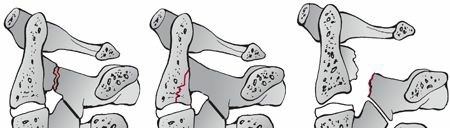
Understanding C2 Lateral Mass Fractures: Diagnosis & Treatment
Introduction & Epidemiology
Cervical spine fractures represent a significant portion of all spinal trauma, with C2 fractures accounting for approximately 15-20% of these injuries. Among C2 fractures, those involving the lateral mass are distinct entities that frequently challenge diagnostic acumen and therapeutic decision-making. These fractures, involving the superior articular facet of the axis, are typically amenable to non-operative management but can necessitate surgical intervention in cases of instability, progressive deformity, or intractable pain.
Patients often present with axial neck pain, particularly exacerbated by motion, and limited range of motion, often without overt neurologic deficits, as noted in the seminal literature. The inherent stability of the C1-C2 segment, combined with the relatively large vertebral canal at this level, contributes to the low incidence of acute spinal cord injury associated with isolated C2 lateral mass fractures. However, the presence of these fractures mandates thorough evaluation for associated injuries, given the complex biomechanical interplay of the upper cervical spine.
The mechanisms of injury are predominantly axial compression and lateral bending forces, frequently encountered in motor vehicle accidents, falls, or direct trauma. A depression fracture of the C2 articular surface, signifying impaction, is a common radiographic finding. These injuries can occur in isolation or, critically, in conjunction with other C2 fracture patterns, such as traumatic spondylolisthesis of C2 (Hangman's fracture) or odontoid fractures, as well as C1 ring fractures. Early diagnosis, primarily facilitated by advanced imaging, is paramount for guiding appropriate management and preventing delayed complications.

Surgical Anatomy & Biomechanics
The axis (C2) is a complex vertebra, serving as a critical transitional segment between the atlantoaxial complex (C1-C2) and the subaxial cervical spine. Its unique morphology, including the odontoid process, pars interarticularis, and prominent lateral masses, dictates its biomechanical function and susceptibility to specific fracture patterns.
The C2 lateral mass, specifically the superior articular facet, articulates with the inferior articular facet of C1, forming the lateral atlantoaxial joint. This joint, along with the median atlantoaxial joint (odontoid-C1 arch), permits the majority of cervical rotation. The superior articular facet of C2 is typically convex in the sagittal plane and contributes to the highly congruent C1-C2 articulation. Inferiorly, the C2 inferior articular facet articulates with C3, forming a more typical subaxial cervical facet joint.
Key anatomical considerations for C2 lateral mass fractures include:
*
Vertebral Artery (VA):
The VAs traverse the transverse foramina of C1 and C2. Within C2, the VA typically runs anterior and lateral to the pars interarticularis. Fractures extending into the transverse foramen or involving significant displacement pose a risk of VA injury (dissection, occlusion, pseudoaneurysm).
*
C2 Nerve Root (Greater Occipital Nerve):
The C2 dorsal root ganglion and nerve root exit posterior to the C1-C2 lateral mass complex. The C2 nerve root is a significant contributor to the greater occipital nerve, making it vulnerable to compression or injury with posterior approaches or severely displaced fractures, potentially leading to occipital neuralgia.
*
Pars Interarticularis:
The C2 pars interarticularis connects the superior and inferior articular facets. While lateral mass fractures primarily involve the superior facet, fracture lines can extend into the pars, potentially compromising C2 stability.
*
Ligamentous Stability:
The C1-C2 segment is stabilized by a robust ligamentous complex, including the transverse atlantal ligament, alar ligaments, and apical ligament. Injury to these structures, often associated with significant trauma, can confer instability to the C1-C2 complex, even in the presence of an apparently "stable" lateral mass fracture.
Biomechanically, the C1-C2 segment accounts for approximately 50% of cervical rotation and 10% of flexion/extension. C2 lateral mass fractures disrupt the integrity of the C1-C2 lateral articulation. The extent of articular surface depression, comminution, and involvement of the C1-C2 joint capsule and ligaments dictates the degree of potential instability. Axial compression and lateral bending forces, particularly when combined, generate high stresses across the C2 superior articular facet. Excessive lateral bending can lead to direct impaction and shear forces, resulting in facet injury.
