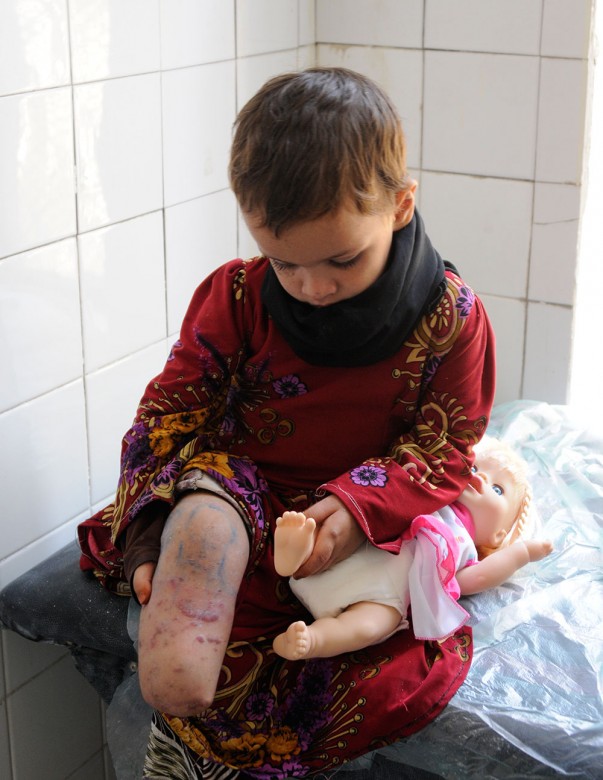
Introduction & Epidemiology
The protracted humanitarian crisis in Yemen presents an unparalleled challenge to healthcare infrastructure, profoundly impacting public health and leading to a substantial burden of orthopedic pathology. Conflict-related trauma, compounded by the collapse of healthcare services, widespread malnutrition, and endemic infectious diseases, has resulted in an alarming prevalence of acute musculoskeletal injuries and neglected orthopedic conditions. As academic orthopedic surgeons and educators, it is imperative to comprehend the complex interplay of these factors to effectively address the critical needs of patients in such austere environments.
Epidemiological data from conflict zones consistently demonstrate a high incidence of extremity trauma, including open fractures, blast injuries, and ballistic wounds. These injuries often occur in the context of limited pre-hospital care, delayed presentation to medical facilities, and compromised initial management due to resource scarcity. Consequently, the rates of complications such as chronic osteomyelitis, nonunion, malunion, and contractures are significantly elevated. Furthermore, the disruption of routine healthcare has led to a surge in neglected congenital deformities (e.g., clubfoot, developmental dysplasia of the hip) and degenerative conditions that progress to severe disability without timely intervention. The patient demographic frequently includes disabled and poor individuals, who are disproportionately affected by the crisis and face profound barriers to accessing necessary medical care and rehabilitation. The goal of orthopedic intervention in these settings extends beyond acute stabilization to encompass long-term functional restoration, dignity, and reintegration into society.

The magnitude of the crisis necessitates a strategic and adaptable approach to orthopedic care, prioritizing limb salvage, infection control, and functional outcomes despite formidable operational constraints. Understanding the specific patterns of injury and pathology prevalent in such environments is the first step towards developing effective surgical strategies.
Surgical Anatomy & Biomechanics
Effective orthopedic management, particularly in complex trauma and neglected conditions, is predicated upon a profound understanding of surgical anatomy and biomechanical principles. In the context of the Yemeni crisis, common injuries include long bone fractures (tibia, femur, humerus), often open and comminuted due to blast or ballistic mechanisms, and complex articular injuries.
Long Bone Anatomy and Internervous Planes
- Tibia: The tibia, being subcutaneously located, is highly susceptible to open fractures. Key anatomical considerations include the anterior compartment (tibialis anterior, extensor hallucis longus, extensor digitorum longus, deep peroneal nerve, anterior tibial artery/vein), lateral compartment (peroneus longus/brevis, superficial peroneal nerve), and posterior compartments (gastrocnemius, soleus, plantaris, tibialis posterior, flexor digitorum longus, flexor hallucis longus, tibial nerve, posterior tibial artery/vein, peroneal artery/vein). Understanding these compartments is crucial for fasciotomy in suspected compartment syndrome and for safe pin placement in external fixation. The relative paucity of soft tissue coverage, particularly in the distal two-thirds, contributes to higher rates of nonunion and infection.
-
Femur:
The femur's robust musculature provides better soft tissue coverage but also poses challenges in access and can mask significant soft tissue damage. Approaches typically exploit internervous planes:
- Anterolateral Approach (Hohmann): Between vastus lateralis (femoral nerve) and rectus femoris (femoral nerve) or tensor fascia lata (superior gluteal nerve) and vastus lateralis. Used for subtrochanteric, diaphyseal, and supracondylar fractures.
- Posterolateral Approach: Between vastus lateralis and biceps femoris (sciatic nerve). Used for distal femur and supracondylar fractures.
- Intramedullary Nailing: Requires precise entry portals (piriformis fossa, greater trochanter) to minimize iatrogenic damage to the hip abductors or femoral head vascularity.
