Patient Presentation & History
Flexor Carpi Radialis (FCR) injuries in the pediatric population, while less common than distal radius fractures, represent a distinct and often diagnostically challenging entity requiring a high index of suspicion. The FCR tendon, originating from the medial epicondyle and inserting primarily into the base of the second metacarpal (with slips to the third), plays a crucial role in wrist flexion and radial deviation. Pediatric FCR injuries typically occur in older children or adolescents due to higher-energy mechanisms or sports-related trauma, contrasting with the more common plastic deformation or physeal injuries seen in younger children.
Our index patient is a 13-year-old male, otherwise healthy, with no significant medical comorbidities or history of connective tissue disorders. He presented to the emergency department following a fall during a skateboard accident. The mechanism of injury involved a significant impact to the volar aspect of the wrist after landing forcefully on an outstretched hand (FOOSH) while attempting a jump. He immediately experienced severe pain localized to the radial aspect of the volar wrist and noted an inability to effectively move his wrist, specifically commenting on weakness with attempted wrist flexion and radial deviation. There was no direct laceration or open wound, but swelling and ecchymosis developed rapidly. Prior to the fall, he denied any chronic wrist pain, previous injuries, or repetitive strain activities.
From a pediatric perspective, such a mechanism commonly results in distal radius fractures, often with associated physeal involvement (Salter-Harris types I, II, or III). However, the specific location of maximal pain and functional deficit, alongside the history of a high-energy impact directly to the volar wrist, prompted a broader differential, including soft tissue injuries. The patient's lack of chronic comorbidities simplified the pre-operative assessment regarding systemic health, but attention to the unique biomechanics and healing potential of pediatric tissues remained paramount.
Clinical Examination
Upon initial examination, the patient was in acute distress, guarding his right wrist.
Inspection:
There was marked diffuse swelling over the volar aspect of the right wrist, extending distally into the thenar eminence. Significant ecchymosis was evident along the radial border of the volar forearm and wrist. No obvious gross deformity of the distal radius or carpus was observed, and the skin integrity was intact without open wounds or signs of tenting. A subtle fullness or "bulge" was noted proximally in the forearm, potentially indicative of tendon retraction, while a divot or gap was not clearly palpable due to the acute swelling.
Palpation: Maximal tenderness was elicited directly over the course of the FCR tendon, approximately 3-4 cm proximal to the wrist crease, extending distally towards the trapezium. Palpation of the distal radius and scaphoid did not elicit the same degree of exquisite tenderness, though diffuse pain was present due to generalized swelling. No crepitus was detected. A careful "gap" in the FCR tendon could not be definitively appreciated due to significant overlying edema and muscle spasm. The median nerve tunnel and Guyon's canal were non-tender.
Range of Motion (ROM): Active ROM was severely restricted due to pain. He exhibited a complete inability to actively perform wrist flexion against gravity and could not radially deviate the wrist. Passive ROM was limited by pain, demonstrating approximately 30 degrees of flexion, 45 degrees of extension, 10 degrees of radial deviation, and 20 degrees of ulnar deviation. A classic finding in FCR rupture, the inability to palpate the FCR tendon during resisted wrist flexion and radial deviation, was observed. He could weakly flex his fingers and thumb, indicating relatively intact extrinsic flexors (FDS, FDP, FPL).
Neurological Assessment: Sensation to light touch and pinprick was intact in all dermatomes of the hand (median, ulnar, radial nerve distributions). Motor function of the median nerve, distal to the FCR, was assessed. He demonstrated full strength in thumb opposition (Opponens Pollicis) and abduction (Abductor Pollicis Brevis), indicating the integrity of the recurrent motor branch of the median nerve. This is a critical finding, as the FCR is innervated by the median nerve, and its injury can sometimes be associated with median nerve contusion or neuropraxia. The superficial radial nerve sensory branch was intact. Ulnar nerve motor and sensory functions were also preserved.
Vascular Assessment: Capillary refill was brisk in all digits (<2 seconds). Radial and ulnar pulses were strong and symmetrical bilaterally. No signs of compartment syndrome were present.
The initial clinical suspicion, based on the mechanism of injury, localized pain, palpable swelling, and specific deficit in resisted wrist flexion and radial deviation, was an FCR tendon injury, potentially a complete rupture or avulsion. The absence of gross bony deformity or focal tenderness over the distal radius and scaphoid helped narrow the differential.
