) | Management Considerations |
|---|---|---|---|---|
| Acetabular Fracture | High or low-energy trauma, often direct impact. | Severe hip/groin pain, inability to bear weight, limb shortening/rotation (variable depending on fracture pattern). Pain with any hip motion. Potential neurovascular compromise (sciatic nerve, superior gluteal vessels). | X-ray: Fracture lines across acetabulum, displacement, articular incongruity. CT: Detailed fracture morphology, comminution, articular step-off, intra-articular fragments, quadrilateral plate involvement, associated injuries. | Non-operative: Rarely for geriatric displaced fractures due to poor outcomes. Operative (ORIF or Primary THA): ORIF for reducible fractures with good bone stock. Primary THA increasingly favored for comminuted fractures involving the dome, severe osteopenia, pre-existing arthritis, or irrecoverable fragments, allowing earlier weight-bearing. Requires careful pre-op planning and consideration of comorbidities. |
| Femoral Neck Fracture | Low-energy fall in elderly, axial load, rotation. | Severe hip/groin pain, shortened and externally rotated limb (especially displaced), inability to bear weight. Groin tenderness. | X-ray: Fracture line across femoral neck (subcapital, transcervical, basicervical). May be occult (stress fracture). CT: Confirms fracture, displacement. MRI: Gold standard for occult fractures. | Operative: Displaced: Hemiarthroplasty (for low-demand/less active) or THA (for high-demand/active). Non-displaced/Impacted: Percutaneous screw fixation (risk of displacement, AVN). Rapid mobilization is key. |
| Intertrochanteric Fracture | Low-energy fall, direct lateral impact or twisting. | Severe hip pain, inability to bear weight, often significantly shortened and externally rotated limb. Swelling and ecchymosis over greater trochanter. | X-ray: Fracture line between greater and lesser trochanters. Classification (e.g., Evans, AO). CT: Detailed comminution, especially posteromedial cortex, pre-op planning. | Operative: Intramedullary nail (preferred for unstable/reverse oblique) or sliding hip screw (for stable, less comminuted). Goal: Stable fixation, early weight-bearing. |
| Pelvic Ring Fracture | Low-energy fall (insufficiency fractures) or high-energy trauma. | Groin/buttock/lumbar pain, inability to bear weight or stand. Tenderness over pubic rami, sacrum, SI joints. | X-ray: Pubic rami fractures common. Sacral insufficiency fractures may be subtle. CT: Essential for unstable patterns, sacral fractures, SI joint disruption. MRI: Best for sacral insufficiency fractures (occult on X-ray/CT). | Non-operative: Stable patterns (isolated rami, stable sacral insufficiency) with protected weight-bearing. Operative: Unstable patterns (posterior ring disruption, vertical shear) may require external fixation, internal fixation of sacrum/ilium. Often multidisciplinary with general surgery for associated visceral injury. |
| Periprosthetic Fracture | Low-energy fall in patient with prior THR/hemiarthroplasty. | Similar to other hip fractures. Pain around prosthesis, inability to bear weight. | X-ray: Fracture around existing prosthesis. Vancouver classification. CT: Details fracture morphology, bone loss, implant loosening. | Operative: Fixation around implant (cables, plates) or revision arthroplasty, depending on stability of implant and fracture pattern (Vancouver A, B, C). |
Surgical Decision Making & Classification
Surgical Decision Making
Given the patient's age, comorbidities, fracture pattern, and functional goals, the decision to proceed with operative intervention was carefully considered.
*
Non-operative management
was deemed unsuitable due to:
* Significant articular displacement and incongruity (>2mm), which carries a high risk of severe post-traumatic osteoarthritis.
* Comminution of the weight-bearing dome and quadrilateral plate, making stable non-union and chronic pain highly likely.
* The patient's pre-injury ambulatory status, where prolonged non-weight-bearing (required for non-operative management of such a fracture) would lead to severe deconditioning, loss of independence, and increased risks of complications like pneumonia, DVT, and pressure ulcers.
* The patient's mild cognitive impairment, which could compromise adherence to strict non-weight-bearing protocols.
*
Operative management
was selected with the primary goals of restoring articular congruity, achieving stable fixation (or immediate load-bearing), and facilitating early mobilization and rehabilitation to restore pre-injury function.
