Introduction & Epidemiology
Sacral insufficiency fractures (SIFs) represent a distinct and increasingly recognized entity within the spectrum of fragility fractures, disproportionately affecting elderly individuals with compromised bone quality. These fractures occur without significant trauma, typically as a result of normal physiological stress on osteoporotic bone. The insidious onset and often vague symptoms, coupled with the inherent limitations of conventional radiography, frequently lead to delayed diagnosis or misdiagnosis, contributing to prolonged pain, reduced mobility, and significant morbidity.
Epidemiologically, SIFs are becoming more prevalent due to an aging population and increased awareness. Risk factors are multifactorial and include:
*
Osteoporosis:
The primary predisposing factor, often exacerbated by underlying medical conditions.
*
Radiation therapy:
Pelvic irradiation, particularly for gynecological or rectal malignancies, significantly compromises sacral bone quality and vascularity.
*
Long-term corticosteroid use:
Contributes to secondary osteoporosis.
*
Rheumatoid arthritis and other inflammatory arthropathies:
Systemic inflammation and associated treatments can impair bone health.
*
Postmenopausal status:
Estrogen deficiency accelerates bone loss.
*
Nutritional deficiencies:
Inadequate calcium and vitamin D intake.
*
Renal insufficiency:
Impaired mineral metabolism.
*
Pelvic tumors:
Can weaken bone architecture, mimicking or predisposing to insufficiency fractures.
The typical clinical presentation involves acute or subacute onset of low back, buttock, or groin pain, often radiating to the lower extremities, exacerbated by weight-bearing and relieved by rest. Neurological symptoms, though less common, can occur if fracture displacement or associated hematoma impinges on sacral nerve roots. Due to the nonspecific nature of these symptoms and the fact that plain radiographs often appear normal, SIFs are a diagnostic challenge, necessitating a high index of suspicion and advanced imaging.
Surgical Anatomy & Biomechanics
A thorough understanding of sacral anatomy and pelvic ring biomechanics is paramount for diagnosing and managing SIFs. The sacrum, a keystone of the pelvic ring, transmits axial loads from the spine to the lower extremities and provides attachments for numerous ligaments and muscles crucial for pelvic stability.
Gross Anatomy:
*
Sacral Alae:
The lateral masses, which articulate with the iliac bones to form the sacroiliac (SI) joints. These are common sites for insufficiency fractures.
*
Sacral Foramina:
Typically four pairs of anterior (ventral) and posterior (dorsal) foramina, allowing passage of sacral nerve roots. Fractures involving these foramina can lead to neurological deficits.
*
Sacral Canal:
Houses the cauda equina and sacral nerve roots.
*
Sacral Promontory:
The anterior superior margin of S1.
*
Lateral Sacral Crests:
Fusion sites of the transverse processes.
*
Median Sacral Crest:
Fusion of spinous processes.
Neuroanatomy:
The sacral plexus (L4-S4) gives rise to major nerves innervating the lower limbs, perineum, and pelvic organs. Proximity of sacral nerve roots to potential fracture lines mandates careful assessment for neurological compromise. S1 nerve roots exit between S1 and S2, S2 between S2 and S3, and so forth.
Pelvic Ring Biomechanics:
The pelvic ring functions as a closed kinematic chain, deriving stability from both anterior (pubic symphysis) and posterior (sacrum and SI joints) elements. SIFs primarily affect the posterior arch. Load transmission across the sacrum is substantial. In osteoporotic bone, the ability to withstand these physiological stresses is diminished, leading to microfractures that propagate into macroscopic fractures. Common fracture patterns for SIFs include:
*
Denis Classification (Zone I-III):
Describes fracture location relative to the sacral foramina.
*
Zone I (Alar):
Lateral to the sacral foramina. Most common type of SIF. Lowest risk of neurological deficit.
*
Zone II (Foraminal):
Through the sacral foramina. Moderate risk of neurological deficit.
*
Zone III (Central/Canal):
Medial to the sacral foramina, involving the sacral canal. Highest risk of neurological deficit and associated with greater instability.