-
Humerus:
The deltoid muscle (axillary nerve), radial nerve in the spiral groove, and ulnar nerve at the medial epicondyle are critical structures.
- Anterolateral Approach: Between deltoid (axillary nerve) and pectoralis major (medial/lateral pectoral nerves), or between deltoid and biceps (musculocutaneous nerve).
- Posterior Approach: Splits the triceps brachii (radial nerve). Essential for distal humerus fractures.
- Forearm (Radius/Ulna): The intricate arrangement of muscles, nerves (median, ulnar, radial), and vessels necessitates meticulous dissection. Pronator teres, brachioradialis, and flexor/extensor compartments are primary considerations.
Biomechanical Principles of Fracture Fixation
The choice of fixation strategy must balance mechanical stability, biological considerations, and the unique challenges of resource-limited environments.
-
External Fixation:
A cornerstone in conflict-related trauma due to its versatility, ability to stabilize open fractures with extensive soft tissue loss, and ease of application.
- Principles: Pins should be placed in "safe zones" away from neurovascular structures. Minimum two pins per fragment, separated by sufficient distance for stability. Avoid crossing joints unless necessary for joint stabilization (e.g., periarticular fractures). Frame configuration (uniplanar, biplanar, circular/Ilizarov) dictates stability and allows for dynamic adjustment, correction of deformity, and bone transport. Biomechanically, stiffness is influenced by pin diameter, pin separation, number of pins, and distance of the connecting bar from the bone.
- Intramedullary Nailing: Provides excellent biomechanical stability for diaphyseal fractures, especially for load-sharing in weight-bearing bones. Reamed nails offer stronger constructs and better biological response by cortical reaming. Unreamed nails are useful in contaminated wounds or systems lacking reaming capabilities. The load-sharing nature of IM nails places less stress on the implant and bone-implant interface compared to plate fixation, reducing stress shielding.
- Plate Fixation: Useful for articular and periarticular fractures, and some diaphyseal fractures. Compression plating, neutralization plating, and bridge plating are standard techniques. Locking plates offer angular stability, particularly valuable in osteoporotic bone or complex comminuted fractures where direct bone contact for friction is minimal. In settings with infection risk, plate fixation may be a less preferred initial option for open fractures compared to external fixation, but can be used for definitive fixation after soft tissue healing and infection control.
- Bone Healing: In a compromised environment (poor nutrition, infection, soft tissue defect), secondary bone healing (callus formation) is often the goal. Relative stability (e.g., IM nail, external fixator) promotes callus. Absolute stability (e.g., lag screw, compression plate) is reserved for articular fractures and requires meticulous reduction. The biological environment (vascularity, soft tissue envelope) is paramount, often taking precedence over purely mechanical considerations in severe trauma.
Indications & Contraindications
The decision-making process for orthopedic intervention in humanitarian crises is complex, balancing acute limb salvage with long-term functional outcomes, all within severe resource constraints. Prioritization is often necessary.
Indications for Operative Intervention
-
Acute Trauma:
- Open Fractures: Gustilo-Anderson Type I-III. All open fractures require surgical débridement and stabilization to prevent infection and facilitate healing. Type III fractures, especially IIIB and IIIC, represent profound soft tissue and bone loss requiring extensive reconstruction.
- Compartment Syndrome: Clinical diagnosis mandates immediate fasciotomy to prevent irreversible muscle and nerve ischemia.
- Vascular Injury with Associated Fracture: Requires prompt vascular repair or bypass and fracture stabilization (often external fixation) to ensure limb perfusion.
- Nerve Entrapment or Transection: Exploration and repair/neurolysis may be indicated depending on the severity and type of injury.
- Unstable Fractures: Those prone to significant displacement, shortening, or malrotation (e.g., displaced diaphyseal fractures, unstable pelvic ring fractures, displaced intra-articular fractures).
- Poly-trauma: Early appropriate care (EAC) with damage control orthopedics (DCO) to stabilize fractures, control hemorrhage, and prevent secondary injuries, followed by definitive fixation once the patient is stable.
- Irreducible Fractures/Dislocations: Requiring open reduction.
-
Neglected Conditions:
- Malunions: Functionally limiting deformities requiring corrective osteotomy and stable fixation.
- Nonunions: Symptomatic nonunions, particularly those with significant pain, instability, or deformity, often require revision surgery, débridement, bone grafting, and stable fixation.
- Chronic Osteomyelitis: Requires aggressive surgical débridement of infected and necrotic bone (sequestrectomy), soft tissue management, and dead space obliteration, often with prolonged antibiotic therapy.
- Severe Contractures/Deformities: Due to previous trauma, burns, or neurological conditions, impeding function or causing pain, may require soft tissue releases, osteotomies, or gradual correction (e.g., Ilizarov).
- Neglected Congenital Deformities: E.g., older children with neglected clubfoot or developmental dysplasia of the hip who present beyond the optimal age for non-operative or simpler surgical interventions, requiring more complex corrective osteotomies or fusion procedures.
Contraindications for Operative Intervention
-
Absolute Contraindications:
- Patient Unfit for Surgery: Severe hemodynamic instability, uncontrolled sepsis, major coagulopathy, or other life-threatening conditions precluding safe anesthesia and surgery. Resuscitation takes precedence.