Imaging & Diagnostics
Following the clinical examination, a structured imaging protocol was initiated to confirm the diagnosis, assess the extent of the injury, and rule out concomitant bony or ligamentous pathologies.
Plain Radiographs:
Standard anteroposterior (AP), lateral, and oblique views of the wrist were obtained. These showed no evidence of acute fracture or dislocation of the distal radius, carpal bones, or metacarpals. Specifically, there were no avulsion fractures noted from the trapezium, scaphoid, or second metacarpal base, which are common insertion points for the FCR or its slips. The distal radial physis (growth plate) appeared open and anatomically aligned, without signs of Salter-Harris injury. The absence of bony injury on plain radiographs, while reassuring for skeletal integrity, shifted the focus more definitively towards soft tissue pathology.
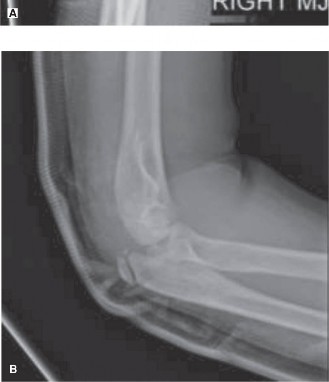
Figure 1: Representative plain radiographs (AP and lateral views) of a pediatric wrist. In this patient, radiographs were unremarkable for acute fracture or dislocation.
Ultrasound (US):
Given the strong clinical suspicion for a tendon injury and the absence of bony pathology on X-ray, a focused ultrasound examination of the wrist was performed. US is an excellent first-line imaging modality for superficial tendon injuries, offering dynamic assessment capabilities and avoiding ionizing radiation, which is particularly advantageous in the pediatric population. The ultrasound revealed a complete discontinuity of the FCR tendon, approximately 3 cm proximal to the wrist crease. The proximal stump was retracted by approximately 4 cm, with evidence of surrounding hematoma and fluid collection. The distal stump appeared irregular and frayed, residing near its insertion point. No significant bony avulsion fragments were definitively visualized. The flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) tendons appeared intact and gliding normally. The median nerve was visualized in its course, appearing structurally intact with no evidence of neuroma or significant swelling, though some contusion could not be entirely ruled out. The radial artery was also noted to be patent with normal flow.
Magnetic Resonance Imaging (MRI):
To further characterize the extent of the FCR injury, assess for associated ligamentous or cartilaginous damage, and confirm the exact location and degree of tendon retraction, an MRI of the wrist was subsequently performed. MRI is considered the gold standard for soft tissue evaluation. The MRI findings corroborated the ultrasound results, demonstrating a complete mid-substance rupture of the FCR tendon. The proximal tendon end was retracted significantly, approximately 4.5 cm from the original rupture site, consistent with the observed "bulge" on clinical inspection. The distal stump was identified near its insertion. Extensive surrounding edema and hemorrhage within the flexor compartment were noted. Crucially, the MRI also confirmed the absence of significant associated injuries to the carpal ligaments (e.g., scapholunate, lunotriquetral), triangular fibrocartilage complex (TFCC), or articular cartilage. The median nerve appeared edematous but anatomically continuous, suggesting a neuropraxic or mild contusion injury rather than a frank transection.
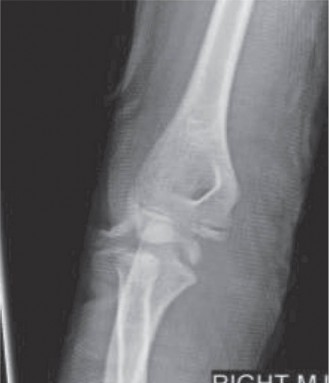
Figure 2: Coronal T2-weighted MRI image of the wrist demonstrating complete disruption of the FCR tendon (arrow), with associated fluid collection and edema.
Templating and Pre-operative Planning:
Based on the MRI, the degree of tendon retraction was quantified, which guided the surgical approach regarding the expected incision length and the necessity for potential tendon lengthening or graft material, though the relatively acute nature of the injury (within 48 hours) suggested direct repair would be feasible. The location of the rupture (mid-substance) also informed the choice of repair technique. The integrity of other flexor tendons and the median nerve was meticulously reviewed to prepare for any unexpected findings intraoperatively.