*
Roy-Camille Classification:
Specifically for sacral fractures, focusing on vertical fracture lines and involvement of the anterior sacral cortex.
*
H-Pattern (or U-pattern) Fracture:
A classic configuration seen in SIFs, characterized by bilateral vertical alar fractures connected by a transverse fracture line through the S1 or S2 body. This indicates significant instability and often requires surgical intervention.
The bone quality in SIFs is universally poor, making traditional reduction and rigid fixation challenging. The biomechanical integrity of the entire pelvic ring must be considered, as compensatory anterior injuries (e.g., pubic rami fractures) or contralateral sacral fractures are not uncommon.
Indications & Contraindications
The management of sacral insufficiency fractures ranges from conservative care to various surgical interventions, dictated by fracture stability, pain severity, neurological status, and patient comorbidities. A high index of suspicion and accurate diagnosis, particularly when X-rays are inconclusive, drives appropriate treatment selection.
Diagnostic Imaging:
*
Plain Radiographs (AP Pelvis, Inlet, Outlet views):
Often
normal
in early SIFs, especially in osteoporotic bone where fracture lines may be subtle or nondisplaced. While useful for excluding other gross pathology, their low sensitivity necessitates further investigation.
*
CT Scan:
Provides excellent bony detail, revealing fracture lines, displacement, and fragmentation that might be missed on X-rays. It is crucial for surgical planning to assess fracture morphology and bone stock.
*
MRI:
The
gold standard
for diagnosing SIFs when plain films are negative. It demonstrates bone marrow edema (low signal on T1, high signal on T2/STIR) indicative of acute or subacute fracture, even before a clear fracture line is visible on CT. It can also assess soft tissue injury and neural impingement. Bone scintigraphy can also be highly sensitive but lacks anatomical detail.
Indications for Non-Operative Management:
* Minimally displaced, stable fractures (e.g., unilateral Zone I without an H-pattern).
* Absence of progressive neurological deficit.
* Pain manageable with conservative measures (analgesia, activity modification).
* Patients with significant comorbidities precluding surgery.
Indications for Operative Management:
* Persistent, intractable pain despite adequate non-operative treatment (typically 6-12 weeks).
* Progressive neurological deficit.
* Fracture displacement or instability (e.g., H-pattern fractures, bilateral sacral fractures, fractures extending into the sacral canal, or associated pelvic ring instability).
* Failure to ambulate or return to function due to pain.
* Non-union or delayed union.
Contraindications for Operative Management:
* Uncontrolled systemic infection.
* Severe medical comorbidities rendering the patient unfit for anesthesia and surgery.
* Extremely poor bone quality where hardware fixation is unlikely to achieve stability (though this is a relative contraindication, as cement augmentation techniques may still be viable).
* Resolved pain with conservative measures and stable fracture on imaging.
The decision for operative versus non-operative management is individualized, requiring a multidisciplinary approach and careful consideration of patient-specific factors.
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Fracture Type | Stable, minimally displaced (e.g., unilateral Zone I) | Unstable (H-pattern, bilateral, Zone II/III with displacement) |
| Pain | Mild to moderate, responsive to analgesia | Severe, intractable, refractory to conservative measures |
| Neurological | Absent or minor, non-progressive radiculopathy | Progressive deficit (weakness, bowel/bladder dysfunction) |
| Mobility | Able to ambulate with assistance; improving | Unable to ambulate due to pain/instability |
| Imaging | Stable fracture on serial imaging | Progressive displacement, non-union |
| Comorbidities | Significant, high surgical risk | Medically optimized, acceptable surgical risk |
| Primary Goal | Pain control, healing, functional recovery | Pain reduction, stabilization, neural decompression, early mobilization |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential for successful surgical outcomes in sacral insufficiency fractures, particularly given the challenges posed by poor bone quality and the proximity of neurovascular structures.
Pre-Operative Assessment:
1.
Comprehensive History and Physical Exam:
* Detailed pain history (location, character, exacerbating/alleviating factors).
* Assessment of baseline functional status and mobility.