Associated injuries, such as traumatic spondylolisthesis of C2 (Hangman’s fracture), warrant particular attention. Hangman's fractures, involving the C2 pars interarticularis, are associated with a significant incidence (up to 30%) of concomitant cervical spine fractures, including C2 lateral mass fractures. The mechanisms for Hangman's fractures often involve motor vehicle accidents and falls with flexion, extension, and axial loads, which can lead to varying degrees of intervertebral disc disruption. In the context of a Hangman's fracture, especially those with significant C2-C3 disc disruption (e.g., Levine and Edwards Type III), C2 lateral mass involvement can further compromise overall cervical stability and increase the complexity of management. The low incidence of spinal cord injury with Type I and II Hangman's fractures reflects the expansiveness of the C2 canal, while Type III injuries, characterized by significant displacement and often anterior C2-C3 disc disruption, carry a higher neurologic risk.

Indications & Contraindications
Management of C2 lateral mass fractures ranges from non-operative immobilization to surgical stabilization, predicated on a comprehensive assessment of fracture stability, neurologic status, patient comorbidities, and fracture morphology.
Non-Operative Indications
Non-operative management is the mainstay for stable, minimally displaced, and neurologically intact C2 lateral mass fractures.
*
Stable Fracture Pattern:
Defined by minimal displacement (<2-3 mm), no significant articular step-off (<2-3 mm), and intact ligamentous structures (assessed clinically and radiographically, including dynamic flexion-extension views once pain allows, if not initially contraindicated).
*
Intact Neurologic Status:
Absence of any neurologic deficit attributable to the fracture.
*
Acceptable Alignment:
Absence of significant kyphosis or rotatory subluxation of C1 on C2.
*
Low Demand Patient:
Older, less active patients who may tolerate a longer period of immobilization or who have medical comorbidities precluding surgery.
Operative Indications
Surgical intervention is considered for unstable fractures, those with neurologic compromise, or in cases where non-operative management has failed.
*
Mechanical Instability:
Defined by significant displacement (>3 mm), substantial articular surface disruption (e.g., severe depression, comminution, >3 mm step-off), or evidence of C1-C2 joint subluxation or dislocation.
*
Neurologic Deficit:
Progressive or new onset neurologic deficit attributable to the fracture.
*
Intractable Pain:
Persistent or severe neck pain despite adequate non-operative measures, indicating ongoing mechanical instability or nerve impingement.
*
Failure of Non-Operative Management:
Progressive deformity, non-union, or pseudoarthrosis despite appropriate bracing.
*
Concomitant Unstable C2 Fractures:
E.g., unstable Hangman's fracture (Levine and Edwards Type IIA or III) where the lateral mass injury contributes to overall instability, or unstable odontoid fractures.
*
Vertebral Artery Compromise:
While not a direct indication for stabilization of the lateral mass itself, VA injury (dissection, pseudoaneurysm) may influence the timing and approach of surgery, especially if decompressing the VA or achieving stable fixation for associated instability.
Contraindications
Absolute contraindications to surgery are rare but include severe medical comorbidities precluding safe anesthesia and surgery, or an active infection at the surgical site. Relative contraindications may include severe osteoporosis, which can compromise screw purchase, or certain anatomical anomalies.
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Stability | - Mechanical instability (e.g., >3 mm displacement, significant articular step-off, C1-C2 subluxation) | - Stable fracture pattern (<2-3 mm displacement, intact ligaments) |
| - Ligamentous disruption of C1-C2 complex | - No evidence of C1-C2 ligamentous injury | |
| Neurologic Status | - Progressive or new neurologic deficit | - Intact neurologic examination |
| Pain | - Intractable pain despite non-operative treatment | - Controlled pain with immobilization |
| Fracture Pattern | - Highly comminuted C2 lateral mass fractures | - Minimally displaced, non-comminuted fractures |
| - Significant C1-C2 joint incongruity/impingement | - Well-reduced articular surface | |
| Associated Injuries | - Unstable concomitant C2 fractures (e.g., Levine and Edwards Type IIA/III Hangman's, unstable odontoid) | - Isolated C2 lateral mass fracture, or stable associated injuries |
| Failed Non-Op | - Progressive deformity, non-union, or pseudoarthrosis | - Satisfactory healing with immobilization |
| Comorbidities | - Patient amenable to surgical risks and recovery | - Severe medical comorbidities precluding surgery |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is essential to ensure optimal outcomes and mitigate risks.
