Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
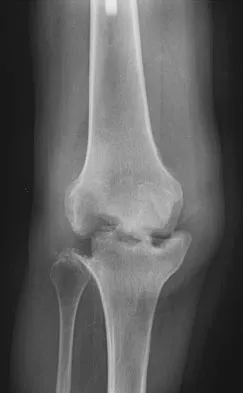
Figure 6 shows the radiograph of a 14-year-old baseball player who felt a pop and had an immediate onset of pain in his elbow after a hard throw from the outfield. The best course of action should be to
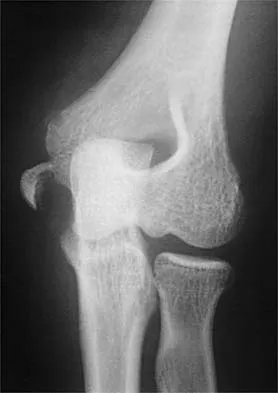
Explanation
The valgus stress at the elbow caused by throwing strains the medial collateral ligament. The medial epicondyle, on which the ligament inserts, is the last ossification center to fuse to the distal humerus, and acute avulsion of the medial epicondyle can occur in adolescents. If the elbow is allowed to heal in a displaced position, valgus instability and loss of elbow extension may result. Valgus instability is especially problematic for the throwing athlete. Surgical treatment with rigid internal fixation is the treatment of choice for displaced medial epicondyle avulsion fractures. Valgus instability is prevented, and the rigid fixation allows for early range of motion. Case SL, Hennrikus WL: Surgical treatment of displaced medial epicondyle fractures in adolescent athletes. Am J Sports Med 1997;25:682-686.
Question 2
A 13-year-old girl is diagnosed with a stage IIB osteosarcoma of the proximal tibia. Following neoadjuvant chemotherapy, local control should consist of
Explanation
Local control of osteosarcoma consists of wide resection and reconstruction. Radiation therapy is not recommended except in unresectable lesions or for palliation. Curettage and bone grafting result in intralesional resection with an unacceptable high rate of local recurrence. Chemotherapy alone is not adequate for local control. Simon M, Springfield D, et al: Osteogenic Sarcoma: Surgery for Bone and Soft Tissue. Philadelphia, PA, Lippincott Raven, 1998, p 274.
Question 3
Which of the following lumbar disk components has the highest tensile modulus to resist torsional, axial, and tensile loads?
Explanation
The annulus fibrosis has a multilayer lamellar architecture mode of type I collagen fibers. Each successive layer is oriented at 30 degrees to the horizontal in the opposite direction, leading to a "criss-cross" type pattern. This composition allows the annulus, which has the highest tensile modulus, to resist torsional, axial, and tensile loads.
Question 4
In children with isolated zone II lacerations of the flexor tendon, poor digital motion is best correlated with
Explanation
In a recent study on restoration of motion following zone I and zone II flexor tendon repairs in children, age was found to have no effect on the results of zone II tendon repairs. Early passive motion offered no better results than immobilization for 3 weeks. Immobilization for more than 4 weeks correlated with poorer results.
Question 5
A 22-year-old competitive volleyball player has shoulder pain, and rest and a cortisone injection have failed to provide relief. Examination reveals atrophy along the posterior scapula, but an MRI scan does not reveal a rotator cuff tear or labral cyst. What is the most likely cause for the shoulder weakness?
Explanation
Repetitive overhead slams and serves may produce a traction injury to the distal branch of the suprascapular nerve. Bankart, biceps, and superior labrum anterior and posterior injuries can occur but usually do not produce visible atrophy. Muscle avulsion is uncommon. Ferretti A, Cerullo G, Russo G: Suprascapular neuropathy in volleyball players. J Bone Joint Surg Am 1987;69:260-263.
Question 6
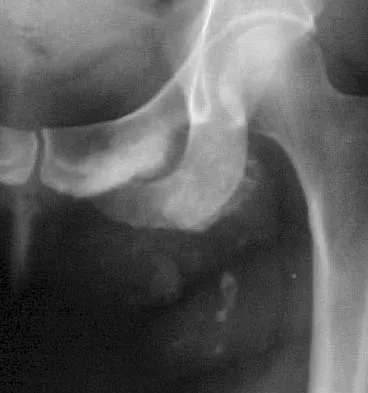
Figure 29 shows the radiograph of a 55-year-old patient who has recurrent total hip dislocation. Dislocation is most likely to occur in this patient when the hip is in which of the following positions?
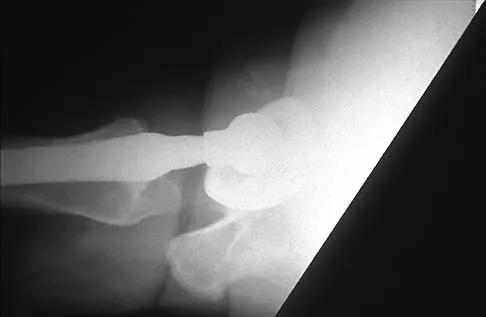
Explanation
The patient has an acetabular component that is placed in excessive anteversion; this is confirmed by the shoot-through radiograph. The most common reasons for dislocation of a total hip replacement include inappropriate positioning of the components, inadequate abductor tension, or impingement. Implants placed without adequate total anteversion tend to dislocate posteriorly, and implants with excessive anteversion tend to dislocate anteriorly. Superior dislocations can occur if the acetabular component is placed in a severely vertical position with inadequate lateral coverage.
Question 7
When comparing the overall outcomes of surgical versus nonsurgical treatment of stable thoracolumbar burst fractures in patients without neurologic injury, 5 years following injury, the principle differences lie in
Explanation
When patients are compared at 5 years follow-up, there are no statistically significant differences between the two groups with respect to kyphosis, the degree of retropulsed bone resorption, pain and function levels, or the ability to return to work. Nonsurgical management of stable neurologically intact burst fractures has a very low incidence of complications. Wood K, Butterman G, Mehbod A, et al: Operative compared with nonoperative treatment of a thoracolumbar burst fracture without neurological deficit: A prospective, randomized study. J Bone Joint Surg Am 2003;85:773-781.
Question 8
Which of the following statements best describes the anatomic considerations of the popliteal artery posterior to the knee joint?
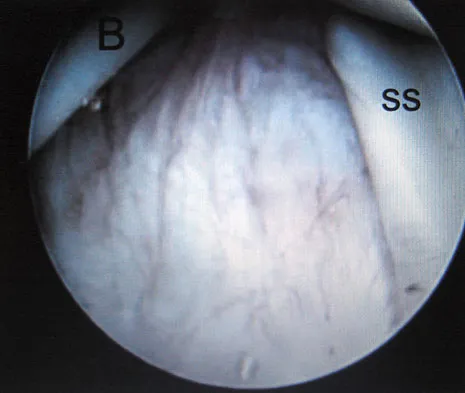
Explanation
Popliteal artery injury during total knee arthroplasty is relatively rare. Knee flexion, the position that occurs during most of the arthroplasty procedure, allows the popliteal vessels to fall posteriorly, further away from harm. Anatomically, the popliteal artery lies anterior to the popliteal vein and 9 mm posterior to the posterior aspect of the tibial plateau in 90 degrees of flexion. Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, p 151.
Question 9
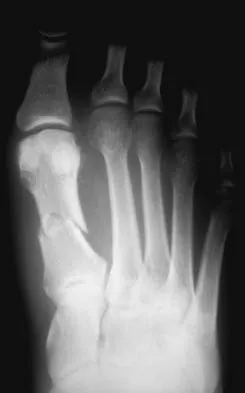
Figures 9a and 9b show the radiographs of a 28-year-old woman who sustained a head injury and a closed injury, without soft-tissue compromise, to her right lower extremity in a motor vehicle accident. Appropriate management of the foot injury should include
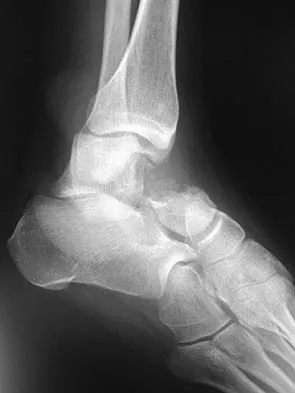
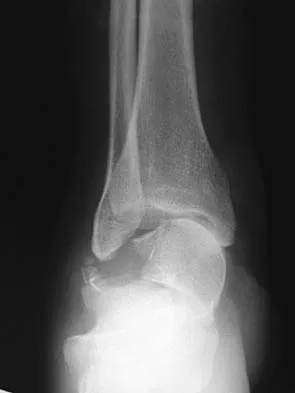
Explanation
The displaced talar neck fracture should be treated with open reduction and internal fixation using screws. Closed reduction and casting will not maintain position, and percutaneous pinning is not able to maintain reduction to allow union. External fixation and amputation are not necessary for this injury unless there is severe soft-tissue loss.
Question 10
A 47-year-old patient has had persistent pain and weakness after undergoing a reamed intramedullary nailing for a midshaft humerus fracture 8 months ago. There is no evidence of infection. Radiographs are shown in Figures 19a and 19b. Management should consist of
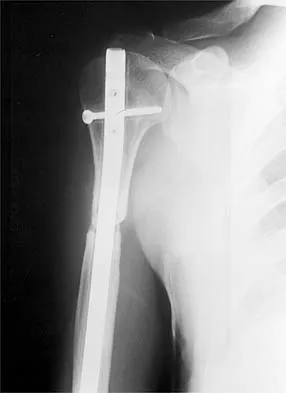

Explanation
Compression plating remains the treatment of choice for most established humeral nonunions. Autograft is felt to be superior to allograft. Electrical stimulation has not been found to improve healing rates in patients with nonunion after intramedullary nailing. Retrograde nailing with flexible nails gives inadequate rotational control to promote healing in this patient. Adding cancellous graft alone will not stabilize the nonunion site. Dynamic locking has been successful only in the lower extremity because the bone can be loaded axially. McKee MD, Miranda MA, Riemer BL, et al: Management of humeral nonunion after the failure of locking intramedullary nails. J Orthop Trauma 1996;10:492-499.
Question 11
The MRI scan of the shoulder shown in Figure 2 was performed with the arm in abduction and external rotation. The image reveals what condition?
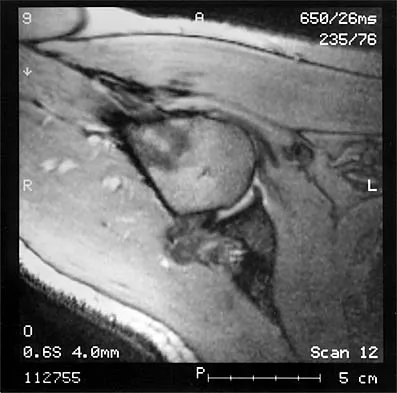
Explanation
Internal impingement of the shoulder is now a well-recognized cause of shoulder pain in the throwing athlete. First described by Walch and associates, it involves contact of the rotator cuff and labrum in the maximally externally rotated and abducted shoulder, such as in the late cocking phase of the throwing motion. Schickendantz and associates have shown this contact to be physiologic in most patients and becoming pathologic with repetitive overhead activity. Schickendantz MS, Ho CP, Keppler L, Shaw BD: MR imaging of the thrower's shoulder: Internal impingement, latissimus dorsi/subscapularis strains, and related injuries. Magn Reson Imaging Clin N Am 1999;7:39-49. Walch G, Boileau P, Noel E, et al: Impingement of the deep surface of the supraspinatus tendon on the posterosuperior glenoid rim: An arthroscopic study. J Shoulder Elbow Surg 1992;1:238-245.
Question 12
A 60-year-old woman reports anterior knee pain 2 years after undergoing primary total knee arthroplasty for rheumatoid arthritis. A Merchant view of the patella is shown in Figure 16. What is the most likely cause of her pain?

Explanation
Patellar complications commonly occur after primary total knee arthroplasty; therefore, proper component positioning is critical in obtaining a successful result. This patient has lateral tilting and subluxation of the patellar component. Internal rotation of the femoral component has the most deleterious effect on patellar tracking. Lateral placement of the femoral component, medial placement of the patellar component, and external rotation of the tibial component have beneficial effects on patellar tracking. Elevation of the joint line, if not excessive, should not impact patellar tracking. Rand JA: Patellar resurfacing in total knee arthroplasty. Clin Orthop 1990;260:110-117.
Question 13
In the preoperative planning of revision acetabular reconstruction, the surgeon should identify significant posterior column deficiency by noting which of the following radiographic features?
Explanation
Proximal and medial migration of the femoral head usually indicates deficiencies of the dome or anterior column. Wear of the polyethylene may result in osteolysis and impingement, which are not indicative of any major bone deficiency. A significant osteolytic lesion in the ischium may represent a major posterior column deficiency that can create a technical challenge during the reconstruction. Paprosky WG, Magnus RE: Principles of bone grafting in revision total hip arthroplasty: Acetabular technique. Clin Orthop 1994;298:147-155.
Question 14
A 7-year-old girl has had a painful forearm for the past 2 months. Examination reveals fullness on the volar aspect of the forearm. Radiographs and an MRI scan are shown in Figures 42a through 42c. Biopsy specimens are shown in Figures 42d and 42e. What is the most likely diagnosis?
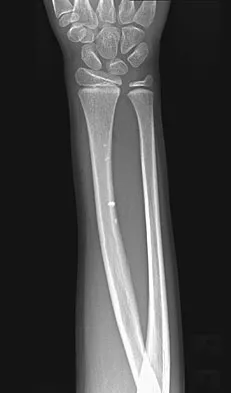
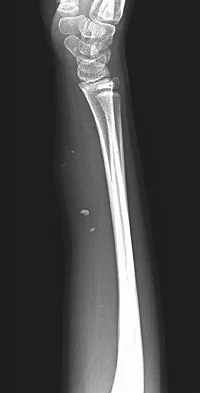
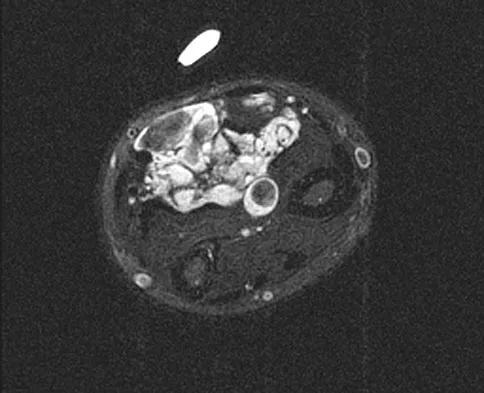
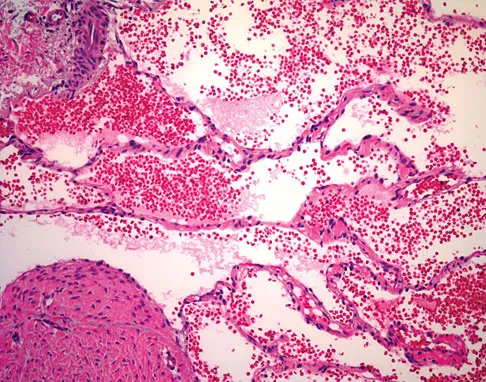
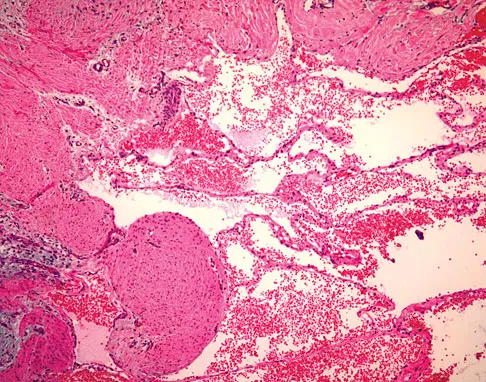
Explanation
The radiographs reveal phleboliths on the volar side of the forearm consistent with hemangioma. The MRI scan reveals a rather well-circumscribed in size, irregular in shape, intramuscular soft-tissue mass in the volar aspect of the distal right forearm within the flexor group musculature. The mass demonstrates heterogeneous mixed signal intensity in both T1- and T2-weighted sequences with increased signal intensity on the T1, suggesting fat within the tumor, typical of hemangioma. The postgadolinium-enhanced sequences demonstrate heterogeneous enhancement. The MRI findings are consistent with a soft-tissue hemangioma. Garzon M: Hemangiomas: Update on classification, clinical presentation and associate anomalies. Cutis 2000;66:325-328.
