Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
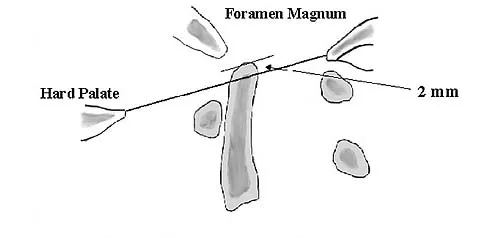
In the anterior forearm approach to the distal radius (Henry approach), the radial artery is located between what two structures?
Explanation
The standard approach to the volar aspect of the distal radius is the Henry approach. Following incision of the skin and subcutaneous tissues, the forearm fascia is incised. The radial artery and venae comitantes lie in the interval between the tendons of the flexor carpi radialis muscle and the brachioradialis muscle. This interval is developed, and the radial artery and veins are retracted in a radial direction. Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics, ed 2. Philadelphia, PA, Lippincott-Raven, 1994, pp 118-131.
Question 2
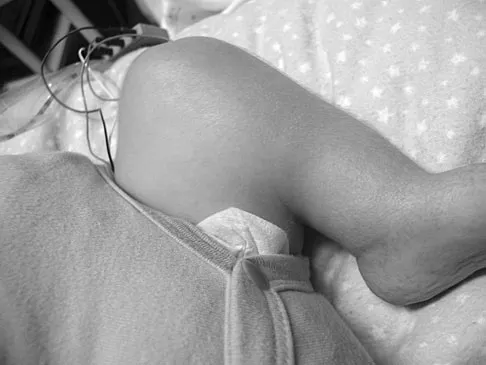
Duchenne's muscular dystrophy is a genetic disorder that is transmitted by which of the following modes of inheritance?
Explanation
Patients with Duchenne's muscular dystrophy show progressive muscular weakness because of the absence of dystrophin and have the clinical picture of progressive muscle weakness. The condition is an X-linked genetic disease. Fitzgerald RH, Kaufer H, Malkani AL: Orthopaedics. St Louis, MO, Mosby Year Book, 2002, pp 1573-1583.
Question 3
A 19-year-old man has had back pain with activity, especially running in soccer and baseball, for the past 4 months. He denies any history of trauma. Examination reveals no motor weakness or sensory changes in the lower extremities. Range of motion shows increased pain with extension and mild limitation with flexion. A sitting straight leg raising test is limited at approximately 60 degrees bilaterally by back and buttocks pain. Plain radiographs are normal. MRI scans are shown in Figures 13a through 13e. What is the most likely diagnosis?
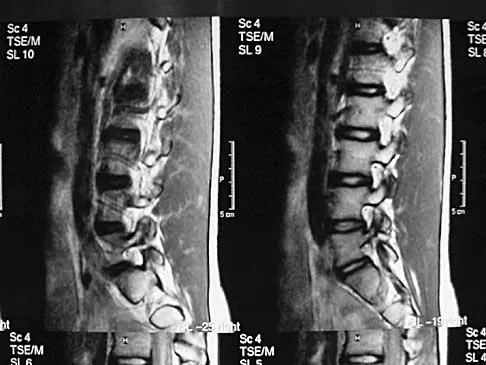
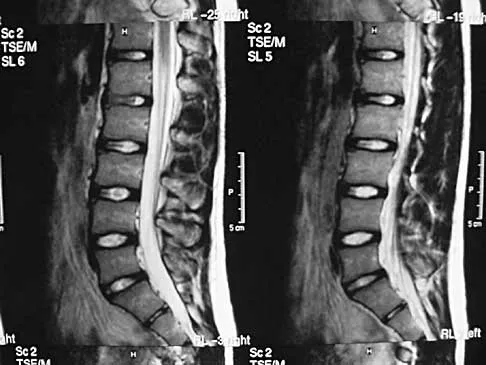
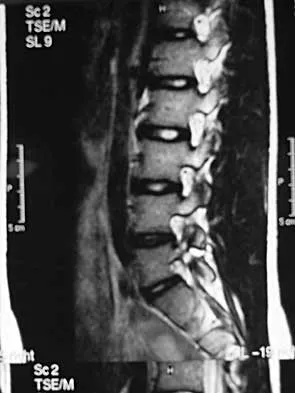
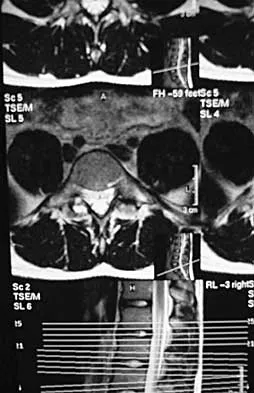
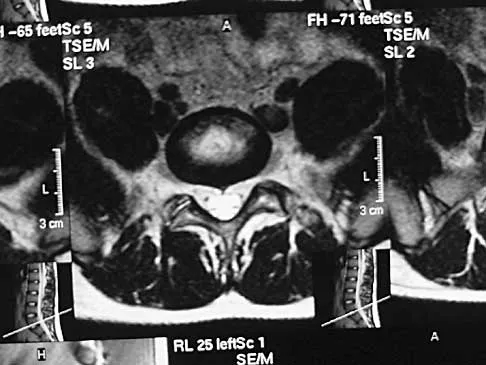
Explanation
The patient has an isthmic spondylolysis. The plain radiographs are normal, but the MRI scans show increased marrow edema and signal at the L5 pars interarticularis. Findings of bilateral hamstring tightness and increased pain with extension over flexion suggests spondylolysis. The MRI scans do not show any signs of the other conditions. Wiltse LL, Rothman SL: Spondylolisthesis: Classification, diagnosis and natural history. Sem Spine Surg 1993;5:264-280.
Question 4
Figure 1 shows the radiograph of an 18-year-old patient who has severe knee pain. Treatment consisting of osteotomy should be perfomed
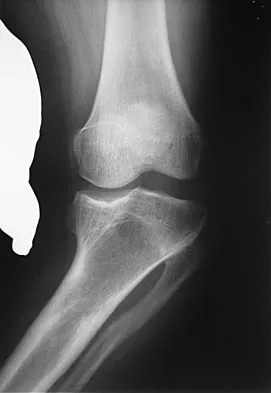
Explanation
Very large corrections of tibial deformity can be achieved at or just below the tibial tubercle. This level of osteotomy maintains the relationship between the tubercle and the rest of the joint, does not alter patellofemoral mechanics, and avoids complicating possible future conversion to total knee arthroplasty. High tibial osteotomy is contraindicated for large corrections because of excessive elevation of the tibial tubercle and overhang of the lateral plateau. Correction in the tibial diaphysis creates a zig zag pattern in the tibia by correcting below the deformity and risks nonunion in cortical bone. There is no evidence that the femur is deformed; therefore, femoral osteotomy is not indicated.
Question 5
Figure 22 shows the radiograph of a 7-year-old boy who underwent retrograde elastic nailing of a femoral shaft fracture. What is the most common problem following this procedure?
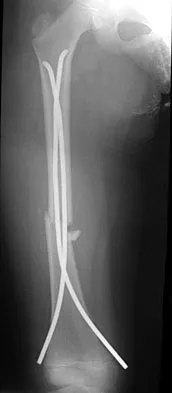
Explanation
Several large clinical studies have shown that the most common problem after elastic nailing of a femoral shaft fracture is persistent pain and irritation at the nail insertion site. Unacceptable shortening and malunion are very rare in a 7-year-old patient. Rotational malalignment also is unusual. Osteonecrosis has been reported in solid antegrade nailing but not with elastic nailing of femoral shaft fractures in skeletally immature patients. Flynn JM, Luedtke LM, Ganley TJ, et al: Comparison of titanium elastic nails with traction and a spica cast to treat femoral fractures in children. J Bone Joint Surg Am 2004;86:770-777. Flynn JM, Hresko T, Reynolds RA, et al: Titanium elastic nails for pediatric femur fractures: A multicenter study of early results with analysis of complications. J Pediatr Orthop 2001;21:4-8.
Question 6
A 15-year-old boy has hindfoot pain and very limited subtalar motion. A CT scan reveals a talocalcaneal coalition involving 40% of the middle facet. He has no degeneration of the posterior subtalar facet. Following failure of nonsurgical management, treatment should consist of
Explanation
The CT scan is an important test to help determine the extent of involvement of the talocalcaneal facet in a talocalcaneal coalition. In a young patient with no arthritis and joint involvement of less than 50%, resection of the coalition and fat pad interposition has been shown to be successful. A calcaneal osteotomy does not address the coalition. Subtalar arthroereisis has been used for treatment of a flexible flatfoot; tarsal coalition patients have a rigid-type flatfoot deformity. Sullivan JA: The child's foot, in Morrissy RT, Weinstein SL (eds): Lovell and Winter's Pediatric Orthopaedics, ed 4. Philadelphia, PA, Lippincott-Raven, 1996, vol 2, pp 1077-1135.
Question 7
A 52-year-old man has pain in the sternal area after landing on his right shoulder in a fall from his bicycle. In addition, he reports that he had difficulty swallowing and breathing immediately after the fall, but the symptoms resolved. A CT scan reveals a posterior sternoclavicular dislocation. Initial management should include
Explanation
Posterior sternoclavicular dislocations require rapid treatment because of the proximity of major neurovascular structures and the airway. Initial management should consist of closed reduction under general anesthesia in the operating room with a chest surgeon available. A successful closed reduction is usually stable. Internal fixation of sternoclavicular injuries should be avoided because of the likelihood of hardware migration and possible injury to the mediastinal structures. If closed reduction is unsuccessful, open reduction is indicated. Treatment following reduction of the sternoclavicular joint includes the application of a figure-of-8 splint and a sling for 6 weeks, followed by stretching and strengthening exercises. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont IL, American Academy of Orthopaedic Surgeons, 1999, pp 287-297.
Question 8
A 20-year-old man involved in a motor vehicle accident is brought to the emergency department with a C6-7 unilateral facet dislocation. His neurologic examination reveals a focal left-sided C7 nerve root palsy. He is awake and cooperative with questioning and has no other obvious traumatic injuries. What is the most appropriate treatment at this time?
Explanation
In the patient who is neurologically intact or has an incomplete injury from a cervical facet dislocation, a closed reduction with weighted tong traction is appropriate when the patient is awake, alert, and cooperative. Although there is a risk that a cervical facet dislocation could occur with an underlying cervical disk herniation, Vaccaro and associates have shown that closed reduction can be safely carried out in the awake, responsive patient. Closed reduction can be performed in the emergency department with traction with skull tongs or a halo ring. A slow stepwise application of weight is added until a reduction is achieved. Any worsening of the neurologic status of the patient requires immediate termination of the closed reduction and further diagnostic imaging before proceeding with further treatment. Vaccaro AR, Falatyn SP, Flanders AE, et al: Magnetic resonance evaluation of the intervertebral disc, spinal ligaments, and spinal cord before and after closed traction reduction of cervical spine dislocations. Spine 1999;24:1210-1217. Hart RA: Cervical facet dislocation: When is magnetic resonance imaging indicated? Spine 2002;27:116-117.
Question 9
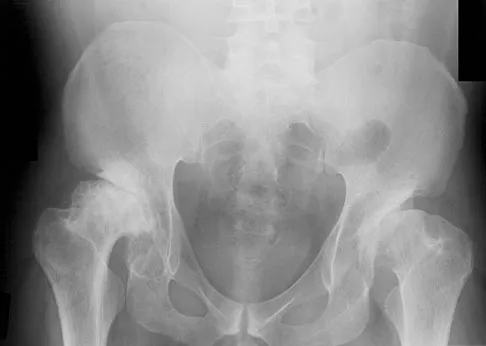
An AP radiograph of the pelvis is shown in Figure 4. What muscle attaches to the avulsed fragment of bone identified by the arrow?
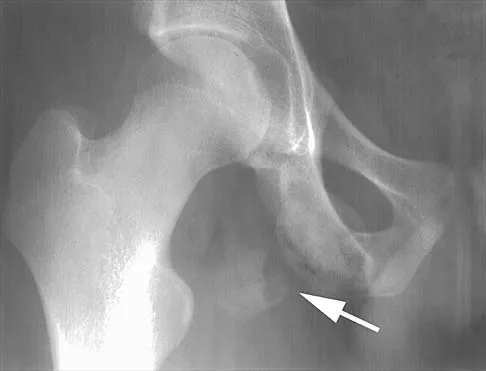
Explanation
The radiograph reveals an avulsion of the ischial apophysis, most likely the result of violent contraction of the attached hamstring tendons (semimembranosus, semitendinosus, and long head of the biceps femoris). The short head of the biceps femoris arises from the linea aspera on the posterior femur. The pectineus and adductor longus attach to the pubic portion of the pelvis. The piriformis runs from the sacrum to the femur. Woodburne RT (ed): Essentials of Human Anatomy. New York, NY, Oxford University Press, 1978, pp 542-545.
Question 10
A 19-year-old soccer player feels a pop in his knee while making a cut and notes the development of an effusion over several hours. Examination reveals medial joint line tenderness, but the knee is stable to manual stress testing of all ligaments. Examination under anesthesia confirms a stable knee. What is the most critical factor in determining healing after repair of the lesion shown in Figure 14?
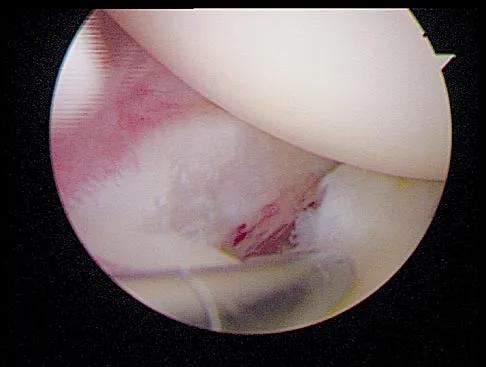
Explanation
Numerous clinical and basic science investigations have evaluated meniscal tear characteristics to identify factors that either promote or mitigate against meniscal healing. Complex tears have been noted to heal poorly, while longitudinal tears heal more predictably. Tear length, time from injury to repair, medial versus lateral meniscal tears, and the use of a fibrin clot have not been shown to consistently affect meniscal healing. However, rim width, the distance of the tear site from the peripheral meniscocapsular junction (vascular supply), has been shown to have a significant role in the ability of a meniscus repair to heal. DeHaven KE, Arnoczky SP: Meniscus repair: Basic science, indications for repair, and open repair. Instr Course Lect 1994;43:65-76.
Question 11
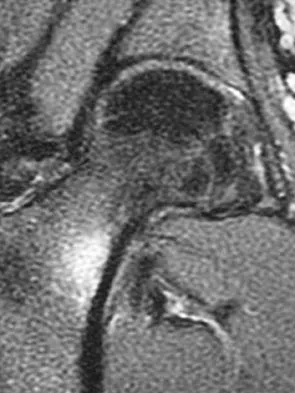
A 21-year-old collegiate female cross-country athlete reports right hip pain that begins about 12 miles into a run, followed by pain resolution when she discontinues running. However, each time she tries to resume a running program, she experiences recurrence of pain deep in the anterior groin. A plain radiograph and MRI scan are shown in Figures 8a and 8b. Management should consist of
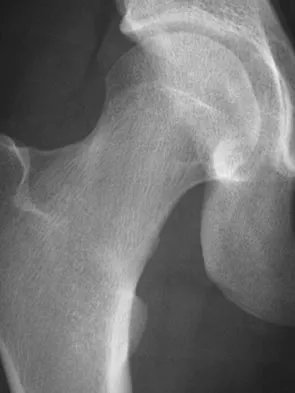
Explanation
The history is consistent with a stress fracture. Findings on the plain radiograph are marginal, but the MRI scan shows evidence of stress reaction in the medial neck of the femur (compression side). A lesion on the compression side is not normally at risk for displacement and usually can be managed nonsurgically. A bone scan would further identify the lesion but is not necessary. A skeletal survey and chest radiograph are used in staging a tumor. Radioisotope injection and guided biopsy are sometimes used for osteoid osteomas. Boden BP, Osbahr DC: High-risk stress fractures: Evaluation and treatment. J Am Acad Orthop Surg 2000;8:344-353.
Question 12
A 50-year-old patient who plays tennis sustained the deformity shown in Figure 27 following a high volley. Further diagnostic work-up should include

Explanation
The patient has a rupture of the long head of the biceps; however, patients older than age 45 years are at greater risk of having an associated rotator cuff tear. An MRI scan should be ordered to avoid missing concomitant rotator cuff pathology. While patients may report pain radiating down the arm at the time of the tendon rupture, an EMG is not indicated. The short head of the biceps is intact and needs no further work-up, even though the muscle descends in most cases. The anterior labrum can be injured but is not associated with this deformity. Neer CS II, Bigliani LU, Hawkins RJ: Rupture of the long head of the biceps related to the subacromial impingement. Orthop Trans 1977;1:114.
Question 13
Bioabsorbable polymers are used in a wide range of orthopaedic devices, including anchors, staples, pins, plates, and screws. What is the primary drawback for bioabsorbable implants?
Explanation
A number of bioabsorbable polymers are used in orthopaedic applications, and all have in common reports of foreign body reactions, which occur in more than 50% of patients in some series. In general, the high cost of these polymers is offset by the elimination of a second surgery to remove the implant. Bioabsorbable polymers are low strength in comparison to metallic alloys but of sufficient strength for many orthopaedic applications. The elastic modulus is not as high as many other orthopaedic biomaterials, making them suitable for applications where lower stiffness is an asset. Ambrose CG, Clanton TO: Bioabsorbable implants: Review of clinical experience in orthopedic surgery. Ann Biomed Eng 2004;32:171-177.
