Introduction & Epidemiology
Distal femoral fractures, defined as those involving the distal 9 cm of the femur, encompass fractures of the metaphyseal or articular region and the distal femoral epiphysis. These complex injuries represent approximately 6-7% of all femoral fractures, with open fractures accounting for 5-10% of cases. The unique anatomical and biomechanical characteristics of the distal femur render these fractures inherently challenging. They frequently present as comminuted and unstable injuries, notoriously difficult to achieve robust fixation. Given their proximity to the knee joint and frequent involvement of the articular surface, they carry a high risk of compromising knee joint function. Historical data and numerous reports indicate elevated rates of malunion, nonunion, and infection, firmly positioning distal femoral fractures among the most challenging injuries in orthopedic traumatology.
Key characteristics of complex distal femoral fractures include:
*
Severe intra-articular damage:
Direct involvement of the knee joint surface, often with significant chondral injury.
*
Extensive comminution:
Particularly in the metaphyseal and condylar regions.
*
Condylar compression or defects:
Resulting in loss of articular congruity and bone stock.
*
High-energy soft tissue injury:
Often accompanies the fracture, complicating surgical access, wound healing, and increasing infection risk.
*
Extension into the quadriceps extension mechanism:
Impairing early mobilization and rehabilitation.

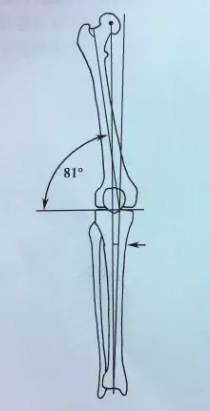
Figure 1: Complex intra-articular comminuted distal femoral fracture.
Surgical Anatomy & Biomechanics
The distal femur is a critical anatomical region characterized by its transition from a diaphyseal cylinder to a broad, triangular metaphyseal segment culminating in the bicondylar articular surface. Understanding this anatomy is paramount for successful management.
Gross Anatomy and Bony Architecture
The distal femur forms a crucial component of the knee joint. The flared metaphysis provides a large cancellous bone volume, which, while beneficial for osteointegration, can be prone to comminution in high-energy trauma or impaction in osteoporotic bone. The articular surface consists of two large condyles, medial and lateral, separated by the intercondylar notch.
-
Condylar Triangle:
The distal femoral condyles form a biomechanically stable "condylar triangle" in the coronal plane, with the articular surface and the medial and lateral cortices forming its sides. However, the intercondylar notch represents a relative weak point. Force directed superiorly or anteriorly can wedge the patella or another bony fragment into this notch, leading to a split of the condyles and resulting in T- or Y-shaped fractures that extend proximally into the supracondylar region.

Figure 2: The condylar triangle, highlighting the intercondylar notch as a potential weak point. -
Cortex and Cancellous Bone:
The supracondylar region represents a transition zone where cortical bone thins and cancellous bone density increases. This area is susceptible to comminution, often leading to significant bone defects. Loss of integrity in the condylar and supracondylar regions destabilizes the distal femoral triangle, disrupting the normal relationship of the articular surface.

Figure 3: Coronal view of the distal femur demonstrating the architectural transition from diaphyseal cortex to metaphyseal cancellous bone and condylar structure.

Figure 4: Axial view of the distal femur, highlighting the geometry of the condyles and intercondylar notch.

Figure 5: Sagittal view illustrating the curvature of the distal femur and articular surface.

Figure 6: Detailed anatomical illustration of the distal femur, indicating key landmarks and cortical thickness.

Figure 7: Antero-posterior view of the distal femur illustrating bone density distribution.

Figure 8: Lateral view depicting the distal femoral shaft and condylar anatomy.

Figure 9: Three-dimensional rendering of the distal femur, useful for understanding complex fracture patterns.
Ligamentous and Soft Tissue Attachments
The strong collateral ligaments (MCL, LCL), cruciate ligaments (ACL, PCL), and the extensor mechanism (quadriceps, patellar tendon) originate or insert around the distal femur. These soft tissue structures are frequently injured in conjunction with fractures and significantly influence fracture stability and fragment displacement.
Neurovascular Structures
The popliteal artery and vein, along with the tibial and common peroneal nerves, pass directly posterior to the distal femur. These critical neurovascular structures are highly vulnerable to direct trauma, stretch, or entrapment by fracture fragments, especially in displaced supracondylar fractures. Vascular injury incidence approaches 1/3 of cases. Nerve injury is less common, occurring in approximately 1% of cases.