Differential Diagnosis
The presentation of acute radial-sided wrist pain and functional deficit in a pediatric patient warrants a comprehensive differential diagnosis. Distinguishing between these entities is crucial for appropriate management.
| Differential Diagnosis | Typical Presentation (Pediatric Context) | Key Clinical Findings | Imaging Modalities | Differentiating Features
FCR Rupture (Primary)
| Acute, significant pain radial side of wrist after forced wrist extension/abduction, especially with resisting flexion/radial deviation. Swelling, instability. Often after trauma. | Pain with resisted wrist flexion/radial deviation. Palpable divot/gap in tendon. Retraction of proximal stump (distinct bulge). Weakness in wrist flexion/radial deviation. Negative for significant bony tenderness. | Plain X-rays (rule out bony avulsion/fracture). Ultrasound (confirms tendon rupture, retraction, hematoma). MRI (gold standard for full characterization, associated soft tissue injuries, nerve involvement). | Loss of function specific to FCR. Imaging confirms tendon discontinuity. Absence of typical bony fracture signs. Specific point tenderness and inability to palpate FCR with activity. |
| Flexor Carpi Radialis (FCR) Rupture | Acute onset of severe pain, focal swelling, and a palpable defect over the FCR tendon. Often related to sudden, forceful wrist hyperextension/abduction or direct trauma. More common in older children/adolescents involved in sports. | Localized tenderness and ecchymosis over FCR. Inability to actively flex and radially deviate the wrist against gravity or resistance. Palpable gap in the FCR tendon often with a retracted proximal stump visible as a bulge. Negative specific bony fracture signs. | X-ray (initial rule out bony avulsion/fracture). Ultrasound (confirms tendon discontinuity, retraction, hematoma). MRI (confirms tear, location, degree of retraction, concomitant soft tissue injuries). |
| Distal Radial Fracture | FOOSH, typical pediatric fractures (often metaphysis). Pain and swelling localized to the distal forearm and wrist. Deformity possible. | Localized tenderness and swelling over distal radius. Deformity (dinner fork or garden spade). Pain with forearm rotation. Crepitus possible. Typically limited range of wrist and forearm motion due to pain. |
|
Distal Radius Fracture (e.g., Colles' or Smith's)
| Common in children, typically secondary to a fall onto an outstretched hand (FOOSH) with the wrist either hyperextended (Colles') or hyperflexed (Smith's). Presentation depends on severity; can range from subtle pain to overt deformity. | Significant localized tenderness and swelling over the distal radius. May have obvious deformity ("dinner fork" with Colles, "garden spade" with Smith). Pain exacerbated by wrist and forearm rotation. Often associated with decreased grip strength. Potential for neurovascular compromise (median nerve symptoms) if displacement is significant. | Plain X-rays (AP, lateral, oblique) are diagnostic, showing the fracture line, displacement, and physeal involvement (Salter-Harris classification). CT scan may be indicated for complex intra-articular fractures or surgical planning. MRI typically not needed unless soft tissue injury is suspected beyond the fracture. | Presence of clear bony fracture line on X-ray. Maximal tenderness directly over the distal radius rather than the FCR tendon itself. Deformity is often more pronounced. While FCR can be injured secondarily, the primary pathology is skeletal. |
| Scaphoid Fracture | Typically due to fall onto an outstretched hand (FOOSH), but may present insidiously with prolonged wrist pain and swelling. Often initially missed on radiographs. | Tenderness specifically in the anatomical snuffbox. Pain with scaphoid compression (e.g., thumb compression test). Pain with resisted radial deviation. Variable swelling; often less pronounced than distal radius fractures. | Plain X-rays (AP, lateral, oblique, Scaphoid views). If initial X-rays negative but clinical suspicion high, repeat X-rays in 10-14 days or consider MRI. CT scan for detailed fracture morphology and surgical planning. MRI is highly sensitive for occult scaphoid fractures. | Palpable tenderness is focused on the anatomical snuffbox, distinct from the FCR tendon or distal radius. Absence of FCR specific functional deficit. The diagnosis relies on targeted clinical findings and often advanced imaging due to high rate of occult presentation. |