Question 14
During the implantation of a cementless acetabular component in total hip arthroplasty, placement of a screw in the anterior superior quadrant puts which of the following structures at risk for damage?
Explanation
A knowledge of the safe quadrants for screw placement for acetabular component implantation is essential when performing total hip arthroplasty. The external iliac vessels are on the inner wall of the pelvis, corresponding to the anterior superior quadrant of the acetabulum. Keating EM, Ritter MA, Faris PM: Structures at risk from medially placed acetabular screws. J Bone Joint Surg Am 1990;72:509-511.
Question 15
A 46-year-old woman reports pain and a shortened appearance of her toe after undergoing a Keller resection arthroplasty 2 years ago for hallux rigidus. Examination reveals mild swelling and motion limited to 25 degrees at the metatarsophalangeal joint. Radiographs show large dorsal osteophytes on the first metatarsal head, 50% resection of the proximal phalanx, and complete loss of the metatarsophalangeal joint space. Which of the following is considered the most reliable procedure to improve her pain and the appearance of her toe?
Explanation
Because the patient has significant arthritis, arthrodesis is the treatment of choice. Adding a bone graft will prevent further shortening and add length to her toe, resulting in improved cosmesis. A cheilectomy will not alleviate her arthritis pain. The toe is too short for an effective Moberg phalangeal dorsiflexion osteotomy. A Waterman first metatarsal dorsal osteotomy will not address the degenerative joint disease or shortening. Silastic arthroplasty may help, but there is the risk of additional problems with foreign body reaction and a significant risk of failure known to occur with Silastic materials. Myerson MS, Schon LC, McGuigan FX, Oznur A:Result of arthrodesis of the hallux metatarsophalangeal joint using bone graft for restoration of length. Foot Ankle Int 2000;21:297-306. Mann RA, Coughlin MJ: Adult hallux valgus, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, pp 252-253.
Question 16
In the nonsurgical management of posterior tibial tendon dysfunction with flexible deformity, a common strategy is to prescribe an ankle-foot orthosis or a University of California Biomechanics Laboratory (UCBL) orthosis with medial posting. A high patient satisfaction rating and favorable outcome with this nonsurgical management is most likely in which of the following situations?
Explanation
Most authors recommend an initial trial of nonsurgical management in the treatment of adult-acquired flatfoot deformity such as posterior tibial tendon dysfunction. Chao and associates found that there is high patient satisfaction with ankle-foot orthoses and UCBL-type inserts in elderly patients with a relatively sedentary lifestyle. Alternatively, there was a higher dissatisfaction rate in young active patients, those with balance and ambulation difficulties (Parkinson's, severe arthritis of the hip or knee), and patients with inflammatory systemic disorders. Chao W, Wapner KL, Lee TH, et al: Nonoperative management of posterior tibial tendon dysfunction. Foot Ankle Int 1996;17:736-741.
Question 17
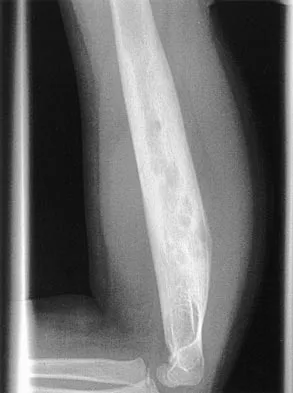
A 6-year-old African-American boy with sickle cell disease has had pain and limited use of his right arm for the past 3 days. History reveals that he sustained a humeral fracture approximately 3 years ago. A lateral radiograph is shown in Figure 25. Based on these findings, a presumptive diagnosis of chronic osteomyelitis is made. What are the two most likely organisms?
Explanation
The risk of Salmonella osteomyelitis is much greater in patients with sickle cell disease than the general population. The exact reason for this increased risk is still unclear, but it appears to be associated with an increased incidence of gastrointestinal microinfarcts and abscesses. Both Staphylococcus aureus and Salmonella have been mentioned as the most prevalent causative organisms. Piehl FC, David RJ, Prugh SI: Osteomyelitis in sickle cell disease. J Pediatr Orthop 1993;13:225-227. Givner LB, Luddy RE, Schwartz AD: Etiology of osteomyelitis in patients with major sickle hemoglobinopathies. J Pediatr 1981;99:411-413. Epps CH Jr, Bryant DD III, Coles MJ, Castro O: Osteomyelitis in patients who have sickle-cell disease: Diagnosis and management. J Bone Joint Surg Am 1991;73:1281-1294.
Question 18
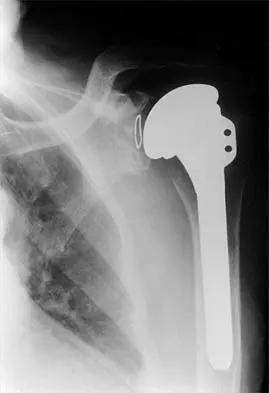
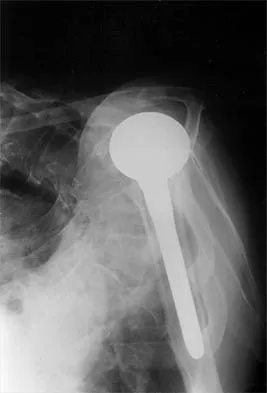
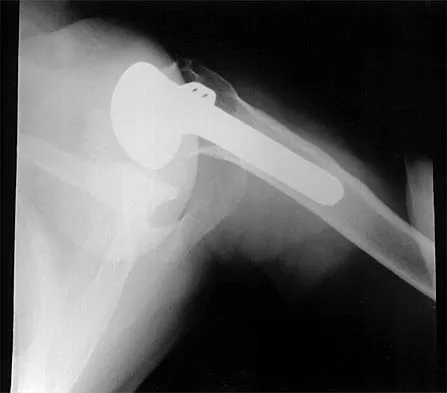
A 72-year-old woman who was doing well after undergoing total shoulder arthroplasty for arthritis 4 months ago is suddenly unable to elevate her arm. Examination reveals 70 degrees of external rotation compared with 45 degrees on the uninvolved side, and she is unable to lift her hand off her lower back. Radiographs are shown in Figures 43a through 43c. Treatment should consist of
Explanation
Results of treatment of subscapularis rupture are best when immediate repair is performed. When the cause of the anterior instability is the result of rupture of the subscapularis tendon and the component position is acceptable, revising the position of the component is unnecessary. Restoring the coracoacromial arch and subacromial decompression are related to superior instability and rotator cuff pathology, respectively, and would not correct the instability caused by subscapularis rupture. Moeckel BH, Altchek DW, Warren RF, Wickiewicz TL, Dines DM: Instability of the shoulder after arthroplasty. J Bone Joint Surg Am 1993;75:492-497.
Question 19
Increasing articular conformity of the tibial polyethylene insert of a fixed-bearing total knee arthroplasty (TKA) prosthesis will have which of the following biomechanical effects?
Explanation
Increasing articular conformity increases the surface area for contact between the polyethylene and the femoral component. Advantages of this include lower peak contact stress within the polyethylene and less risk of polyethylene fatigue failure. Patellofemoral tracking is unchanged by increasing conformity unless gross component apposition is present. A potential disadvantage of increasing conformity includes some restriction in tibial rollback. Modest changes in conformity have not been shown to alter the rate of mechanical loosening. If conformity was increased to the extent of significant constraint, a potential increased risk of loosening would be expected, not a decrease. Design of modern TKAs includes a compromise in achieving enough constraint to lower polyethylene stress, without providing so much constraint as to limit kinematics and stress the fixation interfaces. D'Lima DD, Chen PC, Colwell CW Jr: Polyethylene contact stresses, articular congruity, and knee alignment. Clin Orthop 2001;392:232-238.
Question 20
Which of the following tissues has the highest maximum load to failure?
Explanation
All of the tissues noted above are stronger than native ACL. Although it is often thought that the bone-patellar tendon-bone graft is the strongest when selecting a graft source for ACL reconstruction, biomechanical studies show that the quadruple semitendinosus and gracilis tendons are the strongest of the tissues listed. Woo SL, Hollis JM, Adams DJ, et al: Tensile properties of the human femur-anterior cruciate ligament-tibia complex: The effects of specimen age and orientation. Am J Sports Med 1991;19:217-225. Staubli HU, Schatzmann L, Brunner P, et al: Quadriceps tendon and patellar ligament cryosectional anatomy and structural properties in young adults. Knee Surg Sports Traumatol Arthrosc 1996;4:100-110.
Question 21
A 16-year-old ice hockey player is struck on the chest by the puck. He skates a few strides and then collapses. What is the most likely diagnosis?
Explanation
Sudden cardiac arrest following a blow to the chest in young athletes has been termed "commotio cordis." It is most common in Little League and other youth projectile sports (eg, ice hockey, lacrosse). The cause, although not completely determined, is most likely an arrhythmia related to the impact in a vulnerable time in the cardiac cycle. Resuscitation has proven to be exceedingly difficult, resulting in a high mortality rate. Maron BJ, Strasburger JF, Kugler JD, Bell BM, Brodkey FD, Poliac LC: Survival following blunt chest impact-induced cardiac arrest during sports activities in young athletes. Am J Cardiol 1997;79:840-841.
Question 22
A 15-year-old boy who participates in track reports acute pain along the left iliac crest during a sprint. Examination reveals that the anterior superior iliac spine is nontender. The most likely diagnosis is an injury to the
Explanation
The patient has iliac apophysitis. The radiographic findings are easily overlooked but usually reveal slight asymmetric widening of the iliac crest apophysis. The apophysis is the most vulnerable structure, as it is three to five times weaker than the tendon. This is not an epiphyseal site, and injury to the muscle or the tendinous insertion to bone (enthesis) is unlikely. Clancy WG Jr, Foltz AS: Iliac apophysitis and stress fractures in adolescent runners. Am J Sports Med 1976;4:214-218. Waters PM, Millis MB: Hip and pelvic injuries in the young athlete, in Stanitski CL, DeLee JC, Drez D Jr (eds): Pediatric and Adolescent Sports Medicine. Philadelphia, PA, WB Saunders, 1994, pp 279-293. Lombardo SJ, Retting AC, Kerlan RK: Radiographic abnormalities of the iliac apophysis in adolescent athletes. J Bone Joint Surg Am 1983;65:444-446.
Question 23
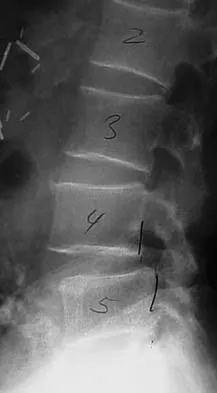
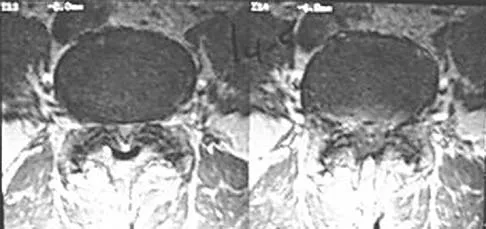
An otherwise healthy 70-year-old man has back and bilateral leg pain in an L5 distribution that is aggravated by standing more than 10 minutes or walking more than 100 feet. He has to sit to get relief. Neurologic and pulse examinations are normal. A radiograph and MRI scan are shown in Figures 4a and 4b. Treatment should consist of
Explanation
The patient has a degenerative spondylolisthesis at L4-5 with associated spinal stenosis. His symptoms are consistent with neurogenic claudication. Based on these findings, the surgical treatment of choice is decompression and posterolateral fusion. Use of instrumentation is controversial. Laminectomy alone is reserved for the patient who is frail medically. There is no role for an anterior approach or for fusion alone without decompression. Fischgrund JS, Mackay M, Herkowitz HN, et al: Degenerative lumbar spondylolisthesis with spinal stenosis: A prospective, randomized study comparing decompressive laminectomy and arthrodesis with and without spinal instrumentation. Spine 1997;22:2807-2812.
Question 24
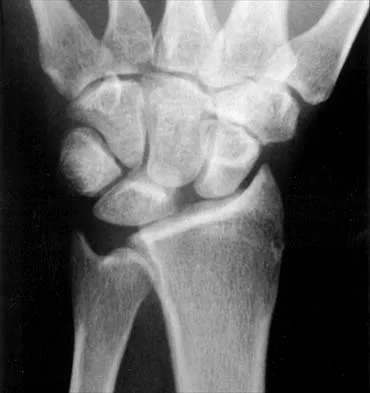
Based on the findings seen in the posteroanterior radiograph of the wrist shown in Figure 17, which of the following structures is torn?
Explanation
The radiograph shows widening between the scaphoid and lunate. The normal variance is up to 5 mm. Although several ligaments may be torn, the scapholunate interosseous ligament must be torn for this widening to occur. Cooney WP, Linscheid RL, Dobyns JH: The Wrist: Diagnosis and Operative Treatment. St Louis, MO, Mosby-Year Book, 1998, vol 1, pp 503-506.
Question 25
In children with isolated zone II lacerations of the flexor tendon, poor digital motion is best correlated with
Explanation
In a recent study on restoration of motion following zone I and zone II flexor tendon repairs in children, age was found to have no effect on the results of zone II tendon repairs. Early passive motion offered no better results than immobilization for 3 weeks. Immobilization for more than 4 weeks correlated with poorer results.
Question 26
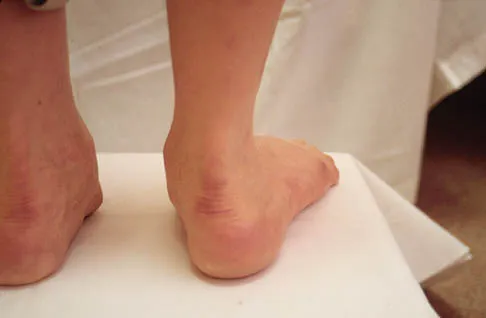
Figure 13 shows the clinical photograph of a 66-year-old man who has had an increasingly painful right foot deformity for the past 3 years. Examination reveals that the subtalar joint is fixed in 15 degrees of valgus, and forefoot supination can be corrected to 10 degrees from neutral. Nonsurgical management has failed to provide relief. Treatment should now consist of
Explanation
The most important determining factor for correction of an adult flatfoot without an arthrodesis is the flexibility of the subtalar and transverse tarsal joints. Rigid deformities cannot be corrected with a medial sliding calcaneal osteotomy with FDL transfer or a subtalar arthroereisis. Isolated subtalar or talonavicular arthrodesis does not correct the deformities entirely. If the patient has forefoot supination that can be corrected to less than 7 degrees, an isolated subtalar fusion is a possible alternative.
Question 27
A 68-year-old woman underwent a successful total right hip arthroplasty with a metal-on-metal articulation and cementless porous-coated components. Three months later, she underwent identical surgery on the left hip. Three months after surgery on the left hip, she reports groin pain on ambulation. Examination reveals significant groin discomfort with passive hip motion, particularly at the extremes of motion. Radiographs are shown in Figures 21a and 21b. Laboratory studies show an erythrocyte sedimentation rate of 35 mm/h and a C-reactive protein of 0.9. Aspiration yields scant growth of Staphylococcus epidermidis in the broth only, with no evidence of loosening on arthrography. A second aspiration yields scant growth of Staphylococcus epidermidis in the broth only. What is the most likely cause of the patient's pain?
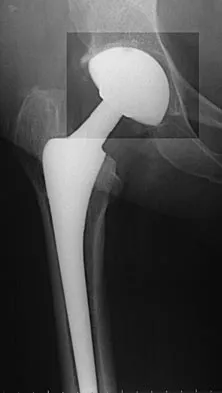
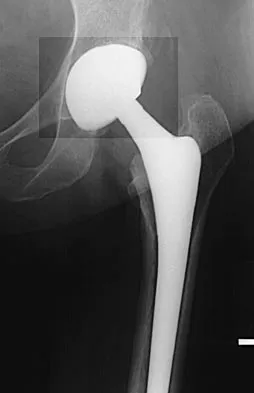
Explanation
The difference in the clinical results combined with the laboratory findings points to infection. While there is a significant risk of false-positive findings with aspiration, the fact that two successive aspirations grew the same organism strongly suggests infection. The radiograph shows that there is more radiolucency around the left acetabular component than the right component. White RE: Evaluation of the painful total hip arthroplasty, in Callaghan JJ, Rosenberg AG, Rubash HE (eds): The Adult Hip. Philadelphia, PA, Lippincott-Raven, 1998, vol 2, pp 1377-1385.
Question 28
When performing a Weil osteotomy of a lesser metatarsal, the desired angle of the saw cut should be approximately
Explanation
Appropriate orientation of the saw cut when performing a Weil osteotomy is approximately parallel with the plantar surface of the foot. This is done in an effort to minimize plantar displacement of the capital fragment. The removal of additional bone from the osteotomy site either by removing a separate wafer of bone or using a thicker saw blade has also been described to minimize plantar displacement of the distal fragment. Trnka H, Nyska M, Parks BG, et al: Dorsiflexion contracture after the Weil osteotomy: Results of cadaver study and three-dimensional analysis. Foot Ankle Int 2001;22:47-50.
