Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 42-year-old woman reports that she has low back pain and had a transient loss of consciousness after falling off a horse. She denies having neck pain but notes that she was involved in a motor vehicle accident 2 years ago and had neck pain at that time. Examination reveals full range of motion of the neck and no localized tenderness. The neurologic examination is normal. A lateral radiograph of the cervical spine is obtained. Figures 41a and 41b show CT and MRI scans. What is the most likely diagnosis?
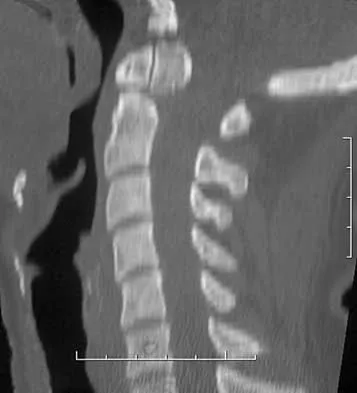
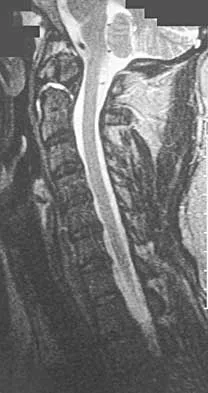
Explanation
The examination findings do not correlate with an acute injury (full range of cervical motion and the absence of pain). Radiographically, the fracture appears old based on the smooth contour of the fracture fragments and the absence of soft-tissue swelling. Flexion-extension radiographs can be obtained to determine potential instability; if present, stabilization and fusion should be considered. Schatzker J, Rorabeck CH, Waddell JP: Non-union of the odontoid process: An experimental investigation. Clin Orthop 1975;108:127-137.
Question 2
A study was conducted in 500 patients to measure the effectiveness of a new growth factor in reducing healing time of distal radial fractures. The authors reported that average healing time was reduced from 9.2 to 8.9 weeks (P < 0.0001). Because the difference was highly statistically significant, they recommended routine clinical use of this drug despite its high cost. A more appropriate interpretation of these results is that they are
Explanation
The results are statistically significant (at the arbitrary level of P < 0.05). That is, they indicate a probability of only 1/10,000 that the observation that the drug is effective in reducing healing time by 0.3 weeks occurred by chance selection of the study subjects. However, because the statistical power of a study increases with the number of subjects included (sample size), a difference that is trivial clinically can occur with a very high level of statistical significance (a very small P-value) if enough patients are included in the study. Because of this, the P-value alone, no matter how small, does not establish clinical significance or importance. Rather, the clinical significance of the observed difference must be assessed taking into consideration the medical importance of the difference if it is, in fact, true in the general population. In this example, the reduction in healing time of only a few days is probably clinically unimportant, particularly if the use of the new growth factor is expensive, complex, and/or has substantial side effects.
Question 3
An obese 56-year-old woman with hypertension has had posterior heel pain for the past 6 months. She also notes some enlargement over the posterior aspect of the heel. Examination reproduces pain with palpation at the insertion of the Achilles tendon. A lateral radiograph is shown in Figure 45. What is the most likely diagnosis?
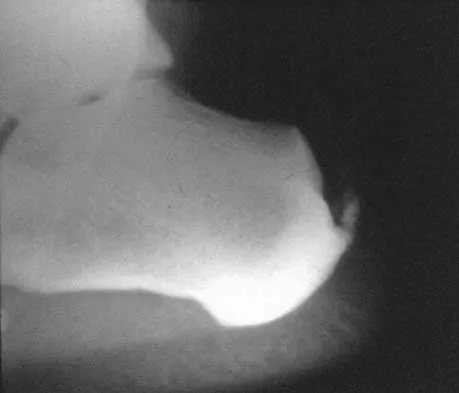
Explanation
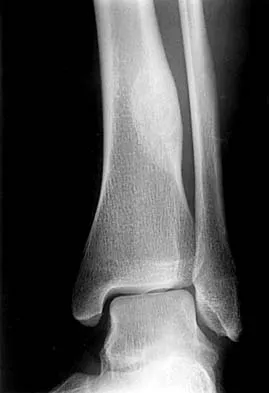
The lateral radiograph shows a traction spur consistent with tendinopathy of the Achilles tendon. There is no displacement of the spur to suggest a rupture of the Achilles tendon, and os trigonum is not seen on the radiograph. The examination findings are not consistent with nerve entrapment. Schepsis AA, Wagner C, Leach RE: Surgical management of Achilles tendon overuse injuries: A long-term follow-up study. Am J Sports Med 1994;22:611-619.
Question 4
Figures 1a and 1b show the clinical photograph and oblique radiograph of a 52-year-old man who has plantar first metatarsal pain. A felt pad in the shoe proximal to the area of pain has failed to provide relief. Management should now consist of
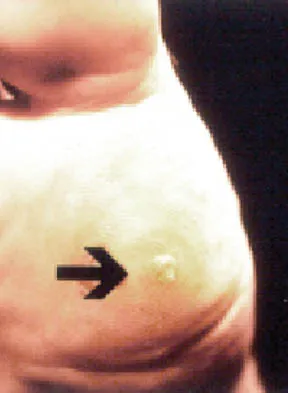
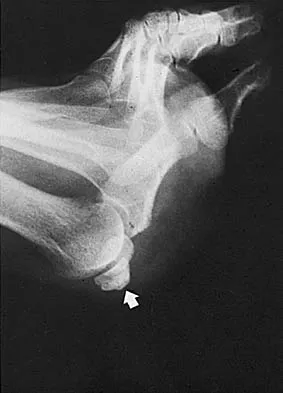
Explanation
The patient has a discrete callus that overlies a prominent medial sesamoid. Calluses typically occur in response to increased pressure on the skin. Initial treatment should be directed at reducing local pressure with a felt pad. Sesamoid shaving is indicated if the felt pad fails to provide relief. Sesamoidectomy should be reserved for refractory callus given the potential complications of transfer metatarsalgia or callus and hallux valgus. A first metatarsal dorsiflexion osteotomy is more appropriate for a diffuse callus that fails to respond to nonsurgical management. Cryoablation and topical salicylic acid are appropriate for plantar warts, which have a rougher appearance with multiple, small black spots in the lesion. Mann RA, Wapner KL: Tibial sesamoid shaving for treatment of intractable plantar keratosis. Foot Ankle 1992;13:196-198.
Scientific References
-
:
Question 5
What is the most common complication following total disk arthroplasty in the lumbar spine?
Explanation
In a midterm (7 to 11 years) follow-up study of lumbar total disk arthroplasty, 5 of 55 patients had transient radicular leg pain without evidence of nerve root compression. Implant migration is rare. Deep venous thrombosis, incisional hernia, and retrograde ejaculation are less common complications of disk arthroplasty.
Question 6
A knock-out mouse for the Vitamin D receptor has which of the following phenotypes?
Explanation
A knock-out mouse to the Vitamin D receptor would cause loss of vitamin D function, resulting in rickets. Renal failure would not occur; although Vitamin D is converted from 25 (OH) D to 1,25 (OH) D in the kidney, the active hormone acts on the gut and bone. Osteopetrosis can be seen as the phenotype for the c fos knock-out mouse; the Jansen-type metaphyseal dysplasia phenotype results from overactivation of the PTH/PTHrp receptor. Although compensatory hyperparathyroidism would occur, excessive PTH would not be able to rescue the skeletal loss and instead phosphoturia and phosphotasia would result. Glowacki J, Hurwitz S, Thornhill TS, et al: Osteoporosis and vitamin-D deficiency among postmenopausal women with osteoarthritis undergoing total hip arthroplasty. J Bone Joint Surg Am 2003;85:2371-2377.
Question 7
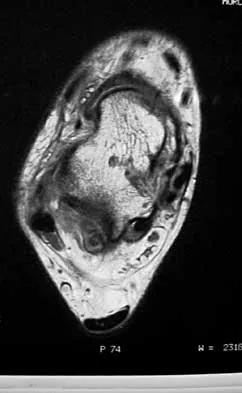
What is the most common MRI appearance of a malignant soft-tissue sarcoma?
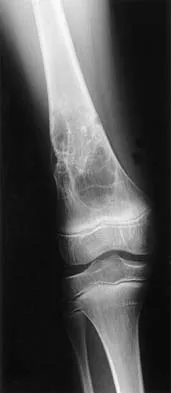
Explanation
The classic MRI appearance of a soft-tissue sarcoma is a well-defined heterogeneous mass deep to the fascia. MRI has greatly enhanced our ability to identify and characterize soft-tissue masses. In many patients, MRI is diagnostic and may obviate the need for biopsy. In other patients, it may indicate with high probability that the mass is malignant and consideration for referral can be made. A common misconception is that sarcomas are infiltrative; therefore, physicians mistakenly exclude the diagnosis of a sarcoma based on a well-defined mass seen on MRI. However, sarcomas grow centrifugally with balloon-like expansion compressing surrounding normal tissue; as such, they appear well defined. Many benign soft-tissue masses such as lipomas are similarly well defined. However, MRI is especially useful in identifying fat. Lipomas appear to be homogeneous masses with fat signal characteristics on all sequences. Ill-defined soft-tissue masses include infection, trauma, and desmoid tumors. Heterogeneity is not unique to malignant tumors but is a characteristic of soft-tissue sarcomas. Bancroft LW, Peterson JJ, Kransdorf MJ, Nomikos GC, Murphey MD: Soft tissue tumors of the lower extremities. Radiol Clin North Am 2002;40:991-1011. Berquist TH, Ehman RL, King BF, et al: Value of MR imaging in differentiating benign from malignant soft-tissue masses: Study of 95 lesions. Am J Roentgenol 1990;155:1251-1255.
Question 8
A 62-year-old man with a long history of ankylosing spondylitis has neck pain after lightly bumping his head on the wall. Examination reveals neck pain with any attempted motion; the neurologic examination is normal. Plain radiographs show extensive ankylosis of the cervical spine and kyphosis but no fracture. What is the next most appropriate step in management?
Explanation
A high level of suspicion must be given for a fracture in any patient with ankylosing spondylitis who reports neck pain, even with minimal or no trauma. The neck should be immobilized in its normal position, which is often kyphotic, and plain radiographs should be obtained. If no obvious fracture is seen, CT with reconstruction should be obtained. The placement of in-line traction can have catastrophic effects because it may malalign the spine. Brigham CD: Ankylosing spondylitis and seronegative spondyloarthropathies, in Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Raven, 1998, pp 724-727.
Question 9
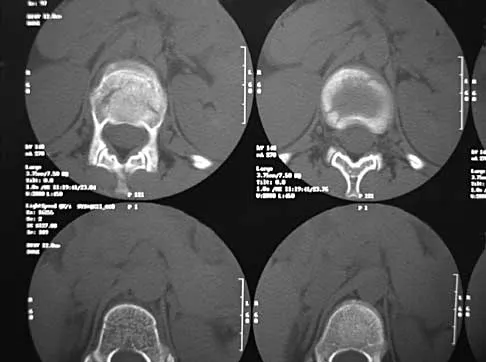
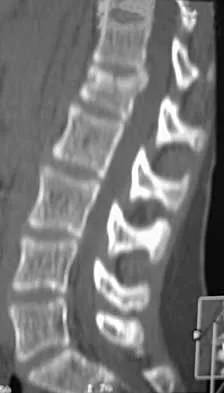
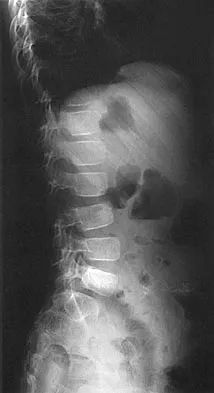
A skeletally mature 15-year-old girl who was thrown from the car in a rollover accident sustained the injuries shown in Figures 23a through 23d. Examination reveals no neurologic deficit, but the patient has moderate posterior spinal tenderness at the level of the injury. What is the most appropriate treatment?
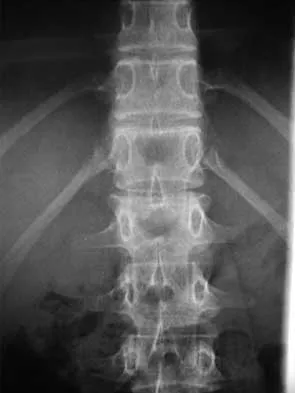
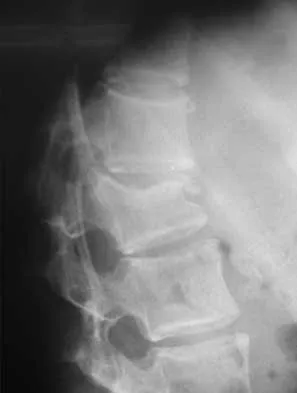
Explanation
The majority of patients with thoracolumbar burst fractures without neurologic deficit can be effectively treated with a TLSO or a hyperextension body cast. Indications for surgery are neurologic deficit and/or significant deformity (greater than 50% loss of anterior vertebral body height or marked kyphosis). Garfin SR, Vaccaro AR (eds): Orthopaedic Knowledge Update: Spine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 197-217.
Question 10
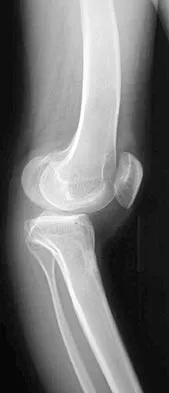
A newborn with bilateral talipes equinovarus undergoes serial manipulation and casting. What is the primary goal of manipulation?
Explanation
Manipulative treatment and casting of talipes equinovarus has become popular because of disappointing surgical results and enthusiasm for the Ponseti method of manipulation. In this technique, the primary goal is to rotate the foot laterally around a talus that is held fixed by the manipulating surgeon's hands. While the navicular may be rotated anterolaterally with this technique, the primary focus is on the calcaneus. The calcaneus is rotated laterally and superiorly, not translated. Some dorsiflexion of the calcaneus can be obtained by manipulation, but the primary focus is on the rotational relationship of the talus and calcaneus, not the degree of calcaneal dorsiflexion. Ponseti IV: Common errors in the treatment of congenital clubfoot. Int Orthop 1997;21:137-141.
Question 11
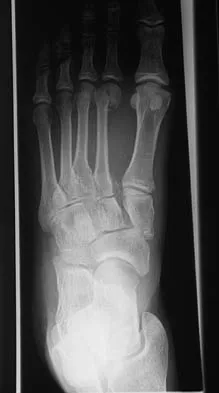
Figure 11 shows the radiograph of an otherwise healthy 22-year-old man who sustained a midfoot injury in a motor vehicle accident 9 days ago. Treatment should consist of
Explanation
The dislocation is between the medial and middle cuneiform. Although the first and second tarsometatarsal joints are aligned, there is a gap between the cuneiforms. The radiograph shows a Lisfranc dislocation variant. In a healthy active individual, open reduction and internal fixation yields the best results. The reestablishment of the normal arch and medial column support with anatomic reduction is critical to obtaining the best possible outcome from these injuries. Teng AL, Pinzur MS, Lomasney L, et al: Functional outcome following anatomic restoration of the tarsal-metatarsal fracture dislocation. Foot Ankle Int 2002;23:922-926.
Question 12
What significant structure is most at risk during a posterior approach of the Achilles tendon near its musculotendinous junction?
Explanation
The sural nerve crosses near the midline at the level of the musculotendinous junction before descending to its more lateral location distally. The saphenous nerve and vein are further medial and at less risk. The posterior tibial nerve is at risk only during deep dissection, such as harvesting flexor hallucis longus tendon graft. The plantaris muscle lies in this area but is of little clinical significance. Webb J, Moorjani N, Radford M: Anatomy of the sural nerve and its relation to the Achilles tendon. Foot Ankle Int 2000;21:475-477.
Question 13
An 8-year-old boy reports progressive difficulty with walking. Examination reveals muscle weakness, with proximal groups more affected than distal muscles. Deep tendon reflexes are within normal limits. Laboratory studies show a creatine kinase level of 7,200 IU. Based on these findings, what is the most likely diagnosis?