* Thorough neurological examination: particular attention to motor and sensory deficits in L4-S5 distribution, anal sphincter tone, perianal sensation, and bladder/bowel function to identify any sacral radiculopathy or cauda equina syndrome.
2.
Imaging Review:
*
MRI:
Confirms diagnosis, identifies bone marrow edema, and rules out competing diagnoses (e.g., infection, tumor).
*
CT Scan:
Crucial for surgical planning. Defines fracture pattern (Denis zones, H-pattern), quantifies displacement, assesses bone quality (e.g., cortical breaches), and identifies safe corridors for screw placement. 3D reconstructions are invaluable for visualizing complex sacral anatomy and planning screw trajectories.
*
Pelvic X-rays:
Baseline assessment, though often insensitive for SIFs.
*
DEXA Scan:
To assess overall bone mineral density and guide post-operative bone health management.
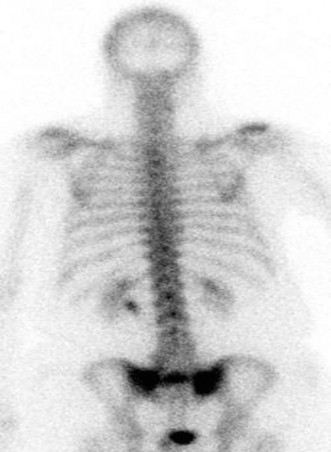
A typical MRI image showing bone marrow edema consistent with a sacral insufficiency fracture. The high signal on STIR sequences highlights the fracture line, often elusive on plain radiographs.
3.
Medical Optimization:
* Assess and optimize comorbidities (cardiac, pulmonary, renal).
* Manage osteoporosis: Vitamin D and calcium supplementation, consider starting or adjusting anti-resorptive or anabolic agents pre-operatively if time permits.
* Anemia correction, nutritional status.
* Coagulation status assessment, especially if percutaneous techniques are planned.
4.
Hardware Selection:
* Consider various fixation options: iliosacral screws, S2 alar-iliac (S2AI) screws, lumbopelvic fixation, cement augmentation (sacroplasty).
* Screw length and diameter are determined from CT measurements. Consideration for cannulated screws facilitates percutaneous placement.
* Augmentation with polymethylmethacrylate (PMMA) or calcium phosphate cement may be planned for severe osteopenia, either primarily or secondary to inadequate screw purchase.
Patient Positioning:
*
Prone Position:
The standard for most posterior sacral fixation techniques.
* Radiolucent table or bolsters to allow unimpeded C-arm access (AP, lateral, inlet, outlet views).
* Arms abducted and padded.
* Hips and knees slightly flexed, or legs extended, ensuring proper padding to prevent pressure sores (e.g., anterior superior iliac spine, knees, shins).
* Abdomen free to minimize caval compression and epidural venous bleeding.
*
Image Intensifier (C-arm):
Positioned to allow rapid acquisition of critical views (lateral for sacral body, inlet/outlet for sacral alae and SI joint, AP for overall pelvic alignment). Registration with navigation systems if utilized.
Detailed Surgical Approach / Technique
The surgical management of sacral insufficiency fractures primarily focuses on stabilization to alleviate pain and promote healing, often utilizing minimally invasive percutaneous techniques. Open reduction and internal fixation are reserved for highly unstable or displaced fractures, or when neurological decompression is required.
Percutaneous Sacroplasty / Sacral Augmentation
This technique involves injecting bone cement (typically PMMA) into the fracture site to provide immediate stability and pain relief. It is particularly effective for fractures in osteoporotic bone where screw purchase may be limited.
- Patient Positioning: Prone on a radiolucent table, as described above.
- Anesthesia: General anesthesia or local anesthesia with sedation.
- Image Guidance: C-arm fluoroscopy is essential. AP, lateral, inlet, and outlet views are used to guide needle placement.
-
Entry Points:
- For fractures of the sacral ala (Denis Zone I), a lateral approach parallel to the SI joint or a posteromedial approach can be used.
- For H-pattern fractures, cement is typically injected into the bilateral vertical alar components and potentially the transverse component.