Question 29
A 68-year-old woman with a history of rheumatoid arthritis has had neck pain and weakness in all four extremities that has become worse in the past 6 months. She has gone from a community to a household ambulator and uses a wheelchair outside of the home. Examination of the extremities reveals poor coordination, diffuse weakness, hyperactive reflexes, and bilateral sustained clonus. She has a broad-based and unsteady gait. The posterior atlanto-dens interval is 12 mm. Based on these findings and the radiograph and MRI scan shown in Figures 13a and 13b, the treatment of choice is surgical decompression and stabilization. However, the patient inquires about the prognosis with surgery compared to nonsurgical management. Assuming there are no complications from surgery, the patient should be informed that, with surgery, she will most likely
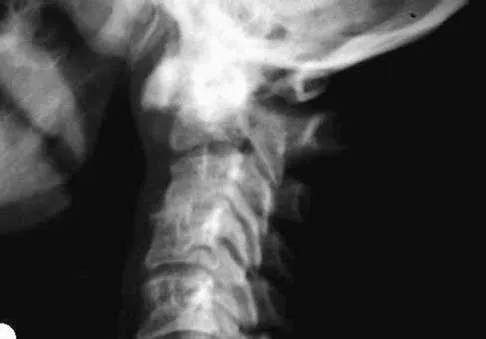
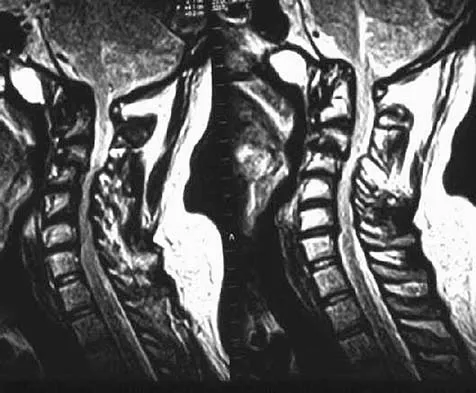
Explanation
The patient has a cervical myelopathy with more than 10 mm of space available for the cord; therefore, she has a reasonable chance of improved neurologic function following surgery. If not treated with surgery, however, her neurologic condition likely will worsen and she will die earlier than if she had surgery. Matsunaga S, Sakou T, Onishi T, et al: Prognosis of patients with upper cervical lesions caused by rheumatoid arthritis: Comparison of occipitocervical fusion between C1 laminectomy and nonsurgical management. Spine 2003;28:1581-1587.
Question 30
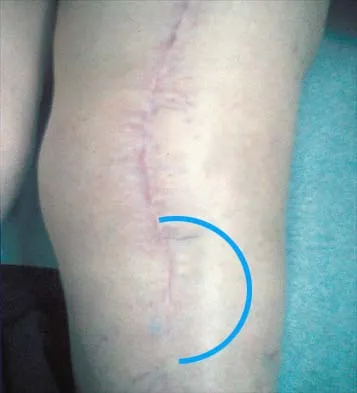
Figures 43a and 43b show the clinical photographs of a 4-month-old child with bilateral popliteal pterygium. The fixed knee contractures measure 100 degrees bilaterally. What future treatment is most likely to successfully correct this deformity?
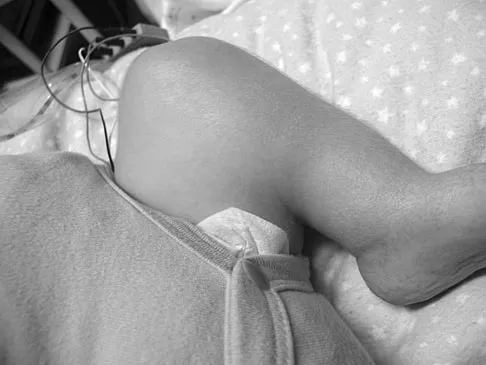
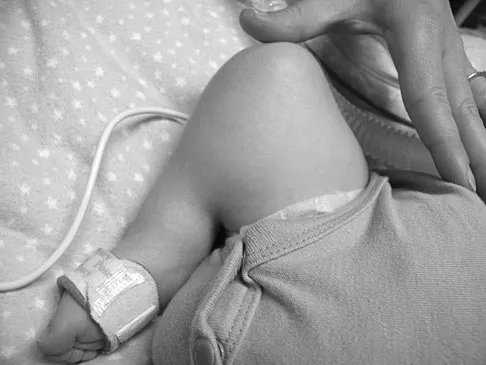
Explanation
Congenital popliteal webbing with contractures of 60 degrees is a difficult deformity to correct. The anatomy of the web is of considerable importance. MRI can delineate the extent of the posterior fibrous band that often stretches from the ischium to the calcaneus. The sciatic nerve, usually shortened, most often runs just anterior to this fibrous band. For mild contractures of less than 20 degrees, nonsurgical management is usually adequate. Hamstring lengthening and postoperative splinting are usually sufficient for contractures of 20 degrees to 40 degrees. Moderate contractures of up to 60 degrees usually require Z-plasties in the popliteal fossa and postoperative serial casting to avoid undue tension on neurovascular structures. Contractures of more than 60 degrees require a femoral shortening osteotomy or gradual correction with an external fixator. However, rapid recurrence following fixator removal is common if formal soft-tissue procedures and postoperative splinting are not performed. Parikh SN, Crawford AH, Do TT, et al: Popliteal pterygium syndrome: Implications for orthopaedic management. J Pediatr Orthop B 2004;13:197-201.
Question 31
A relative contraindication for anteromedial tibial tubercle transfer for patellar instability is arthrosis in what portion of the patella?
Explanation
Anteromedial displacement of the tibial tubercle unloads the distal and lateral facets of the patella and shifts the forces to the proximal and medial facets. Therefore, if findings indicate arthrosis predominately in the medial and proximal areas of the patella, this is considered a relative contraindication because it may accentuate arthritic symptoms. Fulkerson JP: Anteromedialization of the tibial tuberosity for patellofemoral malalignment. Clin Orthop 1983;177:176-181. Bellemans J, Cauwenberghs F, Witvrouw E, et al: Anteromedial tibial tubercle transfer in patients with chronic anterior knee pain and a subluxation-type patellar malalignment. Am J Sports Med 1997;25:375-381.
Question 32
A 25-year-old laborer sustains a transverse fracture of the proximal 25% of the scaphoid. CT reconstructions reveal a 1-mm fracture gap. What is the most appropriate treatment?
Explanation
A higher risk of nonunion and the need for prolonged immobilization is seen after nonsurgical management of proximal pole fractures of the scaphoid. Because of the relatively poor blood supply of the proximal pole, surgical treatment with a compression screw is advocated for fractures of the proximal third of the scaphoid. Clay NR, Dias JJ, Costigan PS, et al: Need the thumb be immobilized in scaphoid fractures? A randomised prospective trial. J Bone Joint Surg Br 1991;73:828-832.
Question 33
A 28-year-old woman has left shoulder pain and a tender soft-tissue mass. Based on the MRI scan and biopsy specimens shown in Figures 74a through 74c, what is the most likely diagnosis?
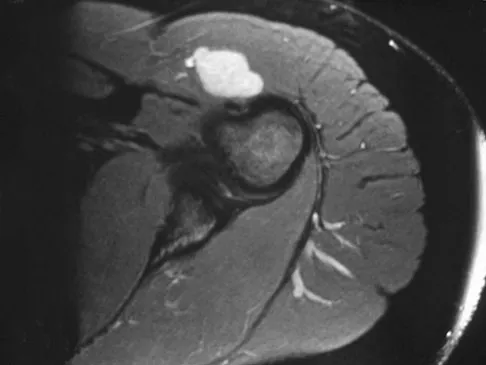
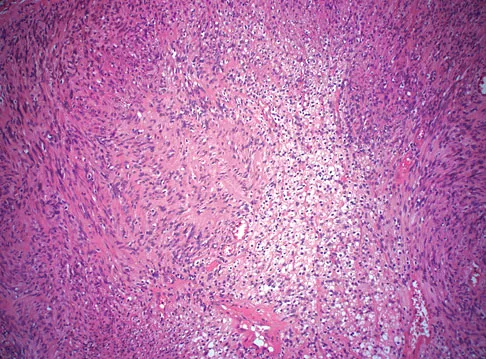
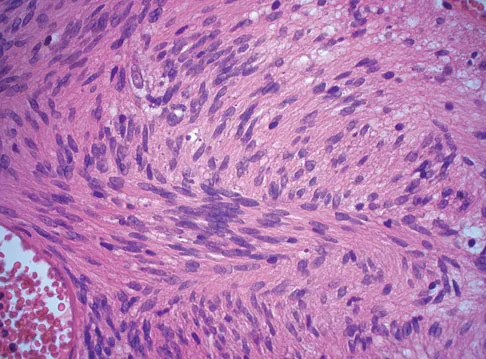
Explanation
Schwannomas (neurilemomas) occur at all ages but are most frequently seen in persons between the ages of 20 and 50 years. MRI features of schwannomas are fairly nonspecific, but when they are associated with a large named nerve, the identification of a mass in continuity with that nerve is highly suggestive of a schwannoma. Most have a fairly homogeneous appearance with a high water content and often fusiform shape. Classically, the histology shows alternating Antoni A (dense spindle cell region) areas and Antoni B (loose myxoid tissue) areas. They also demonstrate uniform intense immunostaining with S-100 protein. Damron TA, Sim FH: Soft-tissue tumors about the knee. J Am Acad Orthop Surg 1997;5:141-152.
Question 34
On MRI, a nonsanguinous effusion has what appearance?
Explanation
Nonbloody effusions that are greater than 1 mL are readily detected by MRI. They appear black on T1-weighted images and white on T2-weighted images. A sanguinous effusion is seen as white on T1-weighted images and black on T2-weighted images. Resnick D, Kang HS: Synovial joints, in Resnick D, Kang HS (eds): Internal Derangements of Joints: Emphasis on MR Imaging. Philadelphia, PA, WB Saunders, 1997, pp 49-53.
Question 35
A 53-year-old man has a 4- x 5-cm high-grade soft-tissue sarcoma in the midthigh. As part of the staging evaluation, regional nodes should be assessed by
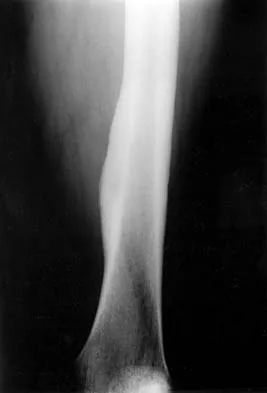
Explanation
In general, soft-tissue metastases to regional nodes are a relatively rare occurrence (less than 5% overall). The incidence of lymphatic metastasis is highest for synovial sarcoma, rhabdomyosarcoma, clear cell sarcoma, and epithelioid sarcoma. Regional nodes should be assessed clinically. CT is not used to routinely assess regional nodes. Evaluation of a sentinal node is not indicated because of the low incidence of regional nodal involvement. Fine needle aspiration may be indicated to assess clinically suspicious nodes. Prophylactic inguinal node dissection is contraindicated because it may lead to unnecessary complications such as lymphedema.
Question 36
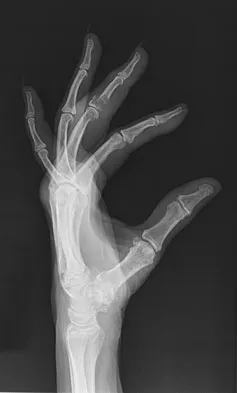
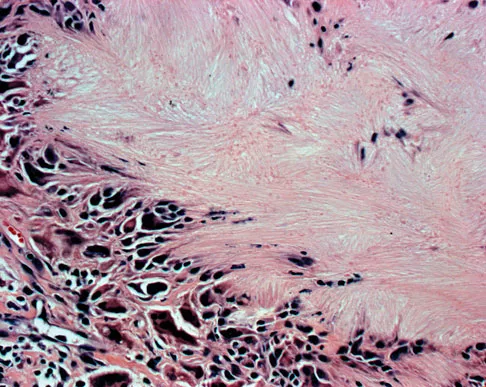
An 83-year-old woman reports pain in her left middle finger after a minor injury. Laboratory studies show a WBC count of 7,000/mm3, an erythrocyte sedimentation rate of 3 mm/h, a uric acid of 10.4 mg/dL, and a normal serum protein electrophoresis. Radiographs are shown in Figures 49a and 49b. A core biopsy specimen is shown is Figure 49c. In addition to treatment of the finger fracture, treatment should include
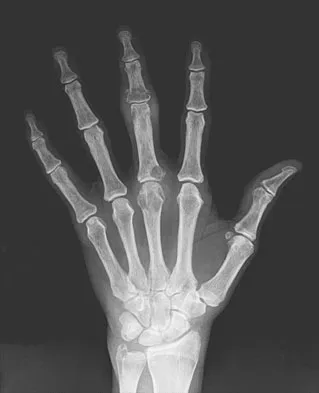
Explanation
This clinical picture is most consistent with periarticular erosions from gout. The patient has multiple periarticular lytic lesions in the hand. The laboratory studies show an elevated serum uric acid level, and the biopsy specimen demonstrates acute and chronic inflammation with prominent clefts. Therefore, the preferred treatment is systemic control of her gout. Radiation therapy, chemotherapy, and/or amputation should be considered for a malignancy; however, the pathology does not demonstrate any evidence of pleomorphism, high nuclear-to-cytoplasmic ratio, nuclear atypia, or mitotic activity. Antibiotics for an infectious process is a consideration, but the minimal elevation in the WBC count and erythrocyte sedimentation rate does not support an infectious process. Wise CM: Crystal-associated arthritis in the elderly. Clin Geriatr Med 2005;21:491-511.
Question 37
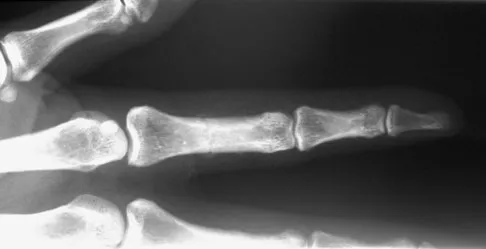
A 25-year-old semiprofessional football player sustains a hyperextension injury to the left foot. He is unable to bear weight. Examination reveals tenderness along the midfoot with swelling and plantar ecchymosis. Radiographs are negative. What is the next step in evaluation of this patient?
Explanation
The patient has a suspected Lisfranc sprain based on the plantar ecchymosis. The first step in diagnosis is a dynamic radiographic study. This should include a physician-assisted midfoot stress examination or standing weight-bearing radiographs to evaluate for displacement. There is no evidence of compartment syndrome, and a bone scan, CT, and MRI are expensive tests that are not warranted. Early JS: Fractures and dislocations of the midfoot and forefoot, in Bucholz R, Heckman JD, Court-Brown CM (eds): Rockwood and Green's Fractures in Adults. Philadelphia, PA, Lippincott Williams and Wilkins, 2006, pp 2337-2400.
Question 38
What is the most likely cause of recurrent symptoms following excision of a third web space neuroma?
Explanation
When a recurrent neuroma forms at the end of the resected nerve, it does not retract far enough because either the transection was not proximal enough or it is tethered by plantar neural branches. The transverse intermetatarsal ligament may reform, but it is not associated with pathology. Synovial cysts and synovitis are part of the differential diagnosis but are not associated with neuroma excision. Complex regional pain syndrome may result from neuroma excision, but this is rare and the symptoms are different. Beskin JL: Recurrent interdigital neuromas, in Nunley JA, Pfeffer GB, Sanders RW, Trepman E (eds): Advanced Reconstruction: Foot and Ankle. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 481-484.
Question 39
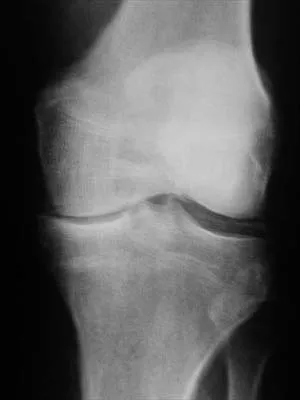
In children between the ages of 4 and 8 years, the major blood supply to the femoral head comes from the
Explanation
From birth until the age of 4 years, the primary blood supply to the femoral head is from the medial and lateral circumflex arteries that traverse the femoral neck. After the age of 4 years, the contribution of the lateral femoral circumflex artery, which traverses the anterior portion of the femoral neck, becomes negligible. The posterosuperior and posteroinferior retinacular vessels, branches of the medial femoral circumflex artery, become the primary blood supply to the epiphysis. The contribution of the artery of the ligamentum teres is minimal after the age of 4 years. Hughes LO, Beaty JH: Fractures of the head and neck of the femur in children. J Bone Joint Surg Am 1994;76:283-292.
Question 40
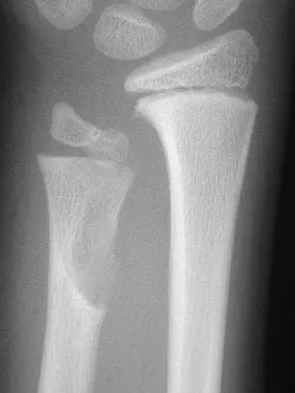
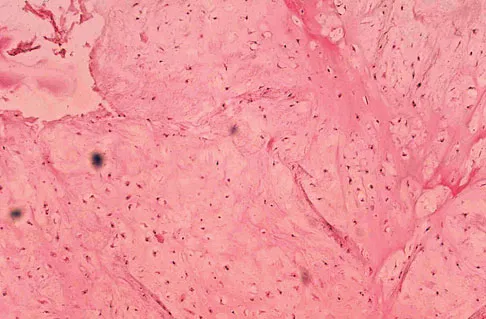
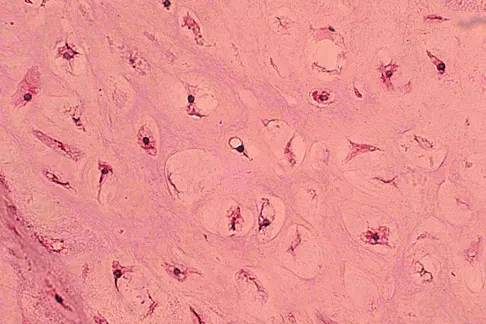
A 10-year-old boy has had wrist pain for the past 3 months. He denies any history of trauma. He reports mild tenderness associated with a palpable mass. A radiograph and biopsy specimens are shown in Figures 52a through 52c. What is the most likely diagnosis?