Explanation
Patients with Becker muscular dystrophy have an abnormality in dystrophin, but unlike patients with Duchenne muscular dystrophy, some dystrophin is present. As a result, the progression of muscle weakness is slower, with the diagnosis typically made after age 8 years. Similar to patients with Duchenne muscular dystrophy, patients with Becker muscular dystrophy have pseudohypertrophy of the calves, markedly increased creatine kinase levels, and X-linked transmission of the condition. In addition, these patients are more prone to cardiomyopathy; a condition that should be carefully evaluated if any surgery is required. Patients with spinal muscular atrophy also have proximal muscle weakness, but the onset of weakness occurs earlier in childhood. These patients also have absent deep tendon reflexes and fasciculations, but pseudohypertrophy is absent and creatine kinase levels are normal. Patients with Emery-Dreifuss dystrophy may have a similar clinical picture to Becker's muscular dystrophy, but pseudohypertrophy is absent and creatine kinase levels are only mildly elevated. In addition, neck extension, elbow flexion, and ankle equinus contractures develop at an early age. Limb girdle dystrophy is a group of progressive muscular dystrophies that is not associated with pseudohypertrophy or a significant elevation of creatine kinase levels. Guillain-Barre syndrome is a condition associated with results from postinfectious demyelination of the peripheral nerve. These patients have the acute onset of weakness, hypotonia, and areflexia; creatine kinase levels are normal. Sussman MD: Muscular dystrophy, in Fitzgerald RH, Kaufer H, Malkani AL (eds): Orthopaedics. St Louis, MO, Mosby, 2002, pp 1573-1583.
Question 14
Figure 6 shows the lateral radiograph of a 22-year-old woman who has painful Scheuermanns's kyphosis in the middle and lower thoracic spine. When planning surgical correction using instrumentation, the distal aspect of the instrumentation should ideally extend to the
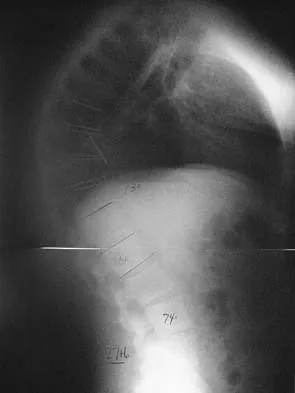
Explanation
Posterior constructs for Scheuermann's kyphosis ideally should extend from the most superior to the most inferior aspect of the Cobb angulation. However, the most distal fusion level must be in a stable or lordotic position to avoid the development of junctional kyphosis. Lowe reported that failure to incorporate the first lordotic segment of the lumbar spine is associated with a higher risk of junctional kyphosis. The first lordotic segment of the lumbar spine is typically at least one level below the distal aspect of the curve as measured by the Cobb technique and most commonly is in the upper part of the lumbar spine. Lowe TG: Scheuermann's disease. Orthop Clin North Am 1999;30:475-487.
Question 15
Figure 33 shows the CT scan of a 40-year-old man who injured his left shoulder while skiing. What structure is attached to the bony fragment?
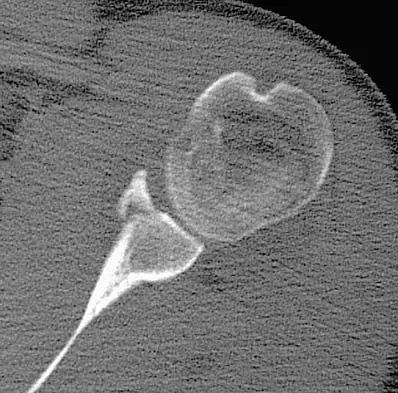
Explanation
The scan reveals a bony Bankart lesion. The anterior band of the inferior glenohumeral ligament is the major restraint to anterior translation of the humeral head and is usually injured with anterior shoulder dislocations. It inserts onto the glenoid labrum at the anteroinferior aspect of the glenoid rim. The labrum most frequently avulses from the glenoid (Bankart lesion), but occasionally the bony attachment is avulsed. O'Brien SJ, Neves MC, Arnoczky SP, et al: The anatomy and histology of the inferior glenohumeral ligament complex of the shoulder. Am J Sports Med 1990;18:449-456.
Question 16
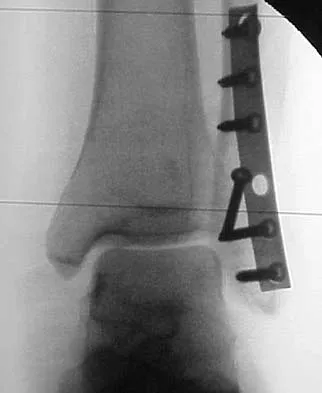
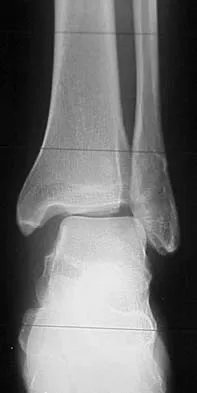
The plate seen in Figure 48a was applied to the fracture seen in Figure 48b, and is functioning in what capacity?
Explanation
A Weber type B ankle fracture occurs with a supination external rotation mechanism of injury. The fibula generally fails with a spiral fracture pattern. The lag screws provide compression, and the plate acts to neutralize rotational and angular bending forces. A buttress plate resists vertical shear forces. A tension band is used over areas that may fail in tension, such as an olecranon fracture. Compression is provided by the lag screws, and distraction is again resisted by the lag screws.
Question 17
Which of the following factors increases the risk of sciatic nerve injury in primary total hip arthroplasty (THA)?
Explanation
Injury to the sciatic nerve is a relatively rare but serious complication of THA. Dissection of the sciatic nerve is not typically done during primary THA, although the nerve can be identified during the surgical approach. An anterolateral approach to THA would not necessarily be associated with any greater incidence of sciatic nerve injury than other approaches. Screw fixation for the acetabular component is often a matter of surgeon preference. Provided that the anatomic safe zones for screw fixation (posterior inferior and posterior superior) are recognized, injury to the sciatic nerve from acetabular screws can be minimized. Restoration of anatomic length is important in primary THA. Overlengthening can result in sciatic nerve palsy. Developmental dysplasia of the hip can lead to a congenitally shortened extremity with concomitant congenital shortening of the associated neurovascular structures. Overlengthening of the extremity during THA for developmental dysplasia of the hip can lead to sciatic palsy. Osteonecrosis is not an associated risk factor for sciatic nerve palsy. DeHart MM, Riley LH Jr: Nerve injuries in total hip arthroplasty. J Am Acad Orthop Surg 1999;7:101-111.
Question 18
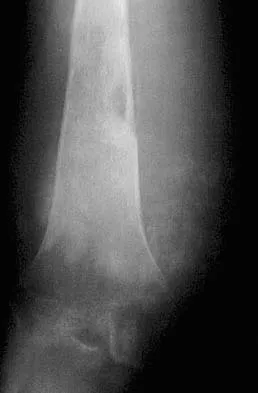
A 40-year-old man with an acetabular chondrosarcoma has a small soft-tissue mass. Treatment should consist of
Explanation
The treatment of choice for pelvic chondrosarcoma is wide resection via an internal hemipelvectomy. Chondrosarcoma requires surgical resection for control and does not respond to traditional chemotherapy or external beam radiation. Hip arthroplasty with acetabular reconstruction and curettage and cementation of the lesion are intralesional procedures that result in a higher incidence of local recurrence of tumor. Pring M, Weber KL, Unni K, Sim FH: Chondrosarcoma of the pelvis: A review of sixty-four cases. J Bone Joint Surg Am 2001;83:1630-1642.
Question 19
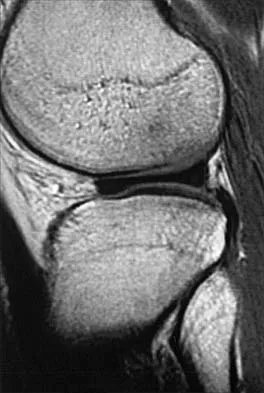
The quadrilateral space in the shoulder contains which of the following structures?
Explanation
The quadrilateral or quadrangular space of the shoulder is formed laterally by the humerus, proximally by the subscapularis (and teres minor viewed from posterior), distally by the teres major, and medially by the long head of triceps. The posterior humeral circumflex artery and axillary nerve pass through it. The axillary artery is more proximal. The radial nerve and profunda brachii pass through a triangular space more inferior. The circumflex scapular artery passes through a triangular space more medial. Hollinshead WH: Textbook of Anatomy, ed 3. Hagerstown, MD, Harper and Row, 1974, pp 205-206.
Question 20
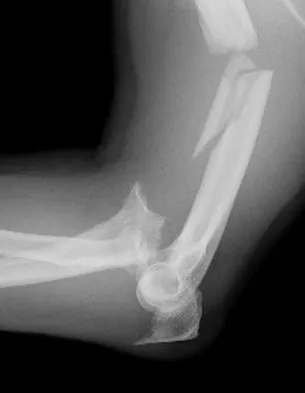
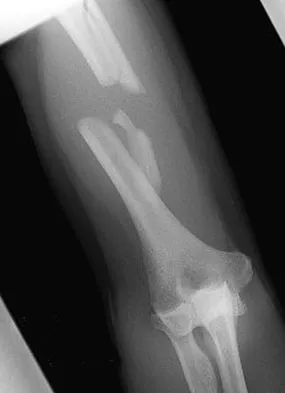
A 30-year-old man has pain in the left arm after a motor vehicle accident. His neurovascular examination is intact, and radiographs are shown in Figures 25a and 25b. What is the best course of management?
Explanation
The floating elbow is best managed with early open reduction and internal fixation of the humeral and forearm fractures, followed by early range of motion. These fractures predispose the elbow to stiffness, and early range of motion is recommended. Solomon HB, Zadnik M, Eglseder WA: A review of outcomes in 18 patients with floating elbow. J Orthop Trauma 2003;17:563-570.
Question 21
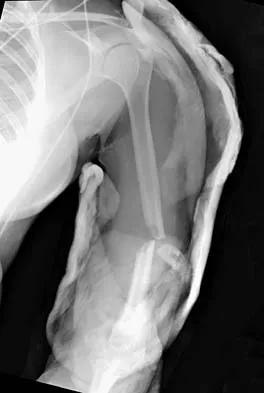
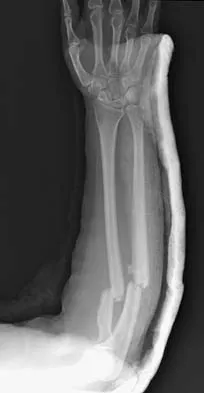
A 32-year-old woman sustained an injury to her left upper extremity in a motor vehicle accident. Examination reveals a 2-cm wound in the mid portion of the dorsal surface of the upper arm and deformities at the elbow and forearm; there are no other injuries. Her vital signs are stable, and she has a base deficit of minus 1 and a lactate level of less than 2. Radiographs are shown in Figures 9a and 9b. In addition to urgent debridement of the humeral shaft fracture, management should include
Explanation
With a severe injury to the upper extremity, the best opportunity for achieving a good functional result for a floating elbow is immediate debridement of the open fracture, followed by internal fixation of the fractures. The ability to do this depends on the patient's physiologic status. In this patient, the procedure is acceptable because she has normal vital signs and no chest or abdominal injuries, and normal physiologic parameters (base excess and lactate) show adequate peripheral perfusion. The surgical approaches will be determined by the associated injury patterns and open wounds. In this patient, the humerus was debrided and stabilized through a posterior approach as was the medial condyle fracture. The ulna was fixed through an extension of the posterior incision and the radius through a separate dorsal approach. Solomon HB, Zadnik M, Eglseder WA: A review of outcomes in 18 patients with floating elbow. J Orthop Trauma 2003;17:563-570.
Question 22
In a patient with a soft-tissue sarcoma treated by wide excision and radiation therapy, the risk of subsequent fracture is probably most influenced by
Explanation
While most pathologic fractures are in the lower extremity in patients treated for soft-tissue sarcomas by wide excision and adjuvant radiation therapy, risk factors for such fractures are bone resection associated with excision of the tumor and soft-tissue sarcomas of the thigh that require periosteal stripping at the time of resection. Such fractures can occur late, often more than 6 months after surgery, are difficult to treat, and often result in nonunion. Bell RS, O'Sullivan B, Nguyen C, et al: Fractures following limb-salvage surgery and adjuvant irradation for soft-tissue sarcoma. Clin Orthop 1991;271:265-271.
Question 23
What is the most common reason an individual with a malignant soft-tissue tumor in the extremities seeks medical attention?
Explanation
Unlike malignant bone tumors, malignant soft-tissue tumors usually are asymptomatic and present with the presence of a mass. Malignant soft-tissue tumors enlarge by centrifugal growth, creating a mass while compressing surrounding tissue. Symptoms may develop as the result of direct compression on neurovascular structures as the tumor enlarges. This is especially true in the pelvis where the tumor can enlarge appreciably without being noticed. However, in the extremities, the tumor is most often apparent before neurologic symptoms develop. An asymptomatic mass is not necessarily benign; therefore, biopsy should not be delayed. It is uncommon for a malignant soft-tissue mass to be discovered incidentally. Soft-tissue tumors are not typically apparent on radiographs; they are best identified with MRI. Brouns F, Stas M, De Wever I: Delay in diagnosis of soft tissue sarcomas. Eur J Surg Oncol 2003;29:440-445. Rougraff B: The diagnosis and management of soft tissue sarcomas of the extremities in the adult. Curr Probl Cancer 1999;23:1-50.
Question 24
Figure 21 shows the radiograph of a 32-year-old patient with right hip pain that has failed to respond to nonsurgical management. What is the most appropriate surgical treatment at this time?
Explanation
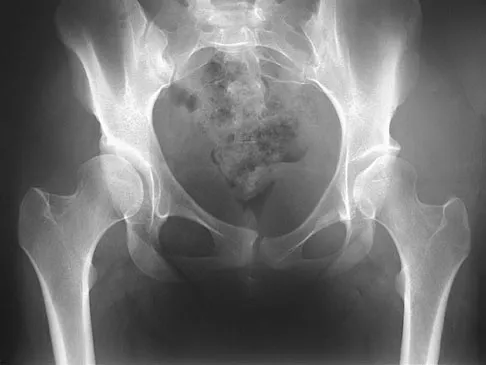
The radiograph reveals developmental dysplasia of both hips. The patient has classic anterolateral undercoverage of the femoral head on the right side as demonstrated by a high acetabular index (measured at 27 degrees). Anterior undercoverage can be determined by drawing the marking for the anterior wall that fails to overlap the femoral head in this patient. Currently in North America, the most accepted surgical management for symptomatic dysplasia of the hip with good joint space is a Bernese (Ganz) periacetabular osteotomy. Surgical dislocation of the hip and femoroacetabular osteoplasty may be considered for patients with symptomatic femoroacetabular impingement of the hip. Ganz R, Klaue K, Vinh TS, et al: A new periacetabular osteotomy for the treatment of hip dysplasias: Technique and preliminary results. Clin Orthop 1988;232:26-36.
Question 25
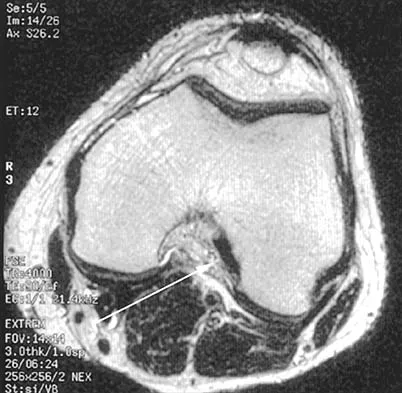
Figure 16 shows an axial MRI scan through the knee joint. What structure is identified by the arrow?
Explanation
The anterior cruciate ligament can be visualized on an axial MRI scan as a low-signal structure lying in the lateral aspect of the intercondylar notch. Visualization in multiple planes increases the accuracy of MRI to view the anterior cruciate ligament. The posterior cruciate ligament and ligament of Wrisberg are located on the medial wall of the notch. The ligamentum mucosum is anterior to the notch, and the popliteus tendon is posterior to the lateral femoral condyle. Resnick D, Kang HS (eds): Internal Derangements of Joints: Emphasis on MR Imaging. Philadelphia, PA, WB Saunders, 1997, pp 675-699.
Question 26
A 28-year-old hockey player has a shoulder deformity after being checked into the boards. Examination reveals that swelling has improved, but there is tenderness along the distal clavicle. Radiographs reveal a grade II acromioclavicular joint separation. Initial management should consist of
Explanation
The most common shoulder injury in hockey players is to the acromioclavicular joint. Early rest and control of pain and inflammation is the preferred management. Surgery is reserved for patients with significant coracoclavicular disruption that has failed to respond to nonsurgical management. Cross-chest stretches and overhead exercises may increase symptoms. A cortisone injection within the glenohumeral joint will have little effect. Nuber GW, Bowen MK: Acromioclavicular joint injuries and distal clavicle fractures. J Am Acad Orthop Surg 1997;5:11-18.