-
Needle Insertion:
Under fluoroscopic guidance, a Jamshidi bone biopsy needle (typically 11- or 13-gauge) is advanced through the skin, muscle, and posterior sacral cortex into the fracture zone. The trajectory is critical to avoid nerve roots and the sacral canal.
-
Key Fluoroscopic Views:
- Lateral: Confirm needle tip is within the sacral body, anterior to the sacral canal.
- Inlet/Outlet: Confirm appropriate mediolateral and craniocaudal positioning within the ala, avoiding the neuroforamina.
-
Key Fluoroscopic Views:
-
Cement Injection:
- Once the needle tip is confirmed in the fracture, liquid PMMA bone cement is slowly injected under continuous fluoroscopic visualization.
- Critical Monitoring: Watch for extravasation of cement into the sacral canal, neuroforamina, SI joint, or presacral venous plexus.
- Injection is stopped when satisfactory fill is achieved, extravasation is noted, or the patient reports increased pain (if awake).
- Post-Procedure: Needles are removed, and sterile dressings applied. Patients are typically mobilized shortly after the procedure.
Percutaneous Sacral Fixation (Iliosacral Screws, S2AI Screws, Lumbopelvic Fixation)
These techniques use cannulated screws to stabilize the sacrum, often combined with cement augmentation for enhanced purchase in osteoporotic bone.
- Patient Positioning & Anesthesia: Prone, general anesthesia. Neuromonitoring (SSEP, EMG) is highly recommended due to the proximity of sacral nerve roots.
- Incision & Exposure: Small stab incisions (typically 1-2 cm) are made for percutaneous screw placement. For S2AI or lumbopelvic constructs, slightly larger incisions may be needed for pedicle screw placement in L4/L5 and rod insertion.
- Image Guidance: Fluoroscopy (C-arm or O-arm with navigation) is indispensable. Navigation systems provide real-time 3D feedback, significantly improving accuracy and reducing radiation exposure.
A. Iliosacral (IS) Screw Fixation
- Indications: Primarily for Denis Zone I and II sacral fractures, especially with unilateral instability or bilateral non-H-pattern fractures.
- Entry Point: The posterior superior iliac spine (PSIS) serves as a landmark. The entry point is typically 1-2 cm inferior and 1-2 cm anterior to the PSIS, directly over the outer table of the ilium.
-
Trajectory (S1 IS screw):
- Inlet View: Screw directed from posterior-lateral to anterior-medial, parallel to the S1 anterior cortex, passing through the S1 ala into the S1 body or contralateral ala. Avoid piercing the anterior cortex or exiting the sacral canal.
- Outlet View: Screw directed superiorly towards the sacral promontory, avoiding S1 nerve root.
- Lateral View: Screw parallel to the S1 superior endplate, aimed towards the sacral promontory.
-
Wire Insertion:
A guide wire is advanced under continuous fluoroscopic control.
- Pitfall: Anterior cortex breach, posterior canal penetration, or nerve root impingement.
-
Screw Placement:
Once wire position is confirmed in all views (AP, lateral, inlet, outlet), the tract is cannulated, tapped (optional for cancellous bone), and a cannulated, partially threaded screw is inserted over the guide wire. Screw length is typically 60-90mm.
A fluoroscopic image demonstrating the correct placement of an iliosacral screw (S1) traversing the sacral ala and body. Note the careful trajectory to avoid neural structures.
B. S2 Alar-Iliac (S2AI) Screw Fixation
- Indications: Offers increased biomechanical stability compared to S1 IS screws, especially for more unstable fractures, H-pattern fractures, or when S1 IS screws are not feasible. Can be used in conjunction with lumbopelvic fixation.
- Entry Point: Approximately 5-10 mm inferior and 5-10 mm medial to the posterior superior iliac spine (PSIS).
-
Trajectory:
- Aims from the PSIS region through the S2 sacral ala, crossing the SI joint into the ilium.
- Inlet View: Screw directed anteriorly and laterally, aimed towards the anterior inferior iliac spine (AIIS).
- Outlet View: Screw aimed towards the anterior superior iliac spine (ASIS).
- Lateral View: Screw angled anteriorly towards the greater sciatic notch.