- Irreversible Limb Ischemia: Prolonged ischemia (typically >6-8 hours warm ischemia) often renders limb salvage futile, necessitating primary amputation.
- Lack of Necessary Resources/Expertise: Performing complex procedures without the requisite surgical skill, equipment, or post-operative care capability is unethical and counterproductive.
-
Relative Contraindications:
- Extensive Contamination/Devitalized Tissue: May necessitate serial débridements and delayed definitive closure/fixation rather than immediate complex reconstruction.
- Mass Casualty Situations: Triage decisions may dictate non-operative management for less severe injuries to prioritize resources for critically injured patients.
- High Risk of Recurrent Infection: In chronic, multi-drug resistant osteomyelitis, long-term suppression or amputation might be considered.
- Severe Comorbidity: Patients with severe, uncontrolled comorbidities (e.g., severe cardiac disease, end-stage renal disease, uncontrolled diabetes) may have significantly increased surgical risk, warranting a careful risk-benefit analysis.
Operative vs. Non-Operative Indications: A Summary Table
| Condition/Injury | Operative Indications | Non-Operative Indications |
|---|---|---|
| Acute Fractures | ||
| Open Fractures | All grades (Gustilo-Anderson I-III) require urgent débridement and stabilization. | None (Débridement and stabilization are mandatory. Definitive fixation may be delayed). |
| Closed Fractures | Displaced, unstable, intra-articular fractures (e.g., femoral neck, tibial plateau, pilon, displaced radius/ulna, unstable ankle). Fractures with neurovascular compromise or impending skin compromise. | Stable, non-displaced fractures. Fractures in patients unfit for surgery where non-operative management does not significantly worsen prognosis (e.g., undisplaced humeral shaft, stable isolated fibula). |
| Compartment Syndrome | Clinical diagnosis mandates immediate fasciotomy. | None (Urgent surgical emergency). |
| Vascular/Nerve Injury | Vascular injury associated with fracture (limb ischemia). Acute nerve transection or entrapment. | Stable vascular injuries without ischemia (rare). Neuropraxia/axonotmesis without complete transection, amenable to observation and electrodiagnostic monitoring. |
| Chronic/Neglected Conditions | ||
| Malunion | Symptomatic malunion causing pain, functional deficit, or secondary joint degeneration. | Asymptomatic malunion with minimal or no functional impairment. |
| Nonunion | Symptomatic nonunion (pain, instability, deformity, progressive disability). Infected nonunion (requires débridement, stabilization, and infection control). | Asymptomatic nonunion in a non-weight-bearing bone, with good functional adaptation, especially in patients with high surgical risk. |
| Chronic Osteomyelitis | Active infection with necrotic bone, sequestra, involucrum formation. | Suppression therapy for medically fragile patients where radical surgery is contraindicated, or for quiescent disease not causing active symptoms. |
| Congenital/Developmental Deformities (e.g., Clubfoot, DDH in older children) | Significant functional impairment or progressive deformity in older children/adolescents. | Mild deformities responsive to conservative measures (e.g., serial casting for very young clubfoot, bracing for mild DDH, though these are often neglected in crisis settings until requiring surgery). |
| Contractures | Severe contractures limiting range of motion and function, causing pain or skin breakdown. | Mild contractures amenable to physical therapy and stretching. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical for successful orthopedic outcomes, especially in challenging environments where resources may be limited and surgical time often constrained.
Pre-Operative Planning
-
Patient Assessment & Resuscitation:
- ATLS Principles: For trauma patients, adhere to Advanced Trauma Life Support (ATLS) protocols: primary survey (Airway, Breathing, Circulation, Disability, Exposure), resuscitation, and secondary survey. Address life-threatening injuries first.
- Hemodynamic Stability: Ensure patient is adequately resuscitated (fluid, blood products if available and indicated) before embarking on definitive orthopedic procedures.
- Nutritional Status: Assess and optimize, if possible, especially for chronic conditions and nonunions, as malnutrition significantly impairs healing and increases infection risk.
- Coagulopathy Management: Correct any coagulopathies.
- Tetanus Prophylaxis: Crucial for open fractures and contaminated wounds. Administer tetanus toxoid and tetanus immunoglobulin as indicated.
- Antibiotic Prophylaxis: Administer broad-spectrum intravenous antibiotics pre-incision for all open fractures and many elective orthopedic procedures, typically a first or second-generation cephalosporin, with additional coverage for Gram-negative organisms or anaerobes if specific contamination (e.g., farm injury, gross fecal contamination) is suspected. For open fractures, antibiotics should be administered as soon as possible, ideally within 3 hours of injury.
-
Imaging Review:
- Plain Radiographs: Essential for initial assessment, evaluating fracture pattern, displacement, comminution, and bone loss. Obtain at least two orthogonal views.
- Advanced Imaging (if available): CT scans provide detailed information on articular involvement, complex fracture patterns, and bone defects, aiding surgical planning. MRI is valuable for soft tissue injuries, occult fractures, or early osteomyelitis but rarely available in austere settings for acute trauma.