| Scaphoid Fracture | Typically due to fall onto an outstretched hand (FOOSH), but may present insidiously with prolonged wrist pain and swelling. Often initially missed on radiographs. | Tenderness specifically in the anatomical snuffbox. Pain with scaphoid compression (e.g., thumb compression test). Pain with resisted radial deviation. Variable swelling; often less pronounced than distal radius fractures. | Plain X-rays (AP, lateral, oblique, Scaphoid views). If initial X-rays negative but clinical suspicion high, repeat X-rays in 10-14 days or consider MRI. CT scan for detailed fracture morphology and surgical planning. MRI is highly sensitive for occult scaphoid fractures. | Palpable tenderness is focused on the anatomical snuffbox, distinct from the FCR tendon or distal radius. Absence of FCR specific functional deficit. The diagnosis relies on targeted clinical findings and often advanced imaging due to high rate of occult presentation. |
| De Quervain's Tenosynovitis | Repetitive thumb or wrist movements (e.g., gaming, specific sports, new parental duties). Less common in true pediatric population, but seen in adolescents. Pain localized to the radial aspect of the wrist, aggravated by thumb and wrist motion. | Tenderness and swelling at the radial styloid. Positive Finkelstein test (pain with passive ulnar deviation of the wrist while the thumb is flexed into the palm). Pain with resisted thumb abduction and extension. | X-ray (rule out bony pathology, though typically normal). Ultrasound (shows thickening of the abductor pollicis longus and extensor pollicis brevis tendon sheaths, tenosynovitis). MRI (can confirm tenosynovitis and rule out other causes of pain). | Pain localized more proximally at the radial styloid. Symptoms worsen with specific thumb movements. Finkelstein test is highly specific. FCR function is typically preserved. |
| Scaphoid Fracture | Typically due to fall onto an outstretched hand (FOOSH), but may present insidiously with prolonged wrist pain and swelling. Often initially missed on radiographs. | Tenderness specifically in the anatomical snuffbox. Pain with scaphoid compression (e.g., thumb compression test). Pain with resisted radial deviation. Variable swelling; often less pronounced than distal radius fractures. | Plain X-rays (AP, lateral, oblique, Scaphoid views). If initial X-rays negative but clinical suspicion high, repeat X-rays in 10-14 days or consider MRI. CT scan for detailed fracture morphology and surgical planning. MRI is highly sensitive for occult scaphoid fractures. | Palpable tenderness is focused on the anatomical snuffbox, distinct from the FCR tendon or distal radius. Absence of FCR specific functional deficit. The diagnosis relies on targeted clinical findings and often advanced imaging due to high rate of occult presentation. |
| Scaphoid Fracture | Typically due to fall onto an outstretched hand (FOOSH), but may present insidiously with prolonged wrist pain and swelling. Often initially missed on radiographs. | Tenderness specifically in the anatomical snuffbox. Pain with scaphoid compression (e.g., thumb compression test). Pain with resisted radial deviation. Variable swelling; often less pronounced than distal radius fractures. | Plain X-rays (AP, lateral, oblique, Scaphoid views). If initial X-rays negative but clinical suspicion high, repeat X-rays in 10-14 days or consider MRI. CT scan for detailed fracture morphology and surgical planning. MRI is highly sensitive for occult scaphoid fractures. | Palpable tenderness is focused on the anatomical snuffbox, distinct from the FCR tendon or distal radius. Absence of FCR specific functional deficit. The diagnosis relies on targeted clinical findings and often advanced imaging due to high rate of occult presentation. |
| |
| | |
| | |
| | |
| | |
| | |
| | |
| | |
|
Scaphoid Fracture (Acute/Occult)
| Typically due to FOOSH, often subtle symptoms initially. Can manifest as persistent wrist pain, especially on the radial side, possibly with localized swelling. May be missed on initial X-rays. In children, physeal injuries around the scaphoid ossification center are also a consideration. | Tenderness in the anatomical snuffbox is the cardinal sign. Pain with scaphoid compression (e.g., direct pressure on the scaphoid tubercle or axial compression of the thumb). Pain with resisted radial deviation. Range of motion may be restricted due to pain, particularly wrist extension. Swelling may be minimal or diffuse. | X-rays (standard views including scaphoid series) are the initial imaging. If X-rays are negative but clinical suspicion remains high, repeat X-rays in 10-14 days after immobilization, or an MRI is highly sensitive for diagnosing occult scaphoid fractures or bone bruising. CT scan may be used for surgical planning if a fracture is confirmed. |
Differentiating from FCR Rupture:
The pain in scaphoid fracture is specifically localized to the anatomical snuffbox, distinct from the FCR tendon's course. While wrist flexion/radial deviation may be painful, there is typically no specific FCR tendon gap or loss of motor function. Imaging confirms bony pathology in scaphoid fractures, while FCR rupture is a soft tissue injury.