Diagnostic Imaging
- Plain Radiographs: Anteroposterior, lateral, and open-mouth odontoid views are initial screening tools. Lateral views provide an overall assessment of cervical alignment and C1-C2 relationships. Open-mouth views are critical for visualizing the C1-C2 joint spaces and the odontoid, but often limited in visualizing the C2 lateral masses themselves.
-
Computed Tomography (CT) Scan:
A fine-cut (≤1 mm slices) CT scan of the cervical spine with sagittal, coronal, and 3D reconstructions is the gold standard for delineating fracture morphology, displacement, comminution, articular surface involvement, and potential extension into the pars or transverse foramen. This allows for precise assessment of vertebral artery canal integrity and screw trajectory planning.
 - Magnetic Resonance Imaging (MRI): MRI is indicated to assess for associated ligamentous injuries (e.g., transverse atlantal ligament, alar ligaments), intervertebral disc integrity (C2-C3), and spinal cord status, particularly in cases with neurologic deficits or suspected ligamentous instability not fully characterized by CT.
- Computed Tomography Angiography (CTA) or Magnetic Resonance Angiography (MRA): Indicated if there is suspicion of vertebral artery injury (e.g., fracture extending into the transverse foramen, C1-C2 subluxation, or signs/symptoms of vertebrobasilar insufficiency). Pre-operative identification of VA anomalies (e.g., high-riding VA, fenestration) is crucial for surgical planning, especially if C1-C2 screw fixation is contemplated.
Surgical Strategy
The primary goals of surgery are neural decompression (if indicated), fracture reduction, and rigid internal fixation to promote fusion and restore stability.
*
Fracture Classification:
While no universally adopted classification system specifically for C2 lateral mass fractures exists, a descriptive understanding of the fracture pattern (e.g., simple articular split, depression fracture, comminuted, involvement of pars/pedicle, extension into transverse foramen) is critical.
*
Fixation Choice:
The choice of implant depends on the fracture pattern, stability, and surgeon preference. Common strategies involve C1-C2 posterior fixation (e.g., C1 lateral mass/C2 pedicle or pars screws, Harms technique, Magerl technique) or, less commonly, C2 pedicle screws if the fracture permits adequate purchase without compromising the lateral mass. The aim is to bridge and stabilize the C1-C2 segment, often requiring fusion.
*
Bone Grafting:
Autologous bone graft (iliac crest, local bone) or allograft is typically used to promote fusion.
Patient Positioning
- General Anesthesia: Typically administered. Awake fiberoptic intubation may be considered in cases of known or suspected airway compromise or C1-C2 instability.
- Prone Position: The patient is carefully turned prone on a radiolucent operating table, ensuring adequate padding to prevent pressure injuries.
- Head Stabilization: The head is secured in a Mayfield skull clamp, allowing for intraoperative manipulation to achieve reduction and maintain alignment. The head should be slightly flexed to maximize exposure of the C1-C2 posterior arch and spinous processes. Excessive flexion should be avoided to prevent undue stress on potentially unstable segments.
- Neuromonitoring: Somatosensory evoked potentials (SSEPs) and motor evoked potentials (MEPs) are standard for upper cervical spine surgery to detect intraoperative neurologic compromise.
- Fluoroscopy/Navigation: Intraoperative fluoroscopy (anteroposterior and lateral views) or 3D navigation (computed tomography-based) is indispensable for accurate screw placement and confirmation of reduction.
Detailed Surgical Approach / Technique
The posterior approach is the most common for C2 lateral mass fractures requiring stabilization. The primary goal is to achieve C1-C2 fusion.
1. Incision and Exposure
- Midline Incision: A standard posterior midline incision is made from the inion inferiorly to approximately C3-C4, centered over the C1-C2 complex.
- Subperiosteal Dissection: The superficial and deep fascial layers are incised. The muscle planes (trapezius, splenius capitis, semispinalis capitis) are carefully dissected subperiosteally from the spinous processes and laminae of C2 and C3.
-
Exposure of C1-C2:
Dissection proceeds laterally to expose the posterior arch of C1 and the C2 spinous process and laminae. Meticulous subperiosteal dissection along the posterior arch of C1 is performed to minimize muscle stripping and venous bleeding. Care is taken to identify and preserve the C2 dorsal root ganglion and nerve root, which emerges beneath the C1-C2 lamina junction. The C2 nerve root may need to be sacrificed if extensive posterolateral exposure for C2 pedicle screw placement or decompression is required, though efforts are made to preserve it if possible to avoid occipital neuralgia.