Explanation
The radiograph shows a benign-appearing cortically based lesion eroding the underlying cortex, producing a saucer-shaped defect typical of a periosteal chondroma. The histology shows benign-appearing neoplastic cartilage. Although enchondroma would have the same histologic appearance, radiographs generally show a lesion with a central medullary epicenter. The benign-appearing histology does not support chondrosarcoma. Chondromyxoid fibroma will generally show histologic elements of its fibrous and myxoid components. Chondroblastoma typically demonstrates histologic findings of polyhedral cells separated by a chondroid matrix with pericellular, lattice-like "chicken wire" calcification. Schajowicz F: Tumors and Tumorlike Lesions of Bone: Pathology, Radiology, and Treatment, ed 2. Berlin, Springer-Verlag, 1994, pp 147-151.
Question 41
A 21-year-old college defensive lineman sustains a minimally displaced (less than 1 mm) midthird scaphoid fracture during the first game of the season. Management should consist of
Explanation
The union rate for minimally displaced midthird scaphoid fractures is quite high with cast immobilization while allowing a return to sports. Inadequate immobilization results in a much higher nonunion rate. Early fixation and rehabilitation have been proposed for sports or positions that are not amenable to cast immobilization. While immobilization of a nondisplaced fracture results in an acceptably high union rate, there is no advantage to fixation in conjunction with immobilization in the course of healing. With adequate immobilization and protection, play restrictions until healing has occurred are unnecessary. Rettig AC, Kollias SC: Internal fixation of acute stable scaphoid fractures in the athlete. Am J Sports Med 1996;24:182-186. Rettig AC, Weidenbener EJ, Gloyeske R: Alternative management in midthird scaphoid fractures in the athlete. Am J Sports Med 1994;22:711-714.
Question 42
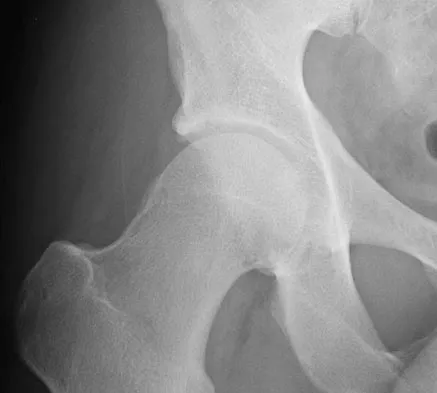
Figure 24 shows the radiograph of a 36-year-old volleyball player with right hip pain. What is the cause of the pain?
Explanation
Femoral acetabular impingement usually presents in active young adults with the slow onset of groin pain that often starts after a minor trauma. Physical examination reveals limitation of motion with a positive impingement test which consists of forceful internal rotation with flexion and adduction. Femoral acetabular impingement is a mechanism for the development of early osteoarthritis in nondysplastic hips. Surgical debridement of the impinging, nonspherical portion of the femoral head restores offset and improves the clearance of the head, thus preventing abutment of the neck against the acetabular rim. The patient has no evidence of osteonecrosis, developmental dysplasia of the hip, rheumatoid arthritis, or femoral neck fracture. Ganz R, Parvizi J, Beck M, et al: Femoroacetabular impingement: A cause for osteoarthritis of the hip. Clin Orthop 2003;417:112-120.
Question 43
A 46-year-old patient with cervical myelopathy undergoes a multilevel posterior cervical laminectomy from C3 to C7. The risk of postlaminectomy kyphosis is greatest with removal of which of the following structures?
Explanation
Removal of more than 50% of a facet joint can lead to segmental instability and compromises the overall strength of the joint. Removal of the lamina, interspinous ligament, and ligamentum flavum are standard features of a cervical laminectomy. Most surgeons favor fusion with instrumentation of a laminectomized cervical spine. If the anterior part of the spine is already ankylosed from previous surgery or from degenerative conditions, or a posterior fusion with instrumentation is included, then the risk of kyphosis or instability is reduced.
Question 44
A 22-year-old female collegiate javelin thrower has shoulder pain. She notes that her pain is primarily located in the posterior aspect of her shoulder, is exacerbated with throwing, and she experiences maximal tenderness in the extreme cocking phase of the throwing cycle. On examination, she reports deep posterior shoulder pain when the arm is abducted 90 degrees and maximally externally rotated to 110 degrees. This reproduces her symptoms precisely. Shoulder radiographs are normal. What is the most likely diagnosis?
Explanation
The patient has internal impingement. Internal impingement is commonly seen in overhead throwing athletes. When positioned in the extreme cocking phase of the throwing cycle, the posterior glenoid impacts the articular surface of the infraspinatus and posterior fibers of the supraspinatus tendon. This impact can cause partial-thickness rotator cuff tearing and posterosuperior labral lesions. She has no evidence of anterior shoulder instability, and her range of motion is excellent which rules out adhesive capsulitis. Subacromial impingement is identified with anterolateral shoulder pain with internal rotation in the abducted position. A full-thickness rotator cuff tear in a 22-year-old individual would require significant trauma and would likely result in pain at rest and with lifting. Meister K, Buckley B, Batts J: The posterior impingement sign: Diagnosis of rotator cuff and posterior labral tears secondary to internal impingement in overhand athletes. Am J Orthop 2004;33:412-415.
Question 45
Examination of a 28-year-old woman reveals a moderate hallux valgus deformity and a prominence of the medial eminence. She reports that she can participate in all activities, wear 3-inch heels with minimal discomfort, and walk in a 1-inch heel with no pain. However, she is concerned that the deformity will get worse and requests recommendations regarding surgical correction. What is the best course of action?
Explanation
Because the patient is essentially asymptomatic, the most appropriate course of action is observation. Prophylactic hallux valgus surgery is not medically indicated. Steroid injection would only risk infection, as well as joint and capsule damage. There are no data to support the use of a custom orthosis to delay the progression of a hallux valgus deformity. Special shoe wear or an extra-depth shoe is not necessary and is unlikely to be accepted by the patient. Donley BG, Tisdel CL, Sferra JJ, Hall JO: Diagnosing and treating hallux valgus: A conservative approach for a common problem. Cleve Clin J Med 1997;64:469-474.
Question 46
What clinical finding is associated with the least favorable prognosis in an adolescent patient who has been diagnosed with a high-grade osteosarcoma of the distal femur?
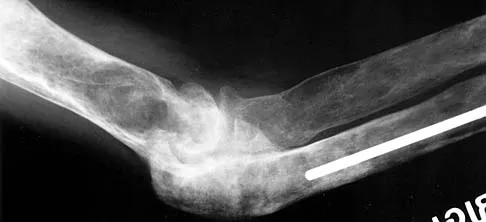
Explanation
The presence of synchronous bone disease in young patients carries a dismal prognosis, one that is even worse than the presence of resectable pulmonary metastasis. Many osteosarcomas cross the physis; therefore, this has not been shown to be of prognostic importance. Similarly, the presence of the soft-tissue mass has less prognostic significance.
Question 47
Compared to postoperative radiation therapy, preoperative radiation therapy has a higher rate of what complication?
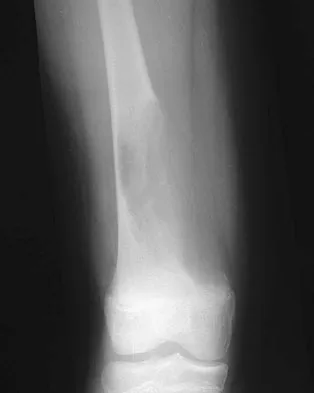
Explanation
Radiation therapy is commonly used as an adjuvant in the treatment of soft-tissue sarcomas, but a controversy exists whether it should be preoperative or postoperative. Radiation therapy can be given prior to or following resection of the tumor. Postoperative radiation is usually given in a higher dose to a larger treatment field. This commonly results in a higher incidence of fibrosis and lymphedema. There is no statistical difference in local recurrence rate between the two radiation treatment plans. Neuropathy is more commonly a complication of chemotherapy. Preoperative radiation therapy has been shown to have a higher wound complication rate than postoperative radiation. Vaccaro AR (ed): Orthopaedic Knowledge Update 8. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2005, pp 197-215.
Question 48
Which of the following findings is considered a contraindication for posterior decompression (with or without fusion) for myelopathy?
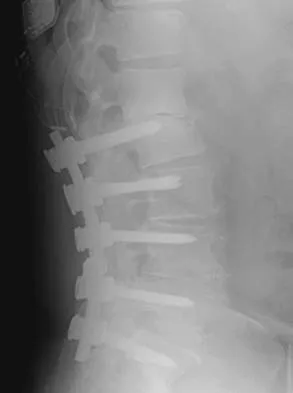
Explanation
Although cervical instability is a contraindication to posterior decompression alone, segmental instability in the myelopathic cervical spine can be addressed with concomitant posterior fusion with instrumentation. Cervical lordosis represents the ideal scenario for posterior decompressive procedures for myelopathy (laminectomy and laminoplasty) because compression from anterior osteophytes, if present, is relieved as the spinal cord migrates posteriorly. The anteroposterior diameter of the spinal canal does not have an impact on the selection of surgical approach. Posterior unroofing-type procedures in kyphotic cervical spines, however, are ineffective because anterior impingement on the spinal cord will remain; therefore, kyphosis of more than 10 degrees is considered a contraindication for posterior decompression. Emery SE: Cervical spondylotic myelopathy: Diagnosis and treatment. J Am Acad Orthop Surg 2001;9:376-388.
Question 49
A 28-year-old hockey player has a shoulder deformity after being checked into the boards. Examination reveals that swelling has improved, but there is tenderness along the distal clavicle. Radiographs reveal a grade II acromioclavicular joint separation. Initial management should consist of
Explanation
The most common shoulder injury in hockey players is to the acromioclavicular joint. Early rest and control of pain and inflammation is the preferred management. Surgery is reserved for patients with significant coracoclavicular disruption that has failed to respond to nonsurgical management. Cross-chest stretches and overhead exercises may increase symptoms. A cortisone injection within the glenohumeral joint will have little effect. Nuber GW, Bowen MK: Acromioclavicular joint injuries and distal clavicle fractures. J Am Acad Orthop Surg 1997;5:11-18.
Question 50
A 51-year-old woman is seen for evaluation of chronic supraspinatus and infraspinatus tendon tears. Three years ago, in an attempted repair the surgeon was unable to repair the supraspinatus and infraspinatus tendon tears. Currently she has a marked amount of pain, reduced range of motion, and weakness. Examination reveals anterosuperior escape. Radiographs show no signs of arthritic changes. You are considering a latissimus dorsi tendon transfer. During the discussion, you mention that
Explanation
Latissimus dorsi tendon transfer is considered a surgical option for treatment in patients with chronic supraspinatus and infraspinatus tendon tears. Preoperative subscapularis function is necessary for good clinical results. Additionally, men with active elevation to shoulder level and active external rotation to 20 degrees have predictably good results. Women with active shoulder elevation limited to below chest level have poor results from this procedure and should not be considered candidates. Postoperatively they lack pain control, active elevation, and active external rotation. Muscular atrophy in the latissimus dorsi does not occur, and glenohumeral arthritic changes frequently develop postoperatively. Gerber C, Maquieira G, Espinosa N: Latissimus dorsi transfer for the treatment of irreparable rotator cuff tears: Factors affecting outcome. J Bone Joint Surg Am 2006;88:113-120.
Question 51
A 4-year-old boy with arthrogryposis has little active motion of his knees or elbows. Both elbows are in full extension with good triceps strength, but he is unable to bring his hand to his face or feed himself. Management should consist of
Explanation
Elbow release and triceps transfer to restore motion can be performed in children who are age 4 years and older. The ability to flex the elbow either actively or passively is of great assistance in activities of daily living. Van Heest A, Waters PM, Simmons BP: Surgical treatment of arthrogrypsosis of the elbow. J Hand Surg Am 1998;23:1063-1070.
Question 52
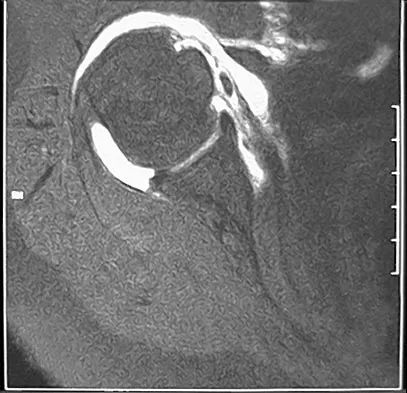
Figure 20 shows the MRI scan of a 20-year-old athlete who has a painful shoulder. This pathology is most commonly seen in
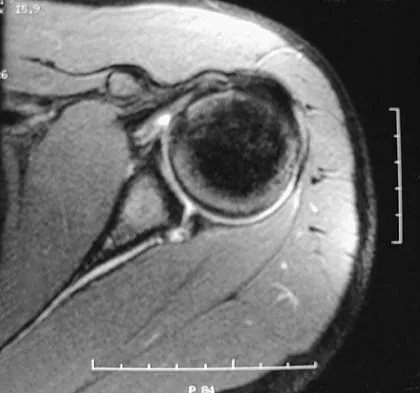
Explanation
The MRI scan reveals a posterior labral detachment. This injury is the result of a posteriorly directed force and is common to football players in blocking positions. Although this injury can occur with trauma in all types of athletes, it is seen with relative frequency in football. Treatment is aimed at labral repair with posterior capsulorrhaphy. Both open and arthroscopic techniques can be used. Misamore GW, Facibene WA: Posterior capsulorrhaphy for the treatment of traumatic recurrent posterior subluxations of the shoulder in athletes. J Shoulder Elbow Surg 2000;9:403-408.
Question 53
Which of the following conditions is not associated with an increased risk of developing Achilles tendinopathy?
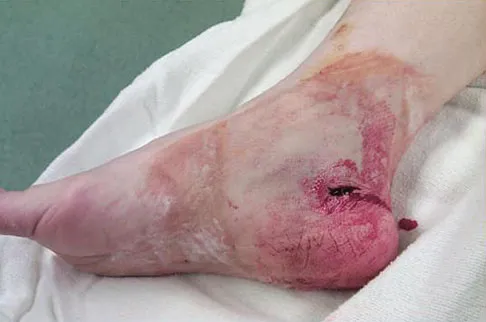
Explanation
Diabetes mellitus, obesity, and exposure to steroids have all been associated with the development of Achilles tendinopathy. In addition, Achilles tendinopathy has been associated with a history of hormone replacement therapy and the use of oral contraceptives. Quinolone antibiotics have also been linked to Achilles tendinopathy. Holmes GB, Lin J: Etiologic factors associated with symptomatic Achilles tendinopathy. Foot Ankle Int 2006;27:952-959.
Question 54
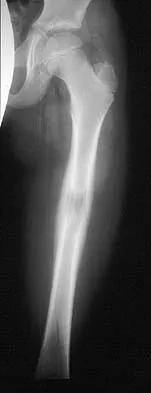
An active 72-year-old woman sustained a mid-diaphyseal right humerus fracture 16 months ago. History reveals that she was first treated with a brace for 7 months. Additional treatment consisted of intramedullary nailing 9 months ago. Recently the rod was removed, and the patient now reports pain and gross motion at the fracture site. Current radiographs are shown in Figures 37a and 37b. What is the next most appropriate step in management?
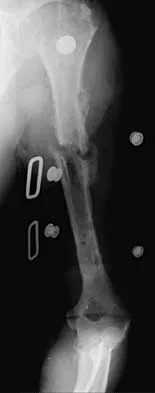
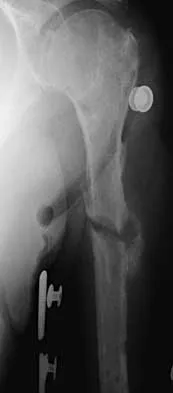
Explanation
The patient has a well-established nonunion in a very porotic bone. Electrical stimulation has been found effective in treating tibial nonunions, but there is very little data on humeral nonunions, especially chronic well-established ones. Ultrasound stimulation is effective in accelerating fracture healing, but there is little data concerning the treatment of nonunions. Intramedullary nailing with bone graft is an option, but it maybe difficult to obtain a rigid construct in a very porotic bone. An Ilizarov-type external fixator would be an alternative, but there is little clinical data for the humerus and it may be poorly tolerated. A plate and screw construct with bone graft combines rigidity with the biologic advantage of the bone graft. A recent series reported on the use of a plate combined with onlay allograft for recalitrant nonunions. Cement augmentation for screw fixation either in the canal or added to the screw holes may be helpful in select cases. Hornicek FJ, Zych GA, Hutson JJ, Malinin TI: Salvage of humeral nonunions with onlay bone plate allograft augmentation. Clin Orthop 2001;386:203-209.
Question 55
Radiographs of a 12-year-old boy who has knee pain show a 2-cm osteochondral lesion of the lateral aspect of the medial femoral condyle. The fragments are not detached from the femur. Initial management should consist of
Explanation
For a pediatric patient without mechanical symptoms, initial management of an osteochondral defect lesion that is not detached should consist of casting in flexion. Failure to respond to several weeks or months of nonsurgical management may warrant surgical treatment.