Differentiating from Distal Radius Fracture:
Tenderness is distinctly radial and carpal, not centered on the distal forearm. Deformity is absent. |
|
Scaphoid Fracture
| Acute, post-trauma (FOOSH), persistent localized pain on radial side of wrist, particularly in the anatomical snuffbox. May initially be missed on X-ray. Pediatric growth plate considerations near ossification centers. | Tenderness in the anatomical snuffbox. Pain with scaphoid compression (axial load on thumb). Pain with resisted radial deviation. Reduced range of motion (flexion, extension, radial deviation) due to pain. Swelling may be subtle. | Plain X-rays (standard views, specific scaphoid views). If clinically suspicious with negative X-rays, repeat X-rays in 10-14 days or order MRI. CT for complex fractures or pre-surgical planning. MRI is definitive for occult fractures and bone edema. |
Loss of FCR Function:
FCR rupture exhibits a distinct loss of active wrist flexion and radial deviation, accompanied by a palpable tendon gap. Scaphoid fracture pain is more localized to the bone, and FCR function is typically preserved, though painful.
Imaging:
X-rays are typically diagnostic for distal radius fractures; FCR rupture is confirmed by ultrasound/MRI. Scaphoid fractures are primarily diagnosed by X-ray (with high suspicion for occult fractures requiring further imaging). |
Surgical Decision Making & Classification
The decision to proceed with operative intervention for FCR injuries in pediatric patients is guided by several factors, including the type and severity of the injury, the patient's age and activity level, and the potential for functional compromise with non-operative management.
Why Operative vs. Non-operative?
*
Non-operative Management:
This is typically reserved for FCR tendinopathy, partial tears without significant functional deficit, or stable bony avulsions without displacement. Treatment involves immobilization (e.g., short arm cast or splint) for 4-6 weeks, NSAIDs, and progressive rehabilitation. The pediatric bone's remodeling potential can be advantageous for small, non-displaced bony avulsions. However, this approach carries a risk of chronic pain, weakness, and persistent instability, particularly in active adolescents.
*
Operative Management:
For a complete FCR tendon rupture, especially in an active adolescent like our patient, surgical repair is the preferred treatment. The primary indications for operative intervention include:
*
Complete tendon rupture:
As seen in our case, complete disruption of the tendon leads to significant functional impairment (loss of wrist flexion and radial deviation) and risks of chronic instability or tenodesis effect if left untreated.
*
Significant tendon retraction:
In our patient, MRI demonstrated 4.5 cm of retraction. Delayed presentation or significant retraction makes primary end-to-end repair challenging or impossible due to muscle contracture and scar tissue formation. Acute repair optimizes the chances of direct repair.
*
Displaced bony avulsion fracture:
If a fragment of bone is avulsed from the trapezium or second metacarpal and is significantly displaced, surgical fixation is indicated to restore anatomy and function.
*
Failure of conservative treatment:
For chronic partial tears or tendinopathy that do not respond to adequate non-operative measures.
*
High functional demand:
Active adolescents involved in sports will require restoration of full strength and function for optimal long-term outcomes.
For our patient, the complete mid-substance rupture of the FCR tendon with significant retraction warranted acute surgical repair to restore the tendon's continuity, prevent further retraction, and optimize functional recovery.
Classification:
While there isn't a universally adopted, specific classification system for FCR tendon injuries akin to Salter-Harris for physeal fractures or Schatzker for tibial plateau fractures, general principles of tendon injury classification apply:
1.
Partial vs. Complete Rupture:
This distinguishes between incomplete tears (tendon fibers partially intact) and full-thickness tears (complete disruption). Our patient had a complete rupture.