Figure 10: Angiographic image depicting associated vascular injury in a distal femoral fracture.
Biomechanical Forces and Displacement
Understanding the deforming forces acting on distal femoral fractures is critical for accurate reduction and stable fixation.
*
Quadriceps and Sartorius:
These muscles cause proximal retraction and shortening of the distal fragment, particularly in supracondylar fractures.
*
Gastrocnemius:
Originating from the posterior aspect of the femoral condyles, the powerful gastrocnemius muscle causes significant posterior angulation and flexion of the distal fragment, making reduction challenging. This deforming force is a primary reason for characteristic posterior displacement.

Figure 11: Illustration of typical injury mechanisms and the resultant fracture patterns.

Figure 12: Diagram illustrating the primary muscular forces leading to fracture displacement.
Injury Mechanisms
Distal femoral fractures occur across all age groups but exhibit distinct patterns based on patient demographics and energy levels:
*
Younger Patients (<35 years):
Typically result from high-energy trauma such as motor vehicle accidents or falls from significant heights. These often present as open, highly comminuted fractures. The majority of these patients are male.
*
Elderly Patients:
More commonly associated with low-energy mechanisms, such as simple ground-level falls. A significant proportion (up to two-thirds) occur in individuals with underlying osteoporosis. The majority are elderly women.
Indications & Contraindications
The decision-making process for distal femoral fractures involves careful consideration of fracture characteristics, patient factors, and potential risks and benefits of operative versus non-operative management. While operative management is generally favored for displaced or unstable fractures, select cases may be treated non-operatively.
Indications for Operative Management
- Displaced or Unstable Fractures: Most distal femoral fractures, particularly those with articular involvement or significant metaphyseal comminution, require anatomical reduction and stable internal fixation to restore joint congruity and limb alignment.
- Intra-articular Fractures (AO/OTA Type 33-C): Requires meticulous anatomical reduction of the articular surface.
- Open Fractures: Surgical debridement and stabilization are mandatory to prevent infection and facilitate soft tissue management.
- Polytrauma Patients: Early stabilization (damage control orthopaedics) is often indicated to reduce systemic inflammatory response and facilitate patient care.
- Vascular or Neurological Compromise: Urgent surgical intervention may be required to address associated neurovascular injuries.
- Pathological Fractures: Stabilization often indicated for pain control and functional recovery.
Indications for Non-Operative Management
- Non-displaced or Minimally Displaced Extra-articular Fractures: Especially in patients with minimal functional demands.
- Medically Unstable Patients: For whom the risks of surgery outweigh the benefits, often managed with traction or bracing.
- Non-Ambulatory Patients or Those with Severe Comorbidities: Where the goal is comfort rather than functional restoration.
- Fractures in Patients with Limited Life Expectancy: Palliative care may be chosen.
Contraindications for Operative Management
- Severe Systemic Comorbidities: Uncontrolled medical conditions that make anesthesia and surgery excessively risky.
- Severe Local Soft Tissue Damage/Infection: Active infection or severely compromised soft tissue envelope precluding safe surgical incision and closure.
- Non-Viable Limb: In cases of devastating injury beyond salvage.
Table 1: Operative vs. Non-Operative Indications for Distal Femoral Fractures
| Feature | Operative Management | Non-Operative Management |
|---|---|---|
| Fracture Type | Displaced, unstable, intra-articular (33-C), open, comminuted | Non-displaced, minimally displaced extra-articular (33-A1) |
| Associated Injuries | Neurovascular compromise, compartment syndrome | No critical associated injuries |
| Patient Status | Polytrauma (DCO), otherwise healthy and active | Medically unstable, severe comorbidities, non-ambulatory |
| Soft Tissue Status | Adequate soft tissue envelope | Severe open wound, active infection, skin necrosis |
| Functional Goal | Restoration of anatomical alignment and joint function | Comfort, palliation |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is the cornerstone of successful management for distal femoral fractures. This includes comprehensive imaging assessment, surgical approach selection, implant choice, and detailed patient positioning strategies.
Imaging Assessment: "C CT MRIDOOPPLER 精准评估" (Precise Assessment with X-ray, CT, MRI, Doppler)
Precise assessment utilizing a multi-modal imaging approach is critical for understanding the complex three-dimensional fracture pattern, assessing associated soft tissue injuries, and planning surgical fixation.
*
Standard Radiographs:
Antero-posterior (AP) and lateral views of the distal femur including the knee joint and approximately 10-15 cm of the femoral shaft proximally. Oblique views may be helpful. These identify the fracture, displacement, and articular involvement.