- Wire Insertion & Screw Placement: Similar to IS screws, under fluoroscopic or navigation guidance. S2AI screws are typically longer (90-120mm) and provide better purchase in the ilium.
C. Lumbopelvic Fixation
- Indications: Reserved for highly unstable sacral insufficiency fractures, severe H-pattern fractures, lumbosacral dissociation, or when previous IS/S2AI fixation has failed. Involves connecting lumbar pedicle screws (typically L4, L5) to iliac fixation (S2AI screws or traditional iliac bolts) with longitudinal rods.
-
Technique:
- Lumbar pedicle screws are inserted at L4 and L5 levels using standard techniques.
- S2AI screws are inserted into the ilium bilaterally, as described above.
- Reduction maneuvers may be performed if displacement is present.
- Contoured longitudinal rods connect the lumbar pedicle screws to the S2AI screws, creating a rigid construct.
- Careful contouring of rods is essential to maintain physiological sagittal alignment.
Key Surgical Principles for SIF Fixation:
*
Minimally Invasive:
Whenever possible, percutaneous techniques are preferred to minimize tissue disruption, blood loss, and infection risk in often frail patients.
*
Accurate Trajectory:
Strict adherence to fluoroscopic or navigation protocols is critical to avoid neurological injury, vascular injury, or hardware malposition.
*
Bone Augmentation:
Consider cement augmentation around screws, or sacroplasty as a primary modality, especially in severe osteopenia, to improve fixation strength and reduce hardware pullout.
*
Biomechanical Stability:
Choose the fixation method that provides adequate stability for the specific fracture pattern and patient needs.
*
Neuromonitoring:
Strongly consider intraoperative neuromonitoring (EMG, SSEP) for any procedure involving sacral screw placement, particularly with complex fractures or revision surgery.
Complications & Management
Despite advances in minimally invasive techniques, complications associated with the surgical management of sacral insufficiency fractures can occur, particularly in a patient population with multiple comorbidities and poor bone quality.
| Complication | Incidence | Salvage Strategy |
|---|---|---|
| Neurological Injury | 1-5% (higher with Zone II/III fractures or malpositioned screws) | Prevention is key: Meticulous pre-operative planning with CT/3D reconstruction, intraoperative fluoroscopy/navigation, neuromonitoring. Management: Immediate hardware removal for acute deficits. Steroids for nerve edema. Surgical decompression if direct compression. Observation for mild, transient deficits. |
| Hardware Malposition | 3-10% (can lead to pain or neural injury) | Prevention: Confirm trajectory with multiple fluoroscopic views, consider navigation. Management: Revision surgery for symptomatic malposition (re-direction or removal). Asymptomatic malposition may be observed. |
| Hardware Failure | 5-15% (screw loosening, fracture, pullout) | Prevention: Proper screw length/diameter, cement augmentation, adequate biomechanical construct. Management: Revision surgery with larger/longer screws, additional fixation (e.g., lumbopelvic), cement augmentation, or alternative fixation methods. Address underlying osteoporosis. |
| Infection | 1-3% (superficial or deep) | Prevention: Sterile technique, prophylactic antibiotics. Management: Superficial: wound care, oral antibiotics. Deep: surgical debridement, intravenous antibiotics, hardware removal if persistent (may require staged reimplantation). |
| Non-Union / Delayed Union | 5-10% (persistent pain, poor healing) | Prevention: Adequate stability, biological augmentation (e.g., bone graft substitute). Management: Revision surgery with enhanced fixation, bone grafting, consideration of biological adjuncts (e.g., BMP). |
| Persistent Pain | Variable (can be due to non-union, hardware, or progression) | Management: Thorough diagnostic workup (imaging, nerve blocks) to identify cause. May require hardware removal, revision surgery, or pain management specialist referral. |
| Vascular Injury | <1% (pelvic vessels, particularly anterior to sacrum) | Prevention: Careful trajectory planning, awareness of anterior sacral anatomy. Management: Urgent vascular surgery consultation, open repair, angiography with embolization. |
| Cement Extravasation | 5-15% (sacroplasty), typically asymptomatic | Prevention: Slow injection under continuous fluoroscopy, stop at first sign of extravasation. Management: Most asymptomatic extravasations are observed. Symptomatic extravasation (e.g., neural compression, vascular compromise) may require urgent surgical removal. |
| Adjacent Segment Fracture | Long-term complication | Prevention: Optimize bone health, avoid excessive rigidity in construct if possible. Management: Treat new fracture as primary SIF. |
| Pressure Sores | 1-5% (prone positioning) | Prevention: Meticulous padding, regular position checks, minimize surgical time. Management: Wound care, pressure relief. |
General Management Principles:
*
Prevention:
The cornerstone of complication management. This includes meticulous pre-operative planning, precise surgical technique with appropriate imaging guidance, intraoperative neuromonitoring, and strict adherence to aseptic protocols.
