Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 75-year-old patient returns for follow-up after undergoing bilateral total hip arthroplasty (THA). The right hip is a hybrid THA performed 12 years ago, whereas the left hip is a cementless THA performed 10 years ago. Both acetabular components are the same type, same size, and from the same manufacturer. Both femoral heads are 28-mm cobalt-chromium components. What is the most likely explanation for the advanced polyethylene wear in one hip?
Explanation
Over the past three decades, gamma irradiation and air has been the most common method of sterilizing polyethylene used in total joint arthroplasty. This method of sterilization results in breakage of the chemical bonds within the polymer. While this promotes cross-linking, it also leaves the polyethylene vulnerable to oxidation, especially if packaged in an air environment. Oxidation has been shown to decrease polyethylene's molecular weight, ultimate tensile strength, elongation, and toughness which results in a stiffer, more brittle material that is less resistant to wear. Severity of oxidation and a decrease in mechanical properties have been shown to be related to the length of time that the component is exposed to air (the shelf life). Currier and associates studied the clinical performance of gamma irradiated in air polyethylene components that had been shelf aged. They demonstrated that for the first 5 years of shelf life, polyethylene oxidized rather slowly. However, polyethylene components with a shelf life of more than 5 years would be expected to have minimal mechanical toughness and would likely fail rapidly if implanted. Bohl and associates evaluated 135 patients who had undergone total knee arthroplasty. Survivorship at 5 years was 100% for components with a shelf life of less than 4 years, 89% for components with a shelf life of 4 to 8 years, and 79% for components with a shelf life of more than 8 years. Sychterz and associates reported no correlation between shelf life and true wear rates for components with a shelf life of less than 3 years. In summary, both in vivo and in vitro data suggest that shelf life in excess of 3 to 5 years has a direct effect on wear of polyethylene. Currier BH, Currier JH, Collier JP, et al: Shelf life and in vivo duration: Impacts on performance of tibial bearings. Clin Orthop 1997;342:111-122. Bohl JR, Bohl WR, Postak PD, et al: The Coventry Award: The effects of shelf life on clinical outcome for gamma sterilized polyethylene tibial components. Clin Orthop 1999;367:28-38.
Question 2
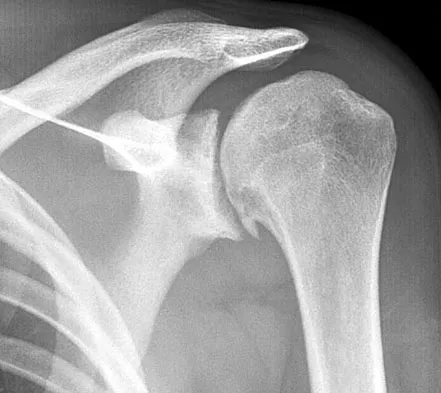
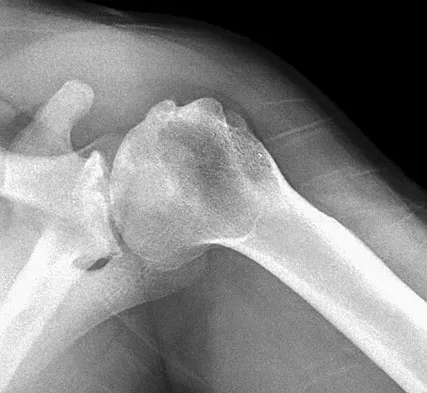
A 40-year-old right hand-dominant construction worker has had a 6-month history of aching left shoulder pain that is worse after working a long day. Examination reveals limited range of motion and good strength when compared to his asymptomatic right arm. He has not had any orthopaedic intervention to date. Radiographs are shown in Figures 43a and 43b. What is the most appropriate treatment?
Explanation
The patient is a young laborer with osteoarthritis. Initial treatment should begin with nonsurgical management that may include anti-inflammatory drugs, cortisone injections, and physical therapy to diminish pain and improve motion. The other choices may eventually be necessary but should only follow a course of nonsurgical management. Norris TR (ed): Orthopaedic Knowledge Update: Shoulder and Elbow 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 257-266.
Question 3
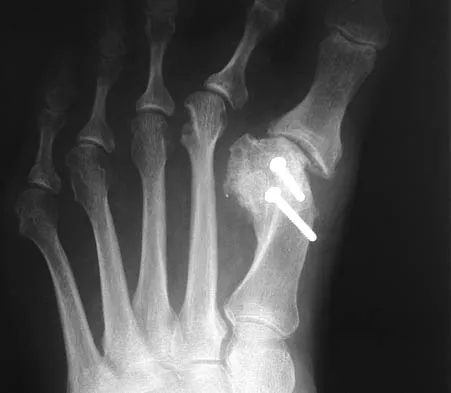
A 7-year-old boy sustained an acute puncture wound of the foot after stepping barefoot on a piece of glass 1 day ago. His mother states that she is not sure if she got the piece of glass out; however, she reports that his immunizations are up-to-date. Examination reveals that the wound is slightly erythematous, less than 1 mm in length on the heel, and is not currently draining. What is the next most appropriate step im management?
Explanation
The child has an up-to-date tetanus; therefore, a booster is not recommended. Pseudomonas coverage is most likely not needed because the child was barefoot. It is too early to evaluate for abscess or osteomyelitis with MRI, and a formal debridement is rarely indicated without signs of an abscess or a retained foreign body. Radiographs with soft-tissue penetration should be obtained to check for a retained foreign body. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 199-205.
Question 4
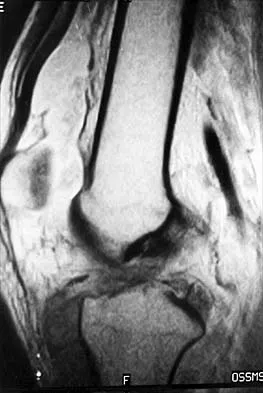
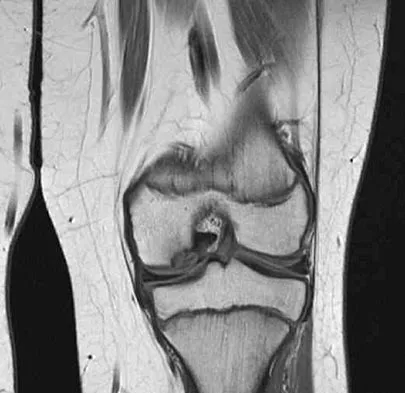
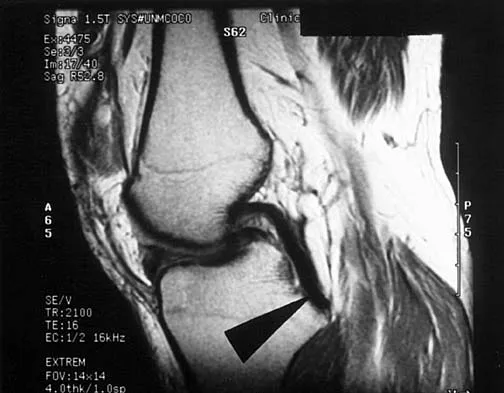
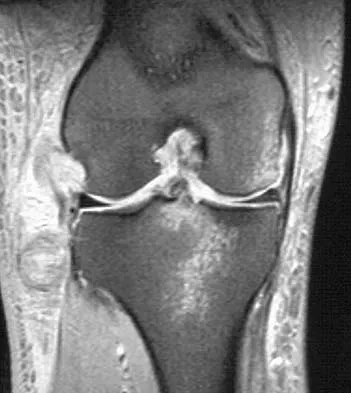
Figure 50 shows the MRI scan of a 20-year-old female college soccer player with knee pain. What is the most likely diagnosis?
Explanation
The MRI scan shows an acute complete tear of the posterior cruciate ligament. No evidence is seen of a quadriceps tendon rupture, a tibia fracture, or a bone contusion. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 533-557.
Question 5
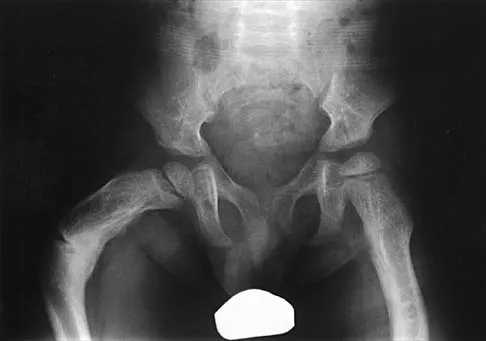
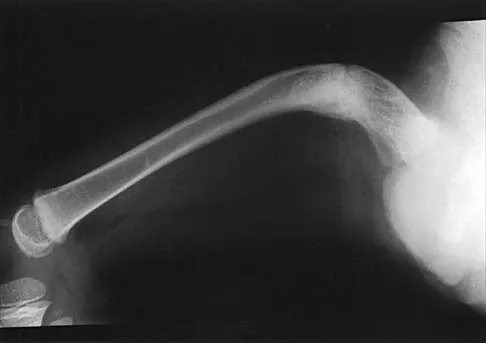
Figures 35a and 35b show the radiographs of a 7-year-old patient who has progressive deformity of the right thigh accompanied by a dull persistent pain radiating to the knee. Examination reveals an obvious bulge in the right thigh, with flexion of the hip beyond 50 degrees only if the hip is allowed to externally rotate. Management should consist of
Explanation
The patient has radiographic signs of osteogenesis imperfecta, including osteopenia, mild acetabular protrusio, cortical thinning, and bowing associated with anterior stress fracturing. The treatment of choice is correction of the bow with osteotomies, followed by intramedullary fixation to prevent further deformity. Biphosphonates, such as pamidronate, may be useful in increasing bone density and preventing fractures. Large multicenter studies on biphosphonate efficacy are currently in progress. Zionts LE, Ebramzadeh E, Stott NS: Complications in the use of the Bailey-Dubow extensible nail. Clin Orthop 1998;348:186-195. Luhmann SJ, Sheridan JJ, Capelli AM, Schoenecker PL: Management of lower-extremity deformities in osteogenesis imperfecta with extensible intramedullary rod technique: A 20-year experience. J Pediatr Orthop 1998;18:88-94.
Question 6
A 7-year-old child is unresponsive, tachycardic, and has a systolic blood pressure of 50 mm Hg after being struck by a car. The patient is intubated and venous access is obtained. The secondary survey reveals an unstable pelvis. Despite adequate resuscitation, the patient continues to be hemodynamically unstable. What is the best course of action?
Explanation
The patient is hemodynamically unstable, so any treatment should be aimed at stabilization. Airway, breathing, and circulation are the most important areas to control initially; the patient has been intubated and has adequate venous access. Despite fluid resuscitation, the child remains hypotensive, indicating continued blood loss. With an unstable pelvic fracture there can be significant hemorrhage. Decreasing the pelvic volume can decrease blood loss related to the pelvic fracture. This can be done in the emergency department by applying a pelvic sling. Other means of decreasing pelvic volume include a pelvic clamp, a simple anterior frame pelvic external fixator, or a simple sheet tied around the pelvis. These maneuvers may stabilize the patient so that further evaluation and treatment can be undertaken. All of the other choices will delay stabilization and should be postponed until the patient is stabilized. Torode I, Zieg D: Pelvic fractures in children. J Pediatr Orthop 1985;5:76-84. Eichelberger MR, Randolph JG: Pediatric trauma-initial resuscitation, in Moore EE, Eisman B, Van Way CE (eds): Critical Decisions in Trauma. St Louis, MO, CV Mosby, 1984, p 344.
Question 7
A 2-year-old girl has had a 2-day history of fever and refuses to move her left shoulder following varicella. Laboratory studies show an erythrocyte sedimentation rate of 75 mm/h and a peripheral WBC count of 18,000/mm3. What is the most common organism in this scenario?
Explanation
The most common bacterial etiologic agent following varicella is group A beta-hemolytic streptococcus. The other organisms are much less common. Staphylococcus aureus is the most common bone infection organism. Staphylococcus epidermidis is increasingly a bone infection organism. Group B streptococcus occurs more commonly in newborns. Kingella kingae is a common joint pathogen but is not as common following varicella. Schreck P, Schreck P, Bradley J, et al: Musculoskeletal complications of varicella. J Bone Joint Surg Am 1996;78:1713-1719.
Question 8
A 16-year-old female swimmer reports several episodes of atraumatic glenohumeral instability that occur with different arm positions. Examination reveals generalized ligamentous laxity and a positive sulcus sign, and her shoulder can be subluxated both anteriorly and posteriorly. Initial management should consist of
Explanation
The patient has multidirectional instability (MDI). It has been reported that a high percentage of patients with MDI respond to a properly structured exercise program that is continued for at least 3 to 6 months. If nonsurgical management fails to provide relief, stabilization with an inferior capsular shift procedure has been effective in a high percentage of patients. Unidirectional repairs, such as the Putti-Platt procedure, are unsuitable for correcting MDI. Thermal capsulorrhaphy has been reported to have a very high failure rate (greater than 50%) for treating MDI. Burkhead WZ Jr, Rockwood CA Jr: Treatment of instability of the shoulder with an exercise program. J Bone Joint Surg Am 1992;74:890-896. Neer CS II, Foster CR: Inferior capsular shift for involuntary inferior and multidirectional instability of the shoulder: A preliminary report. J Bone Joint Surg Am 1980;62:897-908. Pollock RG, Owens JM, Flatow EL, et al: Operative results of the inferior capsular shift procedure for multidirectional instability of the shoulder. J Bone Joint Surg Am 2000;82:919-928.
Question 9
The preferred surgical approach to the elbow of a child with an irreducible type III supracondylar distal humerus fracture and pulseless extremity is through which of the following muscle intervals?
Explanation
In a type III supracondylar distal humerus fracture of the elbow, the brachial artery can become incarcerated, yielding a pulseless extremity. In this situation, closed reduction may not be effective; therefore, open management is often necessary. The preferred surgical approach to the brachial artery and to this fracture is the anterior approach to the cubital fossa. The lacertus fibrosis is incised, and the dissection is carried out between the brachialis (musculocutaneous nerve) and the pronator teres (median nerve), mobilizing the brachial artery. Once the brachial artery is mobilized, the anterior elbow joint capsule may be exposed. The interval between the brachialis and the biceps describes the anterolateral approach to the elbow more commonly used for exposure of the proximal aspect of the posterior interosseous nerve. The dissection interval between the brachioradialis and the pronator teres describes the proximal extent of the anterior approach to the radius. Tubiana R, McCullough CJ, Masquelet AC: An Atlas of Surgical Exposures of the Upper Extremity. Philadelphia, PA, JB Lippincott, 1990, p 115.
Question 10
A 16-year-old girl has had anterior leg pain and a mass for the past 8 months. Figures 2a and 2b show a radiograph and an H & E histologic specimen. Which of the following disorders is believed to be a precursor of this lesion?
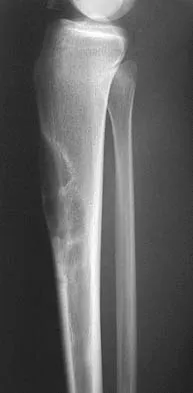
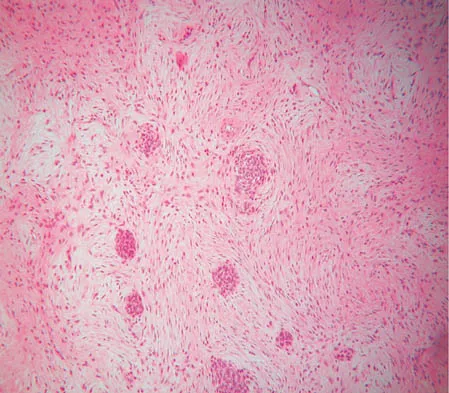
Explanation
The radiograph and pathology are consistent with adamantinoma. While the mechanism underlying adamantinoma has not been identified, it is believed to be closely related to osteofibrous dysplasia, which may represent a precursor. The other diagnoses are not known to give rise to adamantinoma.
Question 11
Figure 21 shows the radiograph of an 18-year-old man who was brought to the emergency department with shoulder pain following a rollover accident on an all-terrain vehicle. Examination reveals a fracture with massive swelling; however, the skin is intact and not tented over the fracture. Based on these findings, initial management should consist of
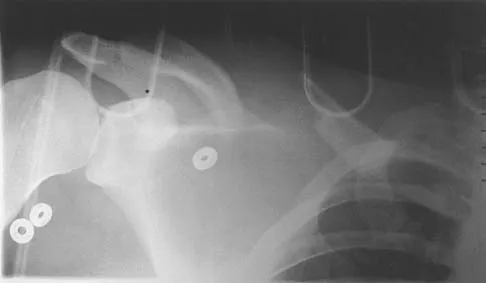
Explanation
The radiographic and clinical findings suggest a scapulothoracic dissociation with a widely displaced clavicular fracture and a laterally displaced scapula. These injuries have a high association with neurovascular injuries to the brachial plexus and subclavian artery. Emergent vascular evaluation with arteriography and possible vascular repair are indicated. This repair can be combined with open reduction and internal fixation of the clavicle to improve stability. Delay in treatment of these vascular injuries can be devastating. Iannotti JP, Williams GR (eds): Disorders of the Shoulder. Philadelphia, PA, Lippincott, 1999, pp 632-635.