-
Surgical Strategy & Implants:
- Definitive Plan: Determine the optimal surgical approach, fixation method (external fixator, IM nail, plate), and any auxiliary procedures (e.g., débridement, bone grafting, soft tissue coverage).
- Damage Control Orthopedics (DCO): For poly-trauma or severely ill patients, a staged approach is often necessary, prioritizing temporary stabilization (e.g., external fixation) followed by definitive fixation once the patient's physiological status has improved.
- Availability of Implants: Critical to confirm the availability of necessary implants and instruments. Flexibility in implant choice may be required.
- Contingency Planning: Always have a backup plan for potential intraoperative challenges (e.g., inability to achieve reduction, implant failure, unexpected bone loss).
-
Wound Management Plan (for Open Fractures):
- Débridement: Plan for thorough débridement of devitalized tissue (skin, subcutaneous fat, fascia, muscle, bone).
- Irrigation: Large volumes of saline irrigation.
- Soft Tissue Coverage: Consider options for delayed primary closure, skin grafting, or local/regional flap coverage. Serial débridements are often necessary before definitive soft tissue closure.
Patient Positioning
Correct patient positioning is paramount for optimal surgical exposure, preventing iatrogenic injury, and ensuring patient safety throughout the procedure.
-
General Principles:
- Airway Management: Secure and protected.
- Pressure Point Padding: Meticulously pad all bony prominences (heels, sacrum, occiput, elbows, knees) to prevent pressure sores.
- Neurovascular Protection: Ensure no undue pressure or stretch on nerves (brachial plexus, ulnar, common peroneal, sciatic) or vessels.
- Sterile Field: Ensure the entire surgical field can be adequately prepped and draped, leaving sufficient access for the planned approach and potential extensions.
- Monitoring Access: Ensure unimpeded access for anesthesia monitoring and interventions.
-
Common Positions for Orthopedic Trauma:
-
Supine:
- Applications: Lower extremity fractures (femur, tibia, ankle, foot), upper extremity (humerus, forearm, hand), pelvic fractures.
- Specifics: On a standard operating table or a fracture table (for traction-assisted reductions, e.g., femoral nailing). For hip fractures, traction can be applied to the affected leg while the contralateral leg is flexed and abducted. Arms are typically tucked or abducted on arm boards.
- Considerations: Head neutral, pressure points padded, maintain lumbar lordosis with a roll if needed.
-
Lateral Decubitus:
- Applications: Proximal femur (trochanteric/subtrochanteric), femoral shaft (less common than supine for nailing), glenohumeral joint, some forearm fractures.
- Specifics: Patient on unaffected side. Axillary roll to protect brachial plexus. Pillows between knees. Secure with hip and shoulder restraints.
- Considerations: Ensure stability, adequate padding, monitor dependent arm and leg.
-
Prone:
- Applications: Posterior approaches to the spine, calcaneus fractures, posterior ankle approaches, posterior thigh/hip.
- Specifics: Torso rolls to elevate chest and pelvis, allowing abdominal breathing and reducing vena caval compression. Head in a well-padded doughnut or prone headrest.
- Considerations: Meticulous airway management, careful padding of eyes, ears, and genitalia.
-
Beach Chair (Semi-Fowler):
- Applications: Shoulder surgery.
- Specifics: Torso elevated 45-70 degrees, knees flexed. Head secured.
- Considerations: Risk of cerebral hypoperfusion; close monitoring of blood pressure.
-
-
Positioning for External Fixation:
- Often performed in supine or lateral position on a radiolucent table to allow fluoroscopy access.
- The limb should be supported to allow reduction maneuvers and pin insertion without obstruction.
- Care is taken to position the limb such that pin insertion trajectories are clear and potential soft tissue coverage (if planned) is not compromised.
Detailed Surgical Approach / Technique
Addressing acute traumatic limb injuries and chronic neglected musculoskeletal conditions in resource-limited settings necessitates a pragmatic yet principled surgical approach. The cornerstone of effective management revolves around meticulous débridement, appropriate fracture stabilization, infection control, and soft tissue coverage.
General Principles for Trauma and Infection Management
-
Débridement: The "Orthopedic Oncologist's Principle":
- Concept: Remove all devitalized, contaminated, or infected tissue – "radical débridement." This is the single most important step in preventing and treating infection in open fractures and osteomyelitis.
-
Technique:
- Extend the wound longitudinally to visualize the entire zone of injury.
- Systematically remove all foreign bodies.
- Excise non-viable skin, subcutaneous tissue, fascia, and muscle until healthy, bleeding tissue is encountered. Non-contracting, non-bleeding muscle is dead.
- Identify and remove all non-viable bone fragments (sequestra in osteomyelitis, loose fragments devoid of periosteal attachment in trauma). Preserve vital bone.
- Aggressively débride the wound margins.
- Serial Débridements: Often, a single débridement is insufficient. "Second-look" surgeries within 24-72 hours are common for grossly contaminated or high-energy open fractures to ensure complete removal of devitalized tissue.
-
Irrigation:
- Principle: High-volume, low-pressure pulsatile lavage (6-9 liters for Gustilo-Anderson Type III fractures).
