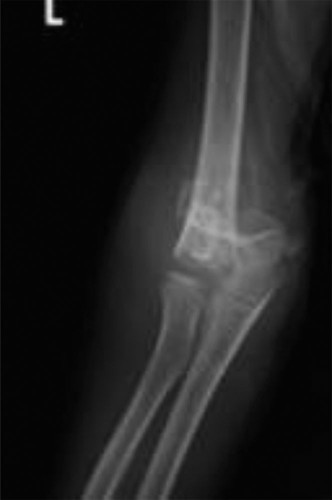
Pediatric Supracondylar Humerus Fractures: Case & Management
Patient Presentation & History
A 7-year-old right-hand dominant male presented to the emergency department following a fall from playground equipment. The reported mechanism of injury was a fall onto an outstretched hand (FOOSH) from approximately 1.5 meters height, with the elbow in extension. The patient immediately experienced severe pain, swelling, and inability to move his left elbow. There was no reported loss of consciousness or other associated injuries. The patient is otherwise healthy, with no significant past medical history or known allergies. Immunization status is up-to-date. Parents deny any history of chronic illness, bleeding disorders, or previous fractures.
Clinical Examination
Upon initial assessment, the patient was alert and cooperative, though distressed due to pain.
- Inspection: Gross swelling and ecchymosis were noted around the left elbow, extending distally. A clear S-shaped deformity of the distal arm was evident, with an obvious posterior displacement of the olecranon relative to the humeral shaft. Skin integrity was intact, with no open wounds or signs of impending skin compromise (e.g., fracture blisters).
- Palpation: Diffuse tenderness was elicited over the distal humerus, particularly in the supracondylar region. There was palpable crepitus with gentle attempted movement. The relationship between the olecranon and the medial and lateral epicondyles was obscured by swelling, but grossly abnormal.
- Range of Motion (ROM): Actively and passively, ROM of the left elbow was severely limited due to pain and guarding. Attempts at flexion and extension were met with resistance and increased pain. Pronation and supination were similarly restricted. No attempt was made to force movements.
-
Neurological Assessment:
A thorough neurological assessment of the left upper extremity was performed.
- Median Nerve: Intact sensation in the palmar aspect of the index finger and thumb. Motor function of flexor pollicis longus (FPL) and flexor digitorum profundus (FDP) to the index finger (anterior interosseous nerve, AIN) was assessed. The patient was able to make an "OK" sign, indicating intact AIN function. Thumb opposition (APB) was also intact.
- Ulnar Nerve: Intact sensation in the little finger and ulnar aspect of the ring finger. Motor function of finger abduction (interossei) was intact.
- Radial Nerve: Intact sensation over the dorsum of the first web space. Motor function of wrist extension and thumb extension (extensor pollicis longus, EPL) was intact.
- All deep tendon reflexes (biceps, brachioradialis, triceps) were diminished on the affected side due to pain.
- Vascular Assessment: Bilateral radial pulses were assessed and found to be symmetrical and strong. Capillary refill was less than 2 seconds in all digits of the left hand. The hand was warm and well-perfused with normal color. There was no evidence of pallor, paresthesias, or paralysis suggestive of acute vascular compromise.
Imaging & Diagnostics
Plain radiographs of the left elbow were obtained immediately in the emergency department. Standard anteroposterior (AP) and true lateral views were requested.
-
X-ray Findings:
- AP View: Revealed a complete transverse fracture through the supracondylar region of the distal humerus. The distal fragment was displaced posteriorly and medially relative to the humeral shaft. The olecranon-epicondylar axis was disrupted. Baumann's angle (the angle formed by a line drawn along the lateral epicondylar physis and a line along the lateral border of the humeral shaft) was measured at 55 degrees (normal range 64-81 degrees, with a difference of <4 degrees compared to the contralateral side being considered normal), indicating significant varus deformity.
- Lateral View: Demonstrated significant posterior displacement and angulation of the distal humeral fragment, with complete loss of cortical contact between the proximal and distal fragments. The anterior humeral line (a line drawn along the anterior cortex of the humeral shaft, which should normally bisect the capitellum on a true lateral view) passed entirely anterior to the capitellum. A prominent posterior fat pad sign was observed, indicating intra-articular effusion and fracture. The anterior fat pad (sail sign) was also evident. The coronoid fossa, which typically appears as a clear lucency above the capitellum, was obliterated by the displaced fragment. No obvious signs of intra-articular extension were noted.
(Figure 1: Pre-operative lateral radiograph demonstrating significant posterior displacement and angulation, classic for a Gartland Type III extension supracondylar humerus fracture. Note the disruption of the anterior humeral line and prominent posterior fat pad sign.)