Figure 13: AP radiograph of a distal femoral fracture.

Figure 14: Lateral radiograph showing a displaced distal femoral fracture.

Figure 15: Pre-operative AP radiograph of a complex distal femoral fracture (e.g., AO/OTA 33-C).

Figure 16: Pre-operative lateral radiograph of a complex distal femoral fracture.

Figure 17: Pre-operative oblique radiograph, providing additional insight into fracture morphology.

Figure 18: Radiograph depicting a severely comminuted intra-articular distal femoral fracture.

Figure 19: Pre-operative imaging demonstrating an open distal femoral fracture.

Figure 20: Pre-operative radiograph indicating a fracture extending into the femoral shaft.

Figure 21: Pre-operative radiograph of a high-energy distal femoral fracture with significant displacement.
-
Computed Tomography (CT) Scan: Essential for all intra-articular fractures. A CT scan with 1-2 mm cuts and 3D reconstructions provides invaluable detail regarding:
- Fracture pattern, fragment size, and displacement.
- Articular surface involvement and step-off/gap.
- Bone loss or impaction, especially in the condyles.
-
Pre-contoured plate selection and screw trajectory planning.

Figure 22: CT scan image demonstrating intra-articular involvement of a distal femoral fracture.

Figure 23: 3D CT reconstruction providing a comprehensive view of the fracture morphology.
-
Magnetic Resonance Imaging (MRI): Indicated when there is suspicion of significant soft tissue injury not visible on X-rays or CT, such as:
- Meniscal tears or collateral/cruciate ligament avulsions.
- Chondral damage not evident on CT.
- Occult osteochondral fractures.
- Assessment of quadriceps or patellar tendon integrity.
-
Doppler Ultrasound/Angiography: Crucial in cases with suspected vascular injury, clinical signs of ischemia, or grossly displaced fractures, especially those with significant posterior displacement. Doppler ultrasound can rapidly assess flow, while CT angiography (CTA) or conventional angiography provides detailed mapping of vascular compromise.
Pre-Operative Assessment and Templating
- Classification: Utilize AO/OTA classification (33-A, 33-B, 33-C) to standardize communication and guide treatment.
- Implant Selection: Based on fracture pattern, bone quality, and patient factors (e.g., locking plates for comminuted metaphysis, non-locking plates for simple fractures, intramedullary nails for select extra-articular or less comminuted patterns).
- Surgical Approach: Determine optimal approach (lateral, medial, dual) based on fracture morphology and soft tissue status.
- Contingency Planning: Anticipate potential challenges such as severe comminution, bone loss, or difficult reduction. Plan for bone grafting if needed.
Patient Positioning
- Supine on a Radioparent Table: Allows for intraoperative fluoroscopy in both AP and lateral planes.
-
Distal Femoral Traction:
Many surgeons prefer a traction table or skeletal traction (e.g., via a proximal tibial pin) to aid in length restoration and indirect reduction. However, a non-traction table with a large sterile bolster under the knee can also be used, providing greater flexibility for knee flexion and varied approaches.