- Fluid: Isotonic saline is preferred. The addition of antibiotics or antiseptics (e.g., povidone-iodine) is controversial and lacks consistent evidence for superior outcomes over saline alone, and can be cytotoxic to cells.
- Goal: Physically remove particulate matter, bacteria, and tissue debris.
-
Stabilization:
-
External Fixation (Ex-Fix):
- Indications: Primary stabilization for most open fractures (especially Gustilo-Anderson Type II/III), polytrauma patients requiring damage control, highly contaminated wounds, and when definitive internal fixation is delayed. Also used for bone transport or correction of deformity (e.g., Ilizarov).
-
Technique (e.g., Tibial Ex-Fix):
-
Pin Placement:
- Proximal Tibia: Anteromedial surface, 1-2 cm medial to the tibial crest, aiming away from the patellar tendon and neurovascular structures. Two pins placed perpendicular to the long axis of the bone, engaging both cortices.
- Distal Tibia: Anteromedial surface, careful to avoid tendons and neurovascular bundles.
- Calcaneus/Metatarsals: For ankle spanning frames, a calcaneal pin can be inserted from lateral to medial, avoiding the posterior neurovascular bundle.
- Frame Assembly: Connect pins with carbon fiber or metal rods. Achieve initial reduction and compression/distraction as needed. Ensure sufficient distance between the frame and skin to allow for swelling and wound care.
- Advantages: Minimally invasive, preserves soft tissue envelope, allows for repeated wound care and access, adjustable.
- Disadvantages: Pin tract infection, discomfort, patient compliance, less robust stability than definitive internal fixation in some cases.
-
Pin Placement:
-
Intramedullary Nailing (IMN):
- Indications: Diaphyseal fractures of the femur and tibia (closed or low-grade open fractures once soft tissues are deemed clean). Humerus.
-
Technique (e.g., Tibial IMN):
- Entry Point: Proximal tibia, infrapatellar approach (patellar tendon splitting or paratendinous). Anteromedial entry point is common.
- Reaming: Ream medullary canal incrementally to match nail diameter. Reaming promotes cortical vascularity and creates bone graft material.
- Nail Insertion: Insert the nail carefully to bridge the fracture.
- Locking: Proximal and distal locking screws for rotational and axial stability.
- Advantages: Load sharing, high stability, early weight-bearing, minimal soft tissue disruption (if closed technique).
- Disadvantages: Risk of infection in open fractures, technical demands, potential for knee pain (proximal tibia).
-
Plate Fixation:
- Indications: Articular fractures, periarticular fractures, selected diaphyseal fractures, nonunions, malunions.
- Technique: Open reduction and internal fixation (ORIF). Anatomical reduction of articular surfaces. Application of plates (e.g., locking compression plates, LC-DCP) and screws according to biomechanical principles (compression, neutralization, bridge plating).
- Advantages: Direct reduction, excellent for articular reconstruction, strong fixation.
- Disadvantages: Requires extensive soft tissue dissection, higher risk of infection in contaminated wounds, greater implant prominence, potential for stress shielding.
-
External Fixation (Ex-Fix):
Soft Tissue Coverage
- Delayed Primary Closure: After serial débridements, if the wound is clean with no signs of infection and viable soft tissue is available, the wound can be closed directly within 3-7 days.
- Skin Grafting: For superficial soft tissue defects with a healthy vascularized bed, split-thickness skin grafts (STSG) or full-thickness skin grafts (FTSG) can be applied.
- Local/Regional Flaps: For larger defects, exposed bone, or tendon, local muscle or fasciocutaneous flaps provide robust, vascularized coverage. Examples include the gastrocnemius flap for proximal tibia, soleus flap for mid-tibia, and free tissue transfer (if microsurgical expertise and equipment are available, which is rare in austere settings).
- Wound Vac/Negative Pressure Wound Therapy (NPWT): If available, NPWT can promote granulation tissue formation, reduce edema, and manage wound exudate, preparing the wound for definitive closure or grafting.
Management of Chronic Osteomyelitis
Chronic osteomyelitis, often a sequela of neglected open fractures, demands aggressive surgical intervention.
- Radical Débridement: The most critical step. Remove all necrotic bone (sequestrum), infected granulation tissue, and any foreign material. Use a rongeur or osteotome to expose healthy, bleeding bone.
-
Dead Space Management:
- Antibiotic-loaded Cement Beads (PMMA): Polymethlymethacrylate beads impregnated with high doses of local antibiotics (e.g., tobramycin, vancomycin) can fill dead space and deliver high local concentrations of antibiotics.
- Muscle Flaps: Vascularized muscle flaps bring in healthy tissue and improve local blood supply and oxygenation, enhancing antibiotic delivery and host immunity.
- Bone Grafting: Autogenous cancellous bone grafting is used to fill residual bone defects after infection is controlled and soft tissue coverage is achieved.
- Stabilization: Stable fixation (often with external fixators or IM nails after débridement) is necessary for bone healing.
- Antibiotic Therapy: Prolonged systemic antibiotics (intravenous initially, then oral) for 6 weeks or more, guided by culture and sensitivity results.