2.
Acute vs. Chronic:
Acute injuries are typically within 2-4 weeks of onset. Chronic injuries (beyond this timeframe) often involve tendon retraction, scarring, and degenerative changes, which can complicate repair and may necessitate tendon grafting. Our patient presented acutely.
3.
Location of Rupture:
*
Avulsion from insertion:
Often involves a bony fragment.
*
Mid-substance rupture:
As in our patient, often due to high-energy trauma.
*
Musculotendinous junction rupture:
Less common for FCR but possible.
In cases involving associated bony injury, relevant fracture classifications would also apply (e.g., Salter-Harris for distal radius physeal fractures). The decision-making process for FCR injuries primarily focuses on the integrity of the tendon (partial vs. complete) and the acuity of the injury, which dictate the urgency and type of intervention.
Surgical Technique / Intervention
The primary goal of surgical intervention for an acute FCR tendon rupture in a pediatric patient is anatomical reduction and robust repair of the tendon to restore its mechanical integrity and function, while minimizing morbidity and preserving surrounding neurovascular structures.
Anesthesia: The patient was placed under general anesthesia. A regional anesthetic block (interscalene or supraclavicular brachial plexus block) was also administered to provide post-operative analgesia and optimize surgical field conditions by reducing muscle tone.
Patient Positioning: The patient was positioned supine on the operating table. The affected arm was abducted to 90 degrees on a radiolucent hand table, with the forearm supinated. A tourniquet was applied to the upper arm and inflated after exsanguination to provide a bloodless field.
Surgical Approach:
1. A longitudinal skin incision was made over the volar aspect of the wrist, centered over the FCR tendon, extending from approximately 5 cm proximal to the wrist crease to the base of the second metacarpal. This length was determined based on the MRI findings of proximal tendon retraction (4.5 cm), ensuring adequate exposure to both the retracted proximal stump and the distal stump.
2. Careful dissection was performed through the subcutaneous tissues. The FCR tendon sheath was identified. Meticulous attention was paid to identifying and protecting critical neurovascular structures. The
radial artery
lies just radial to the FCR tendon in the distal forearm and wrist, and the
median nerve
is located ulnar to the FCR, deeper in the carpal tunnel. These were carefully identified, retracted, and protected throughout the procedure. The cutaneous branches of the median nerve were also protected.
3. The ruptured FCR tendon ends were identified. The proximal stump was significantly retracted within the forearm musculature. A gentle but persistent "milking" maneuver of the flexor muscle belly, combined with a "fishing" technique using a Babcock clamp or fine curved hemostat, was employed to retrieve the proximal end. The distal stump, often frayed, was located near its insertion into the base of the second metacarpal.
4. The tendon ends were debrided of any necrotic or severely contused tissue, freshening the edges to promote healing. The quality of the remaining tendon tissue was assessed. In this acute pediatric case, the tendon substance was robust and suitable for primary repair.
Reduction and Fixation Techniques:
1.
Tendon Approximation:
Once both tendon ends were clearly identified and prepared, the wrist was gently hyperflexed to relax the flexor compartment and facilitate approximation of the tendon ends without excessive tension.
2.
Repair Construct:
A modified Kessler suture technique was chosen for its strong biomechanical properties, providing excellent resistance to gapping and cyclic loading. This was reinforced with an epitendinous running suture.
* Four strands of 3-0 non-absorbable braided polyester suture (e.g., FiberWire) were used for the core modified Kessler repair. The sutures were passed through the tendon ends, taking large bites to maximize tendon-suture interface.
* Following the core repair, a 4-0 non-absorbable monofilament suture (e.g., Prolene) was used to perform an epitendinous running repair (e.g., modified Pennington technique) to enhance strength and smooth the repair site, minimizing adhesions.
3.
Tension Assessment:
After completing the repair, the wrist was gently moved through a range of motion to assess the tension and integrity of the repair. The repair was stable and allowed for passive wrist extension to approximately neutral without gapping.
4.
Associated Injury Management:
A thorough inspection of the surrounding structures was performed. No additional bony avulsions, ligamentous tears, or significant median nerve laceration were identified. The mild median nerve contusion noted on MRI was managed by ensuring adequate decompression of the carpal tunnel during closure to prevent further compression.