Question 15
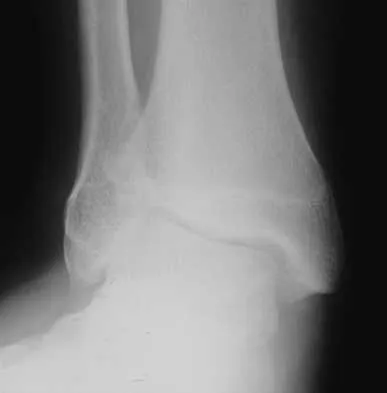
An active 60-year-old man is evaluated 4 years following surgical correction of a hallux valgus deformity. The patient reports that a hallux varus deformity developed rapidly following his initial surgery. Conservative management consisting of wider shoes, toe strapping, and anti-inflammatory drugs has failed to provide relief. Examination reveals a hallux varus deformity with restricted painful motion of the metatarsophalangeal joint and callus formation under the second metatarsal head. What is the next most appropriate step in management?
Explanation
Hallux varus may occur as a complication following hallux valgus surgery, most commonly a modified McBride-type procedure. Conservative management is the initial treatment of choice; however, if unsuccessful, surgical options for reconstruction include soft-tissue reconstruction or metatarsophalangeal joint arthrodesis. The patient has evidence of joint arthrosis, making an arthrodesis the preferred method of reconstruction. Fascial arthroplasty, Silastic arthroplasty, and Keller resection arthroplasty will not correct the underlying deformity. Kitaoka HB, Patzer GL: Arthrodesis versus resection arthroplasty for failed hallux valgus operations. Clin Orthop 1998;347:208-214.
Question 16
What is the primary indication for performing an arthroscopic synovectomy on a patient with hemophilia that is the result of factor VIII deficiency?
Explanation
Improved medical management has changed musculoskeletal outcomes for individuals with hemophilia. Patients with severe hemophilia receiving prophylactic administration of factor VIII may never develop a target joint that requires further orthopaedic intervention. Patients with moderate hemophilia and those patients with severe hemophilia not receiving prophylactic treatment will still develop joints that have recurrent hemarthroses. When recurrent hemarthrosis continues despite optimal medical management, synovectomy is indicated. While synovectomy is predictable in its ability to decrease joint bleeding, it does not necessarily improve joint range of motion or prevent the development of hemophilic arthropathy over time. It will not reverse articular damage to the joint once it has developed. Dunn AL, Busch MT, Wyly JB; et al: Arthroscopic synovectomy for hemophilic joint disease in a pediatric population. J Pediatr Orthop 2004;24:414-426.
Question 17
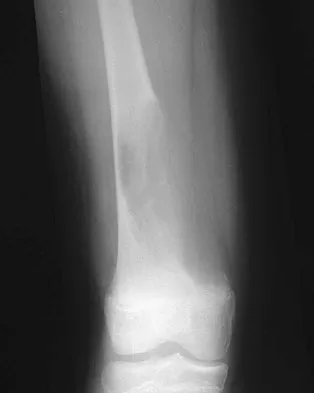
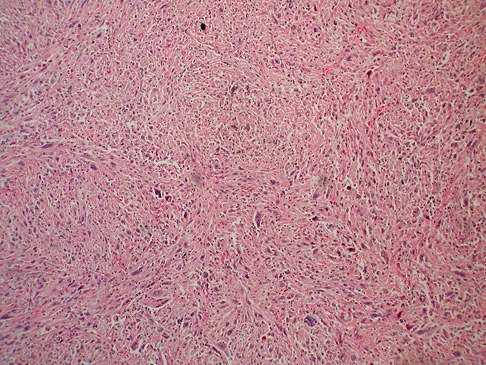
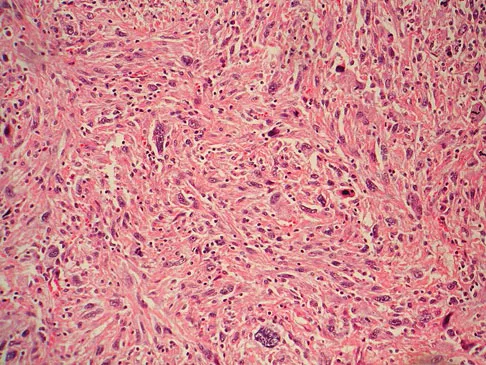
A 12-year-old girl has had increasing left knee pain for the past 3 months. A radiograph is shown in Figure 75a, and low- and high-power photomicrographs are shown in Figures 75b and 75c. What is the most appropriate treatment?
Explanation
The radiograph reveals an aggressive purely lytic lesion of the distal femoral metaphysis. There is no apparent matrix mineralization or periosteal reaction. The photomicrographs show a malignant spindle cell neoplasm in a storiform pattern. Based on these findings, the diagnosis is malignant fibrous histiocytoma of bone. At most institutions, patients with this tumor are treated similar to patients with osteosarcoma with multi-agent chemotherapy and surgery with wide margins (resection or amputation). Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 203-209.
Question 18
A 13-year-old boy is comatose and has irregular breathing after being struck by a car while riding his bicycle. Auscultation suggests a pneumothorax on the right side and swelling about the right arm and leg. Initial management should consist of
Explanation
The first priority is to gain control of the airway with intubation. Following intubation, management should consist of ventilation and placement of a chest tube if needed, vascular access and circulatory stabilization, radiographs of the cervical spine and chest, and CT of the brain. American College of Surgeons Committee on Trauma. Advanced Trauma Life Support Course. Instructor's Manual. Chicago, IL, American College of Surgeons, 1984.
Question 19
A patient undergoes excision of a 3- x 3-cm soft-tissue sarcoma. The final histology results show tumor at the surgical margin. The surgical procedure performed is classified as
Explanation
Surgical margins are classified according to the plane of dissection in relation to the tumor. An intralesional procedure is where the plane of dissection passes through the tumor. A marginal resection involves a resection where the plane of dissection is through the reactive zone of the tumor. A wide resection is through completely normal tissue outside of the reactive zone. A radical resection removes all of the muscles and/or bone of the compartment that are involved by the tumor.
Question 20
A metal-on-metal bearing used for total hip arthroplasty shows which of the following properties?
Explanation
Activity levels do not affect cobalt and chromium ion levels, which are the bulk of serum ion levels. The majority of ions are produced in the run-in period in the first several years. A gradual reduction in ion levels occurs thereafter. The kidneys are responsible for the bulk of clearance from the serum, and to date there is no relationship of cancer to ion levels in the serum.
Question 21
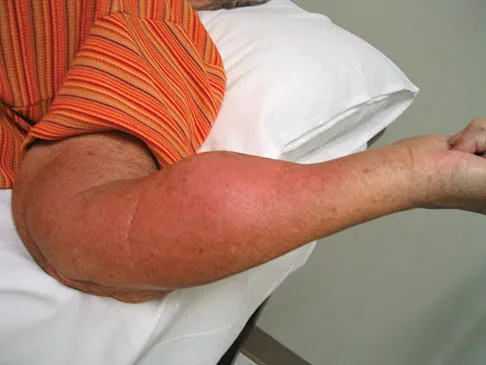
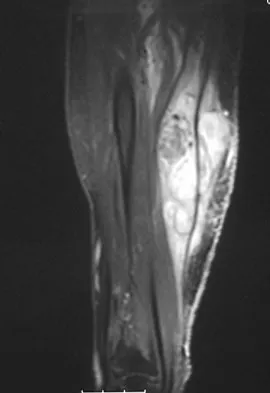
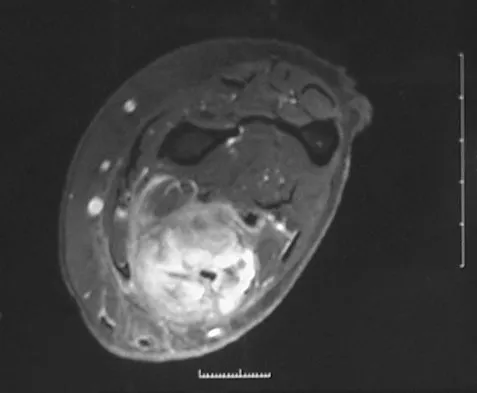
Figure 8a shows the clinical photograph of an 83-year-old woman who has an enlarging left forearm mass. MRI scans are shown in Figures 8b and 8c. What is the next most appropriate step in management?
Explanation
Any large (greater than 5 cm), deep, heterogeneous mass in the extremities should be considered a sarcoma until proven otherwise. Sarcomas are rare, and without a high index of suspicion, the lesions may be misdiagnosed or there may be a delay in diagnosis. Needle biopsies can obtain sufficient tissue for diagnosis and are associated with less morbidity than open biopsy. Marginal resections or excisional biopsies should be reserved for a few select benign lesions and locations. Damron TA, Beauchamp CP, Rougraff BT, et al: Soft-tissue lumps and bumps. Instr Course Lect 2004;53:625-637.
Question 22
Which of the following tumors is most likely to present with a pathologic fracture in a child?
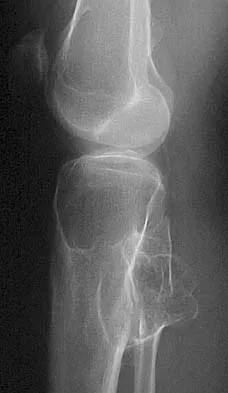
Explanation
In nearly 50% of patients with a unicameral bone cyst, the lesion remains asymptomatic until a fracture occurs, usually as the result of relatively minor trauma. If the lesion expands, the bone is weakened and may cause pain. Fibrous cortical defects are usually an incidental finding and typically asymptomatic. Malignant bone tumors such as osteosarcoma and Ewing's sarcoma most commonly cause pain, and pathologic fracture occurs in less than 10% of patients. Giant cell tumors are uncommon in children and usually are painful. Wilkins RM: Unicameral bone cysts. J Am Acad Orthop Surg 2000;8:217-224. Dormans JP, Pill SG: Fractures through bone cysts: Unicameral bone cysts, aneurysmal bone cysts, fibrous cortical defects, and nonossifying fibromas. Instr Course Lect 2002;51:457-467.
Question 23
A 62-year-old man with diabetes mellitus has had a persistent 2-cm ulcer under the third metatarsal head for the past 4 months. He reports that he has had similar ulcers twice before, and both healed with nonsurgical management. He has used multiple types of commercial walking braces, shoes, and commercial dressings without resolution. He is insensate to the Semmes-Weinstein 5.07 monofilament. When the wound is probed with culture swab, there is no communication with the metatarsal head. Radiographs, bone scans, and laboratory studies reveal no evidence of osteomyelitis. What is the most predictable method of accomplishing wound healing without recurrence?
Explanation
The patient has a persistent diabetic foot ulcer without evidence of osteomyelitis. He has evidence of a sensory peripheral neuropathy and a concomitant motor neuropathy, leading to a dynamic motor imbalance. Use of a total contact cast would offer a high probability of healing the resistant ulcer but with a high potential for recurrence. Combining the total contact cast with Achilles tendon lengthening allows wound healing without a high risk for recurrence. Excision of the noninfected metatarsal head would make the patient vulnerable to the development of a transfer lesion under one of the remaining metatarsal heads. Robertson DD, Mueller MJ, Smith KE, et al: Structural changes in the forefoot of individuals with diabetes and a prior plantar ulcer. J Bone Joint Surg Am 2002;84:1395-1404.
Question 24
Closed-chain exercise differs from open-chain exercise in which of the following ways?
Explanation
Closed-chain exercise requires the distal portion of the extremity to be fixed. It is more commonly used in lower extremity exercise, and movement is produced by co-contraction of muscles. Joint compression is increased, and multiple joints are involved with closed-chain exercise. In open-chain exercise, the distal portion of the extremity is free. Braddom RL (ed): Physical Medicine and Rehabilitation, ed 2. Philadelphia, PA, Saunders, 2000, pp 975-976.
Question 25
A 9-year-old boy has pain over the midfoot medially with activity. Based on the findings shown in Figures 26a and 26b, which of the following is considered the most effective short-term management?
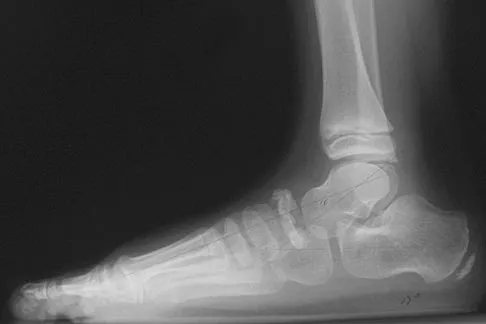
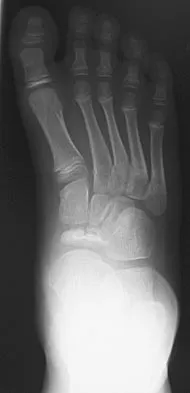
Explanation
While Kohler's disease has a benign course, temporary cast immobilization has been shown to result in a shortened duration of symptoms. Core decompression or other surgery is not warranted because of the benign nature. Shoe inserts may be beneficial, but there are no studies to support their use. Borges JL, Guile JT, Bowen JR: Kohler's bone disease of the tarsal navicular. J Pediatr Orthop 1995;15:596-598.
Question 26
A 39-year-old woman fell onto her flexed elbow and sustained a comminuted displaced radial head and neck fracture. Radiographs confirm concentric reduction of the ulnohumeral joint. Examination reveals pain with compression of the radius and ulna at the wrist. What is the best treatment for the radial head fracture?
Explanation
Patients with comminuted radial neck and head fractures and associated wrist pain have a significant injury to the elbow and forearm. Nonsurgical management is an option, but initial casting will result in stiffness and early range of motion is likely to be unsuccessful secondary to pain. Surgical treatment with open reduction and internal fixation, although possible, is technically demanding and results are unpredictable with comminuted fractures. Excision alone in the face of wrist pain may lead to radial shortening. The treatment of choice is excision and metallic radial head arthroplasty. Silastic implants have been associated with synovitis and wear debris. Furry KL, Clinkscales CM: Comminuted fractures of the radial head: Arthroplasty versus internal fixation. Clin Orthop 1998;353:40-52.
Question 27
A 68-year-old man reports a 1-year history of debilitating neck pain without neurologic symptoms. History reveals a C5-6 anterior diskectomy and bone grafting 10 years ago that provided good relief of arm and neck pain. Radiographs show evidence of fibrous union at C5-6, spondylotic disk narrowing at C4-5 and C6-7, and a fixed 2-mm subluxation at C3-4. Examination reveals cervical stiffness and discomfort at the extremes of movement. His neurologic examination is normal. Treatment should now consist of
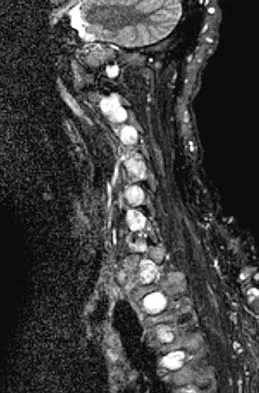
Explanation
Axial pain can be difficult to manage. Pain management is not always successful, and surgical approaches may provide disappointing results unless there is discrete pathology. Whereas planning of a surgical approach should consider prior approaches and preexisting laryngeal dysfunction, no compelling case for surgical intervention can be made for this patient. Therefore, management should consist of patient education, exercise, and nonnarcotic medication. Ahn NU, Ahn UM, Andersson GB, et al: Operative treatment of the patient with neck pain. Phys Med Rehabil Clin N Am 2003;14:675-692. Algers G, Pettersson K, Hildingsson C, et al: Surgery for chronic symptoms after whiplash injury: Follow-up of 20 cases. Acta Orthop Scand 1993;64:654-656.
Question 28
An elite skier training for the Olympics sustains an isolated traumatic dislocation of the peroneal tendons that have spontaneously reduced. The games are 9 months away and the athlete does not want to miss them. Treatment should consist of
Explanation
Most of these injuries occur in young, active patients. Success rates for nonsurgical management are only marginally better than 50%. The treatment of choice is early surgery for patients who desire a quick return to a sport or active lifestyle. Subluxation of the peroneal tendons leads to longitudinal tears over time. McLennan JG: Treatment of acute and chronic luxations of the peroneal tendons. Am J Sports Med 1980;8:432-436.