Question 12
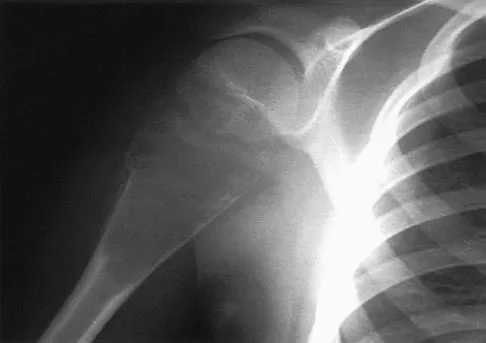
A 72-year-old woman who fell on her right shoulder while using a treadmill is now unable to elevate her right arm. An MRI scan is shown in Figure 7. What is the most likely diagnosis?
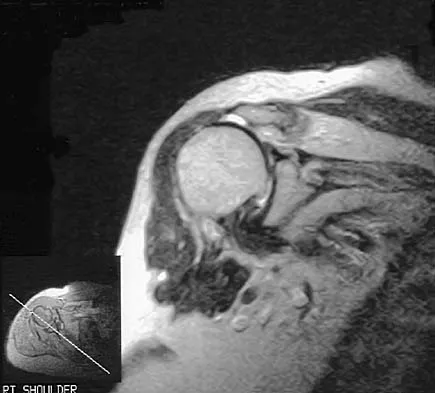
Explanation
The MRI scan reveals a large chronic rotator cuff tear with retraction and fatty infiltration atrophy of the supraspinatus and infraspinatus tendons. This tear is responsible for the patient's severe weakness and inability to elevate the arm.
Question 13
Figure 45 shows the current radiograph of an 11-year-old girl who sustained a simple nondisplaced fracture of the distal radius 4 weeks ago. Management at the time of injury consisted of application of a short arm cast but no manipulation. What is the major concern at this time?
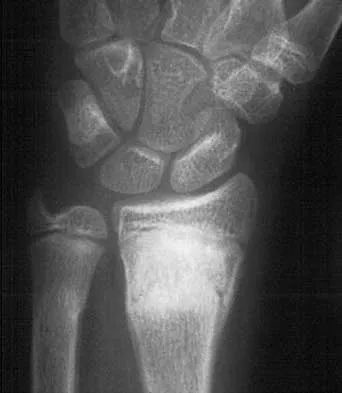
Explanation
The fracture pattern represents a Peterson type I physeal injury, which is a comminuted metaphyseal fracture in which the fracture lines extend up to the physis. Because there is no displacement of the physis and the fracture lines do not cross the physis, there may be a tendency to dismiss this injury as a simple metaphyseal fracture with no significant sequelae. A small percentage of patients (3% in Peterson's series) experience growth arrest. In this patient, a disabling ulnar plus deformity, defined as increased ulnar length in relationship to the distal radius, developed. Peterson HA: Physeal fractures: Part 2. Two previously unclassified types. J Pediatr Orthop 1994;14:431-438.
Question 14
A 45-year-old man who underwent an ankle arthrodesis reports that for the first 6 years he had significant pain relief after the fusion healed. However, he now has increasing pain in the sinus tarsi. AP and lateral radiographs are shown in Figures 8a and 8b. What is the most likely cause of the patient's symptoms?
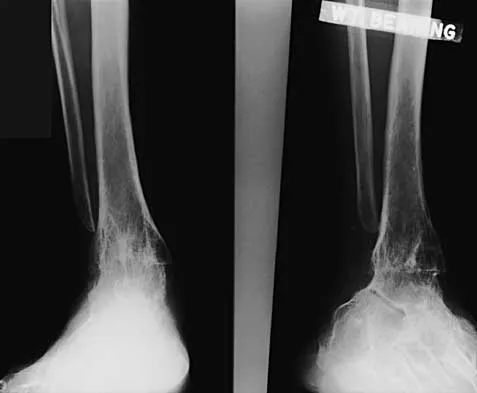
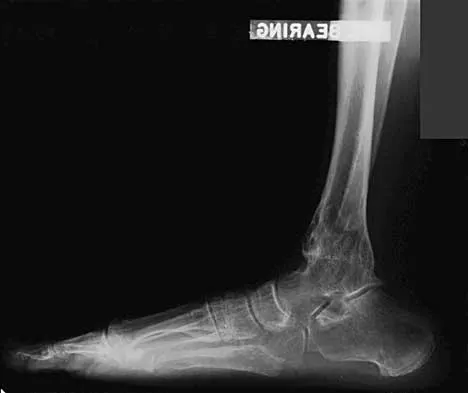
Explanation
The patient has a solid ankle fusion radiographically. With a tibiotalar arthrodesis, the adjacent joints (subtalar and transverse tarsal) take additional stress. Over time, progressive degenerative arthritis will occur in these adjacent joints, often necessitating further surgery. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 613-631.
Question 15
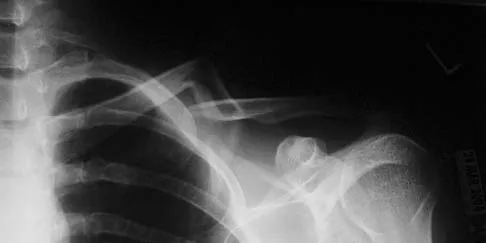
A 26-year-old man was thrown from a car and sustained the injury seen in Figures 44a and 44b. Nonsurgical management of this injury is recommended. Which of the following factors increases the risk of nonunion?
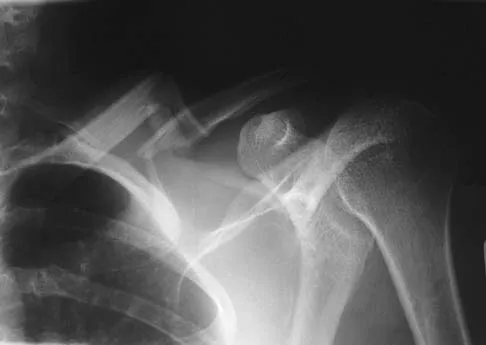
Explanation
The patient has a displaced comminuted clavicle middle one third fracture from a high-energy mechanism. Recent literature on high-energy clavicular fractures suggests a higher rate of nonunion than previously reported. A nonunion rate of 30% has been reported by Hill and associates when the fracture fragments are displaced more than 1.5 cm. In addition, several patients had neurologic symptoms related to the injury. Robinson and associates reported an increased risk of nonunion in women, elderly patients, comminuted fractures, and injuries with a lack of cortical contact. Hill JM, McGuire MH, Crosby LA: Closed treatment of displaced middle-third fractures of the clavicle gives poor results. J Bone Joint Surg Br 1997;79:537-539. Wick M, Muller EJ, Kollig E: Midshaft fractures of the clavicle with a shortening of more than 2 cm predispose to nonunion. Arch Orthop Trauma Surg 2001;121:207-211.
Question 16
Which of the following nerves is most likely responsible for symptoms associated with plantar fasciitis?
Explanation
The first branch of the lateral calcaneal nerve innervates the abductor digiti minimi. It is reported to be trapped at the interval between the abductor hallucis and the quadratus plantae muscles.
Question 17
A 47-year-old man sustained a degloving injury over the pretibial surface and anterior ankle region in a motor vehicle accident. After debridement and irrigation, there is inadequate tissue for closure of the exposed anterior tibial tendon and tibia. Prior to definitive soft-tissue coverage, management should consist of
Explanation
With soft-tissue loss, local or free flap coverage may be necessary to treat exposed tendon and bone. However, a vacuum-assisted closure device is a good temporizing dressing. It prevents external contamination, reduces edema around the wound, increases oxygen tension in the wound, and promotes the formation of granulation tissue. The use of this negative pressure device has been described in both acute traumatic and in chronic wound scenarios. If sufficient granulation tissue forms, closure may be by split graft, avoiding a more complex coverage procedure. Immediate skin grafting over the exposed anterior tibial tendon and tibia would have a low likelihood of success. Dressing changes with sulfasalazine may be beneficial in a burn wound to assist with removal of skin slough; however, in a granulating wound, the material may be toxic to early epithelialization. Xenograft is a foreign body and should not be applied to an acute contaminated open wound. Historically, a cross-leg flap was a treatment alternative for lower extremity soft-tissue loss; however, its current applications are extremely limited. Webb LX: New techniques in wound management: Vacuum assisted wound closure. J Am Acad Orthop Surg 2002;10:303-311.
Question 18
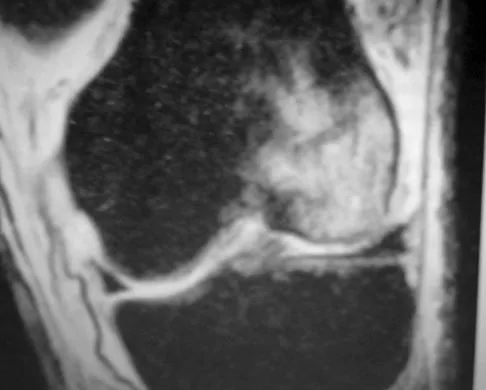
A 28-year-old man has left knee pain after a snow skiing accident. The MRI scan shown in Figure 47 reveals which of the following?
Explanation
Bone bruises are often noted on MRI after anterior cruciate and medial collateral ligament injuries. The significance of these injuries awaits long-term follow-up studies. The areas of increased signal on T2-weighted images represent areas of acute hemorrhage and are secondary to microfractures of the adjacent medullary trabeculae. Wright RW, Phaneuf MA, Limbird TJ, et al: Clinical outcome of isolated subcortical trabecular fractures (bone bruise) detected on magnetic resonance imaging in knees. Am J Sports Med 2000;28:663-667.
Question 19
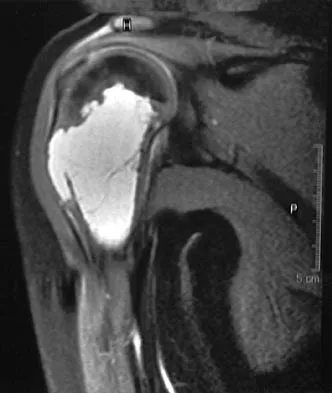
An 11-year-old boy has right shoulder pain and has been unwilling to use the arm after throwing a baseball in a Little League game 3 weeks ago. Examination reveals upper arm and shoulder tenderness with swelling. A radiograph and MRI scan are shown in Figures 27a and 27b. Management should consist of
Explanation
The radiograph is consistent with a unicameral (simple) bone cyst. The MRI scan reveals that the cyst is juxtaposed to the physis and therefore can be classified as active (latent cysts are more than 1 cm away from the physis). Active cysts are treated with aspiration and steroid injection, although repeated injections may be necessary. Curettage and bone grafting results in more reliable healing but may lead to growth arrest in active cysts. Iannotti JP, Williams GR: Disorders of the Shoulder: Diagnosis and Management, ed 1. Philadelphia, PA, Lippincott Williams & Wilkins, 1999, pp 945-946.
Question 20
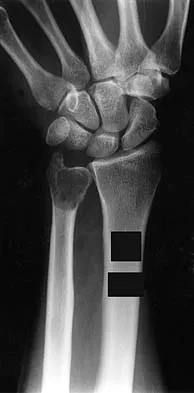
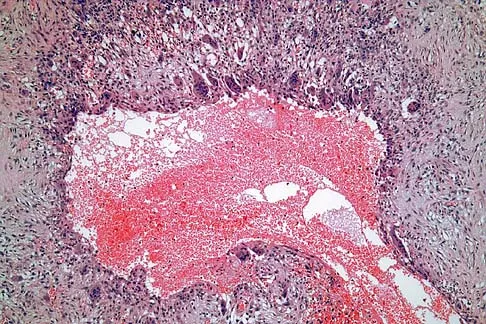
A 30-year-old patient has wrist pain. A radiograph and biopsy specimen are shown in Figures 34a and 34b. What is the most likely diagnosis?
Explanation
Aneurysmal bone cysts typically present as radiolucent lesions with an expansile remodeled cortex. The histologic appearance consists of blood-filled lakes surrounded by a benign lining that contains fibroblasts, giant cells, and hemosiderin. Although the other lesions are in the radiographic differential diagnosis, these histologic findings indicate an aneurysmal bone cyst. Bieselker JL, Marcove RC, Huvos AG, Mike V: Aneurysmal bone cyst: A Clinico-pathologic study of 66 cases. Cancer 1973;26:615.
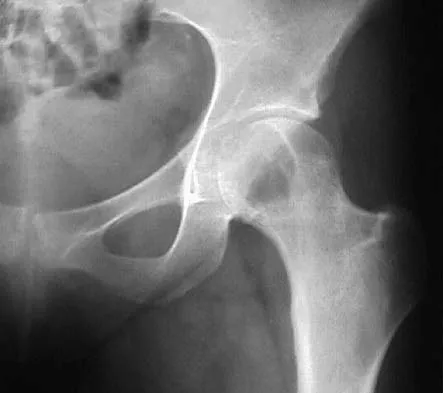
Question 21
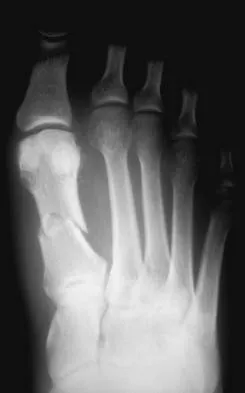
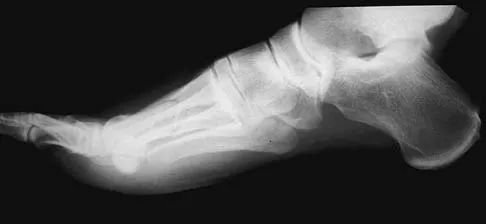
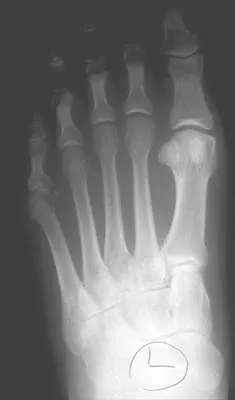
Figures 17a and 17b show the radiographs of a 32-year-old professional athlete who sustained an injury to the first metatarsal. A view of the opposite noninjured side is shown in Figure 17c. Management of the fracture should consist of
Explanation
Parameters for first metatarsal fracture management are different than for shaft fractures of the central second, third, and fourth metatarsals. The first metatarsal carries a greater load and if malunited, can create transfer lesions by virtue of uneven weight distribution; therefore, nonsurgical management is not indicated for this patient. Percutaneous pinning is not as likely to result in an anatomic reduction as open reduction and internal fixation. As his livelihood depends on an expeditious return to function, the choice of open reduction and internal fixation allows for earlier motion and rehabilitation. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 64-65.
Question 22
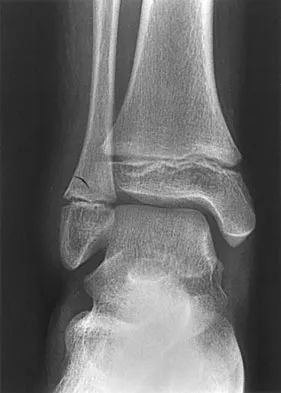
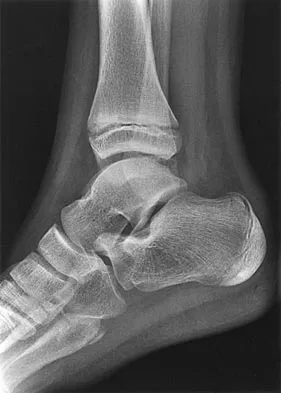
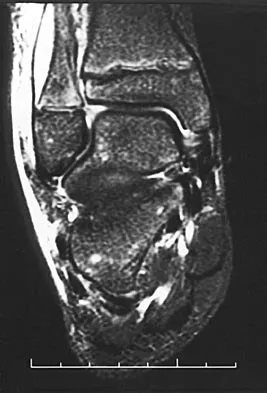
An 11-year-old boy has had a fever and pain and swelling over the lateral aspect of his right ankle for the past 3 days. Examination reveals warmth, swelling, and tenderness over the lateral malleolus, and he has a temperature of 103.2 degrees F (39.5 degrees C). Laboratory studies show a WBC count of 13,200/mm3 with 61% neutrophils, an erythocyte sedimentation rate of 112 mm/h, and a C-reactive protein of 15.7. Radiographs and a T2-weighted MRI scan are shown in Figures 13a through 13c. Aspiration yields 1 mL of purulent fluid. Management should now consist of
Explanation
The initial signs and symptoms of acute hematogenous osteomyelitis vary widely but usually include fever, bone pain, and impaired use of the involved extremity. In lower extremity infections, the child may limp or refuse to walk. Examination often reveals bone tenderness. In more advanced cases, erythema, warmth, and swelling may be present. The WBC and neutrophil counts are not always elevated, but the erythocyte sedimentation rate will be abnormal in more than 90% of patients. When the infection is diagnosed early, before a subperiosteal abscess has formed, antibiotics alone may be adequate to treat the infection. This patient has a more advanced infection, however, with the MRI scan revealing a subperiosteal abscess that was confirmed by aspiration. When an abscess is present, surgical drainage is generally indicated to remove devitalized tissue and to enhance the efficacy of the antibiotics. Further studies, such as bone or indium scans, are not necessary and will delay definitive treatment. Scott RJ, Christofersen MR, Robertson WW Jr, et al: Acute osteomyelitis in children: A review of 116 cases. J Pediatr Orthop 1990;10:649-652.