Closure:
1. The repair site was irrigated thoroughly.
2. The tendon sheath was loosely approximated with absorbable sutures (e.g., 4-0 Vicryl) to contain the repair and provide a biological environment, but not to constrict the tendon.
3. Subcutaneous tissues were approximated with absorbable sutures.
4. The skin was closed using a running subcuticular suture, followed by sterile strips and a soft, bulky dressing.
5. A custom-molded volar plaster splint was applied, immobilizing the wrist in approximately 30-40 degrees of flexion and slight radial deviation to protect the repair from tension. The splint extended from just distal to the elbow to the metacarpal heads, allowing full finger and thumb motion.
Post-Operative Protocol & Rehabilitation
A carefully structured post-operative rehabilitation protocol is critical to protect the FCR tendon repair, prevent complications, and restore optimal wrist function, especially in an active pediatric patient.
Phase I: Immobilization & Protection (Weeks 0-4/6)
*
Immobilization:
The wrist will be immobilized in a short arm cast or custom-molded orthosis with the wrist in approximately 30-40 degrees of flexion and slight radial deviation. This position minimizes tension on the FCR repair. The cast/splint will be worn continuously.
*
Elevation & Edema Control:
Strict elevation of the hand above heart level and regular ice application to reduce swelling.
*
Digit & Thumb ROM:
Active range of motion (ROM) exercises for the metacarpophalangeal (MCP) and interphalangeal (IP) joints of all fingers and the thumb (excluding active wrist motion) are initiated immediately to prevent stiffness and maintain circulation.
*
Shoulder & Elbow ROM:
Full active and passive ROM exercises for the shoulder and elbow are encouraged daily.
*
Weight Bearing:
No weight bearing through the affected wrist.
*
Medication:
Analgesics for pain management. NSAIDs may be used cautiously, considering their potential impact on tendon healing, but for a short duration if necessary for pain and inflammation.
Phase II: Controlled Mobilization (Weeks 4/6 - 8/10)
*
Splint Removal & Initiation of Motion:
At approximately 4-6 weeks post-surgery (depending on intra-operative repair stability and surgeon preference), the immobilization device is removed.
*
Passive ROM:
Gentle passive wrist ROM exercises are initiated under the guidance of a hand therapist. Emphasis on gradual increase in wrist extension, then flexion and deviation.
*
Active ROM:
Once passive motion is tolerated, active wrist flexion and radial deviation are cautiously begun, initially against gravity only. The progression is slow and controlled to avoid overstressing the healing tendon.
*
Soft Tissue Mobilization:
Scar massage and modalities (e.g., ultrasound, iontophoresis) to manage scar tissue and prevent adhesions, especially around the median nerve and radial artery.
*
Grip Strengthening:
Very light isometric grip exercises may be introduced, as long as they do not generate excessive FCR tension.
Phase III: Progressive Strengthening & Return to Function (Weeks 8/10 - 16/24)
*
Increased Resistance:
As tendon healing progresses and active ROM improves, strengthening exercises are gradually introduced. This includes isometric, then isotonic exercises for wrist flexion, extension, radial deviation, and grip strength, using light resistance bands, therapy putty, or small weights.
*
Proprioception & Dexterity:
Exercises to improve wrist stability, proprioception, and fine motor skills.
*
Dynamic Loading:
Introduction of more functional, dynamic movements, progressing towards activities of daily living.
*
Activity Modification:
Continue to avoid high-impact or high-load activities involving the wrist.
Phase IV: Return to Sport & High-Impact Activities (Weeks 16/24 +)
*
Sport-Specific Training:
Once adequate strength, flexibility, and pain-free range of motion are achieved, sport-specific drills and progressive return to activity protocols are initiated.
*
Gradual Return:
Full return to contact sports or high-demand activities typically occurs 4-6 months post-surgery, or when objective strength and functional tests meet specific criteria (e.g., >80-90% strength compared to contralateral limb, good proprioception).
*
Bracing:
Consideration of a protective brace for high-impact activities initially.
Potential Complications:
*
Re-rupture:
Primary concern, often due to premature or aggressive rehabilitation.
*
Wrist Stiffness:
Particularly loss of wrist extension, requiring further therapy or rarely, manipulation under anesthesia.