Question 56
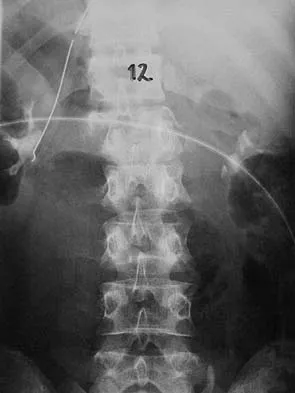
Figures 27a and 27b show the radiographs of a 32-year-old woman who was involved in a high-speed motor vehicle accident. She is neurologically intact. After stabilization and assessment, treatment should consist of
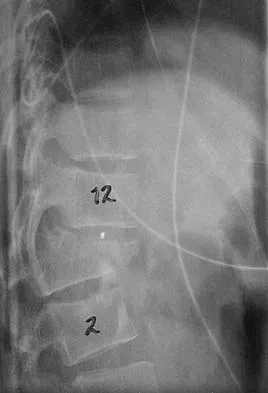
Explanation
The radiographs show a fracture-dislocation with translation in both the coronal and sagittal planes, evidence of significant instability requiring surgical stabilization. Anterior instrumentation is not as effective as posterior instrumentation in restoring stability, and because there is little bony destruction, the anterior column can be successfully reconstructed with simple realignment. The treatment of choice is multisegment posterior fusion with instrumentation. Lewandrowski KU, McLain RF: Thoracolumbar fractures: Evaluation, classification, and treatment, in Frymoyer JW, Wiesel SW (eds): The Adult and Pediatric Spine. Philadelphia, PA, Lippincott Williams and Wilkins, 2004, pp 817-843.
Question 57
A 3-year-old boy with severe cerebral palsy is unable to sit independently and does not crawl. Examination reveals a 40-degree hip flexion contracture by the Thomas test and 25 degrees of passive abduction. A radiograph of the pelvis shows subluxation of both hips, with a migration index of 30%. Management should consist of
Explanation
Progressive hip subluxation occurs in up to 50% of children with spastic quadriparesis. The subluxation is the result of chronic muscle hypertonicity, especially in the adductor muscle group. In time, the constant muscle tension will lead to dislocation, dysplastic changes in the acetabulum, and erosive changes in the cartilage of the femoral head. Many of these children will experience pain. Two recent studies have shown that early soft-tissue releases can successfully prevent progressive subluxation in children who are younger than age 4 years and who have a Reimers index (migration index) of less than 40%. Botulinum toxin A injections may reduce tone in the adductors for 4 to 6 months, but it is difficult to inject into the iliopsoas. Additionally, there are no long-term studies documenting the efficacy of botulinum toxin A to treat progressive hip subluxation in patients who have spastic quadriparesis. In general, proximal femoral osteotomy, combined with soft-tissue release as necessary, is indicated in older children (older than age 4 years) with progressive subluxation. Although selective dorsal rhizotomy has been used in nonambulatory patients, outcomes are less well documented than in ambulatory patients. There are no studies documenting the effect of selective dorsal rhizotomy on progressive hip subluxation in nonambulatory children. Miller F, Cardoso Dias R, Dabney KW, et al: Soft-tissue release for spastic hip subluxation in cerebral palsy. J Pediatr Orthop 1997;17:571-584.
Question 58
Of the following factors, which is considered the most important prognostic indicator in soft-tissue sarcomas?
Explanation
Histologic grade, the presence or absence of metastatic disease, and tumor size are important prognostic factors. Of the available choices, however, the size of the sarcoma is the most important prognostic indicator. A tumor size of greater than 5 cm is a more important prognostic factor than tumor location. Patients with sarcomas that measure 5 cm or less have nearly identical 3-year survival rates regardless of whether the tumor is subcutaneous or deep. Histologic grade (high versus low) is an important factor. However, histologic subtype frequently is not as important a factor as tumor size.
Question 59
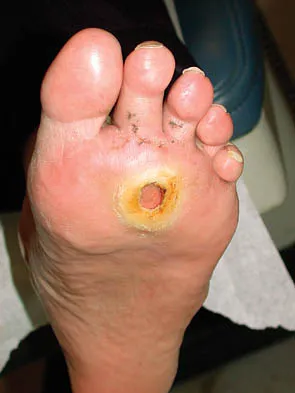
Figure 20 shows the clinical photograph of a man who has had diabetes mellitus controlled with oral medication for the past 10 years. He wears soft-soled shoes and only uses leather-soled shoes for important business meetings. Examination reveals palpable dorsalis pedis and posterior tibial pulses, although they are somewhat diminished. He is insensate to pressure with the Semmes-Weinstein 5.07 monofilament. The ulcer heals after treatment with a full contact cast. What is the best course of action at this time?
Explanation
The patient has not undergone a trial of foot-specific patient education and accommodative/therapeutic shoe wear. He must use therapeutic shoe wear at all times, as even the occasional use of pressure-concentrating shoe wear has a high likelihood of leading to the development of a diabetic foot ulcer. Pinzur MS, Kernan-Schroeder D, Emmanuele NV, et al: Development of a nurse-provided health system strategy for diabetic foot care. Foot Ank Int 2001;22:744-746. Pinzur MS, Shields N, Goelitz B, et al: American Orthopaedic Foot & Ankle Society shoe survey of diabetic patients. Foot & Ankle Int 1999;20:703-707.
Question 60
High Yield
A 16-year-old girl was involved in a motorcycle accident that resulted in a significant right tibial fracture with soft-tissue loss over the distal 4 cm of the anterior medial tibia. The patient has had two irrigations and debridements and recently had an intramedullary nail placed for the skeletal injury. Vacuum-assisted closure (VAC) has been used to cover the defect since the injury. The risk of infection developing in the tibia is
Detailed Explanation
The risk of infection in a 3B open tibia fracture is most directly related to the timing of the soft-tissue coverage and less related to the size or location of the wound. The wound VAC does not lower or raise the risk of infection in open fractures. It does appear to increase the window of time to obtain coverage without increasing the risk of infection. Additionally, the wound VAC may decrease the probability of needing free tissue coverage. Intramedullary nailing has not been shown to lower the risk of infection in 3B fractures. Godina M: Early microsurgical reconstruction of complex trauma of the extremities. Plast Reconstr Surg 1986;78:285-292. Dedmond BT, Kortesis B, Punger K, et al: The use of negative-pressure wound therapy (NPWT) in the temporary treatment of soft-tissue injuries associated with high-energy open tibia shaft fractures. J Orthop Trauma 2007;21:11-17.
Question 61
A study is conducted to measure the difference in bone mineral density between postmenopausal women taking a drug treatment versus those taking a placebo. What is the most important result to be reported from this study?
Explanation
A complete answer necessarily includes the means and standard deviations of bone mineral density in both groups. Given these, which are the basic results of the study, the P-value can be calculated if desired. All of the other options preclude assessment of the actual data, that is, the information collected by the study. P-values and confidence intervals should be perceived as additional information, which help to assess the certainty of relating the study's findings to the general population, but they should not be reported instead of the results (ie, the means and standard deviations).
Question 62
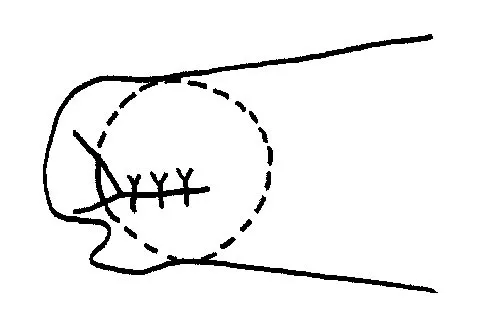
Initial repair of the large U-shaped rotator cuff tear shown in Figure 12 consists of closing the tear side-to-side to take advantage of margin convergence. The most significant biomechanical consequence of this repair step results in
Explanation
Margin convergence refers to the phenomenon that occurs with side-to-side closure of large U- or L-shaped rotator cuff tears in which the free margin of the tear converges toward the greater tuberosity as the side-to-side tear progresses. The creation of the converged cuff margin creates decreased strain in the free margin of the repaired cuff, resulting in a decreased strain in the repair sutures. While the size of the humeral head defect is made smaller with side-to-side closure, biomechanically, this is less significant. The mild increase in thickness of the repair at the side-to-side margin is less important than a reduction in stress in the repaired tissue. Stress in the crescent cable region of the cuff actually increases and becomes more physiologic in transmitting force from the cuff to the greater tuberosity. Burkhart SS: A stepwise approach to arthroscopic rotator cuff repair based on biomechanical principles. Arthroscopy 2000;16:82-90.
Question 63
A 45-year-old man has had left thigh pain for the past 4 months. An AP radiograph, bone scan, MRI scans, and biopsy specimens are shown in Figures 6a through 6f. What is the most appropriate treatment?
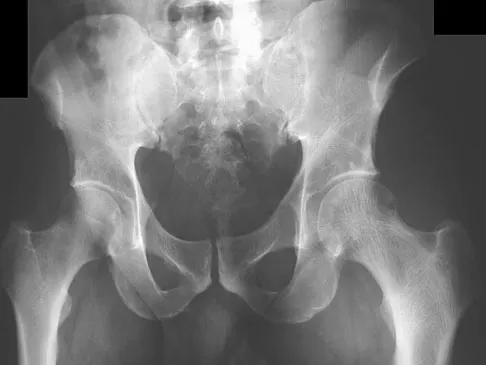
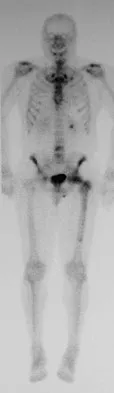
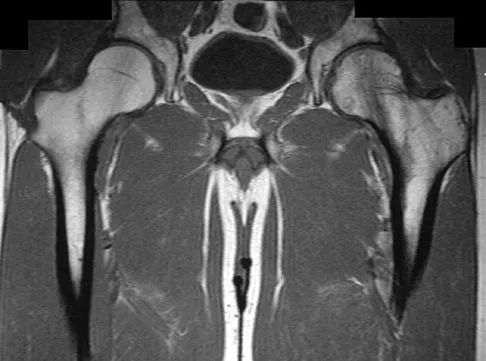
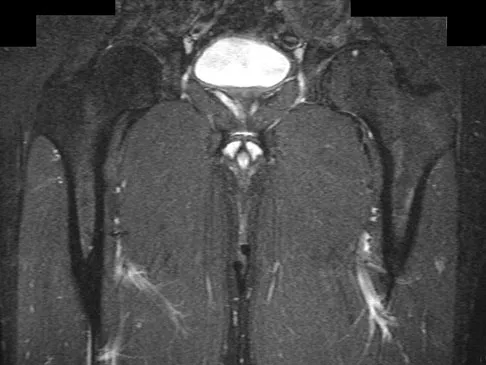
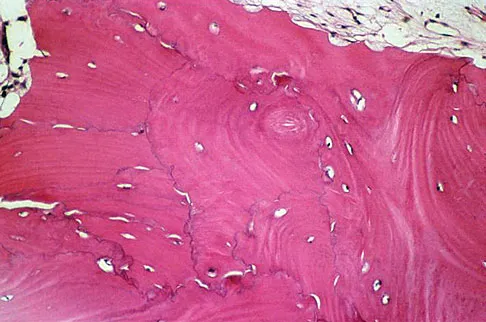
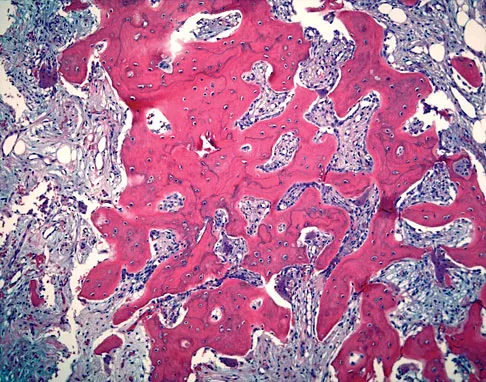
Explanation
The radiograph demonstrates thickened trabeculae and thickened cortices in the left proximal femur compared to the right, and the bone scan shows increased uptake in this area. The MRI scans show thickened trabeculae with normal marrow signal. These findings are diagnostic of Paget's disease. Medical treatment, including bisphosphonates and calcitonin, is indicated for painful bone lesions. Hadjipavlou AG, Gaitanis IN, Kontakis GM: Paget's disease of the bone and its management. J Bone Joint Surg Br 2002;84:160-169.
Question 64
A 14-year-old football player has had right knee pain for the past 2 months; however, he denies any history of trauma. Examination shows an abductor lurch and increased external rotation of the right lower extremity. The best course of action should be to
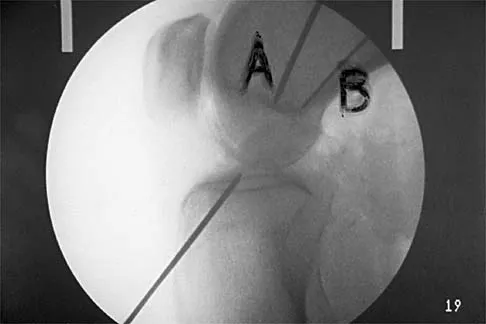
Explanation
Slipped capital femoral epiphysis is the most common pathology involving the hip in adolescents. While patients with acute slips may report severe pain and are unable to ambulate, those with chronic slips often have pain during ambulation, a limp, and increased external rotation of the hip. While 60% of the patients specifically report hip pain, the remainder have pain in the thigh or knee. The initial diagnostic study of choice is AP and frog-lateral radiographs of the pelvis; bilateral involvement is frequently seen. Boyer DW, Mickelson MR, Ponseti IV: Slipped capital femoral epiphysis: Long-term follow-up study of one hundred and twenty-one patients. J Bone Joint Surg Am 1981;63:85-95.
Question 65
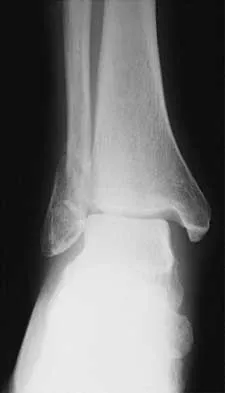
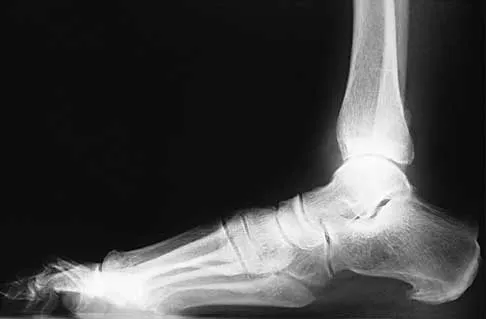
A 57-year-old man has had right ankle pain for the past 10 months following an injury that went untreated. Radiographs are shown in Figures 30a through 30c. Management should consist of
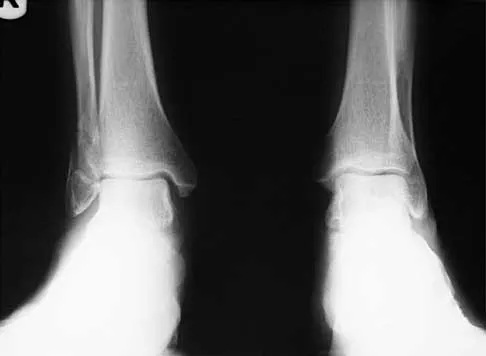
Explanation
The radiographs reveal a malunited distal fibular fracture with shortening. Because there appears to be an adequate cartilage space within the ankle joint, the role of reconstruction would be to prevent arthrosis and the need for ankle arthrodesis, as well as to decrease symptoms. The treatment of choice is restoration of fibular length, alignment, and rotation with osteotomy plating, and bone grafting as needed. There is no indication for ligament reconstruction of a mechanically stable ankle, and tibial shortening osteotomy will not assist in correcting the deformity. Cast immobilization may assist with improvement of symptoms but will not correct the overall process. Determination of fibular length is best done by comparing the talocrural angle of the injured side with the uninjured side. The goal is to perfectly reduce the talus in the ankle mortise. Marti RK, Raaymakers EL, Nolte PA: Malunited ankle fractures: The late results of reconstruction. J Bone Joint Surg Br 1990;72:709-713. Geissler W, Tsao A, Hughes J: Fractures and injuries of the ankle, in Rockwood CA Jr, Green DP, Bucholz RW, Heckman JD (eds): Rockwood and Green's Fractures in Adults, ed 4. Philadelphia, PA, Lippincott-Raven, 1996, pp 2201-2206.