-
CT/MRI Indications: In this case, given the clear radiographic findings and stable neurovascular status, neither CT nor MRI was indicated. These advanced imaging modalities are generally reserved for:
- Cases with equivocal plain radiographs (e.g., subtle Type I fractures where a posterior fat pad is the only sign, or uncertainty regarding physeal injury).
- Suspected intra-articular extension where open reduction is being considered.
- Complex fracture patterns, such as those with significant comminution or associated coronoid/radial head fractures.
- Evaluation of vascular injury when non-invasive methods (Doppler) are inconclusive or an arteriogram is not immediately available.
- Assessment of nerve entrapment, though often clinically evident.
-
Templating: Not typically required for routine supracondylar humerus fractures, as the goal is anatomical reduction and percutaneous pinning. However, pre-operative planning involves deciding on pin configuration (e.g., cross-pinning vs. lateral-only) and anticipating potential challenges during reduction.
Differential Diagnosis
Given the presentation of acute elbow trauma in a child, several other injuries must be considered in the differential diagnosis. A detailed comparison is presented below:
| Feature | Pediatric Supracondylar Humerus Fracture (Extension Type) | Lateral Condyle Fracture (Salter-Harris Type IV) | Radial Head/Neck Fracture | Medial Epicondyle Avulsion Fracture (often with dislocation) |
|---|---|---|---|---|
| Mechanism | FOOSH with elbow in extension. | FOOSH with valgus stress (often pushing off during fall). | FOOSH with valgus or axial compression. | Valgus stress with elbow dislocation; FOOSH. |
| Typical Age | 5-8 years (peak incidence). | 6-10 years. | 6-12 years. | 8-14 years. |
| Location of Pain/Swelling | Diffuse supracondylar region, often with distal extension. | Lateral aspect of elbow. | Radial aspect of elbow, especially with forearm rotation. | Medial aspect of elbow. Often severe swelling if dislocated. |
| Deformity | S-shaped deformity, posterior displacement of olecranon. Gunstock deformity if malunited. | Less obvious gross deformity; potential valgus prominence. | Minimal gross deformity; painful pronation/supination. | Medial prominence (if avulsed and displaced); frank dislocation deformity. |
| X-ray Findings (AP) | Transverse fracture line above condyles. Distal fragment displaced posteriorly/medially. | Oblique fracture line from metaphysis to articular surface, involving capitellum epiphysis. | Fracture line through radial neck/physis. Potential angulation. | Avulsed fragment from medial epicondyle. Check for entrapped fragment in joint. |
| X-ray Findings (Lateral) | Posterior displacement/angulation of distal fragment. Anterior humeral line anterior to capitellum. Prominent posterior fat pad. | Fracture line extending into articular surface. Posterior fat pad. | Angulation of radial head/neck. Anterior humeral line normal. Posterior fat pad. | Medial epicondyle fragment displaced anteriorly/inferiorly, often into joint. |
| Neurovascular Risk | High (median, AIN, radial, brachial artery). | Lower; potential for radial nerve injury (less common). | Lower; potential for posterior interosseous nerve injury. | High with dislocation (ulnar nerve). |
| Management | Gartland Type I: Cast. Type II, III, IV: Closed Reduction and Percutaneous Pinning (CRPP). Open reduction for failed CRPP or vascular compromise. | Non-displaced: Cast. Displaced: Open Reduction and Internal Fixation (ORIF). | Minimal displacement/angulation: Cast. Significant: ORIF or elastic nailing. | Non-displaced: Cast. Displaced/Entrapped: ORIF. Reduce dislocation first. |
| Key Differentiating Features | Classic supracondylar morphology, posterior displacement, high neurovascular risk. | Fracture extending into capitellum, usually intra-articular. | Radial head/neck angulation, painful rotation. | Medial epicondyle avulsion, associated dislocation, ulnar nerve involvement. |
Surgical Decision Making & Classification
Based on the clinical presentation and radiographic findings, this patient's injury was classified as a Gartland Type III extension-type supracondylar humerus fracture .
-
Gartland Classification (Extension Type):
- Type I: Non-displaced. Anterior humeral line intersects capitellum. Only radiographic sign may be posterior fat pad.
- Type II: Displaced posteriorly with an intact posterior cortex (hinge). Anterior humeral line is anterior to the capitellum.
-
Type III:
Completely displaced, with no cortical contact between fragments. Often significant rotation.
- IIIa: Posteromedial displacement (most common).
- IIIb: Posterolateral displacement (higher risk of radial nerve injury).