Question 23
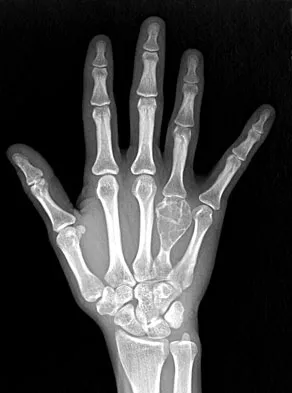
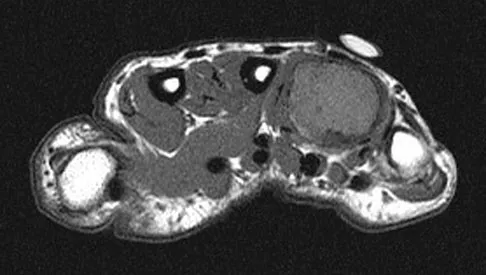
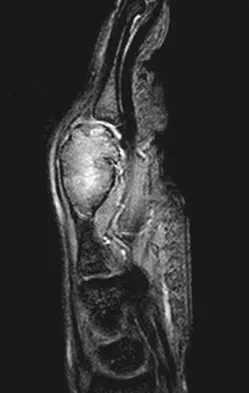
A 26-year-old man has had hand pain and progressive swelling in the knuckle for the past several months. He denies any trauma to the hand. The ring finger metacarpophalangeal joint is tender, and there is loss of motion in the digit. Figure 32a shows the radiograph and Figures 32b through 32d show the T1-weighted, T2-weighted, and gadolinium MRI scans, respectively. What is the most likely diagnosis?
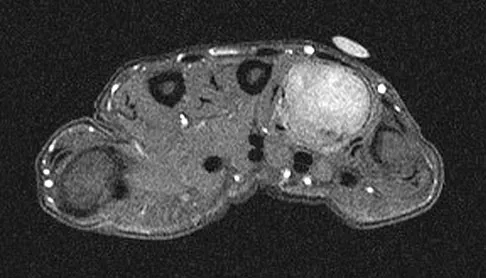
Explanation
The radiograph reveals a subchondral lesion in the metacarpophalangeal joint that is lytic and expansile. The MRI scans show a mass that is moderate in intensity on the T2-weighted image and has some gadolinium uptake. There are no cystic components in this lesion. The subchondral location and expansile nature are highly suggestive of giant cell tumor of bone. A lesion with this appearance might also represent an aneurysmal bone cyst, given the amount of expansion present. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 113-118.
Question 24
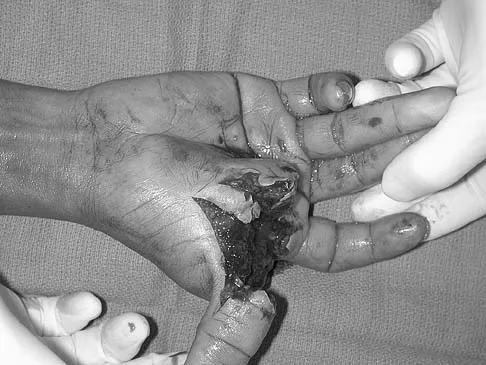
A 30-year-old farmer undergoes replantation of an above-the-elbow amputation. What form of management is most important following this surgery?
Explanation
After major limb replantation, the occurrence of ischemic rhabdomyonecrosis can result in lactic acidosis and myoglobulinemia. These complications can be limited by rapid repair of the arterial supply, potentially using a shunt before skeletal stability. Repair of the venous system should be performed after repair of the artery. High volume fluid replacement will maintain a diuresis, thus limiting the complications from myoglobulinemia. Wood MB: Replantations about the elbow, in Morrey BF (ed): The Elbow and Its Disorders. Philadelphia, PA, WB Saunders, 1985, pp 472-480.
Question 25
What malignant disease most commonly develops in conjunction with chronic osteomyelitis?
Explanation
The most common malignant disease to arise in conjunction with chronic osteomyelitis is squamous cell carcinoma particularly in patients with a long-standing draining sinus tract. Dell PC: Hand, in Simon MA, Springfield D (eds): Surgery for Bone and Soft Tissue Tumors. Philadelphia, PA, Lippincott-Raven, 1998, pp 405-420.
Question 26
A 67-year-old woman undergoes a revision total shoulder arthroplasty for replacement of a loose glenoid component. Examination in the recovery room reveals absent voluntary deltoid and triceps contraction, weakness of wrist and thumb extension, and absent sensation in the palmar aspect of all fingertips and the radial forearm. The next most appropriate step in management should consist of
Explanation
Neurologic injury after shoulder replacement is relatively uncommon, occurring in 4% of shoulders in one large series. The importance of identifying and protecting the musculocutaneous and axillary nerves cannot be overemphasized; it is especially critical during revision arthroplasty when the normal anatomic relationships have been distorted. The long deltopectoral approach leaving the deltoid attached to the clavicle was found to be significant in the development of postoperative neurologic complications. A correlation was found between surgical time and postoperative neurologic complications, with long surgical times being associated with more neurologic complications. The presumed mechanism of injury is traction on the plexus that occurs during the surgery. A neurologic injury after total shoulder arthroplasty usually does not interfere with the long-term outcome of the arthroplasty itself; it is best managed by protective measures with passive range of motion of the involved extremity. Wirth MA, Rockwood CA Jr: Complications of shoulder arthroplasty. Clin Orthop 1994;307:47-69.
Question 27
A 12-year-old boy with an ankle fracture undergoes closed reduction under sedation in the emergency department. Figure 27 shows a lateral radiograph of the ankle after two attempts at closed reduction. Based on these findings, treatment should now consist of
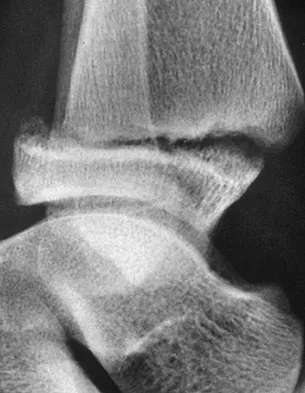
Explanation
The widening of the physis associated with incomplete reduction of this fracture suggests that periosteum is interposed at the fracture site. Clinical and animal study findings suggest that the interposed periosteum may lead to premature physeal closure. Repeated forceful attempts at reduction may subject the physis to further injury and should be avoided. Growth problems are common in children with Salter-Harris type I fractures of the lower extremities. Nonunions are rare in children with Salter-Harris type I fractures. Barmada A, Gaynor T, Mubarak SJ: Premature physeal closure following distal tibial physeal fractures: A new radiographic predictor. J Pediatr Orthop 2003;23:733-739.
Question 28
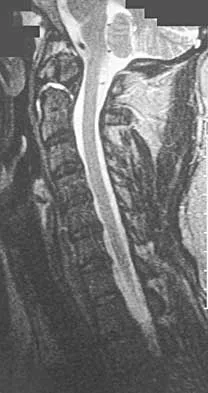
A 42-year-old woman reports that she has low back pain and had a transient loss of consciousness after falling off a horse. She denies having neck pain but notes that she was involved in a motor vehicle accident 2 years ago and had neck pain at that time. Examination reveals full range of motion of the neck and no localized tenderness. The neurologic examination is normal. A lateral radiograph of the cervical spine is obtained. Figures 41a and 41b show CT and MRI scans. What is the most likely diagnosis?
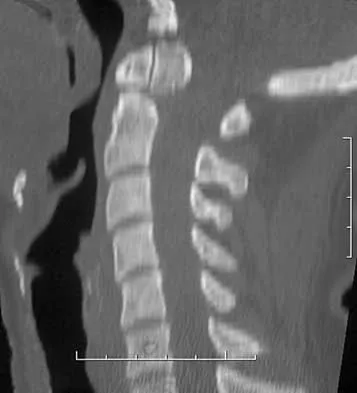
Explanation
The examination findings do not correlate with an acute injury (full range of cervical motion and the absence of pain). Radiographically, the fracture appears old based on the smooth contour of the fracture fragments and the absence of soft-tissue swelling. Flexion-extension radiographs can be obtained to determine potential instability; if present, stabilization and fusion should be considered. Schatzker J, Rorabeck CH, Waddell JP: Non-union of the odontoid process: An experimental investigation. Clin Orthop 1975;108:127-137.
Question 29
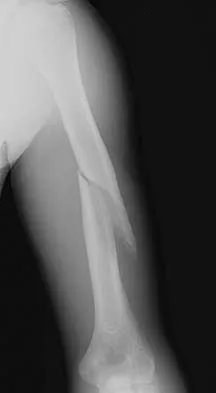
An otherwise healthy 13-year-old boy sustains the fracture shown in Figure 40 while throwing a fastball. Management should consist of
Explanation
Nonsurgical management such as a functional brace, hanging arm cast, or sugar tong splint is the treatment of choice for a fracture of the humeral shaft that is the result of throwing. The fracture surface typically is wide and the degree of displacement is not large; therefore, surgery is not indicated in most patients. Ogawa K, Yoshida A: Throwing fracture of the humeral shaft: An analysis of 90 patients. Am J Sports Med 1998;26:242-246.
Question 30
For halo traction, what is the preferred site for anterior pin placement?
Explanation
The safe zone for anterior halo pin insertion is marked laterally by the anterior border of the temporalis muscle (to avoid penetration of this muscle and relative thin cortex of the skull). Medially, the pin should be placed 4.5 cm lateral to the midline to avoid injury to the supraorbital nerve or the frontal sinus. The safe area is marked superiorly by the head equator to avoid cephalad migration of the pin and inferiorly by the supraorbital ridge to prevent displacement or penetration into the orbit.
Question 31
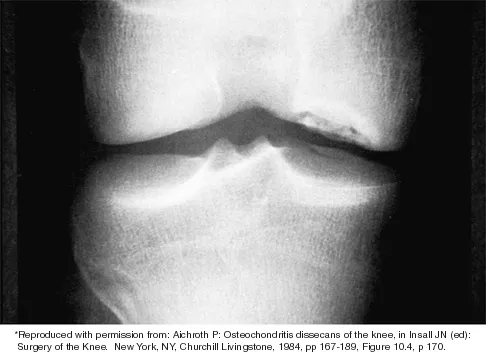
Which of the following primary prognostic factors best predicts the outcome of the knee lesion shown in Figure 22?
Explanation
The patient has osteochondritis dissecans. While location, size, and knee stability are all relevant to the overall prognosis, studies have shown that younger patients with open growth plates have a better prognosis of healing when compared with patients who have closed growth plates. The degree of pain is also relevant to treatment, but it is subjective rather than objective and is not as reliable of a prognostic indicator as age. Stanitski CL: Osteochondritis dissecans of the knee, in Stanitski CL, DeLee JC, Drez D Jr (eds): Pediatric and Adolescent Sports Medicine. Philadelphia, PA, WB Saunders, 1994, vol 3, pp 387-405. Cahill B: Treatment of juvenile osteochondritis dissecans and osteochondritis dissecans of the knee. Clin Sports Med 1985;4:367-384.
Question 32
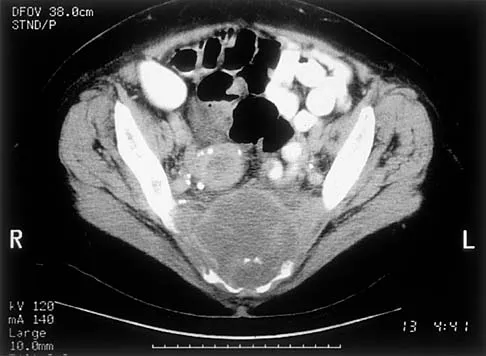
An otherwise healthy 78-year-old woman has low back and buttock pain. Rectal examination reveals a large sacral mass. Figures 7a and 7b show a CT scan and a sagittal MRI scan of the lumbosacral spine. A biopsy specimen is shown in Figure 7c. What is the most likely diagnosis?
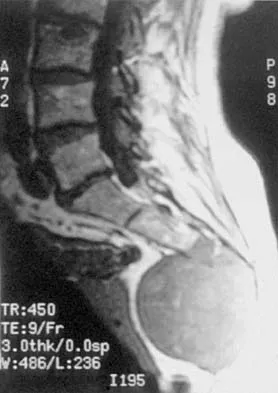
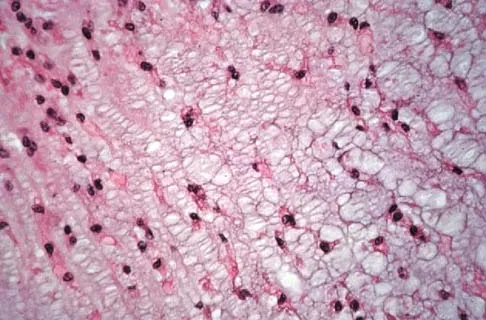
Explanation
A chordoma is a malignant neoplasm originating from remnants of the notochord. It is usually localized to the midline with 50% at the sacrococcygeal area, 35% at the skull base, and 15% at the mobile portion of the spine. Large vacuolated cells (physaliferous cells) are a characteristic of the tumor. Mindell ER: Chordoma. J Bone Joint Surg Am 1981;63:501-505.
Question 33
Osteoclasts originate from which of the following cell types?
Explanation
Osteoclasts originate from the monocyte/macrophage lineage. Fibroblasts and osteoprogenitor cells originate from mesenchymal stem cells and do not form osteoclasts. Plasma cells reside in the bone marrow and are derivatives of the hematopoietic system. Megakaryocytes are also in the bone marrow and synthesize platelets. Zaidi M, Blair HC, Moonga BS, et al: Osteoclastogenesis, bone resorption, and osteoclast-based therapeutics. J Bone Miner Res 2003;18:599-609. Brinker MR: Bone (Section 1), in Miller M (ed): Review of Orthopaedics, ed 2. Philadelphia, PA, WB Saunders, 1996, pp 1-35.
Question 34
A 52-year-old woman has bicompartmental osteoarthritis following patellectomy. Treatment should consist of
Explanation
The patient has extensive degenerative changes in both the medial and lateral compartments within the knee; therefore, arthroscopic debridement or an osteotomy will not be helpful. A patellar arthroplasty will not address the medial and lateral compartments. Because the extensor mechanism provides a significant amount of anteroposterior stability, a posterior cruciate-substituting total knee arthroplasty is the treatment of choice for this patient. Martin SD, Haas SB, Insall JN: Primary total knee arthroplasty after patellectomy. J Bone Joint Surg Am 1995;77:1323-1330.
Question 35
An 18-year-old man sustained closed humeral shaft and forearm fractures of his dominant arm in a motor vehicle accident. Neurovascular examination is intact, and his condition is stable. The best course of action for management of the injuries should be
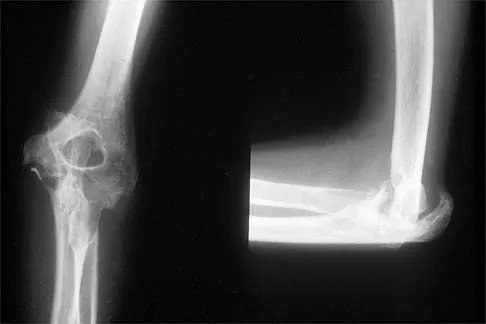
Explanation
Fractures above and below the elbow constitute floating elbow injuries and are best treated with internal fixation to allow early range of motion and to prevent elbow stiffness. Use of a long arm cast would promote elbow stiffness. External fixation is indicated primarily for open injuries. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 271-286.
Question 36
What is the most accurate description of the relationship between gender and knee loading during landing while playing basketball?
Explanation
Ford and associates studied 81 high school basketball players and found that females landed with greater total valgus knee loading and a greater maximum valgus knee angle than male athletes. Hewett and associates reported in a study of 205 female athletes that those with increased dynamic valgus and high abduction loads were at increased risk of anterior cruciate ligament injury. Hewett TE, Myer GD, Ford KR, et al: Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: A prospective study. Am J Sports Med 2005;33:492-501.
Question 37
What is the most common reason for reoperation in total knee arthroplasty?
