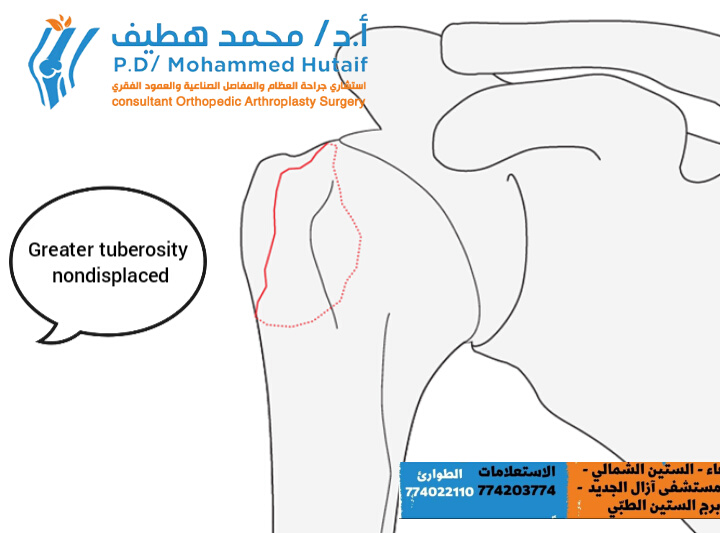
Extra Articular 2-Part, Greater Tuberosity, Non Displaced
 This fracture subgroup consists of fractures of the greater tuberosity which are truly not displaced. They heal typically very well under conservative treatment and do not tend to displace during the healing period.
This fracture subgroup consists of fractures of the greater tuberosity which are truly not displaced. They heal typically very well under conservative treatment and do not tend to displace during the healing period.
These fractures are unifocal extraarticular proximal humerus fractures involving the greater tuberosity. The greater tuberosity is the attachment of supraspinatus and infraspinatus tendons and its integrity is important for proper shoulder function. Proximal displacement, even as little as 5 mm, of a fracture of the greater tuberosity compromise shoulder abduction. This is due to tuberosity impingement on the coracoacromial arch and/or shortening of the involved rotator cuff tendons.
Extraarticular 2-part, greater tuberosity, displaced
 This fracture subgroup consists of fractures of the greater tuberosity which are superiorly and/or posteriorly displaced.
This fracture subgroup consists of fractures of the greater tuberosity which are superiorly and/or posteriorly displaced.
The typical displacement of the greater tuberosity is posterosuperiorly.
A displacement more than 5 mm is usually considered significant and should be treated surgically.
These fractures are unifocal extraarticular proximal humerus fractures involving the greater tuberosity. The greater tuberosity is the attachment of supraspinatus and infraspinatus tendons and its integrity is important for proper shoulder function. Proximal displacement, even as little as 5 mm, of a fracture of the greater tuberosity compromise shoulder abduction. This is due to tuberosity impingement on the coracoacromial arch and/or shortening of the involved rotator cuff tendons.
Extraarticular 2-part, tuberosity, dislocation
 These fractures are those associated with glenohumeral dislocations. The vast majority involve the greater tuberosity. Occasionally, a posterior dislocation results in avulsion of the lesser tuberosity. Very rarely, so-called luxatio in erecta is associated with a greater tuberosity fracture. All such fracture dislocations should be reduced promptly. Beware of a possible occult metaphyseal fracture that may displace during closed reduction (converting the fracture to a 3- or 4-part fracture). Tuberosity displacement must be reassessed after glenohumeral reduction, since it may not require surgical repair. With any glenohumeral fracture dislocation, an open reduction may be necessary.
Extraarticular 2-part fracture of surgical neck with impaction
These fractures are those associated with glenohumeral dislocations. The vast majority involve the greater tuberosity. Occasionally, a posterior dislocation results in avulsion of the lesser tuberosity. Very rarely, so-called luxatio in erecta is associated with a greater tuberosity fracture. All such fracture dislocations should be reduced promptly. Beware of a possible occult metaphyseal fracture that may displace during closed reduction (converting the fracture to a 3- or 4-part fracture). Tuberosity displacement must be reassessed after glenohumeral reduction, since it may not require surgical repair. With any glenohumeral fracture dislocation, an open reduction may be necessary.
Extraarticular 2-part fracture of surgical neck with impaction
General considerations
These fractures are unifocal extraarticular proximal humerus fractures with metaphyseal impaction, sometimes referred to as surgical neck fractures.
The distinguishing features of these fractures are a) their transmetaphyseal location at the level of the surgical neck and b) their impaction. Because of the latter, they are quite stable and are typically treated conservatively.
If stability is in doubt, fracture assessment under image intensification is helpful. The fractures can be further characterized by their direction of angulation, primarily varus or valgus.
Fracture without frontal malalignment

The fractures of this subgroup are without frontal malalignment. They may be posteriorly or anteriorly impacted. This will be shown on the axillary lateral or scapular Y view.
Fracture with varus malalignment

Fractures of this subgroup have varus malalignment. Their impaction may be purely varus or associated with apex anterior or posterior angulation.
Fracture with valgus malalignment

Fractures of this subgroup have valgus malalignment. Their impaction may be either pure valgus or associated with apex anterior or posterior angulation.