Complications & Management
Orthopedic procedures in humanitarian crisis settings are inherently associated with higher complication rates compared to elective surgery in well-resourced environments. Factors such as delayed presentation, severe initial injury (e.g., high-energy open fractures), malnutrition, poor hygiene, and limited access to diagnostics, advanced surgical techniques, and post-operative care all contribute to this elevated risk. Proactive recognition and aggressive management are critical for salvage.
Common Complications and Salvage Strategies
| Complication | Incidence (Approx. in crisis settings) | Salvage Strategies |
|---|---|---|
| Deep Surgical Site Infection (SSI) / Chronic Osteomyelitis | High (20-50% for high-grade open fractures) |
Early Recognition:
Fever, localized pain, erythema, purulent discharge, wound dehiscence.
Aggressive Surgical Débridement: Repeatedly, removing all necrotic and infected tissue (bone, soft tissue). Take cultures. Targeted Antibiotics: Based on culture and sensitivity, prolonged course (e.g., 6 weeks IV then oral). Dead Space Management: Antibiotic-loaded PMMA beads, local muscle flaps. Stable Fixation: Often requires conversion to external fixation or revision internal fixation. Bone Transport/Shortening: For significant bone loss. Amputation: As a last resort for uncontrolled, life-threatening infection or unsalvageable limb. |
| Nonunion | High (10-30% for open diaphyseal fractures) |
Definition:
Absence of healing by 6-9 months, or no progression of healing for 3 consecutive months.
Diagnosis: Clinical instability, pain, persistent fracture line on radiographs. Management: * Hypertrophic Nonunion: Stable fixation (e.g., exchange nailing, larger diameter IM nail, plate with compression). * Atrophic Nonunion: Requires débridement of fibrous tissue, bone grafting (autograft from iliac crest/distal femur/proximal tibia), and stable fixation. * Infected Nonunion: Address infection first with débridement and antibiotics, then stabilize and graft if necessary. Staged approach often required. |
| Malunion | Common (due to suboptimal reduction/fixation) |
Definition:
Fracture healing in an unacceptable anatomical position (angulation, rotation, shortening, translation) causing pain, functional impairment, or cosmetic deformity.
Management: * Asymptomatic/Mild: Observation, bracing. * Symptomatic/Severe: Corrective osteotomy (re-fracture at the site of malunion), acute correction, and stable internal fixation (plate, IM nail). Gradual correction with external fixator (e.g., Ilizarov) for large deformities. |
| Neurovascular Injury | Variable (depends on injury mechanism/location) |
Diagnosis:
Clinical (absent pulses, pallor, paresthesias, paralysis). Doppler ultrasound, angiography (if available).
Vascular Injury: Urgent exploration, repair (primary repair, interposition graft), or bypass. Fracture stabilization (often external fixation) to protect repair. Nerve Injury: * Neurapraxia/Axonotmesis: Observation, bracing, physical therapy. * Neurotmesis (Transection): Primary repair (if acute and clean wound) or delayed nerve grafting. Tendon Injury: Primary repair, tendon transfer for chronic deficits. |
| Compartment Syndrome | Risk with high-energy trauma, revascularization |
Diagnosis:
Clinical (pain out of proportion, pain with passive stretch, paresthesias, tenseness of compartment). Direct compartment pressure measurement (if available).
Management: Urgent four-compartment fasciotomy (lower leg), two-compartment (forearm). Delayed wound closure. Failure to diagnose promptly leads to irreversible muscle necrosis and nerve damage. |
| Amputation | For unsalvageable limbs (Gustilo-Anderson IIIC, severe crush, uncontrolled infection) |
Decision Factors:
MESS score (Mangold Extremity Salvage Score), prolonged ischemia, massive tissue loss, uncontrollable infection, patient factors.
Technique: Preserve maximum limb length consistent with healthy soft tissue coverage. Optimize for prosthetic fitting. Post-amputation Management: Stump care, pain management, physical therapy, prosthetic fitting, psychosocial support. |
| Pin Tract Infection | Common with external fixation (10-60%) |
Diagnosis:
Erythema, pain, discharge at pin site.
Management: * Minor: Local wound care (daily cleaning with chlorhexidine/saline), oral antibiotics if signs of cellulitis. * Moderate: Pin removal and replacement through a new tract, systemic antibiotics. * Severe/Deep: Débridement, IV antibiotics, conversion to alternative fixation if persistent. |
| Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) | Risk in immobilized trauma patients |
Prophylaxis:
Mechanical (foot pumps, compression stockings), pharmacological (low molecular weight heparin, if not contraindicated).
Diagnosis: Clinical suspicion, Doppler ultrasound. Management: Anticoagulation. |
| Psychosocial Impairment | High (PTSD, depression, anxiety, grief, body image issues) |
Diagnosis:
Clinical assessment, screening tools.
Management: Counseling, support groups, family involvement, referral to mental health professionals (if available). Integrated approach to rehabilitation. |
General Principles for Complication Management in Austere Settings
- Prevention: The best management is prevention through meticulous surgical technique, aggressive débridement, appropriate antibiotic prophylaxis, and sterile environment.
- Early Recognition: High index of suspicion for developing complications. Regular wound checks, clinical assessments, and prompt investigation.