Question 27
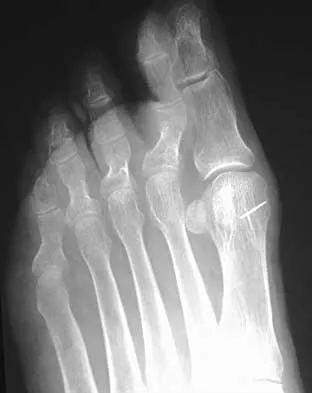
A 68-year-old woman stepped on a needle while walking barefoot 10 days ago. She is not certain but thinks it is imbedded in her foot, and she notes local tenderness at the puncture site and drainage. Her primary care physician has been treating her with oral antibiotics. A plain radiograph is shown in Figure 38. What is the best course of action?
Explanation
Based on the radiographic findings, the patient has a metallic foreign body in her foot that is consistent with a needle. She has local infection secondary to the continued presence of the foreign body. CT is not necessary to localize the foreign body as it is adequately visualized on the plain radiographs. The infection cannot be adequately treated until the foreign body is removed. Attempted removal of foreign bodies without proper anesthesia and fluoroscopy frequently results in frustration because of the inability to localize the foreign body. Removal in a surgical suite with proper anesthesia and fluoroscopy is the preferred option. Once the foreign body is removed, the local infection will resolve rapidly. Combs AH, Kernek CB, Heck DA: Orthopedic grand rounds: Retained wooden foreign body in the foot detected by computed tomography. Orthopedics 1986;9:1434-1435.
Question 28
In the nonsurgical management of posterior tibial tendon dysfunction with flexible deformity, a common strategy is to prescribe an ankle-foot orthosis or a University of California Biomechanics Laboratory (UCBL) orthosis with medial posting. A high patient satisfaction rating and favorable outcome with this nonsurgical management is most likely in which of the following situations?
Explanation
Most authors recommend an initial trial of nonsurgical management in the treatment of adult-acquired flatfoot deformity such as posterior tibial tendon dysfunction. Chao and associates found that there is high patient satisfaction with ankle-foot orthoses and UCBL-type inserts in elderly patients with a relatively sedentary lifestyle. Alternatively, there was a higher dissatisfaction rate in young active patients, those with balance and ambulation difficulties (Parkinson's, severe arthritis of the hip or knee), and patients with inflammatory systemic disorders. Chao W, Wapner KL, Lee TH, et al: Nonoperative management of posterior tibial tendon dysfunction. Foot Ankle Int 1996;17:736-741.
Question 29
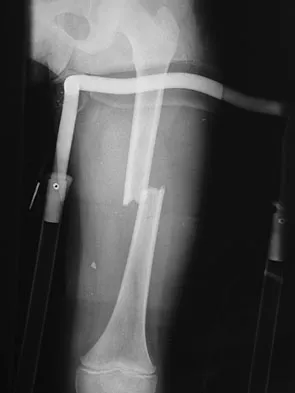
The axis of forearm rotation occurs between what two anatomic points?
Explanation
Forearm rotation results from a complex interaction of osseous articulations and soft tissues including the radiocapitellar articulation, proximal and distal radioulnar joints, the interosseous membrane, and the adjacent forearm muscles. The rotation occurs around a longitudinal forearm axis extending from the center of the radial head proximally through the foveal region of the ulnar head distally. Werner FW, An KN: Biomechanics of the elbow and forearm. Hand Clin 1994;10:357-373.
Question 30
What pharmacologic agents are preferred for the treatment of symptomatic active Paget's disease?
Explanation
Recent medical literature supports the use of bisphosphonates as the treatment of choice for active Paget's disease.
Question 31
Which of the following changes of calcium metabolism accompany the loss of bone during menopause?
Explanation
There is a negative change of calcium balance with a decrease in intestinal absorption and an increase in urinary calcium loss. The reduction of intestinal absorption is accompanied by reduced circulating concentrations of total, but not free 1,25-dihydroxyvitamin D. However, estrogen may also directly regulate intestinal calcium resorption independent of vitamin D. Tubular resorption of calcium is higher in the presence of estrogen. Studies of the levels of PTH in the presence of estrogen are controversial. Oh KW, Rhee EJ, Lee WY, et al: The relationship between circulating osteoprotegerin levels and bone mineral metabolism in healthy women. Clin Endocrinol (Oxf) 2004;61:244-249.
Question 32
A 21-year-old man with neurofibromatosis and multiple cutaneous neurofibromas has a rapidly enlarging painless mass on his buttock. Examination reveals a nontender, well-defined 6- x 6-cm soft-tissue mass that is deep to the fascia. The best course of action should be to order
Explanation
Patients with neurofibromatosis are at risk for development of soft-tissue sarcomas (most commonly malignant peripheral nerve sheath tumors). Clinical indications of development of a neurofibrosarcoma include a rapidly enlarging soft-tissue mass; therefore, this patient should be considered to have a neurofibrosarcoma until proven otherwise. MRI is superior to CT in characterizing the anatomic location of soft-tissue masses and the signal characteristics of the lesion. Areas of necrosis within the tumor may be apparent on MRI that cannot be appreciated on CT, suggesting a malignant tumor. Local imaging studies of suspected malignant tumors should be performed prior to needle or open biopsy so that the biopsy site can be excised at the time of definitive resection. Additionally, postbiopsy changes may lead to MRI artifacts that alter the interpretation of the MRI. Demas BE, Heelan RT, Lane J, Marcove R, Hajdu S, Brennan MF: Soft-tissue sarcomas of the extremities: Comparison of MR and CT in determining the extent of disease. Am J Roentgenol 1988;150:615-620.
Question 33
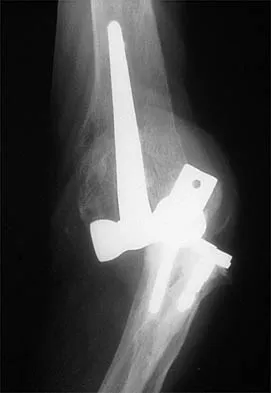
A 20-year-old professional baseball pitcher has had a 3-year history of increased aching in his shoulder that is associated with pitching, and he is now seeking a second opinion. Nonsurgical management consisting of rest, anti-inflammatory drugs, ice, heat, and cortisone injections has failed to provide relief. A previous work-up that included radiographs and gadolinium-enhanced MRI arthrography was negative. Results of an arteriogram suggest quadrilateral space syndrome. Assuming that this is the correct diagnosis, what nerve needs to be decompressed?
Explanation
Quadrilateral space syndrome is a rare condition and is the result of compression of the contents of the quadrilateral space. The contents of the quadrilateral space include the posterior circumflex vessels and the axillary nerve. Cahill BR, Palmer RE: Quadrilateral space syndrome. J Hand Surg 1983;8:65-69.
Question 34
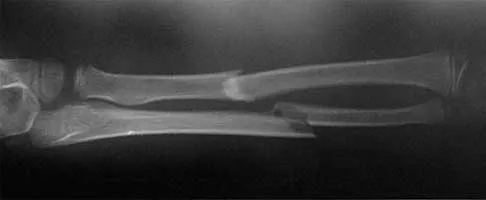
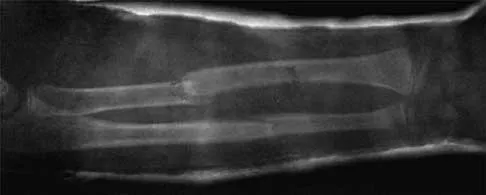
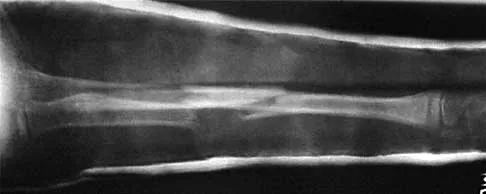
Figures 43a and 43b show the AP and lateral radiographs of the radius and ulna of a 9-year-old patient. The fracture is manipulated and placed in a long arm cast with the elbow flexed to 90 degrees and the forearm to neutral rotation. Figures 43c and 43d show the alignment of the fracture after the manipulation. What is the next most appropriate step in management?

Explanation
By placing the forearm at neutral rotation, as shown in Figures 43c and 43d, the distal fragment has become malrotated by 90 degrees. This is evident by the fact that the bicipital tuberosity is rotated 90 degrees to the radial styloid. Normally, it should be directly opposite (180 degrees) to the radial styloid. The correct alignment was present in the original radiographs shown in Figures 43a and 43b. Another clue to the malrotation in the postreduction radiographs is the difference in the diameters of the opposing radial shafts. To correct this rotational malalignment, the distal fragment needs to be remanipulated into supination so that it is correctly aligned with the supinated proximal radius. Evans EM: Fractures of the radius and ulna. J Bone Joint Surg Br 1951;33:548-561.
Question 35
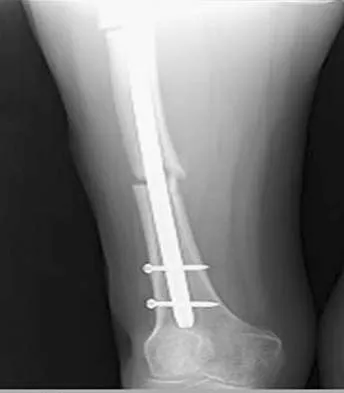
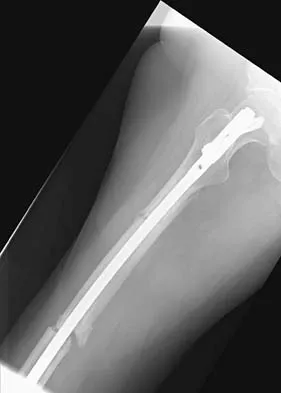
Figures 36a and 36b show the radiographs of a 48-year-old woman who smokes cigarettes and sustained a segmental femoral shaft fracture in a motor vehicle accident 9 months ago. Initial management consisted of stabilization with a reamed statically locked intramedullary nail. She now reports lower leg pain that increases with activity. In addition to advising the patient to quit smoking, management should include
Explanation
The patient has an oligotrophic nonunion of the distal femoral fracture. Although the proximal fracture appears incompletely united, it was stable at exchange nailing. The treatment of choice is exchange reamed nailing to at least 2 mm above the nail in place. Bone grafting is debatable. Recent studies have shown a 70% to 75% success rate with exchange nailing only, so in nonhypertrophic nonunions, bone grafting can be considered. Nonsurgical management consisting of observation or external stimulation runs the risk of implant failure. Plate fixation is acceptable but is considered a second choice because of the need to consider stabilization of the proximal fracture until union is achieved. Also, plate fixation definitely requires bone grafting. Webb LX, Winquist RA, Hansen ST: Intramedullary nailing and reaming for delayed union or nonunion of the femoral shaft: A report of 105 consecutive cases. Clin Orthop 1986;212:133-141. Weresh MJ, Hakanson R, Stover MD, et al: Failure of exchange reamed intramedullary nailing for ununited femoral shaft fractures. J Orthop Trauma 2000;14:335-338.
Question 36
Kinematic analysis of the medial and lateral menisci has demonstrated that the lateral meniscus has which of the following characteristics compared with the medial meniscus?
Explanation
Kinematic analysis of both menisci demonstrates anterior movement with extension and posterior movement with flexion. The lateral meniscus has more mobility than the medial meniscus because of less soft-tissue attachments. Insall JN, Scott WN (eds): Surgery of the Knee, ed 3. New York, NY, Churchill Livingstone, 2001, vol 1, p 474. Thompson WO, Thaete FL, Fu FH, et al: Tibial meniscal dynamics using 3D reconstructions of MR images, in Proceedings of the Orthopaedic Research Society 1990;389.
Question 37
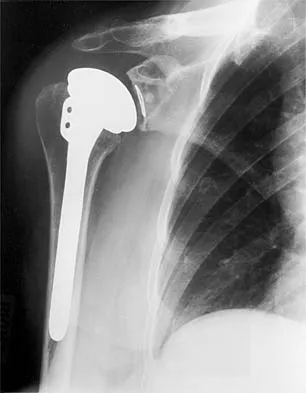
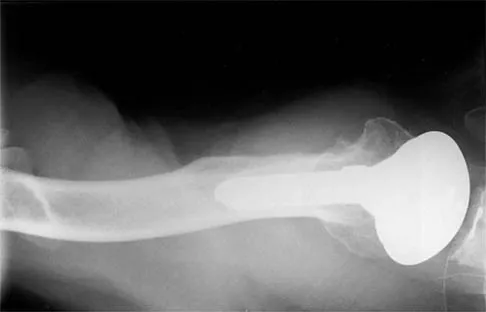
A 54-year-old man undergoes total shoulder arthroplasty for osteoarthritis. Despite compliance with an early passive range-of-motion exercise program, he does not regain more than 90 degrees of elevation, 10 degrees of external rotation, and has internal rotation to the fifth lumbar vertebra. At 6 months, his motion fails to improve. Radiographs are shown in Figures 18a and 18b. What is the best course of action?
Explanation
The patient has a global loss of motion that has failed to improve with 6 months of nonsurgical treatment; because he has reached a plateau, further nonsurgical management will likely be ineffective. Revision in the form of an open release is indicated to lyse intra- and extra-articular adhesions; subscapularis lengthening may be done concurrently as needed. Revising to a smaller head can be considered if adequate motion is not achieved. The radiographs reveal an adequate neck cut with appropriate seating of the component. Removing the glenoid component will decrease capsular tension but will probably increase pain because of the lack of glenoid resurfacing. Increasing humeral retroversion will not improve motion. Cuomo F, Checroun A: Avoiding pitfalls and complication in total shoulder arthroplasty. Orthop Clin North Am 1998;29:507-518.
Question 38
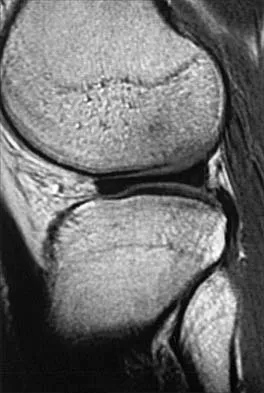
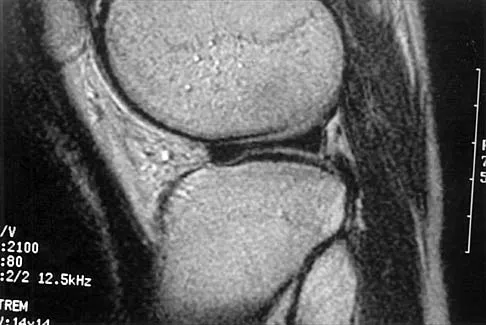
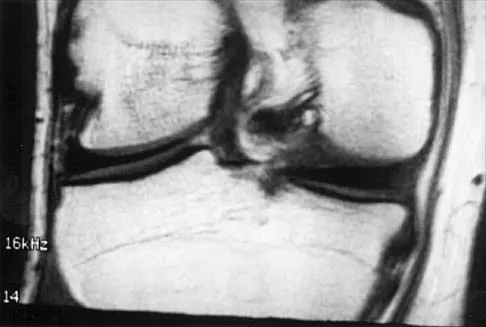
A 26-year-old man has recurrent right knee pain. Figures 9a and 9b show consecutive sagittal T2-weighted MRI scans, and Figure 9c shows a coronal T1-weighted MRI scan. What is the most likely diagnosis?
Explanation
A discoid meniscus is a large disk-like meniscus. It is seen in the lateral meniscus in 3% of the population; a discoid medial meniscus is much less common. It can be identified on the coronal view by noting meniscal tissue extending into the tibial spine at the intercondylar notch. The average width of a normal meniscus is less than 11 mm. A bow-tie appearance should not be seen on more than two consecutive sagittal images because the conventional thickness of the sagittal slices is 3 mm and the interval between two consecutive slices is 1.5 mm. Two sagittal slices will cover a 9-mm thickness. A discoid meniscus can be diagnosed on the sagittal views by noting a bow-tie appearance on more than two consecutive images. Helms CA: MR image of the knee, in Fundamentals of Skeletal Radiology, ed 2. Philadelphia, PA, WB Saunders, 1995, pp 172-191.
Question 39
A previously healthy 14-year-old boy now reports fatigue, and has a bilateral Trendelenburg gait, right hip pain, and bilateral knee and foot pain. Biopsy of a right sacral mass reveals intermediate grade osteosarcoma. There are no metastases. Laboratory studies reveal a serum calcium level of 7.7 mg/dL (normal 8.5 to 10.5), a phosphate level of 2.0 mg/dL (normal 2.7 to 4.5), a 1,25-dihydroxyvitamin D level of less than 10 pg/mL (normal 18 to 62), a parathyroid hormone level of 19 pg/mL (normal 10 to 60), and an alkaline phosphatase level of 428 U/L (normal 15 to 351). What is the most likely cause of the patient's symptoms?