Figure 24: Patient positioned supine on a radiolucent operating table, prepared for draping. - C-arm Access: Ensure unrestricted C-arm access for real-time imaging throughout the procedure.
Detailed Surgical Approach / Technique
The goal of surgical management is to achieve anatomical reduction of the articular surface, restore mechanical axis and length, and provide stable fixation that allows for early functional rehabilitation. The choice of approach and fixation technique depends heavily on the fracture pattern (AO/OTA classification), bone quality, and associated soft tissue injury.
General Principles
- Anatomical Reduction of Articular Surface: This is paramount for intra-articular fractures.
- Restoration of Mechanical Axis, Length, and Rotation: Crucial for long-term knee function and prevention of degenerative changes.
- Stable Fixation: Sufficiently strong to allow early mobilization while promoting biological healing.
- Minimally Invasive Techniques: Where feasible, to preserve soft tissue and vascularity.
Surgical Approaches
-
Lateral Approach (Lateral Parapatellar or Vastus Lateralis Split): Most common approach for distal femoral fractures, particularly for lateral locking plates.
- Incision: Longitudinal incision centered over the lateral femoral condyle, extending proximally along the lateral aspect of the thigh.
- Dissection: The vastus lateralis muscle is identified. A split can be performed along its fibers, or the muscle can be elevated anteriorly from the lateral intermuscular septum. Care is taken to identify and protect the peroneal nerve distally, particularly when extending dissection into the supracondylar region. The anterior femoral cutaneous nerve may be encountered.
-
Exposure:
Provides excellent visualization of the lateral femoral condyle, the lateral aspect of the articular surface, and the supracondylar region.

Figure 25: Marking of the standard lateral surgical incision for distal femoral plating.

Figure 26: Intraoperative image demonstrating the lateral approach with exposure of the distal femur.
-
Medial Approach (Medial Parapatellar or Subvastus): Used for fractures requiring medial plating, often in conjunction with a lateral plate (dual plating) for bicondylar fractures (33-C).
- Incision: Longitudinal incision along the medial aspect of the thigh, extending distally to the medial femoral condyle.
- Dissection: The vastus medialis can be elevated in a subvastus fashion, preserving its blood supply, or split. This approach exposes the medial femoral condyle and the medial aspect of the articular surface.
-
Anterior Approach (Quadriceps Snip/Osteotomy or Extensive Parapatellar Arthrotomy): Rarely used alone. Provides direct visualization of the entire articular surface but carries higher risks of quadriceps weakness and arthrofibrosis. Reserved for highly comminuted intra-articular fractures where direct visualization is critical and cannot be achieved otherwise.
Reduction Techniques
-
Articular Reduction: For intra-articular fractures (33-B, 33-C), the articular fragments must be anatomically reduced first.
- Direct Visualization: Often requires an arthrotomy. Articular fragments are reduced using small clamps (e.g., Jungbluth clamps), K-wires as joysticks, or pointed reduction clamps.
-
Lag Screws:
Once reduced, articular fragments are provisionally fixed with K-wires, then definitive fixation is achieved with lag screws (e.g., 3.5 mm cortical screws or headless compression screws) inserted from non-articular surfaces, achieving absolute stability.

Figure 27: Intraoperative image showing reduction of articular fragments with K-wires.

Figure 28: Direct reduction of a condylar fracture fragment.

Figure 29: Placement of a provisional K-wire for articular fragment stabilization.
-
Metaphyseal-Diaphyseal Reduction: Once the articular block is reconstructed, it is reduced to the femoral shaft.
- Indirect Reduction (Ligamentotaxis): Traction (either manual or skeletal) can help restore length and alignment, utilizing intact soft tissues to guide fragments. An external fixator temporarily applied from the distal femur to the tibia can assist in controlling length and rotation.
- Limited Open Reduction: Small incisions are used to manipulate fragments with reduction clamps or periosteal elevators, minimizing soft tissue stripping to preserve vascularity (biological fixation principles).
-
Direct Reduction:
In some cases, a more extensive exposure is necessary to directly reduce highly displaced or impacted fragments.

Figure 30: Use of a reduction clamp to achieve alignment of the metaphyseal fragments.
Fixation Techniques
The choice of implant depends on the fracture pattern, bone quality, and surgeon preference.
*
Locked Plating (LCP - Locking Compression Plate):
The current gold standard for most distal femoral fractures, especially comminuted metaphyseal and intra-articular patterns.
*
Principles:
LCPs provide angular stable fixation, acting as an internal fixator (bridge plating). Screws lock into the plate, creating a fixed-angle construct that bypasses areas of comminution, particularly beneficial in osteoporotic bone.
*
Application:
Plates are typically pre-contoured to match the anatomical curvature of the distal femur. They are applied laterally or medially (or both). Distal screws capture multiple condylar fragments, while proximal screws achieve strong fixation in the femoral shaft.

Figure 31: A typical distal femoral locking plate.

Figure 32: Intraoperative image showing a distal femoral locking plate being applied.

Figure 33: Intraoperative fluoroscopy image confirming plate position and screw trajectory.