Question 66
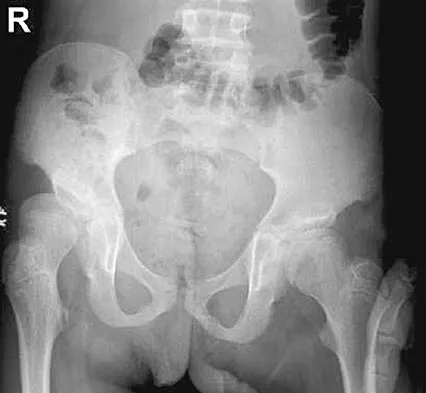
The parents of a 13-year-old boy with Down syndrome report that he has an increasing limp and decreased endurance with activities. Lateral flexion-extension radiographs of the cervical spine show no evidence of instability. Examination reveals a right Trendelenburg limp and an obvious limb-length discrepancy. Hip motion is symmetric except for some decreased abduction on the right side. A standing AP radiograph is shown in Figure 20. Management should consist of
Explanation
Ligamentous laxity and muscle hypotonia seen in Down syndrome contribute to the incidence of hip subluxation and dislocation. These factors can be progressive and lead to degenerative arthritis in adults with Down syndrome. Because this patient has a progressive limp and decreased endurance, observation and a shoe lift are not options. Bracing may be an option in the younger child before significant bony changes occur. Surgical intervention is the treatment of choice in this patient; however, all components of the deformity need to be addressed. Because of the increased capsular laxity, there is a high likelihood of recurrence if capsulorrhaphy is not included with the pelvic and femoral osteotomies. Surgery in these patients is associated with a high rate of complications. Shaw ED, Beals RK: The hip joint in Down's syndrome: A study of its structure and associated disease. Clin Orthop 1992;278:101-107. Aprin H, Zinc WP, Hall JE: Management of dislocation of the hip in Down's syndrome. J Pediatr Orthop 1985;5:428-431.
Question 67
A 75-year-old patient returns for follow-up after undergoing bilateral total hip arthroplasty (THA). The right hip is a hybrid THA performed 12 years ago, whereas the left hip is a cementless THA performed 10 years ago. Both acetabular components are the same type, same size, and from the same manufacturer. Both femoral heads are 28-mm cobalt-chromium components. What is the most likely explanation for the advanced polyethylene wear in one hip?
Explanation
Over the past three decades, gamma irradiation and air has been the most common method of sterilizing polyethylene used in total joint arthroplasty. This method of sterilization results in breakage of the chemical bonds within the polymer. While this promotes cross-linking, it also leaves the polyethylene vulnerable to oxidation, especially if packaged in an air environment. Oxidation has been shown to decrease polyethylene's molecular weight, ultimate tensile strength, elongation, and toughness which results in a stiffer, more brittle material that is less resistant to wear. Severity of oxidation and a decrease in mechanical properties have been shown to be related to the length of time that the component is exposed to air (the shelf life). Currier and associates studied the clinical performance of gamma irradiated in air polyethylene components that had been shelf aged. They demonstrated that for the first 5 years of shelf life, polyethylene oxidized rather slowly. However, polyethylene components with a shelf life of more than 5 years would be expected to have minimal mechanical toughness and would likely fail rapidly if implanted. Bohl and associates evaluated 135 patients who had undergone total knee arthroplasty. Survivorship at 5 years was 100% for components with a shelf life of less than 4 years, 89% for components with a shelf life of 4 to 8 years, and 79% for components with a shelf life of more than 8 years. Sychterz and associates reported no correlation between shelf life and true wear rates for components with a shelf life of less than 3 years. In summary, both in vivo and in vitro data suggest that shelf life in excess of 3 to 5 years has a direct effect on wear of polyethylene. Currier BH, Currier JH, Collier JP, et al: Shelf life and in vivo duration: Impacts on performance of tibial bearings. Clin Orthop 1997;342:111-122. Bohl JR, Bohl WR, Postak PD, et al: The Coventry Award: The effects of shelf life on clinical outcome for gamma sterilized polyethylene tibial components. Clin Orthop 1999;367:28-38.
Question 68
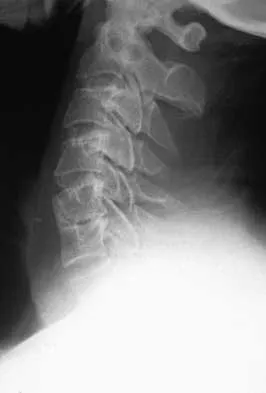
A patient underwent an anterior cervical diskectomy and interbody fusion for a C5-6 herniated nucleus pulposus and left C6 radiculopathy 8 months ago. He now reports new onset of severe neck pain and left C6 radicular pain, with wrist extension weakness. The radiograph and CT scan shown in Figures 26a and 26b reveal pseudarthrosis at C5-6. The next step in management should consist of
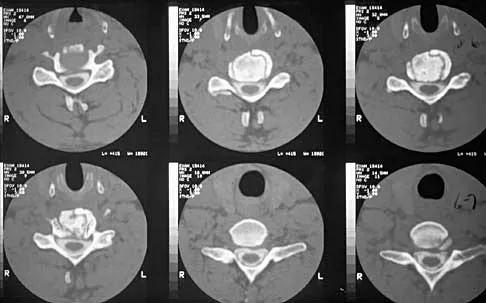
Explanation
Brodsky and associates reviewed 34 cases of cervical pseudarthrosis after anterior fusion. Seventeen were treated with revision anterior fusion and 17 with posterior foraminotomy and fusion. Good results were seen in 75% of patients who underwent revision anterior surgery, but better results (94%) were seen with posterior surgery, including foraminotomy and stabilization. Tribus and associates reported treatment of 16 patients with pseudarthrosis using revision anterior debridement of the fibrous tissue and fusion with autograft and plates. There was improvement of the neck in 75% of the patients, nonunion in 19%, continued weakness in 28%, and dysphagia in 5%. Farey and associates reported on 19 patients treated with posterior foraminotomy, stabilization, and fusion with a fusion rate of 100%, resolution of arm pain in 94%, resolution of weakness in 100%, and resolution of neck pain in 75%. It would appear that posterior foraminotomy is more effective for relieving arm pain and neurologic deficits associated with pseudarthrosis. Posterior fusion has the most reliable rate of arthrodesis in this setting. Dysphagia is reported in some patients undergoing more extensive anterior dissections required for applying plates. A neck brace is unlikely to aid in healing of pseudarthrosis in a patient who underwent surgery 8 months ago. A neck brace would be most effective within the first 3 months if a delayed union is identified. Brodsky AE, Khalil MA, Sassard WR, Neuman BP: Repair of symptomatic pseudarthrosis of anterior cervical fusion: Posterior versus anterior repair. Spine 1992;17:1137-1143. Tribus CB, Corteen DP, Zdeblick TA: The efficacy of anterior cervical plating in the management of symptomatic pseudarthrosis of the cervical spine. Spine 1999;24:860-864.
Question 69
A patient with a cobalt-chromium alloy (Co-Cr) femoral stem has a periprosthetic fracture that is to be fixed with a cable-plate device. The surgeon should make sure that the plate, screws, and cable, respectively, are made of
Explanation
Contact between metals in a biologic environment leads to galvanic corrosion. Reduction potentials of Co-Cr and stainless steel produce the worst combination of metals in commonly used implants. Because the fixation implants are not intended to contact the existing implant, it is not as great a consideration as the plate and the screws and cables that will directly contact each other. Miller MD (ed): Review of Orthopaedics, ed 3. Philadelphia, PA, WB Saunders, 2000, pp 119-144.
Question 70
The additional risk of complications in organ transplant patients receiving a total joint arthroplasty is attributed to
Explanation
Tannenbaum and associates found that patients who had a joint replacement after an organ transplantation had a rate of infection of 19% (five of 27 joint replacements in 16 patients). They retrospectively reviewed the results of 35 joint (hip or knee) replacements in 19 patients who had an organ transplant. The patients received a standard immunosuppressive induction regimen at the time of the transplantation and were maintained on a combination of prednisone, azathioprine, and cyclosporin A. All patients received antibiotics perioperatively, but antibiotic-impregnated bone cement was not used for any procedure. Six joint replacements in three patients (median patient age of 48.2 years at the time of the arthroplasty) were performed before a renal transplantation. Twenty-four joint replacements in 14 patients (average patient age of 40.9 years at the time of the arthroplasty) were performed after an organ transplantation. Two patients, with an average age of 53.8 years at the time of the arthroplasty, each had a joint replacement both before and after a liver transplantation (a total of five joint replacements). The average duration of follow-up after the first joint replacement was 8.8 years (range, 1 to 23 years). An infection developed around the implant in five patients who had undergone the joint replacement after a transplantation. The average interval from implantation of the prosthesis until detection of the infection was 3.4 years (range, 1 to 6 years). Of two patients who underwent a liver transplant, one had Pseudomonas aeruginosa infection and the other Escherichia coli infection. Of three patients who underwent a renal transplantation, one was infected with Staphylococcus epidermidis, one with Enterococcus, and one with Serratia marcescens.
Question 71
During an anterior retroperitoneal approach to the low lumbar spine, the iliac vessels are mobilized along the lateral side, allowing them to be retracted toward the midline. To gain adequate mobility of the common iliac vein for exposure of L5, it is important to identify which of the following structures?
Explanation
The iliolumbar vein is a large tributary that sits along the lateral surface of the common iliac vein. It can be quite substantial in size and must be identified prior to mobilizing the common iliac vein toward the midline. The other structures are not of surgical significance in performing this exposure.
Question 72
The vascular supply to the medial meniscus comes primarily from what artery?
Explanation
The vascular supply to the medial and lateral menisci originates predominantly from the medial and lateral genicular arteries. The popliteal artery splits into the superior genicular, which splits into medial and lateral branches supplying the patellar cartilage and the posterior cruciate ligament. The middle genicular artery also supplies the anterior curciate ligament, posterior cruciate ligament, and collateral ligaments. The inferior genicular splits into medial and lateral branches and supplies the menisci and other knee ligaments. Despite propagation of incorrect terminology, there is no superior or lateral genicular artery.
Question 73
A football player sustains a traumatic anterior inferior dislocation of the shoulder in the last game of the season. It is reduced 20 minutes later in the locker room. The patient is neurologically intact and has regained motion. If the patient undergoes arthroscopic evaluation, what finding is seen most consistently?
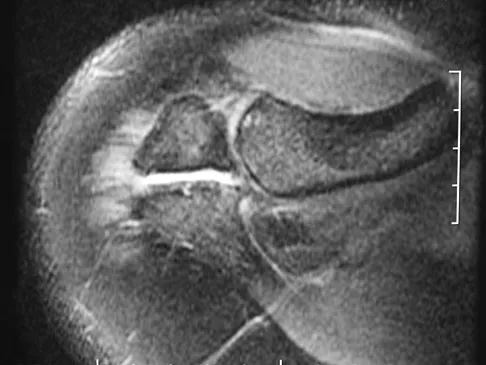
Explanation
In an acute first-time dislocation, arthroscopy has been shown to reveal a Bankart lesion in most shoulders. The classic finding of labral detachment from the anterior inferior glenoid along with occasional hemorrhage within the inferior glenohumeral ligament is the most common sequelae of a traumatic anterior inferior dislocation. Acute treatment, if chosen, is repair of the labral tissue back to the glenoid plus or minus any capsular plication to address potential plastic deformation of the glenohumeral ligament. Acute treatment of a patient sustaining a first-time dislocation remains controversial. The potential indications may be patients whose dislocation occurs at the end of a season and when the desire to minimize risk of future instability outweighs the risks of surgical intervention. Taylor DC, Arciero RA: Pathologic changes associated with shoulder dislocations: Arthroscopic and physical examination findings in first-time, traumatic anterior dislocations. Am J Sports Med 1997;25:306-311. DeBerardino TM, Arciero RA, Taylor DC, et al: Prospective evaluation of arthroscopic stabilization of acute, initial anterior shoulder dislocations in young athletes: Two- to five-year follow-up. Am J Sports Med 2001;29:586-592.
Question 74
What is the heaviest weight that can be safely applied to the adult cervical spine via Gardner-Wells tong traction?
Explanation
Cotler and associates reported on the use of awake skeletal traction to reduce facet fracture-dislocations in 24 patients. Seventeen patients required more than 50 pounds of traction (the "traditional" limit) to achieve reduction. More than 100 pounds of traction was safely used in one-third of the patients in this study. A cadaver study has supported the safe use of traction with weights in excess of 100 pounds. Cotler JM, Herbison GJ, Nasuti JF, et al: Closed reduction of traumatic cervical spine dislocation using traction weights up to 140 pounds. Spine 1993;18:386-390.
Question 75
Figures 10a through 10c show the plain radiograph and MRI scans of a 41-year-old man who has right hip pain. What is the most likely diagnosis?
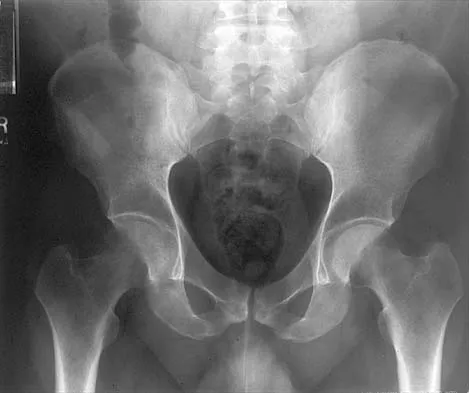
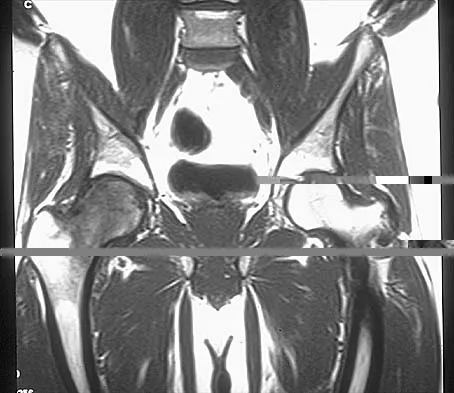
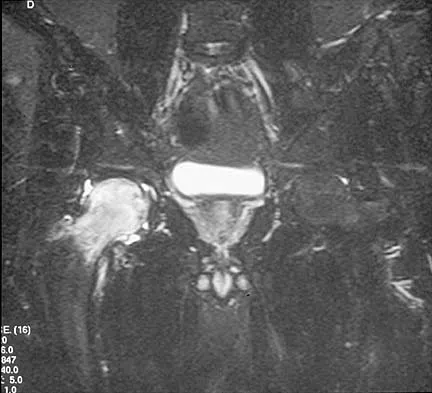
Explanation
Transient osteoporosis is a self-limited painful but reversible disorder. Although first described in pregnant women, it is more common in young to middle-aged men. The radiograph shows loss of mineralization in the right hip relative to the left side. There is no osseous destruction or cortical expansion typical of metastasis or giant cell tumor. The process is confined to the femoral side of the joint unlike rheumatoid arthritis, which would be centered in the joint. Osteonecrosis is better defined with sharp but irregularly shaped margins, and there is no double-line sign. The MRI scans reveal diffuse edema in the femoral head and neck that is atypical for osteonecrosis. Transient osteoporosis may recur in the same or opposite hip.
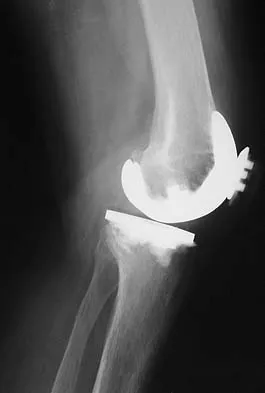
Question 76
Flexion-distraction injuries of the thoracolumbar spine are most frequently associated with injury to what organ system?
Explanation
In patients with flexion-distraction injuries of the thoracolumbar spine, 50% have associated, potentially life-threatening, visceral injuries that occasionally are diagnosed hours or even days after admission. Based on these findings, consultation with a general surgeon is recommended. Blunt and penetrating injuries to the cardiopulmonary system or aorta sometimes can be seen with this type of injury, but they are no more common than with other types of thoracolumbar fractures because of the relatively mild bony injury anteriorly. Neurologic trauma with this type of fracture is also somewhat rare. Levine AM (ed): Orthopaedic Knowledge Update: Trauma. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1996, pp 351-360.
Question 77
The natural history of cervical spondylolytic myelopathy is best described as
Explanation
The natural history of cervical myelopathy has been described by Lees and Turner as exacerbations of symptoms followed by often long periods of static or deteriorating function (or very rarely improvement). This stepwise pattern of decreasing function has been corroborated by Clarke and Robinson. These authors described long periods of stable neurologic function, sometimes lasting for years, in about 75% of their patients. In the majority of the patients, however, the condition deteriorated between quiescent streaks. About 20% of their patients showed a slow, steady progression of symptoms and signs without a stable period, and 5% had rapid deterioration of neurologic function. Emery SF: Cervical spondylotic myelopathy: Diagnosis and treatment. J Am Acad Orthop Surg 2001;9:376-388. Lees F, Turner JA: The natural history and prognosis of cervical spondylosis. Brit Med J 1963;2:1607-1610.
Question 78
A patient who underwent closed reduction of the hips as an infant now reports pain. An abduction internal rotation view shows an incongruous joint. Based on the findings shown in Figure 3, what is the most appropriate type of pelvic osteotomy for the right hip?
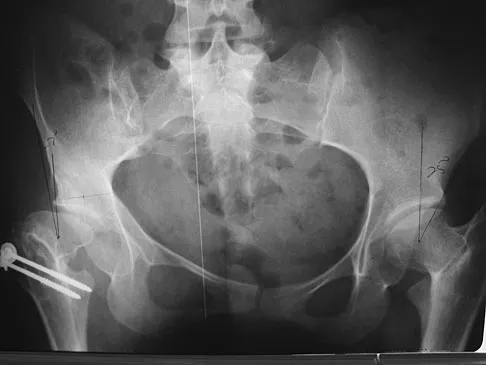
Explanation
Pelvic osteotomies that redirect hyaline cartilage over the femoral head offer the potential for long-term preservation of the hip; however, salvage procedures such as the Chiari osteotomy are indicated in patients without a concentrically reducible hip. Ito and associates reported that moderate dysplasia and moderate subluxation without complete obliteration of the joint space and a preoperative center-edge angle of at least minus 10 degrees are desirable selection criteria. Ohashi H, Hirohashi K, Yamano Y: Factors influencing the outcome of Chiari pelvic osteotomy: A long-term follow-up. J Bone Joint Surg Br 2000;82:517-525.