Explanation
The laboratory findings are typical for rickets. Oncogenic rickets is a paraneoplastic syndrome that results from a substance secreted by the tumor that interferes with renal tubule reabsorption of phosphate. This substance previously had been called phosphatonin but recently has been identified as fibroblast growth factor 23. Nutritional rickets is rare in developed countries. Delayed onset familial hypophosphatemic rickets is possible, but the likelihood of having two rare diseases is unlikely. Osteosarcoma does not sequester calcium. Alkaline phosphatase levels can be elevated in osteosarcoma but does not cause muscle weakness. Tumor cachexia would occur only with advanced metastatic disease. A unilateral sacral mass would not cause a bilateral L5 neuropathy or the abnormal laboratory findings. Case records of the Massachusetts General Hospital. Weekly clinicopathological exercises. Case 29-2001. A 14-year-old with abnormal bones and a sacral mass. N Engl J Med 2001;345:903-908.
Question 40
The posterior circumflex humeral artery and the axillary nerve usually lie in a space bordered superiorly by the
Explanation
The quadrangular space is bordered superiorly by the teres minor, medially by the long head of the triceps, laterally by the humerus, and inferiorly by the teres major. The posterior circumflex humeral artery and the axillary nerve lie in this space. Rockwood CA Jr, Matsen FA III: The Shoulder, ed 2. Philadelphia, PA, WB Saunders, 1998, vol 1, pp 70-71.
Question 41
What is the most common malignant tumor of the foot?
Explanation
Whereas chondrosarcoma is the most frequently occurring malignant bone tumor of the foot and synovial sarcoma is the most common soft-tissue foot malignancy, the most common malignant tumor overall is melanoma. It constitutes approximately 25% of lesions found on the lower extremity. Furthermore, 31% of all melanomas arise in the foot. Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 11-26.
Question 42
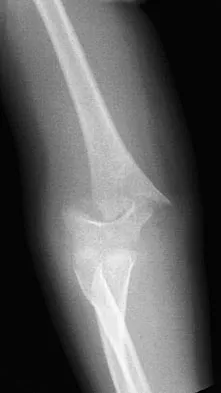
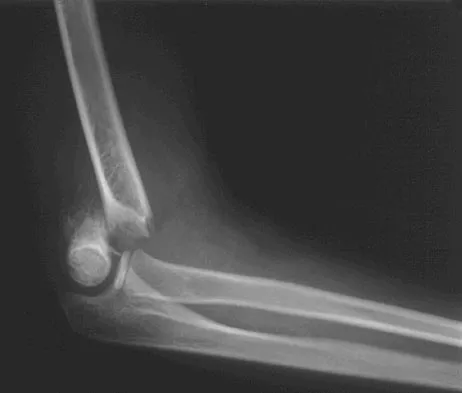
A 5-year-old boy sustained an elbow injury. Examination in the emergency department reveals that he is unable to flex the interphalangeal joint of his thumb and the distal interphalangeal joint of his index finger. The radial pulse is palpable at the wrist, and sensation is normal throughout the hand. Radiographs are shown in Figures 6a and 6b. In addition to reduction and pinning of the fracture, initial treatment should include
Explanation
The findings are consistent with a neurapraxia of the anterior interosseous branch of the median nerve. This is the most common nerve palsy seen with supracondylar humerus fractures, followed closely by radial nerve palsy. Nearly all cases of neurapraxia following supracondylar humerus fractures resolve spontaneously, and therefore, further diagnostic studies and surgery are not indicated. Cramer KE, Green NE, Devito DP: Incidence of anterior interosseous nerve palsy in supracondylar humerus fractures in children. J Pediatr Orthop 1993;13:502-505.
Question 43
An 8-year-old boy with moderate factor VIII hemophilia played kickball earlier in the day and now reports progressively severe groin pain and is unable to walk. Examination reveals marked paresthesias over the medial aspect of the distal tibia. What is the most likely diagnosis?
Explanation
The iliacus muscle is a frequent site of hemorrhage in patients with severe or moderate hemophilia. In patients with moderate hemophilia, hemorrhage into the iliacus muscle often follows play or sporting events that include forceful contraction of the hip flexor muscles. An expanding iliacus hematoma compresses the adjacent femoral nerve, with one study reporting 60% complete femoral nerve palsy in hemophiliacs with an iliacus or iliopsoas hemorrhage. Femoral nerve compression typically includes paresthesias in the distribution of the terminal saphenous nerve branch. Hip joint hemarthrosis may occur, but this condition is not as frequent in hemophiliacs as muscle hemorrhage into the iliacus muscle. More importantly, a hip joint hemarthrosis is not associated with significant compression of the femoral nerve. Avulsion fractures of the anterior superior iliac spine typically occur during adolescence and are not associated with saphenous nerve paresthesias. Slipped capital femoral epiphysis does not have an increased association with hemophilia and usually occurs during the adolescent years. Greene WB: Diseases related to the hematopoietic system, in Morrissy RT, Weinstein SL (eds): Lovell and Winter's Pediatric Orthopaedics, ed 5. Philadelphia, PA, Lippincott Williams and Wilkins, 2001, pp 379-426.
Question 44
Which of the following benign bone lesions can develop lung metastases?
Explanation
Although considered benign bone lesions, lung metastases can develop in giant cell tumors and chondroblastomas. These often can be treated with multiple thoracotomies, resulting in long-term survival. Roberts PF, Taylor JG: Multifocal benign chondroblastomas: Report of a case. Hum Pathol 1980;11:296-298.
Question 45
A 65-year-old man has a painful mass of the middle finger. A clinical photograph, lateral radiograph, coronal MRI scan, and biopsy specimen are seen in Figures 20a through 20d. What is the most likely diagnosis?
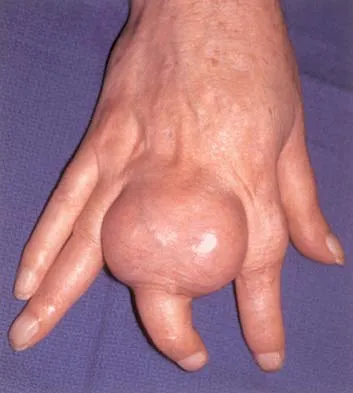
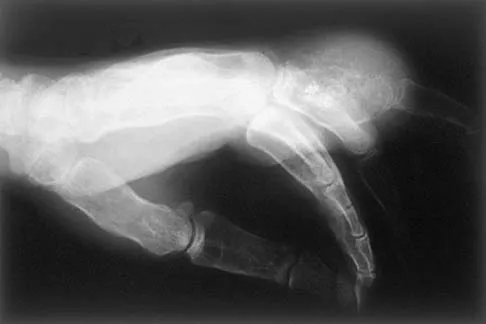
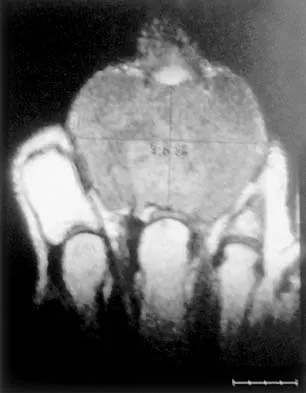
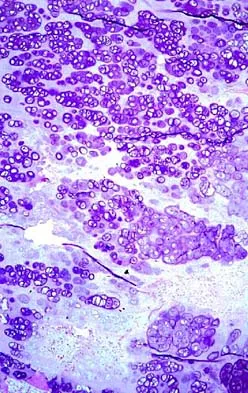
Explanation
Although the degeneration of an isolated benign cartilaginous lesion into a chondrosarcoma is rare, it occurs in roughly 10% of patients with Ollier's disease. Pain is the most common symptom of chondrosarcoma. The treatment of low-grade chondrosarcoma ranges from intralesional excision to wide amputation. The intent of the surgery is to remove all the disease to decrease the chance of local recurrence. Lee FY, Mankin HJ, Fondren G, et al: Chondrosarcoma of bone: An assessment of outcome. J Bone Joint Surg Am 1999;81:326-338.
Question 46
A 10-lb, 2-oz infant who was born via a difficult breech delivery 12 hours ago is now being evaluated for hip pain. Although the infant is resting comfortably, examination reveals that the patient is not moving the right lower extremity and manipulation of the right hip causes the infant to cry. The Galeazzi sign is positive. An AP radiograph of the pelvis shows proximal and superior migration of the right proximal femoral metaphysis. What is the most likely diagnosis?
Explanation
Transphyseal fractures of the proximal femur at birth are more likely to occur in large newborns after a difficult delivery. At rest, the patients are comfortable and show a pseudoparalysis; however, passive motion of the lower extremity results in discomfort. Teratologic hip dislocations will have a positive Galeazzi sign, but are not painful. Development of a septic hip would be unlikely within 12 hours postpartum. Congenital coxa vara is typically painless. Postpartum ligamentous laxity might account for a positive Ortolani sign, but is painless. Weinstein JN, Kuo KN, Millar EA: Congenital coxa vara: A retrospective review. J Pediatr Orthop 1984;4:70-77.
Question 47
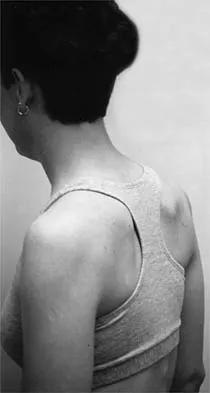
A 22-year-old woman has had progressive upper extremity weakness for the past several years. History reveals no pain in her neck or shoulders. Examination reveals scapular winging of both shoulders and weakness in external rotation. She can abduct to only 120 degrees bilaterally, and there is mild supraspinatus weakness. She is otherwise neurologically intact with normal sensation and reflexes; however, she has difficulty whistling. A clinical photograph is shown in Figure 14. What is the most likely diagnosis?
Explanation
Progressive weakness is a common sign with a large differential diagnosis. Nerve, muscle, and joint problems should be excluded when a patient has diffuse weakness and atrophy. Fascioscapulohumeral dystrophy is a rare disease characterized by facial muscle weakness and proximal shoulder muscle weakness. The weakness is usually bilateral, and scapular winging is common. If the scapular winging becomes pronounced, elevation of the shoulder can be affected. In severe cases, scapulothoracic fusion or pectoralis muscle transfer to the scapula may be indicated. Duchenne muscular dystrophy is typically severe and progressive. The other diagnoses are not compatible with the history or the physical findings. Shapiro F, Specht L: The diagnosis and orthopaedic treatment of inherited muscular diseases of childhood. J Bone Joint Surg Am 1993;75:439-454.
Question 48
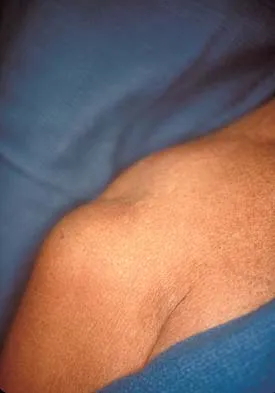
A 58-year-old man has persistent pain and weakness of his right shoulder after undergoing primary rotator cuff repair 1 year ago. A clinical photograph is shown in Figure 11. Which of the following factors might make functional improvement problematic with revision rotator cuff surgery?
Explanation
Functional improvement after revision rotator cuff surgery is most likely to occur in patients with an intact deltoid, good-quality rotator cuff tissue, preoperative active elevation alone to 90 degrees, and only one prior rotator cuff repair. In this patient, the compromised deltoid origin might make functional improvement less likely. Djurasovic M, Marra G, Arroyo JS, et al: Revision rotator cuff repair: Factors influencing results. J Bone Joint Surg Am 2001;83:1849-1855. Bigliani LU, Cordasco FA, McIlveen SJ, et al: Operative treatment of failed repairs of the rotator cuff. J Bone Joint Surg Am 1992;74:1505-1515.
Question 49
A 22-month-old child has scrapes and bruises on his head and a severe deformity of the forearm after being thrown from a car as an unrestrained passenger in a motor vehicle accident. Examination reveals a Glasgow Coma Scale score of 12. Prior to treatment of the forearm, management should include
Explanation
As CT scanning has become available, the use of radiographs of the skull has decreased in importance for evaluation of head trauma. The indications for CT scanning for suspected head trauma include any degree of obtundation, focal neurologic deficit, history of a high-velocity injury, amnesia for the injury, progressive headache, persistent vomiting, children younger than age 2 years, serious facial injury, posttraumatic seizure, skull penetration, or a Glasgow Coma Scale score of 13 or less. Evidence of improved outcome with use of steroids in head trauma is lacking. Steroids are useful for increased intracranial pressure caused by brain tumors or abscesses. High-dose IV methylprednisolone is indicated for spinal cord trauma and improves the ultimate degree of recovery of function. When herniation is suspected in a patient with asymmetric neurologic findings or the patient's condition is deteriorating rapidly, a mannitol infusion may be used. Hall DE: Head injuries, in Hoekelman RA (ed): Primary Pediatric Care. St Louis, Mo, Mosby, 1997, pp 1709-1712. Nelson WE, Behrman RE, Kliegman RM (eds): Nelson Essentials of Pediatrics. Philadelphia, Pa, WB Saunders, 1998, p 712.
Question 50
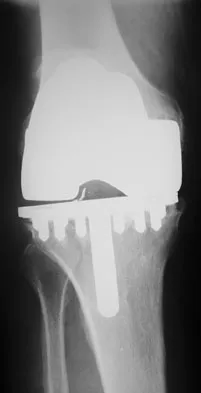
Figure 8 shows the radiograph of a 76-year-old man who has knee pain and swelling. History reveals that he underwent total knee arthroplasty 18 years ago. What is the most likely diagnosis?
Explanation
The radiograph reveals complete loss of joint space with particulate metal debris consistent with total polyethylene failure and metal-on-metal articulation. The components appear to be well fixed and minimal osteolysis is evident. Kilgus DJ, Moreland JR, Finerman GA, et al: Catastrophic wear of tibial polyethylene inserts. Clin Orthop Relat Res 1991;273:223-231.
Question 51
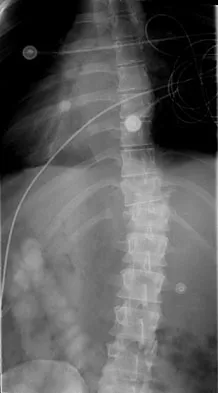
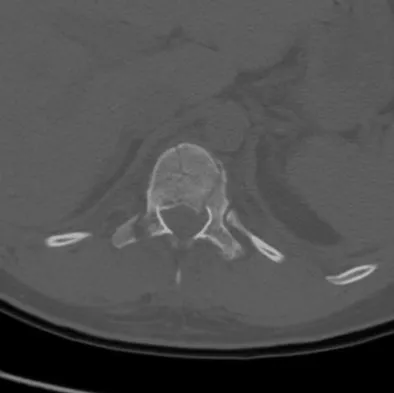
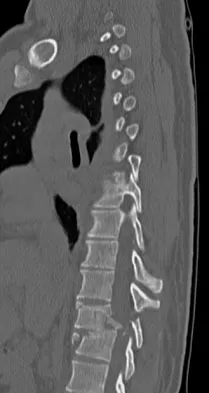
A 23-year-old man is involved in a motor vehicle accident. An AP radiograph is shown in Figure 29a, and axial and sagittal CT scans are shown in Figures 29b and 29c. Neurologic examination shows 1/5 strength of his quadriceps and iliopsoas on the right, with 1/5 quadriceps function on the left. Definitive treatment of his injury should consist of
Explanation
The imaging studies show a fracture-dislocation. Surgical treatment of this injury consists of a decompression reduction, stabilization, and fusion. A posterolateral decompression can also be performed as necessary. An isolated anterior procedure in this type of injury is contraindicated. The anterior longitudinal ligament is most likely intact; therefore, an anterior procedure further destabilizes the spine. Reduction by an anterior approach would also be difficult. Nonsurgical management of the neurologic injury in this patient is not indicated. Theiss SM: Thoracolumbar and lumbar spine trauma, in Stannard JP, Schmidt AH, Kregor PJ (eds): Surgical Treatment of Orthopaedic Trauma. New York, NY, Thieme, 2007, pp 179-207.
Question 52
Figure 21 shows the tomogram of a 26-year-old woman who sustained an axial load injury to her neck in a fall off a horse. What ligament is injured?

Explanation
Levine and Edwards, in their description of the classic C1 burst (Jefferson) fracture, noted that spread of the lateral masses of more than 7 mm is indicative of a transverse ligament rupture. Long-term C1-C2 instability, however, has not been described with this fracture pattern. Although long-term traction followed by halo vest immobilization has been described as the best technique for achieving an ideal result, treatment of this injury remains somewhat controversial. Levine AM, Edwards CC: Fractures of the atlas. J Bone Joint Surg Am 1991;73:680-691.