2. Reduction and Decompression
- Indirect Reduction: For C2 lateral mass fractures with associated C1-C2 subluxation, indirect reduction can often be achieved through careful head positioning in the Mayfield clamp, gentle traction, and extension. Intraoperative fluoroscopy confirms reduction.
- Direct Decompression/Reduction: If significant articular depression or comminution leads to C1-C2 facet impaction or neural compromise, direct decompression of the joint or removal of free bone fragments may be necessary. This can involve limited facetectomy or removal of impinging fragments, while carefully protecting the vertebral artery.
3. Fixation Techniques for C1-C2 Fusion
The most commonly employed fixation methods involve C1 lateral mass screws and C2 pedicle/pars screws, connected by rods.
a. C1 Lateral Mass Screw Placement
- Entry Point: The entry point for C1 lateral mass screws is typically the midpoint of the posterior arch of C1, just superior to the C1-C2 joint line.
- Trajectory: A blunt probe or burr is used to create a starting hole. The screw trajectory is approximately 10-15 degrees medial to engage the lateral mass and 10-15 degrees cephalad to avoid the vertebral artery, which typically runs anterior to the lateral mass. The screw length is typically 22-26 mm, avoiding anterior cortex breach.
- Verification: Confirm screw trajectory with a ball-tipped probe and intraoperative fluoroscopy or navigation.
b. C2 Pedicle Screw Placement
- Entry Point: The entry point for C2 pedicle screws is located at the junction of the lateral mass, lamina, and pars interarticularis, slightly lateral to the center of the C2 inferior articular facet.
- Trajectory: The screw trajectory is critical to avoid vertebral artery injury and spinal cord compromise. It is typically aimed approximately 30-40 degrees medially (converging towards the odontoid) and slightly cephalad (5-10 degrees) or parallel to the C2 endplate. Screw length typically ranges from 24-30 mm.
-
Verification:
Thorough palpation of all four pedicle walls with a ball-tipped probe is crucial before screw insertion. Intraoperative navigation or meticulous fluoroscopy (AP, lateral, and "swimmer's" view) is highly recommended. For comminuted lateral mass fractures, ensuring adequate bone stock within the pedicle is paramount.

c. C2 Pars Interarticularis Screw Placement (Magerl Technique)
- Entry Point: The entry point is located at the intersection of the midpoint of the C2 lamina and the inferior border of the C2 inferior articular facet.
- Trajectory: The screw is directed approximately 30 degrees medially and 30-40 degrees cephalad, traversing the pars interarticularis and engaging the C2 vertebral body.
- Considerations: This technique is often more challenging than pedicle screw placement due to the complex trajectory and potential for VA injury. It may be less suitable if the pars itself is fractured or severely comminuted.
d. C1-C2 Transarticular Screw Placement (Magerl Technique)
- While not directly addressing a C2 lateral mass fracture, transarticular screws can be an option if the C1-C2 joint is unstable and the C2 lateral mass fracture is stable enough to allow screw passage. However, C1 lateral mass/C2 pedicle constructs have largely supplanted this technique due to lower VA risk and technical ease.
4. Rod Contouring and Securement
- Rod Placement: Appropriately contoured rods are placed to connect the C1 lateral mass screws and C2 pedicle/pars screws. The rods are typically pre-bent to match the cervical lordosis.
- Compression/Distraction: Gentle compression or distraction may be applied to optimize reduction and achieve rigid fixation.
- Set Screw Tightening: All set screws are securely tightened.
5. Bone Grafting
- Decortication: The posterior elements of C1 and C2 (lamina, lateral masses, spinous process) are decorticated using a high-speed burr to prepare a bleeding bone bed for fusion.
- Graft Placement: Autologous bone graft (from the iliac crest or local C2/C3 spinous process) or allograft is placed over the decorticated surfaces and around the hardware to create a robust fusion mass.
6. Closure
- Irrigation: Thorough irrigation of the surgical field.
- Drain Placement: A subfascial drain may be placed to reduce hematoma formation.
- Layered Closure: The muscle fascia, subcutaneous tissue, and skin are closed in layers.