Question 29
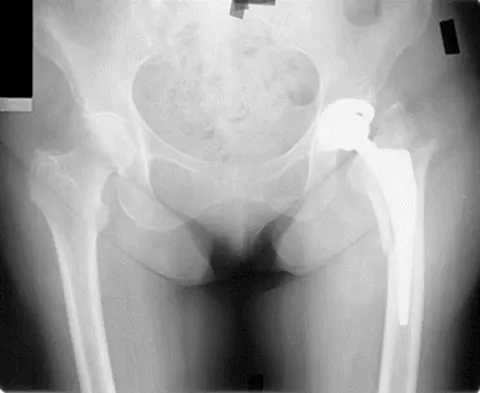
A 53-year-old patient is seen in the emergency department after sustaining a fall onto her left hip. A current radiograph is shown in Figure 40. What is the best treatment option?
Explanation
The patient has sustained a Vancouver B2 periprosthetic femoral fracture (a femoral fracture that occurs around or just distal to a loose stem, with adequate proximal bone stock). The stem is no longer fixed to proximal bone; therefore, retention of the femoral component is not recommended. Nonsurgical management is contraindicated because of the high risk of nonunion and malunion with significant component settling in the distal fragment and leg shortening. Revision femoral arthoplasty must attain distal fixation in adequate host bone, which is usually successful with a porous-coated cylindrical stem. Parvizi J, Rapuri VR, Purtill JJ, et al: Treatment protocol for proximal femoral periprosthetic fractures. J Bone Joint Surg Am 2004;86:8-16.
Question 30
A 24-year-old dancer reports posterior ankle pain when in the "en pointe" position. Examination reveals posteromedial tenderness, no pain reproduction with passive forced planter flexion, and pain with motion of the hallux. What is the most likely diagnosis?
Explanation
Flexor hallucis longus tendinitis is a common cause of posterior ankle pain in dancers. It tends to be more posteromedial and is characterized by a clicking or catching sensation posteromedially with motion of the great toe. A painful os trigonum typically causes more posterolateral ankle pain and may occur after an ankle sprain or plantar flexion injury where there may be a fracture of the os trigonum. Garrick JG (ed): Orthopaedic Knowledge Update: Sports Medicine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 249-261.
Question 31
You are interested in learning a new technique for minimally invasive total knee arthroplasty. The Keyhole Genuflex system seems appealing to you because the instrumentation comes with wireless controls. Which of the following represents an acceptable arrangement?
Explanation
Both the AAOS and AdvaMed, the medical device manufacturer's trade organization, have written guidelines that address potential conflicts of interest regarding interactions between physicians and manufacturer's representatives when it comes to patients' best interest. The AAOS feels that the orthopaedic profession exists for the primary purpose of caring for the patient and that the physician-patient relationship is the central focus of all ethical concerns. When an orthopaedic surgeon receives anything of significant value from industry, a potential conflict of interest exists. The AAOS believes that it is acceptable for industry to provide financial and other support to orthopaedic surgeons if such support has significant educational value and has the purpose of improving patient care. All dealings between orthopaedic surgeons and industry should benefit the patient and be able to withstand public scrutiny. A gift of any kind from industry should in no way influence the orthopaedic surgeon in determining the most appropriate treatment for his or her patient. Orthopaedic surgeons should not accept gifts or other financial support with conditions attached. Subsidies by industry to underwrite the costs of educational events where CME credits are provided can contribute to the improvement of patient care and are acceptable. A corporate subsidy received by the conference's sponsor is acceptable; however, direct industry reimbursement for an orthopaedic surgeon to attend a CME educational event is not appropriate. Special circumstances may arise in which orthopaedic surgeons may be required to learn new surgical techniques demonstrated by an expert or to review new implants or other devices on-site. In these circumstances, reimbursement for expenses may be appropriate. AAOS Standard of Professionalism -Orthopaedist -Industry Conflict of Interest (Adopted 4/18/07), Mandatory Standard numbers 6, 9, 12-15. http://www3.aaos.org/member/profcomp/SOPConflictsIndustry.pdf The Orthopaedic Surgeon's Relationship with Industry, in Guide to the Ethical Practice of Orthopaedic Surgery, ed 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2007. http://www.aaos.org/about/papers/ethics/1204eth.asp
Question 32
An inverted radial reflex is associated with
Explanation
An inverted radial reflex is a hypoactive brachioradialis reflex in combination with involuntary finger flexion. It is a spinal cord "release" sign and is associated with upper motor neuron pathology as seen in cervical stenosis with myelopathy. Radiculopathy is characterized by a diminished reflex but no finger flexion. Peripheral neuropathy is not associated with any reflex change. Parsonage-Turner syndrome is an idiopathic brachial neuritis. Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Williams & Wilkins, 1998, p 762.
Question 33
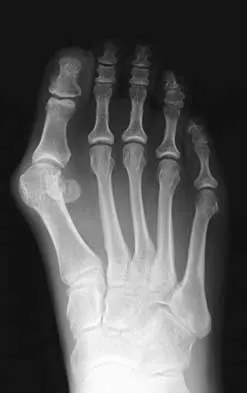
A 47-year-old woman has a right bunion that has been symptomatic despite modifications in shoe wear. She requests surgical correction. An AP radiograph is shown in Figure 37. Treatment should consist of
Explanation
Because the radiograph reveals an intermetatarsal angle of greater than 15 degrees and an incongruent metatarsophalangeal joint, the treatment of choice is a proximal first metatarsal osteotomy with distal soft-tissue realignment. A distal chevron procedure would not correct this degree of deformity. A Keller procedure is reserved for a less active elderly individual. Arthrodesis is appropriate for a patient with advanced arthritis of the metatarsophalangeal joint. The double osteotomy is reserved for the congruent metatarsophalangeal joint with hallux valgus. Coughlin MJ, Carlson RE: Treatment of hallux valgus with an increased distal metatarsal articular angle: Evaluation of double and triple first ray osteotomies. Foot Ankle Int 1999;20:762-770.
Question 34
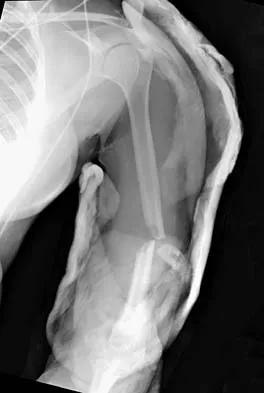
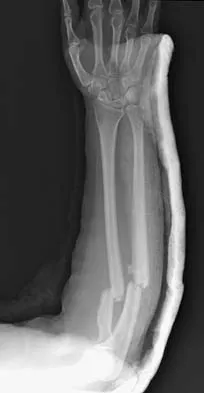
A 32-year-old woman sustained an injury to her left upper extremity in a motor vehicle accident. Examination reveals a 2-cm wound in the mid portion of the dorsal surface of the upper arm and deformities at the elbow and forearm; there are no other injuries. Her vital signs are stable, and she has a base deficit of minus 1 and a lactate level of less than 2. Radiographs are shown in Figures 9a and 9b. In addition to urgent debridement of the humeral shaft fracture, management should include
Explanation
With a severe injury to the upper extremity, the best opportunity for achieving a good functional result for a floating elbow is immediate debridement of the open fracture, followed by internal fixation of the fractures. The ability to do this depends on the patient's physiologic status. In this patient, the procedure is acceptable because she has normal vital signs and no chest or abdominal injuries, and normal physiologic parameters (base excess and lactate) show adequate peripheral perfusion. The surgical approaches will be determined by the associated injury patterns and open wounds. In this patient, the humerus was debrided and stabilized through a posterior approach as was the medial condyle fracture. The ulna was fixed through an extension of the posterior incision and the radius through a separate dorsal approach. Solomon HB, Zadnik M, Eglseder WA: A review of outcomes in 18 patients with floating elbow. J Orthop Trauma 2003;17:563-570.
Question 35
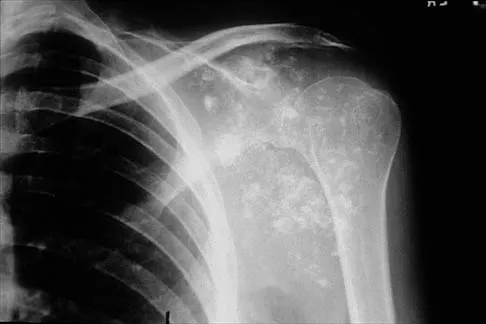
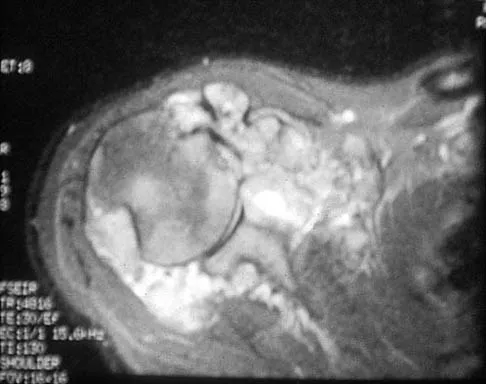
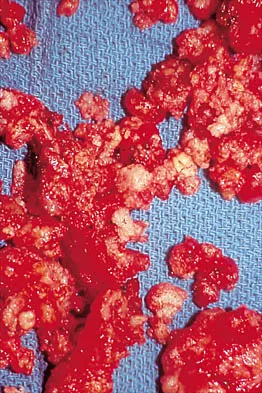
A 32-year-old woman has had pain and a visibly growing mass in the shoulder for 3 years but denies any history of trauma. Examination reveals a swollen, boggy shoulder mass. The AP radiograph and MRI scan are shown in Figures 20a and 20b. Figures 20c through 20e show a portion of the excised mass and the photomicrographs of the biopsy specimen. What is the most likely diagnosis?
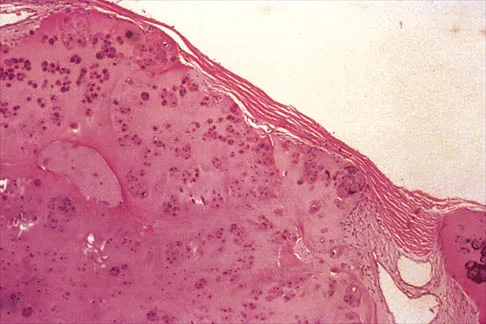
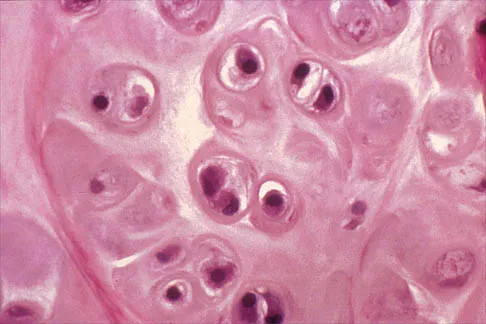
Explanation
The radiographic findings are classic for synovial chondromatosis because of the small calcified opacities within the joint surrounding the synovium. The histologic findings show cartilaginous foci of metaplasia, which may be markedly cellular. However, unlike low-grade chondrosarcoma, it lacks cellular and nuclear pleomorphism. Murphy FP, Dahlin DC, Sullivan CR: Articular synovial chondromatosis. J Bone Joint Surg Am 1982;44:77-86.
Question 36
A patient who is an observant Jehovah's Witness requires major surgery for scoliosis that will likely result in significant blood loss. Which of the following might the patient consider allowing the surgical team to use?
Explanation
Jehovah's Witnesses will not accept the transfusion of blood or blood products such as packed red or white cells, platelets, or plasma. However, many Jehovah's Witnesses will accept the use of a cell saver in a "closed circuit." Jimenez R, Lewis VO (eds): Culturally Competent Care Guidebook. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2007.
Question 37
Which of the following factors will adversely affect bone ingrowth in a revision porous-coated stem?
Explanation
The optimal conditions for bony ingrowth include a pore size of 100 to 400 um, interface micromotion of 50 um or less, intimate contact between the bone and the implant, circumferential porous coating of the implant, and use of a biocompatible material. Stem designs with patch coatings have a poor record of bony ingrowth, especially in the revision setting. Failure of ingrowth in the previous stem would be the result of its own mechanical milieu and would not necessarily predict results for the new stem. Berry DJ, Harmsen WS, Ilstrup D, Lewallen DG, Cabanela ME: Survivorship of uncemented proximally porous-coated femoral components. Clin Orthop 1995;319:168-177. Cook SD, Thomas KA, Haddad RJ Jr: Histologic analysis of retrieved human porous-coated total joint components. Clin Orthop 1988;234:90-101.
Question 38
A 54-year-old woman sustained an elbow injury 3 months ago that was treated with open reduction and internal fixation. She now reports pain and limited elbow motion. Radiographs are shown in Figures 10a and 10b. Treatment should now consist of
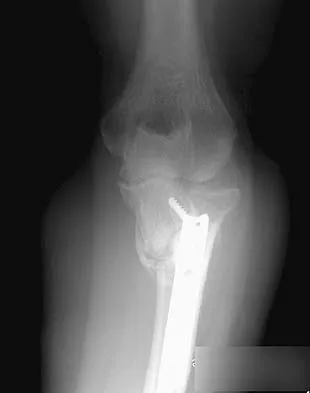
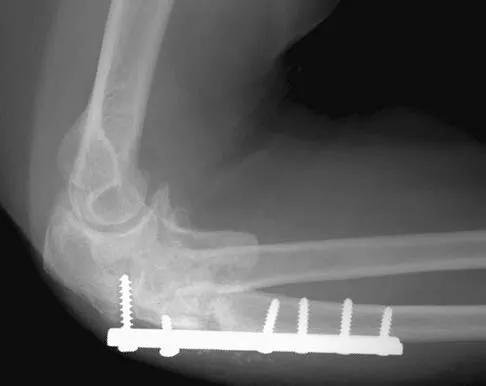
Explanation
Radiographs reveal malunion of a Monteggia fracture-dislocation. Dislocation of the posterior radial head is caused by the malunited ulnar fracture. The deformity includes shortening with an apex posterior angulation. In the acute setting, open reduction of the radial head rarely is necessary; however, in chronic dislocations, open reduction is required. Without ulnar osteotomy, recurrent radial head dislocation is likely.
Question 39
A patient who sustained a cerebrovascular accident (CVA) 18 months ago has a long-standing spastic adduction contracture of the shoulder with a rigid block to passive external rotation. Significant hygiene problems exist with maceration and continued skin breakdown. Management should consist of
Explanation
Following a CVA, the muscular imbalance often leads to a fixed contracture of the shoulder in adduction, internal rotation, and flexion. The responsible muscles include the pectoralis major, subscapularis, teres major, and latissimus dorsi. If stretching cannot produce enough improvement for axillary hygiene, then surgery is an option. If the shoulder resists external rotation during examination with the arm at the side, as in this patient, then the subscapularis is spastic and contributing to the deformity as well and needs to be released along with the pectoralis. Phenol nerve blocks are most effective and best given within 6 months of the initial CVA to be effective. Lidocaine blocks may be helpful in determining whether a deformity is caused by a fixed soft-tissue contracture or by spasticity but play no role once the contracture is present. The modified L'Episcopo procedure is indicated in patients with contracture secondary to brachial plexus birth palsies. Braun RM, Botte MJ: Treatment of shoulder deformity in acquired spasticity. Clin Orthop 1999;368:54-65.
Question 40
What is the most reproducible landmark for the accurate anatomic placement of the tibial tunnel for an anterior cruciate ligament (ACL) reconstruction?
Explanation
The anterior border of the PCL is the most accurate and reproducible landmark for appropriate placement of the tibial tunnel for an ACL reconstruction. The central sagittal insertion point of the ACL is consistently 10 to 11 mm anterior to the anterior border of the PCL ligament. The anterior border of the tibia is not well visualized and does not serve as a reference point. While the posterior border of the anterior horn of the lateral meniscus could be used as a reference point, it has twice the variability of the PCL reference point. The posterior border of the tibia is difficult to identify and has greater variability than the PCL relative to the AP dimension of the proximal tibial surface. The anterior horn of the medial meniscus is also more variable than the PCL. Hutchinson MR, Bae TS: Reproducibility of anatomic tibial landmarks for anterior cruciate ligament reconstructions. Am J Sports Med 2001;29:777-780.