Question 53
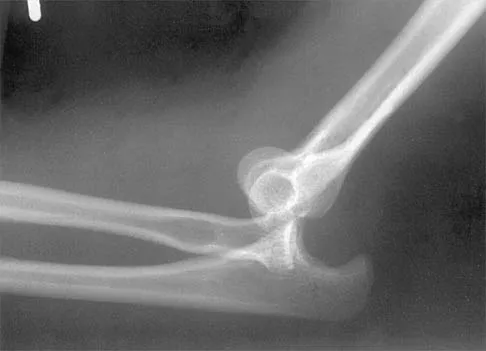
Figure 38 shows the radiograph of a 16-year-old wrestler who injured his elbow when he was thrown to the mat by his opponent. To minimize additional trauma to the medial soft tissues, the elbow should be reduced in
Explanation
The elbow dislocates by a three-dimensional movement of supination and valgus during flexion. Additional trauma during reduction is minimized by recreating the deformity and reducing the elbow in supination. The actual maneuver includes full supination (actually hypersupination) of the elbow in a valgus position. This is followed by pushing the olecranon distally in line with the long axis of the ulna while swinging the elbow into varus, and then relaxing the supination torque. Postreduction stability is enhanced in pronation, except when the soft-tissue disruption is extensive. O'Driscoll SW: Elbow dislocations, in Morrey BF (ed): The Elbow and Its Disorders, ed 2. Philadelphia, PA, WB Saunders, 1993, p 414.
Question 54
A 67-year-old retired steelworker was involved in a motor vehicle accident and sustained a midcervical spinal cord injury. Radiographs and MRI scans reveal severe cervical stenosis and spondylosis without fractures or dislocations. Neurologic examination reveals an ASIA C spinal cord impairment with greater motor involvement of the upper extremities than the lower extremities. What is the probability that the patient eventually will become ambulatory?
Explanation
The patient sustained an incomplete spinal cord injury known as central cord syndrome. Central cord syndrome characteristically has disproportionate involvement of the upper extremities with the lower extremities being relatively spared. It is most commonly seen after cervical injuries in elderly patients with spondylosis and spinal stenosis, often without fracture. Penrod and associates noted that 23 of 59 patients with central cord syndrome (ASIA C and D) ultimately walked. The poorest prognosis, however, was in ASIA C patients older than age 50, in which only 40% walked. Penrod LE, Hegde SK, Ditunno JF Jr: Age effect on prognosis for functional recovery in acute, traumatic central cord syndrome. Arch Phys Med Rehab 1990;71:963-968.
Question 55
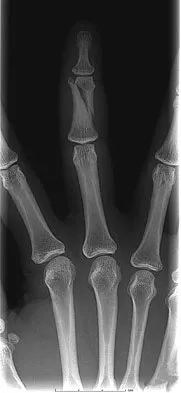
A 47-year-old woman falls and sustains a direct blow to her middle finger. She notes pain and swelling and is unable to move the proximal interphalangeal (PIP) or distal interphalangeal (DIP) joints. Radiographs are shown in Figures 8a through 8c. Proper management should consist of
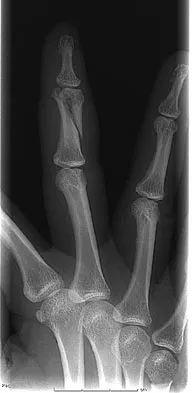
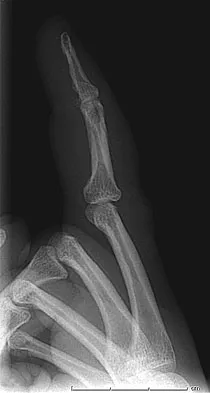
Explanation
The oblique nature of the fracture and extension of the fracture to the condyles implies an unstable fracture. Lag screw fixation provides an excellent chance of union, and the ability to start early range of motion. Stern PJ: Fractures of the metacarpals and phalanges, in Green DP, Hotchkiss RN, Pederson WC, et al (eds): Green's Operative Hand Surgery, ed 5. Philadelphia, PA, Elsevier, 2005, p 281.
Question 56
A 38-year-old woman with metastatic thyroid carcinoma has had increasing pain in the left hip for the past 3 months. An AP radiograph and coronal T1-weighted MRI scan are shown in Figures 28a and 28b. Management should consist of
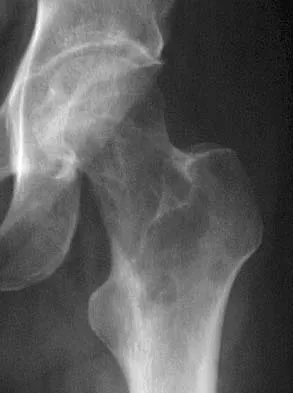
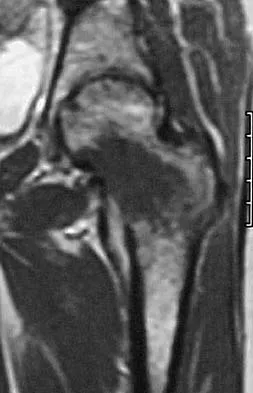
Explanation
The radiograph and MRI scan reveal a lytic lesion in the left femoral neck region that extends to the lesser trochanter. Although external beam radiation and radioactive iodine infusion may be helpful in controlling the local disease, the patient is at high risk for femoral neck fracture given the location of the lesion. Prophylactic surgery is indicated; therefore, the treatment of choice is a cemented bipolar hemiarthroplasty. The use of a compression hip screw and side plate or an intramedullary nail has a high likelihood of failure with disease progression. Postoperative treatment with radiation therapy and bisphosphonates is also indicated. Mirels H: Metastatic disease in long bones: A proposed scoring system for diagnosing impending pathologic fractures. Clin Orthop 1989;249:256-264. Swanson KC, Pritchard DJ, Sim FH: Surgical treatment of metastatic disease of the femur. J Am Acad Orthop Surg 2000;8:56-65.
Question 57
A 26-year-old man sustains a displaced bimalleolar fracture by sliding into second base while playing baseball. Following initial closed reduction and splinting of the fracture, moderate swelling is noted. What is the safest time to perform surgery?
Explanation
Following any closed fracture, the most important determinant for the timing of surgery is the condition of the soft tissues and especially the skin. The best determinant of appropriate soft-tissue condition is the presence of wrinkling of the skin (wrinkle sign) at the site of the incision. A wrinkle sign is present when all the interstitial edema has left the skin; this may take up to 14 to 21 days of elevation. Any abrasion must be epithelialized so that there are no bacteria left at the site. To date, no other method of soft-tissue viability measurement has been shown to be of any clinical benefit. Stover MD, Kellam JF: Articular fractures: Principles, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 105-119. Hahn DM, Colton CL, Malleolar fractures, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 559-581.
Question 58
Which of the following is considered the most useful screening method for the evaluation of protective foot sensation in a patient with diabetes mellitus?
Explanation
Patients with diabetes mellitus should be screened for the presence of protective foot sensation. In the absence of protective foot sensation, patients are at increased risk for the development of neuropathic ulcerations and neuropathic arthropathy. The most reliable screening tool for the presence of protective sensation is the ability to feel the 5.07 Semmes-Weinstein monofilament. Pinzur MS, Shields N, Trepman E, Dawson P, Evans A: Current practice patterns in the treatment of Charcot foot. Foot Ankle Int 2000;21:916-920.
Question 59
Which of the following substances does not have androgenic effects?
Explanation
Growth hormone is the most abundant substance produced by the pituitary gland. Growth hormone has a direct anabolic effect by accelerating the incorporation of amino acids into proteins. It is becoming an increasingly popular anabolic steroid substitute; however, it is expensive and difficult to obtain. Androstenedione is an androgen produced by the adrenal glands and gonads. It acts as a potent anabolic steroid and is converted in the liver directly to testosterone with a resultant increase in levels after administration. DHEA is a naturally occurring hormone made by the adrenal cortex. It is converted to androstenedione, which in turn is converted to testosterone. The beneficial and adverse effects of DHEA can be correlated directly with those of testosterone. Nandrolone is also a potent anabolic steroid. It is commonly taken as 19-norandrostenedione and may be more favored because of its potent anabolic effects with less androgenic effects (no conversion to estrogen compounds). Creatine sales have skyrocketed, and it is a popular nutritional supplement. There is an expectation that creatine can increase strength and power performance; however, direct anabolic effects have not been demonstrated. Creatine serves as a substrate for hydrogen ions and contributes to the resynthesis of ATP (adenosine triphosphate) during maximal exercise. By enhancing ATP production and buffering local pH in muscle, there may be improved tolerance of anaerobic activities. Increases in muscle mass may be related to increased perception of improved training ability or an increase in muscle water content. Silver M: Use of ergogenic aids by athletes. J Am Acad Orthop Surg 2001;9:61-70.
Question 60
An 82-year-old man has had episodic right thigh pain after undergoing a total hip arthroplasty 10 years ago. Initial postoperative radiographs are shown in Figures 26a and 26b, and current radiographs are shown in Figures 26c and 26d. What is the most likely cause of his pain?
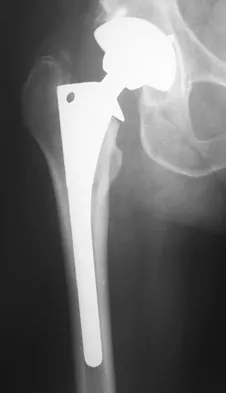
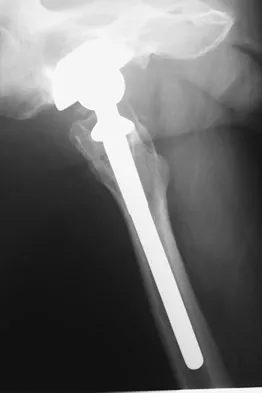
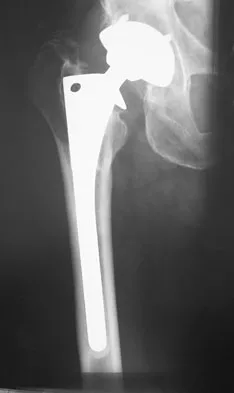
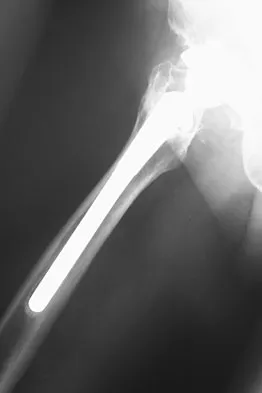
Explanation
These radiographs are dominated by the subsidence of the femoral component. There is also evidence of polyethylene wear and femoral osteolysis in the region of the greater trochanter. There is no evidence of proximal (calcar) stress shielding, and there is a thick distal pedestal. Engh and associates defined two major signs of osseointegration - the absence of radiolucent lines around the porous-surfaced portion of the implant and new bone bridging the gap between the endosteal surface and the porous portion of the implant. Implant migration indicates failure of ingrowth. Osteolysis is a periprosthetic loss of bone secondary to particulate debris and it is often clinically silent unless it is accompanied by pathologic fracture. It is often globular. Acetabular loosening is based on radiolucent lines and implant migration. The current radiographs demonstrate subsidence of the stem with pedestal formation. Engh CA, Massin P, Suthers KE: Roentgenographic assessment of biologic fixation of porous-surface femoral components. Clin Orthop Relat Res 1990;257:107-128.
Question 61
What is the most likely consequence of a vertebral compression fracture associated with osteoporosis?
Explanation
After an osteoporotic vertebral compression fracture, the risk of subsequent fractures at adjacent levels increases. This is felt to be the result of a shifting of the sagittal alignment more anteriorly, putting more stress on the osteopenic vertebral bodies and their anterior cortices. Pain generally resolves with rest, but this may take weeks or months. It has been demonstrated experimentally that osteoporotic vertebral bodies are actually less stiff and weaker after a compression fracture; therefore, deformity predisposes to further deformity. The extensor musculature often fatigues over time and usually does not hypertrophy. Frontal plane deformity is a rare development. Heaney RP: The natural history of vertebral osteoporosis: Is low bone mass an epiphenomenon? Bone 1992;13:S23-S26.
Question 62
The pathophysiology of a claw toe deformity includes muscular imbalance caused by which of the following relatively strong structures?
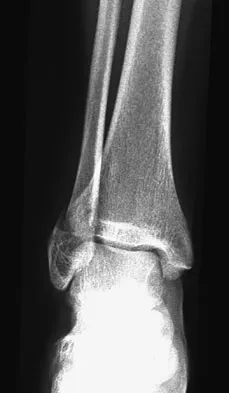
Explanation
The dynamic forces acting to maintain the position of the proximal phalanx at the head of the metatarsal are a balance between the extensor digitorum longus and the weaker intrinsic muscles. With hyperextension at the metatarsophalangeal joint, the intrinsic muscles become less efficient as plantar flexors. Consequently, the hyperextension deformity progresses in the metatarsophalangeal joint as the opposition of the intrinsic muscles to the extensor tendon lessens. This is in contrast to the situation in the interphalangeal joints, where the stronger flexors overpower the weaker intrinsic muscles, which act as the extensors. This combination of events leads to hyperextension at the metatarsophalangeal joint and flexion deformities at the interphalangeal joints, resulting in claw toe. Mizel MS, Yodlowski ML: Disorders of the lesser metatarsophalangeal Joints. J Am Acad Orthop Surg 1995;3:166-173.
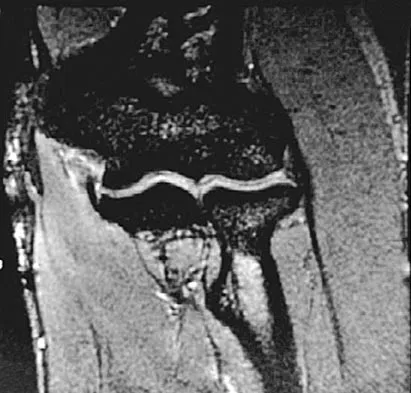
Question 63
What are the most likely symptoms and examination findings related to the mass in zone 2 of Guyon's canal seen in Figure 17?
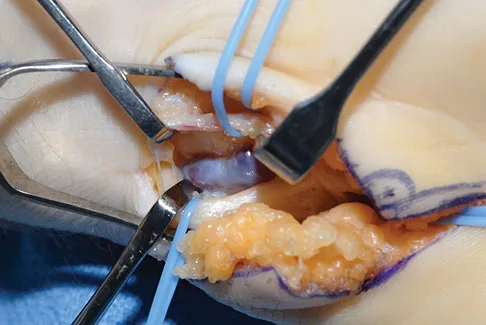
Explanation
The lesion lies in zone II of the ulnar tunnel. In that zone the deep motor branch of the ulnar nerve is susceptible to compression. Distal to the hook of the hamate, the motor branch of the ulnar nerve dives deep to innervate the interossei as it begins to move from an ulnar to radial direction. Because of its course, it has little or no give in response to a mass effect from the floor of Guyon's canal. Ganglions are the most common cause of ulnar nerve entrapment in the wrist. Lesions in zone I can affect both sensory and motor aspects of the ulnar nerve as well as the motor innervation of the hypothenar muscles. Lesions at the elbow or mid-to-proximal forearm are associated with dorsal hand numbness and tingling. Kuschner SH, Gelberman RH, Jennings C: Ulnar nerve compression at the wrist. J Hand Surg Am 1988;13:577-580.
Question 64
Which of the following is a long-term complication of ankle arthrodesis for posttraumatic arthritis?
Explanation
Ankle arthrodesis for posttraumatic ankle arthrosis provides reliable pain relief. However, the long-term sequela of joint arthrodesis is the development of arthrosis in the surrounding joints. Over time, following ankle arthrodesis, the ipsilateral hindfoot and midfoot joints show signs of joint space wear, and this may be symptomatic. With a stable ankle arthrodesis, progressive limb-length discrepancy or talar osteonecrosis is not expected. Ankle arthrodesis has not been definitively linked to ipsilateral knee arthritis or contralateral ankle arthritis. Coester LM, Saltzman CL, Leupold J, Pontarelli W: Long-term results following ankle arthrodesis for post-traumatic arthritis. J Bone Joint Surg Am 2001;83:219-228.
Question 65
A 25-year-old man is involved in a motor vehicle accident and brought to the emergency department at 4 am on Sunday morning. He has a closed distal third femoral shaft fracture. His leg is initially pulseless but after applying inline traction, a distal pulse can be palpated and the limb appears to be viable. The pulse in the injured limb "feels" different than the pulse in the uninjured limb. What is the next step in assessing the vascular status of this limb?