Complications & Management
C2 lateral mass fracture management, particularly surgical intervention, is associated with a range of potential complications. Vigilance and appropriate mitigation strategies are crucial.
| Complication | Incidence (Approx.) | Salvage Strategies / Management |
|---|---|---|
| Vertebral Artery Injury | 0.5-5% | - Intraoperative: Direct compression, ligation (if unilateral patent VA), vascular repair (rare). Intraoperative angiography. - Postoperative: Anticoagulation (for dissection), endovascular coiling (for pseudoaneurysm). |
| C2 Nerve Root Injury/Occipital Neuralgia | 5-15% | - Intraoperative: Meticulous dissection, careful retraction. - Postoperative: Oral NSAIDs, gabapentin/pregabalin, local anesthetic blocks, pulsed radiofrequency ablation, C2 dorsal root ganglionectomy (rarely). |
| Spinal Cord Injury | <1% (surgery); higher in Type III Hangman's | - Intraoperative: Immediate hardware removal, steroid administration, emergent decompression. - Postoperative: Intensive rehabilitation, supportive care. |
| Hardware Failure | 2-10% | - Screw pullout/breakage: Revision surgery with larger/longer screws, different trajectories, or alternative fixation points. - Rod breakage: Rod replacement, potentially revision of screw fixation. |
| Non-Union/Pseudoarthrosis | 5-15% | - Asymptomatic: Observation. - Symptomatic: Revision surgery with additional decortication, bone grafting (autograft preferred), potentially re-instrumentation. |
| Infection | 1-3% | - Superficial: Oral antibiotics, wound care. - Deep: Surgical debridement, IV antibiotics, wound vacuum-assisted closure (VAC), possible hardware removal (after fusion). |
| Dysphagia/Dysphonia | <1% (temporary) | - Usually transient due to intubation or retraction. Speech therapy, swallowing assessment. |
| Adjacent Segment Disease | Long-term; variable | - Management of symptoms (pain, neurological deficit). May require further fusion or motion-sparing procedures at adjacent segments. |
| Malposition of Hardware | 1-5% | - Asymptomatic: Observation. - Symptomatic (neural/vascular impingement): Revision surgery for screw repositioning. |
| Persistent Pain | Variable | - Multimodal pain management, physical therapy, nerve blocks. Revision surgery for non-union or hardware impingement. |

Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following C1-C2 fusion for C2 lateral mass fractures is a phased process designed to protect the fusion, restore function, and prevent complications.
Phase 1: Immediate Post-Operative (0-6 weeks)
- Immobilization: A cervical collar (e.g., Philadelphia collar, Aspen collar) is typically prescribed for 6-12 weeks to provide external support and limit motion, protecting the nascent fusion. The specific type and duration depend on the stability of the construct and surgeon preference.
- Pain Management: Aggressive, multimodal pain management, including opioids, NSAIDs (if not contraindicated for fusion), muscle relaxants, and neuropathic agents (e.g., gabapentin), is crucial.
- Wound Care: Meticulous wound care to prevent infection.
-
Activity Restrictions:
- No lifting, pushing, or pulling >5 lbs.
- Avoidance of cervical flexion, extension, and rotation.
- No overhead reaching.
- Emphasis on log-rolling technique for bed mobility.
- No driving.
- Early Mobilization: Gentle ambulation encouraged as tolerated, emphasizing core stability and avoiding jarring movements.
Phase 2: Early Fusion (6-12 weeks)
- Radiographic Assessment: Plain radiographs (AP, lateral, flexion-extension views) are obtained at 6-8 weeks to assess early fusion progress and alignment. CT scan may be performed if concerns about fusion exist.
- Collar Weaning: Gradual weaning from the cervical collar may begin if radiographic evidence of stable fusion is present and pain allows. This is often done incrementally over several weeks, starting with removal during sleep or sedentary activities.
-
Initiation of Gentle Therapy:
- Posture Education: Reinforcement of neutral spine posture during activities of daily living.
- Scapular Stabilization: Gentle isometric exercises for scapular retractors.
- Core Strengthening: Low-level isometric core exercises.
- Gradual Range of Motion: Very gentle, pain-free active range of motion of the cervical spine, initially focusing on flexion/extension and lateral bending, avoiding rotational stress on C1-C2. This should be carefully supervised by a physical therapist experienced in spinal fusion rehabilitation.
- Progressive Activity: Light cardiovascular exercise (e.g., walking, stationary bike) with cervical spine protection.
Phase 3: Advanced Fusion & Strengthening (12 weeks - 6 months)
- Radiographic Confirmation of Fusion: Repeat imaging (CT scan often recommended) at 3-6 months to definitively confirm solid arthrodesis.
- Full Collar Discontinuation: Once solid fusion is confirmed.