Question 41
Figures 5a and 5b show the clinical photograph and radiograph of a patient who has difficulty wearing shoes and has persistent symptoms medially and laterally at the first and fifth metatarsophalangeal joints. Because shoe modifications have failed to provide relief, management should now consist of
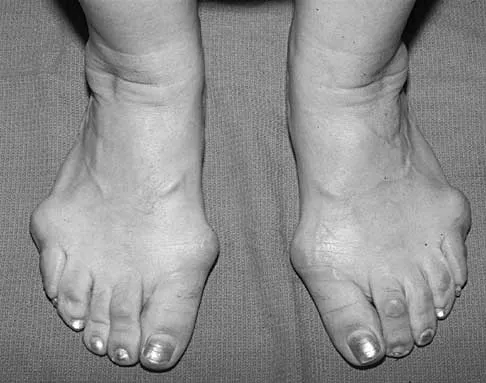
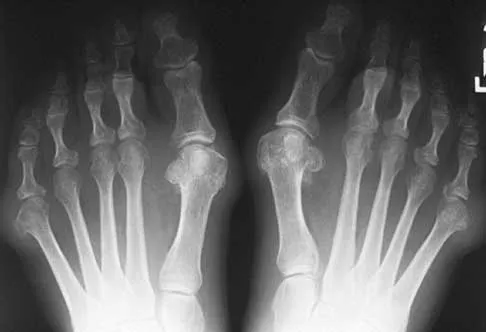
Explanation
A significant bunionette deformity that fails to respond to conservative management is best addressed surgically, in this case with the bunion deformity. The radiograph reveals a prominent lateral condyle at the fifth metatarsal head without a significant increase in the intermetatarsal angle. Simple exostectomy is preferred with less risk of complications. Complete excision would risk transfer lesions to the medial metatarsals. Mann RA, Coughlin MJ: Adult hallux valgus, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, pp 415-435.
Question 42
What procedure can eliminate a sulcus sign?
Explanation
A sulcus sign represents inferior subluxation of the shoulder. The elimination of this sign and correction of the inferior subluxation is best achieved through either an open or arthroscopic rotator interval closure. A SLAP repair stabilizes the biceps anchor but does not affect the sulcus sign. A Bankart repair, which corrects anterior-inferior laxity, is not sufficient to eliminate a sulcus sign. Subacromial decompression and supraspinatus repairs have no effect on inferior subluxation. Field LD, Warren RF, O'Brien SJ, et al: Isolated closure of rotator interval defects for shoulder instability. Am J Sports Med 1995;23:557-563.
Question 43
When an acute infection of a total elbow arthroplasty is managed with irrigation and debridement, which of the following organisms is associated with the highest risk of persistent infection?
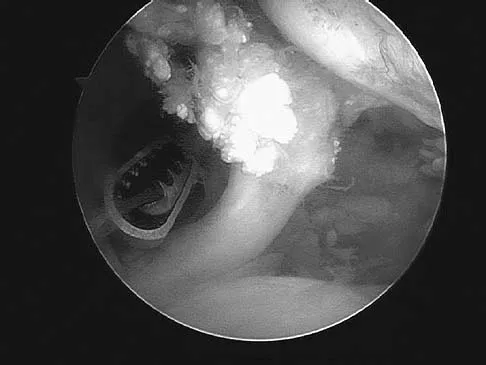
Explanation
Salvage of a total elbow arthroplasty is possible with early aggressive management of acute infection (symptoms for less than 30 days) with serial irrigation and debridement and antibiotic bead placement. This form of treatment is indicated when there are no radiographic or intraoperative signs of loosening. However, successful treatment is largely dependent on the organism. Staphylococcus epidermidis is associated with persistent infection because it is an encapsulating organism, and it is best treated with implant removal and IV antibiotics. Yamaguchi K, Adams RA, Morrey BF: Infection after total elbow arthroplasty. J Bone Joint Surg Am 1998;80:481-491.
Question 44
Which of the following statements describing chordomas is false?
Explanation
Casali and associates provided a recent review of the treatment options for chordomas. These tumors are not radiosensitive; however, modern intensity modulated radiosurgery techniques may be of value. The combination of surgery and radiotherapy compared to surgery alone results in the same disease-free survival time. Complete surgical resection of the chondroma with clean margins offers the best survival; however, its location may make total removal impossible. Thus subtotal resection followed by radiotherapy results in better survival despite the tumor's lack of radiosensitivity.
Question 45
Which of the following is not a reported mode of failure for a constrained acetabular component?
Explanation
There is no evidence of increased polyethylene wear in constrained acetabular components. The rates of wear appear to be the same using standard or constrained liners. Lachiewicz PF, Kelley SS: Constrained components in total hip arthroplasty. J Am Acad Orthop Surg 2002;10:233-238. Anderson MJ, Murray WR, Skinner HB: Constrained acetabular components. J Arthroplasty 1994;9:17-23.
Question 46
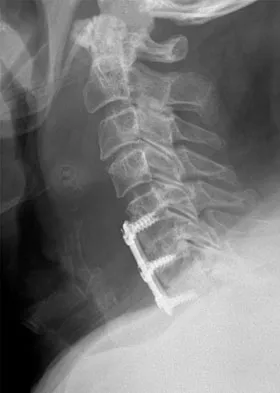
Figure 25 shows the CT scan of an adult patient who has neck pain following a motor vehicle accident. What is the most likely diagnosis?
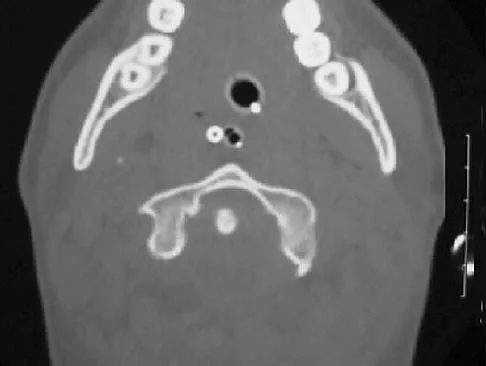
Explanation
If the atlanto-dens interval is greater than 3 mm in an adult, a transverse ligament rupture usually is suspected. The atlanto-dens interval can be seen with CT or in lateral radiographs of the upper cervical spine. Transverse ligament rupture can occur as an isolated entity or in association with an odontoid or a Jefferson's fracture. Patients with this type of injury usually require fusion. Dickman CA, Greene KA, Sonntag VK: Injuries involving the transverse atlantal ligament: Classification and treatment guidelines based upon experience with 39 injuries. Neurosurgery 1996;38:44-50.
Question 47
A 15-year-old boy with epilepsy who is treated with phenytoin sustains a vertebral compression fracture during a breakthrough seizure. Radiographs of the spine reveal generalized osteopenia. What is the most likely cause of the osteopenia?
Explanation
As a side effect of treatment, phenytoin induces osteomalacia, or rickets, in growing children, through interference with metabolism of vitamin D. Oral supplementation of vitamin D can minimize this effect in patients who are undergoing prolonged treatment with phenytoin.
Question 48
A 28-year-old man has a painful nodule on the plantar aspect of his foot in the midarch. Use of a soft orthosis has failed to provide relief. Examination reveals that the mass is approximately 2 1/2 cm in diameter, firm, and tender to palpation. An MRI scan confirms the presence of a plantar fibroma. Management should now consist of
Explanation
Plantar fibromas have an extremely high recurrence rate (approximately 60%) with local excision only. Resection of the entire plantar fascia is effective at irradicating the lesion. There is no role for chemotherapy or amputation with plantar fibromatosis. Radiation therapy may be helpful in combination with resection of the plantar fascia. Kirby EJ, Shereff MJ, Lewis MM: Soft-tissue tumors and tumor-like lesions of the foot: An analysis of 83 cases. J Bone Joint Surg Am 1989;71:621-626.
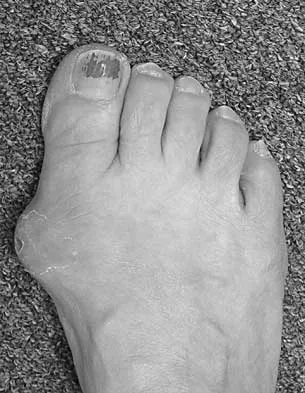
Question 49
A 62-year-old woman with a bone mass density (BMD) T-score of -2.0 sustained a subcapital fracture of her hip. She is an avid tennis player, and history reveals no previous fractures. What is the most appropriate follow-up care?
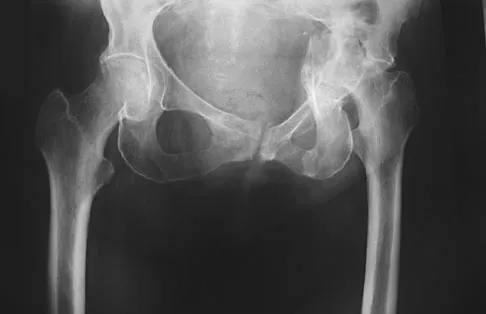
Explanation
A DEXA scan is most appropriately used to establish a baseline score. Even if the bone mineral density is not within the osteoporotic range (T-score less than -2.5), a prior fragility fracture is a strong risk factor for a second fracture as a result of factors other than bone density, such as worsening vision or balance, confusion, or other predispositions to falls. The guidelines of the National Osteoporosis Foundation indicate that, following a fragility hip fracture, active anti-osteoporotic medication should be initiated, whether or not a DEXA scan is performed. A recent study showed that antiresorptive therapy following a hip fracture reduces not only the risk of a second fracture but also overall mortality.
Question 50
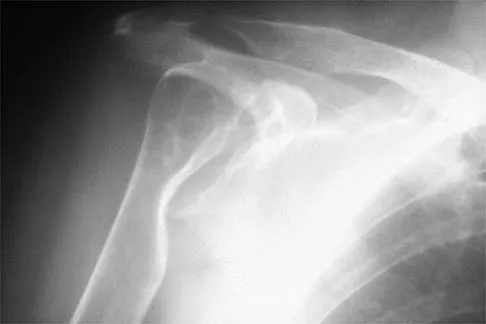
A 79-year-old woman with polyarticular rheumatoid arthritis has had progressively increasing right shoulder pain for the past year, and nonsurgical management has failed to provide relief. Her neurologic examination is entirely normal, but she is unable to elevate her arm against gravity. An AP radiograph is shown in Figure 13. Treatment should consist of
Explanation
Because the patient has end-stage rheumatoid arthritis with glenoid and rotator cuff deficiency, humeral arthroplasty is the treatment of choice. When a patient has an intact rotator cuff and there is sufficient glenoid bone stock to implant a glenoid component, total shoulder arthroplasty is the preferred method because it appears to provide more predictable pain relief. Glenohumeral arthrodesis is generally avoided when there is a functional deltoid or rotator cuff. Open synovectomy is appropriate in early rheumatoid disease before articular changes are present. Anterior acromioplasty with coracoacromial ligament resection is avoided in patients with rheumatoid arthritis because this procedure compromises the coracoacromial arch and may result in anterosuperior instability. Neer CS II, Watson KC, Stanton FJ: Recent experience in total shoulder replacement. J Bone Joint Surg Am 1982;64:319-337. Neer CS II: Glenohumeral arthroplasty, in Neer CS II (ed): Shoulder Reconstruction. Philadelphia, PA, WB Saunders, 1990, pp 143-271. Pollock RG, Deliz ED, McIlveen ST, et al: Prosthetic replacement in rotator cuff deficient shoulders. J Shoulder Elbow Surg 1992;1:173-186.
Question 51
A 27-year-old runner training for his first marathon reports lateral knee pain after an unusually long training run. He states that the most significant pain occurs while running downhill. Examination of the patient while he is laying on the unaffected side reveals increased pain when manual pressure is applied to the lateral femoral epicondylar area during knee range of motion of 30 degrees to 45 degrees. What is the most likely diagnosis?
Explanation
Iliotibial band friction syndrome is one of the most common causes of lateral knee pain in runners. It is caused by increased friction between the iliotibial band and the lateral femoral condyle because of increased tension on the lateral structures. It may be caused by a prominence of the lateral epicondyle or a malalignment of the lower extremity in the runner, including genu varum, tibia vara, heel varus and forefoot supination, or compensating pronation. These structural characteristics can couple with relative muscle imbalance and lead to an altered running gait, enhancing friction between the lateral femoral condyle and the iliotibial band. Management is usually nonsurgical, including stretching of the iliotibial band and strengthening of the hip abductor muscles, with occasional use of cortisone injections or iontophoresis. Noble CA: The treatment of iliotibial band friction syndrome. Br J Sports Med 1979;13:51-54. James SL: Running injuries to the knee. J Am Acad Orthop Surg 1995;3:309-318.
Question 52
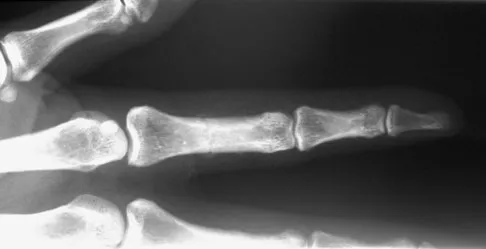
A 25-year-old semiprofessional football player sustains a hyperextension injury to the left foot. He is unable to bear weight. Examination reveals tenderness along the midfoot with swelling and plantar ecchymosis. Radiographs are negative. What is the next step in evaluation of this patient?
Explanation
The patient has a suspected Lisfranc sprain based on the plantar ecchymosis. The first step in diagnosis is a dynamic radiographic study. This should include a physician-assisted midfoot stress examination or standing weight-bearing radiographs to evaluate for displacement. There is no evidence of compartment syndrome, and a bone scan, CT, and MRI are expensive tests that are not warranted. Early JS: Fractures and dislocations of the midfoot and forefoot, in Bucholz R, Heckman JD, Court-Brown CM (eds): Rockwood and Green's Fractures in Adults. Philadelphia, PA, Lippincott Williams and Wilkins, 2006, pp 2337-2400.
Question 53
A patient with a left-sided C6-7 herniated nucleous pulposis would likely have which of the following constellation of findings?
Explanation
A C6-7 herniation affects the C7 root. The C7 root has the middle finger as its predominant sensory distribution. Its motor function is the triceps, wrist extension, and finger metacarpophalangeal extension. The reflex is the triceps. Magee D: Principles and concepts, in Orthopedic Physical Assessment, ed 3. Philadelphia, PA, WB Saunders, 1997, pp 1-18.
Question 54
In the normal adult, the distance between the basion and the tip of the dens with the head in neutral position is how many millimeters?
Explanation
In the normal adult, the distance between the basion and the tip of the dens is 4 mm to 5 mm. Any distance greater than 5 mm is considered abnormal. This is one way to detect occipitocervical dissociation other than using the Power's ratio, which relies on an anterior dislocation. Wiesel SW, Rothman RH: Occipitoatlantal hypermobility. Spine 1979;4:187-191.
Question 55
A study is being designed to compare the effectiveness of an antibiotic. The choice of the number of patients (ie, the sample size) depends on several factors. What type of calculation assesses the potential of the study to successfully address the effectiveness of the antibiotic?
Explanation
Power analysis is used to determine the minimum number of specimens (sample size) such that, if a difference is found that is large enough to be clinically important, the associated level of statistical reliability will be high enough (ie, the P-value will be small enough) for the investigators to conclude that the difference observed in the study also holds in general. For the statistician to do a power analysis, the investigators must first decide on the minimum difference that they consider to be clinically important, for example, a reduction of 3% in the rate of infection. It is important to recognize that the choice of what constitutes the minimum difference in the rate of infection that is clinically (ie, medically) important cannot and should not be done by the statistician. Rather, this is a clinical-medical issue and must be done by the physician researcher based on a comprehensive assessment of the medical risks and benefits. The power analysis also requires an estimate of the variance in the data, which may be based on previous similar studies, if available. A statistician can then calculate the minimum sample size (number of patients) required such that, if a clinically important difference does, in fact, exist between the full populations, there is a reasonable probability or power (typically 80% to 90%) that a difference this large also will occur between the sample populations at the desired level of statistical significance (usually, but not necessarily, P < 0.05). The other answers refer to types of analyses that are usually conducted after the data are collected.