Fracture Classification
The fracture was classified using the
Letournel & Judet Classification
system, which categorizes acetabular fractures based on the two columns (anterior and posterior) and two walls (anterior and posterior) of the acetabulum.
Based on the comprehensive CT analysis, this fracture was classified as an
Associated Anterior Column and Posterior Hemitransverse Fracture with significant comminution of the posterior column and quadrilateral plate
. This pattern involves a fracture line traversing the anterior column and another line splitting the posterior column (hemitransverse) without extending entirely through the posterior column, often involving the superior dome. The extensive comminution, particularly involving the weight-bearing dome and medial wall, is a hallmark of geriatric acetabular fractures and complicates standard ORIF.
Choice of Surgical Strategy in Geriatric Patients
For geriatric acetabular fractures, especially those that are comminuted, involve the weight-bearing dome, and occur in osteoporotic bone, the optimal treatment strategy often diverges from that for younger patients.
*
Open Reduction and Internal Fixation (ORIF):
While standard for younger, more reducible fractures, ORIF in elderly patients with osteoporotic bone presents challenges:
* Difficulty achieving stable fixation due to poor bone quality and comminution.
* Increased risk of hardware cutout or failure.
* Necessity for prolonged protected weight-bearing, which is difficult for elderly, potentially non-compliant patients and increases morbidity.
* High risk of post-traumatic osteoarthritis requiring subsequent total hip arthroplasty.
*
Primary Total Hip Arthroplasty (THA):
This option is increasingly considered for geriatric patients with specific fracture patterns:
* Comminuted acetabular fractures involving the weight-bearing dome.
* Pre-existing osteoarthritis of the hip.
* Significant medial wall comminution or quadrilateral plate involvement, where ORIF alone is unlikely to provide stable support for a non-cemented cup.
* Osteoporotic bone quality making ORIF tenuous.
* Associated femoral head damage.
* The primary advantage is allowing immediate weight-bearing and faster return to functional mobility, which is crucial for preventing geriatric deconditioning and complications.
Considering the extensive comminution of the weight-bearing dome, medial wall involvement, impaction of the femoral head, and the patient's severe osteopenia and comorbidities precluding prolonged non-weight-bearing, the decision was made for a Primary Total Hip Arthroplasty (THA) with reconstruction of the acetabulum . This approach aims to provide a stable, immediate weight-bearing solution, thereby minimizing the risks associated with protracted rehabilitation and potential ORIF failure in this vulnerable patient population.
Surgical Technique / Intervention
Patient Positioning and Anesthesia
The patient was placed in the supine position on a radiolucent table. General anesthesia was administered, along with a regional fascia iliaca block for post-operative pain control. The affected limb was prepped and draped in a sterile fashion. Fluoroscopy was available for intraoperative imaging.
Surgical Approach
A modified Direct Anterior Approach (DAA) was chosen. This approach allows excellent visualization of the anterior column and anterior wall, which were involved in the fracture. While traditionally used for primary THA, its utility in acetabular fracture reconstruction combined with THA is gaining traction due to minimal muscle dissection, potentially lower dislocation rates, and earlier rehabilitation. In this case, it allowed for direct access to the anterior column for preliminary reduction, debridement of intra-articular fragments, and subsequent acetabular preparation.
Reconstruction for Primary THA
The surgical intervention proceeded as follows:
-
Exposure and Debridement:
- Following the DAA, the fracture fragments were meticulously identified. The hematoma was evacuated, and loose intra-articular osteochondral fragments were removed.
- The femoral head was dislocated anteriorly, allowing for full visualization of the comminuted acetabulum. The superior dome, anterior column, posterior hemitransverse components, and quadrilateral plate comminution were evident.
- The labrum was excised.
-
Preliminary Reduction and Preparation:
- Gross reduction of the major acetabular fragments was attempted using gentle traction and manipulation. This was challenging due to the comminution and osteopenia.
- Specific attention was paid to the quadrilateral plate and medial wall defects. A combination of provisional K-wires and gentle impaction techniques were used to reduce the medialized fragments and restore some bony continuity, providing a buttress for the acetabular component.