*
Early Detection:
Vigilant post-operative monitoring for signs of neurological deficit, infection, or escalating pain.
*
Aggressive Management:
Prompt and decisive action when complications arise. This often involves revision surgery, targeted medical therapy, or multidisciplinary team input.
*
Patient Optimization:
Address underlying osteopenia/osteoporosis aggressively both pre- and post-operatively to improve bone quality and reduce the risk of hardware failure and subsequent fractures.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation for sacral insufficiency fractures aims to safely restore mobility, reduce pain, and optimize long-term function while protecting the surgical fixation and promoting bone healing. Protocols are highly individualized based on the fracture pattern, stability of fixation, patient's baseline function, and bone quality.
Immediate Post-Operative Phase (Days 0-2 weeks):
*
Pain Management:
Aggressive, multimodal analgesia to facilitate early mobilization. This includes opioid and non-opioid medications, regional nerve blocks, and patient-controlled analgesia (PCA).
*
Weight-Bearing (WB) Status:
*
Sacroplasty:
Typically full weight-bearing (FWB) as tolerated immediately, as cement provides immediate stability.
*
Percutaneous Screw Fixation (IS, S2AI):
Often partial weight-bearing (PWB) with assistive devices (walker, crutches) for 4-6 weeks, progressing to FWB as pain allows and radiographic healing progresses. In cases of very stable fixation or excellent bone quality, FWB may be permitted earlier.
*
Lumbopelvic Fixation:
Usually PWB or toe-touch weight-bearing (TTWB) initially, due to the severity of the initial injury and the more extensive construct. Progression to FWB is slower.
*
Mobilization:
* Initiate out-of-bed activity on post-operative day 0 or 1.
* Emphasis on transfers, gait training with appropriate assistive devices, and basic activities of daily living (ADLs).
* Avoidance of strenuous activities, heavy lifting, or twisting motions of the trunk.
*
Bone Health Management:
Continue or initiate medical management for osteoporosis (e.g., calcium, vitamin D, bisphosphonates, or anabolic agents) under the guidance of an endocrinologist or metabolic bone specialist.
Early Rehabilitation Phase (Weeks 2-6):
*
Physical Therapy (PT) Progression:
* Continue gait training, progressing from PWB to FWB as tolerated and guided by clinical healing and pain.
* Gentle range of motion (ROM) exercises for hips and spine, avoiding extreme flexion, extension, or rotation.
* Initiate core stabilization exercises (e.g., gentle abdominal bracing, pelvic tilts) within pain limits.
* Light strengthening exercises for hip abductors, extensors, and quadriceps.
*
Activity Modification:
Avoid activities that place high shear or torsional forces on the sacrum.
*
Radiographic Assessment:
Follow-up X-rays at 4-6 weeks to assess fracture healing and hardware integrity.
Intermediate Rehabilitation Phase (Weeks 6-12):
*
Advanced Strengthening:
Progress to more challenging core and lower extremity strengthening exercises.
*
Balance Training:
Incorporate balance and proprioceptive exercises to reduce fall risk.
*
Aerobic Conditioning:
Begin low-impact aerobic activities (e.g., stationary cycling, swimming).
*
Return to Activity:
Gradual return to light functional activities. Avoid high-impact sports or heavy lifting until full radiographic and clinical healing is confirmed.