Question 79
Figure 20 shows the radiograph of a 21-year-old college basketball player who jammed his left index finger on the rim. He reports pain and tenderness over the dorsum of the distal interphalangeal (DIP) joint. Examination reveals that he is unable to actively extend the DIP joint; however, the skin is intact. Management should consist of
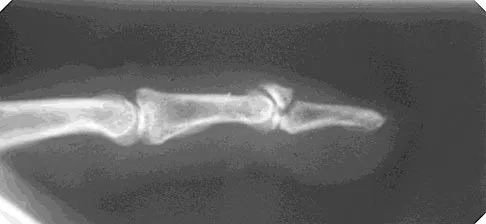
Explanation
Mallet fingers without DIP joint subluxation can be treated with extension splinting. Surgical fixation may be necessary in bony mallet injuries when the joint is subluxated. Size of the bony fragment, while often correlating with stability, is not always an indication for fixation. Buddy taping allows motion; therefore, the fragment will not heal in the appropriate position. Intermittent splinting with range-of-motion exercises also will not allow the fragment to heal in the appropriate position. Crawford GP: The molded polyethylene splint for mallet finger deformities. J Hand Surg Am 1984;9:231-237.
Question 80
Which of the following is considered the most common complication of the impaction grafting technique for femoral revision surgery?
Explanation
Impaction grafting technique for femoral revision surgery has become increasingly popular over the past decade. This technique is designed to address cavitary deficiencies of the femur. The femoral stem is inserted with cement fixation. Its clinical efficacy has not been shown to be superior to extensively porous-coated stems. Early subsidence of the stem has been reported in more than 50% of the patients. However, loss of fixation has occurred infrequently (5%) in reported series conducted by experienced surgeons. It has not been shown to have a higher infection rate. Gie GA, Linder L, Ling RS, Simon JP, Slooff TH, Timperley AJ: Impacted cancellous allografts and cement for revision total hip arthroplasty. J Bone Joint Surg Br 1993;75:14-21.
Question 81
Figures 28a and 28b show the sagittal and axial lumbar MRI scans of a 72-year-old man who reports dull aching back pain that spreads to his legs, calves, and buttocks. He has had the pain for several years and it is precipitated by standing and walking and relieved by sitting. His symptoms have been worsening over the past year and he notes that he is leaning forward while walking to help relieve his symptoms. He has had no treatment to date. What is his prognosis if he chooses to pursue nonsurgical management for this condition?
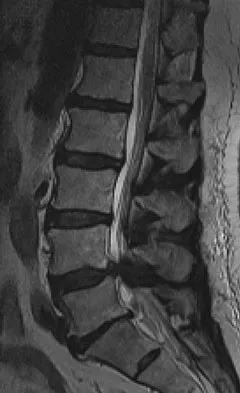
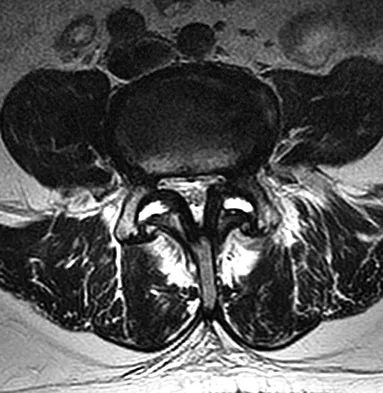
Explanation
The patient has lumbar spinal stenosis and the MRI scans reveal the pathology at L4-5, which is secondary to posterior disk bulging and hypertrophy and infolding of the ligamentum flavum, as well as degenerative facet arthrosis. The degree of spinal stenosis is moderate and his symptoms are positional in nature. Tadokoro and associates reported on a prospective study of 89 patients older than 70 years of age who underwent nonsurgical management for lumbar spinal stenosis. They found the prognosis to be relatively good with patients scoring at "excellent" or "good" for activities of daily living at final follow-up. However, they did note that patients with a complete block on myelography did not respond favorably to nonsurgical management. Amundsen and associates reported on a 10-year prospective study comparing surgical care to nonsurgical management. They concluded that, while the long-term results largely favored surgical treatment, more than half of the nonsurgically managed patients had a satisfactory outcome. They also concluded that a delay of surgery for some months did not worsen the prognosis. Therefore, their recommendation was for an initial primarily nonsurgical approach. Amundsen T, Weber H, Nordal HJ, et al: Lumbar spinal stenosis: Conservative or surgical management? A prospective 10-year study. Spine 2000;25:1424-1435. Hilibrand AS, Rand N: Degenerative lumbar stenosis: Diagnosis and management. J Am Acad Orthop Surg 1999;7:239-249.
Question 82
A 17-year-old high school long distance runner is seeking advice before running a marathon for the first time. What advice should be given regarding his fluid, carbohydrate, and electrolyte intake around the time of the race?
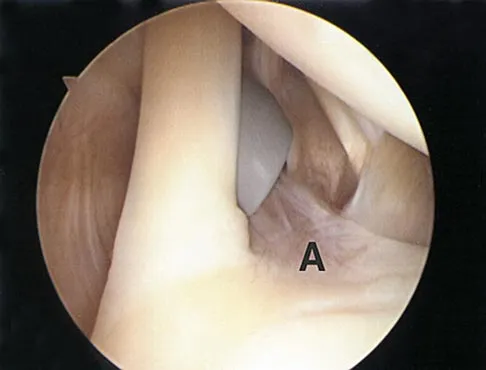
Explanation
The goal of fluid replenishment should be to replace the sweat that has been lost. Sweat is mostly water, with a small concentration of salts and other electrolytes. Absorption is enhanced by solutions of low osmolality. Scientific research has also shown that adding carbohydrates to the drink improves athletic performance. Carbohydrates such as glucose and maltodextrins (glucose polymers) stimulate fluid absorption by the intestines. Fructose slows intestinal absorption of fluids. Drinks that are high in fructose, such as orange juice, can lead to gastrointestinal distress and osmotic diarrhea. Kirkendall D: Fluids and electrolytes, in The U.S. Soccer Sports Medicine Book. Baltimore, MD, Williams and Wilkins, 1996.
Question 83
A 45-year-old man is seeking evaluation of an injury sustained in a motor vehicle accident 10 weeks ago. Current radiographs are shown in Figures 2a and 2b. Based on the radiographic findings, what is the most likely diagnosis?
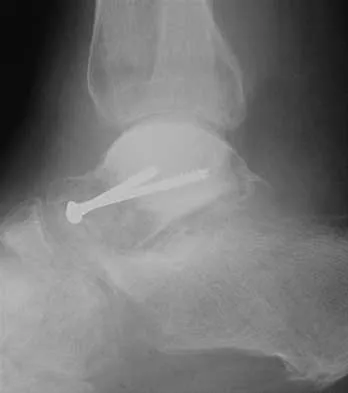
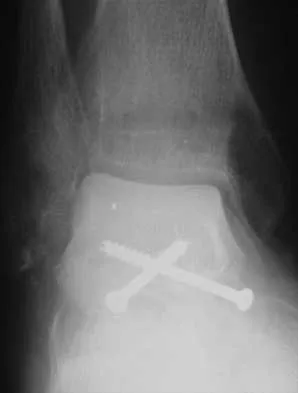
Explanation
An increased density of the talar body compared to the distal tibia following fracture of the talar neck is highly suggestive of vascular compromise of the talar body. Subchondral osteopenia of the talus at 6 to 8 weeks (Hawkins sign) is a favorable sign but does not eliminate the possibility of osteonecrosis. Elgafy H, Ebraheim NA, Tile M, Stephen D, Kase J: Fractures of the talus: Experience of two level 1 trauma centers. Foot Ankle Int 2000;21:1023-1029.
Question 84
An infant is born with a mass that involves both the volar and dorsal compartments of the left arm. A clinical photograph and biopsy specimen are shown in Figures 41a and 41b. What is the best initial course of action?
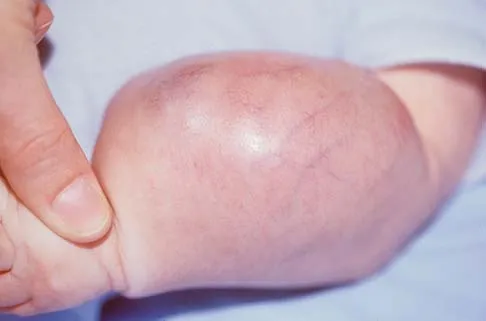
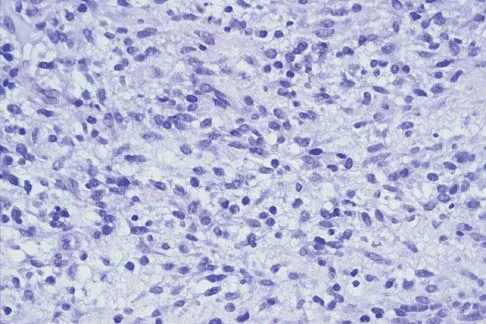
Explanation
The patient has infantile fibrosarcoma. For unresectable lesions, the treatment of choice is chemotherapy with vincristine, actinomycin-D, and cyclophosphamide, followed by excision if there is an adequate decrease in the size of the lesion.
Question 85
A 24-year-old man has had pain in the left knee for the past several months. He reports that initially the pain was associated with weight-bearing activities, but it has now become more constant. He denies any swelling but reports a lateral fullness at the tibial plateau. Figures 23a through 23e show radiographs, a bone scan, and T1- and T2-weighted MRI scans. What is the most likely diagnosis?
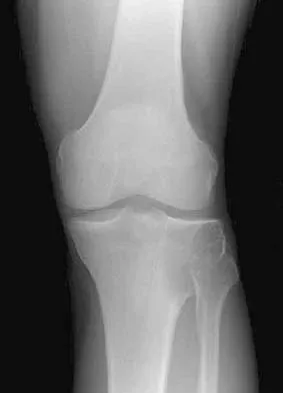
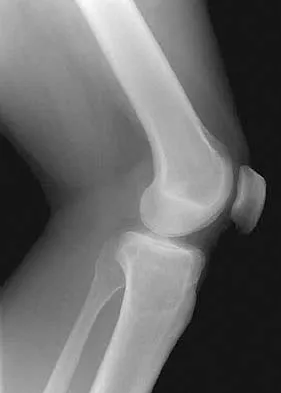
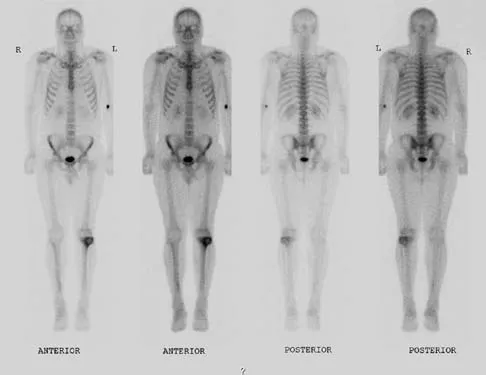
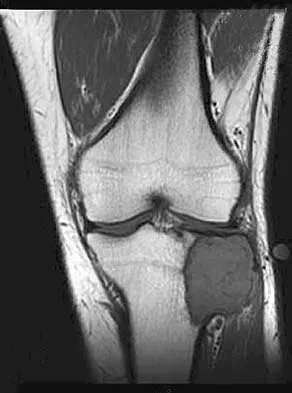
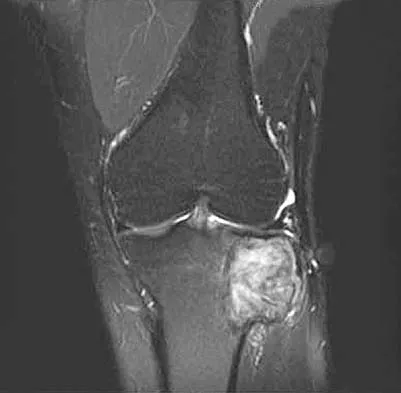
Explanation
The radiographs reveal a lytic subchondral lesion that has a poorly defined margin and lacks mineralization. The bone scan confirms an active lesion that has central photopenia, producing the characteristic doughnut configuration. The MRI scans confirm the presence of a subchondral lesion that is modestly expansile at the lateral plateau and has low signal intensity on the T1-weighted image and a mixed high signal on the T2-weighted image. These features strongly suggest giant cell tumor of bone, more than 50% of which appear around the knee. Simple cyst is excluded by the MRI characteristics. Fibrous dysplasia is unlikely to be in a subchondral location and typically does not show this intensity of uptake on bone scan. Parsons TW: Benign bone tumors, in Fitzgerald RH, Kaufer H, Malkani AL (eds): Orthopaedics. St Louis, MO, Mosby, 2002, pp 1027-1035.
Question 86
What normal tissue has a low signal intensity (appears black) on both T1- and T2-weighted images?
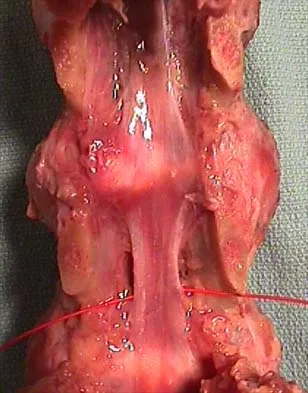
Explanation
Tendons, cortical bone, ligaments, menisci, and fibrous tissue will show low signal intensity (SI) on both T1- and T2-weighted images. Fat-containing tissues, such as subcutaneous fat and bone marrow, will show high SI on T1-weighted images and low SI on T2-weighted images. Tissues with high water content, such as joint fluid, intervertebral disk, and edema, will show low SI on T1-weighted images and high SI on T2-weighted images. Kasser JR (ed): Orthopaedic Knowledge Update 5. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1996, pp 65-70.
Question 87
When using the direct lateral (or Hardinge) approach for hip arthroplasty, three muscles are detached from the femur. In addition to the vastus lateralis, they include the
Explanation
This approach is criticized for the episodic limp associated with the muscle detachment and reattachment. Classically, two thirds of the gluteus medius is detached as a sleeve with the vastus lateralis. This exposes the gluteus minimus and the ligament of Bigelow. These must also be detached to allow dislocation of the hip and osteotomy of the femoral neck. The rectus femoris lies medially and anteriorly and does not need to be addressed. The piriformis and obturator internus are exposed during the posterior approach. Neither the gluteus maximus nor tensor fascia lata attach to the anterior femur. The sartorius and iliopsoas are not exposed during this dissection. Hoppenfeld S, deBoer P (eds): Surgical Exposures in Orthopaedics: The Anatomic Approach. Philadelphia, PA, JB Lippincott, 1984, pp 333-335.
Question 88
A 23-year-old man is involved in a motor vehicle accident. An AP radiograph is shown in Figure 29a, and axial and sagittal CT scans are shown in Figures 29b and 29c. Neurologic examination shows 1/5 strength of his quadriceps and iliopsoas on the right, with 1/5 quadriceps function on the left. Definitive treatment of his injury should consist of
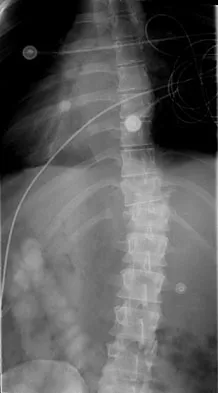
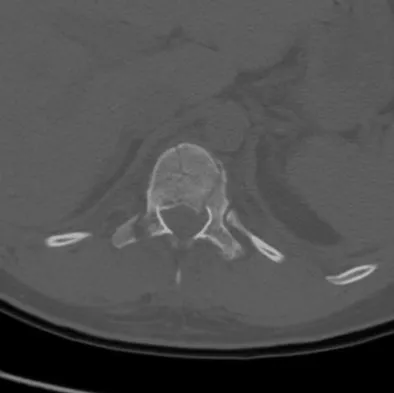
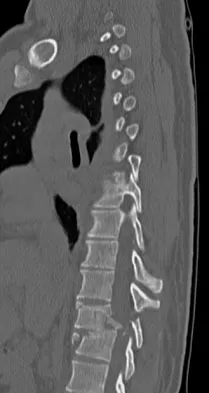
Explanation
The imaging studies show a fracture-dislocation. Surgical treatment of this injury consists of a decompression reduction, stabilization, and fusion. A posterolateral decompression can also be performed as necessary. An isolated anterior procedure in this type of injury is contraindicated. The anterior longitudinal ligament is most likely intact; therefore, an anterior procedure further destabilizes the spine. Reduction by an anterior approach would also be difficult. Nonsurgical management of the neurologic injury in this patient is not indicated. Theiss SM: Thoracolumbar and lumbar spine trauma, in Stannard JP, Schmidt AH, Kregor PJ (eds): Surgical Treatment of Orthopaedic Trauma. New York, NY, Thieme, 2007, pp 179-207.