- Bone grafting (allograft cancellous chips) was packed into areas of significant bone loss, particularly within the medial wall and comminuted posterior column, to provide structural support for the cup.
-
Acetabular Reconstruction:
- Given the significant comminution of the acetabulum and poor bone quality, a custom-made or modular anti-protrusio cage (e.g., Burch-Schneider cage or similar reconstructive cage) was selected for acetabular reconstruction. This provides a rigid framework for primary stability against the compromised bone.
- The acetabulum was reamed judiciously, removing only necessary bone to create a bed for the cage. Careful reaming ensures no further damage to the already compromised bone stock.
- The selected cage was then inserted and secured with multiple cancellous screws into the remaining intact host bone (iliac wings, ischium, pubis). Fluoroscopy was used extensively to confirm screw length and trajectory, avoiding intrapelvic penetration. The cage provided robust medial support and prevented medialization of the cup.
- Following cage fixation, a cemented polyethylene acetabular liner was implanted within the cage. Cemented fixation was preferred for the liner within the cage due to the patient's osteoporotic bone, ensuring immediate and stable fixation within the reconstruction.
-
Femoral Component Implantation:
- The femoral head was resected.
- The femoral canal was prepared using standard broaching techniques.
- A cemented femoral stem was selected. Cemented fixation is often preferred in elderly patients with osteoporotic bone for immediate stability and reduced risk of subsidence, unlike cementless stems which rely on bone ingrowth.
- The stem was implanted, and the cement allowed to cure.
-
Trial Reduction and Final Implantation:
- Trial components (head and liner) were used to assess leg length, offset, and stability through a full range of motion. Adjustments were made as necessary.
- The final femoral head was selected and impacted onto the stem. The final cemented polyethylene liner was placed into the acetabular cage.
- The hip was reduced. Stability was re-checked through a full range of motion, confirming no impingement or dislocation within the typical arc of movement.
-
Closure:
- The wound was irrigated thoroughly.
- A closed suction drain was placed.
- The layers were meticulously closed, ensuring anatomical repair of the interval. Skin was closed with staples.
Post-Operative Protocol & Rehabilitation
Acute Post-Operative Period (Days 0-7)
- Pain Management: Multimodal approach including regional nerve blocks, oral opioids, NSAIDs (if no contraindications), and acetaminophen. Aggressive pain control is paramount for early mobilization.
- DVT Prophylaxis: Low Molecular Weight Heparin (LMWH) initiated post-operatively after hemostasis confirmed, continued for 4-6 weeks. Early mobilization is also a key component of prophylaxis.
-
Mobilization:
- Day 0-1: Out of bed to chair, transfers with physical therapy.
- Day 1-2: Initiate protected weight-bearing as tolerated (WBAT) with an assistive device (walker). The use of an anti-protrusio cage and cemented components in this primary THA allows for immediate, rather than delayed, weight-bearing, which is a significant advantage in geriatric patients.
- Day 3+: Progressive gait training, stair training as tolerated.
- Precautions: Standard hip precautions (e.g., avoiding hip flexion >90 degrees, adduction past midline, internal rotation for posterolateral approach; relevant precautions for DAA).
- Monitoring: Regular neurovascular checks, wound inspection, drain output monitoring.
- Nutrition: Adequate hydration and nutrition support to aid healing and recovery.
- Delirium Prevention: Regular reorientation, consistent sleep-wake cycles, avoiding sedatives where possible.
Subacute Rehabilitation (Weeks 1-6)
-
Physical Therapy:
- Intensive inpatient rehabilitation typically for 2-4 weeks, followed by home health or outpatient therapy.
- Focus on progressive strengthening of hip abductors, extensors, and core musculature.
- Advanced gait training, balance exercises, and functional task practice (dressing, bathing).
- Continue with range of motion exercises within precautions.
- Weight-Bearing: Progress from walker to cane as tolerated, aiming for independence in ambulation.
- Pain Management: Transition to oral analgesics, gradually tapering as pain improves.
- Wound Care: Staple removal typically at 2-3 weeks.
Long-Term Rehabilitation (Months 2-6+)
- Outpatient Physical Therapy: Further strengthening, endurance training, proprioceptive exercises.
- Fall Prevention: Comprehensive fall risk assessment and intervention strategies (home modifications, balance training, medication review).