- Type IV (recently added): Multidirectional instability in flexion and extension. Both anterior and posterior periosteal hinges are torn, leading to instability in both planes. Rare, typically unstable after reduction.
Our patient exhibited complete displacement with loss of cortical contact, consistent with a Gartland Type III fracture. The posterior and medial displacement was clearly visible, further classifying it as a Type IIIa.
Decision for Operative Management:
Gartland Type III (and Type II significantly displaced/unstable after reduction, and Type IV) supracondylar humerus fractures are
indications for operative management
. Non-operative treatment of such displaced fractures leads to unacceptable rates of malunion (cubitus varus, "gunstock deformity"), stiffness, and functional impairment.
The primary goals of operative intervention are:
1. Anatomical or near-anatomical reduction of the fracture.
2. Stable fixation to maintain reduction until healing.
3. Minimizing iatrogenic complications.
4. Allowing early, protected range of motion to prevent stiffness.
Given the stable neurovascular status (warm, pink, good capillary refill, palpable radial pulse, intact neurological function), this was a semi-urgent case, scheduled for the first available operating theatre. Had the patient presented with a "white pulseless" limb (absent radial pulse, pallor, cold extremity), immediate operative intervention for reduction and potential vascular exploration would have been paramount. A "pink pulseless" limb, where the pulse is absent but perfusion appears adequate, often resolves with reduction and requires careful monitoring; however, vascular exploration may still be warranted if the pulse does not return.
Surgical Technique / Intervention
The patient underwent a closed reduction and percutaneous pinning (CRPP) procedure under general anesthesia.
- Patient Positioning: The patient was positioned supine on a radiolucent operating table. The affected left arm was placed on a hand table, ensuring full access for C-arm fluoroscopy in both AP and lateral planes. The shoulder was abducted to 90 degrees, and the elbow was positioned over a bolster to facilitate manipulation and allow for full flexion.
- Anesthesia and Preparation: General anesthesia was induced, and appropriate regional block (e.g., axillary block) was considered for post-operative pain control. The entire left upper extremity, from shoulder to hand, was prepped and draped in a sterile fashion. A tourniquet was applied to the proximal arm but not inflated initially, allowing assessment of vascularity post-reduction.
-
Closed Reduction Techniques:
- Traction: Initial gentle longitudinal traction was applied to the forearm with the elbow in slight flexion to disengage the fracture fragments and restore length. This addresses the posterior sag.
- Correction of Medial/Lateral Displacement: While maintaining traction, varus or valgus stress was applied to correct any medial or lateral displacement. In this case (posteromedial displacement), valgus stress was applied to correct the medial displacement.
- Flexion and Pronation/Supination: Once length was restored and medial/lateral displacement corrected, the elbow was slowly flexed. For posteromedial displacement, the forearm was pronated. For posterolateral displacement, supination would be indicated. This maneuver uses the triceps to reduce the posterior displacement. As the elbow flexes, the olecranon fossa cradles the olecranon, assisting in reduction.
-
Confirmation of Reduction:
C-arm fluoroscopy was used continuously to confirm reduction in both AP and true lateral views.
- Lateral View: The anterior humeral line was checked to ensure it bisected the capitellum. The posterior cortex should be aligned.
- AP View: Baumann's angle was assessed and compared to the contralateral side (if possible) or known norms. The carrying angle was evaluated, ensuring no residual varus or valgus malalignment. Medial and lateral condylar columns should be parallel. Oblique views were sometimes used to check for rotational alignment.
(Self-correction: The initial image shows a lateral view. I need to make sure the second image is integrated as well.)

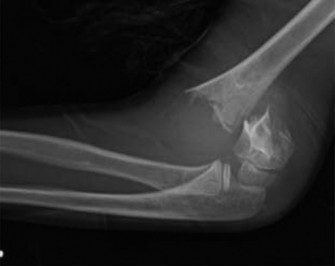
(Figure 2: Intra-operative fluoroscopic image after closed reduction, demonstrating restoration of the anterior humeral line through the capitellum and appropriate alignment. Pinning for stabilization is visible.) -
Fixation Construct (Percutaneous Pinning):
Once anatomical reduction was achieved and confirmed fluoroscopically, fixation with K-wires was performed. The elbow was maintained in approximately 70-80 degrees of flexion throughout the pinning process to maintain reduction and minimize soft tissue tension.-
Pin Configuration:
For Type III fractures, both cross-pinning and lateral-only pinning are viable options, each with advantages and disadvantages.