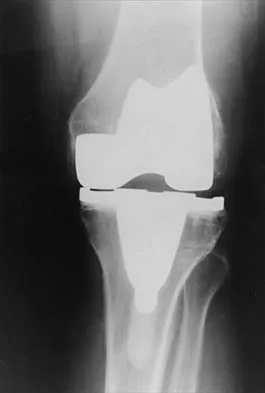
Explanation
Patellar problems currently constitute the largest number of complications after total knee arthroplasty, affecting between 8% and 35% of patients. These problems include patellar instability, fracture, component loosening, surface erosion, and pain. Malalignment, as an isolated reason for revision, is uncommon, yet it contributes to accelerated wear of the components. Joint instability affects up to 6% of patients, and the infection rate in knee arthroplasty is around 1% to 2%. Blasier RB, Matthews LS: Complications of prosthetic knee arthroplasty, in Epps CH (ed): Complications in Orthopaedic Surgery. Philadelphia, PA, JP Lippincott, 1994, pp 1066-1069. Rand JA: The patellofemoral joint in total knee arthroplasty. J Bone Joint Surg Am 1994;76:612-620.
Question 38
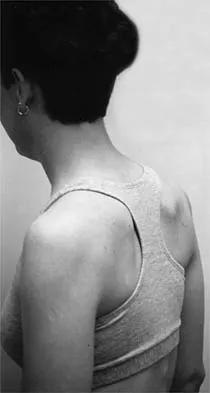
A 22-year-old woman has had progressive upper extremity weakness for the past several years. History reveals no pain in her neck or shoulders. Examination reveals scapular winging of both shoulders and weakness in external rotation. She can abduct to only 120 degrees bilaterally, and there is mild supraspinatus weakness. She is otherwise neurologically intact with normal sensation and reflexes; however, she has difficulty whistling. A clinical photograph is shown in Figure 14. What is the most likely diagnosis?
Explanation
Progressive weakness is a common sign with a large differential diagnosis. Nerve, muscle, and joint problems should be excluded when a patient has diffuse weakness and atrophy. Fascioscapulohumeral dystrophy is a rare disease characterized by facial muscle weakness and proximal shoulder muscle weakness. The weakness is usually bilateral, and scapular winging is common. If the scapular winging becomes pronounced, elevation of the shoulder can be affected. In severe cases, scapulothoracic fusion or pectoralis muscle transfer to the scapula may be indicated. Duchenne muscular dystrophy is typically severe and progressive. The other diagnoses are not compatible with the history or the physical findings. Shapiro F, Specht L: The diagnosis and orthopaedic treatment of inherited muscular diseases of childhood. J Bone Joint Surg Am 1993;75:439-454.
Question 39
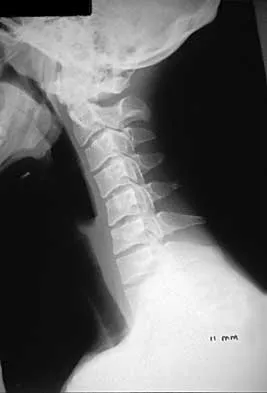
Subluxation caused by rheumatoid arthritis is most commonly seen at what level of the cervical spine?
Explanation
Approximately 65% of cervical subluxations occur at C1-C2. Of these, 50% are anterior, with the remainder being lateral and posterior. The second most common type is basilar invagination, occurring in 40% of patients. The third most common type is subaxial, occurring in 20% of patients with rheumatoid arthritis. Subluxation at more than one level is common. Boden S, Clark CR: Rheumatoid arthritis of the cervical spine, in Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Raven, 1998, p 693. Boden SD, Dodge LD, Bohlman HH, Rechtine GR: Rheumatoid arthritis of the cervical spine: A long-term analysis with predictors of paralysis and recovery. J Bone Joint Surg Am 1993;75:1282-1297.
Question 40
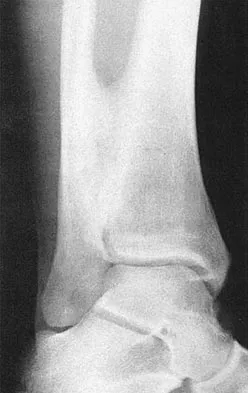
A 28-year-old professional football player reports painless loss of ankle motion after sustaining a "severe" ankle sprain 12 months ago. A mortise radiograph is shown in Figure 1. Surgical treatment should be reserved for which of the following conditions?
Explanation
The radiograph shows posttraumatic tibiofibular synostosis. This condition typically follows an eversion (high) ankle sprain that results in disruption of the interosseous membrane. Ossification usually develops within 6 to 12 months after the injury. Return to sports is possible despite the lack of normal ankle dorsiflexion and mobility between the tibia and fibula. Surgical excision is reserved for persistent pain that fails to respond to nonsurgical management once the ossification is "cold" on bone scintigraphy. Whiteside LA, Reynolds FC, Ellsasser JC: Tibiofibular synostosis and recurrent ankle sprains in high performance athletes. Am J Sports Med 1978;6:204-208. Henry JH, Andersen AJ, Cothren CC: Tibiofibular synostosis in professional basketball players. Am J Sports Med 1993;21:619-622.
Question 41
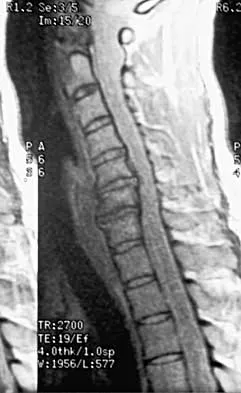
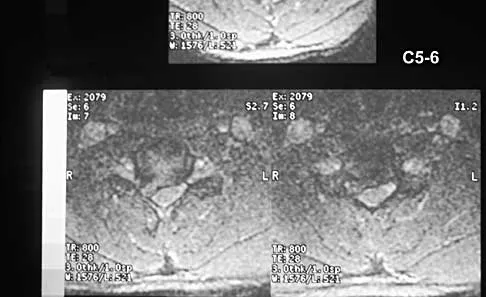
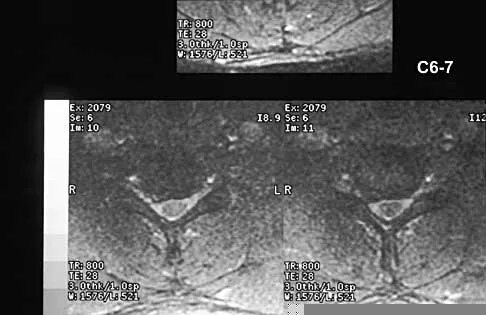
A 40-year-old carpenter has a 3-month history of right arm pain and neck pain that now leaves him unable to work. Examination reveals a positive Spurling test, weakness of the biceps, and a mildly positive Hoffman's sign on the right side. Electromyography and nerve conduction velocity studies show a right C6 deficit. Figures 27a through 27c show MRI scans that reveal two-level spondylotic disease at C5-6 and C6-7, a large herniated nucleus pulposus at C5-6, and a prominent ridge and hard disk at C6-7. Nonsurgical management fails to provide relief, so the patient elects surgical intervention. Which of the following surgical options would give the best long-term results?
Explanation
The patient has a single-level deficit by clinical examination but an adjacent level that may be pathologic. Hilibrand and associates, in a review of 374 patients with myeloradiculopathy treated with single-level or multilevel anterior cervical diskectomy and fusion, showed that 25% of patients had an occurrence of new radiculopathy or myelopathy at an adjacent level within 10 years after surgery. Reoperation rates were highest in those patients where the adjacent nonfused segment was C5-6 or C6-7. Those patients who had multilevel fusions had a lower incidence of adjacent segment disease. The authors recommended incorporating an adjacent level in the initial procedure in patients with myelopathy or radiculopathy when significant disease was noted. Posterior keyhole foraminotomy is an excellent procedure for single-level radiculopathy but is not effective in relieving myelopathy. Anterior cervical diskectomy without fusion has an increased incidence of hypermobility and neck pain on long-term follow-up. In a later review, these authors reported improved fusion rates and better clinical outcomes with the use of strut fusions instead of multilevel interbody grafts. Hilibrand AS, Carlson GD, Palumbo MA, Jones PK, Bohlman HH: Radiculopathy and myelopathy at segments adjacent to the site of a previous anterior cervical arthrodesis. J Bone Joint Surg Am 1999;81:519-528. Henderson CM, Hennessy RG, Shuey HM Jr, Shackelford EG: Posterior-lateral foraminotomy as an exclusive operative technique for cervical radiculopathy: A review of 846 consecutively operated cases. Neurosurgery 1983;13:504-512.
Question 42
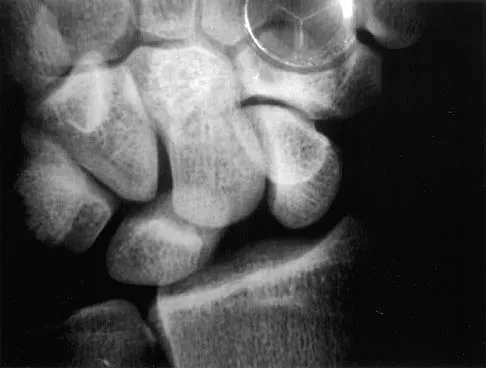
Based on the radiographic findings shown in Figure 41, which of the following wrist ligaments is most likely disrupted?
Explanation
The radiograph shows a diastasis of the scapholunate interval, caused by certain failure of the scapholunate interosseous ligament. The lunotriquetral interosseous ligament stabilizes the lunotriquetral joint. The long radiolunate ligament originates in the volar radius and inserts in the lunate. The short radiolunate ligament originates on the ulnar margin of the radius and inserts on the ulnar margin of the lunate. The ulnolunate ligament originates at the ulnar styloid base and inserts on the volar aspect of the lunate. Linscheid RL, Dobyns JH, Beabout JW, et al: Traumatic instability of the wrist: Diagnosis, classification, and pathomechanics. J Bone Joint Surg Am 1972;54:1612-1632. Mayfield JK, Johnson RP, Kilcoyne RK: Carpal dislocations: Pathomechanics and progressive perilunar instability. J Hand Surg Am 1980;5:226-241.
Question 43
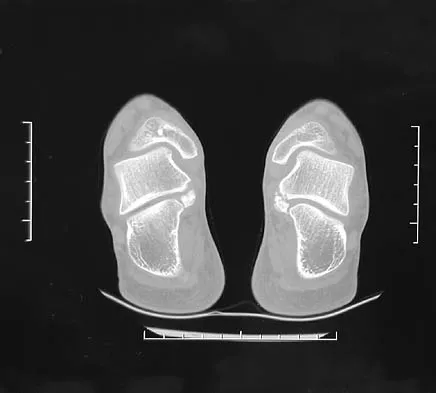
Figure 8 shows the CT scan of an 11-year-old boy who has had a 1-year history of worsening painful flatfeet. He reports pain associated with physical education at school, especially with running and jumping. Management consisting of activity restriction, anti-inflammatory drugs, and casting has failed to provide relief. Treatment should now consist of
Explanation
In most patients with symptomatic talocalcaneal coalition involving less than 50% of the subtalar joint, resection with fat graft interposition is preferred over a subtalar or triple arthrodesis, especially if reasonable range of motion can be achieved. This patient has a synchondrosis that is partially cartilaginous. Although patients may have a residual gait abnormality, most report pain relief after surgery. Scranton PE Jr: Treatment of symptomatic talocalcaneal coalition. J Bone Joint Surg Am 1987;69:533-539. Kitaoka HB, Wikenheiser MA, Schaughnessy WJ, et al: Gait abnormalities following resection of talocalcaneal coalition. J Bone Joint Surg Am 1997;79:369-374.
Question 44
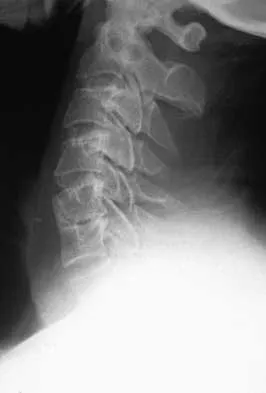
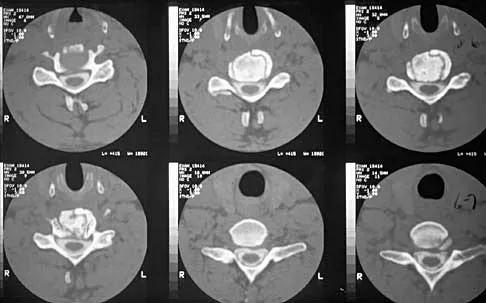
A patient underwent an anterior cervical diskectomy and interbody fusion for a C5-6 herniated nucleus pulposus and left C6 radiculopathy 8 months ago. He now reports new onset of severe neck pain and left C6 radicular pain, with wrist extension weakness. The radiograph and CT scan shown in Figures 26a and 26b reveal pseudarthrosis at C5-6. The next step in management should consist of
Explanation
Brodsky and associates reviewed 34 cases of cervical pseudarthrosis after anterior fusion. Seventeen were treated with revision anterior fusion and 17 with posterior foraminotomy and fusion. Good results were seen in 75% of patients who underwent revision anterior surgery, but better results (94%) were seen with posterior surgery, including foraminotomy and stabilization. Tribus and associates reported treatment of 16 patients with pseudarthrosis using revision anterior debridement of the fibrous tissue and fusion with autograft and plates. There was improvement of the neck in 75% of the patients, nonunion in 19%, continued weakness in 28%, and dysphagia in 5%. Farey and associates reported on 19 patients treated with posterior foraminotomy, stabilization, and fusion with a fusion rate of 100%, resolution of arm pain in 94%, resolution of weakness in 100%, and resolution of neck pain in 75%. It would appear that posterior foraminotomy is more effective for relieving arm pain and neurologic deficits associated with pseudarthrosis. Posterior fusion has the most reliable rate of arthrodesis in this setting. Dysphagia is reported in some patients undergoing more extensive anterior dissections required for applying plates. A neck brace is unlikely to aid in healing of pseudarthrosis in a patient who underwent surgery 8 months ago. A neck brace would be most effective within the first 3 months if a delayed union is identified. Brodsky AE, Khalil MA, Sassard WR, Neuman BP: Repair of symptomatic pseudarthrosis of anterior cervical fusion: Posterior versus anterior repair. Spine 1992;17:1137-1143. Tribus CB, Corteen DP, Zdeblick TA: The efficacy of anterior cervical plating in the management of symptomatic pseudarthrosis of the cervical spine. Spine 1999;24:860-864.
Question 45
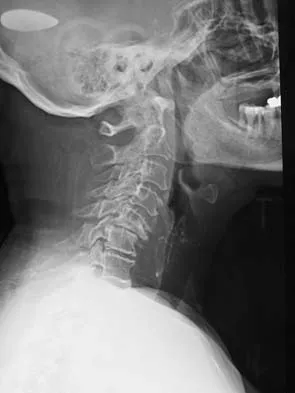
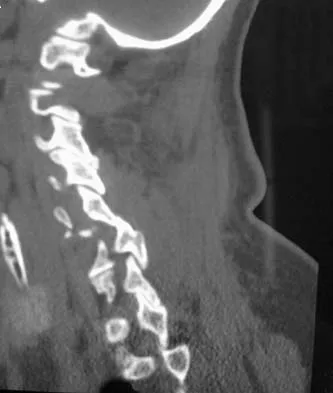
A 65-year-old woman has significant neck pain after falling and striking her head. A radiograph and sagittal CT scan are shown in Figures 23a and 23b. What is the most likely diagnosis?
Explanation
The radiograph shows a displacement of C5 on C6 of approximately 25%. The CT scan shows a perched facet at C5-6. There is no evidence of a facet fracture. A bilateral facet dislocation would show a displacement of more than 50%. Rothman RH, Simeone FA (eds): The Spine, ed 4. Philadelphia PA, WB Saunders, 1999, pp 927-937.
Question 46
Which of the following complications may occur subsequent to resurfacing hip arthroplasty for osteonecrosis of the hip but not after total hip arthroplasty?
Explanation
Advocates of resurfacing hip arthroplasty cite preservation of the proximal femoral bone stock as the main advantage of this procedure over total hip arthroplasty. Fracture of the retained femoral neck has been reported following resurfacing arthroplasty. The exact etiology of the latter is unknown. Technical errors, such as notching of the femoral neck or possibly disruption of the blood supply to the femoral head during extensive soft-tissue exposure, may result in femoral neck fracture. Gabriel JL, Trousdale RT: Stem fracture after hemiresurfacing for femoral head osteonecrosis. J Arthroplasty 2003;18:96-99.
Question 47
The tibiofibular overlap used to diagnose syndesmotic diastasis on an AP view is most commonly measured between the
Explanation
The tibiofibular overlap is measured between the medial border of the fibula and the lateral border of the anterior tibial tubercle. Plain radiographic assessment of the distal tibiofibular syndesmosis requires AP and mortise views. The following criteria have been used as the normal limits in adults: a talocrural angle of + or - 83 degrees with up to 5 degrees of normal difference between both sides, a medial clear space of less than 4 mm, a talar tilt of less than 2 mm, a tibiofibular clear space of less than 5 mm, a tibiofibular overlap of greater than or equal to 0 mm, and a talar subluxation that is a subjective assessment of congruity of the tibial articular surface and the talar dome; any incongruity is abnormal. It has been recommended to obtain the first three measurements on the mortise view and the other three on the AP view. Wuest TK: Injuries to the distal lower extremity syndesmosis. J Am Acad Orthop Surg 1997;5:172-181.