Figure 34: Final intraoperative view of a laterally placed locking plate.

Figure 35: Post-fixation image demonstrating anatomical reduction and stable plating.

Figure 36: Radiographic confirmation of proper plate and screw placement.

Figure 37: Lateral radiograph showing a well-fixed distal femoral fracture with a locking plate.

Figure 38: Post-operative AP radiograph showing stable fixation with a distal femoral locking plate.

Figure 39: Post-operative lateral radiograph of a distal femoral fracture fixed with an LCP.
-
Retrograde Intramedullary Nailing: Primarily indicated for extra-articular (33-A) or simple intra-articular (33-C1) fractures without extensive condylar comminution or impaction.
- Advantages: Minimally invasive, preserves periosteal blood supply, load-sharing implant.
- Disadvantages: Risk of iatrogenic articular damage during nail insertion, difficult to control highly comminuted articular fragments, not ideal for significantly displaced condylar fractures.
-
Dual Plating: For highly comminuted bicondylar fractures (33-C3) or fractures with significant medial comminution/bone loss, a second plate (often a smaller T-plate or L-plate) can be placed medially in addition to the lateral locking plate. This provides enhanced stability against varus collapse.

Figure 40: Intraoperative image showing reduction and initial fixation with a lateral plate, contemplating additional medial support. -
Bone Grafting: If significant metaphyseal bone loss or defects are present, bone grafting (autograft or allograft) may be considered to support the articular surface and promote healing.

Figure 41: Biomechanical principle of bridge plating over a comminuted zone, allowing for bone healing.
Intraoperative Fluoroscopy
Continuous and meticulous use of fluoroscopy is essential to verify:
* Anatomical reduction of articular fragments (AP, lateral, oblique views).
* Restoration of mechanical axis, length, and rotation.
* Correct plate positioning and screw trajectories (avoiding joint penetration).
* Adequate stability of the construct.

Figure 42: Fluoroscopic image demonstrating initial reduction and provisional K-wire fixation.

Figure 43: Fluoroscopic image confirming satisfactory alignment after plate placement.

Figure 44: Final AP fluoroscopic view showcasing the definitive fixation.

Figure 45: Final lateral fluoroscopic view confirming screw lengths and articular congruity.

Figure 46: Post-operative radiograph confirming successful reduction and stable internal fixation.

Figure 47: Post-operative radiograph demonstrating satisfactory alignment in both AP and lateral planes.

Figure 48: Post-operative radiograph illustrating restoration of anatomical axes.