Question 56
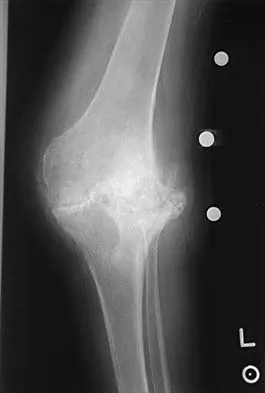
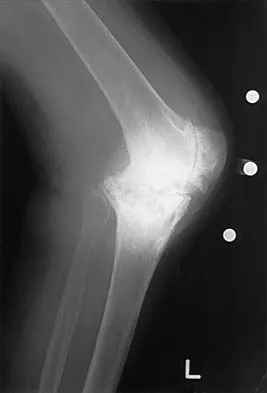
Figures 13a and 13b show the preoperative radiographs of a 60-year-old woman who is scheduled to undergo total knee arthroplasty under epidural anesthesia. Postoperatively she reports a burning sensation on the dorsum of her foot despite the administration of IV analgesics through a patient-controlled analgesia (PCA) pump. Management should now include
Explanation
The patient has a significant flexion contracture and valgus deformity; therefore, the risk of peroneal nerve injury is increased. Idusuyi and Morrey noted that epidural anesthesia also increases the risk of peroneal nerve injury. The initial symptom can be a burning sensation on the foot, followed by pain and then motor weakness. Initial management should consist of release of the dressings and knee flexion. Idusuyi OB, Morrey BF: Peroneal nerve palsy after total knee arthroplasty: Assessment of predisposing and prognostic factors. J Bone Joint Surg Am 1996;78:177-184.
Question 57
Figure 40 shows the plain radiograph of a 30-year-old woman who has had a long history of standing bilateral anterior knee pain and a sense of patellar instability without frank dislocation. Nonsurgical management consisting of anti-inflammatory drugs and physical therapy has failed to provide relief. Examination reveals full range of motion of both knees, with moderate patellofemoral crepitance. Patellar apprehension and patellar grind tests are positive. The Q-angle measures 20 degrees. Management should now consist of
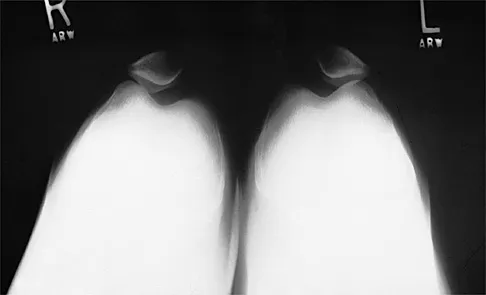
Explanation
The history, physical examination, and radiographs indicate that the patellofemoral pain is most likely caused by excessive lateral patellar pressure and patellar maltracking. Because the radiographs reveal the lateral tilt of the patella and lateral subluxation, the treatment of choice is bilateral lateral releases with anteromedialization of the tibial tubercles. This procedure corrects not only the excessive lateral patellar pressure, but also the lateral subluxation. The use of patella-stabilizing braces or taping may provide temporary relief, but these implements are not well-tolerated and they will not change the underlying biomechanics of the knee. Simple lateral release is indicated for isolated lateral tilt, but it does not correct the lateral subluxation. The use of thermal capsular shrinkage for the medial retinaculum has not been proven to provide long-term correction of the deformity. Boden BP, Pearsall AW, Garrett We Jr, et al: Patellofemoral instability: Evaluation and management. J Am Acad Orthop Surg 1997;5:47-57.
Question 58
A 16-year-old football player sustains a direct blow to the anterior aspect of his flexed right knee. Examination reveals a contusion over the anterior tibial tubercle and a small effusion. MRI scans are shown in Figures 33a through 33c. What is the most likely diagnosis?
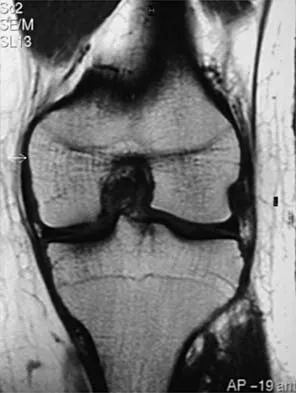
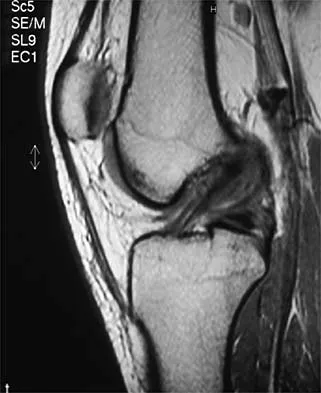
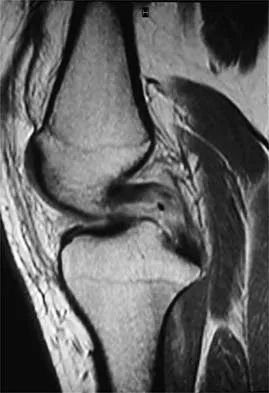
Explanation
The MRI scans show disruption of the fibers of the PCL. Patients sustaining an isolated acute PCL injury can present with only minimal discomfort and have full range of motion. When examination reveals a contusion over the tibial tubercle and discomfort with the posterior drawer examination, with or without instability, a possible injury to the PCL should be considered. In acute injuries, the reported accuracy of MRI imaging for diagnosing PCL tears ranges from 96% to 100%. Resnick D, Kang HS: Internal Derangement of Joints: Emphasis on MRI Imaging. Philadelphia, PA, WB Saunders, 1997, pp 699-700. Harner CD, Hoher J: Evaluation and treatment of posterior cruciate ligament injuries. Am J Sports Med 1998;26:471-482.
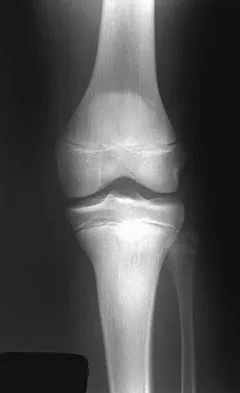
Question 59
Removal of both hallucal sesamoids should be reserved as a salvage procedure because of the high incidence of which of the following postoperative complications?
Explanation
Removal of both sesamoids is associated with a high incidence of postoperative hallux valgus and cock-up deformity of the great toe because of weakening of the flexor hallucis brevis tendon. The sesamoids lie within these tendons and require meticulous repair following excision. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2003, pp 17-25.
Question 60
In the initial evaluation of acute low back pain (duration of less than 4 weeks), plain radiographs are recommended in which of the following situations?
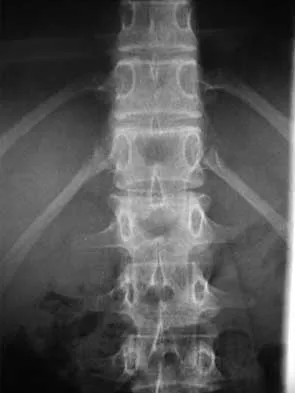
Explanation
Prolonged use of steroids is associated with compression fractures with minimal trauma. Indications for radiography with acute low back pain include possible tumor, fracture, infection, or cauda equina syndrome. Garfin SR, Vaccaro AR (eds): Orthopaedic Knowledge Update: Spine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, Appendix A15.
Question 61
A pediatric orthopaedic surgeon refers a child to a neurologist. The neurologist's office requests the office records of the pediatric orthopaedic surgeon. To maintain Health Insurance Portability and Accountability Act (HIPAA) compliance, what must the surgeon obtain from the parent(s) prior to sending records?
Explanation
The privacy rules do not require an individual's written authorization for certain permitted or required uses and disclosures of the medical records. Patient or parental authorization is not required for disclosures for certain purposes related to treatment, payment, or health care operations. Specifically, HIPAA does not require a covered entity to obtain patient authorization for many of the health care industry's most fundamental activities such as providing care. Carroll R: Risk Management Handbook for Health Care Organizations, ed 4. Hoboken, NJ, Jossey-Bass, 2003, p 1142.
Question 62
A 17-year-old boy who fell on a pitchfork in a barn 1 day ago now has a painful, swollen forearm. Examination reveals erythema, exquisite tenderness, and crepitus to palpation of the forearm. He has a pulse rate of 110/min and a blood pressure of 80/60 mm Hg. Radiographs show subcutaneous air and no fractures. Gram stain of wound drainage reveals a gram-positive bacillus. The next most appropriate step in management should consist of
Explanation
The successful treatment of necrotizing soft-tissue infections such as clostridial myonecrosis depends on prompt recognition and aggressive surgical debridement of all involved muscle, fascia, and soft tissue, resecting to a clearly normal healthy, viable margin. The effective antibiotic regimen for clostridial infection is high-dose penicillin; however, necrotizing infections are frequently polymicrobial so initially broad-spectrum antibiotics are indicated. Hyperbaric oxygen therapy may be used as an adjunct to surgical treatment but is insufficient as a primary therapy. Prolonged application of tourniquets and wound closure should be avoided. Pellegrini VD, Evarts CM: Complications, in Rockwood CA Jr, Green DP (eds): Fractures in Adults, ed 3. Philadelphia, PA, JB Lippincott, 1991, pp 365-370. Gerding DN, Peterson LR: Infections caused by anaerobic bacteria, in Shulman ST, Phair JP, Peterson LR, Warren JR (eds): Infectious Diseases, ed 5. Philadelphia, PA, WB Saunders, 1997, pp 416-417.
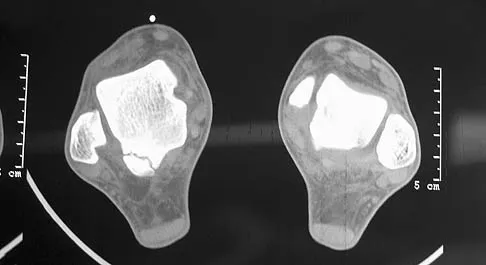
Question 63
In Figure 14, the primary fracture line in a calcaneal fracture is best depicted by which of the following schematics?
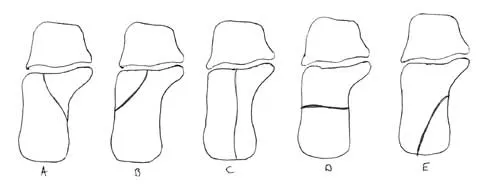
Explanation
The schematic labeled A best depicts the primary fracture line in a calcaneal fracture. The primary fracture line in an axial-loading fracture of the calcaneus occurs from superior-lateral to inferior-medial. This fracture line separates the calcaneus into sustentacular and tuberosity fragments and typically enters the subtalar joint through the posterior facet. Although additional fracture lines typically occur, the primary fracture line is almost always present. If surgical reduction is planned, reducing the primary fracture is always a key step. Macey LR, Benirschke SK, Sangeorzan BJ, Hansen ST: Acute calcaneal fractures: Treatment option and results. J Am Acad Orthop Surg 1994;2:36-43.
Question 64
A 28-year-old man has had a 2-year history of progressive lateral ankle pain. History reveals that he underwent a triple arthrodesis at age 13 for a tarsal coalition. The pain has been refractory to braces, custom inserts, and nonsteroidal anti-inflammatory drugs. Weight-bearing radiographs of the ankle and foot are shown in Figures 3a through 3d. Surgical management should include which of the following?
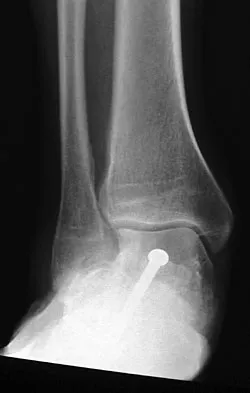
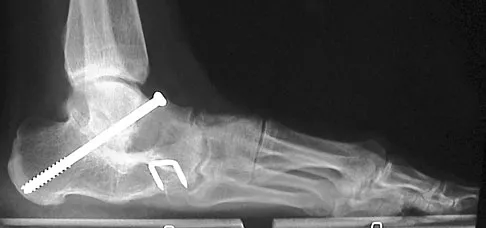
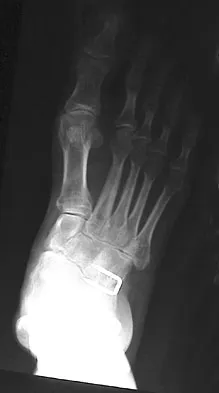
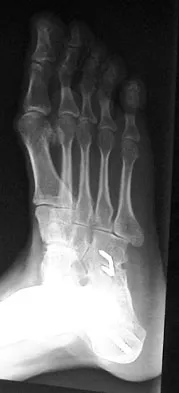
Explanation
The patient has a valgus-supination triple arthrodesis malunion. Weight-bearing radiographs show excessive residual valgus through the subtalar joint, producing lateral subfibular impingement, and residual forefoot abduction and midfoot supination through the talonavicular joint, lateralizing the weight-bearing forces through the foot. The deformity is best managed with a medial displacement calcaneal osteotomy and transverse tarsal derotational osteotomy. Ankle arthroscopy and lateral ligament reconstruction are indicated in the event of ligament instability. Tendon transfer, lateral column lengthening, and heel cord lengthening are used for treatment of adult flatfoot from posterior tibial tendon insufficiency. Ankle arthrodesis and ankle arthroplasty are not indicated in this patient because the lateral ankle symptoms are the result of the underlying deformity in the hindfoot, the patient is young, and the ankle joint is relatively normal. Haddad SL, Myerson MS, Pell RF IV: Clinical and radiographic outcome of revision surgery for failed triple arthrodesis. Foot Ankle Int 1997;18:489-499.
Question 65
Which of the following variables has been shown to have the greatest influence on the higher rate of anterior cruciate ligament (ACL) tears in women when compared to men for similar sports?
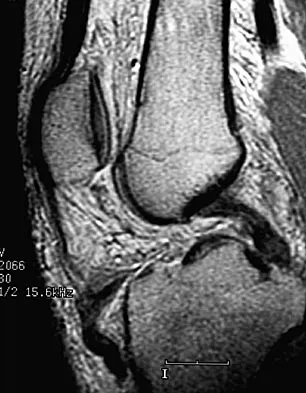
Explanation
All of the variables have been proposed as possible causes for the increased incidence of ACL tears in women versus men. The general differences in the level of neuromuscular training however, specifically conditioning and muscle strength, have been shown to play the greatest role. Harmon KJ, Ireland ML: Gender differences in noncontact anterior cruciate ligament injuries. Clin Sports Med 2000;19:287-302. Arendt EA: Knee injury patterns among men and women in collegiate basketball and soccer. Am J Sports Med 1995;23:694-701.
Question 66
A 25-year-old man injured his dominant shoulder after falling on his outstretched arm 4 months ago. Examination reveals that he cannot lift his arm above 90 degrees, and he has pronounced medial scapular winging. Management should consist of
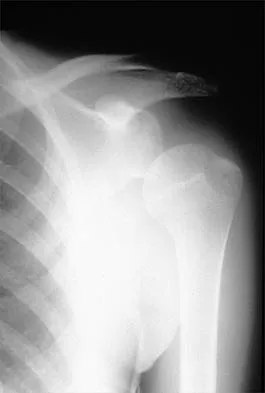
Explanation
Serratus anterior palsy or long thoracic nerve palsy is usually caused by traction injury to the nerve, blunt injury, or iatrogenic injury. The palsy results in winging of the scapula and medial rotation of the inferior pole of the scapula. A patient with this injury will usually recover in 12 to 18 months. Initial treatment should include observation and shoulder strengthening exercises. Nerve exploration with repair has not proven beneficial in changing the outcome. Many orthopaedic surgeons favor using a split pectoralis major transfer for symptomatic patients. Electrodiagnostic studies are helpful in confirming the diagnosis. Post M: Pectoralis major transfer for winging of the scapula. J Shoulder Elbow Surg 1995;4:1-9.
Question 67
A 2-week-old infant has had diminished movement of the right upper extremity since birth. Examination reveals weakness of shoulder abduction and external rotation, elbow flexion, and forearm supination. Both pupils are equally round and responsive to light. The remainder of the examination is normal. Radiographs of the upper limb show a healing middle-third clavicle fracture. Management should consist of
Explanation
The patient has a classic Erb's palsy with weakness of the muscles innervated by the fifth and sixth cervical roots. Horner syndrome, a poor prognostic indicator for recovery, is absent in this infant. All infants with brachial plexus birth palsies initially should be monitored for spontaneous recovery during the first 3 to 6 months of life. During this period of observation, glenohumeral motion, especially external rotation, should be maintained. Many infants will begin to show recovery within the first 6 to 8 weeks after birth and continue on to normal function. The timing of microsurgery is controversial. A recent study found that the outcome of microsurgical repair in patients who had no recovery of biceps function within 3 months after birth was similar compared to those who had recovery of biceps function between 3 and 6 months and no microsurgical repair. The author concluded that microsurgical repair was effective in improving function in those infants who had no evidence of recovery of biceps function within the first 6 months of life. Waters PM: Comparison of the natural history, the outcome of microsurgical repair, and the outcome of operative reconstruction in brachial plexus birth palsy. J Bone Joint Surg Am 1999;81:649-659.