-
Progressive Strengthening:
- Cervical Isometrics: Progress to gentle isometric exercises for cervical flexors, extensors, and lateral rotators, with increasing resistance.
- Endurance Training: Continue and advance cardiovascular activities.
- Proprioception and Balance: Exercises to improve cervical proprioception and balance.
- Functional Training: Integration of cervical spine mobility and strength into functional activities.
- Activity Restrictions: Avoid high-impact activities, heavy lifting, contact sports, and strenuous overhead activities until complete fusion is confirmed and strength is restored.
Phase 4: Long-Term Maintenance (>6 months)
- Return to Full Activity: Gradual return to full activities, including sports and work, as tolerated and approved by the surgeon and physical therapist.
- Self-Management: Emphasis on maintaining good posture, regular exercise, and avoiding activities that provoke pain.
- Monitoring for Adjacent Segment Disease: Patients should be counseled on the long-term risk of adjacent segment disease and symptoms to monitor for.
Throughout all phases, individual patient progression should dictate the rehabilitation timeline, with a multidisciplinary approach involving the surgeon, physical therapist, and pain management specialist.
Summary of Key Literature / Guidelines
The management of C2 lateral mass fractures benefits from a confluence of biomechanical research, clinical experience, and evolving surgical techniques. While a singular classification system for C2 lateral mass fractures remains elusive, understanding their implications for C1-C2 stability is paramount.
- Diagnosis and Imaging: The role of CT imaging as the definitive diagnostic modality for fracture morphology, displacement, and articular involvement is universally acknowledged. MRI is crucial for assessing ligamentous integrity (e.g., transverse atlantal ligament, alar ligaments) and neural elements. CTA/MRA is indispensable for identifying vertebral artery anomalies or injuries, particularly prior to C1-C2 instrumentation.
- Stability Assessment: The decision-making process for C2 lateral mass fractures hinges on the concept of stability. Fractures with minimal displacement and intact ligaments are typically managed non-operatively with rigid cervical immobilization. The criteria for instability , including significant displacement (>3mm), articular step-off, C1-C2 subluxation, or overt ligamentous disruption, often necessitate surgical stabilization.
-
Surgical Techniques:
The evolution of
posterior C1-C2 fusion techniques
has revolutionized the management of upper cervical instability.
- The Harms technique (C1 lateral mass/C2 pedicle screw fixation) has largely become the preferred method due to its high biomechanical stability, reduced risk to the vertebral artery compared to transarticular screws, and high fusion rates. Studies by Harms and Melcher (2001) demonstrated the efficacy and safety of this construct.
- The Magerl technique (C1-C2 transarticular screws) , while historically important, is used less frequently due to the technical demands and higher risk of vertebral artery injury.
- Alternative fixation using C2 pars interarticularis screws (e.g., modified Magerl technique for C2) or C2 laminar screws are available but often less robust biomechanically or carry specific risks compared to pedicle screws for C2.
- Associated Injuries: The high incidence of concomitant cervical spine fractures with traumatic spondylolisthesis of C2 (Hangman's fracture) underscores the need for thorough diagnostic workup. The Levine and Edwards classification for Hangman's fractures provides a framework for understanding their stability and guiding management, ranging from collar immobilization for stable Type I fractures to surgical stabilization for unstable Type IIA and Type III injuries. A C2 lateral mass fracture in conjunction with an unstable Hangman's fracture necessitates a comprehensive approach to address both components of instability.
- Outcomes and Complications: Long-term studies indicate high fusion rates (typically >90%) with modern C1-C2 fixation techniques. However, potential complications, particularly vertebral artery injury and C2 nerve root injury/occipital neuralgia , remain significant concerns, emphasizing the need for meticulous surgical technique, intraoperative neuromonitoring, and advanced imaging for pre-operative planning.
- Rehabilitation: Post-operative protocols are designed to protect the developing fusion and gradually restore function. While initial rigid external immobilization is common, the duration and type of bracing vary based on the construct's stability and surgeon preference. Early, supervised physical therapy focuses on regaining strength and range of motion, with activity restrictions gradually lifted upon radiographic confirmation of solid fusion.
In summary, effective management of C2 lateral mass fractures requires a nuanced understanding of their complex anatomy, biomechanics, and potential for association with other critical C2 injuries. A systematic approach, integrating advanced imaging, comprehensive stability assessment, and a tailored surgical strategy when indicated, is essential for optimizing patient outcomes.
Clinical & Radiographic Imaging