Figure 49: Post-operative radiograph showing comprehensive fixation of a complex distal femoral fracture.
Wound Closure
Meticulous wound closure is crucial, paying attention to the muscle layers, subcutaneous tissue, and skin. Adequate hemostasis is vital, and drains may be used selectively.
Complications & Management
Distal femoral fractures, due to their complexity, anatomical location, and often high-energy mechanism, are associated with a significant risk of complications. Proactive recognition and appropriate management are crucial for optimizing patient outcomes.
Table 2: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence | Etiology | Clinical Presentation | Management/Salvage Strategy |
|---|---|---|---|---|
| Nonunion | 5-20% | Inadequate stability, poor biology, infection, severe comminution, bone loss | Persistent pain, hardware failure, progressive deformity, no radiographic signs of healing |
Aseptic:
Revision fixation (stronger construct, compression), bone grafting (autograft/allograft with growth factors), IM nailing conversion.
Septic: Debridement, antibiotic treatment (local/systemic), temporary external fixation, staged revision internal fixation with bone grafting. |
| Malunion | 10-30% | Inaccurate reduction (angular, rotational, length), early weight-bearing in unstable constructs | Pain, altered gait, arthrosis, patellofemoral dysfunction, limb length discrepancy |
Mild/Asymptomatic:
Observation.
Symptomatic/Significant: Corrective osteotomy (intra-articular or supracondylar) with refixation, total knee arthroplasty (TKA) for severe arthritis. |
| Infection | 2-10% (higher for open) | Contamination, compromised soft tissue, hematoma, hardware | Pain, swelling, erythema, warmth, fever, purulent drainage, elevated inflammatory markers |
Acute (<4-6 weeks):
Irrigation & debridement (I&D), implant retention if stable, targeted antibiotics.
Chronic (>6 weeks): Hardware removal, extensive debridement, targeted antibiotics, possible temporary external fixation, delayed definitive reconstruction. |
| Arthrofibrosis/Stiffness | 10-25% (knee) | Prolonged immobilization, insufficient rehabilitation, extensive soft tissue trauma, intra-articular adhesions | Limited range of motion (ROM), pain, quadriceps contracture |
Early:
Aggressive physical therapy, continuous passive motion (CPM), manipulation under anesthesia.
Late/Refractory: Arthroscopic or open arthrolysis, quadricepsplasty. |
| Hardware Failure | 5-15% | Nonunion, excessive loading, poor bone quality, technical error, infection | Pain, instability, progressive deformity, hardware loosening/breakage |
Associated with Nonunion:
Treat nonunion (see above).
Without Nonunion: Revision fixation with stronger construct, potentially different implant (e.g., conversion to IMN or heavier plating). |
| Neurovascular Injury | <5% (vascular 1/3 in seed) | Direct trauma, entrapment by fragments, iatrogenic during surgery | Absent pulses, pallor, paresthesias, pain, paralysis, cold limb |
Vascular:
Urgent surgical exploration, repair/grafting by vascular surgeon.
Nerve: Observation for neurapraxia, neurolysis, rarely nerve repair/graft. |
| Post-traumatic Arthritis | Variable | Articular incongruity, chondral damage, malalignment | Chronic knee pain, swelling, stiffness, crepitus |
Mild:
Conservative management (NSAIDs, injections, activity modification).
Severe: Total knee arthroplasty (TKA). |
| Complex Regional Pain Syndrome (CRPS) | <1-5% | Idiopathic, nerve injury, prolonged immobility | Disproportionate pain, swelling, skin changes, allodynia, hyperalgesia | Multidisciplinary pain management, physical therapy, nerve blocks, sympathetic blocks. |

Figure 50: Radiograph illustrating a hypertrophic nonunion following distal femoral fracture fixation.

Figure 51: Radiograph demonstrating a malunion with significant angular deformity.

Figure 52: Radiographic evidence of hardware failure, likely secondary to nonunion.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for achieving optimal functional outcomes and preventing complications such as arthrofibrosis. Protocols are typically individualized based on fracture stability, fixation strength, soft tissue integrity, and patient compliance.
Phase 1: Immediate Post-Operative (Weeks 0-6)
- Goals: Control pain and swelling, protect fixation, initiate early range of motion (ROM), maintain muscle tone, prevent DVT.
-
Weight-Bearing:
- Non-weight-bearing (NWB) to Touch-down weight-bearing (TDWB): For most comminuted or intra-articular fractures, or those with tenuous fixation/poor bone quality.
- Partial weight-bearing (PWB): May be allowed earlier for stable extra-articular fractures fixed with intramedullary nails.
-
Range of Motion (ROM):
- Passive ROM: Initiated immediately. Continuous Passive Motion (CPM) machine may be used to assist.
- Active-assisted ROM: Progress as tolerated, focusing on knee flexion and extension.
- Knee Brace: Hinged knee brace typically worn for protection, locked in extension for ambulation, and unlocked for supervised ROM exercises.
-
Exercises:
- Isometric quadriceps and hamstring contractions.
- Ankle pump exercises to prevent DVT.
-
Gentle hip and ankle ROM.

Figure 53: Early knee flexion exercise under supervision.

Figure 54: Non-weight-bearing ankle and foot exercises to maintain circulation and range of motion.
Phase 2: Progressive Strengthening and Weight-Bearing (Weeks 6-12)
- Goals: Gradual increase in weight-bearing, achieve functional knee ROM, initiate strengthening.
- Weight-Bearing: Progress from TDWB/PWB to full weight-bearing (FWB) as radiographic signs of healing appear (callus formation across fracture lines). This typically occurs around 6-10 weeks but varies.
- ROM: Continue to work on achieving full knee flexion and extension.
-
Exercises:
- Closed kinetic chain exercises (e.g., mini-squats, leg presses) at appropriate resistance.
- Open kinetic chain exercises (e.g., knee extension/flexion machines) if deemed safe.
-
Proprioception and balance training.