- Lateral-only pinning (two or three divergent pins): This approach minimizes the risk of iatrogenic ulnar nerve injury. Two pins are typically sufficient for stable fixation; a third can be added for increased rotational stability if needed. The pins are inserted from the lateral epicondylar region, angled proximally and medially, aiming for strong purchase in the medial humeral cortex. The entry points should be sufficiently lateral to avoid the radial nerve.
- Cross-pinning (medial and lateral pins): Historically considered the most rigid construct biomechanically. A lateral pin is inserted first, followed by a medial pin. The medial pin is inserted from the medial epicondyle, aiming proximally and laterally. Crucially, for cross-pinning, a small incision is made and the ulnar nerve identified and protected to avoid iatrogenic injury. This step is often performed under direct visualization. The medial pin is then inserted under fluoroscopic guidance, ensuring it does not impinge on the nerve.
-
Our Case:
Given the Gartland Type IIIa fracture with posteromedial displacement, a
cross-pinning technique
was chosen for maximal stability.
- Lateral Pin Insertion: Two 1.6 mm (0.062 inch) K-wires were inserted from the lateral epicondyle. The first pin was started just proximal to the lateral epicondyle, directed proximally, medially, and slightly anteriorly, aiming for the medial humeral cortex proximal to the olecranon fossa. The second lateral pin was inserted slightly more distally and directed more posteriorly, diverging from the first pin, also aiming for the medial cortex. Both pins provided good purchase and crossed the fracture site.
- Medial Pin Insertion: A small 1 cm incision was made just proximal to the medial epicondyle. The ulnar nerve was carefully identified and protected with a small blunt retractor. A third 1.6 mm K-wire was then inserted from the medial epicondyle, directed proximally, laterally, and slightly anteriorly, ensuring it avoided the ulnar nerve and crossed the fracture site into the lateral humeral cortex. The pin tips were checked to ensure they did not protrude excessively, which could cause soft tissue irritation or joint damage.
- Pin Placement Principles: All pins were inserted with a power drill and checked fluoroscopically for trajectory, divergence, and engagement of the contralateral cortex. The pins should diverge significantly, providing a broad base of support. The goal is at least three cortices engaged per pin for optimal stability (e.g., passing through both cortices of the distal fragment and one cortex of the proximal fragment).
- Final Assessment: After pinning, final AP and lateral fluoroscopic images were obtained to confirm pin placement, fracture reduction, and maintenance of Baumann's angle and anterior humeral line. The elbow was gently ranged to ensure no binding or impingement of the pins. The tourniquet was deflated, and the radial pulse was re-assessed immediately and found to be strong and symmetrical. Peripheral nerve function was re-checked, confirming no new deficits. The K-wires were bent and cut, leaving sufficient length outside the skin for ease of removal, and protected with pin caps. The small incisions were closed with sterile dressings. An above-elbow posterior splint was applied with the elbow at approximately 80-90 degrees of flexion and the forearm in neutral rotation.
-
Pin Configuration:
For Type III fractures, both cross-pinning and lateral-only pinning are viable options, each with advantages and disadvantages.
Post-Operative Protocol & Rehabilitation
The post-operative course focused on maintaining reduction, pain management, and preventing complications.
- Immobilization: The elbow was immobilized in an above-elbow posterior plaster splint, maintaining the elbow at approximately 80-90 degrees of flexion and the forearm in neutral rotation. This position helps maintain the fracture reduction and minimizes swelling. A circular cast was avoided initially due to the risk of compartment syndrome.
- Pain Management: A multimodal approach was employed, including regular acetaminophen and NSAIDs. The regional nerve block provided excellent pain relief in the immediate post-operative period.
- Pin Site Care: Pin sites were kept clean and dry, covered with sterile dressings changed daily by the nursing staff. Parents were educated on signs of infection.
- Neurovascular Monitoring: Rigorous neurovascular checks were performed every hour for the first 24 hours post-operatively, then every 4 hours for the next 24-48 hours. Patients were monitored for the "5 Ps" (pain, pallor, paresthesia, paralysis, pulselessness), indicative of potential compartment syndrome or neurovascular compromise. Any changes would necessitate immediate surgical review.
-
Follow-up Schedule:
- Day 1 Post-Op: A dedicated ward round to re-assess neurovascular status, pain control, and ensure comfort. A formal radiograph (AP and lateral) was obtained to confirm maintenance of reduction and pin position post-operatively.
- 1 Week Post-Op: Clinic visit for wound check, assessment of neurovascular status, and repeat radiographs (AP and lateral) to check for any loss of reduction. If swelling had subsided, the splint could be converted to a well-molded above-elbow fiberglass cast.
