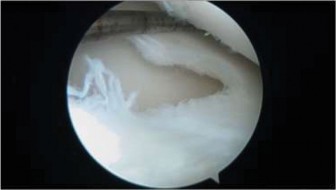
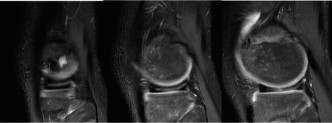
Patient Presentation & History
A 10-year-old male was referred to our Level I Pediatric Trauma Center following a high-energy, rotational injury to his right ankle sustained during a competitive soccer match. The patient reports being tackled from behind while his foot was planted, resulting in an immediate "pop" sensation, excruciating pain, and gross deformity. He was unable to bear any weight on the affected limb and was promptly immobilized at the scene by emergency medical services in a vacuum splint before transport.
His medical history is unremarkable, with no known allergies, bleeding diatheses, or underlying bone metabolic disorders. He is prepubescent, with Tanner stage II development. No previous orthopedic injuries or surgeries. His vaccination status is up-to-date.
Clinical Examination
Upon arrival, the patient was alert, oriented, and hemodynamically stable.
*
Inspection:
The right ankle exhibited significant swelling, diffuse ecchymosis, and a palpable, gross deformity with the foot externally rotated and displaced laterally relative to the tibia. There was notable skin tenting over the medial malleolus, raising concern for impending soft tissue compromise, but no open wounds or blistering were present. The overall skin integrity was intact, with no signs of blanching or severe skin wrinkling.
*
Palpation:
Marked tenderness was elicited over the distal metaphyseal region of the tibia, the distal fibula shaft, and the anterolateral aspect of the ankle joint corresponding to the tibiofibular syndesmosis. No overt compartment tension was palpable in the anterior, lateral, deep posterior, or superficial posterior compartments of the leg.
*
Range of Motion (ROM):
Active and passive ROM of the ankle were severely limited due to pain and gross mechanical disruption. Attempts at even gentle manipulation were met with significant guarding.
*
Neurological Assessment:
Sensation to light touch was intact in the distribution of the saphenous, superficial peroneal, deep peroneal, sural, and tibial nerves. Gross motor function of the toes (ankle dorsiflexion, plantarflexion, great toe extension) was present, though limited by pain.
*
Vascular Assessment:
Distal pulses (dorsalis pedis and posterior tibial) were strong and palpable bilaterally. Capillary refill in the toes was brisk (<2 seconds). The foot was warm and well-perfused. No signs of acute limb ischemia were noted.
Imaging & Diagnostics
Plain Radiographs:
Initial anteroposterior (AP), lateral, and mortise views of the right ankle were obtained.
*
AP View:
Demonstrated a completely displaced Salter-Harris Type II fracture of the distal tibia. The epiphysis and a large metaphyseal fragment (Thurston-Holland fragment) were displaced laterally and posteriorly relative to the main tibial shaft. There was a significant loss of tibiofibular overlap and clear space, indicating widening of the syndesmosis. The lateral malleolus appeared fractured.
*
Lateral View:
Confirmed the posterior and lateral displacement of the epiphyseal-metaphyseal complex. The metaphyseal component was clearly visible extending proximally from the physis. A significant posterior articular step-off was suspected.
*
Mortise View:
Clearly showed widening of the medial clear space and disruption of the tibiofibular syndesmosis, evidenced by an increased tibiofibular clear space (>5mm) and reduced tibiofibular overlap (<10mm) compared to the contralateral side. The distal fibula was fractured obliquely, approximately 3 cm proximal to the tip of the lateral malleolus.
*
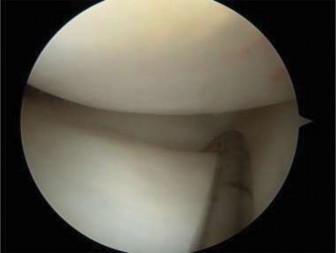
Computed Tomography (CT) Scan:
Due to the significant displacement, high-energy mechanism, and suspicion of articular involvement and syndesmotic disruption, a fine-cut CT scan with 3D reconstructions was performed.
*
Findings:
The CT scan provided critical information:
*
Distal Tibia:
Confirmed the Salter-Harris Type II fracture with a large, postero-lateral Thurston-Holland fragment. More importantly, 3D reconstructions and axial cuts revealed a subtle, non-displaced fracture line extending from the posterior aspect of the physis into the articular surface of the posterior tibial plafond. This identified a critical, albeit small, intra-articular component, making anatomical reduction imperative.
*
Distal Fibula:
The oblique fracture of the distal fibula was precisely characterized, confirming its location and non-comminuted nature.
*
Syndesmosis:
The CT provided definitive evidence of significant widening of the distal tibiofibular clear space and loss of overlap, confirming substantial syndesmotic disruption. No evidence of bony avulsion from the syndesmotic ligaments was noted, suggesting a purely ligamentous injury in this area.
*
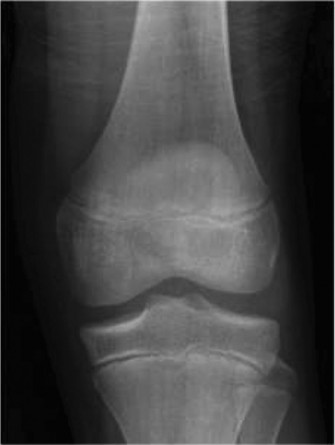
Pre-operative Templating:
Detailed pre-operative templating was performed using the CT images and contralateral ankle radiographs. This included:
* Assessment of fracture patterns to plan reduction sequence.
* Estimation of appropriate implant sizes for cannulated screws and K-wires.
* Visualization of potential screw trajectories to avoid the physis while achieving stable fixation.
* Planning for direct visualization of the articular surface and physis.
*
Differential Diagnosis
The following table compares the presented case features against potential differential diagnoses for pediatric ankle fractures.
| Condition | Key Features & Typical Presentation in Pediatrics |
Clinical & Radiographic Imaging