- Adaptation: Be prepared to adapt management strategies based on available resources. For example, local antibiotic delivery systems may be improvised, or simpler fixation methods preferred.
- Collaboration: Work closely with other medical professionals, rehabilitation specialists, and local community health workers.
- Documentation: Accurate and detailed documentation is crucial for continuity of care, especially in mobile surgical teams or when transferring patients.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an indispensable component of orthopedic care, particularly for patients in crisis zones, whose functional recovery profoundly impacts their ability to regain independence and reintegrate into society. The objective is to optimize functional outcomes, prevent secondary complications, and mitigate long-term disability, acknowledging that resources for rehabilitation are often as scarce as those for acute surgery.
Phases of Rehabilitation
-
Early Mobilization and Pain Management (Acute Post-Operative Phase):
- Pain Control: Essential for facilitating early movement. Utilize multimodal analgesia (NSAIDs, acetaminophen, opioids, regional blocks).
- Wound Care: Meticulous wound care to prevent infection. Regular dressing changes, monitoring for signs of infection (erythema, swelling, discharge, fever).
- Edema Control: Elevation, compression (elastic bandages), gentle massage to reduce swelling.
- Early Range of Motion (ROM): Passive or active-assisted ROM for adjacent joints to prevent stiffness and contractures, provided surgical stability allows. This might include gentle ankle pumps, knee flexion/extension (for non-femoral/tibial injuries), and finger movements.
- Muscle Activation: Isometric exercises to maintain muscle tone without joint movement.
-
Immobilization and Protected Weight-Bearing Phase:
- Protection of Surgical Repair: Depending on the fracture and fixation method, the limb may be immobilized in a cast, splint, or external fixator. Strict adherence to weight-bearing precautions (non-weight-bearing, partial weight-bearing, weight-bearing as tolerated) is paramount.
- Progressive Mobilization: Once initial healing is evident and pain subsides, gradual progression of ROM and strengthening exercises is initiated.
- Weight-Bearing Progression: Follow surgeon's orders for gradual weight-bearing, often starting with touch-down weight-bearing using assistive devices.
- Assistive Devices: Crutches, walkers, or wheelchairs are critical for safe mobility. Instruction on proper use, gait training, and safety is essential.
-
Strengthening and Functional Training Phase:
- Muscle Strengthening: Progressive resistance exercises to rebuild muscle strength and endurance in the affected limb and surrounding musculature.
- Proprioception and Balance Training: Crucial for regaining stability, especially for lower extremity injuries.
- Functional Activities: Incorporate activities of daily living (ADLs) and instrumental ADLs (IADLs) into therapy. This might involve tasks related to self-care, household chores, or vocational activities.
- Gait Training: Refinement of gait pattern, often with increasing distance and terrain challenges.
- Occupational Therapy (OT): Addresses fine motor skills, adaptive equipment, and strategies for resuming work or daily tasks.
-
Long-Term Follow-up and Psychosocial Support:
- Adherence to Protocols: Emphasize the importance of patient and family adherence to rehabilitation protocols.
- Addressing Complications: Continue to monitor for delayed complications such as nonunion, malunion, infection, or chronic pain.
- Assistive Devices and Prosthetics: For patients with limb loss (amputations) or severe functional deficits, appropriate prosthetic fitting and training are life-changing. This requires collaboration with prosthetists and orthotists, which can be challenging in humanitarian settings.
- Psychosocial Support and Counseling: Trauma and disability in conflict zones carry immense psychological burdens (PTSD, depression, anxiety, grief, body image issues). Providing access to counseling, support groups, and family education is vital for holistic recovery and social reintegration. This directly addresses the seed content's mention of "Psychosocial support and counseling."
- Economic Empowerment and Livelihood Opportunities: Facilitating a return to work or engaging in new vocational training programs is critical for restoring dignity and financial independence. This directly relates to the seed content's mention of "Economic empowerment and livelihood opportunities."
- Outcome Tracking: Establishing methods to track patient outcomes and functional improvement is important for program evaluation and continuous quality improvement, even if only basic metrics are collected.
![]()
This pixel, while technically a tracking image, conceptually represents the need for data collection and feedback loops in humanitarian medical programs to understand impact and optimize resource allocation.
Challenges in Rehabilitation in Crisis Settings
- Limited Resources: Scarcity of trained physical therapists, occupational therapists, prosthetists, and specialized equipment.
- Geographic Barriers: Difficulty for patients to access rehabilitation centers due to displacement, insecurity, or lack of transport.
- Cultural and Social Stigma: Disability can carry social stigma, affecting patient participation and reintegration.
- Malnutrition: Undermines healing and physical strength needed for rehabilitation.
- Psychological Trauma: Exacerbates physical pain and hinders motivation for rehabilitation.
- Continuity of Care: Frequent patient displacement and staff rotation make long-term follow-up challenging.
Despite these challenges, innovative and adaptable rehabilitation strategies are crucial. This includes training local community health workers in basic rehabilitation techniques, utilizing locally available materials for assistive devices, and integrating rehabilitation into primary healthcare services where possible.