- 3-4 Weeks Post-Op: Clinic visit for repeat radiographs. By this time, early callus formation should be visible. If radiographic healing is progressing well and the fracture is clinically stable, the K-wires were removed in the clinic setting with local anesthesia. This is typically done with the child awake or with minimal sedation, ensuring a calm environment.
-
Rehabilitation:
- Immediately Post-Pin Removal: A supervised, gentle range of motion program was initiated. No forced movements, passive stretching, or heavy lifting were permitted. The goal was to allow the child to regain motion spontaneously.
- Weeks 4-6: Gradual increase in activities. Physiotherapy referral was made if active range of motion was significantly restricted (e.g., loss of >20 degrees flexion or extension) at 6 weeks post-pin removal. However, most children regain excellent functional range of motion spontaneously.
- 6-8 Weeks: Return to light activities.
- 3 Months Post-Op: Return to full activities, including sports.
Expected Outcome: Full recovery of range of motion and function is expected in the majority of well-managed supracondylar humerus fractures. Some residual loss of terminal extension (typically 5-10 degrees) is common but rarely functionally significant.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Thorough Neurovascular Assessment: This is paramount, both pre-operatively and post-operatively. Document deficits meticulously. Remember the "pink pulseless" vs. "white pulseless" distinction and their implications for urgency. A pulseless limb with a supracondylar fracture is an absolute orthopedic emergency.
- Recognize Gartland Classification: The cornerstone of management. Type I is managed conservatively; Type II (unstable), III, and IV require surgical intervention (CRPP).
- High-Quality Reduction: The most critical step. Spend sufficient time achieving an anatomical or near-anatomical reduction. Fluoroscopic evaluation in multiple planes (AP, lateral, obliques) is essential. The anterior humeral line and Baumann's angle are key radiographic indicators of reduction quality.
-
Appropriate Pin Configuration:
- Lateral-only pins: Preferred by many due to lower risk of iatrogenic ulnar nerve injury. Requires two or preferably three pins that are divergent and engage the medial cortex firmly to achieve rotational stability equivalent to cross-pinning.
- Cross-pins: Biomechanically very stable. If used, always identify and protect the ulnar nerve with a mini-open approach for the medial pin to prevent iatrogenic injury.
- Maintain Elbow Flexion during Pinning: Keeping the elbow flexed (around 70-80 degrees) during pinning helps maintain reduction, relaxes the brachial artery and median nerve, and minimizes tension on soft tissues.
- Assess for Entrapped Soft Tissues: Failed closed reduction should raise suspicion for soft tissue interposition (e.g., periosteum, median nerve, brachial artery). This necessitates open reduction.
- Delayed Surgery for Swelling/Blisters: If the limb is excessively swollen or fracture blisters are present, it is often prudent to delay definitive fixation for 24-48 hours (if neurovascularly stable) to allow swelling to subside and skin to recover. The arm can be placed in traction during this period.
Pitfalls:
- Inadequate Reduction: The most common cause of poor outcomes, primarily leading to cubitus varus (gunstock deformity). This is often due to residual rotation or poor alignment, not just angulation.
- Iatrogenic Ulnar Nerve Injury: A significant complication, particularly with unprotected medial pin placement in cross-pinning. Strict adherence to nerve protection protocols is essential.
- Missed Compartment Syndrome: Swelling post-injury or post-surgery can lead to compartment syndrome. Vigilant monitoring for the 5 Ps and a low threshold for compartment pressure measurement or fasciotomy are crucial.
- Pin Tract Infection: Can occur if pin site care is poor. Usually resolves with antibiotics, but can require early pin removal.
- Pin Migration/Back-out: Can lead to loss of reduction. Proper pin insertion depth and secure placement are key.
- Aggressive Physiotherapy: Forcing elbow range of motion post-pin removal can lead to heterotopic ossification and permanent stiffness. Gentle, self-directed range of motion is the preferred approach in children.
- Premature Pin Removal: Removing pins before adequate radiographic healing can lead to re-displacement. Follow appropriate timelines and radiographic signs of healing.
- Vascular Compromise: Failing to recognize a "white pulseless" limb as an emergency requiring immediate surgical exploration and reduction, possibly with a vascular surgeon on standby. Prolonged ischemia can lead to Volkmann's ischemic contracture.
- Misinterpreting Radiographs: Relying solely on one view or failing to assess all parameters (anterior humeral line, Baumann's angle, fat pads) can lead to missed or inadequately treated fractures. Comparing to the contralateral elbow for Baumann's angle can be helpful.
Clinical & Radiographic Imaging