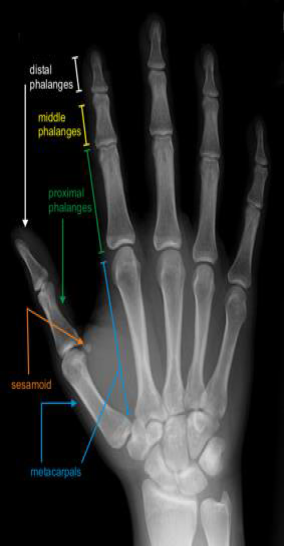
Facts *** Usually the result of high-energy injuries
* Simple dislocations are rare, most are fracture-dislocations
* Hand compartments: dorsal interossei (4), palmar interossei (3), adductor pollicis, thenar and hypothenar
* Compartment syndrome: sustained increase in compartment pressure due to inflammation and edema in one or more of the hand compartments leading to vascular compromise and muscle death
* Signs include tense swelling, pain out of proportion to injury and loss of motion
* Sensory exam may be normal
* Hand may assume intrinsic minus position (MCP extension, IP flexion)
* Compartment pressures must be measured when clinical signs of compartment syndrome are present
* Pressure > 15-20 mmHg warrants release of all 10 compartments
* Transverse carpal ligament requires release as well
Thumb (1st MC-trapezium)
:
* Most occur from axial loading of a partially flexed thumb
* Joint is structured as a reciprocal saddle joint between the 1st MC and the trapezium
* Volar oblique ligament maintains stability
* Dorsal dislocations involve disruption of the dorsoradial ligament
* Most stable in pronation and extension
* Radial artery passes beneath abductor pollicis longus (APL) and extensor pollicis brevis (EPB) just proximal to the CMC joint
* Deforming forces:
* Adductor pollicis: adduction and supination
* APL: radial and proximal
Fingers (2nd MC-trapezoid, 3rd -capitate, 4th/5th -hamate)
:
* Dislocations of the lesser CMC joints are rare due to relatively rigid anatomic configuration
* Strong ligaments provide stability and form a rigid transverse arch
* 2nd and 3rd CMC joints allow < 5° of motion and form the stable keystone of the transverse and longitudinal arch of the hand
* 4th and 5th CMC joints allow 15° and 25° of motion respectively
* Injuries of the 4th and 5th CMC joints occur more frequently
* 2nd CMC base is particularly stable due to its wedge shaped articulation with the trapezoid
* Patients present with pain, swelling and deformity
* Most CMC dislocations are dorsal
* Thumb dislocations often present reduced, requiring stress testing to determine residual instability
* Compare with contralateral side
* The ulnar nerve (motor) is at risk with 5th CMC joint dislocations
* Deep palmar arterial arch is at risk with 3rd CMC joint dislocations
* Fracture-dislocations involving the MC bases and/or the corresponding carpal bones are common
* Disruption of the normal dorsal cascade of MCP joints suggests shortening
Imaging**
Radiographs
* PA, oblique and lateral views of the hand are standard examinations
 Normal PA hand
Normal PA hand
 Normal oblique hand
Normal oblique hand
 Normal lateral hand
Normal lateral hand
-
Thumb series: true AP, oblique, lateral
- Robert view: true AP taken with hand in IR, dorsum of the thumb on the plate
-
Finger series: PA, oblique and lateral
- Lateral demonstrates avulsion fractures
- MC fractures may be better visualized with lateral and off-lateral views
-
5th MC base best visualized with 30° pronated view
Classification
*
Descriptive
Open or closed
Involved digit
Direction
Presence of fractures
-
Base of thumb MC fracture-dislocations
:
-
Often associated with thumb CMC dislocations
Type I : Bennett's fracture: partial articular fracture with volar lip fragment
-
Often associated with thumb CMC dislocations
- Represents avulsion of the strong volar oblique ligament from its insertion on the MC
-
MC is pulled proximally by abductor pollicis longus (APL)
Type II : Rolando's fracture: complete articular fracture (comminuted Bennett's) with Y or T pattern
 Base of thumb fracture-dislocations
Base of thumb fracture-dislocations
-
Base of 5th MC fracture-dislocation
:
- Reverse-Bennett's fracture: the radial-volar fragment remains reduced while remainder of the MC is pulled proximally by extensor carpi ulnaris (ECU)
 Reverse Bennett's fracture
Reverse Bennett's fracture
-
OTA
: carpal-metacarpal joints (70-C)
- 1st Metacarpal-trapezial dislocation
- 2nd MC-trapezium dislocation
- 3rd MC-capitate dislocation
- 4th MC-hamate dislocation
- 5th MC-triquetrum dislocation
- Multiple carpal-metacarpal dislocations Treatment * Acute treatment : dislocations and fracture-dislocations should be grossly reduced and splinted
-
Reduction maneuver: longitudinal traction with pressure on the base of the MC to reverse deformity
Thumb CMC dislocations :
-
Operative
: preferred in almost all cases to decrease instability and arthrosis
- Closed reduction and pinning does not adequately treat this injury
-
Options include open ligament repair with pinning of the joint or early open ligament reconstruction with flexor carpi radialis graft
Thumb CMC fracture-dislocations :
-
Operative
: preferred in almost all cases to decrease instability and arthrosis
- Percutaneous pinning: preferred for Bennett's and comminuted Rolando's fractures
- Following acceptable closed reduction, K-wires are passed across the MC shaft and into the adjacent 2nd MC and/or the trapezium
- ORIF: indicated for less comminuted Rolando's fractures
-
Fixation is achieved with screws ± plate
Finger CMC dislocations and fracture-dislocations :
-
Nonoperative
: indicated for simple dislocations and some minimally displaced fracture-dislocations that are stable after reduction
- Reductions of unstable fracture-dislocations cannot be held effectively reduced with a splint
-
Operative
: generally preferred for most injuries
- Percutaneous pinning: following acceptable closed reduction, K-wires are passed across the metacarapal shaft and into the adjacent stable MCs and/or the carpus
- ORIF: indicated for failed closed reduction or open injuries
- Stabilization can be performed with K-wires
- Reverse Bennett's fracture: often requires ORIF with wire or lag screw due to deforming forces Complications
-
Compartment syndrome: rare
- Compartment pressure > 15-20 mmHg warrants release of all 10 compartments
- Nerve injuries: the ulnar nerve (motor) is at risk with 5th CMC joint dislocations
- Posttraumatic arthritis: 2nd and 3rd CMC joints are highly amenable to arthrodesis
-
Residual instability: can be addressed with arthrodesis
- 5th CMC can be fused in 20° of flexion with little loss of hand motion
- Vascular injuries: the deep palmar arterial arch is at risk with 3rd CMC joint dislocations