Summary of Key Literature / Guidelines
Orthopedic care in humanitarian crises draws upon foundational principles of trauma surgery and infection control, adapted to the severe constraints of resource-limited environments. While specific, high-level evidence from conflict zones is often scarce, established guidelines from international bodies provide critical frameworks.
Trauma Management Guidelines
- Advanced Trauma Life Support (ATLS): Developed by the American College of Surgeons, ATLS provides a standardized, systematic approach to the assessment and management of the severely injured patient. Its principles of primary and secondary surveys, rapid resuscitation, and identification of life-threatening injuries are universally applicable, especially in mass casualty situations.
- WHO Emergency Trauma Care (ETC): The World Health Organization (WHO) offers guidelines for trauma care in emergencies, emphasizing triage, stabilization, and initial management within resource-constrained settings. These guidelines advocate for the use of simple, effective interventions that can be implemented with limited infrastructure.
-
International Committee of the Red Cross (ICRC) War Surgery Manuals:
The ICRC has extensive experience in conflict zones and provides practical, evidence-based guidance on war surgery. Key principles include:
- Aggressive Débridement: The most crucial step in preventing infection in projectile and blast injuries.
- Delayed Primary Closure: Wounds are often left open or closed secondarily after serial débridements.
- External Fixation: Preferred for initial stabilization of open fractures due to its versatility and minimal additional soft tissue disruption.
- Antibiotic Prophylaxis: Essential for all open wounds.
Open Fracture Management
-
Gustilo-Anderson Classification:
The standard for classifying open fractures, guiding management strategies, particularly regarding débridement, antibiotic duration, and risk of infection.
- Type I: Minimal soft tissue damage, wound <1 cm.
- Type II: Moderate soft tissue damage, wound >1 cm, without extensive devitalized tissue.
-
Type III:
Extensive soft tissue damage, high-energy injury.
- IIIA: Adequate soft tissue coverage, high-energy.
- IIIB: Extensive soft tissue loss requiring local or free flap coverage.
- IIIC: Arterial injury requiring repair, regardless of soft tissue damage.
- Antibiotic Regimens: Consensus typically recommends a first-generation cephalosporin (e.g., Cefazolin) for Type I and II. For Type III, an aminoglycoside (e.g., Gentamicin) is added for Gram-negative coverage, and penicillin for clostridial coverage if gross contamination is present. Duration varies, often 24-72 hours for Type I/II and up to 72 hours for Type III post-débridement.
- Timeliness of Débridement: While "within 6 hours" was a traditional dogma, current literature suggests that débridement within 12-24 hours may not significantly worsen outcomes, particularly for lower-grade open fractures, given adequate initial resuscitation and antibiotic administration. However, earlier débridement remains ideal, especially for high-grade injuries.
Osteomyelitis Management
- Cierny-Mader Classification: Describes osteomyelitis based on anatomical involvement (medullary, superficial, localized, diffuse) and physiological status of the host (A: normal, B: compromised, C: severely compromised). This classification helps guide treatment aggressiveness.
- Surgical Débridement: Radical débridement of infected and necrotic bone remains the cornerstone.
- Antibiotic Therapy: Long-term, culture-specific systemic antibiotics (typically 4-6 weeks IV, followed by oral if appropriate). Local antibiotic delivery (PMMA beads) is an important adjunct.
- Dead Space Management: Essential to prevent recurrence. Muscle flaps are often preferred for their vascularity and ability to fill defects.
External Fixation Principles
- Pin Site Care: Crucial to prevent pin tract infections, which can lead to loosening and deep infection. Daily cleaning, minimizing skin tension at pin sites, and appropriate frame construction are vital.
- Frame Stability: Influenced by pin diameter, number of pins, pin spread, bone-to-bar distance, and rod configuration. Uniplanar frames are simpler but less stable than biplanar or circular frames.
- Bone Transport and Deformity Correction: Ilizarov techniques are invaluable for managing large bone defects and complex deformities, providing gradual correction and stimulating osteogenesis.
Rehabilitation Guidelines
- WHO Rehabilitation Guidelines: Emphasize community-based rehabilitation (CBR) in low-resource settings, training local personnel, and utilizing simple, locally adaptable technologies.
- ICRC Physical Rehabilitation Programme: Provides extensive guidance on prosthetic and orthotic services, physical therapy, and vocational training for war-wounded patients, with a focus on sustainable local capacity building.
Challenges in Applying Guidelines in Crisis Settings
- Limited Diagnostics: Lack of advanced imaging (CT, MRI), microbiology labs for culture and sensitivity, and blood banks.
- Infrastructure Damage: Operating theaters, sterilization equipment, and power supply are often unreliable.
- Lack of Trained Personnel: Shortage of orthopedic surgeons, anesthetists, nurses, and rehabilitation specialists.
- Supply Chain Disruptions: Inconsistent availability of implants, antibiotics, and surgical consumables.
- Security Issues: Impeding patient access, staff safety, and delivery of supplies.
Despite these challenges, adherence to fundamental orthopedic principles, coupled with adaptability and innovation, remains critical to delivering the best possible care for patients in urgent need within these complex humanitarian environments. The emphasis shifts from ideal to optimal, striving for functional outcomes that improve quality of life within the prevailing constraints.