Question 48
The brachialis muscle is innervated by what two nerves?
Explanation
The brachialis is innervated by two nerves: medially, the musculocutaneous nerve; laterally, the radial nerve. The muscle is split longitudinally to approach the humerus anteriorly. Henry AK: The distal part of the humerus and front of the forearm, in Henry AK (ed): Extensile Exposure, ed 2. Edinburgh, UK, Churchill Livingstone, 1973, pp 90-115.
Question 49
A female cross-country runner has an insidious onset of right groin pain. Radiographs of the right hip reveal a tension-side stress fracture. History reveals that she was treated for a "foot" fracture 1 year ago. In addition to performing internal fixation of the femoral neck, which of the following should be obtained?
Explanation
Stress fractures in female long distance runners are frequently associated with the Female Athletic Triad. The triad consists of osteoporosis, amenorrhea, and altered eating habits. A thorough menstrual history, including age of menarche, history of amenorrhea, and use of oral contraceptives, is imperative. Amenorrhea leads to osteoporosis and predisposes the athlete to fractures. An MRI of the hip is not necessary because a fracture is evident on the radiograph. Serum calcium levels are normal in osteoporosis, a family history would be noncontributory, and it is highly unlikely that a contralateral hip radiograph will yield useful information. Bennell KL, Malcolm SA, Thomas SA, et al: Risk factors for stress fractures in track and field athletes: A twelve-month prospective study. Am J Sports Med 1996;24:810-818.
Question 50
A 13-year-old girl who is 2 years postmenarche has been referred for management of scoliosis. She denies any history of back pain. Radiographs show a right thoracic curve of 35 degrees. She has a Risser sign of 4 and a bone age of 15.5 years. Management should consist of
Explanation
Because the patient is skeletally mature with a curve of less than 40 degrees, there is no benefit to bracing and surgery is not indicated. Management should consist of observation and follow-up radiographs in 6 months. Lonstein JE, Carlson JM: The prediction of curve progression in untreated idiopathic scoliosis during growth. J Bone Joint Surg Am 1984;66:1061-1071.
Question 51
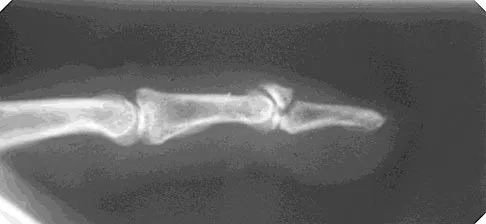
Figure 20 shows the radiograph of a 21-year-old college basketball player who jammed his left index finger on the rim. He reports pain and tenderness over the dorsum of the distal interphalangeal (DIP) joint. Examination reveals that he is unable to actively extend the DIP joint; however, the skin is intact. Management should consist of
Explanation
Mallet fingers without DIP joint subluxation can be treated with extension splinting. Surgical fixation may be necessary in bony mallet injuries when the joint is subluxated. Size of the bony fragment, while often correlating with stability, is not always an indication for fixation. Buddy taping allows motion; therefore, the fragment will not heal in the appropriate position. Intermittent splinting with range-of-motion exercises also will not allow the fragment to heal in the appropriate position. Crawford GP: The molded polyethylene splint for mallet finger deformities. J Hand Surg Am 1984;9:231-237.
Question 52
A 28-year-old painter has had increasing pain in his hand and forearm after sustaining a paint injection wound to the tip of his left index finger 24 hours ago. Management should consist of
Explanation
The clinical presentation soon after injury may be surprisingly innocuous, but all high-pressure injection injuries of various materials are best treated by emergent surgical debridement of all foreign material from the flexor tendon sheath as well as the subcutaneous tissues. Subsequent hospital admission, IV antibiotics, and possible repeat debridements usually are necessary. The use of antibiotics alone is inadequate treatment of this severe injury. Pinto MR, Turkula-Pinto LE, Cooney WP, Wood MB, Dobyns JH: High-pressure injection injuries of the hand: Review of 25 patients managed by open wound technique. J Hand Surg Am 1993;18:125-130. Urbaniak JR, Evans JP, Bright DS: Microvascular management of ring avulsion injuries. J Hand Surg Am 1981;6:25-30. Tsai TM, Manstein C, DuBou R, Wolff T, Kutz JE, Kleinert HE: Primary microsurgical repair of ring avulsion amputation injuries. J Hand Surg Am 1984;9:68-72. Kay S, Werntz J, Wolff T: Ring avulsion injuries: Classification and prognosis. J Hand Surg Am 1989;14:204-213.
Question 53
What is the most common complication of halo vest immobilization in adults?
Explanation
Although pin loosening generally has not been considered a major problem, it has been cited as the most common complication in two published series of halo vest complications. The other possible complications are all significantly less common. Baum JA, Hanley EN Jr, Pullekines J: Comparison of halo complications in adults and children. Spine 1989;14:251-252. Garfin SR, Botte MJ, Waters RL, Nickel VL: Complications in the use of the halo fixation device. J Bone Joint Surg Am 1986;68:320-325.
Question 54
During the application of halo skeletal fixation, the most appropriate position for the placement of the anterior halo pins is approximately 1 cm above the superior orbital rim and
Explanation
Halo fixation is the most rigid form of cervical orthosis, but complications can arise from improper placement of the initial halo ring. A relatively safe zone for anterior pin placement is located 1 cm above the orbital rim and superior to the lateral two thirds of the orbit. This position avoids the supraorbital and supratrochlear nerves and arteries over the medial one third of the orbit. The more lateral positions in the temporal fossa have very thin bone and can interfere with the muscles of mastication. Posterior pin site locations are less critical; positioning on the posterolateral aspect of the skull, diagonal to the contralateral anterior pins, is generally desirable. Botte MJ, Byrne TP, Abrams RA, et al: Halo skeletal fixation: Techniques of application and prevention of complications. J Am Acad Orthop Surg 1996;4:44-53.
Question 55
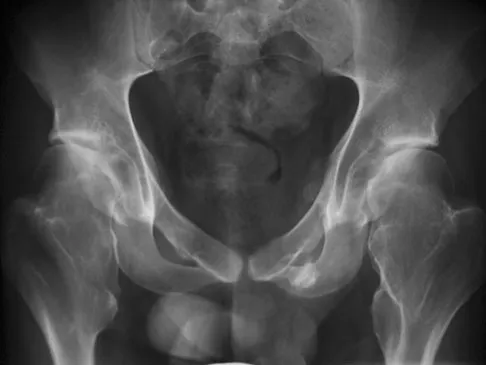
A 22-year-old man has mild hip pain bilaterally and multiple skeletal lesions. Based on the pelvic radiograph shown in Figure 30, what is the inheritance pattern for his disorder?
Explanation
Multiple hereditary exostoses (MHE) is an autosomal dominant disorder manifested by multiple osteochondromas and characteristic skeletal involvement. EXT1 on 8q24.1 and EXT2 on 11p13 are the two genes most strongly associated with MHE. Mutations in these genes affect proper development of endochondral bone, such that in all affected individuals exostoses develop adjacent to the growth plates of long bones, and some exhibit additional bone deformities. Defects in the EXT genes result in increased chondrocyte proliferation and delayed hypertrophic differentiation. Stieber JR, Dormans JP: Manifestations of hereditary multiple exostoses. J Am Acad Orthop Surg 2005;13:110-120.
Question 56
A 19-year-old female long-distance runner has an incomplete tension-side femoral neck stress fracture. Management should consist of
Explanation
Unlike compression-side stress fractures, tension-side stress fractures on the superior side of the femoral neck are at a very high risk of displacement, even if the patient is not bearing weight. It is highly recommended to treat these fractures like acute fractures and to proceed with internal fixation emergently. Once the fracture has displaced, the prognosis is poor in terms of returning to sports, even when reduced and internally fixed. Nonsurgical management, such as limited weight bearing and low-impact activities, works very well for other lower extremity stress fractures. A training program evaluation (shoes, tracks, schedule) is always indicated for all patients with stress fractures.
Question 57
A 3-year-old boy with severe cerebral palsy is unable to sit independently and does not crawl. Examination reveals a 40-degree hip flexion contracture by the Thomas test and 25 degrees of passive abduction. A radiograph of the pelvis shows subluxation of both hips, with a migration index of 30%. Management should consist of
Explanation
Progressive hip subluxation occurs in up to 50% of children with spastic quadriparesis. The subluxation is the result of chronic muscle hypertonicity, especially in the adductor muscle group. In time, the constant muscle tension will lead to dislocation, dysplastic changes in the acetabulum, and erosive changes in the cartilage of the femoral head. Many of these children will experience pain. Two recent studies have shown that early soft-tissue releases can successfully prevent progressive subluxation in children who are younger than age 4 years and who have a Reimers index (migration index) of less than 40%. Botulinum toxin A injections may reduce tone in the adductors for 4 to 6 months, but it is difficult to inject into the iliopsoas. Additionally, there are no long-term studies documenting the efficacy of botulinum toxin A to treat progressive hip subluxation in patients who have spastic quadriparesis. In general, proximal femoral osteotomy, combined with soft-tissue release as necessary, is indicated in older children (older than age 4 years) with progressive subluxation. Although selective dorsal rhizotomy has been used in nonambulatory patients, outcomes are less well documented than in ambulatory patients. There are no studies documenting the effect of selective dorsal rhizotomy on progressive hip subluxation in nonambulatory children. Miller F, Cardoso Dias R, Dabney KW, et al: Soft-tissue release for spastic hip subluxation in cerebral palsy. J Pediatr Orthop 1997;17:571-584.
Question 58
A previously asymptomatic 12-year-old girl sustained a direct blow to the right lateral knee from a baseball bat. Examination reveals an area of ecchymosis and tenderness over the lateral thigh. The patient can walk without pain, but range of motion of the knee causes discomfort. Plain radiographs of the knee are shown in Figures 11a and 11b. To address the bone lesion, management should consist of
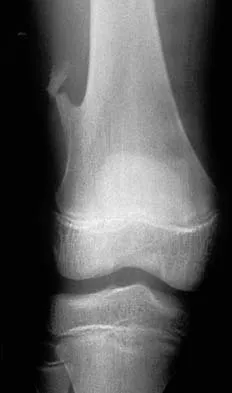
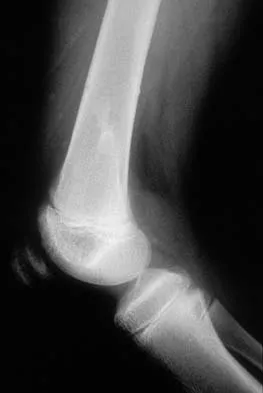
Explanation
The plain radiographs reveal a pedunculated osteochondroma with a fracture. There is a bony growth in the metaphysis of a long bone, on a stalk that is directed away from the nearby epiphysis. On the AP view, the host cortical and medullary bone are shown as "blending" with lesional bone. There is also a fracture through the lesion. Based on these radiographic findings, the diagnosis is an osteochondroma; therefore, initial management of an acute fracture of an osteochondroma is symptomatic treatment alone. Additional imaging studies are not indicated in this patient. At times it may be difficult to distinguish a sessile osteochondroma from a parosteal osteosarcoma. In the latter case, the host medullary bone and lesion bone are not confluent. A CT scan may be helpful to distinguish if the host medullary and cortical bone are confluent with the lesion.
Question 59
During the implantation of a cementless acetabular component in total hip arthroplasty, placement of a screw in the anterior superior quadrant puts which of the following structures at risk for damage?
Explanation
A knowledge of the safe quadrants for screw placement for acetabular component implantation is essential when performing total hip arthroplasty. The external iliac vessels are on the inner wall of the pelvis, corresponding to the anterior superior quadrant of the acetabulum. Keating EM, Ritter MA, Faris PM: Structures at risk from medially placed acetabular screws. J Bone Joint Surg Am 1990;72:509-511.
Question 60
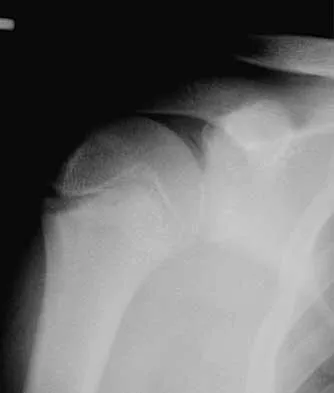
A 72-year-old woman who is right hand-dominant has severe pain in the right shoulder that has failed to respond to nonsurgical management. She reports night pain and significant disability. Examination reveals 30 degrees of active forward elevation. An AP radiograph is shown in Figure 27. Which of the following treatment options will provide the best functional improvement?
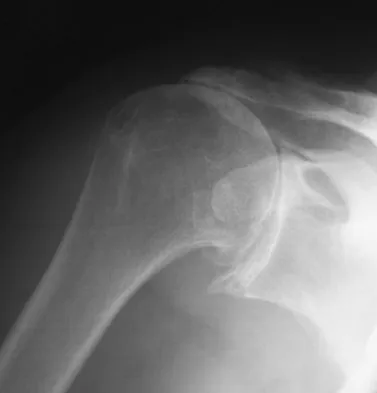
Explanation
The patient has end-stage rotator cuff tear arthropathy. The radiograph shows complete proximal humeral migration (acromiohumeral interval of 0 mm), severe glenohumeral arthritis, and acetabularization of the acromion. In addition, she has "pseudoparalysis" with active elevation of only 30 degrees. Reverse shoulder arthroplasty affords her the best opportunity for pain relief and functional improvement. The other procedures have mixed results but typically are better for pain relief than they are for functional gains. Frankle M, Siegal S, Pupello D, et al: The reverse shoulder prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency: A minimum two-year follow-up study of sixty patients. J Bone Joint Surg Am 2005;87:1697-1705.
Question 61
Figure 6 shows the radiograph of a 14-year-old baseball player who felt a pop and had an immediate onset of pain in his elbow after a hard throw from the outfield. The best course of action should be to
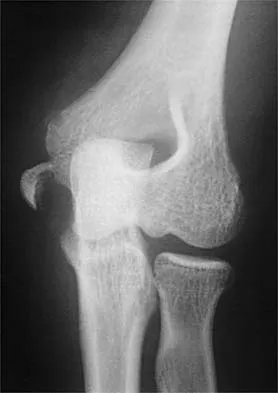
Explanation
The valgus stress at the elbow caused by throwing strains the medial collateral ligament. The medial epicondyle, on which the ligament inserts, is the last ossification center to fuse to the distal humerus, and acute avulsion of the medial epicondyle can occur in adolescents. If the elbow is allowed to heal in a displaced position, valgus instability and loss of elbow extension may result. Valgus instability is especially problematic for the throwing athlete. Surgical treatment with rigid internal fixation is the treatment of choice for displaced medial epicondyle avulsion fractures. Valgus instability is prevented, and the rigid fixation allows for early range of motion. Case SL, Hennrikus WL: Surgical treatment of displaced medial epicondyle fractures in adolescent athletes. Am J Sports Med 1997;25:682-686.
Question 62
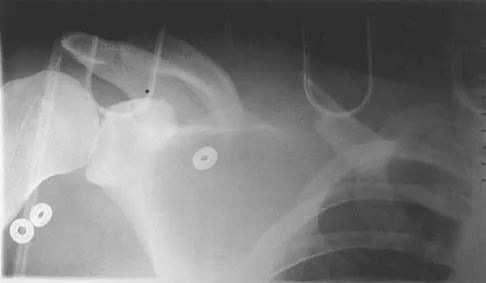
A 72-year-old man injured his right shoulder after tripping over a chair leg. Radiographs obtained in the emergency department reveal an isolated anterior dislocation. After successful closed reduction, the patient has recurrent anterior instability and is unable to elevate the arm. What is the most likely cause of the recurrent instability?
Explanation
A rotator cuff tear is the most common cause of recurrent instability following a first-time dislocation in patients older than age 40 years. Dislocations occur through a posterior mechanism rather than by an isolated labral avulsion or a Bankart lesion as seen in younger patients. Nevaiser RJ, Nevaiser TJ: Recurrent instability of the shoulder after age 40. J Shoulder Elbow Surg 1995;4:416-418.
Question 63
A 17-year-old high school gymnast who has peripatellar knee pain has been unable to practice on a consistent basis for the past 3 years. She denies any specific injury events. Physical therapy for modalities, quadriceps strengthening, and hamstring stretching provide temporary relief. A trial of patellar taping significantly reduces her pain. Examination reveals an 15-degree Q angle, moderate lateral facet tenderness, negative patellar apprehension, and the inability to evert the patella. Radiographs show a moderate lateral patellar tilt. Treatment should now consist of
Explanation
The patient has patellofemoral stress and a tight lateral retinaculum that has failed to respond to nonsurgical management; therefore, the most appropriate treatment includes an arthroscopic lateral retinacular release. A patellar restraining brace may aggravate the peripatellar pain by increasing pressure on the lateral facet. There is no evidence of patellar instability or significant malalignment; therefore, medial retinacular repair or a tibial tubercle transfer is not indicated. A modified Maquet tibial tubercle elevation would be considered only for significant patellofemoral arthrosis. Gambardella RA: Techical pitfalls of patellofemoral surgery. Clin Sports Med 1999;18:897-903.