Question 68
Figures 14a and 14b show the clinical photographs of a patient who was stranded in a subzero region for several days. The photographs were taken the morning after arrival in the hospital. The patient is otherwise healthy and fit, and takes no medication. He has no clinical signs of sepsis. He reports burning pain and tingling in both feet. What is the best treatment?
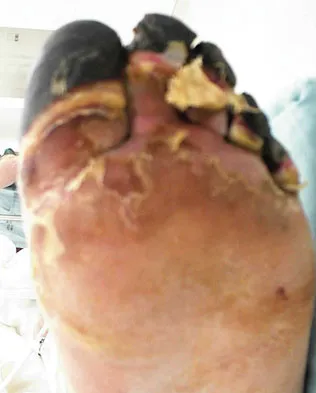
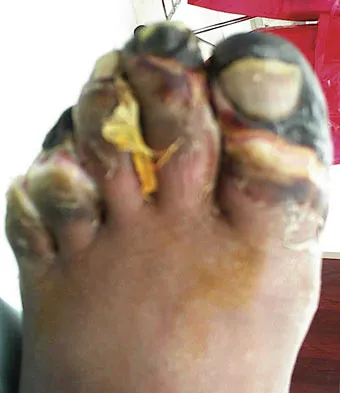
Explanation
The patient has no clinical or observed signs of sepsis. The skin just proximal to the gangrenous tissue appears somewhat hyperemic and is clearly viable. These wounds should be managed much like burn wounds. Moist dressings should be used until the tissue clearly demarcates. Much of the insult may simply be superficial and only require late debridement. McAdams TR, Swenson DR, Miller RA: Frostbite: An orthopedic perspective. Am J Orthop 1999;28:21-26.
Question 69
The diagnosis of an infection after total knee arthroplasty is most reliably proven based on what single study?
Explanation
In a study of 52 patients with infected total knee arthroplasties, Windsor and associates showed that the average leukocyte count was 8,300/mm3 and that aspirated knee fluid was positive in all patients except one. Knee radiographs can be unclear in showing infection, which may be present without radiographic signs of loosening. Technetium Tc 99m and gallium bone scans may not conclusively show the presence of infection, particularly in the first 3 years after knee arthroplasty. Windsor RE, Bono JV: Infected total knee replacements. J Am Acad Orthop Surg 1994;2:44-53.
Question 70
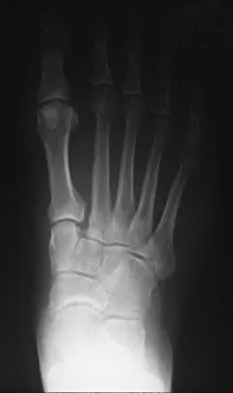
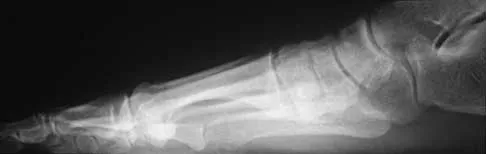
A 42-year-old man has a symptomatic flatfoot deformity and walks with a slight limp after falling off a scaffold 9 months ago. He also reports that he has had difficulty returning to work. Orthotics have failed to provide relief. Current radiographs are shown in Figures 19a and 19b. To relieve his pain and return the patient to work, treatment should consist of
Explanation
Because the patient has sustained a tarsometatarsal injury with midfoot sag, the treatment of choice is a tarsometatarsal arthrodesis. The cause of his flatfoot deformity is secondary to the tarsometatarsal injury and not from posterior tibialis tendon deficiency. Lateral column lengthening, double arthrodesis, and calcaneal osteotomy are not indicated. Although open reduction and internal fixation may be performed late when arthritis is present, these procedures are less likely to succeed. Komenda GA, Myerson MS, Biddinger KR: Results of arthrodesis of the tarsometatarsal joints after traumatic injury. J Bone Joint Surg Am 1996;78:1665-1676.
Question 71
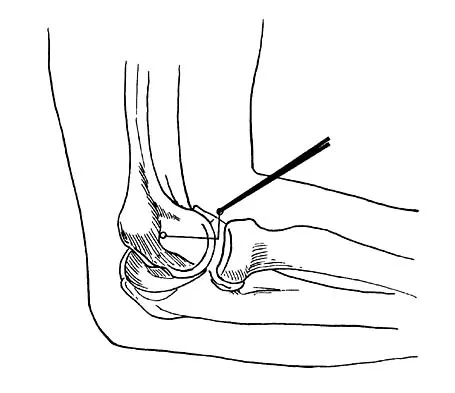
What nerve is at greatest risk of harm from the portal shown in Figure 36?
Explanation
The figure shows the anterolateral portal for elbow arthroscopy, and injury to the radial nerve has been reported in conjunction with this portal site. Studies have shown that closer proximity to the radial nerve is associated with more distal portal sites. The lateral and posterior antebrachial cutaneous nerves are both at less risk of injury. The ulnar and median nerves are both fairly remote to this location. Field LD, Altchek DW, Warren RF, O'Brien SJ, Skyhar MJ, Wickiewicz TL: Arthroscopic anatomy of the lateral elbow: A comparison of three portals. Arthroscopy 1994;10:602-607. Papilion JD, Neff RS, Shall LM: Compression neuropathy of the radial nerve as a complication of elbow arthroscopy: A case report and review of the literature. Arthroscopy 1988;4:284-286.
Question 72
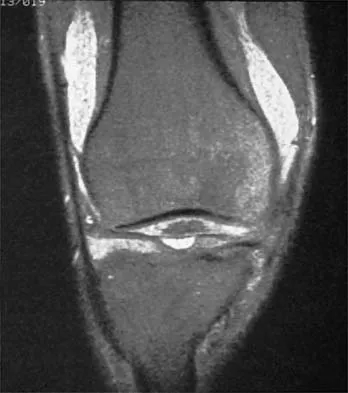
A 30-year-old man who participates in recreational sports reports the spontaneous onset of intermittent pain and swelling about the right knee. Examination reveals a 3+ effusion, with a range of motion of 10 degrees to 60 degrees. He has mild diffuse tenderness but no instability. MRI scans and an arthroscopic view are shown in Figures 39a through 39c. Management should consist of
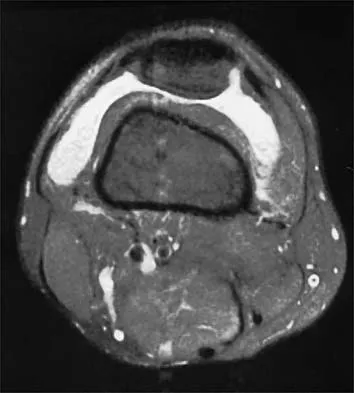
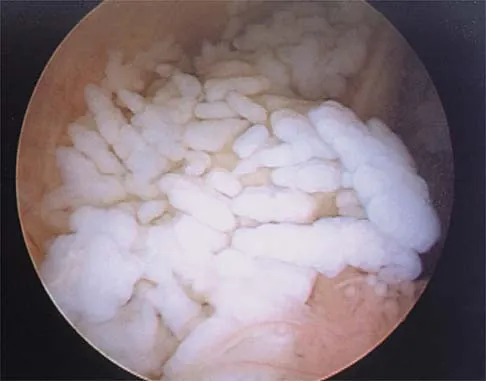
Explanation
The patient has synovial chondromatosis. The MRI scans show multiple small proscribed areas of signal intensity in the gutters and suprapatellar pouch, suggesting very small loose bodies. The arthroscopic view shows the classic appearance of multiple small chondral loose bodies. Synovial chondromatosis is a condition in which the synovium undergoes metaplasia, producing multiple chondral loose bodies that can subsequently ossify. The treatment of choice, removal of the loose bodies and arthroscopic synovectomy, results in a lower incidence of recurrence than other treatment methods. Coolican MR, Dandy DJ: Arthroscopic management of synovial chondromatosis of the knee: findings and results in 18 cases. J Bone Joint Surg Br 1989;71:498-500.
Question 73
What ligament is the primary stabilizer of the wrist following a proximal row carpectomy?
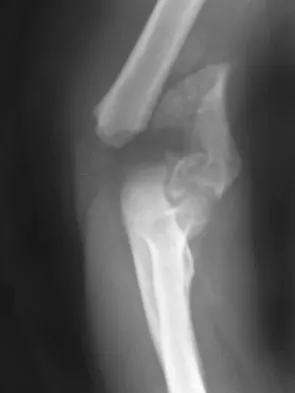
Explanation
The radioscaphocapitate ligament is the prime stabilizer between the radius and capitate, preventing ulnar translocation of the carpus. Its oblique orientation prevents the carpus from drifting ulnarly. This stout ligament must be protected when excising the scaphoid. Stern PJ, Agabegi SS, Kiefhaber TR, et al: Proximal row carpectomy. J Bone Joint Surg Am 2005;87:166-174.
Question 74
A 25-year-old man is brought to the emergency department following a motor vehicle accident. Extrication time was 2 hours, and in the field he had a systolic blood pressure by palpation of 90 mm Hg. Intravenous therapy was started, and on arrival in the emergency department he has a systolic blood pressure of 90 mm Hg with a pulse rate of 130. Examination reveals a flail chest and a femoral diaphyseal fracture. Ultrasound of the abdomen is positive. The trauma surgeons take him to the operating room for an exploratory laparotomy. At the conclusion of the procedure, he has a systolic pressure of 100 mm Hg with a pulse rate of 110. Oxygen saturation is 90% on 100% oxygen, and he has a temperature of 95.0 degrees F (35 degrees C). What is the recommended treatment of the femoral fracture at this time?
Explanation
This is a "borderline trauma" patient where serious consideration for damage control orthopaedic surgery is required. His prolonged hypotension, abdominal injury, and chest injury put him at higher risk for serious postinjury complications. Further surgery, such as definitive fracture fixation, adds metabolic load and injury to his system. It is prudent to consider femoral fracture stabilization with an external fixator until he is physiologically recovered as evidenced by a normal base excess and/or lactate acid levels, as well as all other parameters of resuscitation. A borderline patient has been described as polytrauma with an ISS > 20 and thoracic trauma (AIS > 2); polytrauma and abdominal/pelvic trauma (Moore > 3) and hemodynamic shock (initial BP < 90 mm Hg); ISS > 40; bilateral lung contusions on radiographs; initial mean pulmonary arterial pressure > 24 mm Hg; pulmonary artery pressure increase during intramedullary nailing > 6 mm Hg. Factors that worsen the situation following surgery include multiple long bones and truncal injury (AIS > 2), estimated surgery time of more than 6 hours, arterial injury and hemodynamic instability, and exaggerated inflammatory response (eg, Il-6 > 800 pg/mL). It is incumbent on the orthopaedic surgeon who is a member of the trauma team to make sure that he or she is aware of these factors and guides the team to the best patient care. Pape HC, Hildebrand F, Pertschy S, et al: Changes in the management of femoral shaft fractures in polytrauma patients: From early total care to damage control orthopaedic surgery. J Trauma 2002;53:452-461.
Question 75
A 23-year-old woman has had vague left knee pain for the past 6 months. A radiograph and CT scan are shown in Figures 50a and 50b. What is the most likely diagnosis?
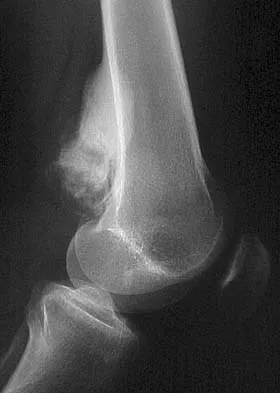
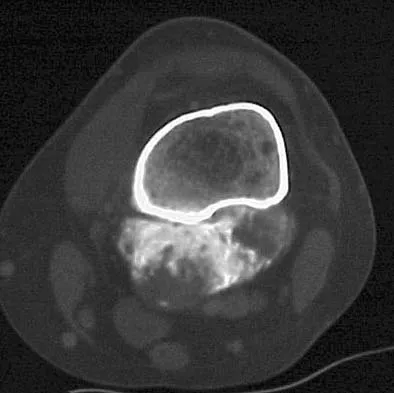
Explanation
The radiographic appearance of the lesion emanating from the posterior cortex of the left distal femur is consistent with a surface bone-producing lesion; therefore, the most likely diagnosis is a parosteal osteosarcoma. In an osteochondroma, the cortex and medullary cavity of the lesion are in continuity with that of the native bone. A dedifferentiated chondrosarcoma has histologic components of a high-grade sarcoma plus a benign or low-grade malignant cartilage tumor. Tumoral calcinosis is characterized by amorphous calcium in the soft tissues and does not emanate from the bone itself. While often confused with parosteal osteosarcoma, myositis ossificans is usually more mature at the periphery of the lesion rather than the center. In addition, myositis ossificans does not involve the underlying cortex but remains separate from the bone. Unni KK: Dahlin's Bone Tumors: General Aspects and Data on 11,087 Cases, ed 5. Philadelphia, PA, Lippincott-Raven, 1996, pp 185-196.
Question 76
Figure 3 shows the clinical photograph of a wrestler who has an acute mass in his ear. He does not wear protective headgear. The area is mildly tender and without erythema. Management should consist of
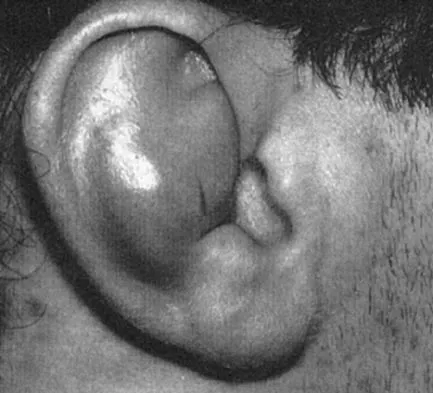
Explanation
The patient has an auricular hematoma. This injury is typically related to blunt trauma, occuring in wrestlers who do not use protective headgear. The goal of treatment is to remove the fluid, reapproximate the perichondrium to the underlying articular cartilage, and limit reaccumulation of the fluid in attempt to prevent cartilage necrosis. Aspiration and application of a compressive dressing offers the best chance to achieve this goal. There are no signs of infection such as marked tenderness, erythema, or surrounding edema to justify antibiotic use or irrigation and debridement. The mass does not warrant excision. Kaufman BR, Heckler FR: Sports-related facial injuries. Clin Sports Med 1997;16:543-562.
Question 77
Retrograde ejaculation is most commonly associated with what surgical approach?
Explanation
Retrograde ejaculation is the sequela of an injury to the superior hypogastric plexus. This structure needs protection, especially during anterior exposure of the lumbosacral junction. Although the superior hypogastric plexus can be injured with anterior or anterolateral spine surgery at any lumbar level, it is most at risk with anterior transperitoneal approaches to the lumbosacral junction. To avoid this complication, the use of monopolar electrocautery should be avoided during deep dissection in this region. The ideal anterior exposure starts with blunt dissection just to the medial aspect of the left common iliac vein sweeping the prevertebral tissues toward the patient's right side. Flynn JC, Price CT: Sexual complications of anterior fusion of the lumbar spine. Spine 1984;9:489-492. Watkins RG (ed): Surgical Approaches to the Spine. New York, NY, Springer-Verlag, 1983, p 107.
Question 78
A 9-year-old child sustains a proximal tibial physeal fracture with a hyperextension mechanism. What structure is at most risk for serious injury?
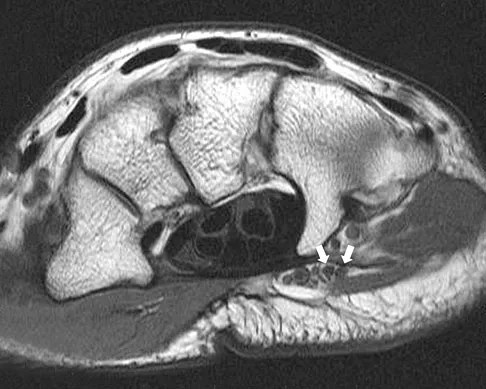
Explanation
The most serious injury associated with proximal tibial physeal fracture is vascular trauma. The popliteal artery is tethered by its major branches near the posterior surface of the proximal tibial epiphysis. During tibial physeal displacement, the popliteal artery is susceptible to injury. Injuries to the other structures are less common.