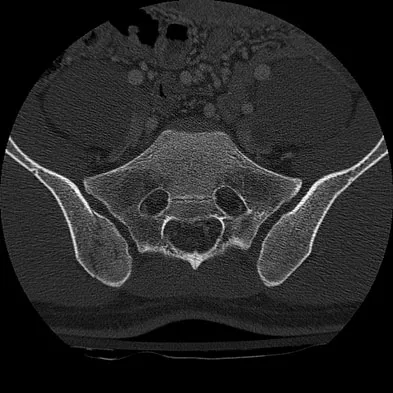
Explanation
The patient initially has a distal third femoral fracture and a pulseless limb. The first step is to reduce the fracture and reassess the vascular status. Although the pulse returns, it feels different than the quality of the pulse in the contralateral uninjured extremity. There is a risk of a vascular injury with this fracture pattern due to tethering of the femoral vessels at the adductor hiatus; therefore, the vascular status needs further assessment since the pulses are not symmetrical. A physical examination is not very accurate in assessing whether a vascular injury is present; therefore, serial examinations are not appropriate. Angiography is very sensitive and specific but is time consuming and can cause complications secondary to the dye and the arterial puncture required to perform it. Duplex ultrasound is effective but is very operator-dependent and may not be available 24 hours a day. The ABI is easily performed and has been shown to be sensitive and specific. If the value is greater than 0.9, the negative predictive value is 99% and when the value is less than 0.9, it is 95% sensitive and 97% specific for a major arterial injury. It has been shown to be useful for blunt lower extremity injuries as well as knee dislocations. Levy BA, Zlowodzki MP, Graves M, et al: Screening for extremity arterial injury with the arterial pressure index. Am J Emerg Med 2005;23:689-695. Abou-Sayed H, Berger DL: Blunt lower-extremity trauma and politeal artery injuries: Revisiting the case for selective arteriography. Arch Surg 2002;137:585-589.
Question 66
A 28-year-old woman fell on her right wrist while rollerblading 2 days ago. She was seen in the emergency department at the time of injury and was told she had a sprain. Examination now reveals dorsal tenderness in the proximal wrist but no snuffbox or ulnar tenderness. Standard wrist radiographs are normal. What is the next most appropriate step in management?
Explanation
When considering the diagnosis of scapholunate ligament injury, standard radiographic views of the hand will not always reveal widening of the scapholunate gap. Although MRI may reveal injury to the ligaments, the PA clenched fist view can be obtained in the office during the initial patient visit. Arthroscopy is not a first-line diagnostic tool. Walsh JJ, Berger RA, Cooney WP: Current status of scapholunate interosseous ligament injuries. J Am Acad Orthop Surg 2002;10:32-42.
Question 67
A 52-year-old woman underwent open reduction and internal fixation for radial and ulnar shaft fractures 2 months ago. In a second fall she refractured her forearm and required revision surgery with bone grafting. One month after the second operation she notes erythema, swelling, and drainage from the volar radial incision. In addition to antibiotic treatment, management should consist of
Explanation
Deep infections after plating of closed fractures of the forearm are unusual. However, the risk increases with repeat surgeries. Debridement of all infected, nonviable tissue is the initial step in management. The fixation may be retained if it is stable, but if the plate and screws are loose, they should be removed and revision performed after removal of nonviable bone. Either external fixation or repeat plating may be performed. Late infections after fracture union may be treated with plate and screw removal, debridement, and IV antibiotics. Kellam JF, Fischer TJ, Tornetta P III, Bosse MJ, Harris MB (eds): Orthopaedic Knowledge Update: Trauma 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 53-63. Moed BR, Kellam JF, Foster RJ, Tile M, Hansen ST Jr: Immediate internal fixation of open fractures of the diaphysis of the forearm. J Bone Joint Surg Am 1986;68:1008-1017.
Question 68
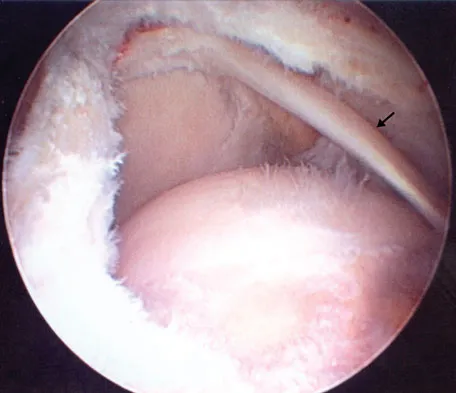
Figure 43 shows an arthroscopic view of a right shoulder through a lateral portal in the beach chair position. The arrow is pointing to what structure?
Explanation
This view from the lateral portal shows a full-thickness rotator cuff tear. The glenohumeral joint can be visualized through this tear. The glenoid, labrum, and biceps tendon attaching to the superior aspect of the glenoid are easily viewed from this portal, and the arrow is pointing to the biceps tendon. Arthroscopic rotator cuff repair can be performed while visualizing from this portal and using anterior and posterior working portals. Mazzocca AD, Noerdlinger M, Cole B, et al: Arthroscopy of the shoulder: Indications and general principles of techniques, in McGinty JB (ed): Operative Arthroscopy, ed 3. Philadelphia, PA, Lippincott Williams & Wilkins, 2003, pp 412-427.
Question 69
Which of the following statements is most accurate regarding undetected intraoperative surgical glove perforation?
Explanation
The incidence of undetected intraoperative surgical glove perforation has been demonstrated at approximately 8.5%, occurring most frequently on the index finger or left hand of the assistant surgeon. The frequency of glove perforation is higher in surgeries lasting longer than 3 hours. Al-Habdan I, Sadat-Ali M: Glove perforation in pediatric orthopaedic practice. J Pediatr Orthop 2003;23:791-793.
Question 70
A 22-year-old wrestler who underwent an open anterior shoulder reconstruction to repair a dislocated shoulder 6 months ago now reports shoulder pain after attempting a takedown. Examination reveals external rotation that is 15 degrees greater than the contralateral side. He has pain associated with abduction and external rotation but no apprehension. Which of the following tests would most likely reveal positive findings?
Explanation
Postoperative subscapularis detachment can be identified with a positive lift-off test that reveals weakness in internal rotation. This complication does not necessarily compromise the anterior capsule repair. The load-and-sift maneuver and articular contrast studies may be normal. Supraspinatus tests for impingement and weakness should be negative. Gerber C, Krushell RJ: Isolated ruptures of the tendon of the subscapularis muscle: Clinical fractures in 16 cases. J Bone Joint Surg Br 1991;73:389-394.
Question 71
An 11-year-old child has Ewing's sarcoma of the femoral diaphysis with a small soft-tissue mass. Staging studies show no evidence of metastases. Treatment should consist of
Explanation
The use of chemotherapy has dramatically improved survival rates of patients with Ewing's sarcoma. Local disease is best handled with wide resection to decrease local recurrence and to avoid the complications of radiation therapy (ie, secondary sarcomas). Radiation therapy alone is reserved for unresectable lesions or poor surgical margins. Amputation generally is not necessary. Toni A, Neff JR, Sudanese A, et al: The role of surgical therapy in patients with non-metastatic Ewing's sarcoma of the limbs. Clin Orthop 1991;286:225. Picci P, Rougraff BT, Bacci G, et al: Prognostic significance of histopathologic response to chemotherapy in non-metastatic Ewing's sarcoma of the extremities. J Clin Oncol 1993;11:1763.
Question 72
Second impact syndrome (SIS) after head injury is characterized by which of the following?
Explanation
SIS is a devastating but preventable complication of head injury. It occurs when return to activities is allowed prior to complete resolution of the symptoms of the first head injury. A second, sometimes trivial, head injury can lead to a devastating series of events that can result in sudden death. The symptoms tend to progress rapidly and often involve the brain stem. The prognosis is poor. Cantu RC: Second-impact syndrome. Clin Sports Med 1998;17:37-44. Saunders RL, Harbaugh RE: Second impact in catastrophic contact-sports head trauma. JAMA 1984;252:538-539.
Question 73
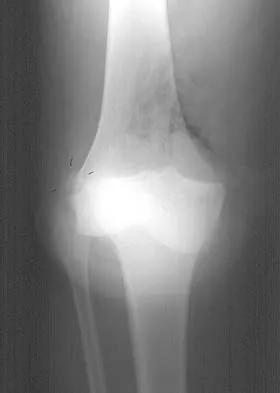
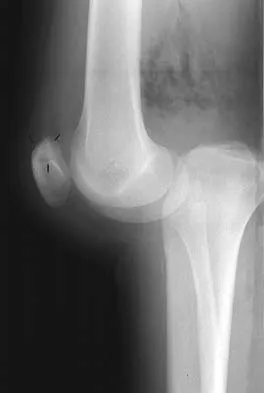
Figures 28a and 28b show AP and lateral radiographs of the knee. Based on these findings, which of the following structures has most likely been injured?
Explanation
The radiographs show a posterior knee dislocation. Knee dislocations almost always involve rupture of both the anterior and posterior cruciate ligaments. Collateral ligament injuries also are common. Arterial, nerve, and tendon injuries each occur in less than half of knee dislocations. Schenck RC Jr, Hunter RE, Ostrum RF, et al: Knee dislocations. Instr Course Lect 1999;48:515-522.
Question 74
A 46-year-old woman reports pain and a shortened appearance of her toe after undergoing a Keller resection arthroplasty 2 years ago for hallux rigidus. Examination reveals mild swelling and motion limited to 25 degrees at the metatarsophalangeal joint. Radiographs show large dorsal osteophytes on the first metatarsal head, 50% resection of the proximal phalanx, and complete loss of the metatarsophalangeal joint space. Which of the following is considered the most reliable procedure to improve her pain and the appearance of her toe?
Explanation
Because the patient has significant arthritis, arthrodesis is the treatment of choice. Adding a bone graft will prevent further shortening and add length to her toe, resulting in improved cosmesis. A cheilectomy will not alleviate her arthritis pain. The toe is too short for an effective Moberg phalangeal dorsiflexion osteotomy. A Waterman first metatarsal dorsal osteotomy will not address the degenerative joint disease or shortening. Silastic arthroplasty may help, but there is the risk of additional problems with foreign body reaction and a significant risk of failure known to occur with Silastic materials. Myerson MS, Schon LC, McGuigan FX, Oznur A:Result of arthrodesis of the hallux metatarsophalangeal joint using bone graft for restoration of length. Foot Ankle Int 2000;21:297-306. Mann RA, Coughlin MJ: Adult hallux valgus, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, pp 252-253.
Question 75
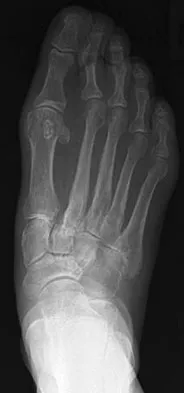
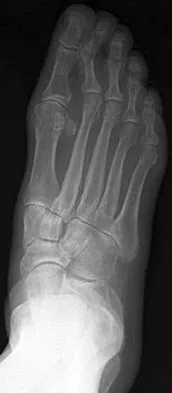
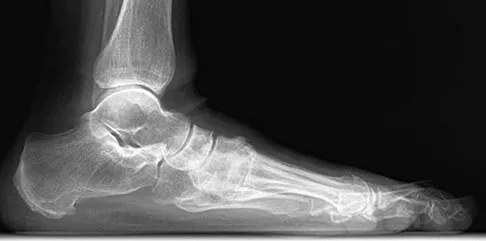
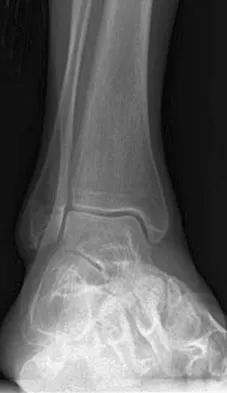
A 75-year-old woman reports foot pain and states that her foot has become progressively "flatter" in the past 3 years. Custom inserts and physical therapy have failed to provide relief. Examination reveals a flexible hindfoot and mild heel cord contracture. The patient is able to perform a single limb heel rise. Weight-bearing radiographs are shown in Figures 21a through 21d. What is the most appropriate surgical management?
Explanation
The patient has end-stage midfoot arthritis, with a secondary flatfoot deformity through the midfoot. The ability to perform a single limb heel rise indicates that the posterior tibial tendon is functioning, and the weight-bearing radiographs show normal calcaneal pitch and talar head coverage, thus confirming that the flatfoot deformity is isolated to the midfoot. Therefore, the most appropriate treatment is medial column arthrodesis and heel cord lengthening. The other listed procedures are not indicated because they are used in the management of adult flatfoot from posterior tibial tendon insufficiency. Toolan BC: Midfoot arthrodesis: Challenges and treatment alternatives. Foot Ankle Clin 2002;7:75-93.
Question 76
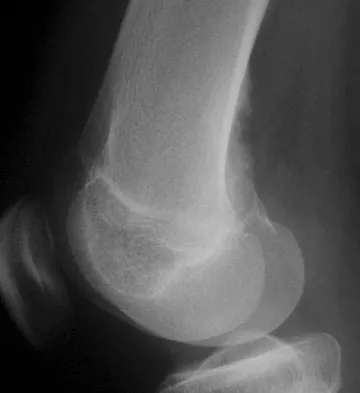
A 14-year-old girl reports bilateral patellofemoral symptoms. Based on the radiograph and MRI scans shown in Figures 23a through 23d, what is the next most appropriate step in management of the lesion?
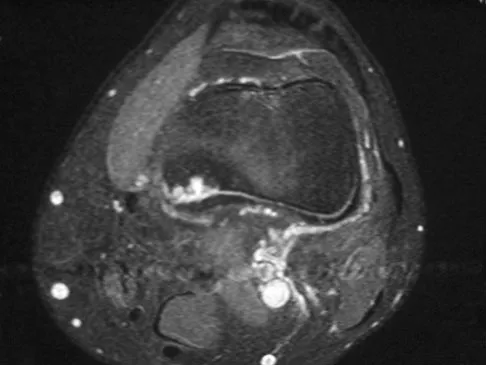
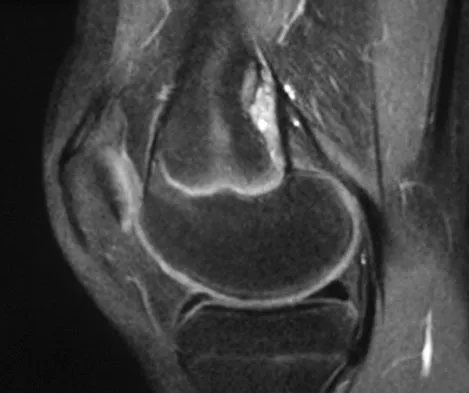
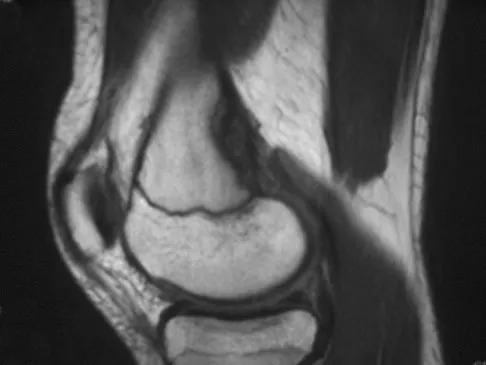
Explanation
A periosteal desmoid lesion is a tumor simulator. It is characterized by a bone irregularity along the posteromedial aspect of the distal femur at the insertion of the adductor magnus or the origin of the gastrocnemius muscle. It most commonly occurs in patients who are age 10 to 15 years. The lesions are asymptomatic, with no palpable mass, pain, or swelling. They are frequently an incidental finding when radiographs are obtained for nonspecific symptoms or trauma about the knee. Following recognition of the characteristic imaging findings, observation is the management of choice. Dunham WK, Marcus NW, Enneking WF, et al: Developmental defects of the distal femoral metaphysis. J Bone Joint Surg Am 1980;62:801-806.
Question 77
The primary function of structure "A" in Figure 29 is to limit
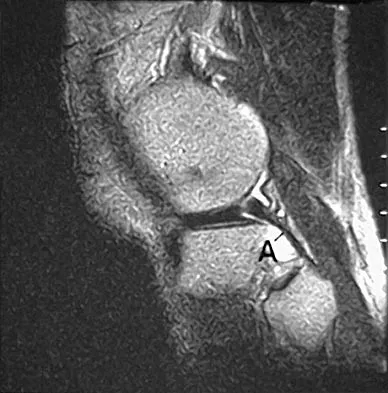
Explanation
The primary function of the popliteofibular ligament is to resist posterolateral rotation of the tibia on the femur, although it also secondarily resists varus angulation and posterior displacement of the tibia on the femur. The posterior cruciate ligament resists posterior tibial displacement, especially at 90 degrees of flexion. The lateral collateral ligament primarily resists varus displacement at 30 degrees of flexion but also resists posterolateral rotatory displacement with flexion that is less than approximately 50 degrees. The anterior and posterior cruciate ligaments resist varus displacement (along with the lateral collateral ligament) at 0 degrees of flexion. The anterior cruciate ligament primarily resists anterolateral displacement of the tibia on the femur. Sugita T, Amis AA: Anatomic and biomechanical study of the lateral collateral and popliteofibular ligaments. Am J Sports Med 2001;29:466-472.