Question 64
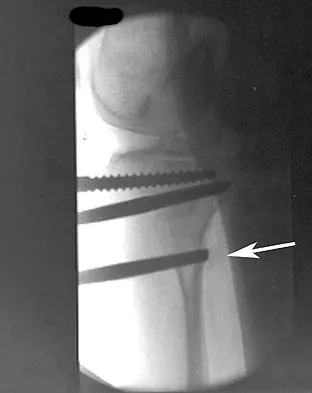
What is the typical MRI signal intensity of bone marrow affected by acute osteomyelitis?
Explanation
The classic MRI findings of osteomyelitis are a decrease in the normally high signal intensity of marrow on T1-weighted images and normal or increased signal intensity on T2-weighted images. This is the result of replacement of marrow fat by inflammatory cells and edema, which causes lower signal intensity than fat on T1-weighted images and higher signal intensity than fat on T2-weighted images. The addition of gadolinium to a T1-weighted sequence reveals increased signal intensity in the hyperemic marrow. Unger E, Moldofsky P, Gatenby R, et al: Diagnosis of osteomyelitis by MR imaging. Am J Roentgenol 1988;150:605-610. Dormans JP, Drummond DS: Pediatric hematogenous osteomyelitis: New trends in presentation, diagnosis and treatment. J Am Acad Orthop Surg 1994;2:333-341.
Question 65
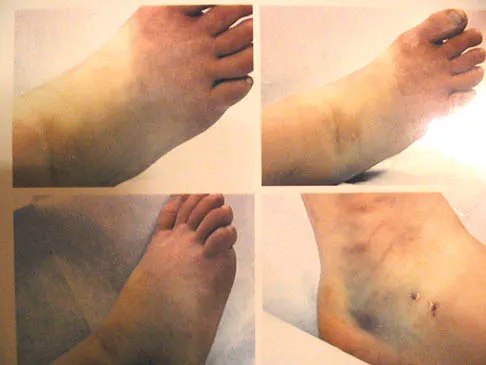
Which of the following is considered the most common infectious organism causing osteochondritis in pediatric puncture wounds of the foot?
Explanation
Pseudomonas aeruginosa is the most common infectious organism causing osteochondritis in pediatric puncture wounds of the foot. Eikenella corrodens is found in human bites, and Pasteurella multocida is characteristically seen with animal bites. Serratia marcescens and Proteus mirabilis have been reported but are much less likely. Jacobs RF, Adelman L, Sack CM, et al: Management of pseudomonas osteochondritis complicating puncture wounds of the foot. Pediatrics 1982;69:432-435.
Question 66
Which of the following best describes athletic pubalgia?
Explanation
Athletic pubalgia refers to a distinct syndrome of lower abdominal and adductor pain that is mostly commonly seen in high performance male athletes. This condition must be distinguished from others such as painful inflammation of the symphysis pubis, referred to as osteitis pubis. Symptoms attributable to the iliopsoas tendon are most commonly associated with snapping of the tendon. Stress fracture of the pubic ramus may cause symptoms in this area, but it is usually confirmed by imaging studies. Neurapraxia of the pudendal nerve is associated with pressure from the seat in cycling sports and also as a complication associated with traction during surgical procedures. Meyers WC, Foley DP, Garrett WE, Lohnes JH, Mandlebaum BR: Management of severe lower abdominal or inguinal pain in high-performance athletes: PAIN (Performing Athletes with Abdominal or Inguinal Neuromuscular Pain Study Group). Am J Sports Med 2000;28:2-8.
Question 67
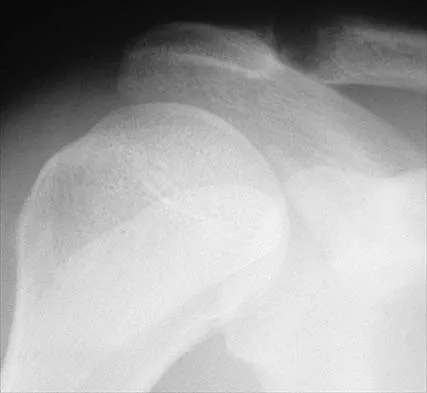
The modified Brostrom lateral ankle ligamentous reconstruction uses which of the following structures to provide supplementary stabilization?
Explanation
The modified Brostrom lateral ankle ligament stabilization procedure uses the remnants of the anterior talofibular and the calcaneofibular ligaments, supplemented by the inferior retinaculum and the transferred talocalcaneal ligament to stabilize the lateral ankle. Chrisman and associates described the use of one half of the peroneus brevis. Watson-Jones and Evans used the entire peroneus brevis. The peroneus longus has been taken by mistake. The plantaris has been used in triligamentous reconstruction. Gould N, Seligson D, Gassman J: Early and late repair of lateral ligament of the ankle. Foot Ankle 1980;1:84-89. Hamilton WG, Thompson FM, Snow SW: The modified Brostrom procedure for lateral ankle instability. Foot Ankle 1993;14:1-7. Chrisman OD, Snook GA: Reconstruction of lateral ligament tears of the ankle: An experimental study and clinical evaluation of seven patients treated by a new modification of the Elmslie procedure. J Bone Joint Surg Am 1969;51:904-912. Evans DL: Recurrent instability of the ankle: My method of surgical treatment. Proc R Soc Med 1953;46:343. Watson-Jones R: Fractures and Joint Injuries, ed 3. Baltimore, MD, Williams and Wilkins, 1946, p 234.
Question 68
Figures 21a and 21b show the radiographs of a 22-year-old man who has had progressive pain and swelling about the knee for the past 6 weeks. Examination reveals limited range of motion and fullness about the knee. What is the most likely diagnosis?
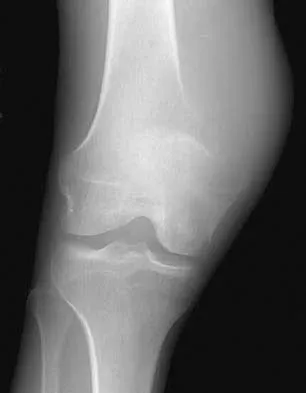
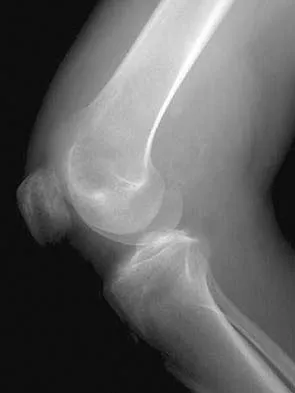
Explanation
The radiographs reveal a destructive lesion in the metaphysis of the distal femur with periosteal changes and an associated soft-tissue mass with subtle mineralization. This suggests an aggressive malignant process. In this age group, the most likely diagnosis is osteosarcoma. Giant cell tumor, which usually is in a more subchondral location, is not typically so aggressive. Aneurysmal bone cyst is usually more geographic, with a well-marginated reactive rim. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 175-186.
Question 69
A 75-year-old woman undergoes hybrid total hip arthroplasty for osteoarthritis. A postoperative radiograph obtained in the recovery room is shown in Figure 18. Treatment should now consist of
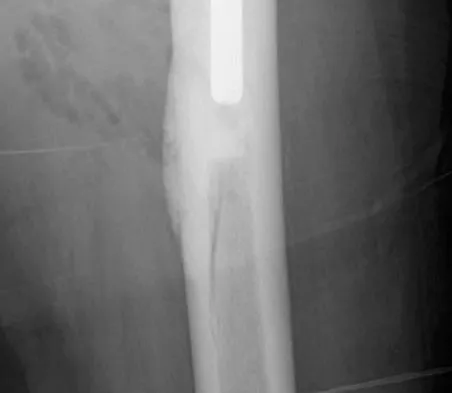
Explanation
Intraoperative femoral fractures can often be avoided by careful preoperative planning to optimize implant design and size. Most fractures occur during implantation of a cementless implant; many can be avoided by careful femoral preparation and component implantation, with particular caution in osteopenic bone. Intraoperative femoral fractures are managed according to fracture severity. Minor cracks that do not affect stability or femoral integrity can often be managed intraoperatively with cerclage fixation, limited weight bearing, and observation. Femoral fractures that compromise implant stability or femoral integrity require fracture fixation with cerclage wires, strut grafts, or plates and may require conversion to a long stem implant. This patient's fracture is nondisplaced and the implant is well seated; therefore, limited weight bearing is considered appropriate management. Lee SR, Bostrom MP: Periprosthetic fractures of the femur after total hip arthroplasty. Instr Course Lect 2004;53:111-118. Kelley SS: Periprosthetic femoral fractures. J Am Acad Orthop Surg 1994;2:164-172.
Question 70
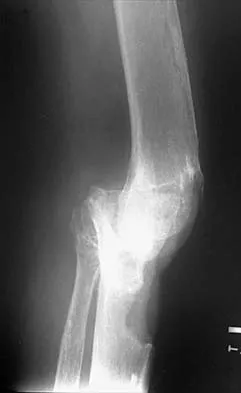
Figures 35a and 35b show the radiographs of a patient who underwent debridement of a chronically infected, fully constrained knee prosthesis and now reports pain and instability despite bracing. History reveals that the patient has had no drainage since undergoing the last debridement 6 months ago. A C-reactive protein level and aspiration are negative for infection. Treatment should now consist of
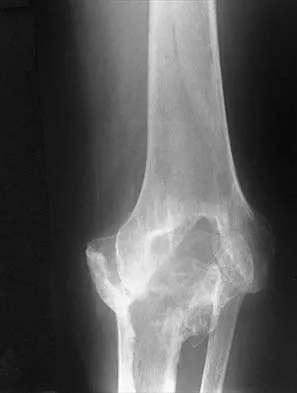
Explanation
The radiographs show a significant loss of the proximal anterior tibial cortex, consistent with an extensively damaged or deficient extensor mechanism. Such a deficit precludes insertion of another knee arthroplasty. Arthrodesis is the treatment of choice for this patient and is indicated for loss of the extensor mechanism and knee instability. A recent report on arthrodesis following removal of an infected prosthesis showed a union rate of 91% using a short intramedullary nail. Insertion of an antibiotic-impregnated PMMA spacer is not indicated because the rationale for using a spacer is to maintain a space for reinsertion of another prosthesis. Reconstruction of the extensor mechanism would not address the loss of the joint. Amputation is the final treatment option if the arthrodesis fails. Rand JA: Alternatives to reimplantation for salvage of the total knee arthroplasty complicated by infection. J Bone Joint Surg Am 1993;75:282-289. Lai KA, Shen WJ, Yang CY: Arthrodesis with a short Huckstep nail as a salvage procedure for failed total knee arthroplasty. J Bone Joint Surg Am 1998;80:380-388.
Question 71
A patient with rheumatoid arthritis has a rupture of the extensor digitorum communis to 4 and 5. You are planning to perform an extensor indicis proprius (EIP) tendon transfer. What effect will this have on index finger extension?
Explanation
EIP transfer results in no functional deficit. If the tendon is cut proximal to the sagittal band, there will be no extensor deficit. Browne EX, Teague MA, Snyder CC: Prevention of extensor lag after indicis proprius transfer. J Hand Surg Am 1979;4:168-172.
Question 72
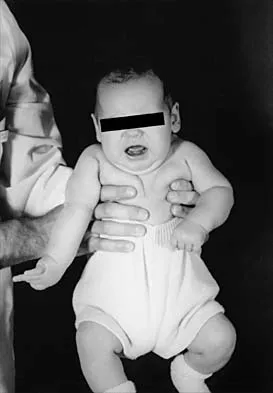
Figure 37 shows the clinical photograph of a 1-day-old infant who weighed 10.25 lb at birth. Examination reveals an absent right Moro reflex and limited active motion of the right shoulder, elbow, and wrist, but flexion of the fingers. Passive range of motion of the shoulder and elbow is normal. What is the most likely diagnosis?
Explanation
The patient's right upper extremity is held in the "head waiter's" posture with the shoulder internally rotated, the elbow extended, and the wrist in flexion. The Erb type of obstetrical brachial plexus palsy involves the C5 and C6 nerve root, and occasionally, as in this child, the C7 nerve root. Obstetrical palsy is a traction injury, and is associated with a high birth weight, shoulder dystocia, cephalopelvic disproportion, or the use of forceps. Erb palsy is four times more common than injury to the entire plexus or injury to the C8 and T1 nerve roots. It results from the shoulder being depressed while the head and neck are laterally rotated, extended, and tilted in the opposite direction. Most patients recover wrist extension and elbow flexion. Patients with residual weakness of shoulder external rotation and abduction will benefit from release of the pectoralis major, latissimus dorsi, and teres major, with transfer of the latissimus dorsi and the teres major to the posterosuperior aspect of the rotator cuff. Recent studies using arthrograms and CT scans have shown a higher incidence of posterior glenoid deficiency and posterior subluxation than that observed with plain radiographs. The posterior subluxation or dislocation can be effectively reduced by tendon release and transfer procedures. Hoffer MM, Phipps GJ: Closed reduction and tendon transfer for treatment of dislocation of the glenohumeral joint secondary to brachial plexus birth palsy. J Bone Joint Surg Am 1998;80:997-1001. Pearl ML, Edgerton BW: Glenoid deformity secondary to brachial plexus birth palsy. J Bone Joint Surg Am 1998;80:659-667.
Question 73
At the L4-5 level, what is the location of the S2-5 nerve roots in relationship to the L5 and S1 nerve roots?
Explanation
The nerve roots of S2-5 are positioned dorsally and in the midline relative to the L5 and S1 nerve roots. The L5 nerve root is located lateral to S1 as it prepares to exit under the L5 pedicle. The S1 nerve root is located lateral and ventral to the S2-5 nerve roots. Garfin SR, Vaccaro AR (eds): Orthopaedic Knowledge Update: Spine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 3-17.
Question 74
A 30-year-old patient has acetabular dysplasia and moderate secondary osteoarthrosis. Which of the following studies will best help predict the success of periacetabular osteotomy?
Explanation
Improvement in the appearance of the hip joint on functional radiographic evaluation (abduction/adduction views) has been shown to be predictive of outcome following joint preserving surgery. CT and MRI findings have not been shown to be predictive of outcome.
Question 75
What changes in muscle physiology would be expected in an athlete who begins a rigorous aerobic program for an upcoming marathon?
Explanation
Muscle fibers can be categorized grossly into two types. Type I muscle, also known as slow-twitch muscle, is responsible for aerobic, oxidative muscle metabolism. It has a much lower strength and speed of contraction than fast-twitch type II muscle but is significantly more fatigue resistant. With training for endurance sports, the type I muscle undergoes adaptive changes to the increased stress. Increases in capillary density, oxidative capacity, mitochondrial density, and subsequent fatigue resistance are all observed changes. Hypertrophy of type IIb muscle is seen in strength training. Simon SR (ed): Orthopaedic Basic Science. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1994, pp 89-125.
Question 76
Spontaneous recovery of upper extremtiy motor function after a cerebrovascular accident occurs in which of the following predictable patterns?
Explanation
Recovery of upper extremity motor function after a cerebrovascular accident follows a predictable pattern. The greatest amount of recovery is seen within the first 6 weeks. Return of function proceeds from proximal to distal. Shoulder flexion occurs first, followed by return of flexion to the elbow, wrist, and fingers. Return of forearm supination follows the return of finger flexion.
Question 77
Hamstring lengthening and posterior transfer of the rectus femoris will be most successful in a patient with cerebral palsy who has which of the following gait abnormalities?
Explanation
Children with cerebral palsy typically ambulate with a crouched gait characterized by excessive flexion of the hips and knees during stance. Many patients exhibit co-contracture of the quadriceps and hamstrings, causing a stiff-knee gait. Normally, the rectus femoris fires at the initiation of swing and in terminal swing through initial contact. Prolonged activity of the rectus femoris throughout the swing phase interferes with normal knee flexion. This contributes to a stiff knee during swing phase and prevents clearance of the foot. Lengthening of the hamstrings alone will not improve foot clearance. Hamstring lengthening is contraindicated when there is hyperextension during stance. Transfer of the rectus femoris to one of the knee flexors has been shown to improve knee flexion during swing by an average of 15 degrees. This allows improved foot clearance. Gage JR, Perry J, Hicks RR, Koop S, Werntz JR: Rectus femoris transfer to improve knee function of children with cerebral palsy. Dev Med Child Neurol 1987;29:159-166.
Question 78
What percent of the adult human meniscus is vascularized?
Explanation
The adult menisci are considered to be relatively avascular structures, with the peripheral blood supply originating predominately from the lateral and medial genicular arteries. Branches of these vessels form the perimeniscal capillary plexus, which supplies the peripheral border throughout its attachment to the joint capsule. Vascular penetration studies have shown that 10% to 30% of the peripheral portion of the medial meniscus and 10% to 25% of the lateral meniscus are vascularized. Arnoczky SP, Warren RF: Microvasculature of the human meniscus. Am J Sports Med 1982;10:90-95.