Figure 55: Progressive weight-bearing exercises with assistance.
Phase 3: Advanced Strengthening and Return to Activity (Weeks 12+)
- Goals: Maximize strength, endurance, and proprioception; gradual return to functional activities, and eventually, sport-specific training if appropriate.
-
Exercises:
- Advanced resistance training (squats, lunges, step-ups).
- Agility drills, plyometrics (if cleared).
- Sport-specific training.
-
Return to Activity:
Varies greatly. Low-impact activities (swimming, cycling) can be introduced earlier. High-impact or demanding sports typically require 6-12 months, contingent on full fracture healing, strength recovery, and absence of pain.

Figure 56: Follow-up radiograph demonstrating advanced fracture healing at a later stage of rehabilitation.
Close communication between the surgeon and physical therapist is essential throughout the rehabilitation process to adjust protocols based on clinical progress and radiographic healing.
Summary of Key Literature / Guidelines
The management of distal femoral fractures has evolved significantly with advances in imaging, implant technology, and surgical techniques. Current literature emphasizes anatomical reduction, stable fixation, and early mobilization.
Classification Systems
-
AO/OTA Classification:
The most widely accepted system (33-A: extra-articular, 33-B: partial articular, 33-C: complete articular) provides a standardized framework for classifying these fractures, guiding treatment decisions, and facilitating research. Understanding the nuances of this classification is fundamental.

Figure 57: Diagram illustrating the AO/OTA classification system for distal femoral fractures.

Figure 58: Comprehensive overview of the AO/OTA classification subtypes for distal femoral fractures.

Figure 59: Representative images for different AO/OTA distal femoral fracture types.
Implant Evolution and Principles
- Conventional Plating (DCP/LC-DCP): Historically used, these plates rely on screw-to-bone compression. While effective for simple fracture patterns, they were associated with higher failure rates in comminuted or osteoporotic fractures due to inadequate angular stability.
-
Locking Plates (LCP): The introduction of locking plates revolutionized the treatment of distal femoral fractures. By providing fixed-angle constructs, LCPs offer superior angular stability, functioning as an internal fixator (bridge plating) to preserve periosteal blood supply and promote secondary healing, especially in comminuted metaphyseal fractures. Studies consistently demonstrate improved outcomes, particularly in elderly and osteoporotic patients, with lower rates of nonunion and hardware failure compared to conventional plates.

Figure 60: Schematic representation of the biomechanical advantage of locking plates over conventional plates.

Figure 61: Illustration of the fixed-angle stability provided by locking screw technology.

Figure 62: Comparison of stress distribution in traditional versus locking plate constructs.

Figure 63: Diagram illustrating the concept of biological fixation achieved with minimally invasive plate osteosynthesis (MIPO) techniques. -
Retrograde Intramedullary Nailing: While less commonly used for complex intra-articular fractures, retrograde IM nailing remains a viable option for specific extra-articular or minimally intra-articular fractures, especially those with minimal comminution. Advantages include load-sharing properties and a relatively less invasive approach. However, careful consideration of insertion portal and potential for iatrogenic knee pain is necessary.
Evidence-Based Recommendations
- MIPO Techniques: Minimally invasive plate osteosynthesis (MIPO) techniques are increasingly advocated to minimize soft tissue dissection, preserve fracture hematoma, and reduce biological insult, thereby enhancing healing potential and reducing infection rates.
- Anatomical Articular Reduction: For intra-articular fractures, achieving anatomical reduction of the joint surface with less than 2mm step-off is critical for preventing post-traumatic arthritis.
- Early Motion: Stable fixation allows for early, protected range of motion, which is crucial for preventing arthrofibrosis and promoting chondral healing.
- Management of Bone Loss: Significant bone loss, especially in the metaphyseal region, may necessitate bone grafting (autograft or allograft) to augment mechanical stability and promote osteogenesis.
- Polytrauma Settings: The principles of damage control orthopaedics (DCO) apply, often involving temporary external fixation followed by definitive internal fixation once the patient is physiologically stable.
Current guidelines emphasize the importance of meticulous pre-operative planning, precise anatomical reduction, stable internal fixation using modern locking plate technology, and structured post-operative rehabilitation to achieve optimal functional outcomes and minimize complications in patients with distal femoral fractures. The role of advanced imaging (CT, MRI, Doppler) in providing a "精準評估" (precise assessment) cannot be overstated in this complex patient population.
Clinical & Radiographic Imaging