Question 78
A 19-year-old woman reports lower back pain following a motor vehicle accident. Radiographs obtained immediately after the accident and a bone scan obtained 4 weeks later are shown in Figures 25a through 25c. The patient asks questions regarding the cause, genetics, and natural history of her condition. She should be informed that the condition was
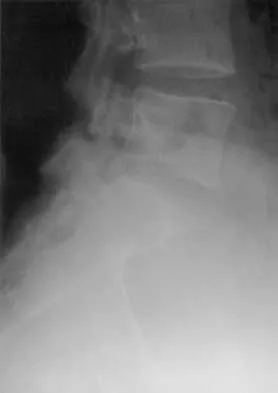
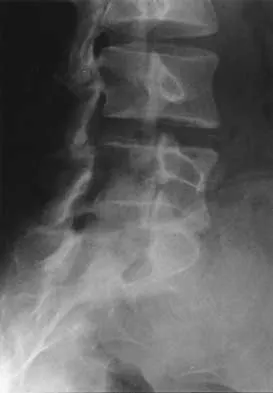
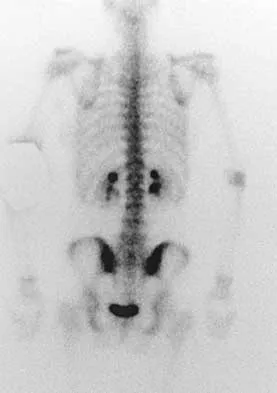
Explanation
The radiographs show L5 spondylolysis without spondylolisthesis (slip). The bone scan is normal, indicating that the pars interarticularis fractures are not acute. The incidence of spondylolysis is approximately 5% in the general population. The lesion generally develops in children age 5 to 6 years, and there is a second peak in the adolescent population. There is a familial predisposition, with reported rates of 27% to 69% in close relatives. A recent long-term follow-up study found that 90% of the spondylolisthesis had occurred before the patient's first visit to the physician. Spondylolisthesis tends to progress during the initial growth spurt and is similar in some respects to idiopathic scoliosis. Progression of a lytic spondylolysis to spondylolisthesis in adulthood has been reported; however, this is exceedingly rare. Lauerman WC, Cain JE: Isthmic spondylolisthesis in the adult. J Am Acad Orthop Surg 1996;4:201-208. Hensinger RN: Spondylolysis and spondylolisthesis in children and adolescents. J Bone Joint Surg Am 1989;71:1098-1107. Seitsalo S, Osterman K, Hyvarinen H, Tallroth K, Schlenzka D, Poussa M: Progression of spondylolisthesis in children and adolescents: A long-term follow-up of 272 patients. Spine 1991;16:417-421.
Question 79
A 21-year-old man is referred for evaluation of a lesion in the left proximal femur that was discovered when he was undergoing an upper gastrointestinal series. He reports no hip or thigh pain. Radiographs are shown in Figures 64a and 64b. What is the best course of action?
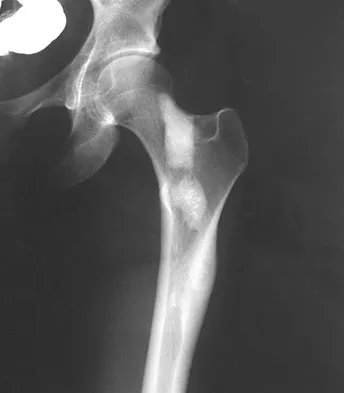
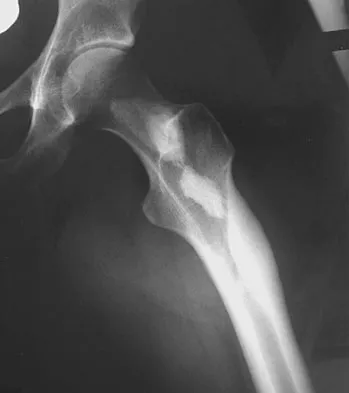
Explanation
Melorheostosis is a rare disorder characterized by the classic radiographic appearance of flowing hyperostosis in a long bone. The hyperostosis may be on the periosteal or endosteal surface of the bone and frequently gives the appearance of wax falling down the side of a candle. The radiographs are diagnostic; therefore, no further work-up is indicated. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 87-102.
Question 80
A 15-year-old diver has had persistent, activity-related low back pain for the past 2 months. He denies any history of trauma. Examination reveals that the pain is localized to the lumbosacral junction, and there are no radicular symptoms. The pain is worse with back extension. Neurologic examination is normal, as are AP, lateral, and oblique radiographs of the lumbosacral spine. Further evaluation should include
Explanation
Spondylolysis may develop as a stress fracture resulting from repetitive hyperextension during athletic activities. In young people, the pars interarticularis is thin, the neural arch has not yet reached maximum strength, and the intravertebral disk is less resistant to shear. While clinical symptoms may lead to the suspicion of spondylolysis, radiographic confirmation may be difficult in early cases. Plain radiographs may be negative initially, and the plain MRI scan may not offer good visualization of the pars. A bone scan with SPECT is very sensitive initially. CT scans with regular axial and reverse-gantry angled cuts may help determine the type of fracture and the course of treatment. Congeni J, McCulloch J, Swanson K: Lumbar spondylolysis: A study of natural progression in athletes. Am J Sports Med 1997;25:248-253.
Question 81
What acetabular procedure for developmental dysplasia of the hip does not require a concentric reduction of the femoral head in the acetabulum?
Explanation
All of the reorientation innominate osteotomies require a concentric reduction of the hip. The Staheli shelf procedure may be performed even with the hip subluxated, but it is a salvage procedure that covers a portion of the femoral head with capsular fibrocartilage rather than hyaline cartilage. Staheli LT, Chew DE: Slotted acetabular augmentation in childhood adolescence. J Pediatr Orthop 1992;12:569-580.
Question 82
A 3-year-old boy sustains a complete paralysis following a high thoracic spinal cord injury consistent with a SCIWORA-type injury (spinal cord injury without radiographic abnormality). Subsequent progressive spinal deformity will develop in what percent of patients with this injury?
Explanation
Spinal cord injury in skeletally immature patients almost always leads to the development of paralytic spinal deformity. The age at injury is the most important factor affecting the development of scoliosis. Spinal cord injury that occurs more than 1 year prior to skeletal maturity is almost always followed by the development of scoliosis. In one study, scoliosis developed in 100% of children who were younger than age 10 years at the time of spinal cord injury. Scoliosis can occur after injury at any level. Spasticity is often a contributing factor. Up to two thirds of patients who have paralytic scoliosis prior to skeletal maturity will eventually require surgery for curve control. Mayfield JK, Erkkila JC, Winter RB: Spine deformity subsequent to acquired childhood spinal cord injury. J Bone Joint Surg Am 1981;63:1401-1411. Lancourt JE, Dickson JH, Carter RE: Paralytic spinal deformity following traumatic spinal cord injury in children and adolescents. J Bone Joint Surg Am 1981;63:47-53.
Question 83
Ganglion cysts about the wrist most commonly arise from what structure?
Explanation
Ganglion cysts are the most common mass or mass-like lesions seen in the hand and wrist. They arise in a variety of locations, including synovial joints or tendon sheaths. The most common location is the dorsal/radial wrist arising from the dorsal scapholunate interosseous ligament.
Question 84
Figures 29a and 29b show a clinical photograph and radiographs of a patient who sustained an open calcaneus fracture in a motor vehicle accident. The patient received immediate IV antibiotics and an emergent irrigation and debridement. The swelling has subsided by 3 weeks and the medial wound is clean. What do you tell the patient about the likelihood of infection if a formal open reduction and internal fixation via a lateral approach is performed?
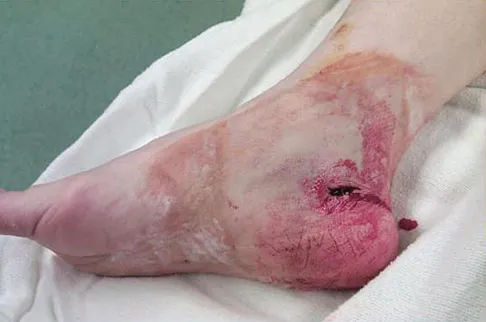
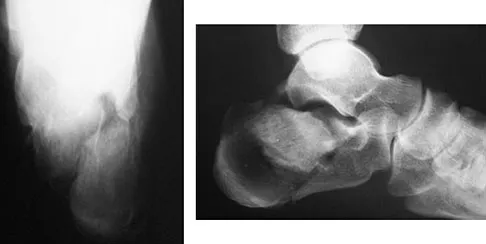
Explanation
Multiple authors have shown similar infection rates for grade 1 and 2 open medial fractures and closed fractures that have been treated with an extensile lateral approach and open reduction and internal fixation. Patients only need IV antibiotics for 2 to 3 days after surgery. Formal open reduction and internal fixation is not recommended for grade 3 medial wounds and most lateral wounds. Heier KA, Infante AF, Walling AK, et al: Open fractures of the calcaneus: Soft-tissue injury determines outcome. J Bone Joint Surg Am 2003;85:2276-2282.
Question 85
An excessively large radial styloidectomy poses a risk for wrist instability. What ligament is at greatest risk for injury?
Explanation
The radioscaphocapitate ligament is the most radial of the extrinsic volar ligaments of the wrist. It has a mean attachment to the radius 4 mm from the tip of the radial styloid. Nakamura T, Cooney WP III, Lui WH, et al: Radial styloidectomy: A biomechanical study on the stability of the wrist joint. J Hand Surg Am 2001;26:85-93.
Question 86
What is the most likely late complication associated with cementless total knee replacement?
Explanation
In cementless total knee replacement, the risk of osteolysis is 30% if both components are placed without cement and screws are used for tibial fixation. The risk is 10% when a cemented tibial component is used, and the risk is 0% when both components are cemented. Loss of motion, patellofemoral pain, heterotopic bone formation, and patellar clunk are complications that can occur after cemented or cementless components are placed.
Question 87
A 74-year-old man reports progressive left hip pain with weight-bearing activities. A radiograph is shown in Figure 30. What is the most likely underlying diagnosis?
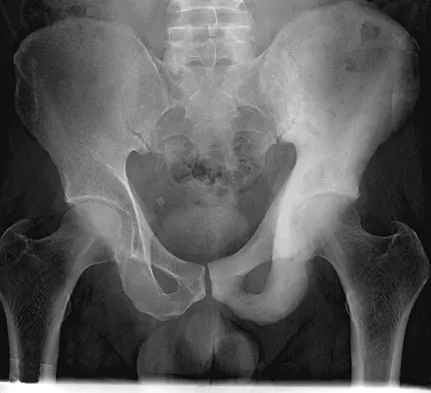
Explanation
The radiograph shows enlargement of the bone, coarse trabeculation, a blastic appearance, and thickening of the cortex, revealing the classic appearance of Paget's disease in the sclerotic phase, the most common presentation. While lymphoma may present as a blastic lesion, it will not have the same enlargement, coarse trabeculation of bone, and the significant sclerosis seen here. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 211-215.
Question 88
A 45-year-old man who underwent an ankle arthrodesis reports that for the first 6 years he had significant pain relief after the fusion healed. However, he now has increasing pain in the sinus tarsi. AP and lateral radiographs are shown in Figures 8a and 8b. What is the most likely cause of the patient's symptoms?
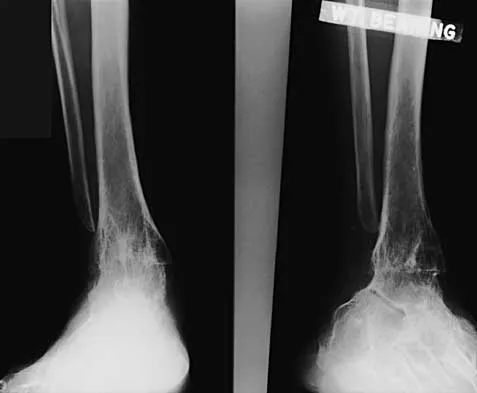
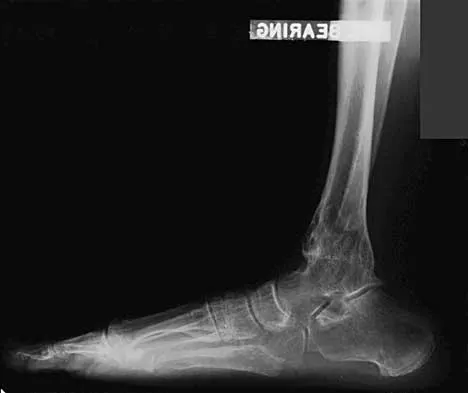
Explanation
The patient has a solid ankle fusion radiographically. With a tibiotalar arthrodesis, the adjacent joints (subtalar and transverse tarsal) take additional stress. Over time, progressive degenerative arthritis will occur in these adjacent joints, often necessitating further surgery. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 613-631.
Question 89
A 59-year-old woman underwent open reduction and internal fixation (ORIF) of her ankle 6 months ago, with subsequent hardware removal 3 months later. She now reports persistent, diffuse ankle pain, swelling, and limited range of motion. Figure 48 shows an oblique radiograph of the ankle. What is the next most appropriate step in management?
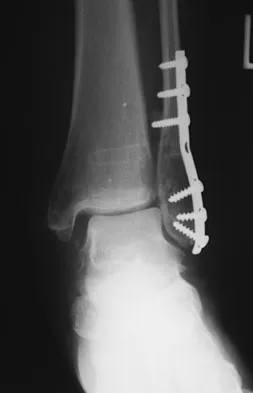
Explanation
The radiographs demonstrate persistent widening of the medial clear space with an ossicle. This represents soft-tissue interposition-scar tissue, the deltoid ligament, or the posterior tibialis tendon. Physical therapy will not improve the symptomatic malalignment. Hardware removal would be indicated for pain localized to the lateral fibula. Repeat syndesmotic screw fixation alone will not reduce the malalignment. Deltoid ligament repair may be necessary but will need to be combined with debridement of the medial ankle and syndesmosis, as well as repeat placement of one or more syndesmotic screws to maintain the reduction. Weening B, Bhandari M: Predictors of functional outcome following transsyndesmotic screw fixation of ankle fractures. J Orthop Trauma 2005;19:102-108.
Question 90
A 59-year-old man underwent interposition arthroplasty for osteoarthritis of the elbow 9 years ago. Over the past year the patient has had increasing pain and elbow instability. There is no clinical evidence of infection, and radiographs show no new bony process. What is the best option for this patient?
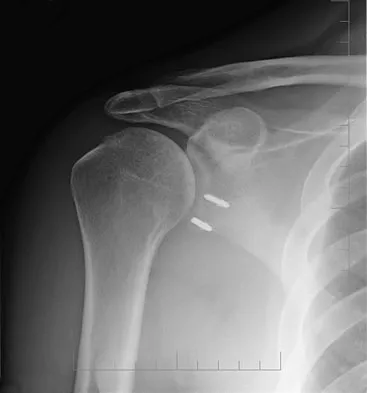
Explanation
In a series reported by Blaine and associates, 12 patients were converted from interposition to total elbow arthroplasty. This procedure was successful in 10 out of 12 patients. Blaine TA, Adams R, Morrey BF: Total elbow arthroplasty after interposition arthroplasty for elbow arthritis. J Bone Joint Surg Am 2005;87;286-292.
Question 91
When performing surgical excision of the lesion shown in the MRI scan in Figure 3, what nerve is most likely at risk?
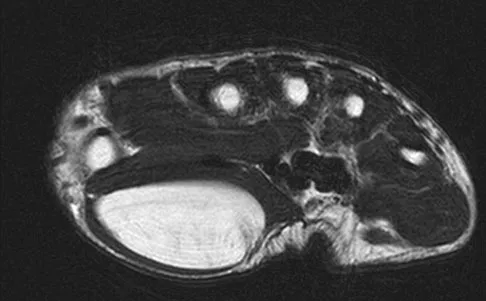
Explanation
The MRI scan shows a large mass (lipoma) in the thenar muscles of the palm. The recurrent motor branch of the median nerve innervates the thenar muscles. The anterior interosseous nerve (AIN) in the proximal forearm innervates the flexor pollicis longus, pronator quadratus, and flexor digitorum pollicis to the index and frequently the middle finger. The terminal branch of the AIN innervates only the wrist capsule. The palmar cutaneous branch of the ulnar nerve is a sensory structure to the hypothenar area. There is no commonly described recurrent branch of the ulnar nerve.