- Return to Activity: Gradual return to light activities and hobbies as cleared by the surgeon and physical therapist. Avoid high-impact activities.
- Follow-up Imaging: X-rays at 6 weeks, 3 months, 6 months, and 1 year post-op to assess component stability, signs of loosening, heterotopic ossification, or other complications.
- Osteoporosis Management: Continue and optimize anti-osteoporosis treatment, including calcium and vitamin D supplementation, given the high risk of future fragility fractures.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Geriatric Acetabular Fractures are Different: Recognize that osteoporotic bone, extensive comminution, and patient comorbidities often mandate different treatment strategies than in younger patients. The threshold for primary THA is lower.
- Comprehensive Imaging is Non-Negotiable: Beyond AP pelvis, Judet views are mandatory. CT with 3D reconstructions is essential for understanding fracture morphology, articular involvement, and pre-operative templating.
- Multidisciplinary Approach: Collaborate with geriatricians, internal medicine, anesthesiology, physical therapy, and social work to optimize patient care and outcomes, especially regarding comorbidities and discharge planning.
- Pre-Operative Optimization: Meticulous medical clearance, management of anticoagulation (e.g., holding Apixaban for 48 hours), and addressing nutritional status are crucial for mitigating surgical risks.
- Primary THA for Specific Patterns: In comminuted fractures involving the weight-bearing dome, significant bone loss (quadrilateral plate), pre-existing arthritis, or in patients who cannot comply with prolonged non-weight-bearing, primary THA with reconstruction (e.g., using anti-protrusio cages and cemented components) often yields better functional outcomes and fewer reoperations than ORIF.
- Robust Fixation: When ORIF is chosen, recognize poor bone quality and use augmented fixation (locking plates, multiple bicortical screws, cement augmentation, bone grafting) to improve stability and prevent cutout.
- Meticulous Reduction: Regardless of strategy, restoring articular congruity (aim for <1-2mm step-off) is paramount to prevent post-traumatic arthritis. In THA, reconstructing the acetabular defect is key for cup stability.
- Early Mobilization: The primary goal in geriatric trauma is rapid return to function and independence. Surgical strategies that allow early weight-bearing (like primary THA) are highly advantageous.
- Neurovascular Assessment: Perform and document thorough neurovascular examination pre- and post-operatively, especially for sciatic nerve function, given its proximity to the posterior acetabulum.
- DVT Prophylaxis: Aggressive chemical prophylaxis combined with early mechanical prophylaxis and mobilization is vital.
Pitfalls
- Underestimating Fracture Severity: Osteoporotic fractures can appear less displaced on X-ray but show extensive comminution and impaction on CT.
- Inadequate Pre-operative Planning: Rushing to surgery without detailed CT analysis, templating, and consideration of all surgical options can lead to suboptimal outcomes.
- Attempting ORIF in Unsuitable Cases: Trying to fix a highly comminuted, osteoporotic dome fracture with ORIF can lead to fixation failure, non-union, early post-traumatic arthritis, and the need for subsequent revision surgery, prolonging morbidity.
- Inadequate Acetabular Reconstruction in THA: Failure to address bone defects or provide stable backing for the acetabular component in primary THA can lead to cup loosening or protrusion.
- Ignoring Comorbidities: Poorly controlled diabetes, cardiac disease, or cognitive impairment significantly increase surgical and post-operative complication rates (infection, delirium, DVT, pulmonary embolism).
- Iatrogenic Injury: Risk of injury to the sciatic nerve during posterior approaches or screw placement, and to the superior gluteal vessels or corona mortis during anterior approaches.
- Heterotopic Ossification (HO): A common complication following acetabular fracture surgery, especially with extensive soft tissue dissection. Prophylaxis with NSAIDs (e.g., Indomethacin) or radiation therapy should be considered.
- Failure to Address Post-Operative Delirium: Common in elderly patients, leading to poor compliance with rehab and increased morbidity. Proactive management is essential.
- Poor Compliance with Rehabilitation: Particularly challenging in cognitively impaired patients or those with severe pain, leading to delayed recovery or complications.
- Lack of Osteoporosis Management: Failure to optimize treatment for underlying osteoporosis increases the risk of future fragility fractures.