Question 79
A 65-year-old woman with a history of diabetes mellitus and plantar ulcers has an erythematous and swollen right foot and ankle. Despite IV antibiotics, the erythema spreads to her lower calf within 24 hours. She has a systolic blood pressure of 80/55 mm Hg and a pulse rate of 120. Laboratory studies show a creatinine level of 1.5 mg. Initial management should consist of
Explanation
Necrotizing fasciitis is an aggressive and rapidly spreading soft-tissue infection, usually caused by group A beta-hemolytic Streptococcus pyogenes. Presentation is typical of a rapidly ascending cellulitis, recalcitrant to antibiotic treatment. Differentiation between cellulitis and impetigo is difficult, and success depends on a high level of suspicion. The skin and subcutaneous tissues are affected, with sparing of the muscles. Septic shock and multi-organ system failure can be fatal. Treatment is aggressive surgical debridement with broad-spectrum antibiotics. Repeat irrigation and debridement may be necessary. Hyperbaric oxygen studies have shown inconsistent results. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2003, pp 199-205.
Question 80
An 11-year-old boy sustained an ankle injury while playing football. Figure 20 shows an AP radiograph obtained the day of injury. Treatment should consist of
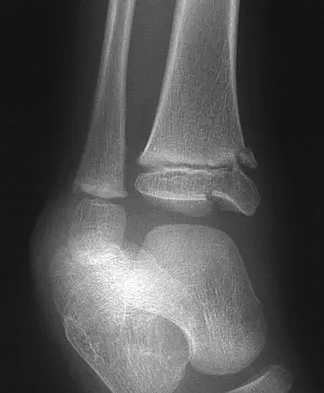
Explanation
The child has an injury involving both the growth plate and the articular surface of the ankle. Because of the significant displacement, open reduction and internal fixation is indicated to realign the physis and joint surface. The best method of fixation to avoid growth arrest is one that does not cross the physis. This is usually achieved by a transverse epiphyseal screw parallel to the physis. If the metaphyseal fragment was large enough, a transverse metaphyseal screw could be used instead. The incidence of growth arrest following physeal ankle injuries is as high as 50%, and long-term follow-up is indicated. Cass JR, Peterson HA: Salter-Harris Type-IV injuries of the distal tibial epiphyseal growth plate, with emphasis on those involving the medial malleolus. J Bone Joint Surg Am 1983;65:1059-1070.
Question 81
Free flap coverage for severe trauma to the upper extremity has the fewest complications when performed within what time period after injury?
Explanation
Flap necrosis and infection rates are lowest if free flap coverage is performed within 72 hours of injury. Delays beyond 72 hours are associated with a higher rate of complications. Godina M: Early microsurgical reconstruction of complex trauma of the extremities. Plast Reconstr Surg 1986;78:285-292.
Question 82
What is the most common primary malignant tumor of bone in childhood?
Explanation
Osteosarcoma is the most common primary malignant tumor of bone in childhood, followed by Ewing's sarcoma. Rhabdomyosarcoma is a soft-tissue sarcoma of childhood. Chondrosarcoma rarely occurs in childhood. Osteochondromas are benign tumors of the bone. Simon M, Springfield D, et al: Osteogenic Sarcoma: Surgery for Bone and Soft Tissue Tumors. Philadelphia, PA, Lippincott Raven, 1998, p 226.
Question 83
Which of the following anatomic structures is often difficult to visualize during elbow arthroscopy?
Explanation
The ulnar collateral ligament is often difficult to visualize during elbow arthroscopy. It can be seen clearly in only 10% to 30% of elbow arthroscopies. All of the other structures should be easily and thoroughly seen and palpated during elbow arthroscopy. Johnson LL: Arthroscopic Surgery: Principles and Practice. St Louis, MO, CV Mosby, 1988.
Question 84
A 15-year-old boy reports leg pain after being tackled during football practice. Radiographs and a CT scan are shown in Figures 46a through 46c. The patient has a pathologic fracture through what underlying lesion?
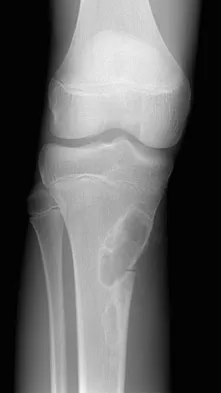
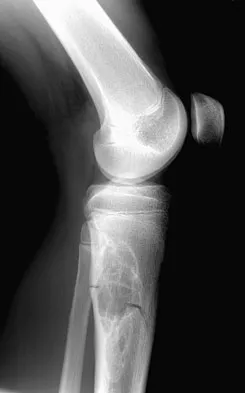
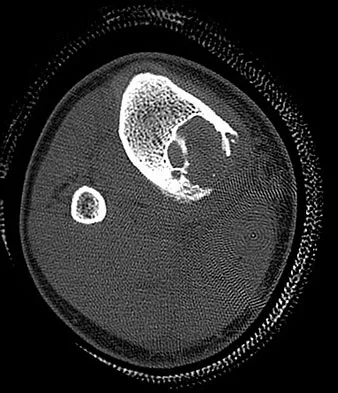
Explanation
The images show a lobulated, eccentric, well-marginated lesion that is typical of a nonossifying fibroma. The lesion is slightly expansile, and the CT scan findings show that the lesion is very well marginated and the cortex is disrupted, which is a common finding. None of the characteristics of this lesion is aggressive in nature. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 69-75.
Question 85
A 16-year-old boy sustains a twisting injury to the left knee while wrestling. MRI scans are shown in Figures 22a through 22c. What is the most likely diagnosis?
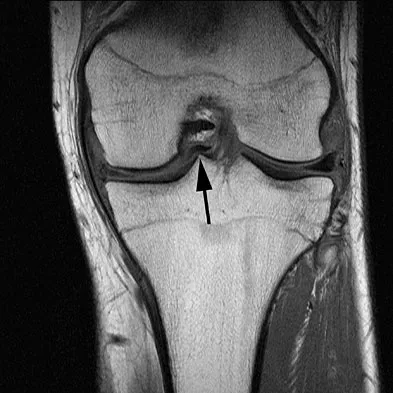
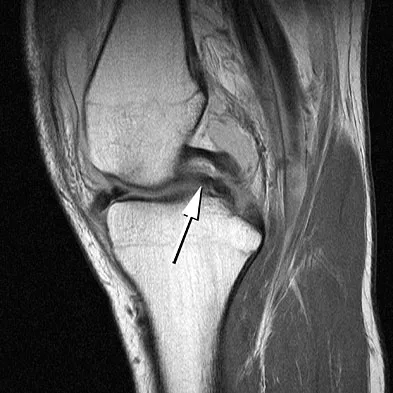
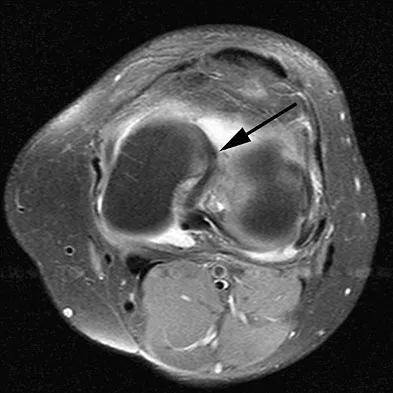
Explanation
The MRI scans show a displaced bucket-handle medial meniscus tear that can be visualized on coronal, sagittal, and axial views. The sagittal view shows the typical "double posterior cruciate ligament sign," in which the low-signal bucket-handle fragment parallels the normal low-signal posterior cruciate ligament. The coronal and axial images both show the displaced medial meniscus in the notch. Sanders TG, Miller MD: A systematic approach to magnetic resonance imaging interpretation of sports medicine injuries of the knee. Am J Sports Med 2005;33:131-148.
Question 86
Which of the following assessment tools most accurately reflects outcomes of well-being, daily function, and general health in a patient treated for cervical myelopathy?
Explanation
The short-form 36 is an excellent tool for measuring the patient's perception of treatment outcome because it is a patient-generated, validated assessment of physical, social, and role function, emotional and mental health, energy/fatigue, pain, health perception, and health change. The Nurick criteria is an evaluation of physical function with gradations of ambulation and daily function. The Japanese Orthopaedic Association score gives points for function in activities of daily living but does not assess perception of general health. The neck disability index assesses the impact of neck pain on daily life, and the Odom criteria are the surgeon's evaluations of degree of radicular pain and deficit. Albert TJ, Mesa JJ, Eng K, McIntosh TC, Balderston RA: Health outcome assessment before and after lumbar laminectomy for radiculopathy. Spine 1996;21:960-963. Swiontkowski MF, Buckwalter JA, Keller RB, Haralson R: The outcomes movement in orthopaedic surgery: Where we are and where we should go. J Bone Joint Surgery Am 1999;81:732-740.
Question 87
A 21-year-old football player who sustained a direct blow to the posterior hindfoot while making a cut is unable to bear weight on the injured foot. Examination reveals tenderness and swelling of the great toe metatarsophalangeal (MTP) joint. Radiographs are shown in Figures 9a and 9b. What is the most likely diagnosis?
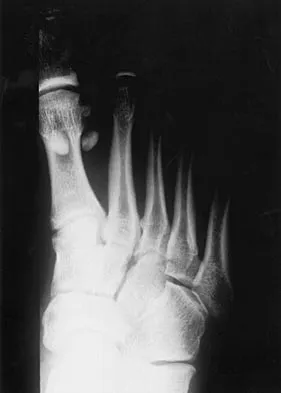
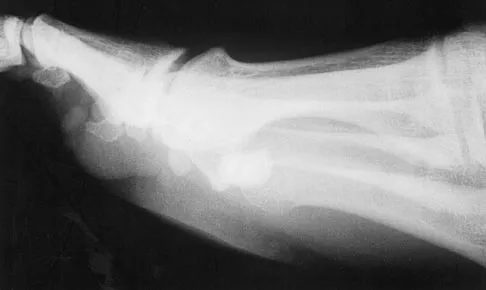
Explanation
Turf toe occurs in collision and contact sports in which the athlete pushes off to accelerate or change direction and there is hyperextension of the great toe MTP joint. Typically, there is also axial loading of the posterior hindfoot, which increases the hyperextension of the MTP joint. The most common presentation is pain and swelling of the MTP joint and inability to hyperextend the joint without significant symptoms. With significant force, fractures of the sesmoids and plantar soft tissues can occur. The radiographs do not show a dislocation of the great toe MTP joint because it is concentrically located on both radiographs. However, the radiographs show a fracture of the lateral sesamoid or a diastasis of a bipartite lateral sesamoid. The medial sesamoid is also proximal indicating a rupture of the plantar (volar) plate. Therefore, the most likely diagnosis is a fracture of the lateral sesamoid with rupture of the plantar plate leading to proximal migration of the proximal fragment of the lateral sesamoid and the medial sesamoid. Rodeo SA, et al: Diastasis of bipartite sesamoids of the first metatarsophalangeal joint. Foot Ankle 1993;l4:425-434.
Question 88
An 83-year-old woman with diabetes mellitus has a history of recurrent infection over the medial aspect of her great toe and has had a painless bunion for the past 45 years. Shoe wear modifications have failed to provide relief. Pedal pulses are palpable. Figures 30a and 30b show the clinical photograph and radiograph. Management should now consist of
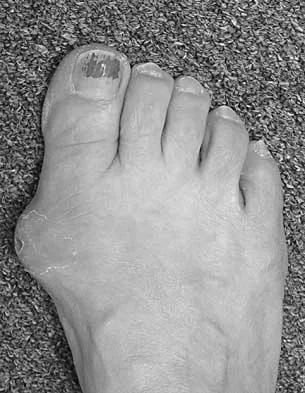
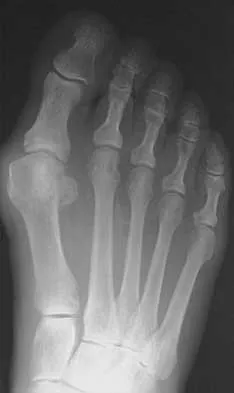
Explanation
The presence of recurrent breakdown over the medial eminence despite shoe wear modifications is an indication for surgery. A number of factors must be considered when deciding on an appropriate course of treatment. These include age, activity level, joint congruency, joint degeneration, and the patient's symptoms and expectations. The indications for a simple bunionectomy are rather limited. In this patient, the goal of surgery is to alleviate the recurrent infection by removal of a large medial eminence. Because the bunion is painless and long-standing, it does not warrant treatment. Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 123-134.
Question 89
A 20-year-old collegiate football player sustains an injury to his left foot 3 weeks before the start of the fall season. Examination reveals localized tenderness over the lateral midfoot and normal foot alignment. Radiographs are shown in Figures 28a through 28c. What is the treatment of choice?
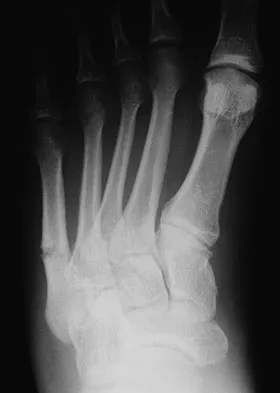
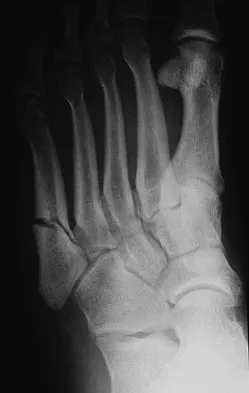
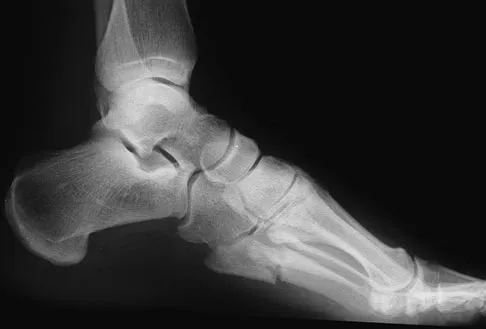
Explanation
Due to the relatively high incidence of delayed union and nonunion associated with this mildly displaced Jones-type fracture, and the temporal proximity to his playing season, intramedullary screw fixation is the treatment of choice in this collegiate athlete to best ensure healing and expedite his return to football. If nonsurgical management were elected, application of a non-weight-bearing short leg cast would be appropriate since a higher likelihood of healing is expected with it versus a short leg walking cast. The risk of recurrent fracture of fractures that heal with nonsurgical management has reportedly been high (approximately 30%). Quill GE: Fractures of the proximal fifth metatarsal. Orthop Clin North Am 1995;26:353-361. Torg JS, Balduini FC, Zelko RR, et al: Fractures of the base of the fifth metatarsal distal to the tuberosity: Classification and guidelines for nonsurgical and surgical management. J Bone Joint Surg Am 1984;66:209-214.
Question 90
Figures 41a and 41b show the radiographs of a 22-year-old woman who has a bunion on her left foot. She denies pain in the foot, but she reports increasing difficulty with shoe wear. Management should consist of
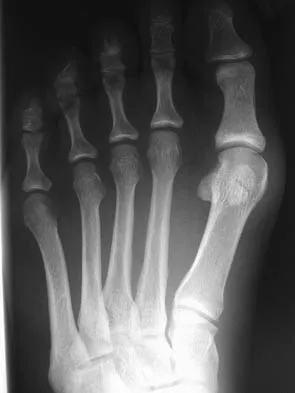
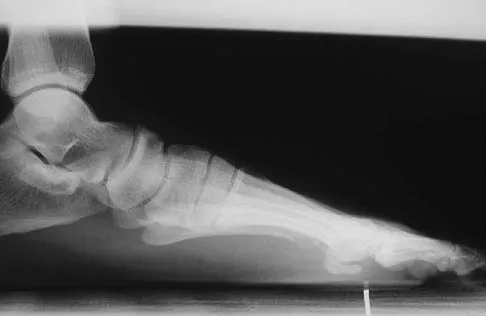
Explanation
Surgery is not indicated in a patient who has a mild deformity and no pain. Shoe wear modifications should be recommended.