Question 92
What is the relative amount of type II collagen synthesis in disease-free adult articular cartilage compared to developing teenagers?
Explanation
Adult articular cartilage has less than 5% of the synthesis rate of type II collagen than that seen in developing teenagers. Both synthesis and degradation of type II collagen in normal adult articular cartilage is very low compared to children. In osteoarthrosis, both synthesis and degradation are increased, but the collagen does not properly incorporate into the matrix. Lippiello L, Hall D, Mankin HJ: Collagen synthesis in normal and osteoarthritic human cartilage. J Clin Invest 1977;59:593-600.
Question 93
A 5-year-old boy has had midfoot pain with activity for the past 3 months. He has no pain at rest. Radiographs are shown in Figures 29a and 29b. Management should consist of
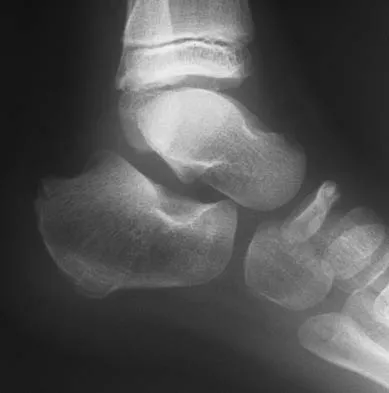
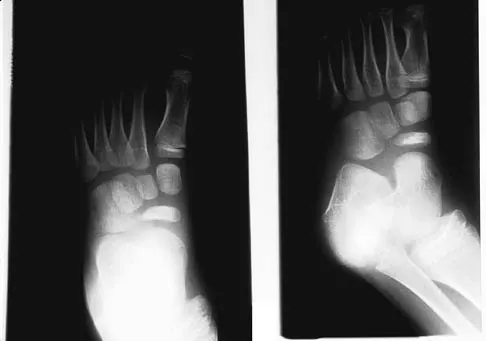
Explanation
The radiographs show classic findings for Koehler's disease (osteochondrosis of the navicular). The patient's age and clinical history are typical for this self-limiting condition. Patients will improve with time, but the duration of symptoms is much shorter if the patient is placed in a cast. There is no role for surgery in this disease.
Question 94
A 40-year-old patient who has a type II odontoid fracture is placed in a halo vest for 12 weeks; however, current radiographs show no evidence of healing. The next most appropriate step in management should consist of
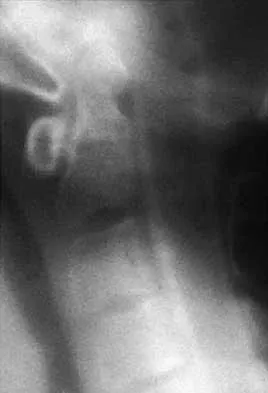
Explanation
Because nonsurgical managment has failed and a significant number of type II odontoid fractures will go on to a nonunion, the salvage treatment of choice is posterior fusion at C1-2. Odontoid screws are contraindicated in patients with a chronic nonunion, which this patient has at the end of 3 months. Montesano PX: Anterior and posterior screw and plate techniques used in the cervical spine, in Bridwell KH, DeWald RL (eds): The Textbook of Spinal Surgery, ed 2. Philadelphia, PA, Lippincott-Raven, 1996, vol 2, pp 1743-1761. Bohler J: Anterior stabilization for acute fractures and non-unions of the dens. J Bone Joint Surg Am 1982;64:18-27.
Question 95
The arrows in the axial T1-weighted MRI scan shown in Figure 25 show which of the following structures?
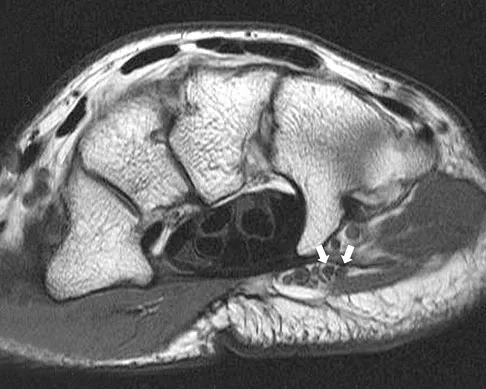
Explanation
The arrows in the figure show the deep branch of the ulnar nerve (more radial) and the superficial branch of the ulnar nerve within Guyon's canal. Guyon's canal is approximately 4 cm long beginning at the proximal extent of the transverse carpal ligament and ends at the aponeurotic arch of the hypothenar muscles. Many structures comprise the boundaries of Guyon's canal. The floor, for example, consists of the transverse carpal ligament, the pisohamate and pisometacarpal ligaments, and the opponens digiti minimi. Within Guyon's canal, the ulnar nerve bifurcates into the superficial and deep branches. The ulnar artery is immediately adjacent and radial to the ulnar nerve. The median nerve is visualized within the carpal tunnel, and the palmar cutaneous branch is more radial to Guyon's canal and volar to the carpal tunnel. The radial and ulnar digital nerves to the little finger are branches off of the superficial branch of the ulnar nerve distal to its emergence from Guyon's canal. The ulnar artery is the round structure located radial to the branches of the ulnar nerve within Guyon's canal. Adjacent to the ulnar artery are two small veins. The dorsal cutaneous branch of the ulnar nerve branches from the ulnar nerve in the distal forearm, well proximal to Guyon's canal. The common digital artery to the fourth web branches from the superficial palmar arch distal to Guyon's canal. The hook of the hamate is clearly seen in the figure, orienting the observer to the ulnar side of the wrist. Gross MS, Gelberman RH: The anatomy of the distal ulnar tunnel. Clin Orthop Relat Res 1985;196:238-247.
Question 96
Figures 35a and 35b show the axial T2-weighted and coronal T1-weighted MRI scans of a patient who has enlargement of the right thigh. What is the most likely diagnosis?
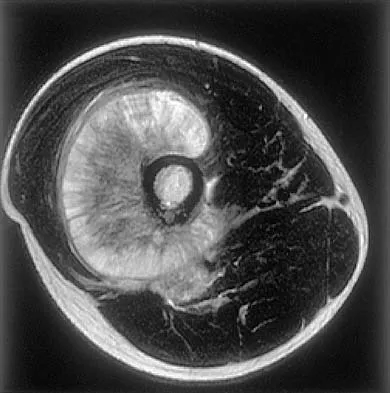
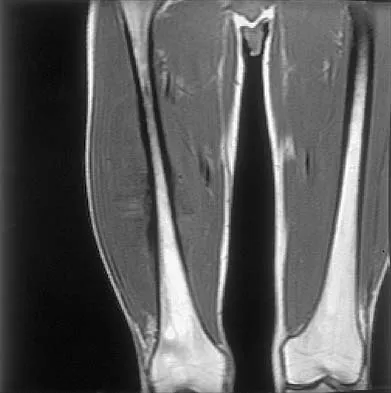
Explanation
The images show a large, almost circumferential, mass surrounding the diaphysis of the femur. The intramedullary signal is normal with minimal cortical destruction, both findings that should be abnormal in conventional osteosarcoma and Ewing's sarcoma. There are very low-signal striations representing osteoid formation that would have a sunburst radiographic pattern. This indicates an osteogenic lesion. Myositis ossificans is not indicated because studies would reveal zonal ossification starting in the periphery rather than the more central pattern seen in this patient. This appearance is typical for periosteal osteosarcoma.
Question 97
A 14-year-old boy reports pain in the distal thigh. He denies any history of trauma. Examination reveals tenderness and swelling of the distal thigh without effusion. A radiograph and CT scan are shown in Figures 10a and 10b. A biopsy specimen is shown in Figure 10c. Management should consist of
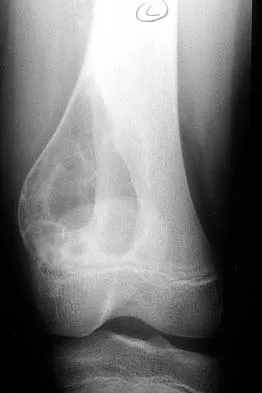
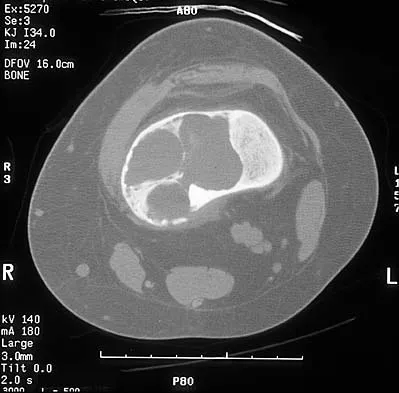
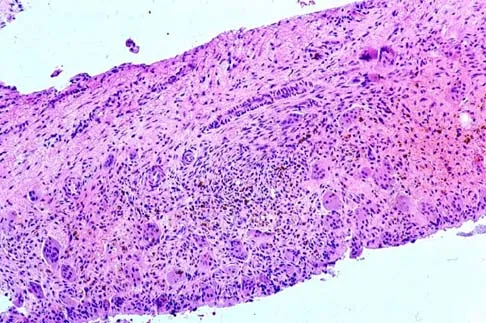
Explanation
Based on these findings, the patient has an aneurysmal bone cyst. Frequently, fluid-fluid levels can be detected on MRI or CT images. The histologic results show a lesion that consists of cavernous spaces filled with blood. The lining of the cavity contains spindle cells, multinucleated giant cells, and reactive bone. Curettage and bone grafting is the preferred treatment method. Without treatment, these lesions can become quite large and destructive. Radiation therapy is not recommended for resectable lesions. Chemotherapy is not required for these benign lesions. Simon MA, Springfield DS, et al: Common Benign Bone Tumors: Surgery for Bone and Soft Tissue Tumors. Philadelphia, PA, Lippincott Raven, 1998, pp 194-200.
Question 98
The modified Brostrom lateral ankle ligamentous reconstruction uses which of the following structures to provide supplementary stabilization?
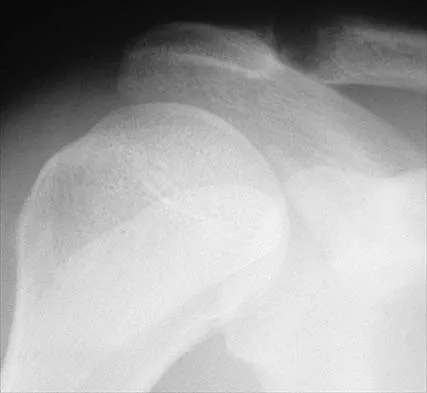
Explanation
The modified Brostrom lateral ankle ligament stabilization procedure uses the remnants of the anterior talofibular and the calcaneofibular ligaments, supplemented by the inferior retinaculum and the transferred talocalcaneal ligament to stabilize the lateral ankle. Chrisman and associates described the use of one half of the peroneus brevis. Watson-Jones and Evans used the entire peroneus brevis. The peroneus longus has been taken by mistake. The plantaris has been used in triligamentous reconstruction. Gould N, Seligson D, Gassman J: Early and late repair of lateral ligament of the ankle. Foot Ankle 1980;1:84-89. Hamilton WG, Thompson FM, Snow SW: The modified Brostrom procedure for lateral ankle instability. Foot Ankle 1993;14:1-7. Chrisman OD, Snook GA: Reconstruction of lateral ligament tears of the ankle: An experimental study and clinical evaluation of seven patients treated by a new modification of the Elmslie procedure. J Bone Joint Surg Am 1969;51:904-912. Evans DL: Recurrent instability of the ankle: My method of surgical treatment. Proc R Soc Med 1953;46:343. Watson-Jones R: Fractures and Joint Injuries, ed 3. Baltimore, MD, Williams and Wilkins, 1946, p 234.
Question 99
A 10-month-old boy has multiple skeletal lesions and a skin rash that he has had since he was a newborn. Based on the radiographs and biopsy specimens shown in Figures 79a through 79d, what is the most likely diagnosis?
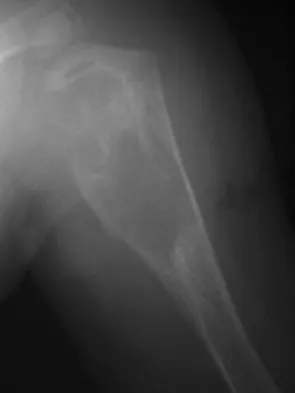
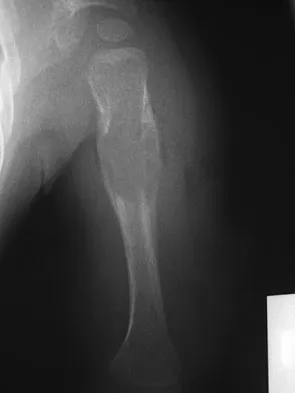
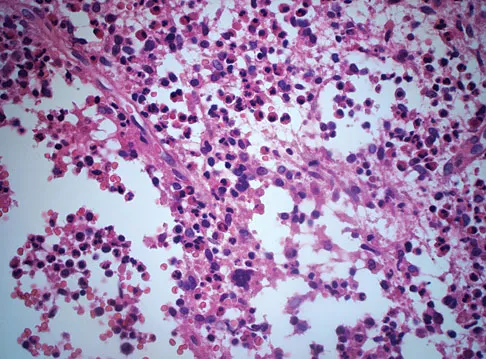
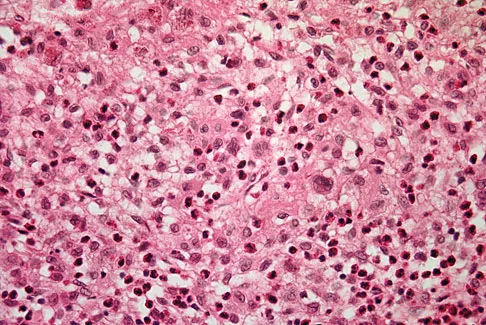
Explanation
Langerhans cell histiocytosis or eosinophilic granuloma is a nonneoplastic lesion that is part of a spectrum of clinical diseases featuring histiocytes. Most occur during the first two decades of life within any bone. Radiographs show a radiolucent lesion, frequently diaphyseal in location. A periosteal response is occasionally seen and can resemble more aggressive lesions such as osteomyelitis or Ewing's sarcoma. Histology demonstrates CD1a positive histiocytes with large oval-shaped nuclei with indentation, and a variable presence of eosinophils. Plasschaert F, Craig C, Bell R, et al: Eosinophilic granuloma: A different behaviour in children than in adults. J Bone Joint Surg Br 2002;84:870-872.
Question 100
A 68-year-old woman has been progressing slowly after undergoing humeral head replacement for a four-part fracture 3 months ago. She has not regained active elevation, she feels an audible clunk on attempting elevation, and she reports pain and weakness. She used a sling for 2 weeks in the immediate postoperative period. Radiographs are shown in Figure 37a through 37c. Management should consist of
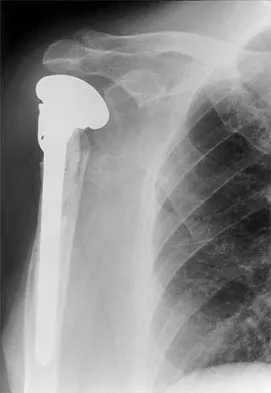
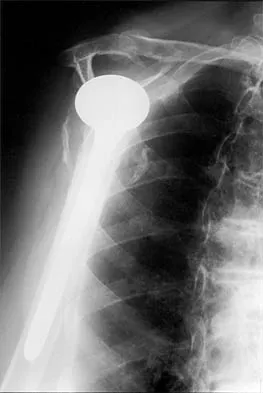
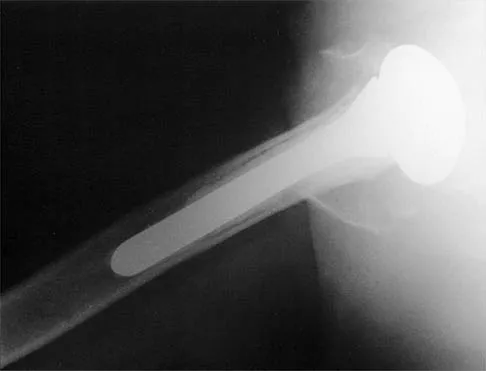
Explanation
Immediate repair of the tuberosity and rotator cuff is recommended on identifying the avulsion or nonunion. Revising the humeral component to increase tension and length will overtighten the cuff and increase the chance of tuberosity pull-off. The glenoid is uninvolved and should not be replaced. Attempts to strengthen the rotator cuff will be unsuccessful because the insertions are no longer attached to the humerus when the tuberosities avulse. Brown TD, Bigliani LU: Complications with humeral head replacement. Orthop Clin North Am 2000;31:77-90.