Question 89
Figures 39a and 39b show the current radiographs of an 8-year-old girl who has had pain in the left thigh for the past 3 months. She was recently diagnosed with hypothyroidism and started treatment 1 week ago. Examination reveals a mild abductor deficiency limp on the left side. She lacks 30 degrees internal rotation on the left hip compared with the right hip. Management should consist of
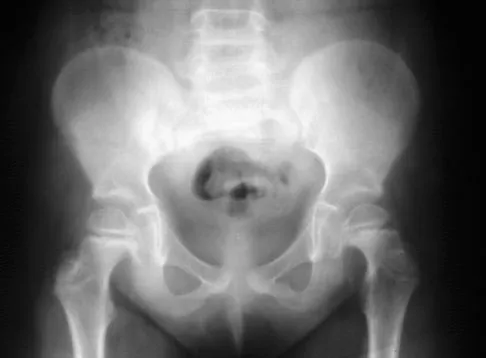
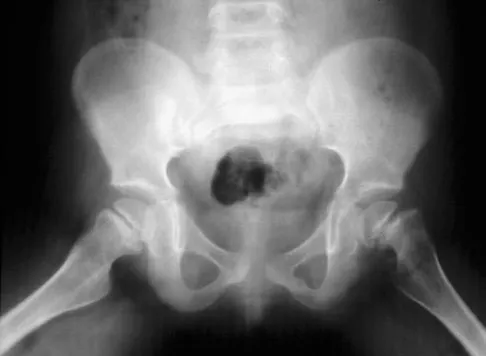
Explanation
The radiographs confirm a slipped capital femoral epiphysis of the left hip, as well as a widened growth plate on the contralateral hip. This is considered a stable slip because the patient is able to walk. Treatment options for stable slips include in situ pinning, bone graft epiphysiodesis, and in some centers severe slips are treated with primary osteotomy and epiphyseal fixation. Percutaneous in situ fixation is the most popular and widely used method of treatment. This juvenile patient has an endocrine condition and a widened growth plate on the right side; therefore, strong consideration should be given to pinning the contralateral hip "pre-slip." Muscle strengthening, hip spica casting, and closed reduction have no place in the primary treatment of a stable slipped capital femoral epiphysis. Loder RT, Richards BS, Shapiro PS, et al: Acute slipped capital femoral epiphysis: The importance of physeal stability. J Bone Joint Surg Am 1993;75:1134-1140. Loder R, Wittenberg B, DeSilva G: Slipped capital femoral epiphysis associated with endocrine disorders. J Pediatr Orthop 1995;15:349-356.
Question 90
A 52-year-old woman reports nagging shoulder pain that has been present for months and is slowly progressive in nature. The patient also reports nocturnal pain and notes that the pain is not activity related. Figures 27a and 27b show the radiograph and bone scan, and Figures 27c through 27e show T1-weighted, T2-weighted, and gadolinium MRI scans, respectively. Based on these findings, what is the most likely diagnosis?
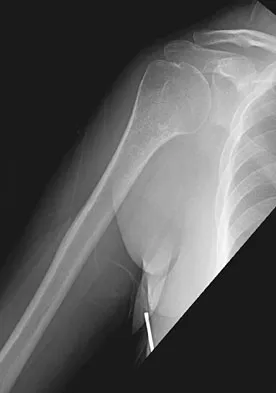
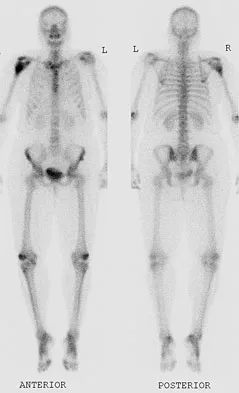
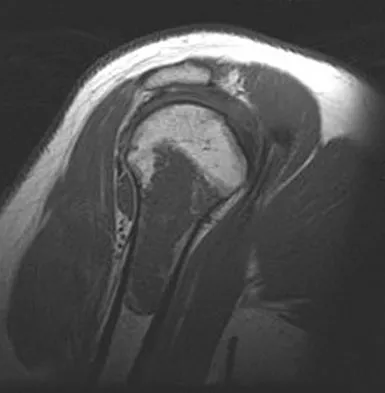
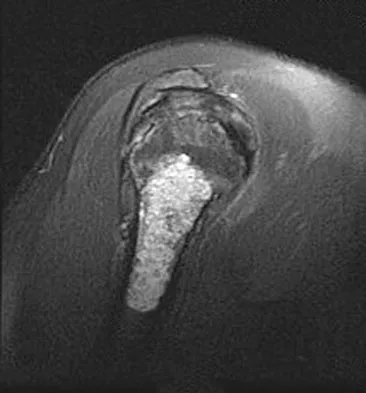
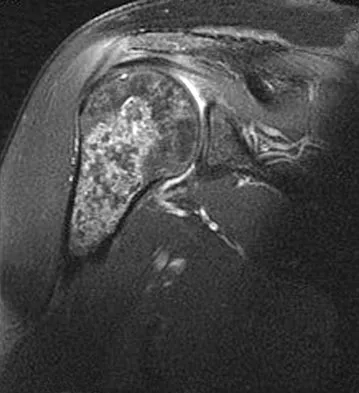
Explanation
The radiograph reveals a metaphyseal lesion with some stippled mineralization suggesting a chondroid tumor. The bone scan shows increased uptake, beyond what is expected for a simple enchondroma, and beyond the limits of the lesion. The MRI sequences shows a lobular lesion on the T1- and T2-weighted (bright on the T2 sequence) images with inhomogeneous uptake of gadolinium; both findings are typical for a chondroid lesion. The history of pain, the positive bone scan, the age of the patient, the size of the lesion, and the central location (enostotic) of the lesion all suggest a malignant cartilage tumor. The images are not consistent with the other diagnoses. In particular, plasmacytoma is more uniformly bright on T2-weighted images and often has a negative bone scan. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 187-194.
Question 91
Figure 42 shows the sagittal T2-weighted MRI scan of a patient's right knee. These findings are most commonly seen with a complete tear of the
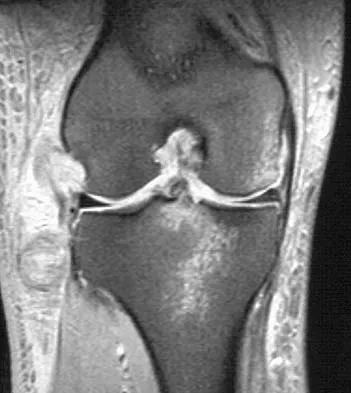
Explanation
The MRI scan reveals disruption of the lateral capsule and ligaments with fluid in the soft tissues laterally. Additionally, there is a large bone bruise on the medial femoral condyle. This combination indicates injury to the posterolateral complex. These injuries often have coexisting anterior and/or posterior cruciate ligament injuries. Failure to recognize the posterolateral corner injury can lead to failure of anterior or posterior cruciate ligament reconstructions. LaPrade RF, Gilbert TJ, Bollom TS, et al: The magnetic resonance imaging appearance of individual structures of the posterolateral knee: A prospective study of normal knees and knees with surgically verified grade III injuries. Am J Sports Med 2000;28:191-199.
Question 92
It is important to avoid which of the following exercises in the immediate postoperative period after humeral head replacement for an acute four-part fracture?
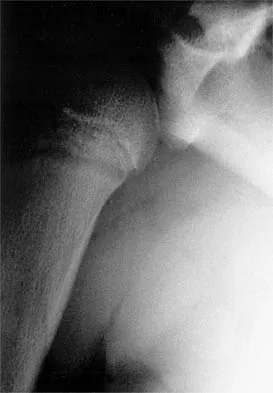
Explanation
It is critical to withhold active range of motion of the shoulder within the first 6 weeks after arthroplasty for acute fracture to prevent tuberosity avulsion. When radiographic and clinical findings show that the tuberosities are healed, active motion may be instituted, usually at 6 to 8 weeks. Immediate passive range-of-motion exercises, including external rotation with a stick, pendulum, and passive elevation, should begin within the limits of the repair on the day of surgery to prevent stiffness. Hartstock LA, Estes WJ, Murray CA, et al: Shoulder hemiarthroplasty for proximal humerus fractures. Orthop Clin North Am 1998;29:467-475.
Question 93
High Yield
Figure 6 shows the clinical photographs of a newborn who underwent a colostomy for an imperforate anus. Examination shows extended knees, flexed hips, and equinovarus feet. Dimpling is noted over the buttocks. Patients with these findings differ from patients with myelodysplasia in that they
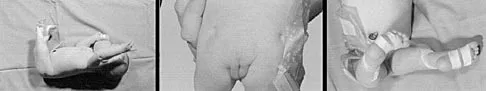
Explanation
The patient has sacral agenesis. Clinical signs include the classic dimpling over the buttocks and the characteristic lower extremity deformities. Imperforate anus is often associated with this disorder. Although motor function correlates with the level of vertebral defect, sensation is usually intact. This is important therapeutically, because patients are not as prone to pressure sores as are those with myelodysplasia. Kyphosis may develop in many patients with lumbosacral agenesis, but lordosis is unusual. Latex allergy and progressive neural deterioration may occur in patients with either myelodysplasia or sacral agenesis but is more common in the former.
Question 94
A 45-year-old woman who recently underwent biopsy of a lymph node in the right posterior cervical triangle now finds it difficult to hold objects overhead and has diffuse aching in the right shoulder region. What is the most likely diagnosis?
Explanation
The trapezius is innervated by the spinal accessory nerve. The nerve is superficial in the area of the posterior cervical triangle and is prone to injury during dissection. Paralysis of the trapezius causes loss of scapular stability when forward flexion or abduction of the shoulder is attempted. Vastamaki M, Solonen KA: Accessory nerve injury. Acta Orthop Scand 1984;55:296-299.
Question 95
Figure 7 shows a sagittal T1-weighted MRI scan. What muscle/tendon is identified by the arrow?
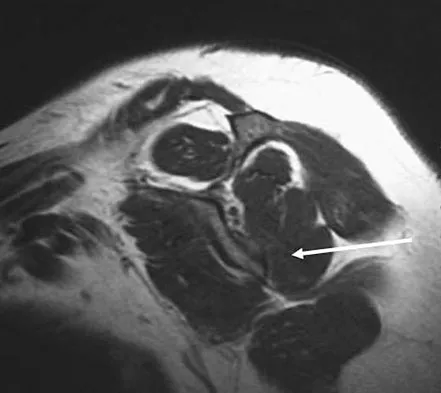
Explanation
The sagittal T1-weighted MRI scan is useful for interpreting the quality of muscle. The arrow is pointing to the teres minor. Goutallier D, Postel JM, Gleyze P, et al: Influence of cuff muscle fatty degeneration on anatomic and functional outcomes after simple suture of full-thickness tears. J Shoulder Elbow Surg 2003;12:550-554.
Question 96
A 3-year-old child has refused to walk for the past 2 days. Examination in the emergency department reveals a temperature of 102.2 degrees F (39 degrees C) and limited range of motion of the left hip. An AP pelvic radiograph is normal. Laboratory studies show a WBC count of 9,000/mm3, an erythrocyte sedimentation rate (ESR) of 65 mm/h, and a C-reactive protein level of 10.5 mg/L (normal < 0.4). What is the next most appropriate step in management?
Explanation
Examination reveals an irritable hip, creating a differential diagnosis of transient synovitis versus pyogenic hip arthritis. Kocher and associates described four criteria to help predict the presence of infection: inability to bear weight, fever, ESR of more than 40 mm/h, and a peripheral WBC count of more than 12,000/mm3. This patient meets three of the four criteria, with a positive predictive value of 73% to 93% for joint infection. Therefore, aspiration of the hip is warranted, with a high likelihood that emergent hip arthrotomy will be indicated. Ideally, intravenous antibiotics should be administered after culture material has been obtained from needle aspiration of the hip. An urgent bone scan is better indicated as a screening test for sacroiliitis or diskitis. If the arthrocentesis proves negative, CT or MRI of the pelvis may be indicated to rule out a pelvic or psoas abscess. Del Beccaro MA, Champoux AN, Bockers T, et al: Septic arthritis versus transient synovitis of the hip: The value of screening laboratory tests. Ann Emerg Med 1992;21:1418-1422. Kocher MS, Mandiga R, Zurakowski D, et al: Validation of a clinical prediction rule for the differentiation between septic arthritis and transient synovitis of the hip in children. J Bone Joint Surg Am 2004;86:1629-1635.
Question 97
A 55-year-old woman with a long history of low back and left lower extremity pain has failed to respond to exhaustive nonsurgical management. MRI scans show bulging and degeneration at L3-4 and L4-5 as well as a normal disk at L2-3 and L5-S1. She undergoes provocative lumbar diskography at L3-4, L4-5, and L5-S1. Post-diskography axial CT images of L3-4 and L4-5 are shown in Figures 6a and 6b, respectively. The injections at L3-4 and L4-5 produce no pain. The injection at L5-S1 produces 10/10 concordant back pain with radiation to the lower extremity. What is the most appropriate recommendation at this time?
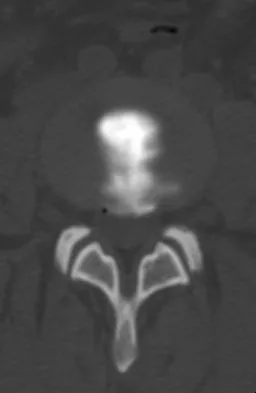
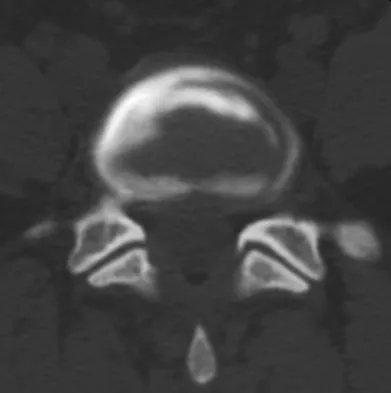
Explanation
The results of this patient's lumbar diskography are equivocal at best. The two disks most likely to be her pain generators, based on their MRI appearance, produced 10/10 pain, however it was nonconcordant and did not reproduce any of her typical left-sided radicular symptoms. The only disk that produced concordant back pain was the normal disk at the L5-S1 level and it reproduced radicular symptoms on the side opposite of her typical pain. Based on these findings, it would be difficult to select a level or levels to include in a lumbar fusion. As such, continued nonsurgical management is the safest treatment option at the current time. Brox and associates reported on a randomized clinical trial comparing lumbar fusion to cognitive intervention and exercise and found similar results in both groups, with significantly less risk in the latter. Brox JI, Sorensen R, Friis A, et al: Randomized clinical trial of lumbar instrumented fusion and cognitive intervention and exercises in patients with chronic low back pain and disc degeneration. Spine 2003;28:1913-1921.
Question 98
Which of the following procedures is considered most appropriate in patients with rheumatoid arthritis?
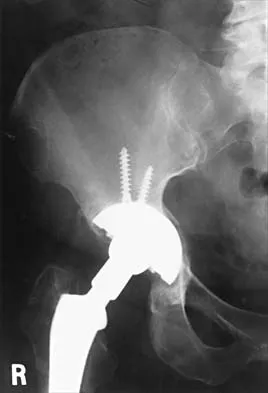
Explanation
Synovectomy of the knee prior to loss of articular cartilage has been shown to consistently relieve pain in patients with rheumatoid arthritis. Partial knee replacement will not arrest the process of joint destruction. Osteotomy of the hip has not been found to be a successful procedure in patients with rheumatoid arthritis. Hip arthrodesis should not be considered because of the multiarticular involvement in patients with rheumatoid arthritis. Core decompression of the hip has not been shown to save the femoral head because the necrosis appears to occur simultaneously with the inflammatory joint process. Granberry WM, Brewer EJ Jr: Early surgery in juvenile rheumatoid arthritis, in Calundruccio RA (ed): Instructional Course Lectures XXIII. St Louis, MO, CV Mosby, 1974, pp 32-37.
Question 99
A 27-year-old woman reports the acute atraumatic onset of burning pain in her right shoulder followed a week later by significant weakness and the inability to abduct her shoulder. One week prior to this incident she had recovered from a flu-like syndrome. Examination reveals full passive motion of the shoulder and the inability to actively raise the arm. Sensation in the right upper extremity is normal. Cervical spine examination is normal. Radiographs of the shoulder and cervical spine are normal. What is the most likely diagnosis?
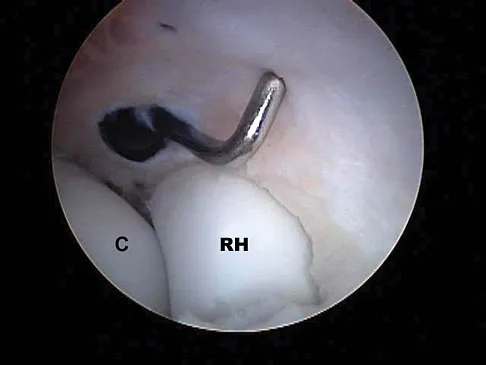
Explanation
The patient has symptoms and examination findings of acute brachial neuritis which is often a diagnosis of exclusion. The recent viral flu-like symptoms have shown a correlation with the development of this disorder. The acute, severe shoulder weakness excludes calcific tendinitis, impingement, and poliomyelitis. A normal cervical spine examination makes cervical disk disease unlikely. Turner JW, Parsonage MJ: Neuralgic amyotrophy (paralytic brachial neuritis). Lancet 1957;2:209-212.
Question 100
Iliosacral screws placed for stabilization of posterior pelvic ring injuries (eg, sacroiliac dislocation) that exit the sacrum anteriorly are most likely to injure which of the following structures?
Explanation
Iliosacral screws have gained popularity for posterior stabilization of pelvic ring disruptions, but complications attributed to incorrect placement are a clinical problem. The L5 nerve root is at greatest risk and is in closest proximity to a malpositioned screw (exiting the sacrum). The L4 root is more anterior at this level. The S1 root is still intraosseous at this level and is at risk but not from the screw exiting anteriorly at this level. The arteries are at risk but are more anterior and are at less risk than the L5 nerve root.