Late Rehabilitation & Long-Term Management (Beyond 12 weeks):
*
Full Functional Recovery:
Aim for full return to pre-injury activity levels, modulated by age and comorbidities.
*
Continued Bone Health Optimization:
Lifelong management of osteoporosis is critical to prevent recurrent fractures. Regular follow-up with bone health specialists.
*
Fall Prevention:
Ongoing focus on environmental modifications, vision checks, and medication review to minimize fall risk.
*
Radiographic Healing:
Confirmation of fracture union on follow-up imaging (CT may be helpful for confirming bony bridge).
Key Considerations:
*
Patient Education:
Crucial for adherence to weight-bearing restrictions and bone health regimen.
*
Individualized Progression:
Avoid "cookbook" protocols. Adjust based on patient pain, progress, and imaging findings.
*
Multidisciplinary Approach:
Collaborate with physical therapists, occupational therapists, pain management specialists, and endocrinologists to optimize outcomes.
Summary of Key Literature / Guidelines
The literature on sacral insufficiency fractures has expanded significantly as recognition of this entity has grown. Key themes in recent guidelines and research emphasize early diagnosis, individualized treatment, and aggressive bone health management.
-
Diagnostic Imperative:
Consensus exists that plain radiographs are often insufficient for diagnosing SIFs. MRI is consistently cited as the diagnostic gold standard due to its high sensitivity for bone marrow edema. CT scans are crucial for surgical planning, delineating fracture morphology, and assessing bone quality.
- Reference: Newhouse et al. (2012) in Radiographics provide an excellent review of imaging features of sacral fractures.
-
Conservative Management First:
For stable, minimally displaced SIFs without neurological deficit, a trial of conservative management with pain control and activity modification is generally recommended as the first line of treatment.
- Reference: Multiple orthopedic and radiology society guidelines often reflect this approach for stable fragility fractures.
-
Role of Sacroplasty:
Percutaneous sacroplasty (cement augmentation) has emerged as an effective and minimally invasive option for pain relief and stabilization in patients with persistent pain despite conservative treatment, especially for H-pattern fractures or diffuse sacral edema. It provides immediate stability and significant pain reduction.
- Reference: Multiple studies, including systematic reviews (e.g., Sun et al., 2018 in Eur Spine J ), support the efficacy of sacroplasty.
-
Percutaneous Screw Fixation:
Iliosacral (IS) and S2 Alar-Iliac (S2AI) screws are well-established techniques for providing biomechanical stability to the posterior pelvic ring in more unstable SIFs. S2AI screws are increasingly favored due to potentially improved purchase and less risk of violating the S1 nerve root.
- Reference: Publications by Routt, Sagi, and others have detailed the techniques and outcomes of percutaneous pelvic fixation.
-
Lumbopelvic Fixation:
Reserved for the most unstable fractures, lumbosacral dissociation, or revision cases where simpler constructs are inadequate. While more invasive, it provides robust stability.
- Reference: Studies on spinopelvic fixation in trauma and fragility fractures often include indications for severe sacral instability.
-
Bone Health Optimization:
A critical component of SIF management, both pre- and post-operatively, is the comprehensive evaluation and treatment of osteoporosis. This includes calcium, vitamin D supplementation, and pharmacotherapy (bisphosphonates, denosumab, teriparatide) to prevent further fragility fractures.
- Reference: Guidelines from the American Academy of Orthopaedic Surgeons (AAOS) and the American Association of Clinical Endocrinologists (AACE) emphasize secondary fracture prevention.
- Multidisciplinary Approach: Optimal care for SIF patients often requires collaboration among orthopedic surgeons, pain management specialists, radiologists, endocrinologists, and physical therapists.
Ongoing research continues to refine indications, optimize surgical techniques, and improve outcomes, particularly concerning the optimal timing of intervention, comparative effectiveness of various fixation methods, and strategies to prevent subsequent fractures. The importance of a high index of suspicion, especially when confronted with the limitations of plain X-rays, remains a central tenet in managing these challenging fractures.