Question 79
Examination of a 10-year-old girl with a hypoplastic breast and atrophic pectoralis major may also reveal which of the following findings?
Explanation
Poland's syndrome has four main features: 1) short digits as the result of absence or shortening of the middle phalanx; 2) syndactyly of the short digits usually consisting of a simple, complete type; 3) hypoplasia of the hand and forearm; and 4) absence of the sternocostal head of the pectoralis major on the same side. Wilson MR, Louis DS, Stevenson TR: Poland's syndrome: Variable expression and associated anomalies. J Hand Surg 1988;13:880-882.
References:
- Poland A: Deficiency of the pectoralis muscle. Guys Hosp Rep 1841;6:191.
Question 80
What is the heaviest weight that can be safely applied to the adult cervical spine via Gardner-Wells tong traction?
Explanation
Cotler and associates reported on the use of awake skeletal traction to reduce facet fracture-dislocations in 24 patients. Seventeen patients required more than 50 pounds of traction (the "traditional" limit) to achieve reduction. More than 100 pounds of traction was safely used in one-third of the patients in this study. A cadaver study has supported the safe use of traction with weights in excess of 100 pounds. Cotler JM, Herbison GJ, Nasuti JF, et al: Closed reduction of traumatic cervical spine dislocation using traction weights up to 140 pounds. Spine 1993;18:386-390.
Question 81
An active 49-year-old woman who sustained a diaphyseal fracture of the clavicle 8 months ago now reports persistent shoulder pain with daily activities. An AP radiograph is shown in Figure 8. Management should consist of
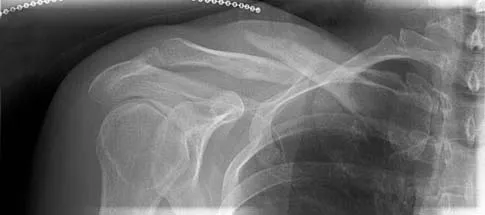
Explanation
The radiograph reveals an atrophic nonunion of the diaphysis of the clavicle. Electrical or ultrasound stimulation may be an option in diaphyseal nonunions that have shown some healing response with callus formation, but these techniques are not successful in an atrophic nonunion. The preferred technique for achieving union is open reduction and internal fixation with bone graft. Percutaneous fixation has no role in treatment of nonunions of the clavicle. Boyer MI, Axelrod TS: Atrophic nonunion of the clavicle: Treatment by compression plating, lag-screw fixation and bone graft. J Bone Joint Surg Br 1997;79:301-303.
Question 82
Figures 28a through 28c show the MRI scans of a 30-year-old woman who weighs 290 lb and has low back and left leg pain. She also reports frequent urinary dribbling, which her gynecologist has advised her may be related to obesity. Examination will most likely reveal
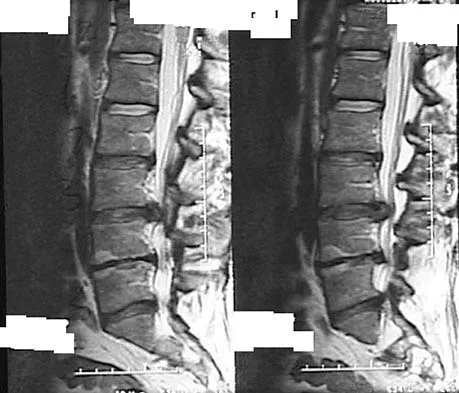
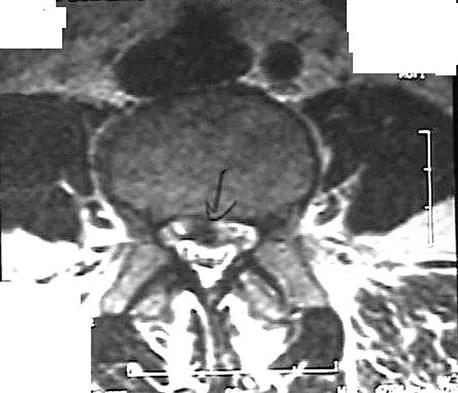
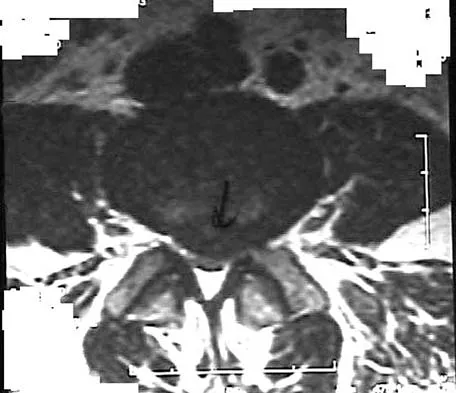
Explanation
The patient will most likely exhibit ipsilateral weakness of the tibialis anterior. Gaenslen's test is designed to detect sacroiliac inflammation as a source of low back pain. Beevor's sign tests the innervation of the rectus abdominus and paraspinal musculature (L1 innervation). The extensor hallucis longus is predominantly innervated by L5. The peroneals are predominantly innervated by S1. Hoppenfeld S: Physical Examination of the Spine and Extremities. Appleton, WI, Century-Crofts, 1976.
Question 83
A 63-year-old man with type I diabetes mellitus who underwent open forefoot amputation now has a high fever, and an elevated WBC count and blood glucose levels. Repeat laboratory studies the day after surgery show a WBC count of 9,500/mm3, a serum albumin level of 1.9 g/dL, and a total lymphocyte count of 1,900/mm3. Examination reveals that he is afebrile, and his blood glucose level is now normal. An ultrasound Doppler of the dorsalis pedis artery shows an ankle-brachial index of 0.6. A transcutaneous partial pressure measurement of oxygen at the ankle joint shows a level of 38 mm Hg. What is the best course of action?
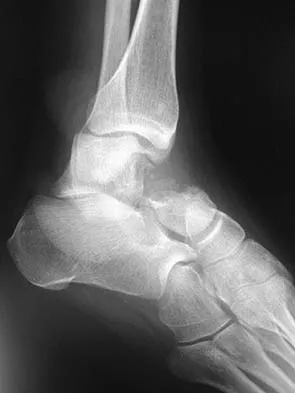
Explanation
This patient appears to have adequate blood supply to heal a Syme's ankle disarticulation but is currently malnourished because of the systemic infection, and is likely to progress to wound failure. Therefore, the initial management of choice is culture-specific antibiotic therapy, open wound management, and nutritional supplementation. If his serum albumin rises to a minimum of 2.5 gm/dL, he can undergo elective Syme's ankle disarticulation. If the serum albumin does not rise within a short period of time, he should undergo transtibial amputation.
Question 84
The correct starting point for an external fixation half pin placed into the anterior inferior iliac spine (AIIS) is labeled by what letter in Figure 3?
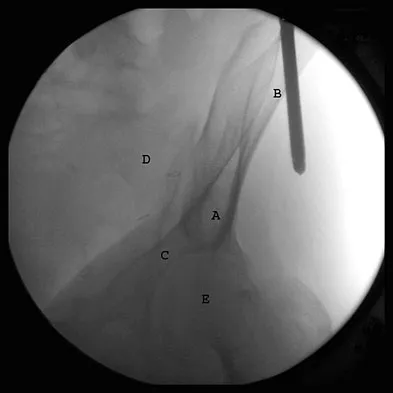
Explanation
Half pins placed in the AIIS are an alternative to pins placed in the iliac crest. A strong pillar of bone runs from the AIIS to the posterior iliac crest and less soft tissue is typically present in this area. The starting point is best seen on an obturator outlet view. The obturator outlet view is a combination of the pelvic outlet view and the obturator view of Judet and Letournel. The beam is rotated "over the top" of the patient since the iliac wing is externally rotated as well as cephalad to best visualize this column of bone running from the AIIS to the posterior iliac spine. This corridor of bone will appear as a teardrop. Once the correct view is obtained, the pin should be started at least 2 cm proximal to the hip joint to avoid placing a pin within the hip capsule. Blunt dissection and a guide sleeve should be used to prevent damage to the lateral femoral cutaneous nerve. An iliac oblique view is used after the pin has been partially inserted to make sure the pin is passing superior to the superior gluteal notch, and an obturator inlet view can be used at the completion of the procedure to make sure the pin is contained within the bone for its entire length. Gardner MJ, Nork SE: Stabilization of unstable pelvic fractures with supra-acetabular compression external fixation. J Orthop Trauma 2007;21:269-273. Haidukewych GJ, Kumar S, Prpa B: Placement of half-pins for supra-acetabular external fixation: An anatomic study. Clin Orthop Relat Res 2003;411:269-273.
Question 85
Which of the following is a true statement regarding thoracic disk herniations?
Explanation
Symptomatic herniations of the thoracic spine are much less common than those of the cervical or lumbar region. They tend to occur most commonly during the third to fifth decades of life and although they can be found at all levels, they are most common in the lower third near the thoracolumbar region. Posterior laminectomy and disk excision has the highest rate of neurologic deterioration and is not recommended. Multiple studies have shown that herniated thoracic disks can be found at one or more levels in 40% of asymptomatic individuals. Shah RP, Grauer JN: Thoracoscopic excision of thoracic herniated disc, in Vaccaro AR, Bono CM (eds): Minimally Invasive Spine Surgery. New York, NY, Informa Healthcare, 2007, pp 73-80.
Question 86
The vessel seen in the clinical photographs shown in Figures 50a and 50b (1,2 intercompartmental supraretinacular artery) is being dissected to be used as a source of vascularized bone graft for a patient who is scheduled to undergo internal fixation of a scaphoid nonunion. This vessel is a branch of what artery?
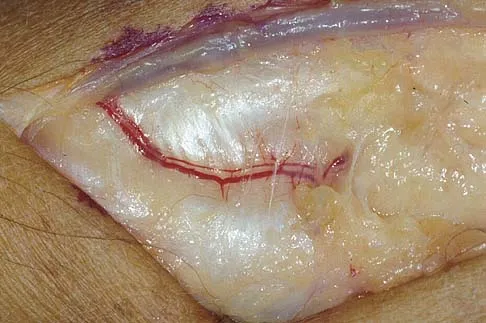
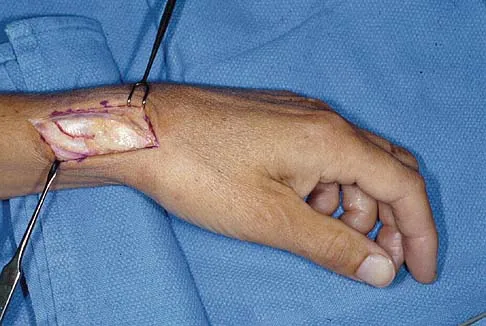
Explanation
The 1,2 intercompartmental supraretinacular artery is a branch of the radial artery. The vessel provides a reliable source of vascularized bone graft with an adequate pedicle length for use in scaphoid nonunions. Sheetz KK, Bishop AT, Berger RA: The arterial blood supply of the distal radius and ulna and its potential use in vascularized pedicled bone grafts. J Hand Surg 1995;20:902-914.
Question 87
A 15-year-old boy falls from his bicycle and sustains an injury to his elbow. Prereduction radiographs are shown in Figure 12a. Closed reduction is performed without difficulty and postreduction radiographs are shown in Figure 12b. What is the next most appropriate step in treatment?
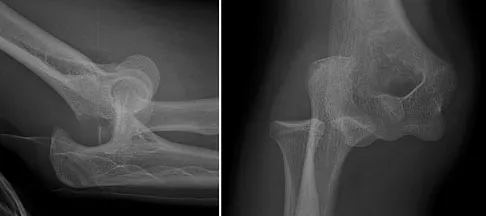
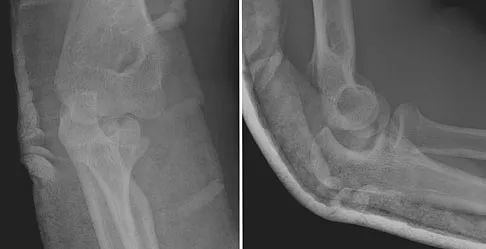
Explanation
Elbow dislocations in children are rare injuries and usually result from a fall on an outstretched arm. The incidence of these injuries increases as patients age and concurrently the incidence of supracondylar humerus fractures decreases. In adolescent patients, simple elbow dislocations are treated with splint immobilization and the initiation of physical therapy once comfortable. The practitioner must be aware of structures that may get caught in the joint on reduction. These include the median nerve as well as the medial epicondyle. In this patient, the radiographs reveal a medial epicondyle fracture. Postreduction radiographs show the joint to be incongruous secondary to intra-articular displacement. At this point, the most appropriate treatment is to perform an open reduction and repair of the medial epicondyle fragment. Rasool MN: Dislocations of the elbow in children. J Bone Joint Surg Br 2004;86:1050-1058.
Question 88
A 19-year-old woman reports lower back pain following a motor vehicle accident. Radiographs obtained immediately after the accident and a bone scan obtained 4 weeks later are shown in Figures 25a through 25c. The patient asks questions regarding the cause, genetics, and natural history of her condition. She should be informed that the condition was
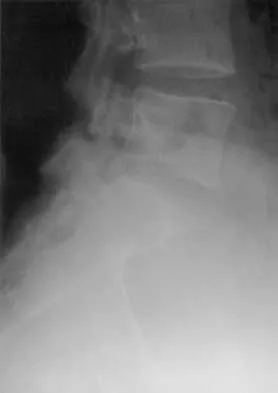
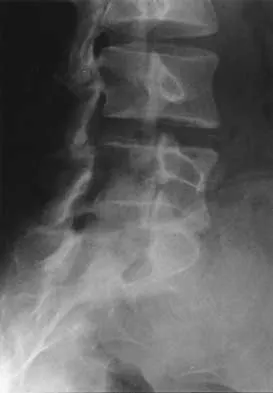
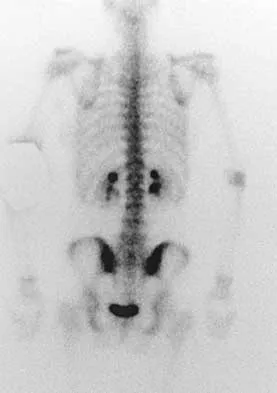
Explanation
The radiographs show L5 spondylolysis without spondylolisthesis (slip). The bone scan is normal, indicating that the pars interarticularis fractures are not acute. The incidence of spondylolysis is approximately 5% in the general population. The lesion generally develops in children age 5 to 6 years, and there is a second peak in the adolescent population. There is a familial predisposition, with reported rates of 27% to 69% in close relatives. A recent long-term follow-up study found that 90% of the spondylolisthesis had occurred before the patient's first visit to the physician. Spondylolisthesis tends to progress during the initial growth spurt and is similar in some respects to idiopathic scoliosis. Progression of a lytic spondylolysis to spondylolisthesis in adulthood has been reported; however, this is exceedingly rare. Lauerman WC, Cain JE: Isthmic spondylolisthesis in the adult. J Am Acad Orthop Surg 1996;4:201-208. Hensinger RN: Spondylolysis and spondylolisthesis in children and adolescents. J Bone Joint Surg Am 1989;71:1098-1107. Seitsalo S, Osterman K, Hyvarinen H, Tallroth K, Schlenzka D, Poussa M: Progression of spondylolisthesis in children and adolescents: A long-term follow-up of 272 patients. Spine 1991;16:417-421.
Question 89
Figure 10 shows the radiograph of an active 75-year-old woman who reports severe leg pain after a fall. Management should consist of
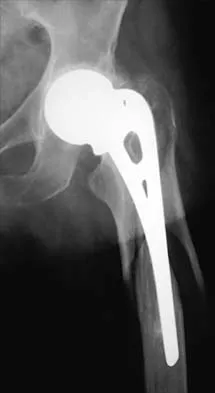
Explanation
The patient has a comminuted fracture of the proximal femur and joint space narrowing of the acetabulum. Therefore, the prosthesis should be converted to a total hip arthroplasty. Because there is extensive comminution, the revision stem should bypass the area of bone loss by two bone diameters. A hemiarthroplasty is not indicated because the patient has no acetabular cartilage. Open reduction and internal fixation may not stabilize the prosthesis. A resection arthroplasty or treatment in traction will not leave the patient with adequate function. Garbuz DS, Masri BA, Duncan CP: Periprosthetic fractures of the femur: Principles of prevention and management, in Cannon WD Jr (ed): Instructional Course Lectures 47. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 237-242.
Question 90
A professional baseball player has had intermittent, mild shoulder pain for the past 2 years. Nonsurgical management has consisted of anti-inflammatory drugs. Examination reveals atrophy of the infraspinatus muscle but not the supraspinatus. There is weakness in external rotation with the arm at his side but not at 90 degrees of abduction. He has no weakness or pain with resisted abduction. Electromyography confirms an isolated lesion of the suprascapular nerve branch to the infraspinatus. He is otherwise neurologically intact. An MRI scan of the shoulder shows no cysts but confirms atrophy of the infraspinatus muscle. What is the next most appropriate step in management?