Question 91
Which of the following palpable bony landmarks is correctly matched with its corresponding vertebral level?
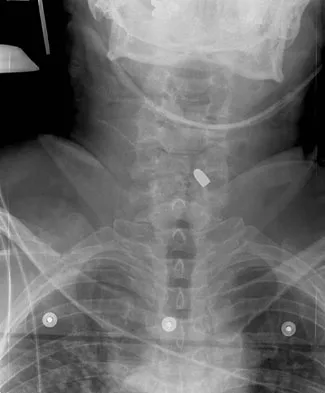
Explanation
The carotid tubercle is usually located at the level of C6. The angle of the mandible is at C1-C2; the hyoid is at C4; the superior portion of the thyroid cartilage is C4-C5; and the cricoid cartilage is at C6. Smith GW, Robinson RA: The treatment of certain cervical-spine disorders by anterior removal of the intervertebral disc and interbody fusion. J Bone Joint Surg Am 1958;40:607.
Question 92
Which of the following pharmacologic agents is most likely to adversely affect the success rate of bony union after lumbar arthrodesis?
Explanation
Glassman and associates reported a significantly higher pseudarthrosis rate when ketorolac was used postoperatively compared to a similar group of patients who were not given ketorolac. Animal studies from the same institution support these clinical findings. To reduce narcotic dosage, nonsteroidal anti-inflammatory drugs (NSAIDs) have been promoted as an adjunct for postoperative analgesia in patients undergoing spinal fusion. However, a high failure rate of arthrodesis has been associated with postoperative use of NSAIDs. The analgesics oxycodone hydrochloride, hydrocodone/acetaminophen, and tramadol, as well as the tricyclic antidepressant imipramine, have not been shown to inhibit fusion. Glassman SD, Rose SM, Dimar JR, et al: The effect of postoperative nonsteroidal anti-inflammatory drug administration on spinal fusion. Spine 1998;23:834-838.
Question 93
An 8-month-old infant has an infection of the fingertip as shown in Figure 22. If neglected, the anticipated path of ascending infection is the fingertip, the flexor sheath, and the
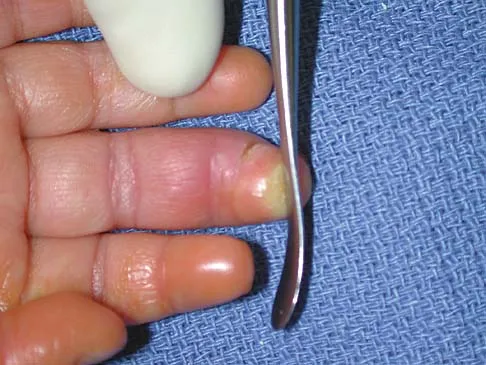
Explanation
The flexor sheaths are in continuity with the deep spaces of the hand. The flexor sheaths of the thumb and little finger communicate with the radial and ulnar bursae, respectively, and these two bursae commonly communicate. The central digits do not communicate as readily with deep spaces of the hand but if flexor tendon sheath infection of the index, long, and right fingers is neglected, the potential exists for rupture into the deep midpalmar spaces. Peimer CA (ed): Surgery of the Hand and Upper Extremity: Acute and Chronic Sepsis. New York, NY, Mcgraw Hill, 1996, pp 1735-1741.
Question 94
A 35-year-old recreational basketball player reports shoulder pain following a sprawl for a rebound. While examination reveals that he can actively elevate the arm with pain, a subacromial injection fails to provide relief. An MRI scan reveals medial subluxation of the long head of the biceps. Which of the following structures most likely has also been injured?
Explanation
Subscapularis tears can be associated with disruption of the transverse ligament supporting the biceps. The remaining aspects of the rotator cuff, superior labrum, and capsule can be intact with this injury. Petersson CJ: Spontaneous medial dislocation of the tendon of the long biceps brachii. Clin Orthop 1986;211:224-227.
Question 95
A 21-year-old woman sustained a minimally displaced traumatic spondylolisthesis of C2 (Hangman's fracture) after striking the windshield with her forehead during a motor vehicle accident. Management should consist of

Explanation
According to the classification of Levine and Edwards, a type I Hangman's fracture is minimally displaced without angulation and represents a stable injury. Good clinical success has been achieved with nonsurgical management consisting of use of a rigid collar until the patient reports pain relief, followed by quick mobilization.
Question 96
An 18-year-old boy has had pain in the right knee for the past 6 months. Examination reveals some fullness behind the knee but no significant palpable soft-tissue mass. There is no effusion, and he has full knee range of motion. The remainder of the examination is unremarkable. A radiograph and MRI scans are shown in Figures 33a through 33c, and biopsy specimens are shown in Figures 33d and 33e. What is the most likely diagnosis?
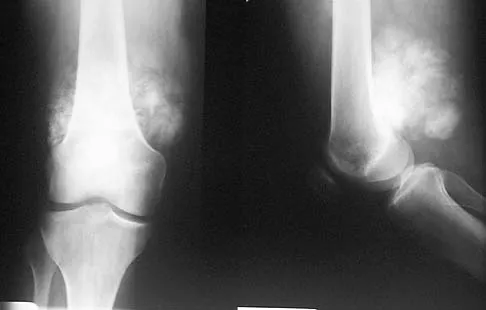
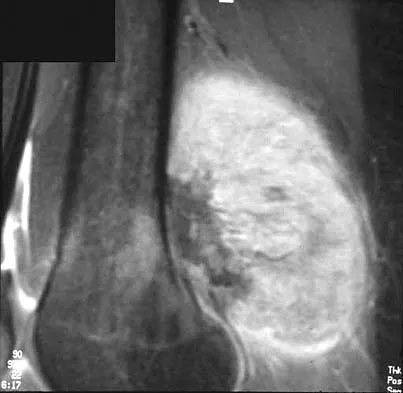
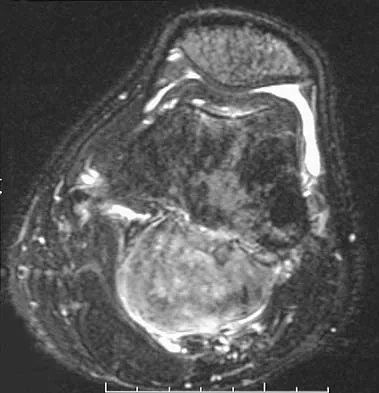
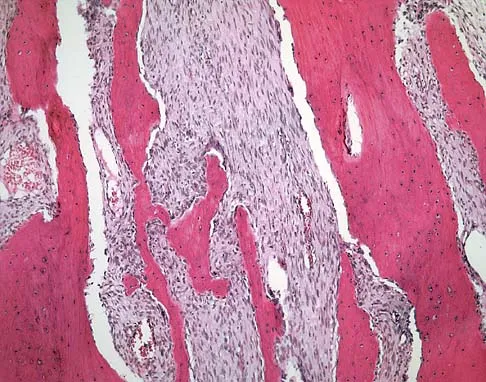
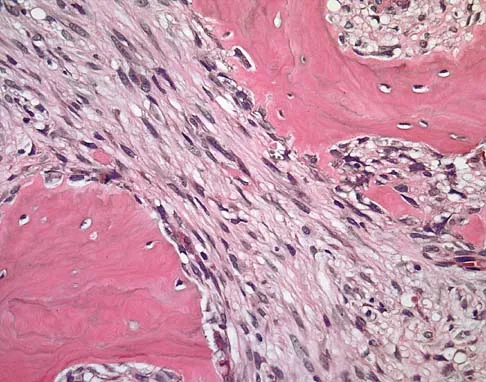
Explanation
The patient has parosteal osteosarcoma. The posterior aspect of the distal femur is the typical location for this variant of osteogenic sarcoma. The imaging studies indicate a surface lesion with no involvement of the adjacent intramedullary canal. The histologic appearance is that of a low-grade fibroblastic osteosarcoma, consisting of relatively mature bone and a bland fibroblastic stroma lacking cytologic atypia and mitotic activity. A cartilaginous component is also frequently seen. Classic osteosarcoma typically has a more aggressive radiologic and histologic appearance. Sessile osteochondromas, while common behind the knee, have a presence of hematopoietic marrow and fat. The cartilage found in the associated cartilaginous cap is oriented. Chondrosarcomas are more typical in an older age group and have a histologic pattern consisting of malignant chondroid. Wold LA, et al: Atlas of Orthopaedic Pathology. Philadelphia, PA, WB Saunders, 1990, pp 20-21.
Question 97
Figures 45a and 45b show the radiographs of a 14-year-old boy who sustained a distal radius fracture while playing hockey. After 1 year the patient is asymptomatic. Follow-up and comparison radiographs and an MRI scan are shown in Figures 45c and 45d. What is the next most appropriate step in management?
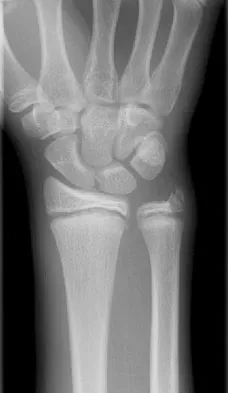
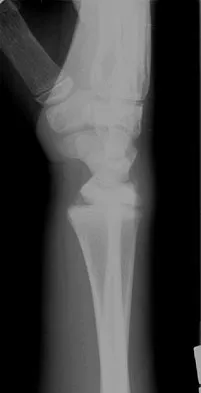
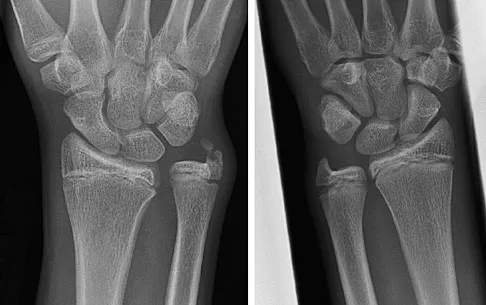
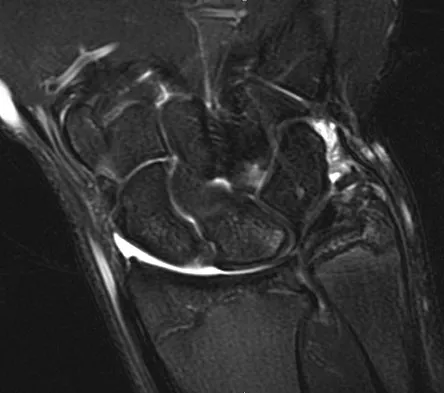
Explanation
The patient sustained a growth plate fracture of the distal radius and ulna. Although treated with closed reduction and casting, the follow-up radiographs demonstrate shortening of the radius in comparison to the ulna, and the MRI scan confirms thinning of the distal radius growth plate and bony bars consistent with a growth arrest. At this time, the discrepancy in length is too minor to consider lengthening of the radius; in addition, excision of a physeal bar with minimal growth potential is not likely to restore the gross discrepancy. Ulnar styloid fractures are rarely symptomatic and do not require treatment in the asymptomatic patient. Closure of the distal ulna growth plate will prevent further discrepancy between the radius and ulna. Vanheest A: Wrist deformities after fracture. Hand Clin 2006;22:113-120.
Question 98
The arrow in Figure 11 points toward a finding consistent with which of the following?
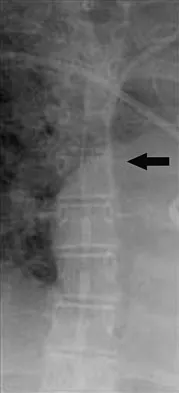
Explanation
The finding of a unilateral absent pedicle is often referred to as a winking owl sign and is a manifestation of pedicle destruction from metastatic disease. As the vertebral body is destroyed from the neoplastic process, it extends into the pedicle and destroys the cortical rim that normally creates the oval ring of the pedicle on an AP image. McLain R, Weinstein J (eds): Rothman-Simeone: The Spine, ed 4. Philadelphia, PA, WB Saunders, 1999, p 1173.
Question 99
A previously asymptomatic 14-year-old girl sustained a twisting injury to her ankle. Radiographs are shown in Figures 2a and 2b. Management should consist of
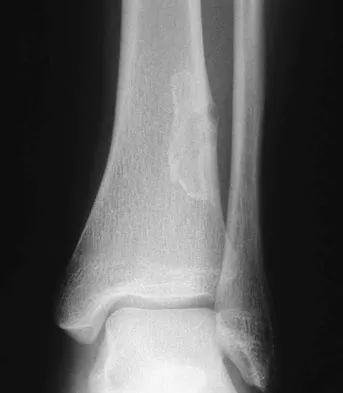
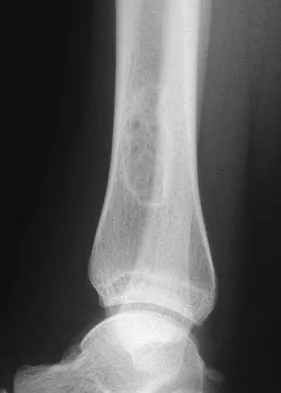
Explanation
The radiographs show a well-defined, irregular, eccentric lesion in the distal tibia metaphysis with a thin sclerotic margin. The radiographs are diagnostic of nonossifying fibroma, a common entity in this age group and in this location. No further work-up is indicated. The patient was asymptomatic prior to the injury and the lesion is small and thus not worrisome for an impending pathologic fracture; therefore, no treatment is indicated beyond observation. The natural history of these lesions is to gradually ossify as the patient reaches skeletal maturity. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 69-75.
Question 100
A 16-year-old girl sustained the injury shown in Figure 7a. CT scans are shown in Figures 7b through 7d. The results of treatment of this injury have been shown to most correlate with which of the following factors?
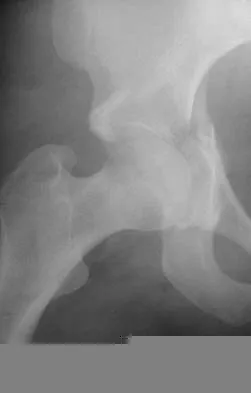
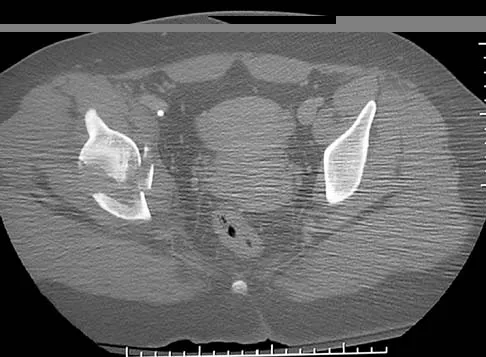
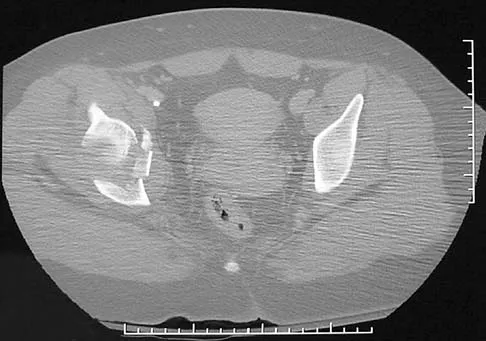
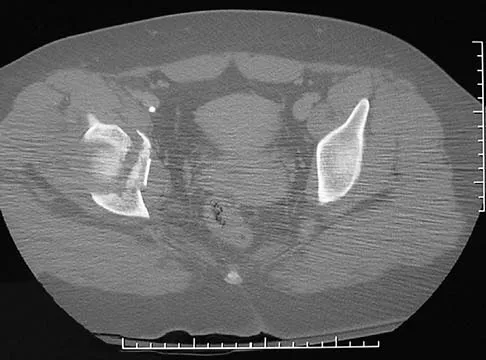
Explanation
The patient has a very low T-type acetabular fracture; however, the head is not congruent under the dome so surgical reduction is necessary. The anterior and posterior columns are displaced and will move independent from each other. The extended iliofemoral is the only approach allowing for visualization and reduction of each column. A combined anterior and posterior approach may also be used. The timing of surgery should be within the first 3 weeks of injury to optimize chances of obtaining an accurate reduction because this is an important factor in determining outcome. Letournel E, Judet R (eds): Fractures of the Acetabulum, ed 2. Berlin, Germany, Springer-Verlag, 1991.