*
Adhesions:
Tendon adherence to surrounding structures, limiting glide and function.
*
Median Nerve Entrapment/Neuropathy:
Due to scarring or swelling around the nerve, requiring further decompression.
*
Infection:
Standard surgical complication, managed with antibiotics.
*
Complex Regional Pain Syndrome (CRPS):
Rare but debilitating, requiring early recognition and multidisciplinary management.
Close communication between the surgeon, physical therapist, and patient/family is paramount, especially in a pediatric population where compliance can be variable. Regular clinical assessments are essential to guide rehabilitation progression and identify potential complications early.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- High Index of Suspicion: For radial-sided wrist pain after trauma in an active pediatric patient, especially with weakness in wrist flexion and radial deviation, FCR injury must be on the differential, even if plain X-rays are normal. It can be easily missed if not specifically sought.
- Clinical Examination is Key: The inability to palpate the FCR tendon with resisted wrist flexion/radial deviation and the presence of a palpable gap or retracted muscle belly are highly indicative. Always compare with the contralateral wrist.
- Ultrasound as First-Line Imaging: Given its non-invasiveness, lack of radiation, and dynamic capabilities, ultrasound is an excellent initial diagnostic tool for suspected FCR tendon rupture in children, especially in acute settings.
- MRI for Confirmation and Associated Injuries: MRI is the gold standard for full characterization of the tendon injury (complete vs. partial, retraction), and crucial for ruling out concomitant soft tissue pathologies (ligamentous tears, cartilage injury, median nerve contusion).
- Acute Repair for Complete Ruptures: For complete FCR ruptures, particularly in adolescents with high functional demands, early surgical repair (within 2-3 weeks) is strongly advocated to prevent tendon retraction, muscle atrophy, and scar tissue formation, optimizing the chance of primary end-to-end repair.
- Anatomical Awareness: During surgical dissection, meticulous identification and protection of the radial artery (radial to FCR) and median nerve (ulnar and deep to FCR) are paramount to avoid iatrogenic injury.
- Robust Repair Technique: Employ biomechanically strong repair constructs (e.g., modified Kessler augmented with epitendinous sutures) to allow for safe, early controlled mobilization and reduce re-rupture rates.
- Controlled Rehabilitation: A gradual, protected rehabilitation protocol is essential. Initial immobilization in flexion/radial deviation, followed by controlled passive and then active ROM, is critical to allow adequate tendon healing while preventing stiffness. Patient/parent compliance is key in pediatric cases.
Pitfalls:
- Missed Diagnosis: The most significant pitfall. FCR injuries are often overshadowed by or misdiagnosed as more common wrist sprains or distal radius fractures, especially if X-rays are normal. Delay in diagnosis leads to tendon retraction, making primary repair more challenging and increasing the need for grafts.
- Inadequate Imaging: Relying solely on negative plain radiographs when clinical suspicion for soft tissue injury is high. This can lead to missed complete ruptures.
- Premature or Overly Aggressive Rehabilitation: Pushing rehabilitation too quickly, especially initiating active resistance before adequate tendon healing, is a major cause of repair failure and re-rupture.
- Failure to Address Concomitant Injuries: Overlooking associated carpal ligamentous injuries, median nerve contusion, or subtle bony avulsions can lead to persistent pain, instability, or neurological deficits despite successful FCR repair. A thorough pre-operative MRI helps mitigate this.
- Iatrogenic Neurovascular Injury: During surgical exposure, inadequate identification or protection of the radial artery or median nerve can lead to devastating complications. Careful, layer-by-layer dissection is imperative.
- Adhesion Formation: While part of the healing process, excessive scar tissue can lead to adherence of the FCR tendon to its sheath or adjacent structures, resulting in restricted glide and reduced function. Early controlled motion and soft tissue mobilization help, but can still be a challenge.
- Inadequate Tension at Repair Site: If the tendon ends are repaired under excessive tension, it can compromise healing or lead to repair failure. Conversely, if too lax, it may result in a weakened functional unit. Proper wrist positioning during repair is crucial.
- Poor Patient Compliance: In the pediatric population, adherence to strict immobilization and rehabilitation protocols can be challenging, directly impacting outcomes. Educating parents and patients thoroughly is vital.