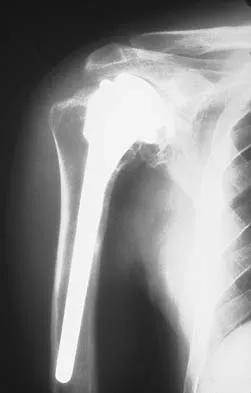
Explanation
Suprascapular nerve injuries are more commonly seen in athletes who participate in overhead activities. When a patient is evaluated for posterior shoulder pain and infraspinatus muscle weakness or atrophy, electrodiagnostic studies are an essential part of the evaluation. In addition, imaging studies are indicated to exclude other diagnoses that can mimic a suprascapular nerve injury. Initial management should consist of cessation of the aggravating activity along with an organized shoulder rehabilitation program. If nonsurgical management fails to provide relief within 6 months to 1 year, surgical exploration of the suprascapular nerve should be considered. Release of the spinoglenoid ligament with resultant suprascapular nerve decompression may result in pain relief and a return of normal shoulder function. In this patient, who has a chronic neuropathy and mild symptoms, surgery is indicated only if nonsurgical management fails to provide relief and he is unable to perform at his position. Cummins CA, Bowen M, Anderson K, et al: Suprascapular nerve entrapment at the spinoglenoid notch in a professional baseball pitcher. Am J Sports Med 1999;27:810-812. Cummins CA, Messer TM, Nuber GW: Suprascapular nerve entrapment. J Bone Joint Surg Am 2000;82:415-424.
Question 91
What effect does deep freezing have on allograft tissue?
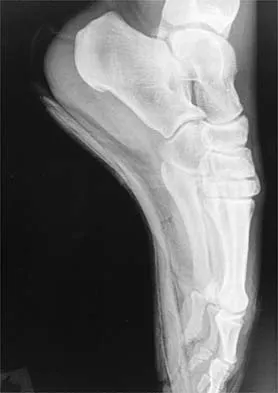
Explanation
Deep freezing is the simplest and most widely used method of ligament allograft storage. All cells in the tissue are destroyed with the freezing. However, for this reason, it is not a preferred storage method for menisci or cartilage allografts. Although this method may enhance success because it removes potential antigens located on the cells, it cannot guarantee elimination of HIV transmission. The advantage of cryopreservation storage is that a significant number of cells will survive the process, a factor important in meniscal allograft survival after implantation. No deleterious effects are noted clinically because of the acellularity of the tissue. Shelton WR, Treacy SH, Dukes AD, Bomboy AL: Use of allografts in knee reconstruction: I. Basic science aspects and current status. J Am Acad Orthop Surg 1998;6:165-168.
Question 92
Figure 33 shows the MRI scan of a 55-year-old woman who has had a 6-week history of back and leg pain. Which of the following clinical scenarios is most consistent with the MRI scan findings at L4-L5?
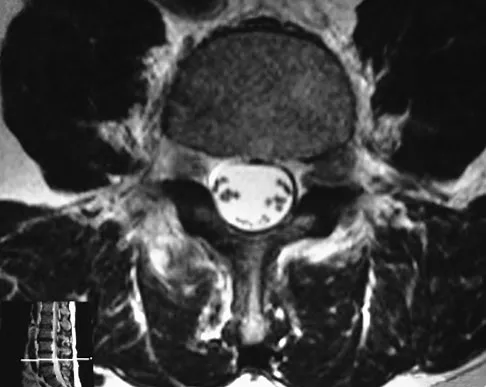
Explanation
The MRI scan reveals a L4-L5 foraminal disk herniation originating from the L4-5 disk space that has migrated up into the foramen, compressing the left L4 nerve root. There is normal distribution of the roots in the cerebrospinal fluid, excluding arachnoiditis as a diagnosis, and disk herniation in this location would not result in cauda equina syndrome or myelopathy.
Question 93
A 51-year-old woman with no preoperative neurologic deficit is undergoing elective anterior cervical diskectomy and fusion (ACDF) with plating and fusion for a C5-6 disk herniation with right-sided neck pain. Thirty minutes into the surgery the neurophysiologic monitoring shows a rapid drop and then loss of amplitude in the right cortical somatosensory-evoked potential waveform. All other waveforms remained normal and unchanged, including right-sided cervical (subcortical) and peripheral (Erb's point), and those from the left-sided upper extremity and both lower extremities. What is the most likely cause of the change?
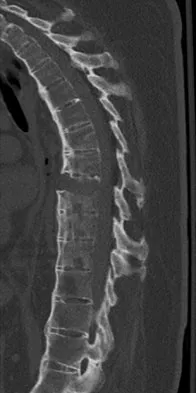
Explanation
The change noted is focal and confined to the cortex, sparing the opposite side, both lower extremities, and the subcortical waveforms, making all the choices unlikely with the exception of carotid compression with focal cortical ischemia. This may be associated with poor collateral flow from the opposite hemisphere due to an incomplete circle of Willis. Drummond JC, Englander RN, Gallo CJ: Cerebral ischemia as an apparent complication of anterior cervical discectomy in a patient with an incomplete circle of Willis. Anesth Analg 2006;102:896-899.
Question 94
Examination of the shoulder seen in Figure 52 shows atrophy and tenderness of the infraspinous fossa and profound weakness in external rotation. The supraspinous fossa shows normal muscle bulk. What is the most likely cause of this condition?
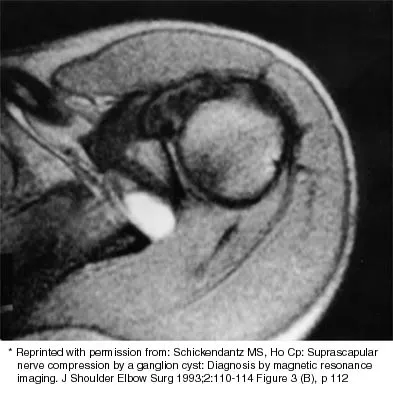
Explanation
Compression of the suprascapular nerve by a ganglion cyst is a well-documented cause of pain and weakness in the shoulder. Isolated involvement of the infraspinatus indicates that the area of entrapment is at the spinoglenoid notch and not the suprascapular notch. The majority of ganglion cysts found in the shoulder are related to tears of the labrum. When such a compressive lesion is found, decompression can be accomplished through either an open or arthroscopic approach. Several authors have shown the value of arthroscopy in the treatment of this condition. It has been shown that it is technically possible to decompress a paralabral ganglion cyst using arthroscopy; this method is usually followed by repair of the torn labrum. Alternatively, arthroscopic repair of the labrum can be performed and the cyst may be aspirated at the time of surgery. Open cyst excision through a posterior approach is also an acceptable method of treatment. Schickendantz MS, Ho CP: Suprascapular nerve compression by a ganglion cyst: Diagnosis by magnetic resonance imaging. J Shoulder Elbow Surg 1993;2:110-114. Thompson RC, Schneider W, Kennedy T: Entrapment neuropathy of the inferior branch of the suprascapular nerve by ganglia. Clin Orthop 1982;166:185-187.
Question 95
A 71-year-old woman undergoes a posterior lumbar decompression and fusion from L4-S1. Thirty-six hours after the procedure, she reports severe right-sided chest pain and shortness of breath. Doppler ultrasound reveals a clot proximal to the knee within the femoral vein. A large pulmonary embolus is confirmed by CT angiography. The next most appropriate step in management should consist of
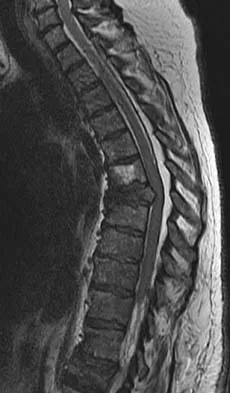
Explanation
In a review of 13,000 spinal procedures, nine patients were treated with heparin following development of pulmonary emboli. Of these patients, six had serious complications ranging from wound drainage to paralysis. Heparin therapy instituted within 10 days of the surgical procedure resulted in a 100% complication rate. Vena cava filter placement has a complication rate of 0.12% to 10.1%. Removable filters are currently in clinical trials. Cain JE Jr, Major MR, Lauerman WC, et al: The morbidity of heparin therapy after development of pulmonary embolus in patients undergoing thoracolumbar or lumbar spinal fusion. Spine 1995;20:1600-1603. Roberts AC: Venous imaging and inferior vena cava filters. Curr Opin Radiol 1992;4:88-96.
Question 96
A 23-year-old man has had heel pain and fullness for the past several months. He reports that initially the pain was present only with activity, but more recently the pain has become constant. Figures 53a through 53d show a radiograph, a bone scan, and T2-weighted and gadolinium MRI scans. What is the most likely diagnosis?
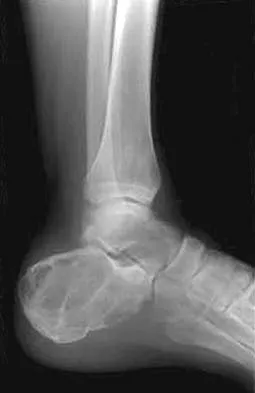
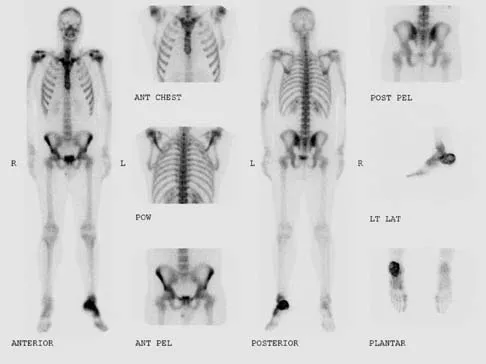
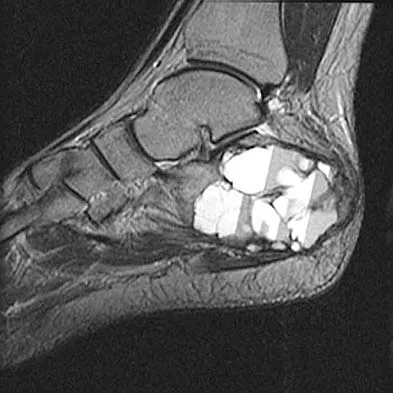
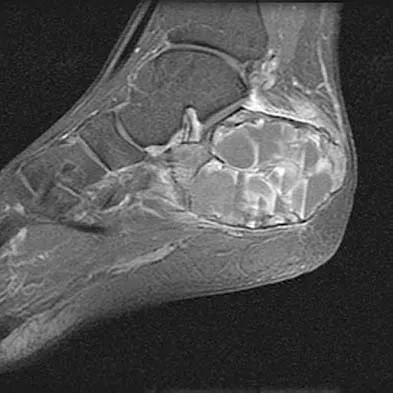
Explanation
The imaging studies reveal an expansile lesion with the classic soap bubble appearance that involves most of the calcaneus. The bone scan reveals a very active lesion with intense uptake, and the MRI scans show the classic, loculated appearance of the lesion with multiple fluid-fluid levels. While it is important to rule out telangiectatic osteosarcoma, the most likely diagnosis is an aneurysmal bone cyst. While giant cell tumor might have a similar appearance, the multiple fluid levels in a expansile lesion strongly favor an aneurysmal bone cyst. Parsons TW: Benign bone tumors, in Fitzgerald RH, Kaufer H, Malkani AL (eds): Orthopaedics. St Louis, MO, Mosby, 2002, pp 1027-1035.
Question 97
In hip arthroplasty, the location of the medial femoral circumflex artery is best described as
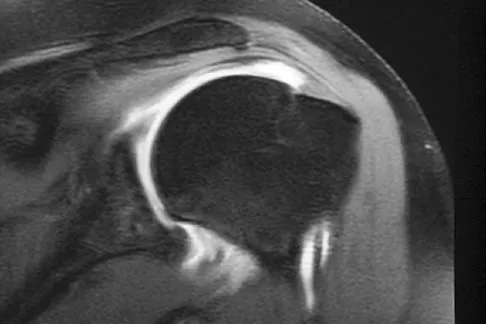
Explanation
The obturator artery lies closest to the transverse acetabular ligament. The femoral artery is closest to the anterior rim of the acetabulum. No named vessel lies within the substance of the gluteus minimus or superior to the piriformis tendon. The medial femoral circumflex artery lies medial or deep to the quadratus femoris muscle. Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics: The Anatomic Approach, ed 1. Philadelphia, PA, JB Lippincott, 1984, Figure 7-53, p 346.
Question 98
An adult patient with a grade I isthmic spondylolisthesis at L5-S1 is most likely to have weakness of the
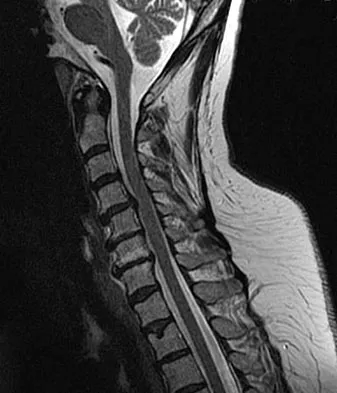
Explanation
Adult patients with isthmic spondylolisthesis most commonly have neurologic symptoms due to foraminal stenosis at the level of the spondylolisthesis. In this scenario, the patient is most likely to have weakness of the L5 myotome, which would cause weakness of the extensor hallucis longus. Spivak JM, Connolly PJ (eds): Orthopaedic Knowledge Update: Spine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 311-317.
Question 99
A 21-year-old man has had progressive right knee pain for the past 2 months that is exacerbated with weight-bearing activities. A plain radiograph and an MRI scan are shown in Figures 43a and 43b. A biopsy specimen is shown in Figure 43c. According to the Enneking staging system of tumor classification, the lesion should be classified as what stage?
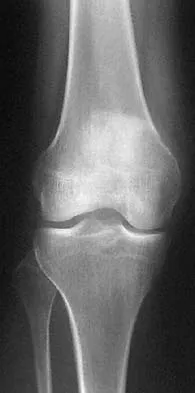
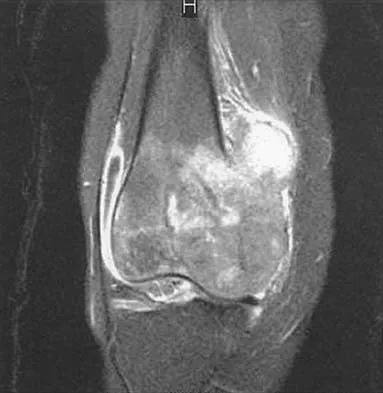
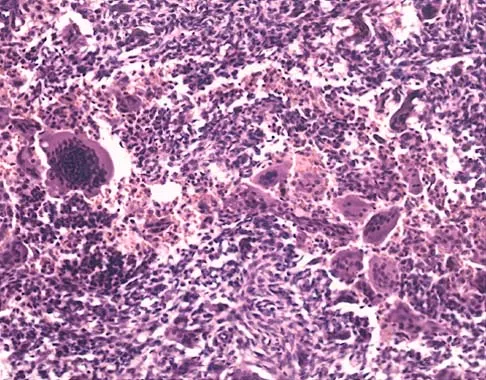
Explanation
The lesion is an eccentric lytic bone lesion within the epiphyseal-metaphyseal end of the proximal tibia. There is geographic destruction with a "fading border" extending to the articular cartilage. There is no matrix formation or periosteal reaction. The MRI scan shows cortical destruction with extension into the soft tissue. According to the Enneking staging system, benign lesions are stage 1, 2, or 3; malignant lesions are stage I, II, or III. Benign stage 1 lesions are latent; stage 2 are active; and stage 3 are benign aggressive. The histology shows a benign giant cell tumor. Given the cortical breakthrough shown on the MRI scan, the lesion should be classified as stage 3. Enneking WF: Clinical musculoskeletal pathology, in Enneking WF (ed): Appendix A. Gainesville, FL, Storter Publishing, 1986, pp 451-466.
Question 100
Which of the following methods is effective in correcting recurrent dislocation following total hip arthroplasty?
Explanation
Recurrent dislocation following total hip arthroplasty is a difficult problem to correct. Studies conducted by the Mayo Clinic show a failure rate of close to 40% with surgical treatment. A variety of methods have been successful, but no specific approach has been reported to be the most predictably successful. To select and institute the proper treatment option, the cause of the dislocation must be identified. Surgical options fall into several broad categories that include increasing soft-tissue tension (trochanteric advancement or longer neck lengths) or more stable articulation (larger diameter head component, bipolar prosthesis, or a constrained component). In a series of total hip arthroplasties done with a constrained cup, the loosening rates of the cup and the stem were reported to be 6% each, comparable to a reported series of complex revision total hip arthroplasties at a similar follow-up interval. Woo RY, Morrey BF: Dislocations after total hip arthroplasty. J Bone Joint Surg Am 1982;64:1295-1306.
